Abstracts
We evaluated 44 patients with tics and Tourette's syndrome (TS) emphasising the age of onset of symptoms, sex, classification and localization of tics, associated symptoms and signs and comorbidities. Thirty-three patients (75.2%) had TS defined criteria whereas 10 (22.7%) had chronic motor and/or vocal tics. Simple motor tics were found in 43 cases (97.7%), mainly affecting the eyes (43.2%), mouth (43.2%), face (34.1%). Simple vocal tics occurred in 33 (75%). Coprolalia was found in just 6 cases (13.6%) and copropraxia in just 2 (4.5%). Obsessive compulsive disorder and/or symptoms were found in 26 cases (59.1%) and attention deficit in 17 (38.6%). Eighteen patients (40.9%) had other disorders, such as alcoholism, tabagism, drug abuse, affective disorders, anxiety, sleep and learning disorders. The data obtained are similar to those found by other authors. We highlight the low frequency of coprolalia, as well as the associated neuropsychiatric disorders.
Tourette's Syndrome; obsessive compulsive disorder; attention deficit disorder
Avaliamos 44 pacientes com tiques e síndrome de Tourette (ST), enfatizando a idade de início dos sintomas, sexo, classificação e localização dos tiques, sinais e sintomas associados e presença de comorbidades. Trinta e três pacientes (75,2%) tinham TS definida, ao passo que 10 (22,7%) tinham tiques motores e/ou vocais crônicos. Tiques motores simples foram encontrados em 43 casos (97,7%), principalmente envolvendo os olhos (43,2%), boca (43,2%), face (34,1%). Tiques vocais simples ocorreram em 33 (75%). Coprolalia estava presente em apenas 6 casos (13,6%) e copropraxia em apenas 2 (4,5%). Sintomas e/ou transtorno obsessivo-compulsivo foi encontrado em 26 casos (59,1%) e déficit de atenção em 17 (38,6%). Dezoito pacientes (40,9%) tinham outras desordens, tais como alcoolismo, tabagismo, abuso de drogas. Os dados encontrados são semelhantes àqueles encontrados por outros autores. Nós enfatizamos a baixa incidência de coprolalia, assim como a presença de transtornos neuropsiquiátricos associados.
síndrome de Tourette; transtorno obssessivo-compulsivo; déficit de atenção
TICS AND TOURETTE SYNDROME
Clinical evaluation of 44 cases
Hélio A.G. Teive1 1 Movement Disorders Unit, Division of Neurology, Department of Internal Medicine, Hospital de Clinicas, Federal University of Paraná, Curitiba PR, Brazil: Assistant Professor of Neurology; 2 Resident of Neurology; 3 Chief of Neurological Service. , Francisco M.B. Germiniani2 1 Movement Disorders Unit, Division of Neurology, Department of Internal Medicine, Hospital de Clinicas, Federal University of Paraná, Curitiba PR, Brazil: Assistant Professor of Neurology; 2 Resident of Neurology; 3 Chief of Neurological Service. , Marcus V. Della Coletta2 1 Movement Disorders Unit, Division of Neurology, Department of Internal Medicine, Hospital de Clinicas, Federal University of Paraná, Curitiba PR, Brazil: Assistant Professor of Neurology; 2 Resident of Neurology; 3 Chief of Neurological Service. , Lineu César Werneck3 1 Movement Disorders Unit, Division of Neurology, Department of Internal Medicine, Hospital de Clinicas, Federal University of Paraná, Curitiba PR, Brazil: Assistant Professor of Neurology; 2 Resident of Neurology; 3 Chief of Neurological Service.
ABSTRACT ¾ We evaluated 44 patients with tics and Tourette's syndrome (TS) emphasising the age of onset of symptoms, sex, classification and localization of tics, associated symptoms and signs and comorbidities. Thirty-three patients (75.2%) had TS defined criteria whereas 10 (22.7%) had chronic motor and/or vocal tics. Simple motor tics were found in 43 cases (97.7%), mainly affecting the eyes (43.2%), mouth (43.2%), face (34.1%). Simple vocal tics occurred in 33 (75%). Coprolalia was found in just 6 cases (13.6%) and copropraxia in just 2 (4.5%). Obsessive compulsive disorder and/or symptoms were found in 26 cases (59.1%) and attention deficit in 17 (38.6%). Eighteen patients (40.9%) had other disorders, such as alcoholism, tabagism, drug abuse, affective disorders, anxiety, sleep and learning disorders. The data obtained are similar to those found by other authors. We highlight the low frequency of coprolalia, as well as the associated neuropsychiatric disorders.
KEY WORDS: Tourette's Syndrome, obsessive compulsive disorder, attention deficit disorder.
Tiques e síndrome de Tourette: avaliação clínica de 44 casos
RESUMO ¾ Avaliamos 44 pacientes com tiques e síndrome de Tourette (ST), enfatizando a idade de início dos sintomas, sexo, classificação e localização dos tiques, sinais e sintomas associados e presença de comorbidades. Trinta e três pacientes (75,2%) tinham TS definida, ao passo que 10 (22,7%) tinham tiques motores e/ou vocais crônicos. Tiques motores simples foram encontrados em 43 casos (97,7%), principalmente envolvendo os olhos (43,2%), boca (43,2%), face (34,1%). Tiques vocais simples ocorreram em 33 (75%). Coprolalia estava presente em apenas 6 casos (13,6%) e copropraxia em apenas 2 (4,5%). Sintomas e/ou transtorno obsessivo-compulsivo foi encontrado em 26 casos (59,1%) e déficit de atenção em 17 (38,6%). Dezoito pacientes (40,9%) tinham outras desordens, tais como alcoolismo, tabagismo, abuso de drogas. Os dados encontrados são semelhantes àqueles encontrados por outros autores. Nós enfatizamos a baixa incidência de coprolalia, assim como a presença de transtornos neuropsiquiátricos associados.
PALAVRAS-CHAVE: síndrome de Tourette, transtorno obssessivo-compulsivo, déficit de atenção.
Georges Gilles de La Tourette first described Tourette's Syndrome (TS) in 1885 as "a nervous affection characterised by lack of motor coordination accompanied by echolalia and coprolalia"; later Charcot named the condition as Tourette's Syndrome1-3. Tics are fast, repetitive and stereotyped involuntary movements of individual muscle groups. Tic disorders are commonly categorised according to age of onset, duration of symptoms, severity of symptoms and findings of vocal and/or motor tics4-10.
Chief among the tic disorders is TS, which is the most severe and is frequently accompanied by neuropsychiatric disorders such as obsessive compulsive disorder (OCD), attention deficit disorder with or without hyperactivity (ADHA) and others4,6,8,9,11,12.
Transitory tic disorder: Tics usually start while the child is in primary school and can be found in up to 18% of all children. The most common tics are blinking, rubbing the nose and making funny faces. Transitory vocalisations are less common and include the sound one makes when "cleaning the throat", among others. Sometimes childhood tics can be bizarre; e.g. licking the palms of the hands or touching the genitalia. Transitory tics last only a few weeks or months and usually aren't related to any kind of behavioural disorder. They are best observed in fatigability or excitatory settings. Like other tic disorders, boys are affected 3 to 4 times more commonly than girls. Even though transitory tics do not last longer than a year by definition, relapsing episodes of transitory tics can occur for several years.
Chronic Tic Disorder: It can be differentiated from transitory tic disorder not only by the persistence of symptoms for several years, but also by its clinical persistent features. Chronic tics can remain unchanged for years. Blinking and facial movements are two examples of tics found in chronic tic disorder.
Tourette Syndrome: According to the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) it's defined by: a) multiple motor tics and one or more vocal tics; b) tics occur several times a day, almost every day or intermittently for one year or more (there cannot be a period free of tics longer than 3 months); c) the disorder causes discomfort and severe social and work compromise; d) onset of tics must occur before the patient is 18 years-old and e) the disorder is not due to the use of drugs nor to another disease.
Chronic Motor/Vocal Tics Disorder: The patient presents with several chronic motor (or vocal) tics. The diagnostic criteria are the same as those for TS, except for a): either simple or multiple motor tics, or vocal tics (they can't be found at the same time)4,10,13-15.
The aim of our study was to perform a clinical evaluation of 44 patients with either TS or other tic disorder and to see whether there were other co-morbid disorders.
METHOD
We retrospectively reviewed the files of 44 outpatients from the Movement Disorder Service of the Hospital de Clínicas da Universidade Federal do Paraná. Age of onset, sex, classification and localisation of tics, associated signs and symptoms, concomitant OCD, ADHA and other neuropsychiatric disorders were evaluated. Classification of all disorders followed the guidelines of the DSM-IV6.
RESULTS
The patients' age ranged from 3 to 60 years (mean age of 13.5 years at the time of our evaluation). 75% (n=33) of all patients fulfilled the diagnostic criteria for TS, 22.7% (n=10) for Chronic Motor/Vocal Tics and 2.3% (n=1) for transitory tics. Sixty-three percent (n=28) of our patients were male and 36.4% (n=16) were female. Most patients had onset of symptoms in the first or second decade (prior to ten years in 56.8 % and from 10 to 20 in 15.9%). Seven percent had onset of symptoms after twenty years and 20% could not recall when they first manifested their symptoms.
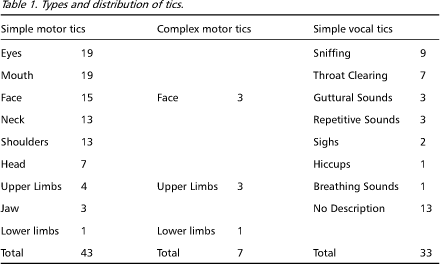
Simple motor tics could be found in 97.7% (n=43), complex motor tics in 15.9% (n=7) and simple vocal tics in 75% (n=33) of our cases. Simple motor tics had a distribution that compromised mostly the head and upper limbs. Thus, nineteen patients had eyes tics, tics involving the mouth muscles were found in 19 patients, 15 had facial tics other than eye or mouth tics, neck and shoulders tics were found in 13 patients each, 7 patients had head tics, 4 had distal upper limbs tics (hands only), 3 had tics of the lower limbs and one patient had jaw tics (Table 1). Complex motor tics occurred in fewer patients, with the following distribution: upper limbs in 3 patients, facial tics in another three and lower limbs in one (Table 1).
Simple vocal tics comprised a complex and varied group of tics. Nine patients presented with sniffing sounds, 7 with "throat clearing" sounds, 3 with guttural sounds, 2 with sighs, one with hiccups and one with breathing sounds. Three patients had repetitive sounds that were hard to classify and 13 had no clear description of their simple vocal tics. Only 13.6% (n=6) of patients had coprolalia (Table 1).
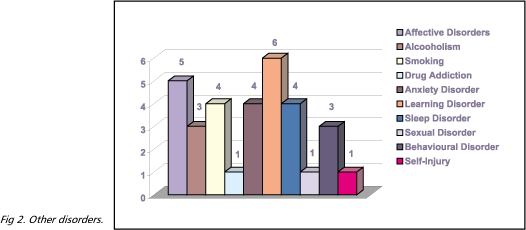
Obsessive Compulsive symptoms/disorder was observed in 59.1% (n=26) and ADHA in 38.6% (n=17) as seen in Figure 1. Other disorders (affective disorders, anxiety disorder, alcoholism, smoking, sleep disorders and learning disorder) were found in 40.9% (n=18) (Fig 2).
DISCUSSION
We evaluated the files of 44 patients and classified the patients according to the diagnostic criteria found in the DSM-IV. Seventy-five percent of all patients fulfilled the criteria for TS while 22.7% had chronic motor/vocal tics. Onset of symptoms prior to the patients being 20 years old could be found in 72.7% of our patients, a result similar to those found in other studies2,7,8,14,16,17.
We were more flexible than other authors and classified patients as having TS as long as they were younger than 20 when they had the onset of their symptoms. This criterion was based on the fact that some authors propose a limit age of onset before the patient is 21 years old, instead of 18, which is the usual time of onset of tics in both TS and chronic motor/vocal tics2,6-9,13-15,17.
In our group the male/female ratio was 1.75:1 (the ratio is usually 3 or 4 men for every woman).
Simple and complex motor tics occurred more commonly in the upper segment, while simple vocal tics could be found in 75% (n=33). Similar results were found in other studies, such as the Tolosa and Bayes, cited by Lees and Tolosa7 and by Cardoso et al.17. In that study the authors found that blinking, grimacing and shoulder elevation were the most common motor tics. The types of simple vocal tics found in their study were mostly sniffing, throat clearing and grunting sounds17.
Even tough it is the mostly well-known symptom of TS (see original description), coprolalia is found in only a minority of patients (5 to 30%). In our study coprolalia was rather uncommon (13.6%, n=6) and was not an obligatory criterion for the diagnosis of TS. In their study, Cardoso et al. found 9 patients (28%) out of 32 with coprolalia17. Only two of our patients (4.5%) had copropraxia and none had echolalia, ecopraxia or palilalia.
Coprophenomena occurred in about one third of the patients in the series by Shapiro et al.2, but are much rarer in Japanese patients with TS according to Lees. This is probably due to the extreme courtesy and decorum of the Japanese culture7.
Ever since Gilles de La Tourette first described it, a clear association between tics and obsessive-compulsive symptoms is usually found. In our group 59.1% of TS patients had OCD (or obsessive-compulsive symptoms), which is similar to the rates found in the literature (28% to 67%)2,4,7,8,11,12,15,17. Even though ADHA affects up to 50 or 80% of TS patients4,7-9,11,15,16, in our group it could only be found in 38.6%, probably due to the small size of our study population. Another study with a group of Brazilian patients had an incidence of 63% for ADHD and 44% for OCD17.
TS and other tic disorders seem to be part of the same phenomenological continuum, and some clinical features of tics, OCD and ADHA can occur in any given person during childhood as part of the normal development18,19. In addition, other studies highlight the role of both genetic and environmental factors in the genesis of tic disorders7-9,13-15,18,20,21.
The data found in our study are similar to the findings of other authors worldwide. We highlight the low occurrence of coprolalia in our patients and emphasise the concomitant neuropsychiatric disorders.
Received 18 january 2001, received in final form 30 April 2001. Accepted 10 May 2001.
Dr. Hélio A.G. Teive - Hospital de Clínicas UFPR - Rua General Carneiro 181/ 12ºandar - 80060-090 Curitiba PR, Brasil. FAX: 41 244 5060. E-mail: hagteive@mps.com.br
- 1. Gilles de La Tourette G. Étude sur une affection nerveuse caracterisée par l'incordination motrice accompagnée d'echolalie et coprolalie. Arch Neurol 1885;9:19-42,158-200.
- 2. Shapiro AK, Shapiro ES, Young JG, Feinberg TE. In Gilles de La Tourette syndrome. 2.Ed. NewYork: Raven Press, 1988:127-193.
- 3. Lees AJ, de La Tourette G. The man and his time. Rev Neurol 1986; 142:808-816.
- 4. Fahn S. Motor and Vocal Tics. In Kurla R (ed). Handbook of Tourette's syndrome and related tic and behavioral disorders. New York: Marcel Dekker, 1993:3-16.
- 5. Jankovic J. Phenomenology and classification of tics: Tourette's syndrome. Neurol Clin N Am 1997;15:267-275.
- 6. American Psychiatric Association.Diagnostic and Statistical Manual of Mental Disorders- DSM-IV. Washington: American Psychiatric Association, 1994.
- 7. Lees AJ, Tolosa E. Tics. In Jankovic J, Tolosa E (eds). Parkinson's disease and movement disorders. 2.Ed. Baltimore: Willians & Wilkins, 1993:329-335.
- 8. Tolosa E, Jankovic J. Ticsand Tourette's syndrome. In Tolosa E, Jankovic J (eds). Parkinson's disease and movement disorders. 3.Ed. Baltimore: Willians & Wilkins, 1998:491-512.
- 9. Weiner WJ, Lang AE. Gilles de la Tourette's syndrome. In Weiner WJ, Lang AE (eds). Movement disorders: a comprehensive survey. New York: Futura Publishing, 1989:532-568.
- 10. Teive HAG. Tiques e syndrome de Tourette: definiçőes básicas, classificaçőes e critérios diagnósticos atuais. Rev Bras Neurol 1998;34: 163-167.
- 11. Comings DE, Comings BG. Comorbid behavioral disorders. In Kurlan R (ed). Handbook of Tourette's syndrome and related tic and behavioral disorders. New York: Marcel Dekker, 1993:111-147.
- 12. George SM, Trimble MR, Ring AH, Robertson MM. Obsessions in obsessive-compulsive disorder with and without Gilles de La Tourette's syndrome. Am J Psychiatry 1993;150:98-102.
- 13. Bruun RD, Cohen DJ, Leckman JF. Guide to the diagnosis and treatment of Tourette syndrome. Harvard: Edu 1997;22:43.
- 14. Singer H S. Tic disorders. Pediatric Annals 1993;22:22-29.
- 15. Leckman JF, Peterson BS, Pauls DL, Cohen DJ. Tic disorders. Psychiatr Clin N Am 1997;20:839-861.
- 16. Dodick D, Adler CH. Tourette's syndrome. Current approaches to recognition and management. Postgraduate Medicina 1992;5:299-308.
- 17. Cardoso F, Veado C C M, Oliveira J T. A Brazilian cohort of patients with Tourette's syndrome. J Neurol Neurosurg Psychiatry 1996;60:209-212.
- 18. Kurlan R. Hypothesis II: Tourette's syndrome is part of a clinical spectrum that includes normal brain development. Arch Neurol 1994; 51:1145-1149.
- 19. Mattos JP, Rosso ALZ. Tiques e síndrome de Giles de la Tourette. Arq Neuropsiquiatr 1995;53:141-146.
- 20. Hanna PA, Janjua FN, Contant CF, Jankovic J. Bilineal transmission in Tourette's syndrome. Neurology 1999;53:813-818.
- 21. Mattos JP, Mattos VMBC. Doença dos Tiques: aspectos genéticos e neuroquímicos atuais. Arq Neuropsiquiatr 1999;57(2):528-530.
Publication Dates
-
Publication in this collection
05 Oct 2001 -
Date of issue
Sept 2001
History
-
Accepted
10 May 2001 -
Received
18 Jan 2001 -
Reviewed
30 Apr 2001