Abstracts
Purpose:
this study investigated the influence of anatomical predictors on difficult laryngoscopy and orotracheal intubation in obese patients by comparing Macintosh and Airtraq(tm) laryngoscopes.
Methods:
from 132 bariatric surgery patients (body mass index = 35 kg m-1), cervical perimeter, sternomental distance, interincisor distance, and Mallampati score were recorded. The patients were randomized into two groups according to whether a Macintosh (n = 64) or an Airtraq(tm) (n = 68) laryngoscope was used for tracheal intubation. Time required for intubation was the first outcome. Cormack-Lehane score, number of intubation attempts, the Macintosh blade used, any need for external tracheal compression or the use of gum elastic bougie were recorded. Intubation failure and strategies adopted were also registered.
Results:
intubation failed in two patients in the Macintosh laryngoscope group, and these patients were included as worst cases scenario. The intubation times were 36.9 + 22.8 s and 13.7 + 3.1 s for the Macintosh and Airtraq(tm) laryngoscope groups (p < 0.01), respectively. Cormack-Lehane scores were also lower for the Airtraq(tm) group. One patient in the Macintosh group with intubation failure was quickly intubated with the Airtraq(tm). Cervical circumference (p < 0.01) and interincisor distance (p < 0.05) influenced the time required for intubation in the Macintosh group but not in the Airtraq(tm) group.
Conclusion:
in obese patients despite increased neck circumference and limited mouth opening, the Airtraq(tm) laryngoscope affords faster tracheal intubation than the Macintosh laryngoscope, and it may serve as an alternative when conventional laryngoscopy fails.
Objetivo:
esse estudo investigou a influência de preditores anatômicos para laringoscopia e intubação orotraqueal difícil em pacientes obesos mediante a comparação dos laringoscópios Macintosh e Airtraq(r).
Métodos:
em 132 pacientes de cirurgia bariátrica foram registrados: perímetro cervical, distância esternomentoniana, distância inter-incisivos e escore de Mallampati. Os pacientes foram randomizados em dois grupos, de acordo com o laringoscópio usado para a intubação traqueal: Macintosh (n = 64) ou Airtraq(r) (n = 68). O tempo até a intubação foi o primeiro desfecho. Também foram registrados: escore de Cormack-Lehane, número de tentativas de intubação, lamina Macintosh usada, necessidade de compressão traqueal externa, ou uso de um bougie elástico de borracha. Também foram anotados o insucesso na intubação e as estratégias adotadas.
Resultados:
houve insucesso na intubação em dois pacientes no grupo com laringoscópio de Macintosh; esses pacientes foram incluídos como o pior cenário de caso. Os tempos para intubação foram 36,9 ± 22,8 seg e 13,7 ± 3,1 seg para os grupos Macintosh e Airtraq(r) (p < 0,01), respectivamente. Os escores de Cormack-Lehane também foram mais baixos para o grupo Airtraq(r). Um paciente no grupo Macintosh com insucesso na intubação foi rapidamente intubado com o laringoscópio Airtraq(r). A circunferência cervical (p < 0,01) e a distância inter-incisivos (p < 0,05) influenciaram o tempo até a intubação no grupo Macintosh, mas não no grupo Airtraq(r).
Conclusão:
em pacientes obesos, apesar da maior circunferência cervical e da limitada abertura da boca, o laringoscópio Airtraq(r) possibilita uma intubação traqueal mais rápida versus laringoscópio Macintosh, podendo funcionar como alternativa, nos casos de insucesso com a laringoscopia convencional.
Obesidade; Intubação; Laringoscopia; Airtraq(r)
Objetivo:
el objetivo de este estudio fue evaluar la influencia de los predictores anatómicos en la laringoscopia e intubación orotraqueal difíciles en pacientes obesos comparando el laringoscopio Macintosh y el videolaringoscopio Airtraq(r).
Métodos:
en 132 pacientes sometidos a cirugía bariátrica (índice de masa corporal = 35 kg/m2), se registraron los valores de perímetro cervical, distancia mentoesternal, distancia interincisivos y puntuación de Mallampati. Los pacientes fueron aleatorizados en 2 grupos de acuerdo con el uso de los laringoscopios Macintosh (n = 64) o Airtraq(r) (n = 68) para intubación traqueal. El resultado primario fue el tiempo necesario para la intubación. Se registraron la puntuación de Cormack-Lehane, el número de intentos de intubación, el uso de lámina Macintosh y cualquier necesidad de compresión traqueal externa o la utilización de introductor del tubo traqueal. Las estrategias de intubación adoptadas y los fallos de las intubaciones también fueron recogidos en el informe.
Resultados:
en el grupo Macintosh, 2 pacientes presentaron fallo en la intubación y fueron incluidos como los peores casos de intubación. Los tiempos de intubación fueron 36,9 ± 22,8 s y 13,7 ± 3,1 s para los grupos Macintosh y Airtraq(r) (p < 0,01), respectivamente. Las puntuaciones de Cormack-Lehane también fueron menores para el grupo Airtraq(r). Un paciente del grupo Macintosh con fallo de intubación fue rápidamente intubado con el Airtraq(r). La circunferencia cervical (p < 0,01) y la distancia interincisivos (p < 0,05) influyeron en el tiempo necesario para la intubación en el grupo Macintosh, pero no en el grupo Airtraq(r).
Conclusión:
en los pacientes obesos, a pesar del aumento de la circunferencia del cuello y de la abertura limitada de la boca, el laringoscopio Airtraq(r) ofrece una intubación traqueal más rápida que el laringoscopio Macintosh, pudiendo servir como una alternativa cuando la laringoscopia convencional falle.
Obesidad; Intubación; Laringoscopia; Airtraq(r)
Introduction
Difficulties in airway management are a concern in obese patients.11. Juvin P, Lavaut E, Dupont H, et al. Difficult tracheal intubation is more common in obese than in lean patients. Anesth Analg. 2003;97:595-600. and 22. Dargin J, Medzon R. Emergency department management of the airway in obese adults. Ann Emerg Med. 2010;56:95-104. Anatomical characteristics such as cervical and occipital fat accumulation, tongue size, airway narrowing, limited neck extension, and limited mouth opening are factors that make tracheal intubation more difficult in obese patients than in those with a lower body mass index.33. Wilson ME. Predicting difficult intubation. Br J Anaesth. 1993;71:333-4. and 44. Kim WH, Ahn HJ, Lee CJ, et al. Neck circumference to thyromental distance ratio: a new predictor of difficult intubation in obese patients. Br J Anaesth. 2011;106:743-8. These factors have been designed to predict difficult laryngoscopy and intubation.
Several devices can be used to facilitate intubation in patients with conditions such as obesity. Airtraq(tm) (Prodol Medic; Biscay, Spain) is a disposable video laryngoscope designed to provide vocal cord visualization without the need to align the mouth and pharynx with the tracheal axis, and has been in clinical use since 2006.55. Maharaj CH, O'Croinin D, Curley G, et al. A comparison of tracheal intubation using the Airtraq or the Macintosh laryngoscope in routine airway management: a randomised, controlled clinical trial. Anaesthesia. 2006;61:1093-9. In several studies, Airtraq(tm) has proven to be better than conventional laryngoscopes for patients with certain conditions, including obesity.66. Ndoko SK, Amathieu R, Tual L, et al. Tracheal intubation of morbidly obese patients: a randomized trial comparing performance of Macintosh and Airtraq laryngoscopes. Br J Anaesth. 2008;100:263-8. , 77. Dhonneur G, Ndoko S, Amathieu R, et al. Tracheal intubation using the Airtraq in morbid obese patients undergoing emergency cesarean delivery. Anesthesiology. 2007;106:629-30. and 88. Ranieri Jr D, Filho SM, Batista S, et al. Comparison of Macintosh and AirtraqTM laryngoscopes in obese patients placed in the ramped position. Anaesthesia. 2012;67:980-5.
The difficult airway anatomical predictors are useful when the Macintosh laryngoscope is used; however, when video laryngoscopy is employed these predictors are uncertain. Thus, the aim of this study was to investigate the influence of demographic data and anatomical characteristics of obese patients in airway management by comparing the Macintosh laryngoscope and Airtraq(tm) video laryngoscope.
Materials and methods
After receiving approval from the Institutional Research Ethics Committee, and registering at Australian and New Zealand Clinical Trials (ANZCT, 12610000136000), candidates aged 18-60 years were invited to participate in this study. All patients provided informed consent and the participants were ASA I-III (American Society of Anesthesiologists) and had a body mass index (BMI) = 35 kg/m2. Patients with a history of untreated gastro-oesophageal reflux, succinylcholine intolerance, or previous difficult or unfeasible intubation were excluded. At preanesthetic assessment, Mallampati score,99. Mallampati SR, Gatt SP, Gugino LD, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J. 1985;32:429-34. interincisor distance, sternomental distance, and neck circumference at the level of the thyroid cartilage were recorded.
The patients were given ranitidine 50 mg and metoclopramide 10 mg intravenously 1 h before surgery. In the operating room after monitoring and prior to anesthesia induction, the patients were randomly assigned (with sealed opaque envelopes) to one of the two groups, according to the device to be used for tracheal intubation: Macintosh or Airtraq(tm) laryngoscope. Patient monitoring included continuous electrocardiography (EKG), pulse oximetry (SpO2) and non-invasive blood pressure.
The patients were placed in the ramped position, which began at the lumbar region and progressed to the subscapular and suboccipital areas, to keep the auditory meatus above the sternal manubrium and the shoulders according to the description by Collins and colleagues.1010. Collins JS, Lemmens HJ, Brodsky JB, et al. Laryngoscopy and morbid obesity: a comparison of the ''sniff'' and ''ramped'' positions. Obes Surg. 2004;14:1171-5. After a 3-min pre-oxygenation, anesthesia was induced with 2.0 µg/kg fentanyl and 2.0 mg/kg propofol. After the corneal-palpebral reflex was lost, the patients were given succinylcholine 1.0 mg/kg. The propofol dose was adjusted according to corrected weight (22 height × height).1111. Lemmens HJ, Brodsky JB, Bernstein DP. Estimating ideal body weight-a new formula. Obes Surg. 2005;15:1082-3. Intubation was performed at complete cessation of visible muscle twitching and was confirmed by capnography curve. Then 0.1 mg/kg vecuronium was injected, and anesthesia was maintained by the administration of sevoflurane (2%-3%) in a mixture of oxygen and air (FiO2 = 0.4).
The intubation was performed by four participating senior anesthesiologists with more than 4 years of clinical experience with conventional laryngoscopy and Airtraq(tm). The maximum time permitted for intubation was 120 s. Anesthesiologists using the Macintosh laryngoscope were free to choose the blade size (3, 4, or 5) and in the case of failure, a new intubation attempt was performed with a different blade size. The regular Airtraq(tm) (size 3) was used in all cases in this group.
Optimizing maneuver for the laryngoscopy was the Backward, Upward, Rightward Pressure (BURP) maneuver.1212. Knill RL. Difficult laryngoscopy made easy with a ''BURP''. Can J Anaesth. 1993;40:279-82. Intubation failures were recorded, and the alternative device could be used. Thus, patients who could not be intubated with the Macintosh laryngoscope could be then intubated with the Airtraq(tm), and vice versa. For cases where intubation could not be performed with either device, or for cases where facemask ventilation posed difficulty, a laryngeal mask airway (Fastrack(tm)) or a flexible bronchoscope could be used. Alternatively, the patient could be awakened and the surgery rescheduled. For women, 7.5-diameter lubricated tracheal tubes were used, and 8.5-diameter was used for men.
Time in seconds from the moment the anesthesiologist picked up the device (Macintosh laryngoscope or Airtraq(tm)) until cuff inflation was our primary outcome. Other secondary outcomes were the Cormack-Lehane scores1313. Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia. 1984;39:1105-11. as reported by the anesthesiologist; the number of intubation attempts; the number of the Macintosh blade used; any need for external tracheal compression by means of a BURP performed by an assistant, or the use of a gum elastic bougie; and intubation failure and the strategies adopted.
The number of participants in this study was calculated considering a minimum time difference for intubation of 21 s with a standard deviation of 27 s, in a series of 20 obese patients intubated with Macintosh laryngoscope or Airtraq(tm), derived from the experience of members of our group in a pilot study. A total of 126 patients were required to produce a significant difference with a power of 0.9 and a = 0.05. Student's t-tests were used for comparing continuous variable with a Bonferroni correction as appropriate. The Mann-Whitney U test was applied to the Cormack-Lehane score. Chi-squared tests were applied to categorical variables. Demographic and anatomical variables were analyzed to verify their influence on the time required for intubation. For this purpose, the multiple linear regression method with dummy variables was used, and correlation coefficient (r) for each group and variable is shown. Values of p < 0.05 were defined as statistically significant. The STATISTICA version 6, 2001 (StatSoft, Inc. Tulsa, OK), was used.
Results
From 158 initially selected patients, 26 were excluded. Nineteen declined to sign the informed consent form, and 7 required sedatives before entering the operating room. The Airtraq(tm) group consisted of 68 patients, each of whom was successfully intubated within the established maximum time of 120 s. The Macintosh laryngoscope group consisted of 64 patients, but 2 were treated considering the worst-case scenario due to failed tracheal intubation (intention to treat analysis) (Fig. 1).
The groups were homogeneous with respect to demographic and airway anatomical variables (Table 1).
Demographic data and airway anatomical measurements. Values are expressed as the means (standard deviation) or counts (gender, physical status, and Mallampati score).
The time required for intubation was significantly longer with the Macintosh laryngoscope (36.9 ± 22.8 s) than with the Airtraq(tm) (13.7 ± 3.1 s), (p < 0.01). In the Macintosh group, 13, 39, and 10 patients were subjected to intubation with blades of size 3, 4, and 5, respectively. In eight patients, the first attempt to intubate was unsuccessful and the blade was replaced with a larger one; for four of these, blade 4 was changed to blade 5, and in the remaining 4, blade 3 was changed to blade 4. Considering these eight patients, a BURP maneuver was required for 6, and of these, a gum elastic bougie was also needed for 1 patient. For 2 patients in the Macintosh group, intubation could not be accomplished within 120 s. One patient required three attempts with blades 4 and 5, and this patient had a Cormack-Lehane score IV. After facemask ventilation, this patient was intubated within 30 s using the Airtraq(tm), resulting in a Cormack-Lehane score I. Another patient exhibited bronchospasm, received facemask ventilation until spontaneous respiration recovered, and the procedure was postponed. The data on airway management are presented in Table 2.
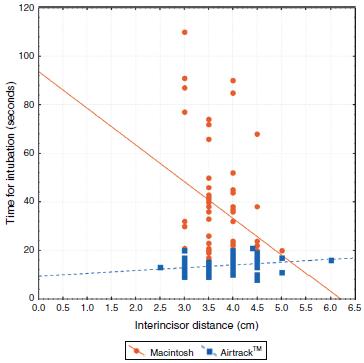
The following factors did not have a significant influence on the time required for intubation: age (p = 0.39), sex (p = 0.07), BMI (p = 0.91), and sternomental distance (p = 0.17). Neck circumference (p < 0.01) ( Fig. 2) and interincisor distance (p < 0.05) ( Fig. 3) did have a significant influence on the time required for intubation with the Macintosh laryngoscope, but not for the Airtraq(tm).
Adjusted correlations for the relationship between cervical perimeter and intubation time, according to intubation method for the Macintosh laryngoscope versus the Airtraq(tm) (p < 0.01).
Adjusted correlations for the relationship between interincisor distance and intubation time, according to intubation method for the Macintosh laryngoscope versus the Airtraq(tm) (p < 0.05).
Discussion
In this study, increased cervical circumference significantly influenced the time for intubation with the Macintosh laryngoscope but not for the Airtraq(tm).
The minimum interincisor distance recommended for Airtraq(tm) oral introduction is 2 cm.77. Dhonneur G, Ndoko S, Amathieu R, et al. Tracheal intubation using the Airtraq in morbid obese patients undergoing emergency cesarean delivery. Anesthesiology. 2007;106:629-30. and 1414. Dhonneur G, Abdi W, Ndoko SK, et al. Video-assisted versus conventional tracheal intubation in morbidly obese patients. Obes Surg. 2009;19:1096-101. The interincisor distance only influenced the time required for intubation with the Macintosh laryngoscope, thus revealing that the Airtraq(tm) can be used for patients with a limited mouth opening.
Studies that have analyzed intubation in obese patients have compared video laryngoscopes with a single Macintosh laryngoscope blade size.66. Ndoko SK, Amathieu R, Tual L, et al. Tracheal intubation of morbidly obese patients: a randomized trial comparing performance of Macintosh and Airtraq laryngoscopes. Br J Anaesth. 2008;100:263-8. , 77. Dhonneur G, Ndoko S, Amathieu R, et al. Tracheal intubation using the Airtraq in morbid obese patients undergoing emergency cesarean delivery. Anesthesiology. 2007;106:629-30. , 88. Ranieri Jr D, Filho SM, Batista S, et al. Comparison of Macintosh and AirtraqTM laryngoscopes in obese patients placed in the ramped position. Anaesthesia. 2012;67:980-5. and 1414. Dhonneur G, Abdi W, Ndoko SK, et al. Video-assisted versus conventional tracheal intubation in morbidly obese patients. Obes Surg. 2009;19:1096-101. In our study, the anesthesiologists selected the Macintosh blade sizes based on their experience and clinical judgment, and they also had the option to change the blade as needed. Blade changing occurred due to the inability to insert it properly into the vallecula; as many obese individuals are also tall, blade 3 (and even blade 4) may not provide adequate vocal cord visualization.
One novel finding from our study is that the increased neck circumference and limited mouth opening made the Macintosh laryngoscope less efficient than the Airtraq(tm) for obese patients. Increased cervical circumference has been associated with intubation difficulty using the Macintosh laryngoscope.44. Kim WH, Ahn HJ, Lee CJ, et al. Neck circumference to thyromental distance ratio: a new predictor of difficult intubation in obese patients. Br J Anaesth. 2011;106:743-8. and 1515. Gonzalez H, Minville V, Delanoue K, et al. The importance of increased neck circumference to intubation difficulties in obese patients. Anesth Analg. 2008;106:1132-6.
Randomized trials with obese patients observed that the time required for intubation was significantly longer with the Macintosh when compared with video laryngoscopes. The time required for tracheal intubation using the Pentax-AWS was significantly longer than that for the Macintosh laryngoscope (38 vs 26 s on average),1616. Abdallah R, Galway U, You J, et al. A randomized comparison between the Pentax AWS video laryngoscope and the Macintosh laryngoscope in morbidly obese patients. Anesth Analg. 2011;113:1082-7. and the intubation lasted significantly longer with GlideScope than Macintosh laryngoscope (48 vs 32 s).1717. Andersen LH, Rovsing L, Olsen KS. GlideScope video laryngoscope vs. Macintosh direct laryngoscope for intubation of morbidly obese patients: a randomized trial. Acta Anaesthesiol Scand. 2011;55:1090-7. Otherwise laryngoscopic Cormack-Lehane views were significantly better with video laryngoscopes. In two patients direct laryngoscopy failed and they were subsequently intubated with GlideScope without problems.
In these studies time to intubate was defined as the time elapsing between the insertion of the laryngoscope into the oral cavity and registration of expired CO2. In our study duration of intubation was defined as the time from gripping the device and tracheal tube cuff inflation. This may explain the very short intubation time with the Airtraq(tm) in the present report. Recorded start and end times for intubation are not consistent among several studies, so absolute comparisons are difficult.
The common tests designed to predict difficult laryngoscopy are of uncertain relevance when video laryngoscopy is employed and the new devices will probably be safer.1818. Martin F, Buggy DJ. New airway equipment: opportunities for enhanced safety. Br J Anaesth. 2009;102:734-8. and 1919. Amathieu R, Combes X, Abdi W, et al. An algorithm for difficult airway management, modified for modern optical devices (Airtraq laryngoscope; LMA CTrach): a 2-year prospective validation in patients for elective abdominal, gynecologic, and thyroid surgery. Anesthesiology. 2011;114:25-33.
We would stress that the Cormack & Lehane grade was described when Macintosh laryngoscope were used, and the importance to find a specific laryngeal view graduation for the video laryngoscopes.2020. Ferck CM, Lee G. laryngoscopy: time to change our view. Anaesthesia. 2009;64:351-4. and 2121. Mines R, Ahmand I. Can you compare the views of video laryngoscopes to the Macintosh laryngoscope. Anesthesia. 2011;66:315-6. These devices have particularities in their designs and procedures for intubation
Video laryngoscopes may be advantageous compared to the Macintosh laryngoscope because they can be used under awake conditions with adequate topical airway anesthesia, or when the patient is lightly sedated.2222. Uakritdathikarn T, Asampinawat T, Wanasuwannakul T, et al. Awake intubation with Airtraq Laryngoscope in a morbidly obese patient. J Med Assoc Thai. 2008;91:564-7. Thus the Airtraq(tm) is less expensive and easier to store and handle than bronchoscopes. As video laryngoscopes are rigid, they can push away excess tissue, secretions or blood, thereby allowing a better view of the vocal cords.2323. Moore AR, Schricker T, Court O. Awake video laryngoscopy-assisted tracheal intubation of the morbidly obese. Anaesthesia. 2012;67:232-5.
This study has several limitations. We did not use Intubation Difficulty Scale-IDS,2424. Adnet F, Borron SW, Racine SX, et al. The intubation difficulty scale (IDS): proposal and evaluation of a new score characterizing the complexity of endotracheal intubation. Anesthesiology. 1997;87:1290-7. which is mentioned quite often in the literature. We chose to use the Cormack-Lehane score and the time required for intubation, which are strongly related to clinical practice evaluation. We monitored only clinically the intubation conditions with no nerve stimulator technique for neuromuscular blockade. Although the study was randomized, it was impossible to blind the operator to the airway device being used.
We conclude that in obese patients, some anatomical characteristics, such as cervical circumference and interincisor distance, do not influence the time required for intubation with the Airtraq(tm), but these factors must be taken into account when using the Macintosh laryngoscope. The use of the Airtraq(tm) would be considered when the Macintosh laryngoscope intubation is unsuccessful for obese patients in the ramped position.
Acknowledgments
Prof. Leo Lynce provided statistical support for the study.
References
-
1Juvin P, Lavaut E, Dupont H, et al. Difficult tracheal intubation is more common in obese than in lean patients. Anesth Analg. 2003;97:595-600.
-
2Dargin J, Medzon R. Emergency department management of the airway in obese adults. Ann Emerg Med. 2010;56:95-104.
-
3Wilson ME. Predicting difficult intubation. Br J Anaesth. 1993;71:333-4.
-
4Kim WH, Ahn HJ, Lee CJ, et al. Neck circumference to thyromental distance ratio: a new predictor of difficult intubation in obese patients. Br J Anaesth. 2011;106:743-8.
-
5Maharaj CH, O'Croinin D, Curley G, et al. A comparison of tracheal intubation using the Airtraq or the Macintosh laryngoscope in routine airway management: a randomised, controlled clinical trial. Anaesthesia. 2006;61:1093-9.
-
6Ndoko SK, Amathieu R, Tual L, et al. Tracheal intubation of morbidly obese patients: a randomized trial comparing performance of Macintosh and Airtraq laryngoscopes. Br J Anaesth. 2008;100:263-8.
-
7Dhonneur G, Ndoko S, Amathieu R, et al. Tracheal intubation using the Airtraq in morbid obese patients undergoing emergency cesarean delivery. Anesthesiology. 2007;106:629-30.
-
8Ranieri Jr D, Filho SM, Batista S, et al. Comparison of Macintosh and AirtraqTM laryngoscopes in obese patients placed in the ramped position. Anaesthesia. 2012;67:980-5.
-
9Mallampati SR, Gatt SP, Gugino LD, et al. A clinical sign to predict difficult tracheal intubation: a prospective study. Can Anaesth Soc J. 1985;32:429-34.
-
10Collins JS, Lemmens HJ, Brodsky JB, et al. Laryngoscopy and morbid obesity: a comparison of the ''sniff'' and ''ramped'' positions. Obes Surg. 2004;14:1171-5.
-
11Lemmens HJ, Brodsky JB, Bernstein DP. Estimating ideal body weight-a new formula. Obes Surg. 2005;15:1082-3.
-
12Knill RL. Difficult laryngoscopy made easy with a ''BURP''. Can J Anaesth. 1993;40:279-82.
-
13Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia. 1984;39:1105-11.
-
14Dhonneur G, Abdi W, Ndoko SK, et al. Video-assisted versus conventional tracheal intubation in morbidly obese patients. Obes Surg. 2009;19:1096-101.
-
15Gonzalez H, Minville V, Delanoue K, et al. The importance of increased neck circumference to intubation difficulties in obese patients. Anesth Analg. 2008;106:1132-6.
-
16Abdallah R, Galway U, You J, et al. A randomized comparison between the Pentax AWS video laryngoscope and the Macintosh laryngoscope in morbidly obese patients. Anesth Analg. 2011;113:1082-7.
-
17Andersen LH, Rovsing L, Olsen KS. GlideScope video laryngoscope vs. Macintosh direct laryngoscope for intubation of morbidly obese patients: a randomized trial. Acta Anaesthesiol Scand. 2011;55:1090-7.
-
18Martin F, Buggy DJ. New airway equipment: opportunities for enhanced safety. Br J Anaesth. 2009;102:734-8.
-
19Amathieu R, Combes X, Abdi W, et al. An algorithm for difficult airway management, modified for modern optical devices (Airtraq laryngoscope; LMA CTrach): a 2-year prospective validation in patients for elective abdominal, gynecologic, and thyroid surgery. Anesthesiology. 2011;114:25-33.
-
20Ferck CM, Lee G. laryngoscopy: time to change our view. Anaesthesia. 2009;64:351-4.
-
21Mines R, Ahmand I. Can you compare the views of video laryngoscopes to the Macintosh laryngoscope. Anesthesia. 2011;66:315-6.
-
22Uakritdathikarn T, Asampinawat T, Wanasuwannakul T, et al. Awake intubation with Airtraq Laryngoscope in a morbidly obese patient. J Med Assoc Thai. 2008;91:564-7.
-
23Moore AR, Schricker T, Court O. Awake video laryngoscopy-assisted tracheal intubation of the morbidly obese. Anaesthesia. 2012;67:232-5.
-
24Adnet F, Borron SW, Racine SX, et al. The intubation difficulty scale (IDS): proposal and evaluation of a new score characterizing the complexity of endotracheal intubation. Anesthesiology. 1997;87:1290-7.
-
☆
Study conducted at the Department of Anesthesiology, Hospital do Coração de Balneário Camboriú, Balneário Camboriú, SC, Brazil.
Publication Dates
-
Publication in this collection
May-Jun 2014
History
-
Received
27 Oct 2012 -
Accepted
21 Nov 2012