Abstracts
BACKGROUND AND OBJECTIVES: Spinal anesthesia may cause hemodynamic changes due to factors related or not to the patient. The density of the anesthetic compared to the CSF, which interferes with the number of dermatomes blocked and, consequently, with the level of the sympathetic blockade and reduction in blood pressure (BP), is one of those factors. The objective of this study was to evaluate the dispersion of 0.5% hypobaric bupivacaine prepared aseptically in a laboratory, with controlled and uniform density. METHODS: Thirty patients, physical status ASA I, II, or III, ages ranging from 18 to 60 years, without cardiovascular comorbidities, who underwent orthopedic surgery of the lower limb, were enrolled in this study. They were sedated with diazepam, 0.03 mg.kg-1, placed in lateral decubitus, with the side to be operated on top. A lumbar puncture in the L3-L4 space was performed with a 27G Quincke needle, and the direction of the bevel and rate of injection were standardized. The sensitive and motor levels (modified Bromage scale) were evaluated. RESULTS: At the end of the surgery, two patients (6.6%) did not present a level 3 motor blockade in the Bromage scale, and the sensitive blockade varied from T4 to T12. Only 12.9% of the patients presented a level of sensitive blockade considered "high" for the proposed surgery (above T6). The reduction in blood pressure was statistically significant, but it did not fall below 20% of basal levels and, therefore, was not clinically significant. The change in heart rate was non-significant. CONCLUSIONS: It was demonstrated that 0.5% hypobaric bupivacaine is a safe choice, with little hemodynamic repercussion in orthopedic surgeries of the lower limbs. The mean duration of the anesthesia, 250 minutes, allows the realization of minor and medium orthopedic procedures.
ANESTHETICS, Local; ANESTHETIC TECHNIQUES, Regional
JUSTIFICATIVA E OBJETIVOS: A raquianestesia causa alterações hemodinâmicas relacionadas com fatores próprios do paciente ou não. Um dos fatores é a densidade do anestésico em relação ao líquor, interferindo no número de dermátomos bloqueados e, conseqüentemente, no nível do bloqueio simpático e na diminuição da pressão arterial (PA). O objetivo do estudo foi avaliar a dispersão da bupivacaína hipobárica a 0,5%, preparada assepticamente em laboratório e com uma densidade controlada e uniforme. MÉTODO: Trinta pacientes, ASA I, II ou III, com idade entre 18 e 60 anos, sem comorbidades circulatórias, submetidos a operações ortopédicas no membro inferior participaram do estudo. Eles foram sedados com diazepam 0,03 mg.kg-1, posicionados em decúbito lateral com o lado a ser operado para cima, e puncionados entre L3-L4, com agulha de Quincke 27G, sendo padronizados o direcionamento do bisel e a velocidade de injeção. Foram avaliados os níveis sensitivos e motor (escala modificada de Bromage). RESULTADOS: Ao fim da operação, dois pacientes (6,6%) não apresentaram bloqueio motor classificado como 3 na escala de Bromage, com o bloqueio sensitivo variando entre T4 e T12. Somente 12,9% dos pacientes apresentaram nível sensitivo considerado "alto" para a operação proposta (acima de T6). A diminuição da pressão arterial foi significativa sob o ponto de vista estatístico, sem atingir 20% abaixo dos valores basais, portanto, sem significância clínica. A variação da freqüência cardíaca não foi significativa. CONCLUSÕES: A bupivacaína hipobárica a 0,5% mostrou ser uma opção segura e com poucas repercussões hemodinâmicas para operações ortopédicas nos membros inferiores. A duração média observada, de 250 minutos, possibilita a realização de procedimentos ortopédicos de até médio porte.
ANESTÉSICOS, Local; TÉCNICA ANESTÉSICA, Regional
JUSTIFICATIVA Y OBJETIVOS: La anestesia espinal causa alteraciones hemodinámicas relacionadas a factores propios del paciente o no. Uno de los factores es la densidad del anestésico con relación al líquor, interfiriendo en el número de dermátomos bloqueados y consecuentemente en el nivel del bloqueo simpático y la disminución de la presión arterial (PA). El objetivo del estudio fue el de evaluar la dispersión de la bupivacaína hipobárica a 0,5%, preparada asépticamente en laboratorio y con una densidad controlada y uniforme. MÉTODO: Treinta pacientes, ASA I, II o III, con edad entre 18 y 60 anos, sin comorbidades circulatorias, sometidos a operaciones ortopédicas en el miembro inferior participaron en el estudio. Se sedaron con diazepam 0,03 mg.kg-1, posicionados en decúbito lateral con el lado a ser operado para arriba, y puncionados entre L3-L4, con aguja de Quincke 27G, siendo estandarizados con bisel y a velocidad de inyección. Se evaluaron los niveles sensitivos y motor (escala modificada de Bromage). RESULTADOS: Al final de la operación, de los pacientes (6,6%) no presentaron bloqueo motor clasificado como 3 en la escala de Bromage, con el bloqueo sensitivo variando entre T4 y T12. Solamente 12,9% de los pacientes presentaron nivel sensitivo considerado "alto" para la operación propuesta (por encima de T6). La disminución de la presión arterial fue significativa bajo el punto de vista estadístico, sin llegar al 20% por debajo de los valores basales, por tanto sin significancia clínica. La variación de la frecuencia cardiaca no fue significativa. CONCLUSIONES: La bupivacaína hipobárica a 0,5% mostró ser una opción segura, y con pocas repercusiones hemodinámicas para operaciones ortopédicas en los miembros inferiores. La duración promedio observada, de 250 minutos, posibilita la realización de procedimientos ortopédicos de medio porte.
SCIENTIFIC ARTICLE
Evaluation of 0.5% hypobaric bupivacaine in spinal anesthesia* * Received from Hospital Universitário Clementino Fraga Filho da Universidade Federal do Rio de Janeiro (HUCFF/UFRJ), RJ
Evaluación de la bupivacaína hipobárica a 0,5% en la anestesia espinal
Marcelo Cursino Pinto dos SantosI; Eduardo KawanoII; Ronaldo Contreiras Oliveira Vinagre, TSAIII; Rosangela Aparecida M. NoéIV
IME3 do CET/SBA Prof. Bento Gonçalves do HUCFF/UFRJ
IIAnestesiologista do Serviço de Anestesiologia da Associação Beneficente Santa Casa de Campo Grande
IIICo-Responsável pelo CET/SBA Prof. Bento Gonçalves do HUCFF/UFRJ
IVEstatística da Comissão de Investigação Científica do HUCFF/UFRJ
Correspondence to Correspondence to: Dr. Marcelo Cursino Pinto dos Santos Rua Conde de Bonfim, 1.156/404 Tijuca 20530-003 Rio de Janeiro, RJ E-mail: m_cursino@yahoo.com.br
SUMMARY
BACKGROUND AND OBJECTIVES: Spinal anesthesia may cause hemodynamic changes due to factors related or not to the patient. The density of the anesthetic compared to the CSF, which interferes with the number of dermatomes blocked and, consequently, with the level of the sympathetic blockade and reduction in blood pressure (BP), is one of those factors. The objective of this study was to evaluate the dispersion of 0.5% hypobaric bupivacaine prepared aseptically in a laboratory, with controlled and uniform density.
METHODS: Thirty patients, physical status ASA I, II, or III, ages ranging from 18 to 60 years, without cardiovascular comorbidities, who underwent orthopedic surgery of the lower limb, were enrolled in this study. They were sedated with diazepam, 0.03 mg.kg-1, placed in lateral decubitus, with the side to be operated on top. A lumbar puncture in the L3-L4 space was performed with a 27G Quincke needle, and the direction of the bevel and rate of injection were standardized. The sensitive and motor levels (modified Bromage scale) were evaluated.
RESULTS: At the end of the surgery, two patients (6.6%) did not present a level 3 motor blockade in the Bromage scale, and the sensitive blockade varied from T4 to T12. Only 12.9% of the patients presented a level of sensitive blockade considered "high" for the proposed surgery (above T6). The reduction in blood pressure was statistically significant, but it did not fall below 20% of basal levels and, therefore, was not clinically significant. The change in heart rate was non-significant.
CONCLUSIONS: It was demonstrated that 0.5% hypobaric bupivacaine is a safe choice, with little hemodynamic repercussion in orthopedic surgeries of the lower limbs. The mean duration of the anesthesia, 250 minutes, allows the realization of minor and medium orthopedic procedures.
Key Words: ANESTHETICS, Local: bupivacaine; ANESTHETIC TECHNIQUES, Regional: hypobaric spinal block.
RESUMEN
JUSTIFICATIVA Y OBJETIVOS: La anestesia espinal causa alteraciones hemodinámicas relacionadas a factores propios del paciente o no. Uno de los factores es la densidad del anestésico con relación al líquor, interfiriendo en el número de dermátomos bloqueados y consecuentemente en el nivel del bloqueo simpático y la disminución de la presión arterial (PA). El objetivo del estudio fue el de evaluar la dispersión de la bupivacaína hipobárica a 0,5%, preparada asépticamente en laboratorio y con una densidad controlada y uniforme.
MÉTODO: Treinta pacientes, ASA I, II o III, con edad entre 18 y 60 anos, sin comorbidades circulatorias, sometidos a operaciones ortopédicas en el miembro inferior participaron en el estudio. Se sedaron con diazepam 0,03 mg.kg-1, posicionados en decúbito lateral con el lado a ser operado para arriba, y puncionados entre L3-L4, con aguja de Quincke 27G, siendo estandarizados con bisel y a velocidad de inyección. Se evaluaron los niveles sensitivos y motor (escala modificada de Bromage).
RESULTADOS: Al final de la operación, de los pacientes (6,6%) no presentaron bloqueo motor clasificado como 3 en la escala de Bromage, con el bloqueo sensitivo variando entre T4 y T12. Solamente 12,9% de los pacientes presentaron nivel sensitivo considerado "alto" para la operación propuesta (por encima de T6). La disminución de la presión arterial fue significativa bajo el punto de vista estadístico, sin llegar al 20% por debajo de los valores basales, por tanto sin significancia clínica. La variación de la frecuencia cardiaca no fue significativa.
CONCLUSIONES: La bupivacaína hipobárica a 0,5% mostró ser una opción segura, y con pocas repercusiones hemodinámicas para operaciones ortopédicas en los miembros inferiores. La duración promedio observada, de 250 minutos, posibilita la realización de procedimientos ortopédicos de medio porte.
INTRODUCTION
Spinal anesthesia has different effects in the organism; some are desirable while others are not. Among the most important alterations is the reduction in blood pressure secondary to a reduction in venous return, reflex vasodilation, and increased venous capacitance, which occurs in approximately 30% of the patients 1-3.
In general, it is believed and hoped that the restricted, unilateral, sympathetic block of a few metameres during the spinal anesthesia causes less severe hemodynamic changes 1,3. This better control of the blood pressure could provide more stable cardiovascular parameters than those observed during isobaric spinal anesthesia when both lower limbs are anesthetized simultaneously, or even in hyperbaric spinal anesthesia when the patient is not placed in lateral decubitus after the block 1.
Another advantage described is the possibility that such blocks would be more "intense" and more prolonged, which is very useful in unexpectedly long surgeries 4,5.
The objective of this study was to observe the dispersion of 0.5% hypobaric bupivacaine in the subarachnoid space and its anesthetic action in both lower limbs, observing the latency of the motor and sensitive blockades in each limb during the first 20 minutes after the injection of the anesthetic, and the hemodynamic changes during this period, while the patients were still in lateral decubitus. Changes in blood pressure and heart rate were also observed during the following 60 minutes, as well as the duration of the sensitive and motor blockades.
METHODS
After approval by the Research Ethics Committee of the Hospital Universitário Clementino Fraga Filho of the UFRJ, 30 patients, scheduled for orthopedic surgeries of the lower limbs, were invited and, after reading and signing the informed consent, agreed to participate in the study.
This was a non-comparative, descriptive study, on the efficiency profile of an anesthetic and its side effects, after industrial preparation at the time it was going to be used. A pilot study was undertaken with 10 patients, observing the low variability in the hemodynamic measurements, duration of the motor and sensitive blockades, and low frequency of adverse effects (~20%). This indicated that, statistically, a homogenous population (coefficient of variation CV < 30%) would need at least 30 (thirty) patients.
The inclusion criteria included ages 18 to 60 years, height of 165 to 175 cm, and patients with physical status ASA I, II or III. Patients with signs or symptoms compatible with hypovolemia, coagulation disorders, infections, important anatomical changes of the spine (kyphosis or scoliosis), and any other change that would constitute a counter indication to subarachnoid blockade were not included in the study, as well as patients who refused to participate. In those patients, the routine anesthetic procedure for the surgeries proposed was used.
Intraoperative monitoring consisted of a cardioscope, non-invasive blood pressure, and pulse oxymetry. Ten minutes before the blockade, patients were sedated with intravenous diazepam, at a maximal dose of 0.03 mg.kg-1. After preparing the region with 70% alcohol, a subarachnoid puncture was performed in the L3-L4 space, using the paramedian approach, with the patient in the lateral decubitus, with the limb to be operated on top. A 27G Quincke needle, with the bevel directed towards the lower limb, was used. We used 0.5% hypobaric bupivacaine (density at 20° = 0.999 g.mL-1), prepared and stored in sterile conditions especially for this study, guaranteeing the uniformity of the density in every ampoule (Laboratório Cristália, São Paulo, Brazil). The aim was to maintain the safety of the mixture, eliminating the possibility of contamination during preparation, besides the variations produced by the manipulation by the anesthesiologist, especially regarding the different densities, caused by several reasons, but mainly by syringes that are not properly graduated, visual difficulty, and tremors of the person preparing the solution at the time of administration.
A total volume of 3 mL (15 mg) was administered, and CSF was not aspirated nor the needle cleaned at the time of the injection of the anesthetic; the patient was maintained in lateral decubitus for 20 minutes, and afterwards placed on dorsal decubitus. During the time they remained in lateral decubitus, patients were hydrated with 10 mL.kg-1 of Ringer's lactate.
The level of the sensitive blockade was assessed by pinprick sensitivity with a 27G needle; the motor blockade was evaluated by the modified Bromage scale (0 = no motor blockade; 1 = able to overcome gravity, but cannot overcome resistance; 2 = able to move the limb, but unable to overcome gravity; and 3 = complete motor blockade). Those parameters were evaluated in the first 20 minutes, while the patient was in lateral decubitus (M1 evaluation immediately after the blockade; M2 at 5 minutes; M3 at 10 minutes; M4 at 15 minutes; and M5 at 20 minutes). In the following 60 minutes, those parameters were evaluated every 5 minutes. Evaluation in the recovery room was done every 15 minutes until the total regression of the blockade.
The maximal level of the sensitive blockade was that obtained at 20 minutes. The complete return of sensitivity and full range of motion of the limb were considered as the end of the sensitive and motor blockades, respectively.
Blood pressure and heart rate were evaluated during the first 20 minutes and, in the following 60 minutes, at 5-minute intervals. Intravenous ephedrine, at a dose of 5 mg, was administered when a fall in systolic blood pressure was greater than 30% of baseline values; intravenous atropine (0.5 mg) was administered when the heart rate fell below 50 bpm.
Any intercurrence during and after the anesthetic-surgical procedure was recorded.
RESULTS
Table I presents the demographic data and the mean duration of the surgeries.
The motor blockade evolved gradually during the first twenty minutes, without the presence of a grade 3 motor blockade in the totality of the patients, even at the 20th minute. At the end of the surgery, two patients (6.6%) did not present motor blockade with the maximal classification in the modified Bromage scale, i.e., they did not present motor blockade in both lower limbs. At the end of the surgery, these two patients received a classification 2. The majority of patients (83.9%) presented complete motor blockade in both legs only after the 20th minute after the injection; when placed in dorsal decubitus, there was an exacerbation of the blockade in the leg that had remained inferior. Up to the 20th minute, while the patients remained in lateral decubitus, the inferior leg did not show any signs of motor blockade with an intensity comparable to that of the superior leg, what was to be expected. The mean duration of the motor blockade was 245.5 minutes with a standard deviation of ± 66.5 minutes. Table II shows the distribution of the motor level achieved in the superior leg.
Regarding the sensitive blockade, the level varied from T4 to T12 in the anterior aspects of patients, i.e., in the region facing up, with a wide variation at the end of the first 20 minutes, which was considered the endpoint of the evaluation. Considering that the surgeries were performed on the lower limbs, the minority of those patients presented sensitive levels considered unnecessarily "high" (only 12.9% of the patients showed a sensitive level equal or above T6). Thus, we did not achieve sympathetic blockade capable of causing hemodynamic instability during the procedures. Table III shows the sensitive levels achieved in the superior metameres.
The duration of the sensitive blockade in the upper leg was of 257.4 ± 105.6 minutes, until the total reversion of the motor blockade. Table IV shows the variation of the hemodynamic parameters in the first 20 minutes.
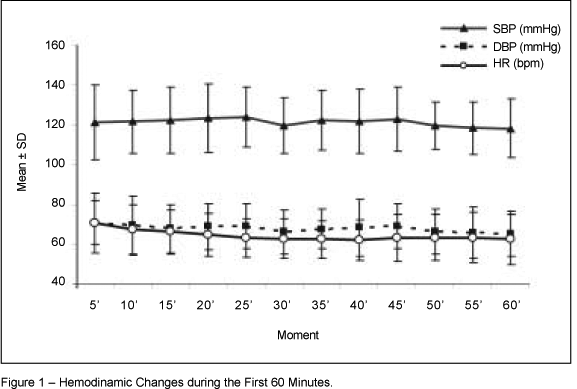
As for the hemodynamic values in the following 60 minutes, the variation in blood pressure was statistically significant. It showed a reduction in systolic blood pressure (SBP), p = 0.008, and in diastolic blood pressure (DBP), p = 0.004. However, it did not reach a 30% fall of baseline values, and was not considered clinically significant. The variation in heart rate (HR) was not statistically significant compared with baseline values (p = 0.092). We used the paired test t Student for those analyses. Figure 1 shows the hemodynamic variations.
Three patients developed hypotension, with a drop in blood pressure greater than 30% of baseline, being treated with fractionated doses of intravenous ephedrine, up to a total of 15 mg. Three patients developed hypotension with nausea; two of them were treated with intravenous ephedrine, up to a total dose of 20 mg. The other patient had bradycardia simultaneously, and was treated with atropine (0.75 mg), which reversed the bradycardia, and was posteriorly treated with a 5 mg dose of ephedrine.
DISCUSSION
Spinal anesthesia with hypobaric drugs has been used for a long time in several types of surgeries. Its use is widespread, especially in anal-rectal proctologic surgeries using the jackknife position, which restricts the anesthetic to the surgical field, with restrict motor blockade and little hemodynamic repercussion. Similar to other forms of subarachnoid block, it can also be used in outpatient anesthesia, allowing the patient to be discharged home on the same day 6-8.
Besides the perineal and orificial, anal-rectal surgeries, it is also widely used in orthopedic surgeries ranging from knee and pelvis arthroscopy to major surgeries of the hips. Vascular and gynecological surgeries, and cesarean sections can also be done using this technique. Richardson et al. 9 did not show any differences between hypobaric and hyperbaric bupivacaine regarding motor function, the need for analgesics, or side effects in the first 48 hours, in patients who underwent cesarean sections.
The Quincke needle does not cause erratic distribution of the local anesthetic and presents a low incidence of postoperative headache 10, and for those reasons it was chosen for this study.
Since the fall in blood pressure is a complication commonly seen in spinal anesthesia, it should be minimized as much as possible. For such, the literature recommends that crystalloid solutions should be administered just before the blockade, since it changes cardiac performance (increases the cardiac index and minimizes the reduction in diastolic blood pressure), especially in unilateral blocks 11. In reality, this is another advantage of hypobaric anesthesia, since its slower installation allows the completion of the infusion before acute hemodynamic changes may occur. In our study, the administration of the crystalloid solution was standardized, with volumes that varied from 500 to 1,000 mL of Ringer's lactate during 20 minutes with the patient in lateral decubitus (10 mL.kg-1). Horlocker et al. 4 concluded that the change in decubitus 10 minutes after the blockade does not cause important hemodynamic changes. Imbelloni et al. 1, studying the same technique, maintained the patients in lateral decubitus for 20 minutes. We decided to maintain the patients in lateral decubitus for 20 minutes to achieve the greatest stabilization possible of the blockade, and to observe the hemodynamic changes between 10 and 20 minutes. We did not observe clinically significant changes between those two moments, as reported by Horlocker et al. 4. Considering that the surgeries were performed in the lower limbs, without cuff inflation, the percentage of 32.2% of patients who presented sensitivity levels between T4 and T6, considered unnecessarily high, was clinically significant. Initially, contradictorily, sympathetic blockades that could cause hemodynamic instability during the procedure were not obtained; this is another factor favoring the use of hypobaric solutions in spinal anesthesias.
The dose of bupivacaine was standardized at 15 mg to study its hemodynamic effects, motor blockade, and level of sensitive blockade achieved. The rate of the injection (1 mL per 5 seconds), gauge and direction of the needle (paramedian approach), and the site of the injection were also standardized, since it is well known that those four factors influence the effects seen in spinal anesthesia. Horlocker 4 studied specifically the rate of the injection and the dispersion of hypobaric bupivacaine, and concluded that the fast administration of 0.3% bupivacaine reaches up to 4 dermatomes higher than with the slow injection and, therefore, causes more hemodynamic repercussions. However, in that same study, they did not demonstrated any differences between the levels achieved between the dependent and non-dependent limbs. The opposite was demonstrated by Faust et al. 5, but his patients remained in lateral decubitus during the procedure (a mean of three hours of duration). In this study, there was a difference between the levels of latency after the first 20 minutes (which were not quantified), but it did not show any differences at the end of the surgery.
According to the literature, patients should remain in lateral decubitus for 10 to 20 minutes after the administration of the anesthetic; it has not been demonstrated any additional advantage by keeping the patient in lateral decubitus for more than 30 minutes 1. However, the dose of the local anesthetic and the length of time the patient should remain in lateral decubitus for this anesthetic technique and obtain unilateral anesthesia have not been established, generating divergent and controversial opinions 1,3,5,12.
Meyer et al. 10 studied the sympathetic blockade with this type of anesthesia and concluded that the same is limited to the surgical side in more than 70% of the cases, thus demonstrating the hemodynamic stability with the technique proposed, which was corroborated by the results observed in this study. Another important argument for the slower installation of the blockade and, consequently, less severe hemodynamic changes, is the slow dispersion of the hypobaric solution 5.
The use of an anesthetic solution whose density is lower than that of the CSF could, in theory, limit the anesthesia to the superior metameres when the block is performed with the patient in lateral decubitus and remains in this position for a few minutes. There are references indicating that to fully achieve this effect, a virtual space must be created inside the subarachnoid space, removing an amount of CSF to allow the accommodation of the liquid to be injected, allowing the fluctuation of the anesthetic in relation to the CSF, acting preferentially on the upside nerve fibers 5,13.
A technique described for the evaluation of the sympathetic blockade (which is responsible for the cardiovascular manifestations) is the loss of thermal sensitivity 3. Another technique described is the determination of the skin blood flow, evaluated by doppler fluxometry (which evaluates the vasomotor constriction reflex as a means of assessing the anesthetic level) 14. The mere visualization of vasodilation in the area one expects to be anesthetized is also a useful method to observe the presence of sympathetic blockade. There is evidence demonstrating that such blockade is limited to the site of the surgery in more than 70% of restricted spinal anesthesias 10,15.
The maximal sensitive level achieved was T4, but in the majority of the patients this level was limited to T8. Among the patients, 67.7% maintained a sensitivity level up to this level, but 32.3% had a higher level, and only 12.9% reached a level above T6.
As demonstrated in table II, 10 minutes after the injection of bupivacaine, the metameric distribution was similar to the one achieved at 20 minutes, and at 15 minutes the results were closer and more similar.
The motor blocked achieved, classified as Bromage 3, was obtained in 83.19% of the patients, which was satisfactory for the surgery, and obtained a high degree of satisfaction both by the patient and the surgical team. Smaller doses have been studied, with similar satisfactory results. Doses of 5 mg were satisfactory, achieving a total motor blockade in 75% of 20 patients who received this type of anesthesia 16.
In this study, there was no need to change to general anesthesia in any patient due to unsatisfactory blockade or even total block failure, and there were no cases of post postdural puncture headache.
We did not have a control group in this study since, as explained before, the objective was a description of the data related specifically to hypobaric bupivacaine, without the need to compare it to other drugs or other densities of the same drug. We demonstrated that, with the anesthetic volume used, the hemodynamic repercussions were not clinically significant, demonstrating that the drug, prepared with industrial pharmacological technique, is a safe option for this type of surgical intervention.
The absence of severe side effects allows it to be used in older patients or, hypothetically, in those who present risk factors for intraoperative hypotension, which, to be demonstrated specifically, requires the extension of this study to include a new group with a different cardiovascular and hemodynamic profile.
Hypobaric bupivacaine at a concentration of 0.5%, prepared homogenously, with stable and well-defined density, besides the assurance of sterility, demonstrated to be a reliable and safe option, with very few hemodynamic repercussions, for orthopedic surgeries of the lower limbs, despite the wide variation in the levels of sensitive blockade observed.
The length of time patients remained in lateral decubitus after the blockade, 20 minutes, was not enough to produce the characteristics of a definitive unilateral anesthesia, motor or sensitive.
The mean duration of the blockade, 250 minutes, allows the realization of minor and medium surgeries of the lower abdomen, extra-peritoneal, and in the lower limbs, without the need of reverting to general anesthesia.
Acknowledgements
To the Laboratório Cristália Produtos Químicos Farmacêuticos Ltda for preparing the Hypobaric Bupivacaine used in this study.
REFERENCES
Submitted em 31 de maio de 2007
Accepted para publicação em 24 de abril de 2007
- 01. Imbelloni LE, Beato L, Gouveia MA Raquianestesia unilateral com bupivacaína hipobárica. Rev Bras Anestesiol, 2002;52: 542-548.
- 02. Carpenter RL, Caplan RA, Brown DL et al. Incidence and risk factors for side effects of spinal anesthesia. Anesthesiology, 1992;76:906-916.
- 03. Casati A, Fanelli G Unilateral spinal anesthesia. State of the art. Minerva Anestesiol, 2001;67:855-862.
- 04. Horlocker TT, Wedel DJ, Wilson PR Effect of injection rate on sensory level and duration of hypobaric bupivacaine spinal anesthesia for total hip arthroplasty. Anesth Analg, 1994;79:773-777.
- 05. Faust A, Fournier R, Van Gessel E et al. Isobaric versus hypobaric spinal bupivacaine for total hip arthroplasty in the lateral position. Anesth Analg, 2003;97:589-594.
- 06. Maroof M, Khan RM, Siddique M et al. Hypobaric spinal anaesthesia with bupivacaine (0,1%) gives selective sensory block for ano-rectal surgery. Can J Anaesth 199;42:691-694.
- 07. Kuusniemi KS, Pihlajamäki KK, Kirvelä AO et al. Spinal anesthesia with hypobaric bupivacaine for knee arthroscopies: effect of posture on motor block. Reg Anesth Pain Med, 2001; 26:30-34.
- 08. Kuusniemi KS, Pihlajamäki KK, Irjala JK et al. Restricted spinal anaesthesia for ambulatory surgery: a pilot study. Eur J Anaesthesiol, 1999;16:2-6.
- 09. Richardson MG, Collins HV, Wissler RN Intrathecal hypobaric versus hyperbaric bupivacaine with morphine for cesarean section. Anesth Analg 1998;87:336-340.
- 10. Meyer J, Enk D, Penner M Unilateral spinal anesthesia using low-flow injection through a 29-gauge Quincke needle. Anesth Analg, 1996;82:1188-1191.
- 11. Casati A, Fanelli G, Berti M et al. Cardiac performance during unilateral lumbar spinal block after crystalloid preload. Can J Anesth, 1997;44:623-28.
- 12. Imbelloni LE, Beato L, Gouveia MA Baixas doses de bupivacaína hipobárica para raquianestesia unilateral. Rev Bras Anestesiol, 2003;53:579-585.
- 13. Gouveia MA Fatores que Controlam a Dispersão das Drogas na Raquianestesia, em: Imbelloni LE Tratado de Anestesia Raquidiana. Curitiba, Medidática Informática, 2001;67-72.
- 14. Ikuta Y, Shimoda O, Ushijima K et al. Skin vasomotor reflex as an objective indicator to assess the level of regional anesthesia. Anesth Analg, 1998;86:336-340.
- 15. Enk D Unilateral spinal anaesthesia: gadget or tool? Curr Opin Anaesthesiol, 1998;11:511-515.
- 16. Fanelli G, Casati A, Aldegheri G et al. Cardiovascular effects of two different regional anaesthetic techniques for unilateral leg surgery. Acta Anaesthesiol Scand, 1998;42:80-84.
Publication Dates
-
Publication in this collection
31 July 2007 -
Date of issue
Aug 2007
History
-
Accepted
24 Apr 2007 -
Received
31 May 2007