ABSTRACT
Objective
To evaluate cutaneous allodynia among patients with chronic and episodic migraine in a tertiary headache clinic.
Methods
80 subjects with episodic migraine and 80 with chronic migraine were assessed in a tertiary hospital. The 12-item Allodynia Symptom Checklist/Brazil questionnaire was applied to classify subjects according to the presence and severity of cutaneous allodynia.
Results
Cutaneous allodynia was identified in 81.3% of the episodic migraine group and 92.5% of the chronic migraine group (p = 0.03). No increased association could be attributed to chronic migraine when adjusted by years with disease (PR = 1.12; 95%CI = 0.99 to 1.27; p = 0.06). The groups also did not differ in the severity of allodynia, and severe presentation was the most frequent.
Discussion
Both groups seemed to be similarly affected in the cephalic and extracephalic regions, with the same severity.
Conclusion
Cutaneous allodynia is more frequent in chronic migraine, and its presence and severity seems to be more associated with the duration of the disease.
hyperalgesia; migraine disorders
RESUMO
Objetivo
Avaliar a característica da alodinia cutânea em indivíduos com migrânea crônica e episódica em um hospital terciário.
Métodos
80 sujeitos com migrânea episódica e 80 com migrânea crônica de um hospital terciário foram avaliados. O questionário 12-item Allodynia Symptom Checklist/Brasil foi aplicado e classificou os sujeitos quanto a presença e severidade da alodinia cutânea.
Resultados
A alodinia cutânea esteve presente em 81,3% dos migranosos episódicos e 92,5% nos crônicos (p = 0.03). Nenhuma associação pode ser atribuída a migrânea ao ser ajustada pela variável anos com doença (PR = 1.12; 95%IC = 0.99 para 1.27; p = 0.06). Os grupos não diferiram em relação à severidade da alodinia e a classificação severa foi a mais frequente.
Discussão
Ambos os grupos pareceram ser igualmente afetados nas regiões cefálicas e extracefálicas com a mesma severidade.
Conclusão
A alodinia cutânea é mais frequente na migrânea crônica, mas a presença e severidade parece estar mais associada com a duração da doença.
hiperalgesia; transtornos da enxaqueca
Migraines affect 10% of the global population11. Robbins MS, Lipton RB. The epidemiology of primary headache disorders. Semin Neurol. 2010;30(2):107-19. https://doi.org/10.1055/s-0030-1249220
https://doi.org/10.1055/s-0030-1249220...
and start as an episodic disease that can evolve to chronicity. Chronic migraine is characterized by the presence of headache on 15 or more days within a month for more than three months22. Carod-Artal FJ, Irimia P, Ezpeleta D. [Chronic migraine: definition, epidemiology, risk factors and treatment]. Rev Neurol. 2012;54(10):629-37. Spanish.. On at least eight days, the headache features should be of a migraine headache and the pain possibly relieved by a triptan or ergot derivative33. Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia. 2013;33(9):629-808. https://doi.org/10.1177/0333102413485658
https://doi.org/10.1177/0333102413485658...
. Cutaneous allodynia, a risk factor for chronic migraine44. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
https://doi.org/10.1212/01.wnl.000031064...
, increases the discomfort and disability of patients with acute migraine attacks55. Kalita J, Yadav RK, Misra UK. A comparison of migraine patients with and without allodynia symptoms. Clin J Pain. 2009;25(8):696-8. https://doi.org/10.1097/AJP.0b013e3181b12dd3
https://doi.org/10.1097/AJP.0b013e3181b1...
and is recognized as a clinical manifestation of central sensitization in migraine patients66. Tietjen GE, Brandes JL, Peterlin BL, Eloff A, Dafer RM, Stein MR et al. Allodynia in migraine: association with comorbid pain conditions. Headache. 2008;49(9):1333-44. https://doi.org/10.1111/j.1526-4610.2009.01521.x
https://doi.org/10.1111/j.1526-4610.2009...
.
Cutaneous allodynia is defined as the perception of pain or discomfort in response to innocuous thermal (heat or cold) and/or mechanical (static or dynamic) stimuli applied to normal skin66. Tietjen GE, Brandes JL, Peterlin BL, Eloff A, Dafer RM, Stein MR et al. Allodynia in migraine: association with comorbid pain conditions. Headache. 2008;49(9):1333-44. https://doi.org/10.1111/j.1526-4610.2009.01521.x
https://doi.org/10.1111/j.1526-4610.2009...
. It occurs in approximately 80% of migraine sufferers, with a greater prevalence among women77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
,88. Burstein R, Yarnitsky D, Goor-Aryeh I, Ransil BJ, Bajwa ZH. Bajwa. An association between migraine and cutaneous allodynia. Ann Neurol. 2000;47(5):614-24. https://doi.org/10.1002/1531-8249(200005)47:5<614::AID-ANA9>3.0.CO;2-N
https://doi.org/10.1002/1531-8249(200005...
,99. Jakubowski M, Silberstein S, Ashkenazi A, Burstein R. Can allodynic migraine patients be identified interictally using a questionnaire? Neurology. 2005;65(9):1419-22. https://doi.org/10.1212/01.wnl.0000183358.53939.38
https://doi.org/10.1212/01.wnl.000018335...
,1010. Ashkenazi A, Silberstein S, Jakubowski M, Burstein R. Improved identification of allodynic migraine patients using a questionnaire. Cephalalgia. 2007;27(4):325-9. https://doi.org/10.1111/j.1468-2982.2007.01291.x
https://doi.org/10.1111/j.1468-2982.2007...
. This symptom is a dynamic phenomenon, the intensity of which varies throughout the course of a migraine episode77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
.
Cutaneous allodynia interferes in the effectiveness of abortive therapy with triptans, reducing their effectiveness in total pain relief and in preventing relapse within 24 hours1111. Burstein R, Collins B, Jakubowski M. Defeating migraine pain with triptans: a race against the development of cutaneous allodynia. Ann Neurol. 2004;55(1):19-26. https://doi.org/10.1002/ana.10786
https://doi.org/10.1002/ana.10786...
. In order to be effective, triptans must be administered before the presence of cutaneous allodynia1212. Misra UK, Kalita J, Bhoi SK. Allodynia in migraine: clinical observation and role of prophylactic therapy. Clin J Pain. 2013;29(7):577-82. https://doi.org/10.1097/AJP.0b013e31826b130f
https://doi.org/10.1097/AJP.0b013e31826b...
. Therefore, identifying the presence of allodynia and educating patients on the particularities of this symptom are essential for adequate treatment.
Among the available methods to identify cutaneous allodynia, the only tool that allows classification of the severity of cutaneous allodynia presentation is the 12-item Allodynia Symptom Checklist (ASC-12) questionnaire77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
. Studies comparing the characteristics of cutaneous allodynia in chronic and episodic migraine sufferers are still scarce and results are conflicting regarding the severity of cutaneous allodynia in both groups. Schwedt et al.1313. Schwedt TJ, Krauss MJ, Frey K, Gereau RW 4th. Episodic and chronic migraineurs are hypersensitive to thermal stimuli between migraine attacks. Cephalalgia. 2010;31(1):6-12. https://doi.org/10.1177/0333102410365108
https://doi.org/10.1177/0333102410365108...
reported differences in the ASC-12 score of migraine sufferers compared to a control group, but no differences were found in the severity of cutaneous allodynia among patients with chronic and episodic migraine. On the other hand, Bigal et al.44. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
https://doi.org/10.1212/01.wnl.000031064...
verified that cutaneous allodynia is influenced by the frequency of attacks, as it is more prevalent and severe in chronic migraine sufferers than in episodic migraine sufferers.
Thus, the objective of this study was to assess cutaneous allodynia in chronic and episodic migraine sufferers at a tertiary outpatient headache clinic. The hypothesis is that cutaneous allodynia is influenced by the frequency of attacks and therefore, chronic migraine sufferers have a higher frequency and severity of cutaneous allodynia compared to episodic migraineurs.
METHODS
Participants
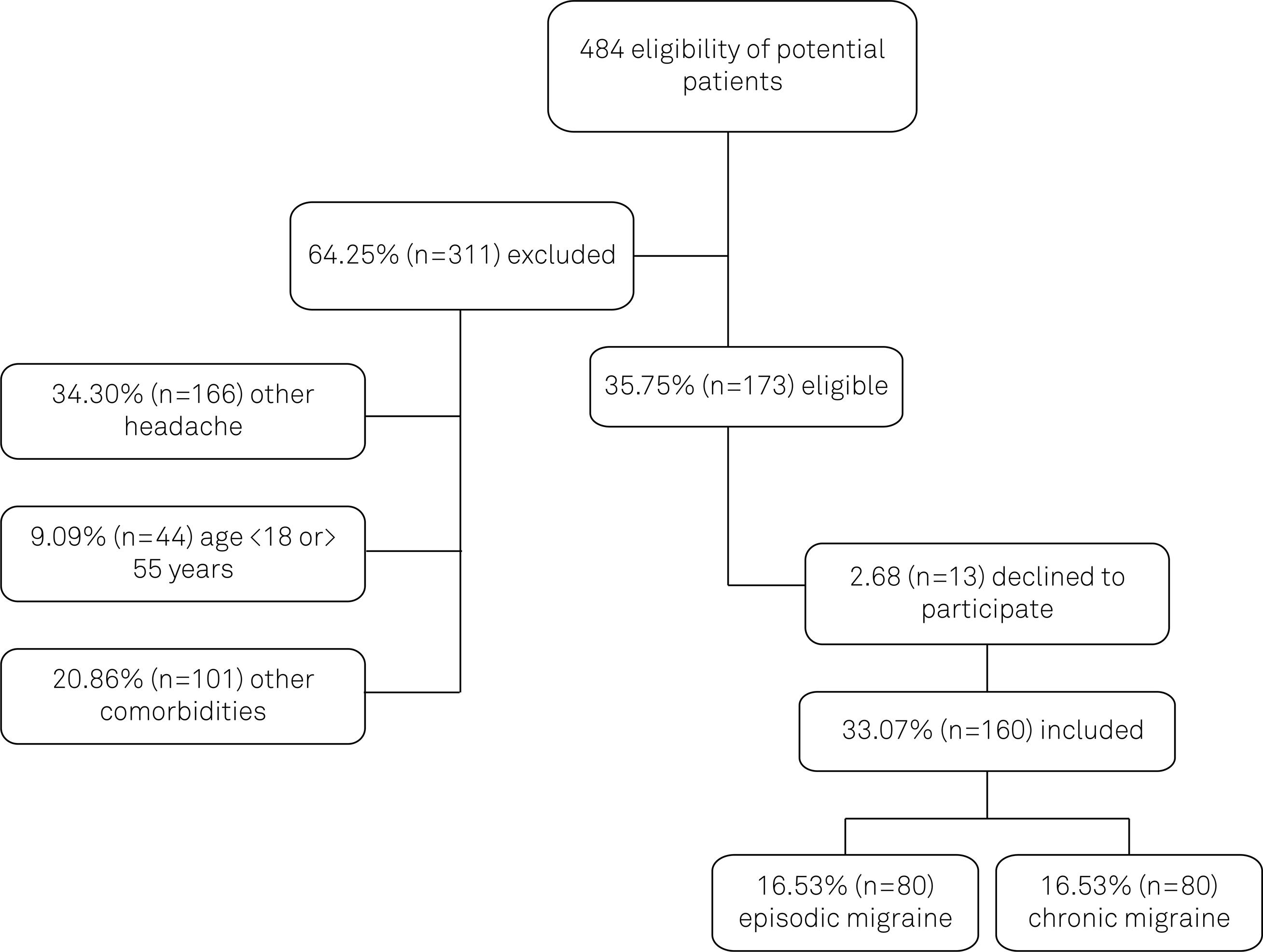
Among of 484 potential patients, 64.25% were excluded and 2.68% declined to participate the study, resulting in a final sample of 160 participants (Figure 1). The sample included patients of both genders between the ages of 18 and 55 who had been diagnosed with migraine, according to the third edition of International Classification of Headache, between July 2013 and May 2014. The diagnosis was made by an experienced neurologist in a tertiary hospital during a routine appointment. Standard neurological examinations were performed and neuroimaging was ordered only if necessary. The neurologist checked the information on the frequency and duration of migraine attacks. The absence of systemic comorbidities was confirmed by medical records. Migraine sufferers were allocated to two groups: the episodic migraine group, comprising patients with headache on fewer than 15 days within a month in the last three months; and the chronic migraine group, comprising those affected by headache on 15 days or more within a month in the last three months1414. Olesen J, Bousser MG, Diener HC, Dodick D, First M, Goadsby PJ et al. New appendix criteria open for a broader concept of chronic migraine. Cephalalgia. 2006;26(6):742-6. https://doi.org/10.1111/j.1468-2982.2006.01172.x
https://doi.org/10.1111/j.1468-2982.2006...
, and who presented with migraine headache features on at least eight attacks, relieved by a triptan or ergot derivative33. Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia. 2013;33(9):629-808. https://doi.org/10.1177/0333102413485658
https://doi.org/10.1177/0333102413485658...
. Exclusion criteria were: 1) diagnosis of another headache associated with migraine, including medication-overuse headache; 2) diagnosis of fibromyalgia, trigeminal neuralgia and systemic diseases that could lead to a peripheral neuropathy; 3) patients with an acute migraine attack. As the protocol of the headache clinic, all patients received individual prescriptions for the use of prophylactic medication. The most prescribed drugs were antidepressants and anticonvulsants, respectively, amitriptyline and topiramate. The most common abortive medications prescribed were triptans, including sumatriptan and naratriptan and all patients received instructions to avoid overuse of analgesics. The study was approved by the local ethics committee (process no. 15580/2012).
A non-blind examiner was in charge of the patient selection: checking all possible patients who met the inclusion criteria and confirming the exclusion criteria in the medical history of the hospital register. Then, the examiner confirmed the criteria by inviting the patient to participate. After acceptance and signing the informed consent, patients were questioned about their migraine characteristics. Years with migraine, the frequency of attacks (days with headache per month) and duration of attacks (hours) was based on self-reports. Then a blind examiner administered the ASC-12.
Questionnaire
The ASC-12 is capable of identifying cutaneous allodynia according to the nature of the stimulus: thermal, mechanical static or mechanical dynamic77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
. It is a self-completion questionnaire and consists of 12 questions regarding discomfort during migraine episodes during everyday activities, such as combing hair, wearing glasses, and taking a shower1515. Florencio LL, Chaves TC, Branisso LB, Gonçalves MC, Dach F, Speciali JG et al. 12 item allodynia symptom cheklist/Brasil: cross-cultural adaptation, internal consistency and reproducibility. Arq Neuropsiquiatr. 2012;70(11):852-6. https://doi.org/10.1590/S0004-282X2012001100006
https://doi.org/10.1590/S0004-282X201200...
. Scores range from 0 to 24 and the presence of cutaneous allodynia is attributed to those who score ≥ 3 points. Classifications of patients according the presence and severity of cutaneous allodynia are: no allodynia (0–2 points), mild allodynia (3–5 points), moderate allodynia (6–8 points) and severe allodynia (9 or more points)77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
. Furthermore, based on an exploratory factor analysis and interpretation by the authors, items were grouped into three domains of cutaneous allodynia: thermal domain, measured by the items “taking a shower,” “exposure to heat,” “exposure to cold,” “resting your face or head on a pillow” and “shaving your face”; the mechanical dynamic domain, measured by the items “combing your hair,” and “pulling your hair back”; and the mechanical static domain, measured by the items “wearing eyeglasses,” “wearing contact lenses,” “wearing earrings,” “wearing a necklace” and “wearing tight clothing.” The Brazilian version of the ASC-12 (ASC-12/Brazil) applied in this study kept all the criteria of the original, and presents an excellent reliability1515. Florencio LL, Chaves TC, Branisso LB, Gonçalves MC, Dach F, Speciali JG et al. 12 item allodynia symptom cheklist/Brasil: cross-cultural adaptation, internal consistency and reproducibility. Arq Neuropsiquiatr. 2012;70(11):852-6. https://doi.org/10.1590/S0004-282X2012001100006
https://doi.org/10.1590/S0004-282X201200...
.
Statistical analysis
Descriptive analysis and percentages were used to characterize the sample and summarize cutaneous allodynia characteristics. Comparison between groups regarding the severity of cutaneous allodynia were made using the chi-square test.
The prevalence ratio, considering allodynia as the outcome, was analyzed through Poisson regression with robust variance, to verify the risk of chronic migraine presenting with the symptom as opposed to episodic migraine. Similarly, prevalence ratios considering the severity of cutaneous allodynia were analyzed using a separate Poisson regression with robust variance. Finally, the prevalence ratio was adjusted for duration of headache in order to verify the risk of chronic migraine sufferers presenting with cutaneous allodynia, and its severity, in comparison with the episodic migraine group.
A more detailed description of the items on the ASC-12/Brazil was conducted, using the frequency of positive responses for each item of the questionnaire in both groups. We then established the correlation between the duration of migraine and the ASC-12/Brazil overall score and each of the three domains by using quantile regression. This process allowed for a comparison among medians aided by STATA 11 software1616. Koenker R, Hallock KF. Quantile regression. Cambridge: Cambridge University Press; 2005.. All statistical analyses adopted a level of significance of 0.05 and a confidence interval of 95% (CI 95%).
RESULTS
Table 1 shows the sample’s sociodemographic and migraine characteristics. Cutaneous allodynia was observed in 139 out of 160 participants (86.87%). The prevalence of cutaneous allodynia in the episodic migraine group was 81.3% and in the chronic migraine group, 92.5% (p = 0.03) (Table 2).
Regarding the severity of cutaneous allodynia, both groups presented with a high percentage of severe cutaneous allodynia: 48.75% chronic migraine and 40% episodic migraine (Table 2). However, there were no differences among levels of severity between the groups.
Quantile regression revealed that only the duration of migraine influenced cutaneous allodynia, and its effect was only evident when considering the overall score (0.08; CI95% 0.01–0.15; p = 0.03)
Therefore, the raw prevalence ratio (PR) was adjusted for the duration of migraine. Before the adjustment, the chronic migraine group presented with a significant increased risk of association with cutaneous allodynia of 14% relative to the episodic migraine group (PR = 1.14; 95%CI = 1.01 to 1.29; p-value = 0.04). However, this risk is lowered when adjusted for duration of the migraine and without evidence of increase (PR = 1.12; 95%CI = 0.99 to1.27; p-value = 0.06).
Comparative analysis between the groups in terms of the presence of cutaneous allodynia revealed a prevalence ratio greater than 1 for all severity classifications. However, there was no evidence that cutaneous allodynia was more associated with the chronic migraine group when the confidence interval was considered, as illustrated in Table 3.
No differences could be demonstrated between the groups regarding the thermal (p = 0.91), mechanical static (p = 0.50) and dynamic domains (p = 0.35). In addition, the chronic migraine group displayed a greater mean overall score on the ASC-12/Brazil questionnaire (8.1 - SD±3.9) compared with the episodic migraine group (7.5 - SD±4.4), Figure 2.
Mean of overall scores and scores for thermal, mechanical static and mechanical dynamic dimensions of the ASC-12/Brazil questionnaire in the episodic migraine and chronic migraine groups.
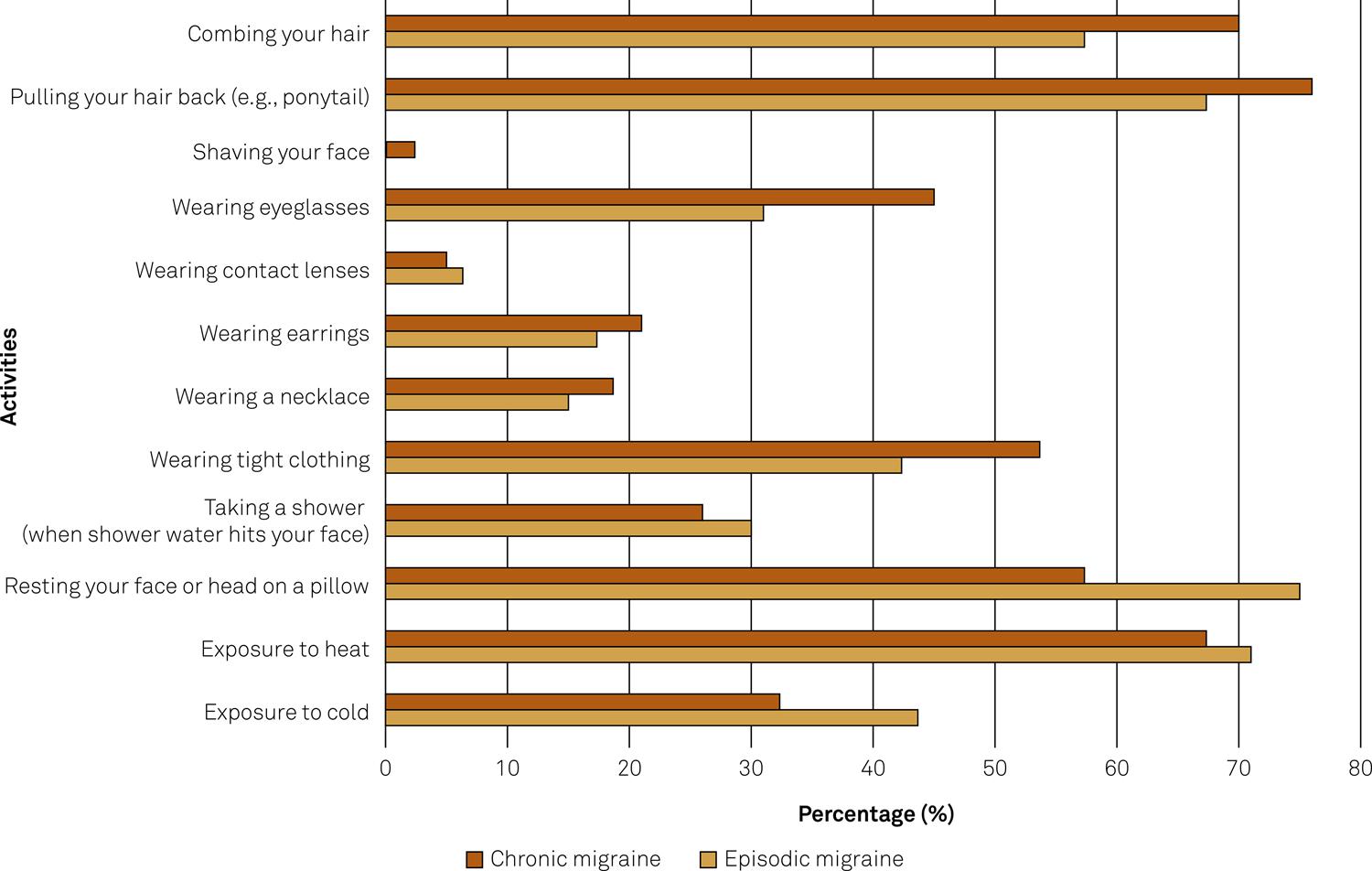
Regarding impaired activities, the chronic migraine group presented with a greater frequency of cutaneous allodynia in seven out of the 12 items. Among episodic migraine sufferers, the most reported activity was in the thermal domain, while in the chronic migraine group, it was in the mechanical dynamic domain. The frequency of positive response to the item “wearing tight clothing” was 42% for episodic migraine sufferers and 53.7% for chronic migraine sufferers indicating that the latter also present with symptoms of extracephalic allodynia (Figure 3).
Frequency of positive responses for each item in the episodic migraine and chronic migraine groups.
DISCUSSION
Our hypothesis that chronic migraine would present with a greater prevalence and worse severity of cutaneous allodynia than episodic migraine cannot be confirmed. The prevalence found was significantly higher in chronic migraine compared to episodic migraine but after adjustment of the years with migraine, no association with increased risk of cutaneous allodynia can be attributed to chronic migraine. Also, the severity of cutaneous allodynia seems to be similar for both according to the ASC-12/Brazil.
The prevalence of cutaneous allodynia observed in episodic migraine (81.3%) and chronic migraine (92.5%) was greater than that reported by Bigal et al.44. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
https://doi.org/10.1212/01.wnl.000031064...
(63.2% and 68.3% respectively), which could reflect the difference between samples. Even so, our results are in agreement in terms of a greater prevalence of the symptom in the chronic migraine group.
The greater prevalence of cutaneous allodynia observed in chronic migraine sufferers compared to episodic migraine sufferers could be explained by central sensitization, clinically represented by cutaneous allodynia. Central sensitization is characterized by increased reactivity of the second-order neurons in the spinal cord or the brainstem, or of the third-order neurons in the thalamus. In the case of migraine, the trigeminal neurons in the pons (second-order neurons) become sensitized by the peripheral stimuli from trigeminal neurons of the meninges (first-order neurons), which occurs in each attack. As the trigeminal nucleus in the pons also receives convergent afferent input from the skin of the craniofacial region, this region presents with cutaneous allodynia44. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
https://doi.org/10.1212/01.wnl.000031064...
,1717. Aguggia M. Allodynia and migraine. Neurol Sci. 2012;33(Suppl 1):S9-11. https://doi.org/10.1007/s10072-012-1034-9
https://doi.org/10.1007/s10072-012-1034-...
. Therefore, the more headache attacks the patient has, the greater will be the presence of cutaneous allodynia. Our results demonstrated that cutaneous allodynia seems to be more frequent in chronic migraine and is associated with the disease duration. However, our findings reinforce that, when considering the years with migraine, the increased association of the risk of chronic migraine resulting in cutaneous allodynia, compared to episodic migraine patients, is attenuated, as after adjustment no significant difference could be attributed to the prevalence ratio.
In both the episodic migraine and chronic migraine groups, cutaneous allodynia was most commonly classified as severe: 40% and 48.75% respectively. However, there were no differences in the proportion of severity between groups. These findings are not in accordance with those of Bigal et al.44. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
https://doi.org/10.1212/01.wnl.000031064...
due to the differences of the studied samples, but they corroborate those of Schwedt et al.1313. Schwedt TJ, Krauss MJ, Frey K, Gereau RW 4th. Episodic and chronic migraineurs are hypersensitive to thermal stimuli between migraine attacks. Cephalalgia. 2010;31(1):6-12. https://doi.org/10.1177/0333102410365108
https://doi.org/10.1177/0333102410365108...
, who also found no differences in the severity of cutaneous allodynia in chronic migraine and episodic migraine patients.
We can infer that the clinical manifestation of cutaneous allodynia between groups is similar, since both groups presented with a higher prevalence for a severe classification and similar distributions between the domains. However, these results do not allow us to say that one group is more sensitized than the other. Instead, we can suggest that individuals with episodic migraine, when cutaneous allodynia is present, exhibit similar clinical allodynia features in relation to chronic individuals, even though the attacks are more sporadic and a lower frequency of cutaneous allodynia is observed. These results do not refute Lipton et al.77. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
https://doi.org/10.1002/ana.21211...
, since our data demonstrated that individuals with episodic migraine exhibit as much allodynia as chronic migraineurs. Because of this, we should be aware of the risk of these individuals developing a chronic course. In this way, we assume that symptom severity is related to the disease itself and not directly related to the frequency of attacks, since chronic migraine patients presented with a longer period of disease than episodic migraine patients.
An association between the severity and the presence of disease was reinforced by the reduction of the prevalence ratio, which did not show any difference between the groups when adjusted for the duration of disease. Therefore, we concluded that the presence of migraine for long periods is possibly a more significant influencing factor than the monthly frequency of attacks. Our results corroborated those of other studies, showing that the younger patients manifest migraine, the more severe the cutaneous allodynia, due to the long period of central sensitization of nociceptive pathways1818. Güven H, Çilliler AE, Çomoğlu SS. Cutaneous allodynia in patients with episodic migraine. Neurol Sci. 2013;34(8):1397-402. https://doi.org/10.1007/s10072-012-1249-9
https://doi.org/10.1007/s10072-012-1249-...
,1919. Louter MA, Bosker JE, Oosterhout WP, Zwet EW, Zitman FG, Ferrari MD et al. Cutaneous allodynia as a predictor of migraine chronification. Brain. 2013;136(11):3489-96. https://doi.org/10.1093/brain/awt251
https://doi.org/10.1093/brain/awt251...
.
Regarding frequency of responses for each activity, the distribution of symptoms among domains in both episodic migraine and chronic migraine was balanced. The presence of cutaneous allodynia being associated with all types of stimuli described here coincided with isolated findings regarding thermal, mechanical static and mechanical dynamic domains2020. Kitaj MB, Klink M. Pain thresholds in daily transformed migraine versus episodic migraine headache patients. Headache. 2005;45(8):992-8. https://doi.org/10.1111/j.1526-4610.2005.05179.x
https://doi.org/10.1111/j.1526-4610.2005...
,2121. Cooke L, Eliasziw M, Becker WJ. Cutaneous allodynia in transformed migraine patients. Headache. 2007;47(4):531-9. https://doi.org/10.1111/j.1526-4610.2006.00717.x
https://doi.org/10.1111/j.1526-4610.2006...
. However, it does not allow us to state that both groups have similar sensitization severity. It only confirms that, when sensitized, they present with similar clinical manifestations. And this is considered the most relevant contribution to migraine knowledge in our study.
Knowing that episodic migraineurs are clinically similar to chronic migraineurs in cutaneous allodynia severity, we should propose strategies to prevent the chronicity of the disease. Therefore, the identification of cutaneous allodynia would help clinicians to offer proper treatment. We draw attention to the frequency of discomfort reported by wearing tight clothing in both groups, 42% in the episodic migraine group and 53.75% in the chronic migraine group. We propose that third-order thalamic neurons are sensitized, as clinical manifestations can be observed in extracephalic regions, suggesting a widespread allodynia2222. Burstein R, Jakubowski M, Garcia-Nicas E, Kainz V, Bajwa Z, Hargreaves R et al. Thalamic sensitization transforms localized pain into widespread allodynia. Ann Neurol. 2010;68(1):81-91. https://doi.org/10.1002/ana.21994
https://doi.org/10.1002/ana.21994...
.
Limitations of this study must be considered. Firstly, although male patients were not excluded, the proportion of them in the sample was very small. It might be a reflection of gender differences regarding the prevalence of migraine as well as differences in the demand for medical care. Therefore, the results described here might be more applied to females. Secondly, the study was performed in a tertiary care unit and results can only be generalized to migraine patients with similar characteristics, such as migraines over a long time and with worse severity. Thirdly, the fluctuation of the frequency of migraine attacks during the past years was not controlled and this can be seen as a limitation, as we could not affirm that episodic migraine patients had never been classified as chronic sufferers. However, the diagnostic criteria considered the frequency of attacks during the previous three months, and this possible limitation concurs with all studies that compare episodic and chronic migraine patients.
In conclusion, the frequency of cutaneous allodynia rises slightly in proportion with an increase in the number of attacks, but its presence and severity seems to be associated with the duration of the disease. Furthermore, no differences of distribution were observed among domains, and both groups were affected similarly in terms of cephalic and extracephalic regions.
Acknowledgments
Professor José Geraldo Speciali for the patient trial support.
References
-
1Robbins MS, Lipton RB. The epidemiology of primary headache disorders. Semin Neurol. 2010;30(2):107-19. https://doi.org/10.1055/s-0030-1249220
» https://doi.org/10.1055/s-0030-1249220 -
2Carod-Artal FJ, Irimia P, Ezpeleta D. [Chronic migraine: definition, epidemiology, risk factors and treatment]. Rev Neurol. 2012;54(10):629-37. Spanish.
-
3Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia. 2013;33(9):629-808. https://doi.org/10.1177/0333102413485658
» https://doi.org/10.1177/0333102413485658 -
4Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D et al. Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology. 2008;70(17):1525-33. https://doi.org/10.1212/01.wnl.0000310645.31020.b1
» https://doi.org/10.1212/01.wnl.0000310645.31020.b1 -
5Kalita J, Yadav RK, Misra UK. A comparison of migraine patients with and without allodynia symptoms. Clin J Pain. 2009;25(8):696-8. https://doi.org/10.1097/AJP.0b013e3181b12dd3
» https://doi.org/10.1097/AJP.0b013e3181b12dd3 -
6Tietjen GE, Brandes JL, Peterlin BL, Eloff A, Dafer RM, Stein MR et al. Allodynia in migraine: association with comorbid pain conditions. Headache. 2008;49(9):1333-44. https://doi.org/10.1111/j.1526-4610.2009.01521.x
» https://doi.org/10.1111/j.1526-4610.2009.01521.x -
7Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML et al. Cutaneous allodynia in the migraine population. Ann Neurol. 2008;63(2):148-58. https://doi.org/10.1002/ana.21211
» https://doi.org/10.1002/ana.21211 -
8Burstein R, Yarnitsky D, Goor-Aryeh I, Ransil BJ, Bajwa ZH. Bajwa. An association between migraine and cutaneous allodynia. Ann Neurol. 2000;47(5):614-24. https://doi.org/10.1002/1531-8249(200005)47:5<614::AID-ANA9>3.0.CO;2-N
» https://doi.org/10.1002/1531-8249(200005)47:5<614::AID-ANA9>3.0.CO;2-N -
9Jakubowski M, Silberstein S, Ashkenazi A, Burstein R. Can allodynic migraine patients be identified interictally using a questionnaire? Neurology. 2005;65(9):1419-22. https://doi.org/10.1212/01.wnl.0000183358.53939.38
» https://doi.org/10.1212/01.wnl.0000183358.53939.38 -
10Ashkenazi A, Silberstein S, Jakubowski M, Burstein R. Improved identification of allodynic migraine patients using a questionnaire. Cephalalgia. 2007;27(4):325-9. https://doi.org/10.1111/j.1468-2982.2007.01291.x
» https://doi.org/10.1111/j.1468-2982.2007.01291.x -
11Burstein R, Collins B, Jakubowski M. Defeating migraine pain with triptans: a race against the development of cutaneous allodynia. Ann Neurol. 2004;55(1):19-26. https://doi.org/10.1002/ana.10786
» https://doi.org/10.1002/ana.10786 -
12Misra UK, Kalita J, Bhoi SK. Allodynia in migraine: clinical observation and role of prophylactic therapy. Clin J Pain. 2013;29(7):577-82. https://doi.org/10.1097/AJP.0b013e31826b130f
» https://doi.org/10.1097/AJP.0b013e31826b130f -
13Schwedt TJ, Krauss MJ, Frey K, Gereau RW 4th. Episodic and chronic migraineurs are hypersensitive to thermal stimuli between migraine attacks. Cephalalgia. 2010;31(1):6-12. https://doi.org/10.1177/0333102410365108
» https://doi.org/10.1177/0333102410365108 -
14Olesen J, Bousser MG, Diener HC, Dodick D, First M, Goadsby PJ et al. New appendix criteria open for a broader concept of chronic migraine. Cephalalgia. 2006;26(6):742-6. https://doi.org/10.1111/j.1468-2982.2006.01172.x
» https://doi.org/10.1111/j.1468-2982.2006.01172.x -
15Florencio LL, Chaves TC, Branisso LB, Gonçalves MC, Dach F, Speciali JG et al. 12 item allodynia symptom cheklist/Brasil: cross-cultural adaptation, internal consistency and reproducibility. Arq Neuropsiquiatr. 2012;70(11):852-6. https://doi.org/10.1590/S0004-282X2012001100006
» https://doi.org/10.1590/S0004-282X2012001100006 -
16Koenker R, Hallock KF. Quantile regression. Cambridge: Cambridge University Press; 2005.
-
17Aguggia M. Allodynia and migraine. Neurol Sci. 2012;33(Suppl 1):S9-11. https://doi.org/10.1007/s10072-012-1034-9
» https://doi.org/10.1007/s10072-012-1034-9 -
18Güven H, Çilliler AE, Çomoğlu SS. Cutaneous allodynia in patients with episodic migraine. Neurol Sci. 2013;34(8):1397-402. https://doi.org/10.1007/s10072-012-1249-9
» https://doi.org/10.1007/s10072-012-1249-9 -
19Louter MA, Bosker JE, Oosterhout WP, Zwet EW, Zitman FG, Ferrari MD et al. Cutaneous allodynia as a predictor of migraine chronification. Brain. 2013;136(11):3489-96. https://doi.org/10.1093/brain/awt251
» https://doi.org/10.1093/brain/awt251 -
20Kitaj MB, Klink M. Pain thresholds in daily transformed migraine versus episodic migraine headache patients. Headache. 2005;45(8):992-8. https://doi.org/10.1111/j.1526-4610.2005.05179.x
» https://doi.org/10.1111/j.1526-4610.2005.05179.x -
21Cooke L, Eliasziw M, Becker WJ. Cutaneous allodynia in transformed migraine patients. Headache. 2007;47(4):531-9. https://doi.org/10.1111/j.1526-4610.2006.00717.x
» https://doi.org/10.1111/j.1526-4610.2006.00717.x -
22Burstein R, Jakubowski M, Garcia-Nicas E, Kainz V, Bajwa Z, Hargreaves R et al. Thalamic sensitization transforms localized pain into widespread allodynia. Ann Neurol. 2010;68(1):81-91. https://doi.org/10.1002/ana.21994
» https://doi.org/10.1002/ana.21994
-
Support: São Paulo Research Foundation (FAPESP).
Publication Dates
-
Publication in this collection
Mar 2017
History
-
Received
02 May 2016 -
Reviewed
29 Sept 2016 -
Accepted
21 Nov 2016