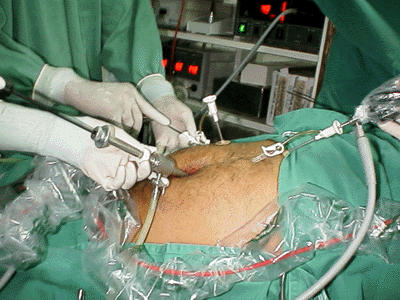
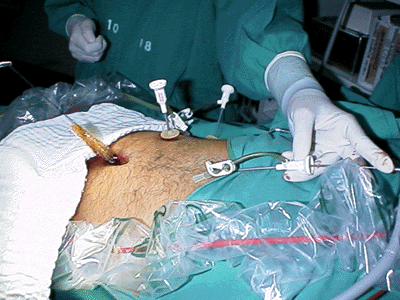
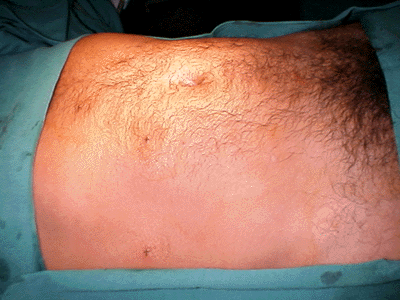
Os autores descrevem a técnica que utilizaram para a realização da colecistectomia agulhascópica no Núcleo de Hospital de Aeronáutica de Manaus, de setembro de 1997 a maio de 1999, e os resultados iniciais obtidos em 83 pacientes (11 do sexo masculino e 72 do feminino, com idades variando de 17 a 87 anos) portadores de doenças da vesícula biliar. Empregaram, além de um equipamento completo de videolaparoscopia, um equipamento acessório composto de um monitor de vídeo, uma microcâmera, com seu processador de imagens, e uma fonte de luz, tudo para o laparoscópio de 1,7 mm MiniSite®. A operação foi realizada principalmente sob monitoramento videolaparoscópico de 10 mm pelo portal umbilical e por meio de três portais de 2 mm (epigástrico, hipocôndrio direito e flanco direito). Utilizou-se o videolaparoscópio de 2 mm pelo portal epigástrico quando se procedeu às ligaduras císticas, ocasião em que o laparoscópio de 10 mm umbilical era substituído pelo aplicador de clipes de 10 mm. Da mesma forma, a vesícula foi retirada da cavidade abdominal pelo portal umbilical sob monitoramento videolaparoscópico de 1,7 mm epigástrico. A maioria dos casos operados (89,2%) não apresentava espessamento da parede vesicular. O tempo cirúrgico médio do procedimento foi de 92 ± 21 min e o de internação foi de 16 h. A principal intercorrência operatória foi a perfuração da vesícula biliar (41%), atribuída à curva de aprendizado no método por que passa a equipe. Vômitos foram a principal complicação pós-operatória (51,8%), não tendo havido infecção de ferida operatória. Oitenta e dois por cento dos casos puderam ser terminados pelo método agulhascópico puro, enquanto em 6% e 3,6%, respectivamente, houve necessidade de trocar um dos portais de 2 mm por um de 5 ou de 10 mm e de converter o procedimento para videolaparoscopia usual. Em 6% dos casos, por problemas de imagem com o microlaparoscópio, realizou-se o procedimento agulhascópico com a assistência de um portal suprapúbico de 10 mm. Dois casos (2,4%) tiveram que ser convertidos para laparotomia convencional, um por problemas operacionais com o equipamento e outro por dificuldades técnicas transoperatórias. Os autores concluem ser o procedimento agulhascópico factível, demandar uma nova curva de aprendizado por parte da equipe e ser demorado em virtude das características de seus instrumental e equipamento.
Colecistectomia; Laparoscopia; Microlaparoscopia; Cirurgia de invasão mínima