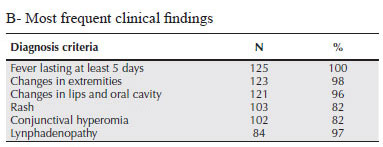
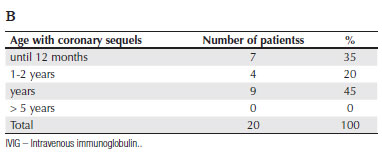
OBJECTIVES: To describe a population of children diagnosed with Kawasaki's disease (KD) in pediatric rheumatology centers of Rio de Janeiro, Brazil, defining the magnitude of the delay period in diagnosing KD and initiating treatment due to confusion with common childhood febrile illnesses and the impact of this delay on the frequency of coronary sequels. METHODS: Data analysis from hospital records summarized in a dedicated form, including name, gender, age, date of first recorded clinical signs, date of admission to the specialty service, information about symptoms, clinical evolution, intravenous immunoglobulin (IVIG) use and coronary sequels. RESULTS: Of 125 patients, 63% were males. 40% were under 2 years at diagnosis. Average lapse between earliest signs and KD diagnosis was 12 days (mean fever duration, 14 d). Only 22.4% had a diagnosis of KD before entering the specialty service. For the remainder, initial hipotheses included: bacterial (60%) and viral infections (12%), rheumatological diseases (4%) and adverse vaccination reactions (1.6%). Hence, prevalent febrile illnesses of childhood were major confounding factors. For records (85.6%) mentioning treatment, 46.7% reported IVIG treatment, beginning after day 10 in 23 cases (21.5%). 20 patients (16%) presented coronary sequels, 9 of which were diagnosed late, including 3 given IVIG after day 10, and 6 given no IVIG. We found no significant association between the frequency of coronary sequels and: a) sex; b) age; c) clinical criteria; d) initiation of IVIG treatment (before or after day 10). CONCLUSIONS: Common febrile illnesses of childhood often confound the diagnosis of KD.
vasculitis; mucocutaneous lymph node syndrome; coronary artery disease; antibiotic prophylaxis