Abstracts
OBJECTIVE: To analyze the prevalence of IgG antibodies to human parvovirus B19. METHODS: Cross-sectional study in a suburban community in São Paulo, Southeastern Brazil, between November 1990 and January 1991. Randomly selected (N=435) representative samples of sera were collected from healthy children older than 15 days old and adults up to 40 years old. IgG antibodies were detected using ELISA. RESULTS: High prevalence of IgG antibodies to B19 parvovirus was found in 87% of newborns. The prevalence of maternally derived IgG antibodies exponentially plunged up to the 19th month of age. Low prevalence of antibodies was found in the first 4 years of life, increasing up to 72% in those aged 31-40 years. It was estimated that the average age of first infection in this population is 21 ± 7 years old and the optimal age for vaccination with a hypothetical vaccine would be 1 year of age. CONCLUSIONS: Parvovirus B19 IgG antibody prevalence was high in newborns and those aged 31-40 years. The analysis by age groups showed a pattern similar to that found in previous studies, i.e., low prevalence of infection in children that increases with age.
Parvoviridae Infections; Parvovirus B19, Human; Risk Groups; Seroepidemiologic Studies
OBJETIVO: Analisar a prevalência de anticorpos IgG ao parvovírus humano B19. MÉTODOS: Estudo transversal em uma comunidade de subúrbio de São Paulo, Brasil, de novembro 1990 a janeiro de 1991. Amostras aleatórias (N=435) e representativas de soro foram coletadas de crianças sadias a partir de 15 dias de idade e de adultos com até 40 anos. Os anticorpos IgG ao parvovírus humano B19 foram detectados pelo teste ELISA. RESULTADOS: A prevalência de anticorpos IgG ao parvovírus B19 foi de 87% dos recém-nascidos. A prevalência de anticorpos IgG de origem materna decaiu exponencialmente até o 19o mês de idade. Baixa prevalência de anticorpos foi observada nos primeiros quatro anos de vida, aumentando até 72% no grupo etário de 31-40 anos. A idade média de aquisição da primeira infecção nesta comunidade é de 21 ± 7 anos. A idade ótima para se vacinar as crianças desta comunidade com uma vacina hipotética é de um ano de idade. CONCLUSÕES: A prevalência de anticorpos IgG ao parvovírus B19 foi alta entre recém-nascidos e no grupo etário 31-40 anos. A análise por estrutura etária mostrou padrão similar aos estudos prévios relacionados à baixa prevalência de infecção em crianças que aumenta com a idade.
Infecções por Parvoviridae; Parvovirus B19 Humano; Grupos de Risco; Estudos Soroepidemiológicos
ARTIGOS ORIGINAIS ORIGINAL ARTICLES
Seroprevalence of human parvovirus B19 in a suburban population in São Paulo, Brazil
Soroprevalência do parvovírus humano B19 em população de subúrbio no Estado de São Paulo, Brasil
E M M HuatucoI; E L DurigonI; F L A S LebrunI; S D PassosII; R E GazetaII; R S Azevedo NetoIII; E MassadIII
IDepartamento de Microbiologia. Instituto de Ciências Biomédicas. Universidade de São Paulo (USP). São Paulo, SP, Brasil
IIDepartamento de Pediatria. Faculdade de Medicina de Jundiaí. Jundiaí, SP, Brasil
IIIFaculdade de Medicina. USP. São Paulo, SP, Brasil
Correspondência | Correspondence Correspondência | Correspondence: Eduardo Massad Instituto Oscar Freire - FMUSP R. Teodoro Sampaio 115 05405-000 São Paulo, SP, Brasil E-mail: edmassad@usp.br
ABSTRACT
OBJECTIVE: To analyze the prevalence of IgG antibodies to human parvovirus B19.
METHODS: Cross-sectional study in a suburban community in São Paulo, Southeastern Brazil, between November 1990 and January 1991. Randomly selected (N=435) representative samples of sera were collected from healthy children older than 15 days old and adults up to 40 years old. IgG antibodies were detected using ELISA.
RESULTS: High prevalence of IgG antibodies to B19 parvovirus was found in 87% of newborns. The prevalence of maternally derived IgG antibodies exponentially plunged up to the 19th month of age. Low prevalence of antibodies was found in the first 4 years of life, increasing up to 72% in those aged 31-40 years. It was estimated that the average age of first infection in this population is 21 ± 7 years old and the optimal age for vaccination with a hypothetical vaccine would be 1 year of age.
CONCLUSIONS: Parvovirus B19 IgG antibody prevalence was high in newborns and those aged 3140 years. The analysis by age groups showed a pattern similar to that found in previous studies, i.e., low prevalence of infection in children that increases with age.
Descriptors: Parvoviridae Infections, epidemiology. Parvovirus B19, Human. Risk Groups. Seroepidemiologic Studies.
RESUMO
OBJETIVO: Analisar a prevalência de anticorpos IgG ao parvovírus humano B19.
MÉTODOS: Estudo transversal em uma comunidade de subúrbio de São Paulo, Brasil, de novembro 1990 a janeiro de 1991. Amostras aleatórias (N=435) e representativas de soro foram coletadas de crianças sadias a partir de 15 dias de idade e de adultos com até 40 anos. Os anticorpos IgG ao parvovírus humano B19 foram detectados pelo teste ELISA.
RESULTADOS: A prevalência de anticorpos IgG ao parvovírus B19 foi de 87% dos recém-nascidos. A prevalência de anticorpos IgG de origem materna decaiu exponencialmente até o 19o mês de idade. Baixa prevalência de anticorpos foi observada nos primeiros quatro anos de vida, aumentando até 72% no grupo etário de 31-40 anos. A idade média de aquisição da primeira infecção nesta comunidade é de 21 ± 7 anos. A idade ótima para se vacinar as crianças desta comunidade com uma vacina hipotética é de um ano de idade.
CONCLUSÕES: A prevalência de anticorpos IgG ao parvovírus B19 foi alta entre recém-nascidos e no grupo etário 31-40 anos. A análise por estrutura etária mostrou padrão similar aos estudos prévios relacionados à baixa prevalência de infecção em crianças que aumenta com a idade.
Descritores: Infecções por Parvoviridae, epidemiologia. Parvovirus B19 Humano. Grupos de Risco. Estudos Soroepidemiológicos.
INTRODUCTION
Human parvovirus B19 was first accidentally detected in a serum sample of healthy blood donors and until recently it has been the only member of the genus Erythrovirus of parvoviridae family known to be pathogenic in humans (Van Regenmortel et al22 2000). B19 virus is a small nonenveloped icosahedral capsid with about 25 nm in diameter and 60 capsomeres containing mainly VP2; VP1 accounts for only about 5% of the capsid protein. Protein folds are created (alpha) on the surface of the assembled capsids where the host's immune system can recognize them as antigenic determinants. The B19 virus has a genome that consists of a single-stranded DNA of 5,596 nucleotides with palindromic inverted terminal that repeats at both ends and forms hairpin structures (Deiss et al9 1990).
B19 virus has a remarkable tissue-tropism for erythroid progenitor cells in human bone marrow (Brown et al5 1993). It is widespread and infection manifestations vary with the host's immunological and hematological status. Cases of B19 virus infection are nearly 30% asymptomatic (Brown4 1997).
Acute B19 virus infection is thought to confer a protective, lifelong immunity (Kajigaya & Momoeda14 1997). B19 virus infection is common, and 40-60% of adults have antibodies against the virus due to previous exposure. Epidemiologically, infection rates increase every 34 years, but there can be longer cycles, with viral activity increases every 47 years (Rodis20 1999). B19 virus is usually spread by respiratory secretions, but it can be transmitted transplacentally and by blood or blood components transfusion (Laub & Strengers15 2002). This virus has also been established as an important cause of chronic anemia and thrombopenia in immunocompromised hosts (Foto et al10 1993). Infections during pregnancy may result in severe intrauterine anemia that can lead to spontaneous abortion, fetal hydrops, or fetal death (Brawn et al6 1984).
In patients younger than five years with fulminating hepatitis of unexplained origin, evidence of acute parvovirus B19 infection was associated with a distinct clinical pattern. In particular, low bilirubin concentrations and rapid recovery of liver function without transplantation were distinctive features.
The overall prevalence of IgG antibodies to parvovirus B19 in healthy adults is 50% in the United States and Japan (Anderson et al3 1986); 60%70% in England and Wales (Gay et al12 1994); 44% in Chile (Abarca et al1 2002), 44.1% in the Czech Republic (Sodja et al21 1995), 50% in India (Abraham et al2 2002) and 53.2% in Spain (Guerri et al13 2000).
In Brazil and Niger, studies with individuals aged more than 10 years old showed a prevalence of IgG antibodies of more than 80% (Nascimento et al17 1990). For that reason, a serological investigation was carried out in a random sample in a small town located in the outskirts of the city of São Paulo, southeastern Brazil.
The objective of the study was to assess parvovirus B19 serological status in a randomly selected representative sample and determine the potential age-specific risk of susceptibility to reinfection or disease.
METHODS
A cross-sectional study was conducted in the city of Caieiras, a northern suburb of the city of São Paulo, southeastern Brazil, between November 18, 1990, and January 18, 1991, as part of a rubella seroepidemiological survey. The sample included healthy subjects up to 40 years old. Standard theory (Cochran7 1977) was applied to achieve a random, two-level cluster-based sample from families randomly selected.
The city of Caieiras (east of the state of São Paulo, Brazil) is appropriate for this investigation because its inhabitants mostly live , study and work in the city. Its urban area coincides with its total population and the residences dispersion is absolutely horizontal. Caieiras had a population of about 30,000 inhabitants in 1990, distributed over an area of 104 km2, mostly (>90%) in the urban area (FIBGE11 1980).
Serum samples were collected using a vacuum system or butterfly needle from children under two years of age. Sera obtained after centrifugation of clotted samples were stored at 20ºC. Age groups of 435 sera samples are presented in Table 1. Detailed sera collection, demographic information and sampling methods have been reported elsewhere (Neto et al18 1994).
Enzyme-linked immunosorbant assay (ELISA Biotrin International, Dublin, Ireland) was used to detect IgG antibodies to parvovirus B-19 virus in human serum. Result interpretation, i.e., whether anti-parvovirus IgG was present or not, was based on an estimated cut-off value (COV). In the interpretation of absorbances, samples with mean absorbance equal to or greater than COV x 1.1 were considered reactive (positive) and those with mean absorbance lower than COV x 0.9 were considered non-reactive (negative) to antiparvovirus B19 IgG.
Children under one year of age who tested positive for parvovirus B19 were retested by reverse transcription-polymerase chain reaction (RT-PCR) analysis. Positive RT-PCR samples were excluded from the analysis because they were naturally (or transplacentally) infected with parvovirus B19.
The mathematical and statistical analysis included:
1. Fitting seroprevalence profiles. The age-dependent maternally derived antibodies curve, M(a), was fitted by maximum likelihood techniques to the following equation:
where M(a) is age-dependent proportion of seropositives and k is a fitting parameter. Therefore, the half-life of decay of maternally derived antibodies T1/2, is given by:
where k is the same as in equation 1. The age-dependent naturally acquired antibodies curve, S+(a), was fitted by the same technique as above to the following equation:
where kii (i = 1,2,3) are fitting parameters.
2. Estimating the average age of first infection. The average age of first infection,
1st, was estimated according to the following equation (Coutinho et al8 1993, Neto et al 1994,18 199519):
where S+(a) is according to equation 3.
3. Estimating the force of infection. The force of infection, i.e., incidence density, l, was calculated according to the catalytic equation (Massad et al16 1995):
4. Calculating the optimum age for vaccination. There is no effective vaccine against human parvovirus B-19 available yet, but it is just a matter of time. Still, the optimum age for vaccination given the seroprevalence profile was estimated. The techniques described in Zanetta et al23 2001 were applied. The expression related to lifetime expected risk of infection due to parvovirus B-19 is given by:
where l is the average force of infection, u(a) is the fraction of those of age a who are susceptible, ô is a normalization constant, and C(a) is vaccine seroconversion. Since the latter is unknown, it was taken as the complement of M(a), the maternally derived antibody function.
Considering that a proportion p of the population is vaccinated at age av, the proportion of remaining susceptible persons, u(a), is then
where ac is a critical age up to which maternal antibodies protect the child.
The average force of infection l,was calculated according to equation 4, since it is the inverse of the average age of first infection (Coutinho et al8 1993, Neto et al 1994,18 199519). The optimum age of vaccination was obtained by evaluating the age of vaccination that minimizes E, as in equation 6.
RESULTS
The Table summarizes the seroepidemiological analysis, by age groups, with a 95% confidence interval.
There are two phases of inverse behaviors. In the first phase, from newborns to children aged 1619 months, the proportion of seropositives decreases. There was a fast decline in maternal antibody after the first month of age, with the highest proportion of infants seronegative for parvovirus B19 between 16 and 19 months of age. In the second phase, from children aged 20 months to adults older than 40 years old, there is a progressive increase in the proportion of seropositives immune to parvovirus B19. In this phase, the seropositive proportion increases flatly with age, so that 53.85% develop immunity between 23 and 30 years of age.
A comparative analysis was performed in seropositive subjects and they were divided into six age groups: <1 month, 14 months, 519 months, 2048 months, 530 years, 3140 years, as shown in Figure 1.
There was found 87% prevalence of IgG antibodies anti-parvovirus B19 in infants under 15 days. Also, there was seen a decrease in seropositives as from the first month of life and an increase as from five years up to 40 years of age. In the latter age group, prevalence was 72.7%. The chi-square test showed significant differences in the proportions of seropositive in high prevalence age groups (p<0.0001, df=5). When differences among proportions of seropositive subjects in low prevalence age groups (14 months, 519 months and 2048 months) were checked using the chi-square test, no significant differences were seen (p=0.278).
After establishing the proportion of seropositive at each age group (Table), data were fitted to two continuous functions by the maximum likelihood technique, one for the maternally derived antibody decay phase, M(a), and the other for naturally acquired infection phase, S+(a).
In the maternal antibody decay phase, M(a) was fitted to an exponential curve as in equation 1. Estimations were made using the regression module for SPSS pack version 10.0. The half-life of maternally derived antibody decay, T1/2, was 0.093 months, a very rapid decay. Figure 1 shows the curve M(a) adjusted to the decay phase.
A rapid decay of maternally derived antibodies was seen in the first month, alternating slow decays and increases from the 12th up to the 14th month. Between the 14th and the 19th month there were only decays up to complete elimination of motherly antibodies.
For scheming the ascending phase of naturally acquired infection, S+(a) was fitted to equation 3, as shown in Figure 2.
The arrow points to the average age of first infection, calculated according to equation 4 in 21 ± 7 years of age, a very high average age of first infection acquisition.
Figure 3 shows the age-dependent force of infection, calculated according to equation 5.
The force of infection dropped quickly from the age of one onwards, stabilizing at low levels after the age of ten. The average force of infection was 0.047 new cases per susceptible per year, which in turn resulted in an estimated very high average age of first infection acquisition of 21 years.
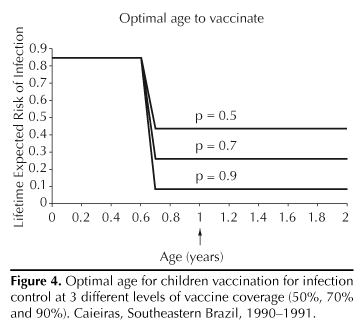
Figure 4 shows the optimal age to vaccinate children against parvovirus B19.
Regardless of vaccine coverage, the age that minimized the expected lifetime risk of infection was one year (arrow). Such younger age may be an unexpected result since first infection on average occurs at an older age. However, as shown in Figure 3, the mass of the force of infection distribution is concentrated at younger ages, implying that the virus is probably circulating among the youngsters.
DISCUSSION
Epidemiologically, there can be made considerations based on the profile found in the present study. A major finding is the high proportion of motherly derived parvovirus B19 antibodies at birth (Figure 1), revealing that the great majority of childbearing women already had been infected, and evidencing that antibodies cross the placenta due to IgG active transplacental transport.
Possibly high levels of IgG may be explained by facilitating mechanisms for newborn protection over a longer period of time by means of immunity acquired during gestation. Immunoglobulin mother-fetus transference has been reported during pregnancy indicating that human placenta develops a specific IgG mechanism of transference.
As from the first month of life, the proportion of seropositive individuals declined every month up to the age of 16 months, when IgG antibodies against parvovirus B19 were no longer detected in children. The immune status lasted up to the 19th month of life (Figure 1). The half-life of maternally derived antibody decay, T1/2, was 0.093 months, which is a rapid decay. This motherly-derived antibodies loss in children changes in the same fashion as in England, and in children younger than 12 months, there are decreasing levels of IgG motherly-derived antibodies to B19. 10
The serological profile in this community also indicates that B19 infection rates are low before the age of five, being slow between one and four years of age. This can be explained by apparently low exposure between susceptible and infected individuals in these age groups. As from the age of five, the proportion of infected individuals grows fast, declining slowly after 16 years of age (36.4%, Figure 1), which results in high susceptibility during childbearing years between the age of 16 and 30 years with intense viral activity in these age groups.
Increased antibody prevalence (Figure 4) is possibly due to infection. As from the age of 20 months, exposure to B19 virus is frequent and the proportion of individuals with detectable antibodies increases flatly. Despite variations, there was seen an increasing trend in the proportion of seropositive individuals as age increases.
The continuous growth in the proportion of seropositive individuals during adult life evidences that new exposure and possibly B19 reinfection were relatively frequent, infecting a significant proportion of adults and disseminating the virus. The high IgG prevalence in adults resulted in high motherly derived antibody acquisition by a large proportion of newborn children. In spite of the low immunity prevalence, which also implies a low incidence of disease, this was observed in Japan during different epidemic cycles.20
The fact that the force of infection drops very quickly from the age of one onwards, stabilizing after the age of 10 at very low levels results in very high average age of first infection acquisition, at an estimated age of 21 years.
Finally, although there is no effective vaccine available against human parvovirus B19, the optimal age for vaccination in this community was estimated. The age that minimizes the expected lifetime risk of infection is one year. Such younger age is probably due to the fact that the mass of the force of infection distribution is concentrated at younger ages, implying that the virus is probably circulating among the youngsters.
Received: 5/14/2007
Reviewed: 11/20/2007
Approved: 12/6/2007
Supported by grants from Laboratórios de Investigação Médica do Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo and Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq Grant 307914/2004-6).
- 1. Abarca K, Cohen BJ, Vial PA. Seroprevalence of Parvovirus B19 in urban Chilean children and young adults, 1990 and 1996. Epidemiol Infect. 2002;128(1):59-62.
- 2. Abraham M, Rudraraju R, Kannangai R, George K, Cherian T, Daniel D, Ramalingam R, Sridharan G. A pilot study on the seroprevalence of parvovirus B19 infection. Indian J Med Res. 2002;115:139-43.
- 3. Anderson LJ, Tsou C, Parker RA, Chorba TL, Wulff H, Tatersall P, Mortimer P. Detection of antibodies and antigens of human parvovirus B19 by enzyme-linked immunosorbent assay. J Clin Microbiol. 1986;24(4):522-6.
- 4. Brown KE. Human parvovirus B19 epidemiology and clinical manifestations. In: Anderson LJ, Young NS, editores. Human parvovirus B19. New York: Karger ; 1997. p. 42-60. (Monographs in Virology, 20).
- 5. Brown KE, Anderson SM, Young NS. Erythrocyte P antigen: cellular receptor for B19 parvovirus. Science 1993;262(5130):114-7.
- 6. Brown T, Anand A, Ritchie LD, Clewley JP, Reid TM. Intrauterine parvovirus infection associated with hydrops fetalis. Lancet 1984;2(8410):1033-4.
- 7. Cochran WG. Sampling Techniques. 3. ed. New York: John Wiley & Sons; 1977.
- 8. Coutinho FAB, Massad E, Burattini MN, Yang HM, Azevedo Neto RS. Effects of vaccination programmes on transmission rates of infections and related threshold conditions for control. IMA J Math Appl Med Biol. 1993;10(3):187-206.
- 9. Deiss V, Tratschin JD, Weitz M, Siegl G. Cloning of the human parvovirus B19 genome and structural analysis of its palindromic termini. Virology 1990;175(1):247- 54.
- 10. Foto F, Saag KG, Scharosch LL, Howard EJ, Naides SJ. Parvovirus B19-specific DNA in bone marrow from B19 arthropathy patients: evidence for B19 virus persistence. J Infect Dis. 1993;167(3):744-8.
-
11Fundação Instituto Brasileiro de Geografia e Estatística. IX Recenseamento geral do Brasil:1980. Rio de Janeiro; 1983.
- 12. Gay NJ, Hesketh LM, Cohen BJ, Rush M, Bates C, Morgan-Capner P, et al. Age specific antibody prevalence to parvovirus B19: How many women are infected in pregnancy? Commun Dis Rep CDR Rev. 1994;4(9):R104-7.
- 13. Guerra ML, Prior C, Merino R, Zapico R. Seroprevalencia de parvovirus B19 en nuestra área y su distribucion por edades y sexos. Enferm Infecc Microbiol Clin. 2000;18(5):243-4.
- 14. Kajigaya S, Momoeda M. Immune response to B19 infection. In: Anderson LJ, Young NS, editores. Human parvovirus B19. Switzerland: Karger; 1997. p.120-36. (Monographs in Virology, 20).
- 15. Laub R, Strengers P. Parvovirus and blood products. Pathol Biol (Paris). 2002;50(5):339-48.
- 16. Massad E, Azevedo-Neto RS, Burattini MN, Zanetta DMT, Coutinho FAB, Yang HM, et al. Assessing the efficacy of a mixed vaccination strategy against rubella in São Paulo, Brazil. Int J Epidemiol. 1995;24(4):842-50.
- 17. Nascimento JP, Buckley M, Brown K, Cohen BJ. The prevalence of antibodies to human parvovirus B19 in Rio de Janeiro, Brazil. Rev Inst Med Trop Sao Paulo. 1990;32(1):41-5.
- 18. Neto RSA, Silveira ASBS, Nokes DJ, Yang HM, Passos SD, Cardoso MRA, Massad E. Rubella seroepidemiology in a non-immunized population of São Paulo State, Brazil. Epidemiol. Infect. 1994;113(1):161-73.
- 19. Neto RSA, Richard A, Nokes DJ, Silveira ASB, Cohen BJ, Passos SD, et al. Salivary antibody detection in epidemiological surveys: A pilot study after a mass vaccination campaing against rubella in São Paulo, Brazil. Trans R Soc Trop Med Hyg. 1995;89(1):115-8.
- 20. Rodis JF. Parvovirus infection. Clin Obstet Gynecol. 1999;42(1):107-20
- 21. Sodja I, Mrázová M, Smelhausová M, Kotrbová K, Pazdiora P, Bruj J, et al. Seroprevalence of IgG antibodies against parvovirus B19 in the Czech Republic. Epidemiol Mikrobiol Imunol.1995;44(4):171-4.
- 22. Van Regenmortel MHV, Fauquet CM, Bishop DHL. Virus taxonomy: classification and nomenclature of viruses. In: Seventh report of the International Committee on Taxonomy of Viruses; San Diego, CA. San Diego: Academic Press; 2000.
- 23. Zanetta RAC, Amaku M, Azevedo RS, Zanetta DMT, Burattini MN, Massad E. Optimal ages for vaccination against measles in the State of São Paulo, Brazil, taking into account the mother's serostatus. Vaccine 2001;20(1-2):226-34.
Publication Dates
-
Publication in this collection
10 Apr 2008 -
Date of issue
June 2008
History
-
Reviewed
20 Nov 2007 -
Received
14 May 2007 -
Accepted
06 Dec 2007