Abstracts
OBJECTIVE: To evaluate the impact of music therapy on breastfeeding rates among mothers of premature newborns. METHOD: In this open randomized controlled trial, mothers of premature neonates weighting < 1,750 g were submitted to music therapy sessions three times a week for 60 minutes. The endpoints were breastfeeding rates at the moment of infant hospital discharge and at follow-up visits (7-15 days, 30 and 60 days after discharge). RESULTS: A total of 94 mothers (48 in the music therapy group and 46 in the comparison group) were studied. Breastfeeding was significantly more frequent in the music therapy group at the first follow-up visit [relative risk (RR) = 1.26; 95% confidence interval (95%CI) = 1.01-1.57; p = 0.03; number needed to treat (NNT) = 5.6]. Moreover, this group showed higher breastfeeding rates at the moment of infant discharge (RR = 1.22; 95%CI = 0.99-1.51; p = 0.06; NNT = 6.3) and at days 30 and 60 after discharge (RR = 1.21; 95%CI = 0.73-5.6; p = 0.13 and RR = 1.28; 95%CI = 0.95-1.71; p = 0.09, respectively), but those results were not statistically significant. CONCLUSIONS: This study demonstrated that music therapy had a significant effect in increasing breastfeeding rates among mothers of premature newborns at the first follow-up visit, and also a positive influence (although not significant) that lasted up to 60 days after infant discharge. Music therapy may be useful for increasing breastfeeding rates among mothers of premature newborns.
Breastfeeding; music therapy; maternal welfare; infant; newborn
OBJETIVO: Avaliar o impacto da musicoterapia nos índices de aleitamento materno entre mães de recém-nascidos prematuros. MÉTODO: Neste ensaio clínico controlado, randomizado e aberto, mães de neonatos prematuros com peso < 1.750 g foram submetidas a sessões de musicoterapia três vezes por semana durante 60 minutos. Os desfechos foram os índices de aleitamento materno na ocasião da alta hospitalar do bebê e em consultas de seguimento (7-15 dias, 30 e 60 dias após a alta). RESULTADOS: Foram avaliadas 94 mães (48 no grupo da musicoterapia e 46 no grupo controle). O aleitamento materno foi significativamente mais frequente no grupo da musicoterapia na primeira consulta de seguimento [risco relativo (RR) = 1,26; intervalo de confiança de 95% (IC95%) = 1,01-1,57; p = 0,03; número necessário para tratar (NNT) = 5,6]. Esse grupo também apresentou índices mais elevados de aleitamento materno na ocasião da alta do bebê (RR = 1,22; IC95% = 0,99-1,51; p = 0,06; NNT = 6,3), e 30 e 60 dias após a alta (RR = 1,21; IC95% = 0,73-5,66; p = 0,13 e RR = 1,28; IC95% = 0,95-1,71; p = 0,09, respectivamente), mas esses resultados não foram estatisticamente significativos. CONCLUSÕES: Este estudo demonstrou que a musicoterapia teve efeito significativo no aumento do índice de aleitamento materno entre mães de recém-nascidos prematuros na primeira consulta de seguimento, e uma influência positiva (embora não significativa) que se estendeu até 60 dias depois da alta. A musicoterapia pode ser útil para elevar os índices de aleitamento materno entre mães de prematuros.
Aleitamento materno; musicoterapia; bem-estar materno; lactente; recém-nascido
ORIGINAL ARTICLE
IMT, MSc. Maternidade Escola, Universidade Federal do Rio de Janeiro (UFRJ), Rio de Janeiro, RJ, Brazil
IIMD, PhD. Department of Pediatrics, School of Medicine at Instituto de Puericultura e Pediatria Martagão Gesteira, UFRJ, Rio de Janeiro, RJ, Brazil
IIIMT. Maternidade Escola, UFRJ, Rio de Janeiro, RJ, Brazil
Correspondence
ABSTRACT
OBJECTIVE: To evaluate the impact of music therapy on breastfeeding rates among mothers of premature newborns.
METHOD: In this open randomized controlled trial, mothers of premature neonates weighting < 1,750 g were submitted to music therapy sessions three times a week for 60 minutes. The endpoints were breastfeeding rates at the moment of infant hospital discharge and at follow-up visits (7-15 days, 30 and 60 days after discharge).
RESULTS: A total of 94 mothers (48 in the music therapy group and 46 in the comparison group) were studied. Breastfeeding was significantly more frequent in the music therapy group at the first follow-up visit [relative risk (RR) = 1.26; 95% confidence interval (95%CI) = 1.01-1.57; p = 0.03; number needed to treat (NNT) = 5.6]. Moreover, this group showed higher breastfeeding rates at the moment of infant discharge (RR = 1.22; 95%CI = 0.99-1.51; p = 0.06; NNT = 6.3) and at days 30 and 60 after discharge (RR = 1.21; 95%CI = 0.73-5.6; p = 0.13 and RR = 1.28; 95%CI = 0.95-1.71; p = 0.09, respectively), but those results were not statistically significant.
CONCLUSIONS: This study demonstrated that music therapy had a significant effect in increasing breastfeeding rates among mothers of premature newborns at the first follow-up visit, and also a positive influence (although not significant) that lasted up to 60 days after infant discharge. Music therapy may be useful for increasing breastfeeding rates among mothers of premature newborns.
Keywords: Breastfeeding, music therapy, maternal welfare, infant, newborn.
Introduction
Music therapy has been shown to have positive effects in several areas, such as mental health, special education, rehabilitation, and social development. Some studies have demonstrated that music therapy can reduce maternal anxiety, helping mothers to cope with their infants' stay in the neonatal intensive care unit (NICU), and also influences preterm behavior, providing greater periods of quiet sleep states, less crying, and an increase in weight gain1-4; but none of the studies have addressed the influence of music therapy on breastfeeding rates.
Promoting breastfeeding is a well-known, simple, and efficient strategy to decrease morbidity and mortality in children all over the world5; therefore, any intervention that can increase breastfeeding rates may be of interest to healthcare personnel. This study aims to evaluate the impact of music therapy, which was applied to mothers of premature newborns during hospital stay, on breastfeeding rates at the time of infant discharge from hospital and at follow-up visits. The hypothesis is that music therapy can increase those rates.
Methods
This was an open randomized controlled trial (RCT) with mothers of premature newborns admitted to the NICU, to the intermediate care unit, and to the kangaroo-care nursery of the Maternity Hospital of Universidade Federal do Rio de Janeiro (UFRJ), Brazil.
Inclusion criteria were as follows: mothers of premature infants with a birth weight < 1,750 g and that were clinically stable (lower risk of mortality), as defined by the NICU medical staff, and mothers who had provided written informed consent. Exclusion criteria were the following: mothers that are HIV positive, mothers of neonates with clinical problems that impaired breast suction (e.g., encephalopathy with severe hypotonia, oro-facial anomalies, and heart problems), and mothers with severe hearing deficiencies. Mothers who, for any reason, had three or less music therapy sessions and those whose neonates died during hospital stay were also excluded.
Sample size was calculated considering the expected breastfeeding rate at the time of the infant hospital discharge and at the first follow-up visit (between 7 and 15 days after discharge). According to data of the follow-up service, this rate was around 75%. Expecting an absolute difference of 22% between groups, 95% confidence level (5% alpha error), and 80% power (20% beta error), 92 subjects would need to be enrolled (46 in each study arm). Estimating a 7.5% loss after randomization, the total number of subjects considered necessary to conduct the study was 100.
Breastfeeding was defined, according to the World Health Organization,6 as one of the following conditions: exclusive breastfeeding, predominant breastfeeding, and complementary breastfeeding, all of which, for the purposes of this study, were collectively called "any breastfeeding". Infants who were not receiving breastfeeding at all were classified as "non-breastfeeding".
The endpoints were the rates of breastfeeding at the time of infant hospital discharge, at the first follow-up visit (7-15 days after discharge), and at 30 and 60 days after discharge.
Demographic, socioeconomic and obstetric variables, such as: age, marital status, occupation, education level, religion, number of other children, planned pregnancy, prenatal care, and income were studied in both groups.
The control group (CG) received only the usual care during hospital admission and follow-up visits.
Music therapy intervention
Music therapy sessions were systematically offered to all mothers in the intervention group, three times a week, but they were not mandatory. The sessions were conducted by two music therapists (MNSV and ASC), in an appropriate room, for 60 minutes, using the following instruments: keyboard, acoustic guitar, caxixi, shaker, conga, tumba, surdo, ganzá, triangle, afuche, egg-shake, metallophone, clave, rattle, tambourine, pandeirola, and tantã. Sessions were divided into four movements:
- First movement (5-10 minutes) - verbal expression / reception: the session started with the reception of the mothers by the music therapy team. It was a moment when they could talk freely about themselves and their babies.
- Second movement (20-30 minutes) - musical expression / sound continent: musical instruments were freely available, and therapists interacted with mothers through playing and/or singing any type of music they wanted.
- Third movement - lullabies and relaxation (15-20 minutes): at this time, music therapists offered, through singing and playing, a set of Brazilian lullabies previously selected. Moreover, instrumental erudite recorded musical pieces could be played, like Thäis-Meditation by Massenet (5 minutes of duration), Lullaby by Brahms (2 minutes of duration), and Air on the G String by Bach (5 minutes of duration). During this movement, the lights were turned off, which favored relaxation.
- Fourth movement - closing (5 minutes): at this moment, lights were turned on, and a free conversation, about the session and about what happened during the past days, was held.
Mothers in kangaroo-care participated in the music therapy sessions accompanied by their children.
Randomization and data collection
After enrollment, subjects were randomized in a 1:1 fashion to the intervention group [music therapy group (MTG)] or to the comparison group [control group (CG)], using a table of random numbers.7 Block randomization was used, with eight subjects (four for each arm).
The sequence of random numbers was known to only one of the authors (APB). A system of centralized randomization was used. As soon as a subject considered eligible signed the informed consent, the music therapy team contacted the author responsible for the randomization, who provided the allocation group of the subject.
To assess breastfeeding type at the moment of infant hospital discharge and at the follow-up visits, a health professional not involved in the study and not aware of the study objectives and of the group assignment interviewed the mothers with the purpose of filling in a pre-formatted question with a four-option answer, previously attached to medical charts, signaling one of the two possibilities defined as "any breastfeeding" or "non-breastfeeding".
Statistical analysis
Dichotomous variables were compared using a chi-square test or a Fisher exact test, when appropriate. Parametric data were compared using the Student t test, and non-parametric data were compared using the Mann-Whitney U test. In the analysis of data, when there were missing values regarding breastfeeding, it was attributed the worst outcome (non-breastfeeding). A value of p = 0.05 was considered to indicate statistical significance. Relative risks (RR), with 95% confidence intervals (95%CI), were also used to evaluate the impact of the intervention on the outcome, and the number needed to treat (NNT) was calculated.
Ethics
This study was approved by the Research Ethics Committee of Instituto de Puericultura e Pediatria Martagão Gesteira from the UFRJ, and is in accordance with the Helsinki Declaration of 1975, as revised in 1983. The trial registration number of the study at www.clinicaltrials.gov is: NCT00930761.
Results
Between March 2004 and June 2007, 190 eligible mothers were selected. Of those, 89 were excluded: 26 because their neonates fulfilled one of the exclusion criteria, 18 because their newborns died before being considered clinically stable by the medical staff, 11 because they did not agree to participate, and 34 because they could not be accessed during the newborn hospital stay, most due to receiving early hospital discharge. Thus, 101 mothers were randomized, 51 for the MTG, and 50 for the CG. After data collection started, there were seven losses (three in MTG for not reaching the minimum established number of three sessions; four in CG, three because the newborns died during the study period, and one because the mother refused to continue in the study). In the end, 94 mothers remained, 48 in the MTG and 46 in the CG (Figure 1).
Characteristics of the subjects
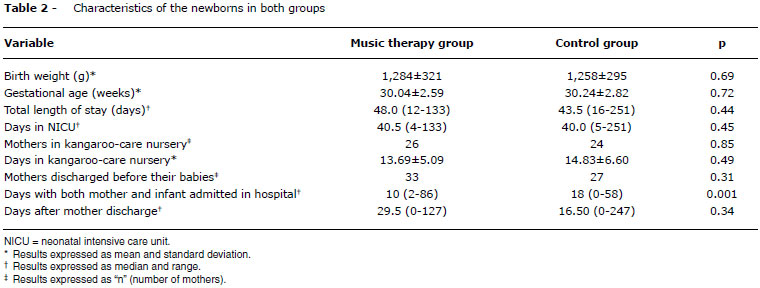
The demographic, socioeconomic and obstetric characteristics of participating mothers were similar in the two groups (Table 1). Birth weight, gestational age, total length of stay, days in NICU, and days in kangaroo-care nursery were all similar in both groups. In the CG, the mothers stayed significantly more days admitted, accompanying their babies, than in the MTG (Table 2).
In the intervention group, the ratio between music therapy sessions attended and those offered (adherence) varied from 17.5 to 100% (median: 65%), with a mean of 9±5.8 (range: 3-25) and a median of seven sessions per subject. The mean time between birth and the beginning of music therapy sessions (time for infants to reach clinical stability) was 11±7.3 days (median: 9).
Endpoints
At the moment of infant discharge from the hospital, 42 mothers (88%) continued to offer some type of breastfeeding (exclusive, predominant or complementary) to their children in MTG, and 33 (72%) in CG (RR = 1.22; 95%CI = 0.99-1.51; p = 0.06; NNT = 6.3). At the time of the first follow-up visit (between 7 and 15 days after discharge), five mothers did not attend the consultation (one in MTG and four in CG). Considering these mothers as having the worst outcome (non-breastfeeding), 42 mothers (88%) continued to offer some type of breastfeeding to their children in MTG, and 32 (70%) in CG (RR = 1.26; 95%CI = 1.01-1.57; p = 0.03; NNT = 5.6). At 30 days after the infant hospital discharge, two mothers did not attend the consultation (both in CG). Attributing to these mothers the worst outcome (non-breastfeeding), 38 mothers (79%) continued to offer some type of breastfeeding to their children in MTG, and 30 (65%) in CG (RR = 1.21; 95%CI = 0.73-5.66; p = 0.13). At 60 days, only one mother did not attend the consultation (CG), 36 mothers (75%) were still offering some type of breastfeeding in MTG, and 27 (59%) in CG (RR = 1.28; 95%CI = 0.95-1.71; p = 0.09), as detailed in Table 3.
Discussion
This study demonstrated a positive impact of music therapy on breastfeeding rates among mothers of premature newborns, mainly closer to the intervention, showing a statistically significant difference between the groups at the first follow-up visit (p = 0.03), and a trend towards significance at the time of infant hospital discharge, as well as at 30- and 60-day follow-up visits (p = 0.06; p = 0.13; p = 0.09, respectively).
The choice for studying mothers of hospitalized premature newborns was based on two reasons: a) the high stress level generally found among those mothers, due to their children's prematurity and critical state of health; and b) the fact that most mothers stayed at the hospital during the period of their children's admission, some for a prolonged period, allowing for the application of the music therapy intervention on a regular basis.
The use of music as a complementary tool in the promotion of health has been recently reported in the medical literature. Defined as the therapeutic use of music or of musical activities in the treatment of somatic and mental diseases, music therapy has been accumulating scientific evidence of its effectiveness in the handling of pain, anxiety and emotional stress, among other conditions.1-4,8-11
In obstetrics, one study demonstrated that the fetus responds to musical stimuli and to the human voice, by increasing heart rate and movements, to a significantly greater extent than to a sham stimulus,12 and others studies have concluded that sessions of passive music therapy (i.e., hearing of selected recorded music) have a favorable influence on feelings of comfort, and also reduce stress and anxiety levels during labor and delivery.13,14 In neonatology, some studies have shown that listening to music may reduce parents' and premature babies' stress in the NICU15; reduce the fall in oxygen saturation during endotracheal tube aspiration, and accelerate the recovery of saturation levels after the procedure16; furthermore, improve physiological parameters in infants, reduce their weight loss and shorten their length of stay in the NICU and at the hospital,17 and also increase non-nutritive sucking in premature infants.18
To our knowledge, this is the first RCT to evaluate the impact of music therapy on breastfeeding rates among mothers of premature neonates. Lai et al. studied the influence of the hearing of lullabies for 60 minutes a day, for 3 consecutive days, in mothers and premature newborns weighting less than 1,500 g.1 The authors found no differences in physiological parameters in the newborns, and, although they did detect a reduction of anxiety levels in mothers of the study group, the influence of music therapy on the rate of breastfeeding was not studied. Nöcker-Ribaupierre reported that the use of music therapy applied to mothers of premature newborns was capable of reducing stress and increasing breastfeeding rate, but the authors did not conduct a RCT.19
The present study used mainly active music therapy, allowing mothers to participate in the act of "making music," that is, the musical production originating from the subject's own expressive internal motivations, in which one chooses the musical instruments, the way of playing them, the songs, and can also make improvisations, in a spontaneous linkage. Arnon et al. demonstrated, in a RCT with newborns admitted to the NICU, that live music therapy showed significantly better results than those observed in subjects who heard recorded music or did not hear any music (CG), both in subjective evaluations (behavioral scale) and in objective parameters (e.g., heart rate, breathing rate, and oxygen saturation).20
In this study, the two groups were similar with regard to the mothers' obstetric, social-demographic, and cultural characteristics, as well as the newborn profiles. The only significant difference was in the total number of days that mothers stayed admitted while their babies were in the NICU; but this difference, in our point of view, favors the intervention, because, although the mothers in the MTG stayed admitted for a shorter time, they still have a greater tendency to keep breastfeeding. The median length of hospital stay of 48 days in the MTG allowed for an average of 9±5.8 sessions (range: 3-25, median: 7).The aim was to provide the largest possible number of sessions, in order to increase the exposure to the intervention; but, unfortunately, this was not always possible. Some higher birth weight newborns were discharged earlier, and some mothers needed to leave the hospital, although their neonates stayed admitted. In any case, we obtained a median of seven sessions per subject, which was equivalent to 3 weeks of treatment. This number, compared to most of the published studies, may be considered a success. As the sessions were not mandatory, the adherence of mothers to the sessions was not 100%, but, even so, the median adherence of 65% (range: 17-100%) was also considered excellent. Krout, studying the effect of music therapy in the state of relaxation, physical comfort, and pain control in terminal patients, concluded that the method was effective when a minimum of three sessions were conducted.21
The model used for the music therapy sessions was extremely singular, in comparison to other studies in the literature. Sessions of 1 hour duration, divided into four parts, allowed for an initial spontaneous verbal expression, in which each mother could express their enormous anguish due to their fragile newborns being admitted to a NICU, preparing the ground so that emotions could be brought up to proceed into the musical expression phase. These initial moments provided a therapeutic atmosphere for the reduction of stress and anxiety, with the expected positive impact on the decision to engage in breastfeeding. Additionally, more important than hearing music, the act of "making music" is recognized thoroughly as one of the primary mechanisms of the effectiveness of music therapy. In our study, it was in the second phase of the sessions that those mothers could try (some for the first time) to manipulate the musical instruments and to experience their capacity to participate in "making music" and its special beneficial effects. In the third movement, the use of lullabies stimulated the mother-infant bonding and the strengthening of those affectionate bonds, which increased the likelihood of success in promoting breastfeeding. The final phase, of integration, allowed for the exchange of experiences between the participating mothers and the team. This model is unique. The existing studies are scarce, and, in most reports, passive music therapy prevails, which means there is little interaction with musical instruments.
The results of this study suggest that music therapy may have a positive impact on breastfeeding rates at the time of discharge (p = 0.06) and at the first follow up visit (p = 0.03), taking into account all breastfeeding types. We included all of them in the analysis because we believe that the effect on all breastfeeding types (not only exclusive breastfeeding) is important for the premature infant. Although this was an open trial with no placebo group, the study design used is more powerful than the ones used in previous studies. The NNTs found indicate that, for one mother to benefit from this therapy, during the hospitalization period, five to seven needed to participate in the sessions. This small number suggests a good cost-effectiveness relationship, especially because the music therapy sessions are necessarily conducted in groups. Additionally, it is reasonable to think that, if the sessions could continue after the neonate's hospital discharge, the positive effects could be prolonged.
There were three exclusions in the MTG and four in the CG after randomization, but, even if it was used an intention-to-treat analysis, the results obtained would not be different. Another point that may be raised is that sessions included both music therapy and verbal interactions, but the time designated to these interactions was only the first 5 to 10 minutes and the last 5 minutes, leaving 45-50 minutes to music therapy itself. The only way to overcome this bias would be the assignment of a third group that would have only the first 5 to 10 minutes of talking with the therapeutic team and no music therapy at all; but this would require at least more 50 subjects, and a very long time to end the study, turning the research unviable. In spite of the issue mentioned above, this study clearly shows the benefits of music therapy, in the singular way it was offered, that is, combined with other stress-relieving component. However, it needs to be replicated in other settings, with larger sample sizes, to confirm the results we found. In addition, if our findings are confirmed, music therapy could be an additional, relatively simple, and low-cost strategy to be implemented in hospital maternities for increasing breastfeeding rates among mothers of premature infants and, consequently, its associated benefits.
The results of this study suggest that music therapy may have a positive impact on the maintenance of breastfeeding in mothers of hospitalized premature neonates. A relatively low NNT and the characteristics of the intervention with groups of mothers suggest that this approach could be useful in increasing breastfeeding rates among mothers of premature newborns.
References
- 1. Lai HL, Chen CJ, Peng TC, Chang FM, Hsieh ML, Huang HY, et al. Randomized controlled trial of music during kangaroo care on maternal state anxiety and preterm infants' responses. Int J Nurs Stud. 2006;43:139-46.
- 2. Cevasco AM. The effects of mothers' singing on full-term and preterm infants and maternal emotional responses. J Music Ther. 2008;45:273-306.
- 3. Kemper KJ, Hamilton C. Live harp music reduces activity and increases weight gain in stable premature infants. J Altern Complement Med. 2008;14:1185-6.
- 4. Keith DR, Russell K, Weaver BS. The effects of music listening on inconsolable crying in premature infants. J Music Ther. 2009;46:191-203.
- 5. Jones G, Steketee RW, Black RE, Bhutta ZA, Morris SS; the Bellagio Child Survival Study Group. How many child deaths can we prevent this year? Lancet. 2003;362:65-71.
-
6World Health Organization. Indicators for assessing breastfeeding practices: reprinted report of an informal meeting. Geneva: WHO, 1991. http://whqlibdoc.who.int/hq/1991/WHO_CDD_SER_91.14.pdf Acesso: 30 Nov 2010.
- 7. Fisher RA, Yates F. Statistical tables for biological, agricultural and medical research. 6th ed. Edinburgh and London: Oliver and Boyd Ltd; 1963.
- 8. Klassen JA, Liang Y, Tjosvold L, Klassen TP, Hartling L. Music for pain and anxiety in children undergoing medical procedures: a systematic review of randomized controlled trials. Ambul Pediatr. 2008;8:117-28.
- 9. Berbel P, Moix J, Quintana S. Music versus diazepam to reduce preoperative anxiety: a randomized controlled clinical trial. Rev Esp Anestesiol Reanim. 2007;54:355-8.
- 10. Wong HL, Lopez-Nahas V, Molassiotis A. Effects of music therapy on anxiety in ventilator-dependent patients. Heart Lung. 2001;30:376-87.
- 11. Hatem TP, Lira PI, Mattos SS. The therapeutic effects of music in children following cardiac surgery. J Pediatr (Rio J). 2006;82:186-92.
- 12. Al-Qahtani NH. Foetal response to music and voice. Aust N Z J Obstet Gynaecol. 2005; 45:414-7.
- 13. Chang MY, Chen CH, Huang KF. Effects of music therapy on psychological health of women during pregnancy. J Clin Nurs. 2008;17:2580-7.
- 14. Phumdoung S, Good M. Music reduces sensation and distress of labor pain. Pain Manag Nurs. 2003;4:54-61.
- 15. Desquiotz-Sunnen N. Singing for preterm born infants music therapy in neonatology. Bull Soc Sci Med Grand Duche Luxemb. 2008; Spec No 1:131-43.
- 16. Chou LL, Wang RH, Chen SJ, Pai L. Effects of music therapy on oxygen saturation in premature infants receiving endotracheal suctioning. J Nurs Res. 2003;11:209-16.
- 17. Caine J. The effects of music on the selected stress behaviors, weight, caloric and formula intake, and length of hospital stay of premature and low birth weight neonates in a newborn intensive care unit. J Music Ther. 1991;28:180-92.
- 18. Whipple J. The effect of music-reinforced nonnutritive sucking on state of preterm, low birthweight infants experiencing heelstick. J Music Ther. 2008;45:227-72.
- 19. Nöcker-Ribaupierre, M. Music therapy for premature and newborn infants. Gilsum, NH: Barcelona Publishers; 2004.
- 20. Arnon S, Shapsa A, Forman L, Regev R, Bauer S, Litmanovitz I, et al. Live music is beneficial to preterm infants in the neonatal intensive care unit environment. Birth. 2006;33:131-6.
- 21. Krout RE. The effects of single-session music therapy interventions on the observed and self-reported levels of pain control, physical comfort, and relaxation of hospice patients. Am J Hosp Palliat Care. 2001;18:383-90.
Music therapy may increase breastfeeding rates among mothers of premature newborns: a randomized controlled trial
Publication Dates
-
Publication in this collection
27 Sept 2011 -
Date of issue
June 2011
History
-
Accepted
25 Jan 2011 -
Received
27 Sept 2010