Abstracts
OBJECTIVES: To describe causes of death and factors involved in the decision-making process related to life support limitation at three university-affiliated pediatric intensive care units in the south of Brazil. METHODS: A retrospective study was conducted, based on a review of the medical records of all deaths occurring during 2002 at three pediatric intensive care units in Porto Alegre. Three previously trained pediatric fellows from each service performed the study. Data were assessed relating to general case characteristics, causes of death (failed cardiopulmonary resuscitation, brain death, do-not-resuscitate orders, withholding or withdrawing life-sustaining treatment - the last three modes were classified as the life support limitation group), length of stay in hospital, end-of-life plans and the participation of patients' families and Ethics Committees. The Student t test, Mann Whitney, chi-square, odds ratio and multivariate analyses were used for comparisons. RESULTS: Close to 53.3% of fatal cases had received full cardiopulmonary resuscitation. The incidence of life support limitation was 36%, with statistical differences (p = 0.014) between the three hospitals (25 versus 54.3 and 45.5%, respectively). The most frequent form of life support limitation was a do-not-resuscitate order (70%). Life support limitation was associated with the presence of chronic disease (odds ratio = 8.2; 95%CI 3.2-21.3) and length stay in the pediatric intensive care unit (odds ratio = 4.4; 95%CI 1.6-11.8). The rate of involvement of families and Ethics Committees in the decision-making process was lesser than 10%. CONCLUSIONS: Cardiopulmonary resuscitation is offered more frequently than is observed in northern countries. In contrast, life support limitation is offered through do-not-resuscitate orders. These findings and the low participation of the families in the decision-making process reflect the difficulties to be overcome by those professionals who are responsible for handling critically ill children in southern Brazil.
Death; ethics; pediatric intensive care; forgoing life support; do-not-resuscitate orders
OBJETIVO: Avaliar os modos de morte e fatores associados à limitação de suporte de vida em três unidades de terapia intensiva pediátrica do sul do Brasil. MÉTODO: Estudo transversal e retrospectivo em que foram revisados todos os óbitos ocorridos em 2002 em três unidades de terapia intensiva pediátrica de referência de Porto Alegre por uma equipe de pesquisadores treinados para esse fim. Foram avaliadas as características gerais, o modo de morte (ressuscitação cardiopulmonar, morte encefálica, ordem de não reanimar, não oferta e retirada de suporte vital - esses três últimos agrupados em limitação de suporte de vida), o tempo de internação - hospitalar e na unidade de terapia intensiva pediátrica -, o plano de final de vida e a participação da família nessa decisão. Para as comparações, foram utilizados o teste t de Student, Mann Whitney, qui-quadrado, odds ratio e análise multivariada. RESULTADOS: Aproximadamente 53,3% dos óbitos receberam ressuscitação cardiopulmonar. A incidência de limitação de suporte de vida foi de 36,1%, havendo diferença significativa (p = 0,014) entre os hospitais (25 versus 54,3 e 45,5%). A forma de limitação de suporte de vida mais freqüente foi "ordem de não reanimar" (70%). Observou-se associação entre limitação de suporte de vida com presença de doença crônica (odds ratio = 8,2; IC95% = 3,2-21,3) e tempo de internação na unidade de terapia intensiva pediátrica > 24h (odds ratio = 4,4; IC95% = 1,6-11,8). A participação da família e dos comitês de ética no plano de final de vida foi inferior a 10%. CONCLUSÕES: A ressuscitação cardiopulmonar ainda é oferecida em uma freqüência maior do que a descrita nos países do hemisfério norte, enquanto que a limitação de suporte vital é realizada preferentemente através da ordem de não reanimar. Esses achados e a pequena participação da família refletem dificuldades em relação às decisões de final de vida enfrentadas por intensivistas do sul do Brasil.
Morte; bioética; tratamento intensivo pediátrico; reanimação cardiopulmonar; limitação de suporte de vida
ORIGINAL ARTICLES
Life support limitation at three pediatric intensive care units in southern Brazil
Patrícia M. LagoI; Jefferson PivaII; Délio KipperIII; Pedro Celiny GarciaIII; Cristiane PrettoIV; Mateus GiongoIV; Ricardo BrancoIV; Fernanda BuenoV; Cristiane TraiberV; Taisa AraújoV; Daniela WortmannVI; Graziela LibrelatoVI; Deise SoardiVI
IMSc. Pediatrician, Pediatric Intensive Care Unit (ICU), Hospital de Clínicas de Porto Alegre (HCPA), Porto Alegre, RS, Brazil
IIProfessor, Department of Pediatrics, School of Medicine, Pontifícia Universidade Católica do Rio Grande do Sul (PUCRS) and Universidade Federal do Rio Grande do Sul (UFRGS). Chief of the pediatric ICU, Hospital São Lucas, PUCRS, Porto Alegre, RS, Brazil
IIIProfessor, Department of Pediatrics, School of Medicine, PUCRS. Chief of the pediatric ICU, Hospital São Lucas (HSL-PUCRS), Porto Alegre, RS, Brazil
IVResident, Pediatric ICU, HSL-PUCRS, Porto Alegre, RS, Brazil
VResident, Pediatric ICU, HCPA, Porto Alegre, RS, Brazil
VIResident, Pediatric ICU, Hospital da Criança Santo Antônio, Porto Alegre, RS, Brazil
Correspondence Correspondence to Patrícia M. Lago Rua Furriel Luis Vargas, 238/201 CEP 90470-130 Porto Alegre, RS, Brazil Tel.: (51) 3335.3098 E-mail: lagopatricia@terra.com.br
ABSTRACT
OBJECTIVES: To describe causes of death and factors involved in the decision-making process related to life support limitation at three university-affiliated pediatric intensive care units in the south of Brazil.
METHODS: A retrospective study was conducted, based on a review of the medical records of all deaths occurring during 2002 at three pediatric intensive care units in Porto Alegre. Three previously trained pediatric fellows from each service performed the study. Data were assessed relating to general case characteristics, causes of death (failed cardiopulmonary resuscitation, brain death, do-not-resuscitate orders, withholding or withdrawing life-sustaining treatment - the last three modes were classified as the life support limitation group), length of stay in hospital, end-of-life plans and the participation of patients' families and Ethics Committees. The Student t test, Mann Whitney, chi-square, odds ratio and multivariate analyses were used for comparisons.
RESULTS: Close to 53.3% of fatal cases had received full cardiopulmonary resuscitation. The incidence of life support limitation was 36%, with statistical differences (p = 0.014) between the three hospitals (25 versus 54.3 and 45.5%, respectively). The most frequent form of life support limitation was a do-not-resuscitate order (70%). Life support limitation was associated with the presence of chronic disease (odds ratio = 8.2; 95%CI 3.2-21.3) and length stay in the pediatric intensive care unit (odds ratio = 4.4; 95%CI 1.6-11.8). The rate of involvement of families and Ethics Committees in the decision-making process was lesser than 10%.
CONCLUSIONS: Cardiopulmonary resuscitation is offered more frequently than is observed in northern countries. In contrast, life support limitation is offered through do-not-resuscitate orders. These findings and the low participation of the families in the decision-making process reflect the difficulties to be overcome by those professionals who are responsible for handling critically ill children in southern Brazil.
Key words: Death, ethics, pediatric intensive care, forgoing life support, do-not-resuscitate orders.
Introduction
In the last few decades, technological improvement and sophistication of intensive care on a worldwide basis have allowed for the increased survival of a large number of patients with incurable diseases and with a poor prognosis. However, prolongation of life is often attained at the cost of patients' and family's suffering. The end of life of ICU patients is no longer an intimate moment shared only among family and friends; it has become a solitary moment surrounded by technology and, not uncommonly, pain.1
Several studies have been published, especially in the USA, since 1990, that question the principle of "life at any cost."2,3 End-of-life decisions are now widely discussed, placing a high value on the respect for the patient, including a growing concern with maintaining dignity at the end of life and humanization of death.4 Concomitantly, the concept of life support limitation (LSL), which includes do-not-resuscitate orders, and withholding and withdrawal of life support, has appeared in medical practice to avoid the use of treatments that only prolong life but do not improve patient outcome, usually leading to useless treatments and needless suffering.5
Currently, 90% of deaths occurring at adult ICUs in North America are preceded by some type of limitation of supportive care.6 Studies about modes of death at pediatric intensive care units (PICU), conducted in Europe and in the United States, showed an LSL incidence of 30 to 60%.7-11
In Latin American countries, which use the principles of paternalistic medicine, too little research is carried out into end-of-life decisions, especially regarding pediatric patients. The death of an infant or child always involves a lot of grief. Discussion about LSL under these circumstances often is extremely painful, and for that reason, it is usually avoided. The first studies about modes of death at PICUs were published in 1993 by Vernon. In the last decade, however, little has been known about LSL practices in Brazil.5,12 There are only two extensive studies about this topic in Latin America: one in Argentina, published in 2003 by Althabe et al., and another one in Brazil, by Kipper et al. in 1999/2000.13,14
The present study was carried out to assess the modes of death at three PICUs in southern Brazil in 2002, describing the incidence of LSL and related factors.
Method
A cross-sectional, observational and retrospective study was conducted, including all infants/children who died at three referral PICUs, located in southern Brazil, in 2002. This study was a continuation of another study undertaken by the same authors, using the same methodology.14 The present study was approved by the local Research and Ethics Committees of the three hospitals involved. The research was conducted in three tertiary referral teaching hospitals of Porto Alegre: PICU of Hospital São Lucas (affiliated with PUCRS), PICU of Hospital de Clínicas de Porto Alegre (HCPA) and PICU of Hospital da Criança Santo Antônio da Irmandade Santa Casa de Misericórdia de Porto Alegre (ISCMPA). The three PICUs were similar, with medical staffs comprised of professors of pediatrics, assistant physicians and second-year and third-year resident doctors. During duty periods, the patients were seen by two assistant physicians and two resident doctors. The actions regarding each patient were planned in daily meetings with the entire staff (morning and evening rounds).
All patients who had died at these three PICUs between January 1st and December 31st, 2002, were included in the study. The identification of patients and of their medical records were made by the analysis of admission to and discharge from each PICU. Three resident doctors from each PICU were selected for the data analysis, who independently collected the information from the medical charts. None of them had attended to the patients in the previous year. All the physicians who helped with the research received a previous training before the data collection, in which they had to read classic articles on "modes of death in the ICU," followed by simulate cases for the classification of the modes of death and a theoretical lesson on the subject.5,15 Two sessions were necessary so that the reliability of the data, assessed by kappa statistics, reached 0.9. Data collection only started after this value was reached. The data were stored in a spreadsheet specifically developed for this purpose (when no agreement was reached which occurred in only 10% of medical charts , researchers gathered together until they reached an agreement).
The medical charts were revised considering the following aspects: a) patient characteristics; b) length of hospital and PICU stay; c) mode of death; d) existence of cardiopulmonary resuscitation (CPR) simulation; e) and existence of well-documented planned actions; f) participation of parents; g) participation of the ethics committee.
Modes of death were defined as failure in cardiopulmonary resuscitation (CPR) maneuvers, brain death, do-not-resuscitate orders, and withholding and withdrawal of life support. The latter three were classified as LSL.
Based on the records of each PICU in the last few years, it was estimated that each unit in the year 2002 had had around 500 admissions, with a mortality rate of approximately 10% (or 50 deaths per PICU), so the study population ranged between 140 and 160 deaths. The continuous variables were expressed as means and standard deviations (SD), whereas those variables without a normal distribution were expressed as median and interquartile range (IQR25-75%). T tests and ANOVA were used for the comparison of continuous variables with a normal distribution, and the Kruskal-Wallis and Mann-Whitney tests were used for the variables without a normal distribution (e.g.: length of stay in the ICU, patient age, length of hospital stay). Categorical variables were expressed as percentage values (e.g.: frequency of LSL, frequency of deaths across hospitals) and were compared using the chi-square test. Association tests were also performed for some variables that could influence the LSL decisions (e.g.: age, presence of chronic disease or length of hospital stay). Those variables that were significant in the bivariate analysis were analyzed together using a multivariate analysis (odds ratio). The statistical analysis was made using the SPSS 10.0 program.
Results
In 2002, 1,633 patients were admitted to the three PICUs, among whom 155 died, resulting in a mortality rate of 9.4%. Of the 155 deaths, only 150 medical charts could be revised (49/hospital I, 42/hospital II, 59/hospital III), since five medical charts (3.2%) had been lost and could not be retrieved until the end of the data collection period.
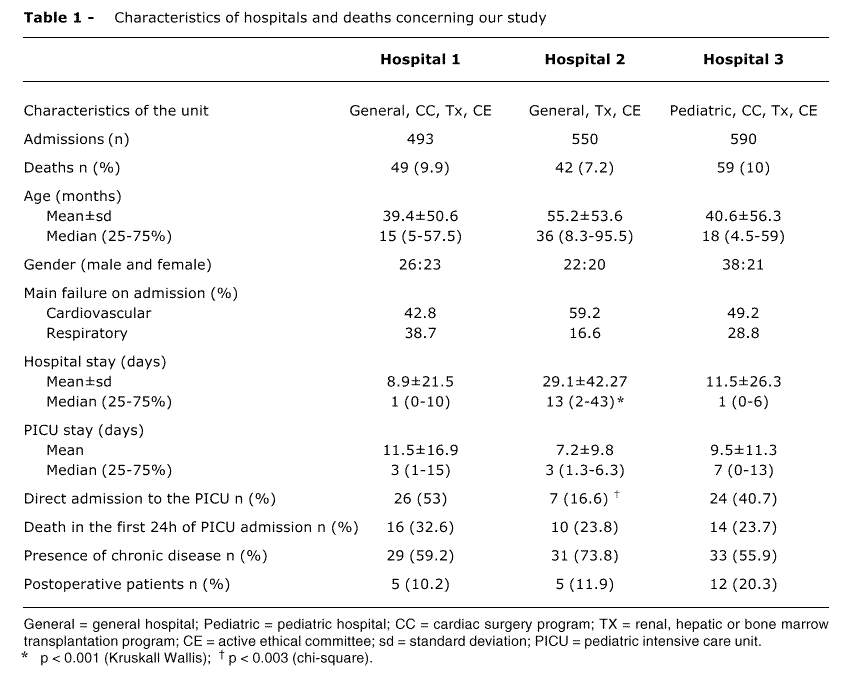
In this sample, no sex predominance or significant differences were observed across hospitals. The mean age ranged from 39 to 55 months in all hospitals (medians of 15; 36 and 18 months) with no statistically significant difference (Table 1). No significant difference was noted between the number of deaths that had occurred on the day shift during the week (41.3%) and those that had occurred on the night shift on weekends and holidays (58.7%).
The median length of hospital stay prior to admission to the PICU was significantly higher (p < 0.001, Kruskal-Wallis) at hospital II (13 days) compared to hospital I (0 days) and III (1 day). The overall incidence of admissions from the emergency room of the hospital or referred from other emergency services (direct admissions to the PICU) was 38.3%. In this regard, hospital II showed a significantly lower incidence (p = 0.003) of direct admissions to the PICU than hospitals I and III (16.6 against 53 and 40.7%, respectively).The median length of stay in the PICU was similar in all hospitals (Table 1). In 40 patients (26.6%), death occurred in the first 24 hours of admission to the PICU, and no difference was observed across hospitals (p = 0.55).
More than 50% of the deaths were of infants with chronic diseases (62%), with no difference across hospitals. The chronic diseases were classified as congenital heart diseases (12), solid or nonsolid tumors (31), bronchopulmonary dysplasia (seven), chronic encephalopathies (20), multiple malformations (10), neuromuscular disease (two), acquired immunological diseases or not (nine) and liver diseases (two).
The most prevalent organ failures during hospital stay were cardiovascular ones (45.2%) followed by respiratory ones (36.6%). It should be underscored that ten deaths (6.6%) occurred in patients who had been admitted only for observation.
In 53.3% (80/150) of the cases, full resuscitation procedures were carried out. Brain death occurred in 16 cases (10.6%), whereas the remaining 54 deaths (36.1%) occurred after some kind of LSL, which involved do-not-resuscitate orders, and withholding and withdrawal of life support (Table 2). The most frequent type of LSL was do-not-resuscitate order, which occurred in 70.3% (38/54) of LSL cases. Only five cases of life support withdrawal were observed. In four of them, the administration of inotropic agents was discontinued, whereas mechanical ventilation was interrupted in one case.
The cases of brain death were excluded from the study in order to determine and compare the incidence of LSL and CPR at the PICUs with increased accuracy. LSL at hospital I (25%) was significantly lower (p = 0.014) than at hospitals II (54.3%) and III (45%). Thus, it was possible to estimate that, at hospital I, the occurrence of death followed by resuscitation has a relative risk of 1.45 (95%CI = 1.1-1.9) compared to the other two hospitals (Figure 1 and Table 2).
The bivariate analysis showed that some factors were associated with LSL, such as: length of hospital stay longer than three days (prior to admission to the PICU) with an odds ratio of 2.9 (95%CI = 1.3-6.5); length of stay at the PICU longer than or equal to 24 hours with an odds ratio of 4 (95%CI = 1.5-11.2) and presence of chronic disease with an odds ratio of 4.8 (95%CI = 1.8-13.3) (Table 3). However, when these factors were submitted to a multivariate analysis, only the length of stay at the ICU longer than or equal to 24 hours (odds ratio = 4.4; 95%CI = 1.6-11.8) and the presence of chronic disease (odds ratio = 8.2; 95%CI = 3.2-21.3) showed statistical significance.
Of the 54 patients who died after LSL, the medical charts of only 38 (70%) contained a planned sequence of events. The mean time between the planned action and death was two days. The diagnosis and prognosis of the disease influenced the LSL decision (92.1%). The participation of the patient's family in the LSL decision was described in only five cases (9.2%), and ethics committees participated in end-of-life decisions in only five cases (9.2%). The families of patients with LSL were present at the time of death in eight cases (14.8%). By comparing the data on medical orders with the data recorded by the nursing staff, we observed that two cases suggested CPR simulation.
Discussion
Several studies have been published in the international literature since the 1990s, revealing an increase in LSL prior to the patients' death, both at the adult and pediatric ICUs . Depending on the country of origin, on the type of ICU and on patient age, the incidence of deaths that followed LSL decisions has ranged between 30 and 90%.6-11 In this study, similar rates were found in three PICUs in southern Brazil.
There was a significant increase in LSL in the three hospitals analyzed compared to a similar study conducted by Kipper et al. at the same institutions in 1988, 1998 and 2000.14 In this 14-year period (including the data of the 2002 study), there occurred an increase in LSL from 6 to 36% of PICU deaths in this region . However, it should be highlighted that CPR is still performed in a large number of patients before death. These studies showed that there are different responses related to the increase in LSL and to the reduction of CPR at the three hospitals, with an extremely higher frequency of do-not-resuscitate orders compared to the withholding or withdrawal of life support. The LSL cases in this study were associated with a longer stay at the PICU and with the presence of chronic disease. Moreover, the participation of family members in end-of-life decisions and at the time of death (quality of death) is still much lower than expected and than that which is observed in northern hemisphere countries.
By comparing the data obtained from studies on modes of death conducted at U.S. and Canadian hospitals, it is observed that the incidence of CPR prior to the death of patients at the three analyzed PICUs (53%) was extremely high.6,10,15 One should recall that CPR is indicated in cases of unexpected cardiorespiratory arrest. A large number of infants who die at PICUs every day have chronic diseases and stand no chance to have their disease controlled. In this case, cardiorespiratory arrest would not be an unexpected event, but a natural and expected outcome.16 These discrepant results in studies about modes of death at the ICU in certain countries may be explained by the different populations analyzed, as well as by cultural, ethical and religious aspects concerning the medical staff, patients and their families.17-19
The increase in LSL in the last 14 years (1988 = 6% to 2002 = 36%) indicates a change in the behavior of the medical community in our setting towards end-of-life decisions. Nowadays, there seems to be a growing concern with the quality of care patients receive, also at their time of death, and the principle of "life at any cost" has been criticized.20 The disproportionate increase in LSL at the three PICUs analyzed may be ascribed to the difference among the patients of each unit (larger or smaller number of "acute" versus "chronic" cases), the specific characteristics of each hospital (details of the organizational system of each PICU) that were not properly evaluated in this study or that were not associated with the moral, cultural, ethical and scientific values of each member of the medical staff in this study.
The do-not-resuscitate order (DNR) is regarded by most authors as an intermediate option between total investment in the patient and the withdrawal of life support. Similarly to other studies, in our setting, the do-not-resuscitate (DNR) order was the most frequently used form of LSL.13,14 The predominance of this do-not-resuscitate order prior to death suggests the difficulty the medical staff has taking on a more active attitude towards LSL. Nevertheless, it should be emphasized that from the ethical and moral point of view, there is no difference in the forms of LSL. The ethics committee of the Society of Critical Care Medicine does not show preference for a form of LSL over the others, but states that the medical staff should always prioritize patient's comfort.19,21
With the improvement in primary care, prevention of contagious infections and progress in public health care, the number of patients admitted to the PICU due to acute diseases remarkably decreased in the last decade. As a consequence, most infants/children who die at these facilities have chronic diseases, as demonstrated in this study (62%). The presence of chronic diseases was significantly associated with LSL decisions, quite probably because these infants have a sufficiently well-known disease, with a poor prognosis, and prolonging their lives would sometimes result in useless treatments and unnecessary suffering.4,6
On the other hand, the deaths that occurred in the first 24 hours of admission had received CPR more frequently, presumably because those were patients who had been admitted to the units without any established diagnosis, which resulted in high hopes for reversibility and had a yet unknown prognosis.6
Of the revised medical charts that included death after LSL, 30% did not contain the description or filing of a planned sequence of events. We take for granted that there may have been a discussion about this issue, but that the failure to file information into the medical charts probably occurred due to the fear of legal prosecution or due to the difficulty the medical staff had in assuming end-of-life decisions.22 The often unfounded fear of legal actions may influence LSL decisions. Most countries accept to discontinue or not to initiate useless treatments, but some physicians have difficulty adopting these practices.23 The fear of legal prosecution is unfounded because LSL decisions are made to the patients' benefit and, therefore, they are totally acceptable from an ethical point of view.22,24
Curiously enough, the participation of family in end-of-life decisions (9.2%) is lower than that reported in other countries, where it amounts to 100%, in some cases.21,25,26 There may be several causes for this limited participation: the well-established paternalistic medicine attitude in Brazil, the disorganization of the Brazilian health system, cultural aspects of the population, lack of tradition in the defense of patients' interests, among others. It is common knowledge, however, that most Brazilian physicians find it difficult to deal with end-of-life issues. This presumably occurs due to their poor academic background, to scarce publications on the topic and also to the paternalistic medicine in southern hemisphere countries,27,28 where decisions are taken in a unilateral fashion with the passive participation of family, which do not exercise their right to decide and, often disrespecting the patient autonomy. It is a common agreement that the family is the best representative of pediatric patients' rights and should therefore be invited to participate in LSL decisions.27 However, as verified in this study, the participation of family in these and in other decisions has been poorly encouraged and accepted (or respected) in our setting. Conversely, in northern hemisphere countries, promoting a "good death" is a priority, and the presence of family at the time of death is quite common.4,29,30 In this regard, Brazilian and South American pediatric intensive care should be improved and modified in the short run, so as to make end-of-life decisions a priority in medical education in our setting.30,31
This study, just like most retrospective studies on death, has some limitations. The investigation of death and of end-of-life decisions is always complicated due to several factors, such as lack of consistent definitions, use of tools that have not been validated, assessment of incomplete data and frequent lack of objective descriptions on the medical charts. This may lead to conclusions that are sometimes inaccurate and to the underassessment of the actual incidence of LSL. In addition, the training of researchers based on simulate medical cases and theoretical lessons, albeit rigid (three researchers at each unit), may have an interpretation bias produced by the training physician. Even so, after considering these possible biases in the adopted method, the data in this study are consistent, show internal and external coherence, and are similar to data from studies carried out in other countries, such as Argentina13, France8 and Italy.10
This study might represent the reality in just one Brazilian region and, therefore, other studies are necessary to assess end-of-life situations at the PICUs all over the country. The use of well-defined end-of-life protocols validated by other pediatric intensive care units may be useful to clearly determine what has been done about the infants/children who die at Brazilian PICUs.
References
Manuscript received Jul 21 2004, accepted for publication Dec 22 2004
- 1. Carlet J, Lambertus T, Antonelli M. Challenges in end-of-life care ICU. Statement of 5th International Consensus Conference in Critical Care: Brussels (Belgium, April 2003). Intensive Care Med. 2004;30:770-84.
- 2. Prendergast TJ, Claessens MT, Luce JM. A national survey of end-of-life care for critically ill patients. Am J Resp Crit Care Med. 1998;158:1163-7.
- 3. Prendergast TJ, Luce JM. Increasing incidence of withholding and withdrawal of life support from the critically ill. Am J Resp Crit Care. 1997;155:15-20.
- 4. Garros D. Uma boa morte em UTI pediátrica: isso é possível? J Pediatr (Rio J). 2003;79 Supl 2:S243-54.
- 5. Vernon DD, Dean M, Timmons OD, Banner W, Allen-Web EM. Modes of death in the pediatric intensive care unit: withdrawal and limitation of supportive care. Crit Care Med. 1993;21:1978-92.
- 6. Garros D, Rosuchuk R, Cox P. Circumstances surrounding end of life in a pediatric intensive care unit. Pediatrics. 2003;112:371-9.
- 7. Deliens L, Mortier F, Cosyns M. End-of-life decisions in medical practice in Flanders, Belgium: a nationwide survey. Lancet. 2000;356:1806-11.
- 8. Ferrand E, Robert R, Ingrand P. Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. Lancet. 2001;357:9-14.
- 9. Haverkate I, van Delden J, van Nijen A. Guidelines for the use of do not resuscitate orders in Dutch hospitals. Crit Care Med. 2000;28:3039-43.
- 10. Heide A, Deliens L, Nilstun T. End-of-life decision in six European countries: descriptive study. Lancet. 2003,362:345-50.
- 11. Devictor D, Nguyen D. Forgoing life-sustaining treatments in children: a comparison between northern and southern European pediatric intensive care units. Pediatr Crit Care Med. 2004;5:211-5.
- 12. Carvalho P, Rocha T, Lago P. Modos de morrer na UTI pediátrica de um hospital terciário. Rev Ass Med Bras. 2001;47:325-31.
- 13. Althabe M, Cardigni G, Vassallo J, Allende D, Berrueta M. Dying in the intensive care unit: Collaborative multicenter study about forgoing life-sustaining treatment in Argentine pediatric intensive care units. Pediatr Crit Care Med. 2003;4:164-9.
- 14. Kipper D, Piva J, Garcia PC, Einloft P, Bruno F, Lago P, et al. Evolution of the medical practices and modes of death on pediatric intensive care units (picus) in southern Brazil. Pediatr Crit Care Med. 2004; no prelo.
- 15. Keenan HT, Diekema DS, O'Rourke PP, Cumminngs P, Woodrum DE. Attitudes toward limitation of support in the pediatric intensive care unit. Crit Care Med. 2000;8:1590-4.
- 16. Tomlinson T, Brody H. Ethics and communications in do not-resuscitate orders. N Engl J Med. 1998;318:43-5.
- 17. Levin PD, Sprung CL. Cultural differences at the end of life. Crit Care Med. 2003;31 Suppl:S354-7.
- 18. Stevens L, Cook D, Guyatt G. Education, ethics, and end-of-life decisions in the intensive care unit. Crit Care Med. 2002;30:290-6.
- 19. Truog RD, Cist AF, Brackett SE, Burns JP. Recommendations for end-of-life care in the intensive care unit: The Ethics Committee of the Society of Critical Care Medicine. Crit Care Med. 2001;29:2332-48.
- 20. Burns J, Mitchel C, Outwater J. End-of-life care in pediatric care unit after the forgoing of life-sustaining treatment. Crit Care Med. 2000;28:3060-6.
- 21. Zawistowski C, DeVita M. A descriptive study of children dying in the pediatric intensive care unit after withdrawal of life sustaining treatment. Pediatr Crit Care Med. 2004;5:216-22.
- 22. Kipper D, Martin L, Fabro L. Decisões médicas envolvendo o fim da vida o desafio de adequar as leis as exigências éticas. J Pediatr (Rio J). 2000;76:403-6.
- 23. Devictor D, Nguyen D. Forgoing life-sustaining treatments: how the decision is made in French Pediatric Intensive Care Units. Crit Care Med. 2001;297:1356-9.
- 24. Torreão LA, Reis AG, Troster EJ. Ressuscitação cardiopulmonar: discrepância entre o procedimento de ressuscitação e o registro no prontuário. J Pediatr (Rio J). 2000;76:429-33.
- 25. Meert K, Thurston MA, Sarnik A. End-of-life decision-making and satisfaction care: parental perspectives. Pediatr Crit Care Med. 2000;1:179-85.
- 26. Meyer E, Burns J, Griffith J. Parental perspective on end-of-life care in the pediatric intensive care unit. Crit Care Med. 2002;30:226-31.
- 27. Roig CG. Art of communication. Pediatr Crit Care Med. 2003;4:259-60.
- 28. Frader JE. Global paternalism in pediatric intensive care unit end-of-life decision. Pediatr Crit Care Med. 2003;4:257-8.
- 29. Levy M. End-of-life care in intensive care unit: can we do better? Crit Care Med. 2001;29 Suppl:N56-61.
- 30. Sahler OJ, Frager G, Leventown M. Medical education about end of life care in pediatric setting. Principles, challenges, and opportunities. Pediatrics. 2000;105:575-84.
- 31. Kipper DJ, Loch JA, Piva JP, Garcia PCR, Pithan LH, Zanini RD. Dilemas éticos, morais e legais em UTIP. In: Piva JP, Garcia PC, editores. Piva & Celiny - Medicina Intensiva em Pediatria. Rio de Janeiro: Revinter; 2005. p. 753-71.
Correspondence to
Publication Dates
-
Publication in this collection
30 July 2005 -
Date of issue
Apr 2005
History
-
Accepted
22 Dec 2004 -
Received
21 July 2004