Abstracts
OBJECTIVE: To assess the association between conservative management of high-grade cervical squamous intraepithelial lesions and recurrence rates and age groups. METHODS: Cross-sectional, retrospective, analytical observational study of 509 women (aged 15 to 76) with abnormal Pap smears attending a public reference center in the city of Maringá, southern Brazil, from 1996 to 2006. Data was collected from medical records, and the variables definitive diagnosis, type of treatment provided, occurrence of high-grade cervical squamous intraepithelial lesions and recurrence were studied. Pearson's chi-square test and Fisher's exact test were used in the statistical analyses. RESULTS: There were 168 cases of cervical high-grade cervical squamous intraepithelial lesions, of these, 31 were treated with cold-knife conization, 104 loop electrosurgical excision procedure, 9 hysterectomy and 24 conservative treatment (i.e., clinical and cytological follow-up or cervical electrocoagulation). A total of 8 (33.3%) women receiving conservative and 10 (6.9%) receiving non-conservative management had recurrent disease and this difference was statistically significant (p=0.0009), PR = 4.8 (95%CI 2.11;10.93). Three (30.0%) women among those undergoing clinical and cytological follow-up and five 5 (35.7%) among those submitted to cervical electrocoagulation had recurrent disease within three years, but the difference was not significant (p=0.5611). Recurrent rates in those younger and older than 30 were 13.8% (7 women) and 12.2% (11 women) (p = 0.9955). CONCLUSIONS: Age is not a predictor of disease recurrence. Conservative treatment is only recommended in exceptional situations due to its high recurrence rates. Careful cytological and colposcopic follow-up is required for three years when most recurrences occur.
Cervix Uteri; Uterine Cervical Neoplasms; Cervical Intraepithelial Neoplasia; Conization; Electrocoagulation; Cross-Sectional Studies
OBJETIVO: Analisar a associação entre a conduta conservadora em lesão intraepitelial cervical de alto grau com o índice de recidiva da neoplasia e faixa etária. MÉTODOS: Estudo transversal e retrospectivo realizado com 509 mulheres (15-76 anos) atendidas no período de 1996 a 2006, com colpocitologia oncótica alterada, em um serviço público de referência em Maringá, PR. Os dados foram coletados dos prontuários médicos e estudadas as variáveis diagnóstico definitivo, tipos de tratamento, ocorrência da lesão e recidivas, analisados por meio de testes de associação de qui-quadrado de Pearson e teste exato de Fisher. RESULTADOS: A lesão intraepitelial cervical de alto grau ocorreu em 168 casos; destes, 31 mulheres foram submetidas à amputação cônica, 104 a cirurgias de alta frequência, nove histerectomizadas e 24 receberam conduta conservadora. Dentre as mulheres com lesão de alto grau e tratadas de forma conservadora, oito (33,3%) recidivaram, enquanto dentre as submetidas à conduta não conservadora dez (6,9%) recidivaram, sendo essa diferença estatisticamente significante (p = 0,0009), RP = 4,8 (IC95% 2,11;10,93). Para aquelas que fizeram o seguimento clínico-citológico, três (30,0%) e, dentre as cauterizadas, cinco (35,7%) recidivaram no prazo de três anos, sem diferença significante (p = 0,5611). A recidiva abaixo e acima de 30 anos ocorreu, respectivamente, em sete (13,8%) e 11 (12,2%) mulheres (p = 0,9955). CONCLUSÕES: A idade da mulher não influencia o prognóstico de recidiva. O tratamento conservador deve ser indicado como conduta de exceção, dada a alta taxa de recidiva, e o seguimento deve ser rigoroso, com acompanhamento citológico e colposcópico de até três anos, período em que ocorre a maioria das recidivas.
Colo do Útero; Neoplasias do Colo do Útero; Neoplasia Intraepitelial Cervical; Conização; Eletrocoagulação; Estudos Transversais
OBJETIVO: Analizar la asociación entre la conducta conservadora en lesión intraepitelial cervical de alto grado con el índice de reincidencia de la neoplasia y grupo etario. MÉTODO: Estudio transversal y retrospectivo realizado con 509 mujeres (15-76 años) atendidas en el período de 1996 a 2006, con colpocitología oncótica alterada, en un servicio público de referencia en Maringá, Sur de Brasil. Los datos fueron colectados de los prontuarios médicos y se estudiaron las variables diagnóstico definitivo, tipos de tratamiento, ocurrencia de la lesión y reincidencias y se analizaron por medio de pruebas de asociación de chi-cuadrado de Pearson y exacto de Fisher. RESULTADOS: La lesión intraepitelial cervical de alto grado ocurrió en 168 casos; de estos, 31 mujeres se sometieron a la amputación cónica, 104 a cirugías de alta frecuencia, nueve a histerectomías y 24 recibieron conducta conservadora. Entre las mujeres con lesión de alto grado y tratadas de forma conservadora, ocho (33,3%) reincidieron, mientras que de las sometidas a la conducta no conservadora, diez (6,9%) reincidieron, siendo esta diferencia estadísticamente significativa (p=0,0009), RP=4,8 (IC95% 2,11;10,93). En aquellas que hicieron seguimiento clínico-citológico, tres (30,0%) y, entre las cauterizadas, cinco (35,7%) reincidieron en el plazo de tres años, sin diferencia significativa (p=0,5611). La reincidencia por debajo y por encima de los 30 años ocurrió, respectivamente, en siete (13,8%) y 11 (12,2%) mujeres (p=0,9955). CONCLUSIONES: La edad de la mujer no influencia el pronóstico de la reincidencia. El tratamiento conservador debe ser indicado como conducta de excepción, dada la alta tasa de reincidencia, y el seguimiento debe ser riguroso, con acompañamiento citológico y colposcópico por inclusive tres años, período en el que ocurre la mayoría de las reincidencias.
Cuello del Útero; Neoplasias del Cuello Uterino; Neoplasia Intraepitelial del Cuello Uterino; Conización; Electrocoagulación; Estudios Transversales
ORIGINAL ARTICLES
Evaluation of conservative management of high-grade cervical squamous intraepithelial lesion
Evaluación de la conducta conservadora en la lesión intraepitelial cervical de alto grado
Nelson Shozo UchimuraI; Taqueco Teruya UchimuraI; João Paulo de Oliveira Branco MartinsI; Fernando AssakawaI; Liza Yurie Teruya UchimuraII
IDepartamento de Medicina. Centro de Ciências da Saúde. Universidade Estadual de Maringá. Maringá, PR, Brasil
IIPrograma de Residência Médica em Medicina de Família e Comunidade. Centro de Ciências Biológicas e da Saúde. Pontifícia Universidade Católica do Paraná. Curitiba, PR, Brasil
Correspondence Correspondence: Nelson Shozo Uchimura Hospital Universitário de Maringá Departamento de Medicina Av. Mandacaru, 1590, zona 21, Laranjeiras 87083-240 Maringá, PR, Brasil E-mail: nuchimura@hotmail.com
ABSTRACT
OBJECTIVE: To analyze the association between conservative management of high-grade cervical squamous intraepithelial lesions and recurrence rates and age groups.
METHODS: Cross-sectional, retrospective, analytical observational study of 509 women (aged 15 to 76) with abnormal Pap smears attending a public reference center in the city of Maringá, southern Brazil, from 1996 to 2006. Data was collected from medical records, and the variables definitive diagnosis, type of treatment provided, occurrence of high-grade cervical squamous intraepithelial lesions and recurrence were studied. Pearson's chi-square test and Fisher's exact test were used in the statistical analyses.
RESULTS: There were 168 cases of cervical high-grade cervical squamous intraepithelial lesions, of these, 31 were treated with cold-knife conization, 104 loop electrosurgical excision procedure, 9 hysterectomy and 24 conservative treatment (i.e., clinical and cytological follow-up or cervical electrocoagulation). A total of 8 (33.3%) women receiving conservative and 10 (6.9%) receiving non-conservative management had recurrent disease and this difference was statistically significant (p=0.0009), PR = 4.8 (95%CI 2.11;10.93). Three (30.0%) women among those undergoing clinical and cytological follow-up and five (35.7%) among those submitted to cervical electrocoagulation had recurrent disease within three years, but the difference was not significant (p=0.5611). Recurrent rates in those younger and older than 30 were 13.8% (7 women) and 12.2% (11 women) (p = 0.9955).
CONCLUSIONS: Age is not a predictor of disease recurrence. Conservative treatment is only recommended in exceptional situations due to its high recurrence rates. Careful cytological and colposcopic follow-up is required for three years when most recurrences occur.
Descriptors: Cervix Uteri, anatomy & histology. Uterine Cervical Neoplasms, therapy. Cervical Intraepithelial Neoplasia, therapy. Conization. Electrocoagulation. Cross-Sectional Studies.
RESUMEN
OBJETIVO: Analizar la asociación entre la conducta conservadora en lesión intraepitelial cervical de alto grado con el índice de reincidencia de la neoplasia y grupo etario.
MÉTODO: Estudio transversal y retrospectivo realizado con 509 mujeres (15-76 años) atendidas en el período de 1996 a 2006, con colpocitología oncótica alterada, en un servicio público de referencia en Maringá, Sur de Brasil. Los datos fueron colectados de los prontuarios médicos y se estudiaron las variables diagnóstico definitivo, tipos de tratamiento, ocurrencia de la lesión y reincidencias y se analizaron por medio de pruebas de asociación de chi-cuadrado de Pearson y exacto de Fisher.
RESULTADOS: La lesión intraepitelial cervical de alto grado ocurrió en 168 casos; de estos, 31 mujeres se sometieron a la amputación cónica, 104 a cirugías de alta frecuencia, nueve a histerectomías y 24 recibieron conducta conservadora. Entre las mujeres con lesión de alto grado y tratadas de forma conservadora, ocho (33,3%) reincidieron, mientras que de las sometidas a la conducta no conservadora, diez (6,9%) reincidieron, siendo esta diferencia estadísticamente significativa (p=0,0009), RP=4,8 (IC95% 2,11;10,93). En aquellas que hicieron seguimiento clínico-citológico, tres (30,0%) y, entre las cauterizadas, cinco (35,7%) reincidieron en el plazo de tres años, sin diferencia significativa (p=0,5611). La reincidencia por debajo y por encima de los 30 años ocurrió, respectivamente, en siete (13,8%) y 11 (12,2%) mujeres (p=0,9955).
CONCLUSIONES: La edad de la mujer no influencia el pronóstico de la reincidencia. El tratamiento conservador debe ser indicado como conducta de excepción, dada la alta tasa de reincidencia, y el seguimiento debe ser riguroso, con acompañamiento citológico y colposcópico por inclusive tres años, período en el que ocurre la mayoría de las reincidencias.
Descriptores: Cuello del Útero, anatomía & histología. Neoplasias del Cuello Uterino, terapia. Neoplasia Intraepitelial del Cuello Uterino, terapia. Conización. Electrocoagulación. Estudios Transversales.
INTRODUCTION
The most effective approach to cervical cancer control is early diagnosis and treatment of precursor lesions called cervical intraepithelial neoplasia (CIN) and invasive lesions at early stages, with chance of cure in nearly 100%.9
Cervical cancer prevention and control strategies in Brazil have been planned based on distribution of cervical lesions by age and frequency of Pap smears. Declining cervical cancer rates can be attributed to both the "Viva Mulher" Program, which increased detection of CIN, low-grade cervical squamous intraepithelial lesion (LGSIL) and high-grade cervical squamous intraepithelial lesion (HSIL), and the successful treatment referral through the See and Treat program, which was implemented by the Brazilian Ministry of Health in 1997. At the See and Treat program, a woman cytologically and colposcopically diagnosed with LGSIL undergoes loop electrosurgical excision procedure (LEEP).13 LEEP is a relatively safe, low-cost outpatient procedure performed under local anesthesia that allows pathological examination of the excised cervical specimen.15
However, there is a risk of overtreatment when LEEP is performed without prior cervical biopsy because of cellular atypia leading to false-positive results on cytology17 and spontaneous remission, or even small lesions that could be completely removed in a regular biopsy.10 Though it is simple, low-cost procedure LEEP may cause complications such as bleeding, infection, stenosis and cervical obliteration resulting in hematometra or even infertility and pregnancy complications.14
Cervical changes have been increasingly found in young childbearing women due to risk factors such as human papillomavirus (HPV) infection, multiple sexual partners, low socioeconomic condition, oral contraceptive use, early sexual initiation and smoking.2,8
The See and Treat method is not recommended for treating adolescents with HSIL. The latest guidelines suggest conservative management of these women with semiannual cytologic and colposcopic monitoring.3 Clinical and cytologic follow-up and cervical cauterization are conservative managements while LEEP, cold-knife conization and hysterectomy are non-conservative managements.11 Cervical conization and cold-knife conization are both diagnostic and treatment procedures. The diagnosis is made by histological examination and treatment is given through lesion removal in the excised surgical specimen. Despite being a simple procedure, this procedure has complications including infection, bleeding, stenosis or cervical os obliteration, as well as cervical incompetence causing serious fertility issues. These are costly procedures including hospitalization and anesthesia.6
Adequate HSIL treatment is affected by several factors including age, desire to maintain fertility and health status.
As for early diagnosis of HSIL, there was no significant difference between immediate colposcopy and cytologic follow-up during clinical and cytologic follow-up every three to six months.16
Clinical and cytologic follow-up is intended for monitoring potential remission of lesions an preventing an ablative procedure.16 Forty percent of women younger than 30 with HSIL show remission within one year.7 When an invasive carcinoma is ruled out by cytology, colposcopy and biopsy, cauterization can be a destructive treatment approach.1,11
This study aimed to assess the association between conservative management of HSIL and cancer recurrence rates and age groups.
METHODS
A cross-sectional retrospective study with women attending a public reference center was conducted in the city of Maringá, Southern Brazil.
All patients with abnormal Pap smears during the first visit were included in the study from January 1996 to December 2006. Exclusion criteria included prior hysterectomy; women with only one abnormal Pap smear and/or biopsy and no subsequent visits; endocervical polyps; and condylomata acuminate with no abnormal Pap smears.
Data were collected from medical records. Demographic (age, marital status), gynecological (number of pregnancies, births, cesarean deliveries and abortions, number of sexual partners, sexually transmitted diseases, hormonal contraceptive use) and behavioral information (smoking and alcohol use) was collected.
The following clinical variables were studied: definitive diagnosis, type of treatment provided, incidence of HSIL and recurrence after treatment.
Definitive diagnosis was made after colposcopy, Pap smears and histology examination. Conservative management included clinical and cytologic follow-up and cervical cauterization and non-conservative management included LEEP, cold-knife conization and hysterectomy.
Recurrence of a lesion was defined as cytological atypia, abnormal colposcopic findings, and histopathology findings of HPV or CIN in the follow-up within six months after treatment. HSIL remission was considered for all other cases with no recurrence.
Qualitative variables (types of treatment -conservative or non-conservative; conservative treatment -follow-up or cauterization; age - <30 or >30 years; and recurrences) were described as absolute and relative frequencies. The associations between variables were assessed using Pearson's chi-square test and Fisher's exact test at a 5% significance level. Prevalence ratios and 95% confidence intervals were calculated. Data were collected using Microsoft Excel® spreadsheets and analyzed using Statistica v.8.0.
The study was approved by the Standing Human Research Ethics Committee of Universidade Estadual de Maringá (protocol nr. 121/2006).
RESULTS
A total of 509 patients aged 15 to 76 years with a median of 34 years were studied. During the study period HSIL was diagnosed in 168 cases (33.2%); LSIL in 104 (20.4%); invasive cancer in 36 (7.0%); and chronic cervicitis in 201 (39.4%).
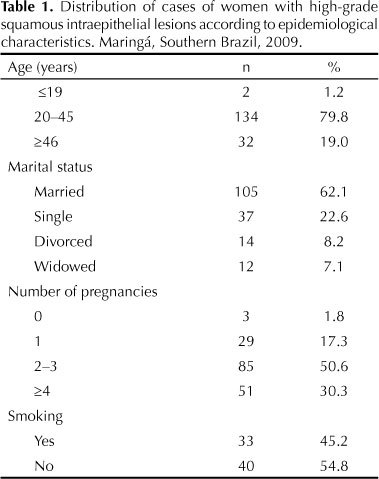
There were two cases (1.2%) of HSIL among adolescents and younger women and 134 (79.8%) cases among those aged between 20 and 45 years.
As for pregnancy, three women (1.8%) were nulligravida, and 29 (17.3%) had one child (Table 1).
Most cases (31; 18.5%) were treated with cold-knife conization; 104 (61.8%) with LEEP; nine (5.4%) with hysterectomy; and 24 (14.3%) with conservative treatment.
Among those with a definitive diagnosis of HSIL after conservative or non-conservative treatment, 18 (10.7%) recurred within three years. Of these, nine (50%) recurred within one year and nine within one to three years. the rate of remission of HSIL was 89.3% (150/168) Therefore, regardless of the type of treatment, (Table 2).
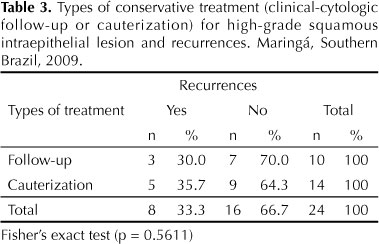
Among women undergoing conservative treatment, 10 received clinical-cytologic follow-up every three months and 14 underwent cervical cauterization with recurrence rates of 30.0% (3 cases) and 35.7% (five cases) within three years. The rate of spontaneous remission of HSIL was 70% (7/10) while remission after cauterization was 64.3% (9/14), but this difference was not significant (p = 0.5611) (Table 3).
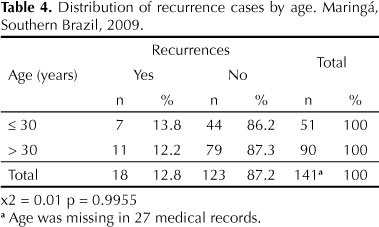
All types of treatment were grouped as no significant difference was seen between types of treatment and age at recurrence in the univariate analysis (Fisher's exact test). Recurrence was seen in seven (13.8%) women younger than 30 and 11 (12.2%) older than 30 (Table 4). This difference was not statistically significant (p = 0.9955).
DISCUSSION
Many studies have been conducted aiming at improving cost-effectiveness of HSIL treatment. Less aggressive treatments including LEEP and laser conization have been developed. Although these are surgical procedures that do not require hospitalization and show better outcomes in terms of complications such as stenosis and cervical incompetence, they are costly interventions requiring trained staff and use of sophisticated equipment.
Conservative management of HSIL could be a simple, affordable and feasible treatment option that can be performed in outpatient gynecological settings and primary care units. However, there is no consensus in the literature regarding spontaneous remission and recurrence after treatment of HSIL.
The ASCUS (atypical squamous cells of undetermined significance) / LSIL (low-grade squamous intraepithelial lesions) Triage Study for Cervical Cancer was a multicenter randomized study conducted in several U.S. sites that evaluated women with ASCUS and LSIL referred to colposcopy-guided biopsy and hybrid capture 2 test who received two-year clinical follow-up. The clinical-cytologic follow-up showed 40% remission of CIN-2 lesions, and HPV-16-positive lesions had a worse prognosis than other oncogenic HPV lesions. There was no evidence of remission in CIN-3 lesions.4
A studya a Lian IT. A eletrocoagulação na terapêutica das lesões intra-epiteliais escamosas de alto grau do colo uterino. [Master's dissertation]. Botucatu: UNESP Medical School; 2001. carried out in Botucatu (2003), Southeastern Brazil, including 116 women with HSIL reported lesion remission after cauterization in 73.5% and spontaneous remission in only 22.4%. The authors concluded that cauterization is not an effective treatment of HSIL because of failure of achieving complete remission of lesions as three women (6.1%) in the study showed progression to invasive cancer.
The Cervical Intraepithelial Neoplasia Cohort Study, a retrospective study of cytology records conducted by the British Columbia Cancer Agency between 1986 and 2000, evaluated lesion regression in CIN cases treated with criocauterization, loop diathermy conization, cold-knife conization, laser vaporization and laser excision conization and receiving long-term follow-up (six years). It showed that conservative treatment with criocauterization is associated with high recurrence rates (34%) and three times likelihood of developing cancer after treatment (OR = 2.98, 95%CI 30.9;37.1) when compared to other treatments.12
Recurrence rates found in our study corroborate those reported in the literature as women treated conservatively with clinical-cytologic follow-up (30.0%) and cauterization of the cervix (35.7%) had recurrence within three years, and this difference not significant (p = 0.5611). Furthermore, the risk of recurrence was five times higher than that with non-conservative treatment (PR = 4.8, 95%CI 2.11;10.93) (Table 3).
In view of its high recurrence rate, a conservative approach should be recommended to young women who want to conceive or those with high surgical risk and it is required a strict follow-up every three months for the first year and twice a year for the second year. If HSIL persists after 24 months of follow-up, it is recommended treatment with loop diathermy conization.18
Patient age should also be taken into consideration because remission rate in women younger than 30 is significantly higher compared to those older than 30, probably due to a more competent immune response.18 In the present study, recurrence rate in women younger than 30 was 13.8% (86.2% spontaneous remission) while in those older than 30 was 12.2% (87.8% remission), but this difference was not significant (p = 0.9955). Thus, age was not a prognostic predictor of recurrence despite the limitations of a small sample size.
The recurrence rate of 6.9% found in this study for non-conservative treatment is corroborated in the literature when about 10% of women were treated with conization. Yet, all recurrences were seen within three years, confirming the expected rate within 30 months.6 Women treated with hysterectomy showed no recurrence; many authors consider hysterectomy the definitive treatment of HSIL because the literature shows a recurrence rate of 7.3% in the vaginal vault.5
Our findings show that treatment approach for HSILs should be weighed up carefully. Given its high recurrence rates a conservative approach should be recommended only in exceptional situations in settings where treatment is provided by an integrated multidisciplinary team and cytology, colposcopy, and histopathology are available.
REFERENCES
Received: 5/21/2011
Approved: 12/11/2011
The authors declare no conflicts of interests
- 1. Boss JD. The use of electrosurgical techniques in the management of premalignant diseases of the vulva, vagina, and cervix: an excisional rather than an ablative approach. Am J Obstet Gynecol 1993;169(5):1081-5.
- 2. Brisson J, Morin C, Fortier M, Roy M, Bouchard C, Leclerc J, et al. Risk factors for cervical intraepithelial neoplasia: differences between low and high-grade lesions. Am J Epidemiol1994;140(8):700-10.
- 3. Campos LRF, Marotta HMOM, Marski HS, Anjos IC, Andrade LZ, Monteiro DLM. Conduta conservadora em adolescentes com lesão intraepitelial cervical de alto grau. Femina 2010;38(12):645-9.
- 4. Castle PE, Schiffman M, Wheeler CM, Solomon D. Evidence for Frequent Regression of Cervical Intraepithelial Neoplasia-Grade 2. Obstet Gynecol 2009;113(1):18-25.
- 5. Coronel-Brizio P, Olivares Nowak J, Palafox Sánchez F. Recurrencia de la lesión intraepitelial escamosa de alto grado posterior a histerectomia. Ginecol Obstet Mex.1999;67(9):415-8.
- 6. Derchain SFM, Longatto Filho AL, Syrjanen KJ. Neoplasia intra-epitelial cervical: diagnóstico e tratamento. Rev Bras Ginecol Obstet 2005;27(7):425-33. DOI:10.1590/S0100-72032005000700010
- 7. Fuchs K, Weitzen S, Wu L, Phipps MG, Boardman LA. Management of cervical intraepithelial neoplasia 2 in adolescent and young women. J Pediatr Adolesc Gynecol 2007; 20(5):269-74. DOI:10.1016/j.jpag.2007.04.012
- 8. Galloway DA. Papillomavirus vaccines in clinical trails. Lancet Infect Dis 2003;3(8):469-75. DOI:10.1016/S1473-3099(03)00720-5
- 9. Intituto Nacional de Câncer. Neoplasia Intra-epitelial cervical -NIC. Condutas do INCA/MS - Procedures. Rev Bras Cancer 2000;46(4):355-7.
- 10. Juliato CRT, Teixeira JC, Derchain SFM, Barbosa SB, Martinez EZ, Panetta K, et al. Correlação entre o diagnóstico histológico da biópsia e o da conização por Cirurgia de Alta Frequência por Alça (CAF) no tratamento da neoplasia intra-epitelial cervical. Rev Bras Ginecol Obstet 2000;22(2):65-70. DOI:10.1590/S0100-72032000000200002
- 11. Lian IT, Sampaio Neto LF, Ferro MC, Menegoci JC, Traiman P. O uso da eletro coagulação na terapêutica das lesões intra-epiteliais escamosas de alto grau do colo uterino. Rev Ginecol Obstet 2003;14(2):60-2.
- 12. Melnikow J, McGahan C, Sawaya GF, Ehlen T, Coldman A. Cervical intraepithelial neoplasia outcomes after treatment:long-term follow-up from the British Columbia Cohort Study. J Natl Cancer Inst 2009;101(10):721-8. DOI:10.1093/jnci/djp089.
- 13. Monteiro ACS, Russomano F, Reis A, Camargo MJ, Fialho SA, Tristão MA, et al. Effectiveness of see-and-treat for approaching pre-invasive lesions of uterine cervix. Rev Saude Publica 2009;43(5):846-50. DOI:10.1590/S0034-89102009000500014
- 14. Monteiro ACS, Russomano FB, Camargo MJ, Silva KS, Veiga FR, Oliveira RG. Cervical stenosis following electrosurgical conization. Sao Paulo Med J 2008;126(4):209-14. DOI:10.1590/S1516-31802008000400002
- 15. Ryu A, Nam K, Chung S, Kim J, Lee H, Koh E, et al. Absence of dysplasia in the excised cervix by a loop electrosurgical excision procedure in the treatment of cervical intraepithelial neoplasia. J Gynecol Oncol 2010;21(2):87-92. DOI:10.3802/jgo.2010.21.2.87
- 16. TOMBOLA Group. Cytological surveillance compared with immediate referral for colposcopy in management of women with low grade cervical abnormalities: multicentre randomised controlled trial. BMJ. 2009;339:b2546. DOI:10.1136/bmj.b2546
- 17. Uchimura NS, NakanoK, Nakano LCG, UchimuraTT. Qualidade e desempenho das colpocitologias na prevenção de câncer de colo uterino. Rev Assoc Med Bras 2009;55(5):569-74. DOI:10.1590/S0104-42302009000500021
- 18. Wright Jr TC, Massad LS, Dunton CJ, Spitzer M, Wilkinson EJ, Solomon D. 2006 consensus guidelines for the management of women with abnormal cervical cancer screening tests. Am J Obst Gynecol 2007;197(4):346-55. DOI:10.1016/j.ajog.2007.07.047
Publication Dates
-
Publication in this collection
27 Mar 2012 -
Date of issue
June 2012
History
-
Received
21 May 2011 -
Accepted
11 Dec 2012