Abstracts
BACKGROUND: Infection with hepatitis-B virus has been a significant cause of morbidity claiming more than a million lives every year. Epidemiological data reveals that there are 360 million carriers of hepatitis-B virus throughout the globe and 78% of the world populations’ hail from Asia. Though several studies from Indian sub-continent have provided an estimate of the prevalence of this viral infection, there exist only few studies, which reflect the status in the general population. AIM: The present study was designed to investigate the prevalence of hepatitis-B infection in North Indian general population. METHODS: The study population comprised of 20,000 healthy blood donors who were screened for hepatitis-B surface antigen (HBsAg) status using third generation ELISA kit. Seroprevalence rate of seropositive donors was calculated and stratified by age, sex and blood groups. Statistical analysis was performed using tests of proportions, chi-square and confidence interval. RESULTS: The study showed that out of 20,000 donors, 450 (2.25%) were HBsAg positive (95% confidence interval (CI), 2.0445-2.4554). Higher prevalence of HbsAg was found among males (440/19235) than females (10/765). The age specific prevalence rose from 1.78% (108/6058) in donors aged 19-25 years to a maximum of 3.03% (96/3161) in donors aged 35-45 years and decreased in older age groups. The peaks were detected in male donors aged 35-45 years and in females aged 25-35 years. Rh-negative blood group donors (21/873) and Rh-positive group donors (429/19127) had almost equivalent prevalence rates of HBsAg. HBsAg was more prevalent in blood group B donors (174/7426) and less prevalent in AB blood group donors (38/2032). CONCLUSION: It was found that variables including gender and age were significantly associated with HBsAg positivity. HBsAg positivity in our population was statistically not associated with ABO blood groups.
Hepatitis-B virus; Hepatitis B surface antigen; Blood donors; Seroepidemiologic studies; Risk factors; India
RACIONAL: A infecção pelo vírus B da hepatite é considerada uma significante causa de morbidade, responsável por mais de 1 milhão de casos, a cada ano. Dados epidemiológicos revelam que existem 360 milhões de portadores de vírus da hepatite B no mundo e 78% da população natural da Ásia. Embora vários estudos realizados na Ásia sub-continental tenham fornecido uma estimativa de prevalência desta infecção viral, existem poucos estudos que avaliam esta condição na população geral. OBJETIVO: Investigar a prevalência da infecção pelo víirus B da hepatite na população geral do nordeste da Índia. MÉTODOS: A população estudada compunha-se de 20.000 doadores de sangue sadios, selecionados através de positividade do antígeno de superfície da hepatite B (HBsAg), utilizando-se o kit ELISA de 3ª geração. A taxa de soroprevalência dos doadores soropositivos foi calculada e estratificada por idade, sexo e grupos sangüíneos. Análise estatística foi obtida usando-se testes de proporções, do qui ao quadrado e intervalo de confiança (CI). RESULTADOS: O estudo revelou que dos 20.000 doadores, 450 (2,25%) eram HBsAg positivos (95% CI 2.0445-2.4554). Prevalência maior de HBsAg foi encontrada em homens (440/19235) do que em mulheres (10/765). A prevalência por faixa etária aumentou de 1,78% (108/6058) em doadores entre 19 a 25 anos, para máximo de 3,03% (96/3161) naqueles entre 35-45 anos e decresceu nos grupos de maior idade. Os picos foram detectados em doadores masculinos de 35-45 anos e em mulheres de 25-35 anos. O grupo de doadores Rh negativo (21/873) e o grupo Rh positivo (4299/19127) mostraram taxas de prevalência de HBsAg quase equivalentes. HBsAg foi mais prevalente no grupo de doadores de tipo sangüíneo B (174/7426) e menos no grupo de tipo sangüíneo AB (38/2032). CONCLUSÃO: Verificou-se que variáveis incluindo gênero e idade foram significantemente associadas à positividade do HBsAg e que esta não foi estatisticamente associadas aos grupos sangüíneos ABO.
Vírus da hepatite B; Antígenos de superfície da hepatite B; Doadores de sangue; Estudos soroepidemiológicos; Fatores de risco; Índia
ARTIGO ORIGINAL ORIGINAL ARTICLE
Seroprevalence and risk factors for hepatitis B virus infection among general population in Northern India
Soroprevalência e fatores de risco para infecção pelo vírus da hepatite B na população geral do nordeste da Índia
Rachna BehalI; Renu JainII; Krishan K. BehalI; Ajay BhagoliwalIII; Nakshatra AggarwalIV; T. N. DholeV
IDepartment of Faculty of advanced studies in the Life Sciences, CSJM University, Kanpur, India
IIDepartment of Pathology, GSVM Medical College, Kanpur, India
IIIDepartment of Social and Preventive Medicine, SN Medical College, Agra, India
IVRS Diagnostic and Research Centre, Kashipur, India
VDepartment of Microbiology, Sanjay Gandhi Post Graduate Institute of Medical Sciences, Lucknow, India
Correspondence Correspondence: Prof. T. N. Dhole Department of Microbiology, Sanjay Gandhi Post Graduate Institute of Medical Sciences Raibarelli road, Lucknow, U.P India 226014 E-mail: tndhole@hotmail.com
ABSTRACT
BACKGROUND: Infection with hepatitis-B virus has been a significant cause of morbidity claiming more than a million lives every year. Epidemiological data reveals that there are 360 million carriers of hepatitis-B virus throughout the globe and 78% of the world populations' hail from Asia. Though several studies from Indian sub-continent have provided an estimate of the prevalence of this viral infection, there exist only few studies, which reflect the status in the general population.
AIM: The present study was designed to investigate the prevalence of hepatitis-B infection in North Indian general population.
METHODS: The study population comprised of 20,000 healthy blood donors who were screened for hepatitis-B surface antigen (HBsAg) status using third generation ELISA kit. Seroprevalence rate of seropositive donors was calculated and stratified by age, sex and blood groups. Statistical analysis was performed using tests of proportions, chi-square and confidence interval.
RESULTS: The study showed that out of 20,000 donors, 450 (2.25%) were HBsAg positive (95% confidence interval (CI), 2.0445-2.4554). Higher prevalence of HbsAg was found among males (440/19235) than females (10/765). The age specific prevalence rose from 1.78% (108/6058) in donors aged 19-25 years to a maximum of 3.03% (96/3161) in donors aged 35-45 years and decreased in older age groups. The peaks were detected in male donors aged 35-45 years and in females aged 25-35 years. Rh-negative blood group donors (21/873) and Rh-positive group donors (429/19127) had almost equivalent prevalence rates of HBsAg. HBsAg was more prevalent in blood group B donors (174/7426) and less prevalent in AB blood group donors (38/2032).
CONCLUSION: It was found that variables including gender and age were significantly associated with HBsAg positivity. HBsAg positivity in our population was statistically not associated with ABO blood groups.
Headings: Hepatitis-B virus. Hepatitis B surface antigen. Blood donors. Seroepidemiologic studies. Risk factors. India.
RESUMO
RACIONAL: A infecção pelo vírus B da hepatite é considerada uma significante causa de morbidade, responsável por mais de 1 milhão de casos, a cada ano. Dados epidemiológicos revelam que existem 360 milhões de portadores de vírus da hepatite B no mundo e 78% da população natural da Ásia. Embora vários estudos realizados na Ásia sub-continental tenham fornecido uma estimativa de prevalência desta infecção viral, existem poucos estudos que avaliam esta condição na população geral.
OBJETIVO: Investigar a prevalência da infecção pelo víirus B da hepatite na população geral do nordeste da Índia.
MÉTODOS: A população estudada compunha-se de 20.000 doadores de sangue sadios, selecionados através de positividade do antígeno de superfície da hepatite B (HBsAg), utilizando-se o kit ELISA de 3ª geração. A taxa de soroprevalência dos doadores soropositivos foi calculada e estratificada por idade, sexo e grupos sangüíneos. Análise estatística foi obtida usando-se testes de proporções, do qui ao quadrado e intervalo de confiança (CI).
RESULTADOS: O estudo revelou que dos 20.000 doadores, 450 (2,25%) eram HBsAg positivos (95% CI 2.0445-2.4554). Prevalência maior de HBsAg foi encontrada em homens (440/19235) do que em mulheres (10/765). A prevalência por faixa etária aumentou de 1,78% (108/6058) em doadores entre 19 a 25 anos, para máximo de 3,03% (96/3161) naqueles entre 35-45 anos e decresceu nos grupos de maior idade. Os picos foram detectados em doadores masculinos de 35-45 anos e em mulheres de 25-35 anos. O grupo de doadores Rh negativo (21/873) e o grupo Rh positivo (4299/19127) mostraram taxas de prevalência de HBsAg quase equivalentes. HBsAg foi mais prevalente no grupo de doadores de tipo sangüíneo B (174/7426) e menos no grupo de tipo sangüíneo AB (38/2032).
CONCLUSÃO: Verificou-se que variáveis incluindo gênero e idade foram significantemente associadas à positividade do HBsAg e que esta não foi estatisticamente associadas aos grupos sangüíneos ABO.
Descritores: Vírus da hepatite B. Antígenos de superfície da hepatite B. Doadores de sangue. Estudos soroepidemiológicos. Fatores de risco. Índia.
INTRODUCTION
Hepatitis B virus (HBV) infection is one of the major global health problems. Of the approximately 2 billion people, who have been infected worldwide more than 350 million are chronic carriers of HBV(34). HBV infection accounts for 5,00,000 to 1.2 million deaths each year(22) and is the 10th leading cause of death. The prevalence of HBV infection varies markedly in different geographic areas of the world. In developed countries like Northern Europe and America, HBV infection occurs in less than 1% of the population of these countries. In developing countries of Asia and Africa, particularly those of Far East and South Africa, HBV infection occurs in 5%-10% of the general population. India is considered to be in the region of intermediate endemicity, with nearly 3%-4% of the population infected by the virus(6).
Data on burden of HBV infection in India come primarily from studies on HBsAg seroprevalence. A large number of studies on the epidemiology of HBV infection have been carried out in this country over the last two decades. There are several levels of variability amongst these studies which include the sample size, the methodology for assay of HBV serological markers, the age group covered, general population sample versus blood donors, risk-population samples, ethnicity and geography of the study groups. All these factors have also been shown to influence the prevalence of HBV infection. Of the studies among various groups, those among voluntary blood donors are most closely representative of the rates in the general population. Though these studies have used laboratory tests with different sensitivity and specificity rates, they provide a good estimate of HBV burden in the country.
Earlier studies have reported that HBsAg prevalence among blood donors ranged from 1% to 4.7%(1). There are conflicting reports on the prevalence rates of HBsAg in India. Adequate data on age, sex and blood group specific prevalence is also lacking. Therefore the present study was undertaken to estimate the age, sex and blood group specific prevalence of HBsAg in blood donors, representing general population in Northern India.
METHODS
Study population and laboratory tests
Twenty thousand subjects visiting Ganesh Shankar Vidyarthi Memorial (GSVM) Medical College, Kanpur, India, from March 2002 to June 2006 were included in the present study. Three milliliter blood sample from apparently healthy blood donors belonging to all socioeconomic group was collected in EDTA vaccutainers. The blood bank caters to a wide area of Northern India therefore healthy donors comprised of general population. A thorough clinical history, medical examination and selection of donors were done; prior obtaining signed consent form from all the donors. All the donors were screened for hepatitis-B surface antigen (HBsAg) test by third generation enzyme linked immunosorbent assay (HBsAg ELISA 3.0, Span Diagnostics, India) along with other mandatory tests for blood donation. Blood group of each donor was tested and the donors were categorized according to their respective blood groups, sex, age and correlated with risk factors.
Statistical analysis
The data was analyzed statistically, using appropriate statistical tests like tests of proportions, Chi-square tests and confidence interval. P value was calculated using SPSS Software. A P value <0.05 was considered statistically significant. 95% Confidence Interval of the proportions of HBsAg prevalence was determined as follows: P ± (√ pq/n)*Zd/2
where P = proportions of population found positive for HBsAg
q = 1-p
n = total number of cases
z = standard normal variate (1.96)
d= degree of freedom
RESULTS
Overall and gender specific prevalence
The overall prevalence of HBsAg among blood donors aged 19-55 years was 2.45% (n = 20,000) (95% CI: 2.0445-2.4554). The prevalence of HBsAg in males was 2.28% (440/19235) compared to 1.30% (10/765) in females. The difference was found to be statistically significant (P = 0.0206) (Table 1).
Age specific prevalence
HBsAg seroprevalence increased with age, 1.78% in 19-25 year age group to 3.03% in 35-45 year age group. The difference was found to be statistically significant (P = 0.0381) (Table 1). The study showed maximum prevalence of HBsAg at 3.10% (94/3025) in male donors aged 35-45 years and at 1.76% (6/339) in female donors aged 25-35 years. For both genders minimum prevalence was seen in the donors aged 19-25 years. We could not establish any significant association between age and gender in relation to HBsAg positivity (data statistically insignificant) (Table 2).
Blood group specific prevalence
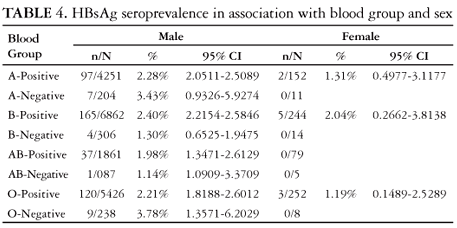
The prevalence of HBsAg did not vary significantly (P>0.05) and was marginally high among the Rhesus-negative group (2.40%) than those with Rhesus-positive group (2.24%) [(P = 0.7623)]. HBsAg prevalence was higher in blood group B at 2.34% (174/7426) and lowest in blood group AB at 1.87% (38/2032). The difference though was statistically not significant (P = 0.1768) (Table 1). The present study showed highest seroprevalence of HBsAg in blood group B (2.39%) and lowest in blood group AB (1.90%) among Rh-positive group. Among Rh-negative group the highest seroprevalence was seen in blood group O (3.65%) and lowest in blood group AB (1.08%) (Table 3). Among male blood donors, HBsAg was found to be more prevalent in O-negative blood group at 3.78% (9/238) and lowest in AB-negative at 1.14% (1/87). Among the female donors, highest seroprevalence of HBsAg was seen in B-positive blood group at 2.04% (5/244) (Table 4).
DISCUSSION
Hepatitis-B is found throughout the world, it has no seasonal distribution. The reported prevalence of carrier in different population varies widely from 0.1% in the advanced countries to 20% in the developing nations. The carrier rate is higher in the tropical than in the temperate regions. In South East Asia, roughly 14 to 16 million people are infected with hepatitis B virus every year. Prevalence of hepatitis B varies from country to country and depends upon a complex interplay of behavioral, environmental and host factors. In general, it is lowest in countries or area with high standards of living (eg: Australia, North America, North Europe) and highest in countries or areas where socio economic level is lower (eg: China, South East Asia, South America)(7).
The study showed 2.25% seroprevalence of HBsAg among blood donors. The frequency of HBsAg seropositivity was found to be lower than that reported in Tamil Nadu 24.5%(13), Madras 5.5%(30), Vellore 7.17%(29). The rate was comparable to that reported from Lucknow 2.2%(5), North India 2.5%(25), Mumbai 2.02%(9), Pakistan 2.21%(24), Calcutta 2.8%(4) and Bangladesh 2.4%(17).
When the results of the present study was compared with those reported from similar blood donors of other countries like Cameroon 11.72%(35), Taiwan 4.5%(32), Ethiopia 14.4%(27), Mauritania 20.3%(20), Thailand 4.51%(21), Djibouti 10.4%(8), Mangolia 8.2%(33), this study showed relatively lower prevalence of the hepatitis-B surface antigen whereas countries like Brazil 1.9%(23), Iran 1.07%(12), Turkey1.5%(28) and US Community 0.15%(18), showed lower HBsAg positivity in comparison to the present study.
Sex specific prevalence
With respect to sex related prevalence, this study showed 2.28% prevalence of HBsAg in males and 1.30% prevalence in females, (statistically significant, P = 0.0206). This finding of the present study is in concern with other studies, which demonstrated a higher prevalence of HBsAg among the male population(2, 3, 11, 15, 26). The high prevalence of HBsAg infection in male blood donors was responsible for the overall high prevalence in blood donors, which were predominated by male donors. Another important contributing factor responsible for a higher prevalence among the male population of the present study is that plasma disappearance rate for HBsAg in males is lower than females(31).
Age specific prevalence
The present study revealed significant trend of HBV seropositivity with relation to age. The positivity for HBsAg increased with age. This is comparable with the study conducted by JAYARAM(16). Some other studies have shown similar results(3, 14, 19, 23). Higher prevalence in older age groups may be attributed to birth cohort effect or iatrogenic factors including vaccinations by the use of unsterilized kits. Further the trend of immunization against hepatitis-B has been introduced in the recent few years. Therefore the older age group population having a higher prevalence of HBsAg detected in the present study is presumptively due to lack of immunization against the disease in their times. In the present study, declining seropositive rates in individuals aged 45 years or over was observed for both genders. Self-selection due to persistent HBV infection may partly account for such tendencies(2).
Blood group specific prevalence
The present study showed no significant association between ABO blood group distribution and HBsAg seroprevalence (data not statistically significant P = 0.1768). This is in accordance with other studies(10, 11). However, earlier studies had reported no prevalence of HBsAg in AB blood group donors, whereas the present study reported 1.87% HBsAg seroprevalence. The possible reason for this variance may be a large variation in the sample size.
Higher prevalence of HBsAg in blood group B could be because of the fact that blood group B is more prevalent in our area (37.13%). The study also demonstrated no significant difference in the HBsAg positivity among donors with Rh-negative group (2.40%) and Rh-positive group (2.24%). This slight variation observed may be accorded due to random chance variation.
CONCLUSION
In conclusion, the results of the present study hint at the importance of presenting integrated information and educational programs among these target groups, for preventing and controlling HBV transmission. Further, future surveillance studies warranting investigations for this viral infection in a broader population would enable us to determine strategies for combating the threats caused by hepatitis-B virus. In addition, epidemiologic studies like the present one from different states of India would be helpful to estimate real statistics of hepatitis-B infection in India.
ACKNOWLEDGEMENTS
The authors would like to thank Dr. T. N. Dhole, Professor, Department of Microbiology, Sanjay Gandhi Post Graduate Institute of Medical Sciences, Lucknow, India for his consistent patronage and support.
Recebido em 28/8/2007.
Aprovado em 29/11/2007.
- 1. Aggarwal R. Universal neonatal Hepatitis B virus vaccination in India: why? Hep B Annual. 2004;1:60-71.
- 2. Asakura T, Tachibana K, Watanabe S, Teshima D, Ikeda M, Tokudome S. Concomitant carriage of hepatitis B virus and human T-lymphotropic virus type I among blood donors in Kitakyushu, Japan. J Infect. 1991;23:33-7.
- 3. Baikie M, Ratnam S, Bryant DG, Jong M, Bokhout M. Epidemiologic features of Hepatitis B virus infection in northern Labrador. CMAJ. 1989;141:791-5.
- 4. Chakraborthy MS, Mukherjee KK, Mithra KK. Association between Australia antigen and leprosy in Calcutta. Bull Cal School Trop Med. 1977;25:19-21.
- 5. Choudhury N, Ramesh V, Saraswat S, Naik S. Effectiveness of mandatory transmissible diseases screening in Indian Blood donors. Ind J Med Res. 1995;105:229-32.
- 6. Chowdhury A. Epidemiology of Hepatitis B virus infection in India. 2004;1:17-24.
- 7. Dienstag JL, Isselbacher KJ. Acute viral Hepatitis. In: Fauci AS, Braunwald E, Isselbacher KJ, Wilson JD, Martin JB, Kasper DL, Hauser SL, Longo DL, editors. Harrisons Principles of Internal Medicine. New York: Mc Graw Hill; 1998. p.1677-92.
- 8. Dray X, Dray-Spira R, Bronstein JA, Mattera D. Prevalence of HIV, hepatitis B and hepatitis C in blood donors in the republic of Djibouti. Med Trop. 2005;65:39-42.
- 9. Elavia AJ, Banker DD. Hepatitis B Virus infection in hospital personnel. Natl Med J India. 1992;5:265-8.
- 10. Emeribe AO, Ejezie GC. ABO blood groups distribution in relation to Hepatitis B surface antigen and the presence of lipoidophil antibodies. East Afr Med J. 1992;69:146-8.
- 11. Farzadegan H, Harbour C, Ala F. The prevalence of hepatitis B surface antigen and it's antibody in blood donors and high risk groups in Iran. Vox Sang. 1979;37:182-6.
- 12. Ghavanini AA, Sabri MR. Hepatitis B surface antigen and anti-hepatitis C antibodies among blood donors in the Islamic Republic of Iran. East Mediterr Health J. 2000;6(5-6):1114-6.
- 13. Hussain AI, Rajendran P, Thyagarajan SP. HBsAg and HIV antibody in tribal populations of Tamilnadu, India. Virus Inf Exch New Lett 1991; 8: 62.
- 14. James L, Fong CW, Foong BH, Wee MK, Chow A, Shum E, Chew SK. Hepatitis B seroprevalence study 1999. Singapore Med J 2001;42:420-4.
- 15. Jayaprakash PA, Shanmugham J, Hariprasad D. Hepatitis B surface antigen in blood donors. An epidemiologic study. Transfusion. 1983;23:346-7.
- 16. Jayaram S. Prevalence of HBV markers in different age groups in Madras. (thesis) " Prevention and control of Hepatitis B in Tamil Nadu" . University of Madras; 1992.
- 17. Khan M, Hussain M, Yano M, Hashizume K, Yousuf M, Tanaka E, Matsumoto A, Furuta S, Kiyosawa K. Comparison of seroepidemiology of hepatitis C in blood donors between Bangladesh and Japan. Gastroenterol Jpn. 1993;28(Suppl 5):28-31.
- 18. Kim WR, Benson JT, Therneau TM, Torgerson HA, Yawn BP, Melton LJ 3rd. Changing epidemiology of hepatitis B in a US Community. Hepatol. 2004;39:811-6.
- 19. Kurien T, Thyagarajan SP, Jeyaseelan L, Peedicayil A, Rajendran P, Sivaram S, Hansdak SG, Renu G, Krishnamurthy P, Sudhakar K, Varghese JC, STD Study Group. Community prevalence of hepatitis B infection and modes of transmission in Tamil Nadu, India. Indian J Med Res. 2005;121:670-5.
- 20. Lo BB, Meymouna M, Boulahi MA, Tew M, Sow A, Ba A, Sow MB. Prevalence of serum markers of Hepatitis B and C virus in blood donors of Nouakchott, Mauritania. Bull Soc Pathol Exot. 1999;92:83-4.
- 21. Luksamijarulkul P, Thammata N, Tiloklurs M. Seroprevalence of hepatitis B, hepatitis C and human immunodeficiency virus among blood donors, Phitsanulok Regional Blood Center, Thailand. Southeast Asian J Trop Med Public Health. 2002;33:272-9.
- 22. Mahoney FJ. Update on diagnosis, management and prevention of Hepatitis B virus infection. Clin Microbiol Rev. 1999;12:351-66.
- 23. Martelli CM, de Andrade AL, das Dores D, Cardoso P, Almeida e Silva S, Zicker F. Methodological considerations in the interpretation of serologic screening for hepatitis B virus among blood donors. Rev Saude Publica. 1991;25:11-6.
- 24. Mujeeb SA, Aamir K, Mehmood K. Seroprevalence of HBV, HCV and HIV infections among college going first time voluntary blood donors. J Pak Med Assoc. 2000;50:269-70.
- 25. Nanu A, Sharma SP, Chatterjee K, Jyoti P. Markers for transfusion transmissible infections in North Indian voluntary and replacement blood donors: prevalence and trends: 1989-1996. Vox Sang. 1997;73:70-3.
- 26. Pal SR, Dutta DV, Choudhary S. HBsAg among patients with liver diseases and voluntary blood donors - a prospective study. Ind J Med Res. 1973;61:1784.
- 27. Rahlenbeck GI, Yohannes G, Molla K, Reifen R, Assefa A. Infection with HIV, syphilis and hepatitis B in Ethiopia: a survey in blood donors. Int J STD AIDS. 1997;8:261-4.
- 28. Sakarya S, Oncu S, Ozturk B, Oncu S. Effect of preventive applications on prevalence of hepatitis B virus and hepatitis C virus infections in West Turkey. Saudi Med J. 2004;25:1070-2.
- 29. Sumathy S, Thyagarajan SP, Latif R, Madanagopalan N, Raguram K, Rajasambandam P, Gowans E. A dipstick immunobinding enzyme linked immunosorbent assay for serodiagnosis of hepatitis B and Delta virus infections. J Virol Methods. 1992;38:145-9.
- 30. Tandon BN, Joshi YK, Gandhi BM, Irshad M, Gupta H, Gupta ML. Epidemiology of HBsAg carriers in India. A holistic approach to control of hepatitis B reservoir. J Gastroenterol Hepatol. 1986;1:39-43
- 31. Thursz MR. Host genetic factors influencing the outcome of Hepatitis. J Viral Hepatitis. 1997;4:215-20.
- 32. Tsai SJ, Chen CJ, Hsieh YS, Yang CS. Seroprevalence of anti-HCV among voluntary blood donors in Taiwan. Zhonghua Min Guo Wei Sheng Wu Ji Mian Yi Xue Za Zhi. 1991;24:61-70.
- 33. Tsatsralt-Od B, Takahashi M, Nishizawa T, Inoue J, Ulaankhuu D, Okamoto H. High prevalence of Hepatitis B, C and delta virus infections among donors in Mongolia. Arch Virol. 2005;150:2513-28.
-
34WHO - World Health Organization. Hepatitis B fact sheet number 204/WHO. (revised October 2000). Available: (http://who.int/inf.fs/en/fact204.html.
- 35. Zekeng L, Kaptue L. HIV-1 serology and carrier state for HBs and HBe in blood donors at Yaounde University Hospital Centre, Cameroon. Ann Soc Belg Med Trop. 1990;70:49-53.
Publication Dates
-
Publication in this collection
07 July 2008 -
Date of issue
June 2008
History
-
Accepted
29 Nov 2007 -
Received
28 Aug 2007