Abstracts
OBJECTIVE: To investigate the influence of support groups on the family of risk newborn infants and on neonatal unit workers. METHODS: We used a qualitative approach, and as theoretical basis, family-centered care. The study was conducted in the neonatal unit of Hospital Prontolinda, in Pernambuco, Brazil. From January to June 2004, 25 meetings were held by the family support group. Data were collected through the observations of participants and through tape-recorded interviews with 13 mothers, six fathers, two grandmothers and 16 healthcare workers. The interviews were submitted to speech content analysis (thematic modality). RESULTS: The analysis revealed that the support group to the family of risk newborns provided parents and family members with information, emotional support and strengthening so that they could come to terms with the birth of their child and his/her admission to the neonatal unit, in addition to enabling parents to take care of the newborn infant. There was interpersonal growth in the interaction between parents, family members, and healthcare workers. CONCLUSIONS: The support group to the family of risk newborns uses an approach that is based on family-centered care. These principles allow restoring parental competence, helping healthcare workers to respect values and feelings of family members, and establishing a collaborative work between parents and healthcare workers in the neonatal unit.
Self-help groups; family; newborns; neonatal intensive care unit
OBJETIVO: Investigar o significado do grupo de apoio para a família de recém-nascidos de risco e equipe de profissionais na unidade neonatal. METODOLOGIA: Utilizou-se a abordagem qualitativa e, como referencial teórico, o cuidado centrado na família. O estudo foi realizado na unidade neonatal do Hospital Prontolinda, em Pernambuco. No período de janeiro a junho de 2004, foram realizadas 25 reuniões do grupo de apoio para a família. A coleta de dados foi realizada através da observação participante das reuniões do grupo e de entrevistas gravadas com 13 mães, seis pais, duas avós e 16 profissionais de saúde. As falas foram submetidas à análise de conteúdo, modalidade temática. RESULTADOS: A análise evidenciou que o grupo de apoio para a família de neonatos de risco proporcionou informação, apoio emocional e fortalecimento aos pais e familiares para que vivenciassem o nascimento e a hospitalização do filho na unidade neonatal, além de tê-los capacitado para assumir os cuidados com o recém-nascido. Paralelamente, houve crescimento interpessoal mútuo na interação entre pais, familiares e equipe de profissionais da unidade neonatal. CONCLUSÕES: O grupo de apoio para a família de neonatos de risco na unidade neonatal representa uma abordagem fundamentada nos princípios do cuidado centrado na família. A partir de tais princípios, pode-se restabelecer a competência parental, ajudar a equipe de profissionais a respeitar valores e sentimentos dos familiares, bem como contribuir para que pais e profissionais trabalhem em parceria na unidade neonatal.
Grupos de apoio; família; recém-nascidos; unidade terapia intensiva neonatal
ORIGINAL ARTICLE
The influence of support groups on the family of risk newborns and on neonatal unit workers
Virgínia BuarqueI; Marilia de Carvalho LimaII; Russel Parry ScottIII; Maria Gorete L. VasconcelosIV
IMestre, Universidade Federal de Pernambuco (UFPE), Recife, PE, Brasil. Neonatologista, Hospital das Clínicas, UFPE, Recife, PE, Brasil. Coordenadora, Unidade Neonatal, Hospital Prontolinda, Olinda, PE, Brasil
IIPhD, London School of Hygiene and Tropical Medicine (LSHTM), London, England. Professora adjunta, Departamento Materno-Infantil,UFPE, Recife, PE, Brasil
IIIPhD, University of Texas, Austin, USA. Professor adjunto, Departamento de Ciências Sociais, Programa de Pós-Graduação em Antropologia, UFPE, Recife, PE, Brasil
IVDoutora, Escola de Enfermagem de Ribeirão Preto, Universidade de São Paulo (USP), São Paulo, SP, Brasil. Professora adjunta, Departamento de Enfermagem, UFPE, Recife, PE
Correspondence Correspondence : Virgínia Buarque Rua Vitoriano Palhares, 218/501 - Torre CEP 50710-190 - Recife, PE - Brazil Tel.: +55 (81) 9282.8282 E-mail: virginia.buarque@bol.com.br
ABSTRACT
OBJECTIVE: To investigate the influence of support groups on the family of risk newborn infants and on neonatal unit workers.
METHODS: We used a qualitative approach, and as theoretical basis, family-centered care. The study was conducted in the neonatal unit of Hospital Prontolinda, in Pernambuco, Brazil. From January to June 2004, 25 meetings were held by the family support group. Data were collected through the observations of participants and through tape-recorded interviews with 13 mothers, six fathers, two grandmothers and 16 healthcare workers. The interviews were submitted to speech content analysis (thematic modality).
RESULTS: The analysis revealed that the support group to the family of risk newborns provided parents and family members with information, emotional support and strengthening so that they could come to terms with the birth of their child and his/her admission to the neonatal unit, in addition to enabling parents to take care of the newborn infant. There was interpersonal growth in the interaction between parents, family members, and healthcare workers.
CONCLUSIONS: The support group to the family of risk newborns uses an approach that is based on family-centered care. These principles allow restoring parental competence, helping healthcare workers to respect values and feelings of family members, and establishing a collaborative work between parents and healthcare workers in the neonatal unit.
Keywords: Self-help groups, family, newborns, neonatal intensive care unit.
Introduction
By analyzing the changes neonatal care has been put through, we can perceive that the presence of family has been much more frequent, and that they have interacted with healthcare workers in the neonatal intensive care unit (NICU). In this context, it is essential that the effects of birth and admission of the risk newborn to the NICU on parents and family members be evaluated. It is also important to find the best way to approach the family in order to help them adapt to the critical situation the newborn infant, parents and family members are experiencing, and share their feelings with the neonatal unit healthcare workers.
Risk newborns are those most likely to die during or after labor or those with a congenital or perinatal disease that requires immediate intervention.1
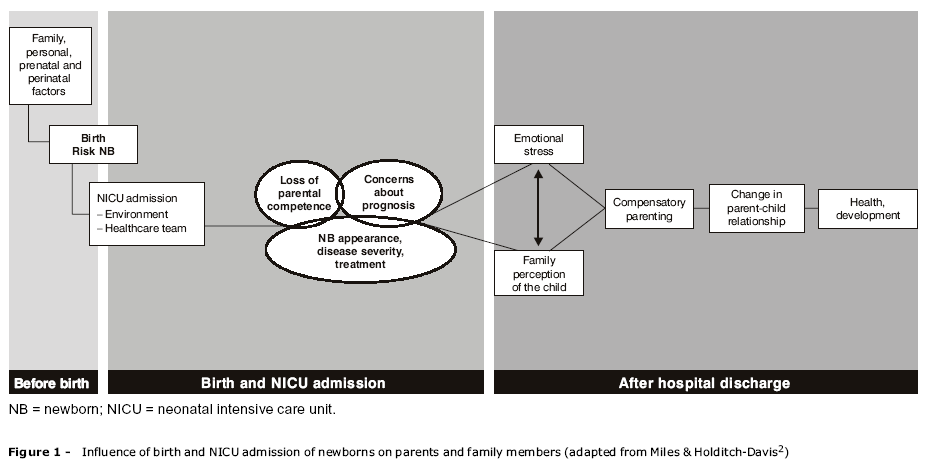
Figure 1 shows the effects of birth and NICU admission of newborns and possible triggers of stress to parents and family members.2 Emphasis is placed on the importance of knowing the family, personal, prenatal and perinatal history of parents in order to better understand what families carry with them in terms of life experience, enabling them to come to terms with the birth and hospitalization of their children.
When newborns are admitted to the NICU, some interrelated aspects exist that may cause stress on the family:2-5 the physical appearance of a newborn that is either preterm or unhealthy is stressful to parents, since the child does not meet their expectations, interfering with the bonding and interaction between parents and children;3 the severity of the disease and the treatment are a primary source of stress, as the newborn infant is in an NICU.6,7 Concerns about the prognosis, i.e., uncertainties about the well-being and about long-term outcomes regarding the child's health add to these sources of stress. Loss of parental competence can negatively and prematurely interfere with parent-child relationships, being the major stress factor to parents of preterm infants.2-5,8,9
Variables related to the environment and to the NICU workers are included in this whole situation experienced by parents, who should not only have to adapt to a high-tech hospital environment, but also come to terms with being parents in a collective and unknown place.10
Therefore, the emotional stress of childbirth and the perception of parents that their child "is different from a healthy newborn, recognizing their image as "special" for having survived admission to the NICU and "vulnerable" for the fear of future sequelae, lead to compensatory parenting, with influence on the parent-child relationships.
A wrong perception makes parents overprotect11 their children, since they tend to focus more on their deficiencies and vulnerability than on their virtues. This change in parenting style can influence children's health and development.8,12
The quality of the family environment has a larger predictive value for children's neuropsychomotor development than perinatal risks.8,12 Factors such as high level of family stress, low maternal responsiveness, and impaired parental competence, seem to play a direct role in children's development.13
There are two types of support to parents of risk newborns in the NICU: formal support, provided by some healthcare workers, and informal support, provided by the family and friends.14
The literature highlights the role of healthcare workers in mobilizing and strengthening family resources by implementing support groups, as a way to organize the work in the NICU, meeting the needs of newborn infants, and giving parents the opportunity to deal with the birth of their child and to cope with his/her hospitalization.15 Ideally, this group should be interdisciplinary, including a neonatologist, a nurse, a psychologist, and other health professionals.16-19
Several NICUs have a support group.14,17-19 Participants interact more with their children during the hospital stay and show greater interest in their development after hospital discharge.17,19
At Hospital Prontolinda, a support group was created in 2001. In this regard, the study was carried out to investigate the influence of the support group on the family of risk newborns and on neonatal unit workers.
Methods
A qualitative approach was used. According to Minayo,20 this approach takes into account the effects of the meaning and intention of actions on relationships and social structures, investigating deep into social relationships, which cannot be measured by figures and variables. So, we chose family-centered care as theoretical basis. This type of care has been regarded by the Association for Children's Care as the philosophy of care that acknowledges and respects the pivotal role of family in the newborn's life. Its major components, as cited by Shelton et al.,21 are described in Table 1.
The study was carried out at Hospital Prontolinda, a private tertiary care hospital for the treatment of risk mothers and newborns, located in Olinda, a town in the Metropolitan Area of Recife, state of Pernambuco, Brazil.
After admission of the newborn to the NICU, the family members are invited to join the support group, whose interdisciplinary team includes a neonatologist, a nurse, a psychologist, a breastfeeding expert, in addition to the main researcher (Virginia Buarque). In the sequential group meetings, held every week, these professionals address issues related to the necessities of family members (Table 2).
For methodological rigor, the triangulation method, based on Denzin,22 was used. Special emphasis was given to the speeches and actions of family members and healthcare workers. The investigation was based on the observation of support group meetings (with note-taking of the adherence and participation of family members and healthcare workers in the meetings, of discussed topics, of the interaction between participants, and of their opinions and comments) and on an open interview, where the following question was asked: "What's your opinion about the family support group"? The interviews were conducted in a private place, had an average duration of 45 minutes, were tape-recorded, and carried out by the main researcher.
The inclusion criteria were the following: being a volunteer participant; having a newborn infant who required admission to the NICU for 7 or more days; participating in at least three meetings; having an established date for hospital discharge, moment in which newborns and families will have gone through the different stages of hospitalization. Parents or relatives of newborns whose neonatologist was the main researcher were excluded from the study.
The selected healthcare workers were those who spent more time with families in the NICU and who concomitantly worked at other private hospitals, with a similar healthcare structure to that of the investigated hospital. The only difference was that they could miss some support group meetings, being therefore able to compare their involvement with families in the NICU with and without the help of the support group.
Following these criteria and the sampling principles adopted for qualitative research20 (giving privilege to social subjects that are important to the in-depth analysis and understanding of the problem being investigated, and data saturation), we interviewed 13 mothers, six fathers, two grandmothers and 16 healthcare workers. The study was approved by the Research Ethics Committee of the Center for Health Sciences (Centro de Ciências da Saúde) and an informed consent form was obtained.
The interviews were submitted to speech content analysis (thematic modality)23 and some speeches were presented for illustration.
Results and discussion
From January to June 2004, 25 family support group meetings were held, with larger participation of mothers (73 times), than of fathers (27 times) and grandmothers (26 times). Of these family members, 21 met the inclusion criteria and were interviewed.
Among the newborns included in the study, 85.7% were preterm and 92.8% weighed less than 2,500 g at birth. Hospital stay ranged from 14 days to 5 months, 50% had a severe outcome, and 78.6% were discharged from hospital.
Of the healthcare workers interviewed, 50% worked as nurse assistants, 25% as nurses and 25% as neonatologists. About 87.5% work in other NICUs. None of them had information about support groups of other NICUs.
Based on the perception of family members and of NICU workers about the meaning of support group, five key values were identified: information, emotion, qualification, strengthening and mutual learning.
The information value of the support group was highlighted in the first and third stages of group dynamics with the definition of risk newborns, their peculiarities, development, prognosis, special situations (deaths and malformations), NICU standards and routine practices, etc. The information value reduces the concern of family members and calms them down.
- The neonatologist says: "Parents will be informed about the problems experienced by the babies and how they are reacting" (Field logbook).
- "You don't refrain from explaining everything... you clear all doubts about what is happening to the baby and about NICU stuff... and you eventually calm parents down" (Mother 11).
- "Parents are more aware of the disease and of the necessity of their baby having to stay in the NICU and... they don't suffer so much because they are aware of everything that is happening to their baby" (Nurse assistant 1).
The emotional value, correlated with the second stage of support group dynamics, was perceived by the discussion of issues related to parent's adaptation after childbirth and during NICU admission and stay, allowing parents to express their feelings (fear, guilt, anger, uncertainty, etc.), and to tackle the difficulties related to the separation from and bonding with their child.
- "You get emotionally unstable... I blamed myself for what was happening... I was afraid of losing my daughter. (...) It was not only information about her health status I sought in the group, but the emotional aspect as well ... being able to speak out and being listened to... I felt more self-confident" (Mother 5).
- The mother (Mother 4) is being discharged from the maternity ward, but her son will have to stay in the NICU; she says: "I'm feeling awful!" (Field logbook).
- "With the support group, emotional support relieves stress... they have the chance to get it all off their chest" (Nurse 2).
The qualification value corresponds to the fourth stage of support group dynamics, where the family members get prepared for taking care of the newborn infants in different stages of their lives under the guidance of the NICU staff.
- "That moment in the support group was important because, if all that information hadn't been provided, it would've been harder for her (the mother) to take care of her preterm baby, and eventually she didn't have any difficulty whatsoever" (Grandmother 1 newborn 4).
- "I feel safe enough to go home now, this was actually a learning experience for me... I learned how to take care of my daughter" (Mother 10).
For healthcare workers, qualification is a routine practice that is inserted in neonatal care, and it is not directly correlated with and dependent upon the support group dynamics.
The strengthening value of the support group involves sharing different experiences between family members and their newborn infants during their different developmental stages, and also between family members and the NICU staff.
- "I found it interesting to exchange feelings... this gives you a lot of strength. (...) Listening to and being open to other parent's opinions. (...) The group provides such support" (Father 2 newborn 5).
- One of the participants (Mother 10) said: "Several times, I gained strength from the statements of more experienced mothers in the group" (Field logbook).
- "It is a time when families can sit down, talk about their experience, share it with other people who are going through the same ordeals... share their experience with healthcare workers ... families become stronger" (Neonatologist 2).
With regard to the value of mutual learning between families and healthcare workers, several other values were cited: trust, hope, safety, truth, honesty, respect, attention, consideration, compassion, helpfulness, affection, friendship, esteem, acceptance, motivation, humanization, empathy, harmony, among others.
- "They make ourselves comfortable... give us the opportunity to speak out. (...) Affection, attention, caring (...) and respect towards family members... being able to speak the truth, this set me at ease, after that I found trust and self-confidence" (Grandmother 1 newborn 4).
- "In the group, we perceive the participation of the health team. I felt safe and welcome," says the father (Father 8) (Field logbook).
- "Everybody learns there. (...) I feel parents get more confident and respect more our work... I feel their trust... we work in harmony" (Nursing assistant 2).
Obviously, the kind of support given during the support group meetings to families that have to cope with the admission of their children to the NICU depends on the status of each newborn, if he/she is in the acute or chronic stage, or on the severity of his/her condition.16
After childbirth and during the acute stage of NICU admission, parents and family members keep investigating further into the situation and gathering as much information as possible about the newborn. Based on the issues discussed in the support group, their perceptions about their child are down-to-earth and minimally propelled by fantasies, provided that they are given regular, repeated, and careful information that is appropriate to their level of concern and understanding.
It is important to include not only the problems experienced by newborns, but also the positive aspects, instead of focusing on the equipment or on the disease. Thus, several authors have underscored the necessity of accurate and up-to-date information so that family members can successfully adapt to the birth and NICU admission of their child and be reassured that the NICU has all the necessary technical resources, in addition to qualified professionals.24,25
On the other hand, the emotional value of the support group is related to neonatal care, which should prepare family members to cope with and adapt to the situation after the birth of their child and during the NICU stay. Parents remain observant of negative feelings throughout the crisis, and are able to express them verbally or by any other means by interacting with other families and with the NICU staff. Special attention should be given to the work developed by the psychologist, who addresses specific issues, and to the support from other parents and family members whose newborns are at different developmental stages.
Smith et al.16 report that parents who participated in support groups remarkably reduced stress and their feelings of social isolation, interacted more with their child, improving their parenting skills, with positive effects on their child's development.8,9,15,17,25-27
Several authors, in consistency with the qualification value of the support group, have mentioned that the participation of parents in child care restores their competence and parental confidence; they are more responsive to the presence of their child, and there is more interaction between parents and children, and parents are more able to control their feelings during the stay of their child in the NICU.6,18,24,25,28
The parents of a chronically ill newborn experience feelings of uncertainty, because they do not know for sure whether their child will have a remarkable improvement, whether they will remain chronically ill, or whether they will die. Therefore, support should encompass information, emotional, strengthening and qualification aspects. These parents need less information and more emotional support, since they often feel isolated.16 For Wiggins,24 parents should be instructed to assess their child's process on a regular basis, perhaps weekly instead of daily, so that they can alleviate their feelings of frustration.
Among the activities developed in the support group to parents of chronically ill newborns, "parent-to-parent support" is a highlight. In this type of support, former participants bear their testimony and help these parents in an effective and consistent way, thus emphasizing the strengthening value of this approach to family members.6,29 The participation of grandmothers is also of great importance, and certainly expands support to parents in the hospital and household environments.
In situations in which newborns are at imminent risk of death, or when they die, the approach should be made at an individual level. Parents and family members recognize the importance of information, emotional and strengthening values of the group support. Honest, repeated and up-to-date information about the unfavorable outcome of the newborn, the certainty that the child received appropriate care, and the concern about parent's well-being should be a constant throughout this stage.
In all development stages of the newborn, his/her family members interact with the NICU staff. The value of mutual learning concerns the process of taking care, which allows for effective interaction, with interpersonal growth between parents and NICU workers. Several authors have underscored the importance of interaction between parents, family members, and NICU staff, i.e., mutual collaboration and confidence with shared responsibility and limitations.17,18,27,28
Smith et al.16 have pointed out the disadvantages of support groups that use only the formal approach. Possibly, listening to the experience of other parents in similarly traumatic situations may result in a larger emotional load for those who have been trying to control their own emotions. A more direct approach (from family members, for instance) would be more appropriate to these parents, since they would not have to return the support.
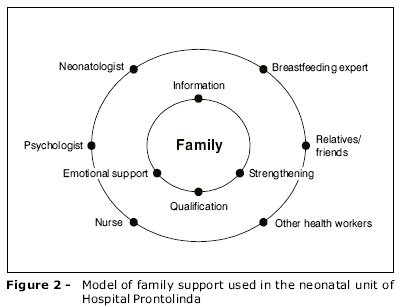
Figure 2 shows the model of family support group, based on the results of the present study. Family is the focus of attention which, in turn, provides help by developing strategies for emotional, strengthening and information support, enhancing the healthy perception about the birth and NICU admission of a risk newborn, in addition to restoring parental competence. The support group should use formal support, provided by an interdisciplinary team, and informal support, provided by family members, throughout the process. Intergenerational support30 also plays a crucial role and so does parent-to-parent support.
The work involving a support group to family members of risk newborns is based on the principles of family-centered care. These principles allow restoring parental competence, helping healthcare workers to respect the values and feelings of family members and enabling parents and healthcare workers to establish a partnership in neonatal care.
References
Manuscript received Sep 27 2005, accepted for publication Mar 22 2006.
- 1. Kenner C. Enfermagem neonatal. 2Ş ed. Rio de Janeiro: Reichmann & Affonso; 2001.
- 2. Miles MS, Holditch-Davis D. Parenting the prematurely born child: pathways of influence. Semin Perinatol. 1997;21:254-66.
- 3. Affonso DD, Hurst I, Mayberry LJ, Haller L, Yost K, Lynch ME. Stressors reported by mothers of hospitalized premature infants. Neonatal Netw. 1992;11:63-70.
- 4. Miles MS, Funk SG, Kasper, MA. The neonatal intensive care unit environment: sources of stress for parents. AACN Clin Issues Crit Care Nurs. 1991;2:346-54.
- 5. Miles MS, Funk SG, Kasper MA. The stress response of mothers and fathers of preterm infants. Res Nurs Health. 1992;15:261-9.
- 6. Roman LA, Lindsay JK, Boger RP, DeWys M, Beaumont EJ, Jones AS, et al. Parent-to-parent support initiated in the neonatal intensive care unit. Res Nurs Health. 1995;18:385-94.
- 7. Singer LT, Bruening P, Davillier M, Hawkins S, Yamashita T. Social support psychological distress and parenting strains in mothers of very low birth weight infants' family relations. Fam Relat. 1996;45:343-50.
- 8. Linhares MBM, Carvalho AEV, Padovani FHP, Bordin MBM, Martins IMB, Martinez FEA Compreensão do fator de risco da prematuridade sob a ótica desenvolvimental: In: Marturano EM, Linhares MBL, Loureiro SR. Vulnerabilidade e proteção: indicadores na trajetória de desenvolvimento do escolar. São Paulo: Casa do Psicólogo; 2004. p. 11-37.
- 9. Santelli B, Turnbull A, Higgins C. Parent to parent support and health care. Pediatr Nurs. 1997;23:303-6.
- 10. Bialoskurski M, Cox CL, Hayes JA. The nature of attachment in neonatal intensive care unit. J Perinat Neonatal Nurs. 1999;13:66-77.
- 11. Brazelton TB. Momentos decisivos do desenvolvimento infantil. São Paulo: Martins Fontes; 1994.
- 12. Miles MS, Holditch-Davis D. Compensatory parenting: how mothers describe parenting their 3-year-old prematurely born children. J Pediatr Nurs. 1995;10:243-53.
- 13. Allen EC, Manuel JC, Legault C, Naughton MJ, Pivor C, O'Shea TM. Perception of child vulnerability among mothers of former premature infants. Pediatrics. 2004;113:267-73.
- 14. Gomes MM. As repercussões familiares da hospitalização do recém-nascido na UTI neonatal: construindo possibilidades de cuidado [tese]. São Paulo: Escola Paulista de Medicina, Universidade Federal de São Paulo; 1999.
- 15. Sylvest A, Peitersen B. Parent groups. Crisis intervention for parents of extremely premature infants during hospitalization. Ugeskr Laeger. 2000;162:659-62.
- 16. Smith K, Gabard D, Dale D, Drucker A. Parents opinions about attending parent support groups. Child Health Care. 1994;23:127-36.
- 17. Bracht M, Ardal F, Bot A, Cheng CM. Initiation and maintenance of a hospital-based parent group for parents of premature infants: key factors for success. Neonatal Netw. 1998;17:33-7.
- 18. Pearson J, Andersen K. Evaluation of a program to promote positive parenting in the neonatal intensive care unit. Neonatal Netw. 2001:20:43-8.
- 19. Eriksson BS, Pehrsson, G. Evaluation of psycho-social support to parents with an infant born preterm. J Child Health Care. 2002;6:19-33.
- 20. Minayo MCS. O desafio do conhecimento: pesquisa qualitativa em saúde. 8Ş ed. São Paulo: Hucitec; 2004.
- 21. Shelton TL, Jeppson ES, Jonhnson BH. Family-centered care for children with special health care needs. Washington: Association for care of children's health; 1987.
- 22. Denzin NK. The research act. 3rd ed. New York: McGraw Hill; 1989.
- 23. Bardin L. Análise de conteúdo. Lisboa: Edições 70; 1979.
- 24. Wiggins JB. A família na unidade de terapia intensiva neonatal. In: Avery GB, Fletcher MA, MacDonald MG. Neonatologia: fisiopatologia e tratamento do recém-nascido. 4Ş ed. Rio de Janeiro: Medsi; 1999. p. 69-78.
- 25. Barros L. Initial beliefs, emotions and coping processes of parents of high-risk babies. http://aifref.uqam.ca/actes/pdf_ang/barros.pdf. Acesso: 25/04/2004.
- 26. Ward K. Perceived needs of parents of critically ill infants in a neonatal intensive care unit (NICU). Pediatr Nurs. 2001;27:281-6.
- 27. Vasconcelos MGL. Implantação de um grupo de apoio à mãe acompanhante de recém-nascido pré-termo e de baixo peso em um hospital amigo da criança na cidade de Recife, PE [tese]. São Paulo: Universidade de São Paulo; 2004.
- 28. VandenBerg KA. Supporting parents in the NICU: guidelines for promoting parent confidence and competence. Neonatal Netw. 2000;19:63-4.
- 29. Lindsay JK, Roman L, DeWys M, Eager M, Levick J, Quinn M. Creative caring in the NICU: parent-to-parent support. Neonatal Netw. 1993;12:37-44.
- 30. Prudhoe CM, Peters DL. Social support of parents and grandparents in the neonatal intensive care unit. Pediatr Nurs. 1995;21:140-6.
Correspondence
Publication Dates
-
Publication in this collection
12 Sept 2006 -
Date of issue
Aug 2006
History
-
Accepted
22 Mar 2006 -
Received
27 Sept 2005