Abstracts
OBJECTIVE: To develop and validate a short health literacy assessment tool for Portuguese-speaking adults. METHODS: The Short Assessment of Health Literacy for Portuguese-speaking Adults is an assessment tool which consists of 50 items that assess an individual's ability to correctly pronounce and understand common medical terms. We evaluated the instrument's psychometric properties in a convenience sample of 226 Brazilian older adults. Construct validity was assessed by correlating the tool scores with years of schooling, self-reported literacy, and global cognitive functioning. Discrimination validity was assessed by testing the tool's accuracy in detecting inadequate health literacy, defined as failure to fully understand standard medical prescriptions. RESULTS: Moderate to high correlations were found in the assessment of construct validity (Spearman's coefficients ranging from 0.63 to 0.76). The instrument showed adequate internal consistency (Cronbach's alpha=0.93) and adequate test-retest reliability (intraclass correlation coefficient=0.95). The area under the receiver operating characteristic curve for detection of inadequate health literacy was 0.82. A version consisting of 18 items was tested and showed similar psychometric properties. CONCLUSIONS: The instrument developed showed good validity and reliability in a sample of Brazilian older adults. It can be used in research and clinical settings for screening inadequate health literacy.
Health Literacy; Aged; Questionnaires; Translations; Validation Studies; Health Education; SAHLPA
OBJETIVO: Desenvolver e validar um instrumento breve para avaliação de alfabetismo em saúde na língua portuguesa. MÉTODOS: O instrumento desenvolvido consiste de 50 itens que avaliam a capacidade do indivíduo de pronunciar e compreender termos médicos comuns. As propriedades psicométricas foram avaliadas em uma amostra de 226 idosos brasileiros. A validade de construto foi estabelecida pela correlação com o número de anos de escolaridade, relato de alfabetismo funcional e desempenho cognitivo global. A validade discriminativa foi estabelecida pela acurácia do instrumento na detecção de alfabetismo em saúde inadequado, definido como a incapacidade de compreender corretamente prescrições médicas padronizadas. RESULTADOS: As correlações com os critérios de construto apresentaram magnitude moderada a alta (coeficientes de Spearman = 0,63 a 0,76). O instrumento apresentou ainda consistência interna satisfatória (Cronbach = 0,93) e boa confiabilidade teste-reteste (coeficiente de correlação intraclasse = 0,95). A área sob a curva característica de operação do receptor para detecção de alfabetismo inadequado foi 0,82. Uma versão com 18 itens foi derivada e apresentou propriedades psicométricas similares. CONCLUSÕES: O instrumento desenvolvido apresentou boa validade e consistência em uma amostra de idosos brasileiros e pode ser utilizado em ambientes clínicos ou de pesquisa com a finalidade de detectar alfabetismo em saúde inadequado.
Alfabetização em Saúde; Idoso; Questionários; Traduções; Estudos de Validação; Educação em Saúde; SAHLPA
OBJETIVO: Desarrollar y validar un instrumento breve para evaluación de alfabetismo en salud en el idioma portugués. MÉTODOS: El instrumento desarrollado consiste de 50 itens que evalúan la capacidad del individuo de pronunciar y comprender términos médicos comunes. Las propiedades psicométricas se evaluaron en una muestra de 226 ancianos brasileños. La validez del constructo se estableció por la correlación con el número de años de escolaridad, relato de alfabetismo funcional y desempeño cognitivo global. La validez discriminatoria fue establecida por la exactitud del instrumento en la detección de alfabetismo en salud inadecuado, definido como la incapacidad de comprender correctamente prescripciones médicas estandarizadas. RESULTADOS: Las correlaciones con los criterios de constructo presentaron magnitud moderada a alta (coeficientes de Spearman = 0,63 a 0,76). El instrumento presentó también consistencia interna satisfactoria (Cronbach = 0,93) y buena confiabilidad examen-reexamen (coeficiente de correlación intra-clase = 0,95). El área bajo la curva característica de operación del receptor para detección de alfabetismo inadecuado fue 0,82. Una versión con 18 itens fue derivada y presentó propiedades psicométricas similares. CONCLUSIONES: El instrumento desarrollado presentó buena validez y consistencia en una muestra de ancianos brasileños y puede ser utilizado en ambientes clínicos o de investigación con la finalidad de detectar alfabetismo en salud inadecuado.
Alfabetización en Salud; Anciano; Cuestionarios; Traducciones; Estudios de Validación; Educación en Salud; SAHLPA
Short Assessment of Health Literacy for Portuguese-speaking Adults
Avaliação breve de alfabetismo em saúde em português
Evaluación breve de alfabetismo en salud en portugués
Daniel ApolinarioI; Rafaela de Castro Oliveira Pereira BragaI; Regina Miksian MagaldiI; Alexandre Leopold BusseI; Flavia CamporaI; Sonia BruckiII; Shoou-Yih Daniel LeeIII
IServiço de Geriatria. Faculdade de Medicina (FM). Universidade de São Paulo (USP). São Paulo, SP, Brasil
IIDepartamento de Neurologia. FM-USP. São Paulo, SP, Brasil
IIISchool of Public Health. University of Michigan. Ann Arbor, MI, USA
Correspondence Correspondence: Daniel Apolinario Universidade de São Paulo - USP Av. Dr. Enéas de Carvalho Aguiar, 155 8º Andar, Bloco 8 - Cerqueira Cesar 05403-900 São Paulo, SP, Brasil E-mail: daniel.apolinario@usp.br
ABSTRACT
OBJECTIVE: To develop and validate a short health literacy assessment tool for Portuguese-speaking adults.
METHODS: The Short Assessment of Health Literacy for Portuguese-speaking Adults is an assessment tool which consists of 50 items that assess an individual's ability to correctly pronounce and understand common medical terms. We evaluated the instrument's psychometric properties in a convenience sample of 226 Brazilian older adults. Construct validity was assessed by correlating the tool scores with years of schooling, self-reported literacy, and global cognitive functioning. Discrimination validity was assessed by testing the tool's accuracy in detecting inadequate health literacy, defined as failure to fully understand standard medical prescriptions.
RESULTS: Moderate to high correlations were found in the assessment of construct validity (Spearman's coefficients ranging from 0.63 to 0.76). The instrument showed adequate internal consistency (Cronbach's alpha=0.93) and adequate test-retest reliability (intraclass correlation coefficient=0.95). The area under the receiver operating characteristic curve for detection of inadequate health literacy was 0.82. A version consisting of 18 items was tested and showed similar psychometric properties.
CONCLUSIONS: The instrument developed showed good validity and reliability in a sample of Brazilian older adults. It can be used in research and clinical settings for screening inadequate health literacy.
Descriptors: Health Literacy. Aged. Questionnaires. Translations. Validation Studies. Health Education. SAHLPA.
RESUMO
OBJETIVO: Desenvolver e validar um instrumento breve para avaliação de alfabetismo em saúde na língua portuguesa.
MÉTODOS: O instrumento desenvolvido consiste de 50 itens que avaliam a capacidade do indivíduo de pronunciar e compreender termos médicos comuns. As propriedades psicométricas foram avaliadas em uma amostra de 226 idosos brasileiros. A validade de construto foi estabelecida pela correlação com o número de anos de escolaridade, relato de alfabetismo funcional e desempenho cognitivo global. A validade discriminativa foi estabelecida pela acurácia do instrumento na detecção de alfabetismo em saúde inadequado, definido como a incapacidade de compreender corretamente prescrições médicas padronizadas.
RESULTADOS: As correlações com os critérios de construto apresentaram magnitude moderada a alta (coeficientes de Spearman = 0,63 a 0,76). O instrumento apresentou ainda consistência interna satisfatória (Cronbach = 0,93) e boa confiabilidade teste-reteste (coeficiente de correlação intraclasse = 0,95). A área sob a curva característica de operação do receptor para detecção de alfabetismo inadequado foi 0,82. Uma versão com 18 itens foi derivada e apresentou propriedades psicométricas similares.
CONCLUSÕES: O instrumento desenvolvido apresentou boa validade e consistência em uma amostra de idosos brasileiros e pode ser utilizado em ambientes clínicos ou de pesquisa com a finalidade de detectar alfabetismo em saúde inadequado.
Descritores: Alfabetização em Saúde. Idoso. Questionários. Traduções. Estudos de Validação. Educação em Saúde. SAHLPA.
RESUMEN
OBJETIVO: Desarrollar y validar un instrumento breve para evaluación de alfabetismo en salud en el idioma portugués.
MÉTODOS: El instrumento desarrollado consiste de 50 itens que evalúan la capacidad del individuo de pronunciar y comprender términos médicos comunes. Las propiedades psicométricas se evaluaron en una muestra de 226 ancianos brasileños. La validez del constructo se estableció por la correlación con el número de años de escolaridad, relato de alfabetismo funcional y desempeño cognitivo global. La validez discriminatoria fue establecida por la exactitud del instrumento en la detección de alfabetismo en salud inadecuado, definido como la incapacidad de comprender correctamente prescripciones médicas estandarizadas.
RESULTADOS: Las correlaciones con los criterios de constructo presentaron magnitud moderada a alta (coeficientes de Spearman = 0,63 a 0,76). El instrumento presentó también consistencia interna satisfactoria (Cronbach = 0,93) y buena confiabilidad examen-reexamen (coeficiente de correlación intra-clase = 0,95). El área bajo la curva característica de operación del receptor para detección de alfabetismo inadecuado fue 0,82. Una versión con 18 itens fue derivada y presentó propiedades psicométricas similares.
CONCLUSIONES: El instrumento desarrollado presentó buena validez y consistencia en una muestra de ancianos brasileños y puede ser utilizado en ambientes clínicos o de investigación con la finalidad de detectar alfabetismo en salud inadecuado.
Descriptores: Alfabetización en Salud. Anciano. Cuestionarios. Traducciones. Estudios de Validación. Educación en Salud. SAHLPA.
INTRODUCTION
Health literacy is defined as the ability to perform basic reading and numerical tasks required to function in the health care environment.1 There is increasing evidence that health literacy skills are related to important health outcomes, even after adjustments for confounding factors such as education, age, and gender. Inadequate health literacy has been independently associated with lower utilization of preventive services, poor self-management of chronic conditions, low medication adherence, increased hospitalization, and higher death rates.4
Some population groups are at greater risk for inadequate health literacy including the socioeconomically disadvantaged, immigrants, and older adults. Inadequate health literacy may disproportionately affect the health of older people, not only as a result of generation gap in education, but also because the elderly have more medical conditions, use more health care services, and are more likely to require complex therapeutic regimens.12
Because years of formal schooling alone are not a reliable indicator of health literacy and individuals with lower health literacy skills may try to hide it, it is difficult to recognize those patients with inadequate health literacy during routine clinical care.15 Developing valid and reliable health literacy instruments is critically important as they help health care providers to identify patients who may require special communication needs and benefit from targeted interventions in clinical settings.
The most commonly used instruments for assessing literacy in health care settings are the Test of Functional Health Literacy in Adults (TOFHLA)22 and the Rapid Estimate of Adult Literacy in Medicine (REALM).9 The TOFHLA presents tasks that simulate real-life situations and has good psychometric properties in English- and Spanish-speaking populations of developed countries. However, besides that the TOFHLA procedure may be intimidating to people with lower education, it does not adequately assess rudimentary reading skills such as comprehension of isolated words and short sentences. Thus, the TOFHLA may have limited application in populations with lower education in developing countries. In addition, the administration of TOFHLA is time-consuming; taking up to 22 minutes to administer the original version. Still, a short version of this instrument (S-TOFHLA) takes up to 12 minutes to complete.2
The REALM is an easy-to-use alternative tool that takes no more than three minutes to complete. Its design is based on the assumption that reading is a basic literacy skill and that there is high correlation between pronunciation and comprehension in English. It requires subjects to pronounce medical words that are presented in ascending order of difficulty. The REALM correlates well with other literacy tests and has high test-retest reliability.2 An effort to translate the REALM into Spanish was unsuccessful.21 Unlike English, Spanish has high phoneme-to-grapheme correspondence and regular pronunciation. A direct Spanish translation of the REALM was not able to adequately distinguish different health literacy levels because those with minimal level of education could correctly pronounce most medical words despite not fully understanding their meaning.
The Short Assessment of Health Literacy for Spanish-speaking Adults (SAHLSA) overcame the issue of phoneme-to-grapheme correspondence in Spanish by including a comprehension test.16 In the SAHLSA the examinees are asked to read aloud 50 medical terms and choose, from a list of two options, the word that is closer in meaning to each medical term. In a validation study with 201 Spanish-speaking adults living in the United States, the SAHLSA presented a significant correlation with the TOHFLA (r=0.65), good test-retest reliability (r=0.86) and high internal consistency (Cronbach's α=0.92). A short version of the SAHLSA with 18 items was later developed, and essentially showed the same psychometric properties.17
In Brazil, despite the progress made towards universal basic education in recent decades, educational attainment and functional literacy rates remain very low in some areas and in subsets of the Brazilian population. A recent cross-sectional study performed in 204 cities showed that 27% of Brazilian elders reported being illiterate and an additional 22% reported basic reading and writing problems.ª a Neri AL. Idosos no Brasil: vivências, desafios e expectativas na terceira idade. São Paulo: Edições SESC SP; 2007. Despite heterogeneous composition of the Brazilian population and its low education level, health literacy issues remain virtually unexplored in Brazil due to the lack of a valid and reliable instrument to assess it.
While planning to develop a pronunciation-based health literacy instrument in Portuguese, we realized we would have the same problem as the Spanish translation of REALM because Portuguese also has transparent orthography with high grapheme-to-phoneme correspondences. We hypothesized that the SAHLSA could be translated into Portuguese without any structural changes and with minimal semantic adjustments. The objective of this study was to adapt the SAHLSA for Portuguese-speaking population and assess the instrument's psychometric properties in a sample of Brazilian older adults.
METHODS
Translation and Adaptation
The forward translation of the SAHLSA from Spanish into Portuguese was conducted independently by two bilingual health professionals who were not involved in the study. The translators were informed on the purpose of the study and target population. To ensure concept equivalence, the translated versions of the instrument were reviewed by four members of the research team to solve any discrepancies and a consensus version was drafted. This version was pre-tested in a pilot sample of 20 older adults to identify idiomatic and cultural issues. The results were satisfactory, requiring no changes in the medical terms. Only one association word was replaced to improve clarity.
The back translation from Brazilian Portuguese into Spanish was carried out by a professional translator who was unaware of the study objectives and did not participate in any of the previous steps of the study. The assessment of equivalence showed satisfactory results; 99% of the back translation showed semantic agreement with the SAHLSA. The resulting instrument was then named the Short Assessment of Health Literacy for Portuguese-speaking Adults (SAHLPA).
SAHLPA Administration and Scoring
The administration of the SAHLPA is similar to that of the SAHLSA. We used laminated flash cards, each with a medical term printed in boldface on the top and two association words at the bottom. One of the words was meaningfully associated with the medical term and the other was not. Respondents were shown a flash card one at a time and asked to read aloud the medical term in boldface. The interviewer then read the two association words and asked the respondent which one was meaningfully associated with the medical term. Because the purpose of the association questions was to assess comprehension, respondents were instructed not to guess and say "don't know" if they did not know the correct association. The answer was deemed correct only when the respondent correctly pronounced the medical term and made the correct association. One point was scored for each correct item with a maximum score of 50. User instructions and laminated card sets are available upon request from the corresponding author.
Subjects for Validation Tests
A convenience sample of 226 older adults was interviewed from June 2009 to February 2011. Subjects were recruited from two public outpatient geriatric clinics in the city of São Paulo, southeastern Brazil. Research staff reviewed their medical records and spoke with patients to determine their eligibility. To be eligible the subject had to meet the following criteria: (1) age > 60 years; (2) self-reported ability to read and speak Portuguese; (3) no diagnosis of dementia; (4) no vision or hearing problems that would not allow adequate interaction with the interviewers. Individuals who were self-reported illiterate, i.e., were not able to read at all, were excluded from the study as testing health literacy would be purposeless. All subjects were informed of the study purpose and procedures. An informed consent was obtained before the interview.
To assess test-retest reliability a randomly selected subsample of 20 subjects was administered the SAHLPA a second time on a different day. It has been postulated that a very short time interval gives rise to practice effects, i.e., respondents become familiar with test material and test-taking procedures, whereas longer time interval increases the chances that a real change in status could occur.18 For practical reasons, the study subjects were retested during their next routine clinical visit. The mean time interval between the first and the second tests was 153 days (SD = 91 days). Because literacy skills are relatively stable over time, we believe that this time interval would provide a reasonable balance between recollection bias and unwanted clinical change.
Measures
There are no validated instruments for measuring health literacy in Portuguese and no universally accepted gold standard for the construct. Thus, we assessed the validity of the SAHLPA by correlating the test scores with variables that were shown to be conceptually and empirically associated with health literacy.6-8 For the assessment of construct validity three variables were used - formal education, self-reported functional literacy, and global cognitive functioning - and the testing was conducted in the entire sample of 226 older adults. To assess discriminative validity we correlated the SAHLPA scores with understanding of standard medical prescriptions in a sub-sample of 93 older adults.
Functional literacy was measured using the parameters of the National Functional Literacy Index,23 an initiative to assess literacy in Brazilian population. Literacy was categorized into four levels: (1) illiterate: individuals who cannot perform simple tasks involving words and numbers; (2) rudimentary: individuals who can find explicit information in short materials (e.g. advertisements, signs) and can read numbers in specific contexts (e.g. price, time); (3) basic: individuals who can read average length materials (e.g. magazine reports) and perform simple calculations (e.g. addition and subtraction); and (4) advanced: individuals who can read longer materials, make inferences, calculate percentages, interpret tables and read maps. The level of functional literacy was determined by a trained interviewer who conducted a semi-structured interview with respondents regarding their reading and numeracy abilities and then assigned them to one of the four levels based on the reported skills.
The Mini-Mental State Examination (MMSE) is a quantitative measure of cognitive status.11 It has a multi-task structure with items representing temporal orientation (five points), spatial orientation (five points), registration of words (three points), calculation skills (five points), recall of words (three points), naming of objects (two points), repetition of a sentence (one point), verbal command (three points), written command (one point), writing a sentence (one point) and coping two intersecting pentagons (one point). The total MMSE score ranges from 0 to 30, with higher scores indicating better cognitive performance. Previous studies found that performance in the MMSE was strongly and independently correlated with REALM and S-TOFHLA scores.3,19 For this study we applied a widely used Brazilian version of the MMSE.5
We adapted a structured protocol from a previous study to assess comprehension of medical prescriptions.10 A five-item electronically generated prescription was presented to the respondents with the following instructions: (1) Lactulose 667 mg/mL: "Take one tablespoon by mouth three times a day;" (2) Amlodipine Besylate 5 mg: "Take one tablet by mouth once daily;" (3) Furosemide 40 mg: "Take one tablet by mouth in the morning and one tablet at 5 pm;" (4) Calcium Citrate 200 mg: "Take two tablets by mouth twice daily;" (5) Norfloxacin 400 mg: "Take one tablet by mouth twice daily for seven days." The interviewer showed the respondent the medicine containers with standard labels, one at a time, and asked: "Following the instructions given by the doctor in the prescription, how would you take this medicine?" The respondent's verbatim answer was recorded and rated as either correct or incorrect. An answer was correct only if it included all aspects of the instructions including dosage, time, and length of drug use, if applicable. In addition, respondents were tested on numeracy skills using the calcium citrate label. After answering the question "How would you take this medicine?", they were asked "Show me how many pills you would take in one day." The medicine container was filled with tablets for respondents to count out the correct amount.
Statistical Analysis
We performed descriptive statistics to characterize the sample and the study variables. For validating the SAHLPA, we first conducted a exploratory factor analysis to assess unidimensionality - that is, all test items measuring a dominant underlying dimension. To assess the suitability of the dataset for factor analysis we performed Kaiser-Meyer-Olkin Measure of Sampling Adequacy (KMO) and the Bartlett's Test of Sphericity. A principal component factor analysis was conducted with eigenvalues and the scree plot as the extraction strategy. We used Spearman's rank test to examine the correlations between the SAHLPA and the variables in the construct validity testing because the SAHLPA scores were negatively skewed and the Kolmogorov-Smirnov test rejected normality. The discriminant validity was tested by calculating the SAHLPA ability to identify individuals who incorrectly answered one our more questions related to their comprehension of medical prescriptions. Receiver operating characteristic (ROC) curves and the areas under the curves (AUCs) were calculated. The significance level of the difference between AUCs was calculated using the DeLong's nonparametric method. Internal consistency was assessed using Cronbach's alpha coefficient. The test-retest reliability of the SAHLPA total score was estimated using intraclass correlation coefficients (ICC) in a two-way mixed model computed using absolute agreement.20
We performed an additional analysis to shorten the original SAHLPA based on the classical test theory. The general goal was to exclude items that had poor construct validity, strong floor and ceiling effects, and low internal consistency. The procedures involved: (1) eliminating items that showed poor rank biserial correlations (rrb< 0.30) with all three variables in construct validity testing (i.e., formal education, self-reported functional literacy, and global cognitive functioning); (2) excluding items with the proportion of correct answers <10% or >90% to minimize floor or ceiling effects; and (3) removing items with corrected item-total correlation coefficient <0.40 to maintain discriminative power. To generate the shortest instrument while maintaining adequate psychometric properties, we also excluded individual items with the lowest item-total correlation and repeated the procedure until Cronbach's alpha coefficient fell to 0.90. A Cronbach's alpha above this cutoff would probably reflect unnecessary duplication of content, suggesting redundancy rather than internal consistency.24
ROC curves analyses were performed using MedCalc version 11.6 (MedCalc Software, Mariakerke, Belgium). All other analyses were conducted using the Statistical Package for Social Sciences version 17.0 (SPSS Inc., Chicago, IL). All statistical tests were two-tailed, and an alpha level of less than 0.05 was used to indicate the statistical significance.
The research protocol was approved by the Research Ethics Com-mittee of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo.
RESULTS
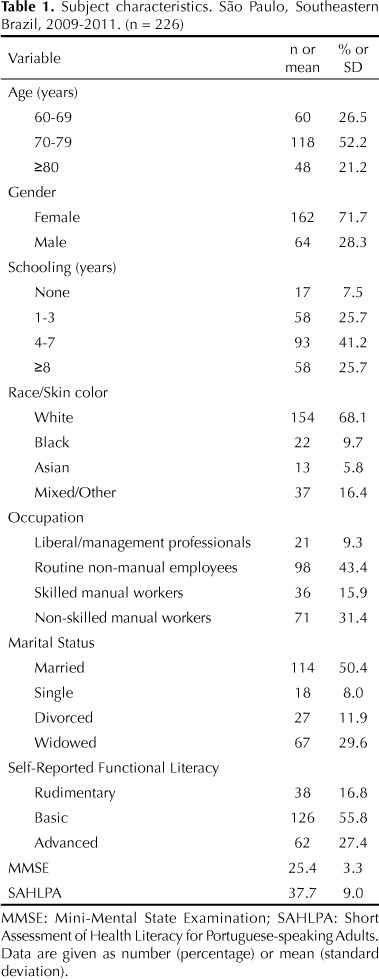
Of the 360 patients who were recruited during the study period, 17 were illiterate, 59 had a diagnosis of dementia, 4 had severe sensory impairment, 9 refused to participate, and 45 did not attend the scheduled interview. Our final sample consisted of 226 older adults with a mean age of 74.4 (SD = 6.9) years, 71.7% female, and an average 5.3 (SD = 4.0) years of schooling. The overall mean SAHLPA score was 37.7 (SD = 9.0). Based on the assessment of self-reported functional literacy, 38 (16.8%) subjects were at the rudimentary level, 126 (55.8%) at the basic level, and 62 (27.4%) at the advanced level of literacy. The mean MMSE score was 25.4 (SD = 3.3) (Table 1).
The KMO index achieved adequate level (0.87) and the Bartlett's Test of Sphericity was significant (p<0.001), indicating that the raw data were suitable for factor analysis. In the principal component analysis the ratio of the first to the second eigenvalue was 4.4 (12.8/2.9), exceeding the criterion of a ratio greater than 4.0 for evidence of unidimensionality.14 In addition, a visual examination of the scree plot showed a unidimensional factor structure (Figure 1).
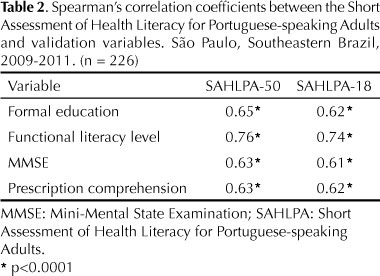
The SAHLPA score had high correlation with formal education (Spearman's r=0.65), self-reported functional literacy (Spearman's r=0.76), and MMSE score (Spearman's r=0.63), all were statistically significant, suggesting that the SAHLPA had good construct validity (Table 2).
Of the 93 subjects evaluated for comprehension of medical prescriptions, 54 (58.1%) made at least one error and were deemed to have inadequate health literacy. The SAHLPA AUC for detection of inadequate health literacy was 0.82 (95% confidence interval [95%CI] 0.74;0.90). In contrast, the formal schooling AUC was 0.67 (95%CI 0.56;0.77). By using DeLong's method, the SAHLPA had better accuracy when compared to years of formal schooling (p=0.0025). The best cutoff value of SAHLPA to detect individuals with inadequate heath literacy was <42, with 87% sensitivity and 61.5% specificity (Figure 2).
The Cronbach's alpha coefficient was 0.93, showing that the SAHLPA had satisfactory internal consistency. The test-retest reliability was excellent with an ICC of 0.95 (95%CI 0.87;0.98).
Following the validation of the psychometric properties of SAHLPA, we then proceeded to item reduction. Of the 50-item original instrument, 32 items were removed: 14 had a low correlation with all three variables used in construct validity testing, 11 showed a strong ceiling effect, and 7 had a low item-total correlation. The results of the stepwise item-reduction analysis are summarized in Table 3. The 18 remaining items comprised the shortened form of the instrument that was named SAHLPA-18 to differentiate it from the 50-item SAHLPA, SAHLPA-50. The SAHLPA-50 and SAHLPA-18 scores were highly correlated (rs=0.96; p<0.0001) and had similar correlation coefficients with the variables used in validity testing (Table 2).
With an AUC of 0.82 (95%CI 0.74; 0.91), the SAHLPA-18 was as accurate as the SAHLPA-50 in detecting inadequate health literacy. For the shortened version, a cutoff of <14 achieved the best accuracy, with 83.3% sensitivity and 66.7% specificity. Test-retest reliability was excellent for the SAHLPA-18, with an ICC of 0.91 (95% CI 0.76; 0.96). The Cronbach's alpha coefficient was 0.90, suggesting good internal consistency.
DISCUSSION
This is the first report of the validation of an instrument designed to assess health literacy in Portuguese speakers. The administration of the SAHLPA proved to be easy and well received by the study respondents. The time to complete it was short - approximately 3-6 minutes for the full version and about 1-2 minutes for the short version. In a sample of Brazilian older adults, the SAHLPA showed good to excellent psychometric properties. Moderate to high (but not excellent) correlations of the SAHLPA with validation criteria were expected, indicating that they are measuring related, but not the same constructs. An 18-item version was derived from the longer version using classical test theory, which had similar validity and reliability.
It has been suggested that health literacy probably works like a continuous construct, with higher health literacy associated with better health outcomes. However, there may be a threshold for some outcomes, i.e., a certain health literacy level is needed for a good outcome and health literacy higher than this level adds little benefit.25 Accordingly, the ability or inability to fully understand a medical prescription was used to define this threshold and set a cutoff. We believe that such a cut-off can improve the clinical usefulness of the instrument, especially when it is applied for patient screening. Further studies are needed to confirm whether the proposed threshold is appropriate.
The SAHLPA-50 found 66% of the study sample with inadequate health literacy. Although this proportion is alarming, it seems consistent with the sociodemographic composition of the sample. We anticipate that the rate of inadequate health literacy would be higher in the entire Brazilian older adult population because the mean education attainment rate reported in the national population census is slightly lower than that seen in the study sample (4.2 versus 5.3 years).b b Instituto Brasileiro de Geografia e Estatística. Pesquisa Nacional por Amostra de Domicílios: síntese de Indicadores 2008. Rio de Janeiro: IBGE; 2009.
Although health literacy and years of formal schooling were associated, 30% of the older adults with high school education had inadequate health literacy defined by the SAHLPA-50 score. On the other hand, 17% of the respondents with very low schooling (0-4 years) were considered to have adequate health literacy. Thus, we were unable to define a schooling level above which adequate literacy may be assumed without testing. Likewise, we cannot assume inadequate literacy in every individual with very low level of formal schooling.
Some limitations of the study should be noted. First, we found that SAHLPA scores were negatively skewed, suggesting that it may be more useful as a screening instrument for identifying individuals with inadequate health literacy and that it may be limited as a continuous variable for measuring health literacy skills. Second, another drawback of the SAHLPA is that it only tests reading, including pronunciation and comprehension, but not numeracy skills. It is now recognized that numeracy skills do not necessarily correlate to reading skills, especially in specific disadvantaged groups. This point to the need for developing a complementary numeracy test.13 Third, it was not possible to establish concurrent validity in our study due to the lack of an appropriate validated instrument in Brazil. Fourth, although the convenience sample recruited was relatively diverse, the study results cannot be generalized to the entire Brazilian older adult population and further research studies using a representative sample are needed to validate our findings. Finally, people from some areas in Brazil and other Portuguese-speaking countries have different accents, which may be unfamiliar to the examiner and make it difficult to determine correct pronunciation. We are unable to estimate the extent of this problem because the study subjects were recruited in only one metropolitan area and we did not test inter-rater reliability.
We conclude that the SAHLPA-50 and its short form (SAHLPA-18) are valid and reliable instruments for assessing health literacy. We believe that the development and validation of this instrument is an essential step for health literacy research in Brazil and potentially for other Portuguese-speaking countries. We hope that the development of this tool will encourage further studies and promote actions to detect inadequate health literacy and alleviate its negative impact on health outcomes.
ACKNOWLEDGEMENT
To the Centro de Referência do Idoso da Zona Norte for providing logistic support.
Received: 10/8/2011
Approved: 3/11/2012
The authors declare no conflicts of interests.
- 1. American Medical Association. Health literacy: report of the Council on Scientific Affairs. JAMA 1999;281(6):552-7. DOI:10.1001/jama.281.6.552
- 2. Baker DW, Williams MV, Parker RM, Gazmararian JA, Nurss J. Development of a brief test to measure functional health literacy. Patient Educ Couns 1999;38(1):33-42. DOI:10.1016/S0738-3991(98)00116-5
- 3. Baker DW, Gazmararian JA, Sudano J, Patterson M, Parker RM, Williams MV. Health literacy and performance on the Mini-Mental State Examination. Aging Ment Health. 2002;6(1):22-9. DOI:10.1080/13607860120101121
- 4. Berkman ND, Sheridan SL, Donahue KE, Halpern DJ, Crotty K. Low health literacy and health outcomes: an updated systematic review. Ann Intern Med. 2011;155(2):97-107. DOI:10.1059/0003-4819-155-2-201107190-00005
- 5. Brucki SM, Nitrini R, Caramelli P, Bertolucci PHF, Okamoto IH. Sugestões para o uso do mini-exame do estado mental no Brasil. Arq Neuropsiquiatr. 2003;61(3B):777-81. DOI:10.1590/S0004-282X2003000500014
- 6. Brucki SMD, Mansur LL, Carthery-Goulart MT, Nitrini R. Formal education, health literacy and Mini-Mental State Examination. Dement Neuropsychol. 2011;5(1):26-30.
- 7. Carthery-Goulart MT, Anghinah R, Areza-Fegyveres R, Bahia VS, Brucki SMD, Damin A, et al. Performance of a Brazilian population on the test of functional health literacy in adults. Rev Saude Publica 2009;43(4):631-8. DOI:10.1590/S0034-89102009005000031
- 8. Chew LD, Bradley KA, Boyko EJ. Brief questions to identify patients with inadequate health literacy. Fam Med 2004;36(8):588-94.
- 9. Davis TC, Long SW, Jackson RH, Mayeaux EJ, George RB, Murphy PW, et al. Rapid estimate of adult literacy in medicine: a shortened screening instrument. Fam Med. 1993;25(6):391-5.
- 10. Davis TC, Wolf MS, Bass PF 3rd, Thompson JA, Tilson HH, Neuberger M, et al. Literacy and misunderstanding prescription drug labels. Ann Intern Med 2006;145(12):887-94.
- 11. Folstein MF, Folstein SE, McHugh PR. "Mini-mental state": a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975;12(3):189-98. DOI:10.1016/0022-3956(75)90026-6
- 12. Gazmararian JA, Baker DW, Williams MV, Parker RM, Scott TL, Green DC, et al. Health literacy among Medicare enrollees in a managed care organization. JAMA 1999;281(6):545-51. DOI:10.1001/jama.281.6.545
- 13. Golbeck A, Paschal A, Jones A, Hsiao T. Correlating reading comprehension and health numeracy among adults with low literacy. Patient Educ Couns 2011;84(1):132-4. DOI:10.1016/j.pec.2010.05.030
- 14. Hattie J. Methodology review: assessing unidimensionality of tests and items. Applied Psychol Meas. 1985;9(2):139-64. DOI:10.1177/014662168500900204
- 15. Kelly PA, Haidet P. Physician overestimation of patient literacy: a potential source of health care disparities. Patient Educ Couns 2007;66(1):119-22. DOI:10.1016/j.pec.2006.10.007
- 16. Lee SY, Bender DE, Ruiz RE, Cho YI. Development of an easy-to-use Spanish Health Literacy test. Health Serv Res 2006;41(4 Pt 1):1392-412. DOI:10.1111/j.1475-6773.2006.00532.x
- 17. Lee SY, Stucky BD, Lee JY, Rozier RG, Bender DE. Short Assessment of Health Literacy-Spanish and English: a comparable test of health literacy for Spanish and English speakers. Health Serv Res 2010;45(4):1105-20. DOI:10.1111/j.1475-6773.2010.01119.x
- 18. Marx RG, Menezes A, Horovitz L, Jones EC, Warren RF. A comparison of two time intervals for test-retest reliability of health status instruments. J Clin Epidemiol 2003;56(8):730-5. DOI:10.1016/S0895-4356(03)00084-2
- 19. Mayeaux Jr EL, Davis TC, Jackson RH, Henry D, Patton P, Slay L, et al. Literacy and self-reported educational levels in relation to Mini-mental State Examination scores. Fam Med 1995;27(10):658-62.
- 20. McGraw KO, Wong SP. Forming inferences about some intraclass correlation coefficients. Psychol Methods 1996;1(1):30-46. DOI:10.1037/1082-989X.1.1.30
- 21. Nurss JR, Baker DW, Davis TC, Parker RM, Williams M V. Difficulties in functional health literacy screening in Spanish-speaking adults. J Read 1995;38(8):632-7.
- 22. Parker RM, Baker DW, Williams MV, Nurss JR. The test of functional health literacy in adults: a new instrument for measuring patients' literacy skills. J Gen Intern Med 1995;10(10):537-41. DOI:10.1007/BF02640361
- 23. Ribeiro VM, Vóvio CL, Moura MP. Letramento no Brasil: alguns resultados do Indicador Nacional de Alfabetismo Funcional. Educ Soc 2002;23(81):49-70. DOI:10.1590/S0101-73302002008100004
- 24. Streiner DL. Starting at the beginning: an introduction to coefficient alpha and internal consistency. J Pers Assess 2003;80(1):99-103. DOI:10.1207/S15327752JPA8001_18
- 25. Wolf MS, Feinglass J, Thompson J, Baker DW. In search of 'low health literacy': threshold vs. gradient effect of literacy on health status and mortality. Soc Sci Med 2010;70(9):1335-41. DOI:10.1016/j.socscimed.2009.12.013
Publication Dates
-
Publication in this collection
10 July 2012 -
Date of issue
Aug 2012
History
-
Received
10 Aug 2011 -
Accepted
03 Nov 2012