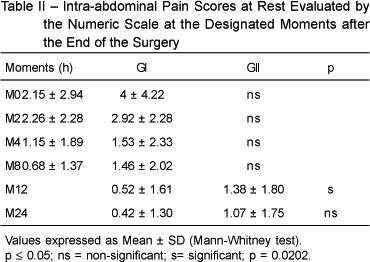
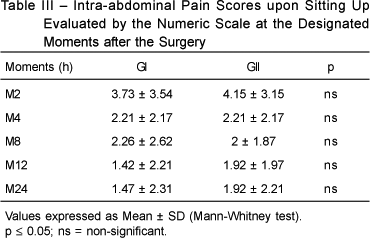
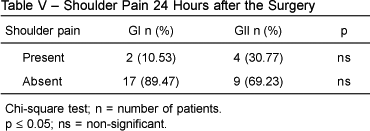
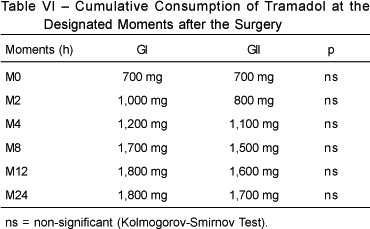
BACKGROUND AND OBJECTIVES: The analgesic effect of intraperitoneal administration of local anesthetics after laparoscopic cholecystectomy is a controversial issue, and the results described vary from considerable pain relief to little reduction in pain. The objective of this study was to evaluate the efficacy of the intraperitoneal administration of 50% enantiomeric excess bupivacaine (S75-R25) for the postoperative pain relief of laparoscopic cholecystectomy. METHODS: A randomized, double blind, placebo controlled study was conducted with 40 patients undergoing laparoscopic cholecystectomy, who were divided in two groups: GI (n = 20) received 80 mL of intraperitoneal 0,125% S75-R25 bupivacaine at the end of the procedure; and GII (n = 20) received 80 mL of intraperitoneal normal saline. Both groups received 40 mg of tenoxicam and 30 mg.kg-1 of intravenous dypirone shortly before the end of the surgery. Tramadol was used for postoperative analgesia (PO). Pain scores were evaluated at rest, sitting up, and during the Valsalva maneuver, according to a numeric scale upon waking up and 2, 4, 8, 12, and 24 hours postoperatively; the presence of shoulder pain was assessed, as well as the length of time until the first request of analgesic and its cumulative consumption. RESULTS: There was a statistically significant difference in resting pain scores at 12 hours PO (GI < GII). The length of time until the first request of tramadol was greater in GI and this group presented smaller consumption of this drug, but these differences were not statistically significant. CONCLUSIONS: The intraperitoneal instillation of 80 mL of 0.125% S75-R25 bupivacaine provided for lower resting pain scores, which was statistically significant only at the 12th postoperative hour.
ANALGESIA; ANESTHETICS, Local; ANALGESIC TECHNIQUE; SURGERY, Abdominal