Abstracts
INTRODUCTION: Semantic relations among words and repetition enhance free recall, but it is unknown if these facilitating factors are effective in dementia. METHOD: Alzheimer's patients (MILD-Alz, MOD-Alz) were compared to healthy elderly. Fifteen-word lists were read out to the subjects. In four sets of lists the words in intermediary input positions were semantically related or not, or the midlist words were repeated, or they were repeated and semantically related. RESULTS: The usual third peak of recall of semantically related words was not observed in MOD-Alz, repetition of words did not increase recall of the patients, and the combination of relatedness and repetition benefited only MID-Alz. In a second experiment, with related or unrelated midlist words, and list length shortened from 15 to 9 words, semantic facilitation was observed in mild and moderate Alzheimer´s patients, although diminished compared to controls. CONCLUSION: Progression of dementia turns facilitating factors of recall less effective.
memory; word list recall; Alzheimer's disease; semantic relations; repetition
INTRODUÇÃO: Relacionamento semântico e repetição facilitam a recordação livre mas não se sabe se esses fatores continuam efetivos na demência. MÉTODO: O desempenho de pacientes com doença de Alzheimer (MILD-Alz e MOD-Alz) foi comparado com o de idosos sadios na recordação livre de listas de 15 palavras, utilizando quatro diferentes conjuntos de listas que continham ou não palavras relacionadas nas posições intermediárias, palavras repetidas, ou ainda palavras repetidas e semanticamente relacionadas. RESULTADOS: O terceiro pico usual na recordação das palavras semanticamente relacionadas não foi observado em MOD-Alz; a repetição não aumentou a recordação dos pacientes; a combinação de relacionamento e repetição beneficiou apenas MILD-Alz. Em outro experimento, com palavras intermediárias relacionadas ou não, e em que a extensão das listas foi reduzida para 9 palavras, observou-se facilitação semântica em MILD-Alz e MOD-Alz. CONCLUSÃO: A progressão da demência diminui a eficácia de fatores facilitadores da recordação.
memória; recordação livre de palavras; doença de Alzheimer; relação semântica; repetição
ARTICLES
Effects of semantic relations, repetition of words, and list length in word list recall of Alzheimer's patients
Efeitos da relação semântica, repetição de palavras e extensão das listas na recordação de pacientes com doença de Alzheimer
Orlando F.A. BuenoI; Paulo H.F. BertolucciII; Maria Gabriela M. OliveiraI; Jacqueline Abrisqueta-GomezIII
IProfessor Adjunto do Departamento de Psicobiologia
IIProfessor Adjunto do Departamento de Neurologia e Neurocirurgia
IIIDoutora em ciências, Universidade Federal de São Paulo - UNIFESP, São Paulo SP, Brazil
ABSTRACT
INTRODUCTION: Semantic relations among words and repetition enhance free recall, but it is unknown if these facilitating factors are effective in dementia.
METHOD: Alzheimer's patients (MILD-Alz, MOD-Alz) were compared to healthy elderly. Fifteen-word lists were read out to the subjects. In four sets of lists the words in intermediary input positions were semantically related or not, or the midlist words were repeated, or they were repeated and semantically related.
RESULTS: The usual third peak of recall of semantically related words was not observed in MOD-Alz, repetition of words did not increase recall of the patients, and the combination of relatedness and repetition benefited only MID-Alz. In a second experiment, with related or unrelated midlist words, and list length shortened from 15 to 9 words, semantic facilitation was observed in mild and moderate Alzheimer´s patients, although diminished compared to controls.
CONCLUSION: Progression of dementia turns facilitating factors of recall less effective.
Key words: memory, word list recall, Alzheimer's disease, semantic relations, repetition.
RESUMO
INTRODUÇÃO: Relacionamento semântico e repetição facilitam a recordação livre mas não se sabe se esses fatores continuam efetivos na demência.
MÉTODO: O desempenho de pacientes com doença de Alzheimer (MILD-Alz e MOD-Alz) foi comparado com o de idosos sadios na recordação livre de listas de 15 palavras, utilizando quatro diferentes conjuntos de listas que continham ou não palavras relacionadas nas posições intermediárias, palavras repetidas, ou ainda palavras repetidas e semanticamente relacionadas.
RESULTADOS: O terceiro pico usual na recordação das palavras semanticamente relacionadas não foi observado em MOD-Alz; a repetição não aumentou a recordação dos pacientes; a combinação de relacionamento e repetição beneficiou apenas MILD-Alz. Em outro experimento, com palavras intermediárias relacionadas ou não, e em que a extensão das listas foi reduzida para 9 palavras, observou-se facilitação semântica em MILD-Alz e MOD-Alz.
CONCLUSÃO: A progressão da demência diminui a eficácia de fatores facilitadores da recordação.
Palavras-chave: memória, recordação livre de palavras, doença de Alzheimer, relação semântica, repetição.
One of the first and most prominent manifestations of Alzheimer's disease (AD) is memory impairment, being episodic memory severely and consistently affected (for review see1). It is also known that operations that require controlled processing, as in attention demanding tasks, decay very soon in AD patients2. Moreover, many studies have shown the loss of the ability to access and use semantic knowledge, as has been demonstrated in several kinds of tasks3,4. Impairment in the capacity to use semantic knowledge may be due to a degradation of semantic memory5,6, but this interpretation is not consensual7,8 as the possibility of a disruption of the information accessing process was not ruled out. The word free recall test is largely used to study memory dysfunctions. The subject is presented with lists of words that are read out one by one. At the end of each list, s/he is asked to remember as many words as s/he can, in any order. By studying the input positions of the remembered words, a U-shaped curve is obtained, reflecting a better recollection of the words placed in the beginning of the list (primacy effect), as well as the words in the last positions (recency effect). The primacy effect reflects an aspect of long-term memory, possibly resulting from a prolonged processing of the first words in the list when compared to those in the middle9, the recency effect, on the other hand, can be supported by short-term memory10. The introduction of semantically related words alters the pattern of the serial position curve, producing peaks of high recollection of these words11,12. Repetition of words in the middle of the lists also causes another peak of recollection of these repeated words11. The performance of AD patients in verbal free recall is impaired (e.g.12-14), with a decrease in the total number of remembered words and alterations in the serial position curve due to the absence or considerable deficit of the primacy effect and a decrease (usually modest and sometimes none at all) of the recency effect15-17.
To our knowledge no work has been done to investigate the beneficial effects of spaced repetition of items and only one18 the relatedness of words in free recall in AD patients. If the capacity to use semantic knowledge is lost because semantic memory is degraded, the result would be the lack of benefit produced by semantically related words.
In the present study we manipulated the three midlist words, introducing semantically related words or repeating words throughout the lists, in order to verify if Alzheimer's patients in mild or moderate stage would still profit from these mnemonic enhancers.
METHOD
Experiment 1
Subjects - Fifteen patients with probable AD and 9 healthy subjects (CON) with similar age and academic background were examined. The patients, referred by the Department of Neurology of Hospital São Paulo, had a history of cognitive decline and memory problems, but normal consciousness. The diagnosis of probable Alzheimer's disease was given according to the criteria of the National Institute of Neurological Disorders and Communicative Disorders and Stroke-Alzheimer's Disease and related Disorders Association - NINCDS-ADRDA 1 and the Diagnostic and Statistical Manual of Mental Disorders, third edition (DSM-III)19. Patients were tested using clinical-neurological examinations comprising laboratory, imaging (computerized tomography and magnetic resonance) as well as neuropsychological testing (including the score obtained in the Mini-Examination of the Mental State (MMSE), adapted for the Brazilian population20. Severity of clinical state was assessed by the Clinical Dementia Rating scale (CDR)21, applied by the medical staff. A clinical examination and semi-structured interview was carried out previously and confirmed by an informant (e.g., a family member). At the end, 6 patients that presented with CDR=1 were classified as mild (MILD-Alz) stage and 9 that presented with CDR=2 were classified as moderate (MOD-Alz) stage, and following the recommendations of the Brazilian Academy of Neurology as regarding cognitive evaluation22. Table 1 shows the demographic characteristics of the sample and MMSE data. All patients lived with their families and did not require special care. Patients with other specific causes of dementia, or with brain lesions, delirium and depression were excluded. After the clinical tests, the patients were referred to neuropsychological evaluation performed in several sessions in which lists of words were applied.
Material - Twenty-four lists of words were prepared and tested in advance, each list containing 15 words, 2-3-syllable common nouns or adjectives of the Portuguese language taken from a pocket dictionary. In the first set of 6 lists all words had no apparent semantic relations with each other (unrelated lists); a second set of 6 lists (related lists) contained three semantic related words in the intermediary positions (corresponding to the input positions 7, 8 and 9), as for example, the Portuguese words for milk, cheese and butter. In other set of 6 unrelated words, the three intermediary words were the same across the lists (repeated lists). Finally, in other 6 lists, the three repeated midlist words were also semantically related (repeated-related lists). Besides the midlist words of the related and repeated-related lists, no other words within the same list were semantically related. Phonetic relations within the same list such as rhymes and sequences of words starting with the same sound were avoided.
Procedure - The first two sets of lists were applied in one session and the other two sets in another session. In each session each kind of list was alternated with the other. The lists were read out slowly (approximately one word per second) and an oral retrieval of the words, written down by the examiner, was done immediately after each list. The participants were said to recall as many words as possible without worrying about their order. Time for recall was free.
Experiment 2
Subjects - Twenty-nine (18 mild and 11 moderate) other patients with probable AD and 24 healthy elderly with similar age and schooling background participated in this experiment (See Table 1). Inclusion and exclusion criteria were the same of Experiment 1.
Material - Eight lists of 9 words each were prepared. The midlist words (positions 4-5-6) were either semantically related (4 unrelated lists) or not (4 unrelated lists). The lists were presented in a quasi-random sequence, avoiding more than two lists of the same type in sequence.
Procedure - The procedure was the same as that of Experiment 1.
Data analysis
The total number of correctly recalled words in the various lists was first analysed by one-way ANOVA, followed by Tukey's a posteriori test for unequal samples. After that, the input positions were grouped in five blocks of three words. The first block was considered as the generator of the primacy effect, and the last one the generator of the recency effect. The group in the middle corresponded to the positions 7,8 and 9 where the manipulations (semantic relations and/or repetition) were introduced. To evaluate the number of recalls, a two-way ANOVA for repeated measures, having as factors the groups of subjects (CON, MILD-Alz and MOD-Alz) and the types of list (unrelated, related, repeated and repeated-related or input positions, followed by Tukey's test for unequal samples. All the tests were two-tailed and the level of significance was 5%.
RESULTS
Experiment 1
Total number of words recalled - The total number of words remembered can be seen in Table 2. Significant differences were detected in all types of lists: unrelated lists (F(2,21)=10.9; p=0.0005); related F(2,21)= 12.1; p=0.0003); lists with repeated words (F(2,21)=31.2; p=0.0001); and in repeated-related lists (F(2,21)=31.9; p=0.0003). A higher performance was seen in the control group as compared to the MILD-Alz and MOD-Alz groups in all types of lists (ps<0.04 at least, Tukey's test). The MILD-Alz group achieved a higher performance than the MOD-Alz group in the repeated-related lists (p=0.03).
Removing either the first 3 or the last 3 words in each list from the calculations, the statistically significant differences remained the same in most cases; an exception was seen in that the control group was superior to MOD-Alz (p=0.02) but not to MILD-Alz when the first 3 words were not considered.
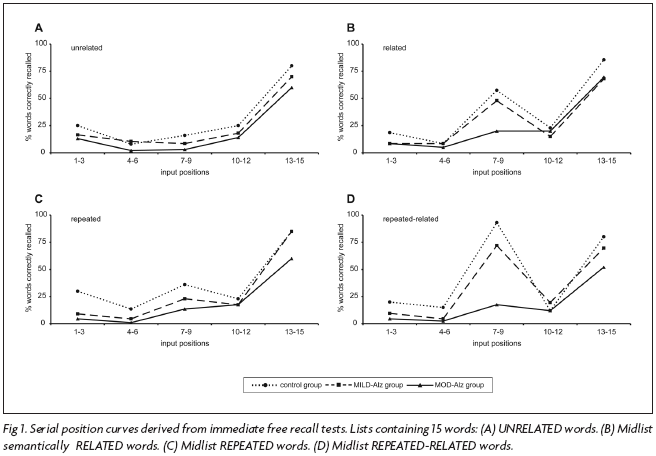
First 3 input positions - A two-way ANOVA showed significant differences between groups [F(2,21)=17.8; p=0.00003] and between types of lists [F(3,63)=3.6; p=0.01], but no interaction between these factors [F(6,63)=1.7; p=0.11] (Fig 1 shows the serial position curves for all types of lists). Differences between controls and MILD-Alz were seen in the repeated lists (p=0.0006; Tukey); between controls and MOD-Alz in the repeated lists (p=0.0001), and in the repeated-related lists (p=0.012). In the unrelated lists the difference between controls and MOD-Alz was marginally significant (p=0.059). Primacy of normal participants and of the two groups of patients, MILD-Alz and MOD-Alz, was not different in the various types of lists.
Intermediary input positions - Differences between groups [F(2,21)=32.4; p<0.00001] and between types of list [F(3,63)=53.24; p<0.0001] were detected, as well as an interaction of these factors [F(6,63)=8.82; p=0.000001].
Tukey's test showed that control's recall of the semantically related words was superior than the recall of the unrelated words in the same intermediary positions in the all-unrelated lists (p=0.0001), as well as the repeated-related lists compared to the repeated and unrelated lists (p=0.0001). Repetition alone did not reach statistical significance. But, repetition enhanced the facilitating effect of semantic relations in recalling midlist words (p=0.0002). Controls had a superior performance than MOD-Alz (p=0.0001) in the related words, and had better performance than MILD-Alz (p=0.03) and MOD-Alz (p=0.0001) in the repeated-related words.
The MILD-Alz group recalled more semantically related midlist words than the unrelated words occupying the same positions in the all-unrelated lists (p=0.02); this group, however, did not benefit from the repetition of words alone. This group also recalled more repeated-related words than repeated but semantically unrelated words (p=0.0001), and was superior to MOD-Alz group (p=0.0001) in repeated-related words. Statistically significant differences were not detected in the group MOD-Alz. Therefore, these patients did not benefit from semantic relations between words nor from repetition of words across lists, neither isolately or in conjunction.
Last 3 input positions - There were differences between groups [F(2,21)=3.6; p=0.04) and between types of lists [F(3,63)=3.37; p=0.01] but no interaction between these factors [F(6,63)=0.95; p=0.46]. The performance of group MOD-Alz in the repeated lists was significantly inferior compared to controls (ps between 0.03 and 0.06).
In the experiment 1, we observed that MOD-Alz patients had no increment in recall of semantically related words. The purpose of the experiment 2 was to investigate if this impairment is due to a degradation of semantic memory or to a difficulty of accessing the semantic store. To address this question we asked whether the lack of benefit from semantic relatedness is related to the length of the list. If the semantic memory is deteriorated the capacity to benefit should be entirely lost and reduction in list length should not bring back the beneficial effect of the semantically related words. Otherwise, if this impairment is not related in a crucial way to a degradation of semantic memory, but rather to its accessibility, the introduction of semantically related words would enhance recall in shorter lists.
Experiment 2
Total number of words recalled - A two-way ANOVA for the total number of remembered words detected a statistically significant group effect (F(2,50)=12.76432; p<0.0001). The Tukey post-hoc test showed that the control group had a higher performance as compared to the other two groups (p<0.05). The list effect was also significant as the lists containing semantic related words were more remembered as compared to all-unrelated lists (F(1,50)=9.79677; p=0.003). No interaction of type of list and group was seen (F(2,50)=0.41328; p=0.66).
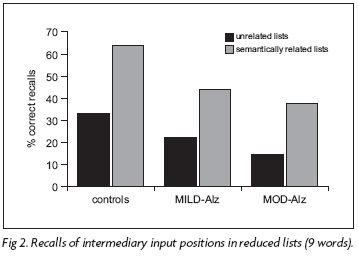
Intermediary input positions - A two-way ANOVA for the midlist positions revealed differences between groups [F(2,50)=11.7; p<0.001) and between types of lists [F(1,50)=64,64; p<0.0001], but no interaction between these factors [F(2,50)=0.95; p=0.39] (Fig 2). Tukey test showed that the semantically related words were more recalled than the unrelated ones in all three groups, although the performance of the two AD groups were significantly inferior in comparison with controls (ps<0.01). The difference between the two AD groups was not statistically significant.
DISCUSSION
The results corroborate the impairment of verbal free recall in AD patients. Moreover, we detected a deficit not only in moderate AD patients, but also in the early stage of the disease, both in the common unrelated lists and in the lists with repetition of the midlist words. Even when removed, for the purpose of analysis, the three initial words, corresponding to the primacy effect (more pronounced in normal subjects) or the three last words, corresponding to the recency effect (still very marked in AD patients), the decrease in the score of total remembered words remained. Therefore, the test proved to be sensitive enough to detect memory deficiencies in AD patients even in the early stages of the disease. Differences between MILD-Alz and MOD-Alz occurred only in lists with repeated words in the middle.
Absence or reduction of primacy in AD patients is a well substantiated finding and Bemelmans and Goekoop23 reported that the absence of primacy in these patients is related to the length of the list, being present in lists of up to 9 words, but not of 15, showing, thus, that the primacy effect is not entirely lost. In our MOD-Alz patients, but not in MILD-Alz, primacy was decreased when compared to normal subjects. It can be noticed, however, that primacy in the control subjects was already relatively low, which is in accordance with previous reports that show a decline in these measure in elderly subjects24. It should also be stressed that patients in the two stages of the disease did not differ from each other, that is, the severity of dementia does not seem to be an important factor in the decline of primacy, in disagreement with Pepin and Eslinger15 who found a reduction of primacy correlated with the severity of the dementia. Our data suggest that primacy becomes deficient with aging, and that AD simply increases the impairment.
In the present study we observed recency in AD patients, though a slight decrease can be noted in the moderate stage of the disease, especially in the lists in which the middle words were repeated. Some authors17 have reported a recency deficit in AD patients, but others (e.g.,16) did not confirm this deficiency. Such discrepancies may be due to different degrees of severity of the disease in the various studies, as according to Pepin and Eslinger15. Recency is only affected in a more advanced stage of dementia,.or to methodological differences, as the recency effect is, to a certain extent, arbitrarily defined, there being a great variability in the number of final words that different authors take as a measure of recency. In any case, impairment of short-term memory evidenced by a decline of recency is not a robust phenomenon in AD.
Repetition of midlist words brought about a third peak in the serial position curve of normal subjects, but not of AD patients, even in the early stage. As the same type of list was always alternated with other type, there was a considerable gap between the appearance of the repeated words. They were repeated at intervals of 2 to 3 minutes, which is the approximate time it took for a list to be read out and the words to be remembered, resembling a delayed instead of immediate retrieval. During this period, the ability to retrieve the repeated words may have vanished in these severely amnesic patients. This can explain the absence of the repetition effect, that is, the patients simply did not remember that some words were repeated.
The presence of semantically related words in the intermediary input positions of longer lists also caused a third peak in the serial position curve in the normal subjects and in the mild stage patients. Patients in the moderate stage did not profit from the semantic facilitating effect in 15-word lists. The association of semantically related words and the repetition of the same words in intermediary positions led to an even higher increase of retrieval in normal subjects. Mild AD patients did benefit from the association of these two facilitating factors, even though they presented a slightly lower score than that of normal subjects. Moderate AD patients, however, did not get any profit from this association. A comparison can be made with other patients that also suffer from an impairment of memory but due to other etiologies, as is the case of multiple sclerosis patients in which both semantically related words and repetition of midlist words across several lists, enhance free recall of the target words11.
Degradation of semantic knowledge could be responsible for the lack of benefit in the lists containing semantically related words in patients of the group MOD-Alz. However, the experiment 2 showed that the capacity to use semantic information is not entirely lost because it reappears in 9-word lists. It seems, then, that the semantic information brought about by semantic relatedness is made unaccessible rather than lost when the patient has to cope with a large number of to-be-remembered items; with smaller sets of material the appropriate semantic information is available. Interestingly, a similar result, but regarding the primacy effect, was obtained by Bemelmans and Goekoop23 who have shown that in AD patients primacy is evident in lists of up to 9 words, but not of 15. We suggest that a diminished working memory span can be an important factor in determining these deficiencies in AD patients.
Baddeley's25 working memory framework offer several possibilities to interpret the present findings, since impairment of several aspects of working memory has been reported in AD, such as reduction of attentional resources18,26,27, and in tasks demanding executive processes28. In fact, Germano and Kinsella29 have argued that acquisition deficits in early AD may be related to impairment either in working memory storage capacity, in allocation of attention (a function considered to be exerted by the central executive), or in episodic buffer function. In consonance with this idea, we have found that even in healthy older subjects small deficits of semantic facilitation as well as of primacy effect were related to working memory functioning30. It should be noted, however, that the gain in semantic facilitation with shorter lists was not complete, indicating that deterioration of semantic memory also plays a partial role in determining MOD-Alz deficit.
The data from the present study show that mild AD patients still retain considerable mnemonic abilities that can help in a neuropsychological rehabilitation program aimed at improving their cognitive performance. But they also show a dramatic loss of these capacities as fhe disease develops.
ACKNOWLEDGEMENTS - We thank regina A. Ueta, Elisângela C. Oliveira, Fabíola Canali and Vera Lucia D. Vieira for their help in collecting data and in neuropsychological testing.
Received 14 May 2007, received in final form 7 March 2008. Accepted 24 March 2008.
Dr. Orlando F.A. Bueno - Department of Psychobiology / Universidade Federal de São Paulo / Escola Paulista de Medicina - Rua Napoleão de Barros 925 - 04024-002 São Paulo SP - Brasil. E-mail: tarso@dfvneuro.com.br
Financial support: Associação Fundo de Incentivo à Psicofarmacologia (AFIP) and conselho Nacional de Pesquisa e Tecnologia (CNPq)
- 1. Carlesimo GA, Oscar-Berman M. Memory deficits in Alzheimer's patients: a comprehensive review. Neuropsychol Rev 1992;3:119-169.
- 2. Jorm AF. Controlled and automatic information processing in senile dementia: a review. Psychol Med 1986;16:77-88.
- 3. Bayles KA, Tomoeda CK. Confrontation naming impairment in dementia. Brain Lang 1983;9:98-114.
- 4. Martin A, Fedio P. Word production and comprehension in Alzheimer's disease: the breakdown of semantic knowledge. Brain Lang 1983;19:124-141.
- 5. Binetti G, Magni E, Cappa SF, Padovani A, Bianchetti A, Trabucchi M. Semantic memory in Alzheimer's disease: an analysis of category fluency. J Clin Exp Neuropsychol 1995;17:82-89.
- 6. Hodges JR, Salmon DP, Butters N. Semantic memory impairment in Alzheimer's disease: failure of access or degraded knowledge. Neuropsychologia 1992;30:301-314.
- 7. Diaz M, Sailor K, Cheung D, Kuslansky G. Category size effects in semantic and letter fluency in Alzheimer's patients. Brain Lang 2004;89:108-114.
- 8. Nicholas M, Obler LK, Au R, Albert ML. On the nature of naming errors in aging and dementia, a study of semantic relatedness. Brain Lang 1996;54:184-195.
- 9. Rundus D. Analysis of rehearsal processes in free recall. J Exp Psychol 1971;89:63-77.
- 10. Capitani E, Della Sala S, Logie RH, Spinnler H. Recency, primacy, and memory: reappraising and standardising the serial position curve. Cortex 1992;28:315-342.
- 11. Andrade VM, Oliveira MGM, Miranda MC, Oliveira ASB, Oliveira EML, Bueno OFA. Semantic relations and repetition of items enhance the free recall of words by multiple sclerosis patients. J Clin Exp Neuropsychol 2003;25:1070-1078.
- 12. Nogueira AML, Pompéia S, Galduróz JCF, Bueno OFA. Effects of a benzodiazepine on free recall of semantically related words. Human Psychopharmacol Clin Exp 2006;21:327-336.
- 13. Desgranges B, Baron J-C, Giffard B, et al. The neural basis of intrusions in free recall and cued recall: a PET study in Alzheimer's disease. Neuroimage 2002;17:1658-1664.
- 14. Moulin CJA, James N, Freeman JE, Jones RW. Deficient acquisition and consolidation: intertrial free recall performance in Alzheimer's disease and mild cognitive impairment. J Clin Exp Neuropsychol 2004;26:1-10.
- 15. Pepin EP, Eslinger PJ. Verbal memory decline in Alzheimer's disease: a multiple-processes deficit. Neurology 1989;39:1477-1482.
- 16. Spinnler H, Della Sala S, Bandera R, Baddeley A. Dementia, aging, and the structure of human memory. Cog Neuropsychol 1988;5:193-211.
- 17. Wilson RS, Bacon LD, Fox JH, Kaszniak AW. Primary memory and secondary memory in dementia of the Alzheimer type. J Clin Neuropsychol 1983;5:337-344.
- 18. Carlesimo GA, Mauri M, Graceffa AM, et al. Memory performances in young, elderly, and very old healthy individuals versus patients with Alzheimer's disease: evidence for discontinuity between normal and pathological aging. J Clin Exp Neuropsychol 1998;20:14-29.
- 19. McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM. Clinical diagnosis of Alzheimer's disease: report of the NINCDS-ADRDA work group under the auspices of Department of Health and Human Services Task Force on Alzheimer's disease. Neurology 1984;34:939-944.
- 20. Bertolucci PHF, Brucki SMD, Campacci SR, Juliano Y. O Mini-Exame do Estado Mental em uma população geral: impacto da escolaridade. Arq Neuropsiquiatr 1994;52:1-7.
- 21. Morris JC. The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 1993;43:2412-2414.
- 22. Nitrini R, Caramelli P, Bottino CMD, Damasceno BP, Brucki SMD, Anghinah R. Diagnosis of Alzheimer's disease in Brazil: cognitive and functional evaluation. Recommendations of the Scientific Department of Cognitive Neurology and Aging of the Brazilian Academy of Neurology. Arq Neuropsiquiatr 2005;63:720-727.
- 23. Bemelmans KJ, Goekoop JG. The contribution of list length to the absence of the primacy effect in word recall in dementia of the Alzheimer type. Psychol Med 1991;21:1047-1050.
- 24. Raymond BJ. Free recall among the aged. Psychol Rep 1971;29:1179-1182.
- 25. Baddeley A. Working memory: looking back and looking forward. Nature Rev Neurosci 2003;4:829-839.
- 26. Baddeley AD, Baddeley HA, Bucks RS, Wilcock GK. Attentional control in Alzheimer's disease. Brain 2001;124:1492-1508.
- 27. Nestor PG, Parasuraman R, Haxby JV, Grady CL. Divided attention and metabolic brain dysfunction in mild dementia of the Alzheimer's type. Neuropsychologia 1991;29:379-387.
- 28. Morris RG. Working memory in Alzheimer-type dementia. Neuropsychology 1994;8:544-554.
- 29. Germano C, Kinsella GJ. Working memory and learning in early Alzheimer's disease. Neuropsychology Rev 2005;15:1-10.
- 30. De Luccia GCP, Bueno OFA, Santos R F. Recordação livre de palavras e memória operacional em idosos. Disturb Comunic 2005;17:347-358.
Publication Dates
-
Publication in this collection
29 Sept 2008 -
Date of issue
June 2008
History
-
Received
14 May 2007 -
Accepted
24 Mar 2008