Abstracts
BACKGROUND AND METHODS: Until recently, bupivacaine had been the anesthetic of choice for loco-regional blocks due to the quality and duration of the anesthesia. But its cardiovascular toxicity is a source of concern for anesthesiologists who seek new pharmacological options with a smaller degree of this problem. Its levorotatory isomer, levobupivacaine, that would be less cardiotoxic due a smaller affinity for the receptors of the sodium channels of the cardiac cell, is one of these options. In Brazil, a presentation containing 75% of the levorotatory isomer and 25% of the dextrorotatory isomer, called 50% enantiomeric excess mixture is available. The aim of this study was to evaluate the hemodynamic repercussions of the intravascular injection of a toxic dose of those three agents to determine which one has the least impact in the case of an accident. METHODS: Large White pigs were anesthetized with thiopental, intubated, and placed on mechanical ventilation. Hemodynamic monitoring was achieved with a Swan-Ganz catheter and invasive blood pressure. After a period of rest, the animals were randomly divided in three groups. The intoxication was performed, on a double-blind fashion, with 4 mg.kg-1 of one of the drugs. Hemodynamic parameters were evaluated during 30 minutes. Analytical tests were used to compare the results among the groups. RESULTS: The 50% enantiomeric excess mixture and levobupivacaine had greater hemodynamic repercussions than the racemic mixture, which were more pronounced with the first drug. These results go against those found in humans, especially regarding the pure levorotatory isomer, but are similar to recent results reported in animals. One should be careful when extrapolating the data obtained in pigs to humans and further studies are necessary. CONCLUSIONS: In pigs, the 50% enantiomeric excess mixture, in particular, and levobupivacaine were more toxic when administered intravenously than racemic bupivacaine.
ANESTHETICS, Local; ANIMAL; COMPLICATIONS
JUSTIFICATIVA E OBJETIVOS: Até recentemente, a bupivacaína tem sido o anestésico de escolha nos bloqueios locorregionais em razão da qualidade da anestesia proporcionada e pela sua duração. Apesar disso, sua toxicidade cardiovascular preocupa os anestesiologistas que procuram novas opções farmacológicas com menor grau desse inconveniente. Uma destas é o seu isômero levógiro, a levobupivacaína, que por uma menor afinidade aos receptores dos canais de sódio da célula cardíaca, seria menos cardiotóxica. Em nosso meio está disponível a apresentação contendo 75% do isômero levógiro e 25% do isômero dextrógiro, denominada mistura com excesso enantiomérico de 50%. O objetivo deste estudo foi avaliar as repercussões hemodinâmicas da injeção intravascular de dose tóxica desses três agentes, buscando encontrar qual deles tem menor impacto em caso de acidente. MÉTODO: Suínos da raça Large White foram anestesiados com tiopental, intubados e ventilados mecanicamente, sendo em seguida instalada monitorização hemodinâmica com cateter de Swan-Ganz e pressão invasiva para estudo das variáveis hemodinâmicas. Após repouso, foram divididos de forma aleatória em três grupos e realizada intoxicação duplamente encoberta com um dos agentes na dose de 4 mg.kg-1. Os resultados hemodinâmicos foram avaliados durante 30 minutos. Aos resultados foram aplicados testes estatísticos para comparação entre os grupos. RESULTADOS: A mistura com excesso enantiomérico de 50% e a levobupivacaína causaram maiores repercussões hemodinâmicas do que a mistura racêmica, sendo estas mais pronunciadas com o primeiro agente. Esses resultados se opõem aos encontrados em humanos, sobretudo quando da utilização do isômero levógiro puro, mas estão de acordo com resultados recentes também em animais. Extrapolar dados obtidos em suínos para seres humanos exige muita cautela e novos estudos são necessários. CONCLUSÔES: Em suínos, a mistura com excesso enantiomérico de 50% particularmente, e a levobupivacaína mostraram-se mais tóxicas quando administradas por via venosa do que a bupivacaína racêmica.
ANESTÉSICOS, Local; ANIMAL; COMPLICAÇÕES
JUSTIFICATIVA Y OBJETIVOS: La bupivacaína ha sido hasta hace poco tiempo el anestésico por elección en los bloqueos loco-regionales en razón de la calidad de la anestesia proporcionada y por su duración. A pesar de eso, su toxicidad cardiovascular preocupa a los anestesiólogos que buscan nuevas opciones farmacológicas con un menor grado de ese inconveniente. Una de ellas es su isómero levógiro, la levobupivacaína, que por una menor afinidad con los receptores de los canales de sodio de la célula cardiaca, sería menos cardiotóxica. En nuestro medio está disponible la presentación que contiene un 75% del isómero levógiro y un 25% del isómero dextrógiro, denominada mezcla con exceso enantiomérico de 50%. El objetivo de este estudio fue el de evaluar las repercusiones hemodinámicas de la inyección intravascular de dosis tóxica de esos tres agentes, buscando encontrar cuál de ellos registra un menor impacto en caso de accidente. MÉTODO: Cerdos de la raza Large White fueron anestesiados con tiopental, intubados y ventilados mecánicamente, siendo a continuación instalada la monitorización hemodinámica con catéter de Swan-Ganz y presión invasiva para estudio de las variables hemodinámicas. Después del reposo, fueron divididos aleatoriamente en tres grupos y realizada intoxicación doble encubierta con uno de los agentes en dosis de 4 mg.kg-1. Los resultados hemodinámicos fueron evaluados durante 30 minutos. A los resultados se les aplicó pruebas estadísticas para la comparación entre los grupos. RESULTADOS: La mezcla con exceso enantiomérico de 50% y la levobupivacaína causaron mayores repercusiones hemodinámicas que la mezcla racémica, siendo esas más fuertes con el primer agente. Esos resultados se oponen a los ya encontrados en humanos, particularmente cuando se utiliza el isómero levógiro puro, pero están a tono con los resultados recientes también obtenidos en animales. Rebasar los datos obtenidos en cerdos con los obtenidos en seres humanos, exige mucha cautela y nuevos estudios se hacen necesarios. CONCLUSIONES: En cerdos, la mezcla con exceso enantiomérico de 50% particularmente, y la levobupivacaína fueron más tóxicas cuando se administraron por vía venosa que la bupivacaína racémica.
SCIENTIFIC ARTICLE
Hemodynamic effects of the acute intoxication with bupivacaine, levobupivacaine and 50% enantiomeric excess mixture. An experimental study in pigs* * Received from Laboratório de Anestesia Experimental do Núcleo de Medicina e Cirurgia Experimental da Faculdade de Ciências Médicas da Universidade Estadual de Campinas (FCM/UNICAMP), Campinas, SP
Efectos hemodinámicos de la intoxicación aguda con bupivacaína, levobupivacaína y mezcla con exceso enantiomérico de 50%. Estudio experimental en cerdos
Artur Udelsmann, TSAI; Sílvia Elaine Rodolfo de Sá LorenaII; Samira Ubaid GirioliIII; William Adalberto SilvaIV; Ana Cristina de MoraesIV
IProfessor-Doutor do Departamento de Anestesiologia FCM/UNICAMP; Laboratório de Anestesia Experimental do Núcleo de Medicina e Cirurgia Experimental da FCM/UNICAMP
IIPós-Graduanda do Departamento de Cirurgia da FCM/UNICAMP
IIIMédica Cardiologista, Pós-Graduanda do Departamento de Farmacologia da FCM/UNICAMP
IVBiólogo do Núcleo de Medicina e Cirurgia Experimental da FCM/UNICAMP
Correspondence to Correspondence to: Dr. Artur Udelsmann Av. Prof. Atílio Martini, 213 13083-830 Campinas SP E-mail: audelsmann@yahoo.com.br
SUMMARY
BACKGROUND AND METHODS: Until recently, bupivacaine had been the anesthetic of choice for loco-regional blocks due to the quality and duration of the anesthesia. But its cardiovascular toxicity is a source of concern for anesthesiologists who seek new pharmacological options with a smaller degree of this problem. Its levorotatory isomer, levobupivacaine, that would be less cardiotoxic due a smaller affinity for the receptors of the sodium channels of the cardiac cell, is one of these options. In Brazil, a presentation containing 75% of the levorotatory isomer and 25% of the dextrorotatory isomer, called 50% enantiomeric excess mixture is available. The aim of this study was to evaluate the hemodynamic repercussions of the intravascular injection of a toxic dose of those three agents to determine which one has the least impact in the case of an accident.
METHODS: Large White pigs were anesthetized with thiopental, intubated, and placed on mechanical ventilation. Hemodynamic monitoring was achieved with a Swan-Ganz catheter and invasive blood pressure. After a period of rest, the animals were randomly divided in three groups. The intoxication was performed, on a double-blind fashion, with 4 mg.kg-1 of one of the drugs. Hemodynamic parameters were evaluated during 30 minutes. Analytical tests were used to compare the results among the groups.
RESULTS: The 50% enantiomeric excess mixture and levobupivacaine had greater hemodynamic repercussions than the racemic mixture, which were more pronounced with the first drug. These results go against those found in humans, especially regarding the pure levorotatory isomer, but are similar to recent results reported in animals. One should be careful when extrapolating the data obtained in pigs to humans and further studies are necessary.
CONCLUSIONS: In pigs, the 50% enantiomeric excess mixture, in particular, and levobupivacaine were more toxic when administered intravenously than racemic bupivacaine.
Key Words: ANESTHETICS, Local: bupivacaine, 50% enantiomeric excess mixture, levobupivacaine; ANIMAL: pig; COMPLICATIONS: hemodynamic.
RESUMEN
JUSTIFICATIVA Y OBJETIVOS: La bupivacaína ha sido hasta hace poco tiempo el anestésico por elección en los bloqueos loco-regionales en razón de la calidad de la anestesia proporcionada y por su duración. A pesar de eso, su toxicidad cardiovascular preocupa a los anestesiólogos que buscan nuevas opciones farmacológicas con un menor grado de ese inconveniente. Una de ellas es su isómero levógiro, la levobupivacaína, que por una menor afinidad con los receptores de los canales de sodio de la célula cardiaca, sería menos cardiotóxica. En nuestro medio está disponible la presentación que contiene un 75% del isómero levógiro y un 25% del isómero dextrógiro, denominada mezcla con exceso enantiomérico de 50%. El objetivo de este estudio fue el de evaluar las repercusiones hemodinámicas de la inyección intravascular de dosis tóxica de esos tres agentes, buscando encontrar cuál de ellos registra un menor impacto en caso de accidente.
MÉTODO: Cerdos de la raza Large White fueron anestesiados con tiopental, intubados y ventilados mecánicamente, siendo a continuación instalada la monitorización hemodinámica con catéter de Swan-Ganz y presión invasiva para estudio de las variables hemodinámicas. Después del reposo, fueron divididos aleatoriamente en tres grupos y realizada intoxicación doble encubierta con uno de los agentes en dosis de 4 mg.kg-1. Los resultados hemodinámicos fueron evaluados durante 30 minutos. A los resultados se les aplicó pruebas estadísticas para la comparación entre los grupos.
RESULTADOS: La mezcla con exceso enantiomérico de 50% y la levobupivacaína causaron mayores repercusiones hemodinámicas que la mezcla racémica, siendo esas más fuertes con el primer agente. Esos resultados se oponen a los ya encontrados en humanos, particularmente cuando se utiliza el isómero levógiro puro, pero están a tono con los resultados recientes también obtenidos en animales. Rebasar los datos obtenidos en cerdos con los obtenidos en seres humanos, exige mucha cautela y nuevos estudios se hacen necesarios.
CONCLUSIONES: En cerdos, la mezcla con exceso enantiomérico de 50% particularmente, y la levobupivacaína fueron más tóxicas cuando se administraron por vía venosa que la bupivacaína racémica.
INTRODUCTION
Some anesthetic procedures require large doses of local anesthetics and there is always the risk of toxic reactions, especially in the cardiovascular and central nervous systems, in case of an accidental intravascular injection. Due to the quality of the anesthesia and the prolonged action, bupivacaine is one of the local anesthetics used more often 1,2. However, since the publication in 1979 of the Anesthesiology editorial on the severe cardiovascular effects of the intoxication with this drug 3, several studies have been conducted to find new long-acting local anesthetics with reduced toxic potential. Although bupivacaine is synthesized in the form of two isomers, dextrorotatory R(+) and levorotatory L(-) 4, until recently it was commercialized only in the racemic presentation, which contains 50% of each isomer. However, it is known, since 1972, that the levorotatory isomer is less toxic 5,6. Recently, this levorotatory isomer, known as levobupivacaine, became the focus of several studies and, in animal models, it has been shown that its lethal dose would be up to 1.6 times greater than that of the racemic mixture 7! In humans, levobupivacaine would have a smaller negative inotropic effect and would cause a smaller increase in the PR and QT intervals in the electrocardiogram, characteristics of the racemic intoxication. However, although this new agent presents the same analgesic potency 8, it is not devoid of problems: decreased motor blockade 9. For this reason, besides levobupivacaine, the pharmaceutical industry also manufactures a product with 75% of the levorotatory isomer and 25% of the dextrorotatory isomer, known as "50% enantiomeric excess mixture". Since this is a genuinely national product, the aim of this study was to determine its hemodynamic impact in case of an accidental intoxication, and to compare it with the intoxication with levobupivacaine and the racemic mixture.
METHODS
After approval by the Animal Experiment Ethics Committee of UNICAMP, 60 healthy Large White pigs of both genders, with weight ranging between 17 and 29 kg, were submitted to the following protocol:
The results of the categorical variables were analyzed by the Chi-square test and, whenever necessary, Fisher Exact test. One-way ANOVA was used to compare the distribution of the continuous variables in one moment, while the ANOVA was used to study the continuous variables measured in several moments. A level of 5%, i.e., p < 0.05 was considered significant; results between 5% and 10% were considered a tendency.
RESULTS
Table I shows the mean and standard deviation of the weight, body surface area, hematocrit, and hemoglobin of the three groups.
The groups were homogenous regarding gender (p = 0.803), weight (p = 0.88), hematocrit (p = 0.58), hemoglobin (p = 0.2), and body surface area (p = 0.91). There were no differences in hemodynamic parameters at rest among the groups.
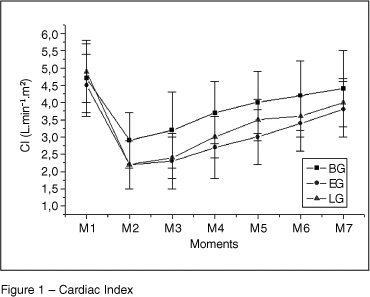
After the intoxication, the cardiac index (Figure 1) was reduce in all three groups, but it was more pronounced in EG and LG (p = 0.0051). The values in BG were higher than EG until M6 and than LG until M4 (p = 0.0001).
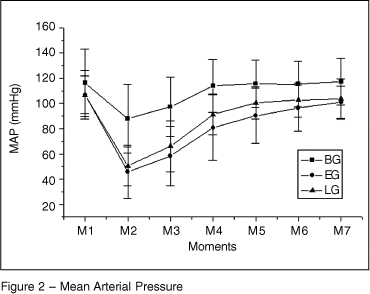
Mean arterial pressure (Figure 2) demonstrated a marked reduction in the three groups at M2, but it was more pronounced in EG and LG. The bupivacaine group had higher values than the other two groups until M7 (p = 0.0001). Blood pressure returned to baseline values in BG at M4, in LG at M5, and in EG at M6 (p = 0.0001).
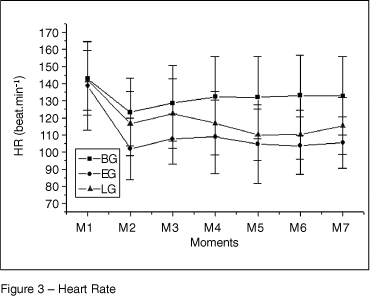
After the intoxication the heart rate (Figure 3) decreased in all three groups, and this difference was maintained until the end of the experiment (p = 0.0001). In EG this reduction had a sustained statistically significant difference when compared with BG until the end of the experiment, and until M3 when compared with LG (p = 0.0007).
Central venous pressure (Figure 4) showed a marked increase in the three groups after intoxication (p = 0.0001); however, it was more pronounced in EG and LG. The difference between EG and BG persisted throughout the experiment, while the difference between LG and BG persisted until M5 and from then on both groups had similar parameters (p = 0.0311).
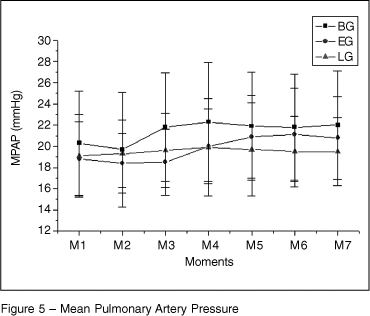
There were no differences in MPAP (Figure 5) between the groups but, from M4 on the results were different than those at rest for the three groups (p = 0.0001).
Pulmonary capillary pressure (Figure 6) in the three groups at M2 was different than at M1; this change persisted until the end of the experiment (p = 0.0001) but without differences among the groups.
There was a marked reduction in the work index (Figure 7) in the three groups from M2 to M5 (p = 0.0001). Statistical analysis demonstrated that LG values were smaller than BG values until M3 (p = 0.001).
The systemic vascular resistance index (Figure 8) showed important variations after the intoxication in all three groups (p = 0.0001). It was more pronounced in LG than in EG but in BG it showed a slight increment. There was a significant difference between BG and LG and EG at M2 and M3 (p = 0.0463).
The pulmonary vascular resistance index (Figure 9) was higher than at rest from M2 on (p = 0.0001) but there were no significant differences among the groups.
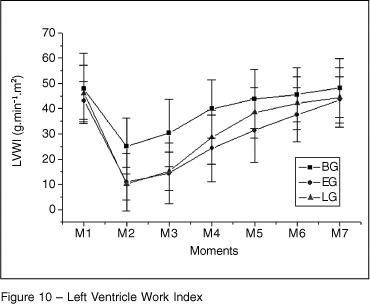
The left ventricle work index (Figure 10) showed a marked reduction in the three groups after intoxication (p = 0.0001), and this reduction persisted until M4 in BG and until M5 in LG and EG (p = 0.0001). Comparing the groups, BG was higher than EG until M6 and higher than LG until M4; LG was higher than EG at M5 (p = 0.0005).
The right ventricle work index (Figure 11) was also decreased after the intoxication and remained so in BG until M3, in LG until M4, and in EG until M5 (p = 0.0001). The values in LG and EG were significantly inferior to BG until M5 (p = 0.0006).
DISCUSSION
Levobupivacaine causes less motor blockade than the racemic mixture 7,14-17 the reason why the interest in adding a small amount of the dextrorotatory isomer to reduce this effect 16. The national industry synthesized this product and since then it has been widely used, because it is also considered less toxic. Since this presentation is available only in Brazil, the aim of this study was to determine its cardiotoxicity in pigs, comparing it to racemic bupivacaine and levobupivacaine. The decreased toxicity of the S(-) isomer would be a consequence of its decreased affinity for the sodium channels of the cardiac cells, inferior to that of the R(+) isomer 18, which had been demonstrated in animals. Such data should be considered with caution before extrapolating to humans. Like to the animal data of other authors comparing levobupivacaine, racemic bupivacaine, and ropivacaine showing that levobupivacaine had similar 19, or even greater, toxicity20,21, our results demonstrated that the hemodynamic consequences of the 50% enantiomeric excess mixture were more pronounced, followed by levobupivacaine and racemic bupivacaine in case of an acute intoxication in pigs, similar to the accidental administration of the drug during loco-regional anesthesia in humans. This is evident in the marked reduction of the cardiac index, mean blood pressure, heart rate, and left ventricle work load. These results confirm the data obtained previously comparing racemic bupivacaine and 50% enantiomeric excess mixture in dogs 22. Animal results should be analyzed carefully and their extrapolation to humans demand caution. However, these results allow for some reflections and should stimulate further studies, since this is the second series with similar results. The accidental intravenous administration of high doses, with toxic reactions, when applying loco-regional anesthesia have decreased drastically in the last 30 years, from 0.2% to 0.01%, and peripheral nerve blocks account for the majority of the cases (7.5 per 10.000) 23. Such reflections should encourage renewed efforts at developing drugs and techniques that would allow the morbidity and mortality to be closer to zero. This purpose is aimed at protecting patients from undesirable and unforeseen effects resulting from loco-regional anesthetic techniques with high doses of local anesthetics and, therefore, protecting the anesthesiologist, avoiding the consequences of legal actions that are so common nowadays.
ACKNOWLEDGEMENTS
To the Cristália Laboratory.
REFERENCES
Submitted em 08 de maio de 2006
Accepted para publicação em 27 de novembro de 2006
- 1. Groban L, Deal DD, Vernon JC et al - Cardiac resuscitation after incremental overdosage with lidocaine, bupivacaine, levobupivacaine, and ropivacaine in anesthetized dogs. Anesth Analg 2001;92:37-43.
- 2. Chang DH-T, Ladd LA, Copeland S et al - Direct cardiac effects of intracoronary bupivacaine, levobupivaciane and ropivacaine in the sheep. Br J Pharmacol 2001;132:649-658.
- 3. Albright GA - Cardiac arrest following regional anesthesia with etidocaine or bupivacaine. Anesthesiology 1979;51:285-287.
- 4. Ohmura S, Kawada M, Ohta T et al - Systemic toxicity and resusciation in bupivacaine, levobupivacaine, or ropivacaine-infused rats. Anesth Analg 2001;93:743-748.
- 5. Åberg G - Toxicological and local anaesthetic effects of optically active isomers of two local anaesthetic compounds. Acta Pharmacol Toxicol 1972;31:273-286.
- 6. Luduena FP, Bogado EF, Tullar BF - Optical isomers of mepivacaine and bupivacaine. Arch Int Pharmacodyn 1972; 200:359-369.
- 7. Foster RH, Markham A - Levobupivacaine. A review of its pharmacology and use as a local anaesthetic. Drugs 2000; 59:551-579.
- 8. Lyons G, Columb M, Wilson RC et al. - Extradural pain relief in labour:potencies of levobupivacaine and racemic bupivacaine. Br J Anaesth, 1998;81:899-901.
- 9. Héctor JL, Columb MO: The relative motor blocking potencies of bupivacaine and levobupivacaine in labour. Anesth Analg, 2003;97:1509-1513.
- 10. Bardsley H, Gristwood R, Baker H et al - A comparison of the cardiovascular effects of levobupivacaine and rac-bupivacaine following intravenous administration to healthy volunteers. Br Clin Pharmacol 1998;46:245-249.
- 11. Smith AC, Ehler WJ, Swindle MMl - Anesthesia and Analgesia in Swine, em: Kohn DF, Wixson SK, White WJ et al - Anesthesia and Analgesia in Laboratory Animals, 1st ed., New York, Academic Press,1997;313-336.
- 12. Ettinger SJ: Textbook of Veterinary Internal Medicine, 1st ed., Philadelphia, WB Saunders, 1975
- 13. Lefrant JY, Muller L, de La Coussaye JE et al - Hemodynamic and cardiac electrophysiologic effects of lidocaine-bupivacaine mixture in anesthetized and ventilated piglets. Anesthesiology 2003;98:96-103.
- 14. Delfino J, Vale NB do - Bupivacaína levógira a 0,5% pura versus mistura enantiomérica de bupivacaína (S75-R25) a 0,5% em anestesia peridural para cirurgia de varizes. Rev Bras Anestesiol 2001;51:474-481.
- 15. Tanaka PP, Souza RO, Salvalaggio MF et al - Estudo comparativo entre bupivacaína a 0,5% e a mistura enantiomérica de bupivacaína (S75-R25) a 05% em anestesia peridural em pacientes submetidos a cirurgia ortopédica de membros inferiores. Rev Bras Anestesiol 2003;53: 331-337.
- 16. Gonçalves RF, Lauretti GR, Mattos Al - Estudo comparativo entre bupivacaína 0,5% e mistura enantiomérica de bupivacaína (S75-R25) em anestesia peridural. Rev Bras Anestesiol 2003;53:169-176.
- 17. Lacassie HJ, Columb MO - The relative motor blocking potencies of bupivacaine and levobupivacaine in labor. Anesth analg 2003;97:1509-1513.
- 18. Valenzuela C, Snyders DJ, Bennett PB et al - Stereoselectivite block of cardiac sodium channels by bupivacaine in guinea pig ventricular myocytes. Circulation 1995;92:3014-3024.
- 19. Royse CF, Royse AG - The myocardial and vascular effects of bupivacaine, levobupivacaine, and ropivacaine using pressure volume loops. Anesth Analg 2005;101:679-687.
- 20. Masuda R, Takeda S, Yoshii S et al. - Levobupivacaine exerts the most detrimental effect on the cardiovascular system among enantiomers of bupivacaína in anesthetized dogs. Anesthesiology 2004;101:A652.
- 21. Jung CW, Lee KH, Choe YS et al. - Comparison of resuscitative effect of insulin between bupivacaine and levobupivacaine induced cardiovascular collapse in dogs. Anesthesiology 2004; 101:A649.
- 22. Udelsmann A, Munhoz DC, Silva WA et al - Comparação entre os efeitos hemodinâmicos da intoxicação aguda com bupivacaína racêmica e a mistura com excesso enatiomérico de 50% (S75-R25). Estudo experimental em cães. Rev Bras Anestesiol 2006;56:391-401.
- 23. Cox B, Durieux ME, Marcus MA - Toxicity of local anaesthetics. Best Pract Res Clin Anaesthesiol 2003;17:111-136.
Publication Dates
-
Publication in this collection
19 Jan 2007 -
Date of issue
Feb 2007
History
-
Received
08 May 2006 -
Accepted
27 Nov 2006