Abstracts
OBJECTIVE: To determine the prevalence of exclusive breastfeeding during the first 3 months of life and its determinant factors in a city in the South region of Brazil. METHODS: Prospective study of a cohort of babies born between September 2002 and May 2003 in the city of Pelotas, RS. Data were obtained in interviews, at maternity units and during home visits, with mothers of babies aged between 1 and 3 months. Factors related to the cessation of breastfeeding were subjected to univariate, bivariate and multivariate analysis. RESULTS: Nine hundred and forty mothers of children aged 3 months or less were interviewed, 39% of whom were still exclusively breastfeeding and around 1/3 of whom no longer breastfed. Multivariate analysis by logistic regression demonstrated a significant association between interruption of exclusive breastfeeding before 3 months and maternal employment, use of a pacifier, low family income (between one and three times the minimum wage), and less than 5 years' paternal education. CONCLUSIONS: Exclusive breastfeeding throughout the first 3 months of life is an uncommon practice among the population of Pelotas, RS, in particular when the mother works away from home, the father has little education and the child is given a pacifier, which reinforces the need to continue stimulating exclusive breastfeeding during the first months of life.
Breastfeeding; lactation; infant nutrition
OBJETIVO: Determinar a prevalência do aleitamento materno exclusivo nos 3 primeiros meses de vida e os fatores determinantes em uma cidade da Região Sul do Brasil. MÉTODOS: Estudo de coorte prospectivo, envolvendo bebês nascidos entre setembro de 2002 e maio de 2003 na cidade de Pelotas (RS). Os dados foram obtidos através de entrevistas, nas maternidades e no domicílio, com mães de bebês entre 1 e 3 meses de idade. Para análise dos fatores relacionados à interrupção do aleitamento materno, foram realizadas análises univariada, bivariada e multivariada. RESULTADOS: Foram entrevistadas 940 mães de bebês com até 3 meses de idade, sendo que 39% destes recebiam aleitamento exclusivo e cerca de 1/3 já não mamava mais. Após análise multivariada por regressão logística, trabalho materno, uso de chupeta, renda familiar entre um e três salários mínimos e escolaridade paterna menor que 5 anos mostraram associação significativa com interrupção do aleitamento exclusivo antes dos 3 meses de vida. CONCLUSÕES: O aleitamento materno exclusivo nos primeiros 3 meses é pouco praticado na população de Pelotas (RS), em especial quando a mãe trabalha fora do lar, o pai tem pouca escolaridade e a criança faz uso de chupeta, o que reforça a necessidade de se continuar estimulando a amamentação exclusiva nos primeiros meses de vida.
Aleitamento materno; lactação; alimentação infantil
ORIGINAL ARTICLE
Prevalence of exclusive breastfeeding and its determiners in the first 3 months of life in the South of Brazil
Maria Laura W. MascarenhasI; Elaine P. AlbernazII; Mirian B. da SilvaIII; Regina B. da SilveiraIV
IMestre em Saúde e Comportamento, Universidade Católica de Pelotas (UCPEL), Pelotas, RS. Professora assistente, Núcleo de Pediatria, UCPEL, Pelotas, RS, Brasil
IIDoutora em Epidemiologia, Universidade Federal de Pelotas (UFPEL), Pelotas, RS. Professora adjunta, Programa de Pós-Graduação em Saúde e Comportamento, UCPEL, Pelotas, RS, Brasil
IIIMestre em Saúde e Comportamento, UCPEL, Pelotas, RS. Professora assistente, Núcleo de Pediatria, UCPEL, Pelotas, RS, Brasil
IVMestre em Saúde e Comportamento, UCPEL, Pelotas, RS. Professora assistente, Núcleo de Pediatria, UCPEL, Pelotas, RS, Brasil
Correspondence Correspondence: Maria Laura Wrege Mascarenhas Rua Canoas, 553, Laranjal CEP 96090-130 - Pelotas, RS - Brazil Tel.: +55 (53) 3226.3822 E-mail: malaura.m@terra.com.br
ABSTRACT
OBJECTIVE: To determine the prevalence of exclusive breastfeeding during the first 3 months of life and its determinant factors in a city in the South region of Brazil.
METHODS: Prospective study of a cohort of babies born between September 2002 and May 2003 in the city of Pelotas, RS. Data were obtained in interviews, at maternity units and during home visits, with mothers of babies aged between 1 and 3 months. Factors related to the cessation of breastfeeding were subjected to univariate, bivariate and multivariate analysis.
RESULTS: Nine hundred and forty mothers of children aged 3 months or less were interviewed, 39% of whom were still exclusively breastfeeding and around 1/3 of whom no longer breastfed. Multivariate analysis by logistic regression demonstrated a significant association between interruption of exclusive breastfeeding before 3 months and maternal employment, use of a pacifier, low family income (between one and three times the minimum wage), and less than 5 years' paternal education.
CONCLUSIONS: Exclusive breastfeeding throughout the first 3 months of life is an uncommon practice among the population of Pelotas, RS, in particular when the mother works away from home, the father has little education and the child is given a pacifier, which reinforces the need to continue stimulating exclusive breastfeeding during the first months of life.
Keywords: Breastfeeding, lactation, infant nutrition.
Introduction
There is no doubt that the ideal food for children during the first months of their lives is breastmilk. The advantages have been very well documented in the global literature.1-3 Based on scientific evidence, the World Health Organization (WHO) recommends the practice of exclusive breastfeeding for 6 months, in addition to its continuation with the addition of supplementary foods until 2 years or more.4
Studies have demonstrated that children exclusively fed at the breast are less susceptible to diseases such as diarrhea5 and dehydration.6 There is evidence that breastfeeding during the first months of life reduces the risk of hospital admissions due to pneumonia.7 Further advantages include gains in cognitive faculties8 and protection against atopic disease.9
A study published in 1998 provides exclusive breastfeeding rates for two cohorts from the city of Pelotas.10 In 1993, at 3 months of age, 13% of babies were exclusively breastfed and 39% had already been weaned. In 1998, at the same age, around 57% of babies were exclusively breastfed and 11% had already been weaned. The second cohort, however, comprised children with no growth restriction (full term, non-smoking mothers, good socioeconomic status and free from perinatal morbidity) and whose mothers had received additional support to maintain exclusive breastfeeding.
An intervention study undertaken in the same city in 2000 found that, at 4 months of age, 29% of babies were exclusively breastfed and 31% had been weaned. This study also employed a sample that was not representative of the general population (babies with growth restriction and mothers who also received additional breastfeeding support).11
Some studies12-14 indicate factors that are positively associated with exclusive breastfeeding, such as higher maternal educational level, stable marital relationship, infants born with gestational ages greater than 37 weeks, mothers with previous experience of breastfeeding and women who live in their own houses. Another study15 demonstrates that cessation of exclusive breastfeeding during the first months is associated with low family income, low maternal age, primiparity and mothers returning to work.
It was observed that these studies demonstrate that the practice of breastfeeding in different locations is heterogeneous, including in different regions within Brazil. This in turn led to the belief that diagnosing of the local state of breastfeeding is of fundamental importance to the planning of policies to encourage breastfeeding.
The objective of this study was to evaluate the prevalence of exclusive breastfeeding during the first 3 months of life of babies in the city of Pelotas and to identify factors that interfere with the practice.
Methods
This was a prospective cohort study investigating several different outcomes. The research project was structured in two phases: perinatal (hospital screening) and follow-up (home visits when babies were 1, 3 and 6 months of age). The perinatal phase consisted of interviews with all mothers whose children were born in the maternity units in the city of Pelotas, between September 2002 and May 2003, with an estimated frequency of 400 births/month. Follow-up visits were carried out between September 2002 and November 2003. The sample chosen for follow-up, approximately 30% of all mothers interviewed at maternity units, was selected by means of a randomized list produced by the Statistical Package for the Social Sciences (SPSS) software program. This study utilized information from the perinatal phase and from the follow-up home visits at 90 days.
All infants born to mothers resident in the city of Pelotas were eligible for the study as long as they were free from contraindications against breastfeeding (e.g. newborn infants with severe malformations or mothers seropositive for HIV). All mothers were duly informed about the research and signed a consent form. Mothers and their babies that were not located for application of the questionnaires, or who refused to participate or continue in the study, were considered losses.
The sample size was calculated based on a confidence interval of 95% (95%CI) and statistical power of 90% for exposure variables, varying from 15 to 80%, with an estimated relative risk (RR) of 2.0. A further 15% was added to account for possible losses and to control for potential confounding factors, which resulted in a sample of 600 mothers and their babies. Since this study was part of a larger research project investigating several different outcomes, the actual sample comprised 973 mothers and their babies. Both at the maternity units and during follow-up, standardized questionnaires were applied by previously trained medical students. The veracity of information provided in response to the questionnaires was checked by means of the application of a synthesized questionnaire to 10% of the sample, selected at random.
The breastfeeding classification categories used in this study are those laid out by the WHO/Pan American Health Organization (WHO/PAHO, 1991),16 i.e.: exclusive breastfeeding is defined as when children are given just breastmilk; breastfeeding predominant as when children are given breastmilk and water, teas or juices; and breastfeeding as when children are given any daily quantity of breastmilk, irrespective of whether or not they are being given other foods. Partial breastfeeding was defined as when children were being given breastmilk plus some other type of milk and children were defined as having been weaned if breastfeeding ceased during the follow-up period.
Epi-Info 6.0 and SPSS for Windows 8.0 were used for data analysis, adhering to the hierarchical model created previously, with variables related to demographic (baby's sex and color and maternal age) and socioeconomic factors (family income and parents' education) on the first level, maternal characteristics (parity, smoking, type of delivery, number of prenatal consultations and maternal employment, defined as whether or not mothers were employed during the month of the visit) on the second level, and, on the third level the babies' characteristics (gestational age, birth weight and pacifier use, defined as whether or not babies were being given pacifiers during the month of the visit). The frequencies of variables were calculated and bivariate analysis were performed between individual exposure factors and the outcome, between exposure factors and other variables and between the outcome and other variables. For all analyses, the cutoff for statistical significance was set at p < 0.05. For the multivariate analysis all variables whose associations with the outcome had a p value < 0.20 were selected in order to study possible confounding factors.
The research project was approved by the Research Ethics Committees at the Santa Casa de Misericórdia de Pelotas and the Fundação de Apoio Universitário (FAU). It was also approved by the Research Ethics Committee at the Universidade Federal do Rio Grande do Sul and by the Scientific Commission at the Universidade Católica de Pelotas.
Results
During the study period there were 3,449 births, 81% (2,799) of whom were born to mothers resident in the city of Pelotas. Twenty-nine of these children were not born in hospital, but were included in the study. Ten patients were discharged from hospital early and could not be located again, and 26 were seropositive for HIV, being duly excluded. Fourteen mothers (0.4%) did not agree to take part in the study, and eight refused to do so because of early death of their babies. The final population interviewed during the perinatal phase was 2,741 mothers, which represented 98% of births within the target population. Nine hundred and seventy-three of these mothers were selected for follow-up at 1, 3 and 6 months postpartum.
At the 3-month follow-up, 940 questionnaires were answered, with a total of 3.4% losses, being 13 deaths, five unlocatable addresses, six moves away from the city and five exclusions (one HIV-positive mother, two with mental disease and two adoptions). There were also four refusals.
There were no statistically significant differences in terms of the distribution of demographic, socioeconomic or reproductive characteristics between the whole population screened at hospital and the sample selected at random for home follow-up. Around 68% of the sample were in the low family income bracket of up to three times the minimum wage (MW), 45% of fathers and 41% of the mothers had received between 5 and 8 years' schooling. Around 50% of the mothers were aged 20 to 29 years, 39% had delivered by caesarian, 66% did not work and 1/4 had smoked during pregnancy. A majority of the mothers (76%) had attended six or more prenatal consultations; the incidence of low birth weight was approximately 9%, and 12% of babies were born before 37 weeks' gestation.
In relation to feeding patterns at 3 months, it can be observed that just 39% of the sample were being breastfed exclusively. The use of water/teas was observed in 13% of the sample. The main reason that mothers gave for introducing liquids was colic (41%). Around 19% were on partial breastfeeding and the reason given for the introduction of supplementary foods was that babies were hungry (46%). At 3 months, 1/3 of the babies were already weaned. Pacifiers were being given to 64% of the babies, and the reason given by mothers was that they calmed their babies (53%).
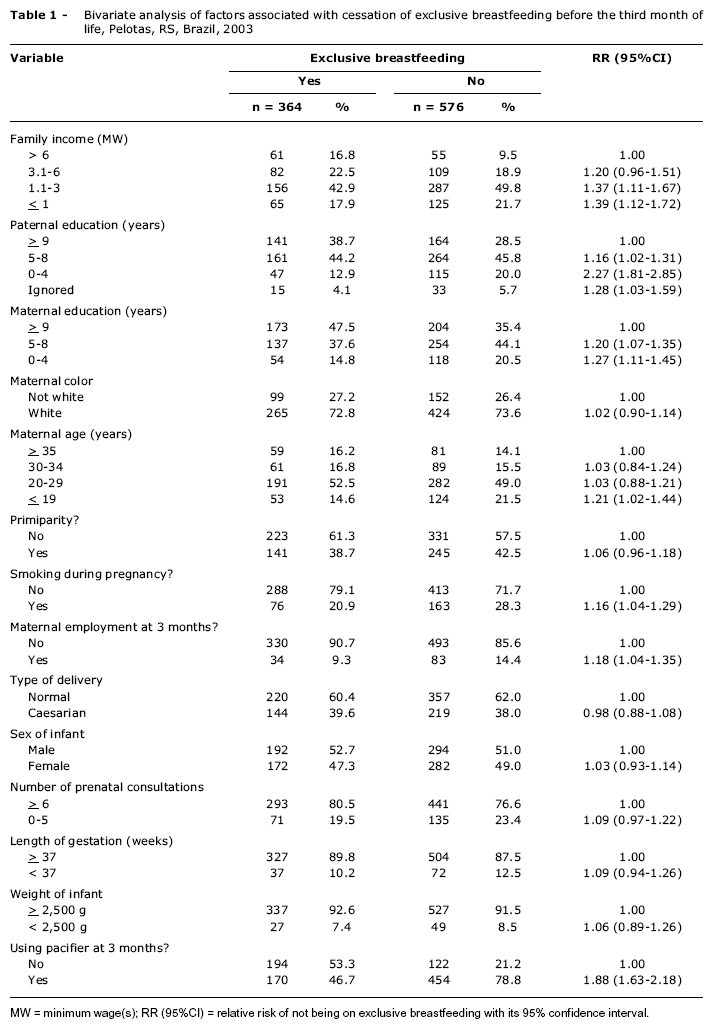
Table 1 shows the results of the bivariate analysis of factors related to cessation of exclusive breastfeeding before 3 months of age. Family income less than or equal to three times the MW, parental education of 8 years or less, smoking during pregnancy, mothers at work by 3 months and use of a pacifier at 3 months were all related with absence of exclusive breastfeeding at the third month. The factors family income and maternal education demonstrated a dose-response effect, and pacifier use increased the risk of these babies not being exclusively breastfed by 90%.
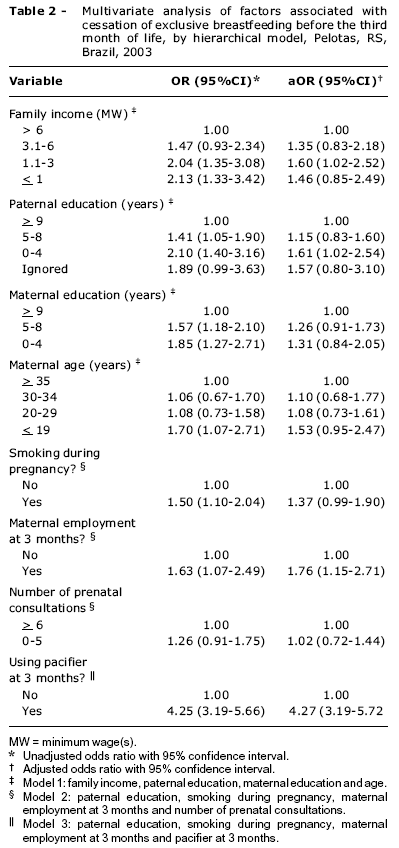
Table 2 contains results of the multivariate analysis of variables related with exclusive breastfeeding at the third month. It will be observed that certain factors did not maintain their association with outcome after adjustment for confounding factors. Only mothers working away from the home, family income between one and five times the MW, fathers educated for less than 5 years and pacifier use exhibited statistically significant associations. Babies given pacifiers had a four times greater risk of not being exclusively breastfed. There was a tendency (p = 0.06) for mothers who smoked during pregnancy to breastfeed exclusively less.
Discussion
Exclusive breastfeeding is a safe, economical and emotionally satisfying means of feeding babies, especially in developing countries.
This was a longitudinal population-based study that enabled breastfeeding rates to be evaluated and the factors associated with cessation of exclusive breastfeeding within the first 3 months of life to be determined. Since this study is part of a wider research project that assessed several outcomes, it is limited by the fact that specific frequency data was not collected either for pacifier use or for supplementary foods.
Breastfeeding rates in Pelotas, RS are not yet ideal, as is demonstrated by data found in studies undertaken in the city in 1993, 199810 and 2000.11 These studies were not, however, representative of the general population.
It will be observed that a lower level of paternal education was directly associated with cessation of exclusive breastfeeding within the first 3 months. It is possible that fathers with more education are better informed and aware of the benefits of breastfeeding, confirming the influence that fathers have on breastfeeding, generally underestimated by health professionals. The results found in a study undertaken by Litmann17 also indicated this possibility.
The results of this study found evidence of an association between the living conditions and cultural habits of the population and feeding practices during the first 3 months of life. Babies from low-income families (between one and three times the MW) had a greater chance of ceasing exclusive breastfeeding before the third month. This factor gains singular importance to the extent that it is exactly these children who are most exposed to other factors that increase infant morbidity and mortality.
It is interesting to observe that children from extremely poor families (earning the MW or less) did not have an increased risk of not being on exclusive breastfeeding at 3 months, probably due to a complete lack of the means of acquiring any substitute for breastmilk.
After analysis by adjusted logistic regression, there was no significant association with length of gestation or birth weight, in contrast with another study in which low birth weight was negatively associated with starting and continuing exclusive breastfeeding.18
The relationship between to maternal smoking during pregnancy and cessation of exclusive breastfeeding before the third month of life had no statistical significance after confounding factors were controlled.
A tendency was observed, however, for mothers who had smoked during pregnancy to breastfeed exclusively for shorter periods. There is a possibility that the same emotional factors that lead a woman to acquire a smoking habit also interfere negatively with her motivation to breastfeed. A similar result is to be found in a study performed by Silveira et al.19
A statistically significant association was observed between maternal employment at 3 months and absence of exclusive breastfeeding at the same age. It is very probable that this is the result of some women returning to work from maternity leave during this period, separating them from their babies for around 8 hours a day, which demonstrates not only the importance of maternity leave, but also of teaching women to express their milk so that their babies can still be fed exclusively on breastmilk even in their absence.
Some studies have demonstrated that the introduction of water or teas (predominant breastfeeding) is a frequent practice, particularly in developing countries.7,20 The results of the current study were similar since it was observed that these liquids were offered early on. This combination reduces the protection conferred by breastmilk against infection and also reduces breastfeeding duration,21 in addition to being an unnecessary practice when babies are breastfeeding exclusively, even in countries with tropical climates.22 Other Brazilian authors have also demonstrated that the offer of liquids to children exclusively breastfed occurs early.23,24 These infusions are offered in the belief that they have calming and laxative properties and this is a practice that is deeply rooted in our culture, even in populations who have been taught not to use them.
A strong association was observed between pacifier use at 3 months and absence of exclusive breastfeeding at the same age, which demonstrates that, although the population is instructed to avoid pacifiers, this is a cultural habit that is difficult to control and eradicate. In a study undertaken in Pelotas, RS, in 1993, it was observed that 67% of babies were given pacifiers during their first month and 80% in the third month.25
A study by Soares demonstrated that pacifier use was more frequent among children not exclusively breastfed.26 Kramer et al. demonstrated that, 73% of babies exposed to pacifiers had discontinued exclusive breastfeeding before 3 months of age, whereas babies not exposed had a prevalence of 58% cessation.27 Victora et al. confirmed this observation, concluding that the association between pacifier use and early weaning is complex and that pacifiers are a factor that contributes to weaning among mothers who do not feel completely comfortable with breastfeeding. It is possible that pacifiers are actually a marker of lactation difficulties and not the direct cause of weaning.28
The current study detected a number of factors that can interfere with the duration of exclusive breastfeeding and, consequently, in the health of children during their first months of life. Many different studies have demonstrated the protective effect of breastmilk against infant morbidity and mortality, which is the reason for the fundamental importance of adopting this practice, especially in poor populations, in which children's risk of death from infectious diseases is elevated.3,6-8
Data obtained in a national survey, carried out in 1999,29 demonstrate a growing tendency towards breastfeeding. Nevertheless, no significant increase was detected in exclusive breastfeeding, which fact confirms the global tendency whereby, despite major advances, exclusive breastfeeding duration is far from that laid out by the WHO.4
The results reported here suggest that the practice of exclusive breastfeeding is still at levels well below those recommended, which in turn reinforces the need to continue stimulating breastfeeding during the first months of life.
References
Manuscript received Jun 27 2005, accepted for publication Mar 22 2006.
- 1. Cohen RJ, Brown KH, Canahuati J, Rivera LL, Dewey KG. Effects of age of introduction of complementary foods on infant breast milk intake, total energy intake, and growth: a randomized intervention study in Honduras. Lancet. 1994;344:288-93.
- 2. Aggett PJ. Research priorities in complementary feeding: International Paediatric Association (IPA) and European Society of Paediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) Workshop. Pediatrics. 2000;106:1271.
- 3. Victora CG, Smith PG, Vaughan JP, Nobre LC, Lombardi C, Teixeira AM, et al. Evidence for protection by breast-feeding against infant deaths from infectious diseases in Brazil. Lancet. 1987;2:319-22.
-
4World Health Organization. Infant and young child nutrition: global strategy on infant and young child feeding. Geneva; 2002. (Fifty-fifth World Health Assembly, A55/15).
- 5. Victora CG, Smith PG, Vaughan JP, Nobre LC, Lombardi C, Teixeira AM, et al. Infant feeding and death due to diarrhea: a case-control study. Am J Epidemiol. 1989;129:1032-41.
- 6. Victora VG, Fuchs SC, Kirkwood BR, Lombardi C, Barros FC. Breast-feeding nutritional status and other prognostic factors for dehydration among young children with diarrhea in Brazil. Bull World Health Organ. 1992;70:467-75.
- 7. Cesar JA, Victora CG, Barros FC, Santos IS, Flores JA. Impact of breast feeding on admission for pneumonia during postneonatal period in Brazil: nested case-control study. BMJ. 1999;318:1316-20.
- 8. Lucas A, Morley R, Cole TJ, Lister G, Leeson-Payne C. Breast milk and subsequent intelligence quotient in children born preterm. Lancet. 1992;339:261-4.
- 9. van Odijk J, Kull I, Borres MP, Brandtzaeg P, Edberg U, Hanson LA, et al. Breastfeeding and allergic disease: a multidisciplinary review of the literature (1966 2001) on the mode of early feeding in infancy and its impact on later atopic manifestations. Allergy. 2003;58:833-43.
- 10. Albernaz E, Giugliani ER, Victora CG. Supporting breastfeeding: a successful experience. J Hum Lact. 1998;14:283-5.
- 11. Albernaz E, Victora CG, Haisma H, Wrigth A, Coward WA. Lactation counseling increases breast-feeding duration but not breast milk intake as measured by isotopic methods. J Nutr. 2003;133:205-10.
- 12. Vituri SC, de Brito ASJ. Prevalência do aleitamento materno em crianças até o sexto mês de idade na cidade de Maringá, estado do Paraná, Brasil. Acta Sci Health Sci. 2003;25:141-6.
- 13. Aidam BA, Perez-Escamilla R, Lartey A, Aidam J. Factors associated with exclusive breastfeeding in Accra, Ghana. Eur J Clin Nutr. 2005;59:789-96.
- 14. Venâncio SI, Escuder MML, Kitocco P, Rea MF, Monteiro CA. Freqüência e determinantes do aleitamento materno em municípios do Estado de São Paulo. Rev Saude Publica. 2002;36:313-8.
- 15. Oliveira LPM, Assis AMO, Gomes GSS, Prado MS, Barreto ML. Duração do aleitamento materno, regime alimentar e fatores associados segundo condições de vida em Salvador, Bahia, Brasil. Cad Saude Publica. 2005;21:1519-30.
- 16. Organización Mundial de la Salud. Indicadores para evaluar las practicas de lactancia materna. Genebra; 1991. (OMS/CED/SER/91,14).
- 17. Littman H, Medendorp SV, Goldfarb J. The decision to breastfeed: the importance of father's approval. Clin Pediatr (Phila). 1994;33:214-9.
- 18. Clements MS, Mitchell EA, Wright SP, Esmail A, Jones DR, Ford RP. Influences on breastfeeding in southeast England. Acta Paediatr. 1997;86:51-6.
- 19. Silveira FJF, Lamounier JA. Fatores associados à duração do aleitamento materno em três municípios na região do alto Jequitinhonha, Minas Gerais, Brasil. Cad. Saude Publica. 2006;22:69-77.
- 20. Wayland C. Breastfeeding patterns in Rio Branco, Acre, Brazil: a survey of reasons for weaning. Cad Saude Publica. 2004;20:1757-61.
- 21. Brown KH, Black RE, Romaña GL, Kanashiro HC. Infant-feeding practices and their relationship with diarrhea and other diseases in Huascar (Lima), Peru. Pediatrics. 1989;83:31-40.
- 22. Sachdev HP, Krishna J, Puri RK, Satyanarayana L, Kumar S. Water supplementation in exclusively breastfed infants during summer in the tropics. Lancet. 1991;337:929-33.
- 23. Marques NM, Lira PIC, Lima MC, Silva NL, Batista Filho M, Huttly SR, et al. Breastfeeding and early weaning practices in northeast Brazil: a longitudinal study. http://www.pediatrics.org/cgi/content/full/108/4/e66. Acesso: 24/04/2006.
- 24. Vieira GO, Silva LR, Vieira TO, Almeida JAG, Cabral VA. Hábitos alimentares em crianças menores de 1 ano amamentadas e não-amamentadas. J Pediatr (Rio J). 2004;80:411-6.
- 25. Victora CG, Tomasi E, Olinto MT, Barros FC. Use of pacifiers and breastfeeding duration. Lancet. 1993;341:404-6.
- 26. Soares MEM, Giugliani ERJ, Braun ML, Salgado ACN, Oliveira AP, Aguiar PR. Uso de chupetas e sua relação com o desmame precoce em população de crianças nascidas em Hospital Amigo da Criança. J Pediatr (Rio J). 2003;79:309-16.
- 27. Kramer MS, Barr RG, Dagenais S, Yang H, Jones P, Ciofani L, et al. Pacifier use, early weaning, and cry/fuss behavior. A randomized controlled trial. JAMA. 2001;286:322-6.
- 28. Victora CG, Behague DP, Barros FC, Olinto MT, Weiderpass E. Pacifier use and short breastfeeding duration: cause, consequence or coincidence? Pediatrics. 1997;99:445-53.
-
29Brasil, Ministério da Saúde, Secretaria de Políticas de Saúde, Área de Saúde da Criança. Prevalência de aleitamento materno nas capitais brasileiras e no Distrito Federal. Brasília: Ministério da Saúde; 2001.
Correspondence:
Publication Dates
-
Publication in this collection
12 Sept 2006 -
Date of issue
Aug 2006
History
-
Received
27 June 2005 -
Accepted
22 Mar 2006