Abstracts
The first case of eumycetoma by Madurella grisea occurred in Southern Brazilian Region is herein related. In addition, Brazilian literature on this subject was reviewed and, the geographic distribution of this eumycetoma is presented.
Eumycetoma; Madurella grisea; Mycetoma; Subcutaneous mycoses
É relatado o primeiro caso de eumicetoma por Madurella grisea ocorrido na Região Sul (Brasil). Além disso, a literatura brasileira correspondente foi revisada e a distribuição geográfica deste tipo de eumicetoma é apresentada.
EUMYCETOMA BY Madurella grisea. REPORT OF THE FIRST CASE OBSERVED IN THE SOUTHERN BRAZILIAN REGION
Luiz Carlos SEVERO(1 (1 ) Pesquisador do CNPq; Faculdade de Medicina, Universidade Federal do Rio Grande do Sul (UFRGS), Brasil. (2 ) Serviço de Dermatologia, UFRGS, Santa Casa, Porto Alegre, RS, Brasil. (3 ) Laboratório de Microbiologia Clínica, Instituto Especializado em Pesquisa e Diagnóstico (IPD), Santa Casa, Porto Alegre, RS, Brasil. (4 ) Universidade Federal de Santa Maria, Santa Maria, RS, Brasil. ), Gerson VETORATTO(2 (1 ) Pesquisador do CNPq; Faculdade de Medicina, Universidade Federal do Rio Grande do Sul (UFRGS), Brasil. (2 ) Serviço de Dermatologia, UFRGS, Santa Casa, Porto Alegre, RS, Brasil. (3 ) Laboratório de Microbiologia Clínica, Instituto Especializado em Pesquisa e Diagnóstico (IPD), Santa Casa, Porto Alegre, RS, Brasil. (4 ) Universidade Federal de Santa Maria, Santa Maria, RS, Brasil. ), Flávio de Mattos OLIVEIRA(3 (1 ) Pesquisador do CNPq; Faculdade de Medicina, Universidade Federal do Rio Grande do Sul (UFRGS), Brasil. (2 ) Serviço de Dermatologia, UFRGS, Santa Casa, Porto Alegre, RS, Brasil. (3 ) Laboratório de Microbiologia Clínica, Instituto Especializado em Pesquisa e Diagnóstico (IPD), Santa Casa, Porto Alegre, RS, Brasil. (4 ) Universidade Federal de Santa Maria, Santa Maria, RS, Brasil. ) & Alberto Thomaz LONDERO(4 (1 ) Pesquisador do CNPq; Faculdade de Medicina, Universidade Federal do Rio Grande do Sul (UFRGS), Brasil. (2 ) Serviço de Dermatologia, UFRGS, Santa Casa, Porto Alegre, RS, Brasil. (3 ) Laboratório de Microbiologia Clínica, Instituto Especializado em Pesquisa e Diagnóstico (IPD), Santa Casa, Porto Alegre, RS, Brasil. (4 ) Universidade Federal de Santa Maria, Santa Maria, RS, Brasil. )
SUMMARY
The first case of eumycetoma by Madurella grisea occurred in Southern Brazilian Region is herein related. In addition, Brazilian literature on this subject was reviewed and, the geographic distribution of this eumycetoma is presented.
KEYWORDS: Eumycetoma; Madurella grisea; Mycetoma; Subcutaneous mycoses.
INTRODUCTION
In Brazil black grain eumycetoma have been caused by three species of fungi. They are: Madurella grisea, Madurella mycetomatis, and Exophiala jeanselmei, in that order of frequency. Cases of eumycetoma due to M. grisea have been recorded in the Brazilian States located above the Tropic of Capricorn, the majority of which in states of the Northeastern Brazilian Region2,3,11-13,15,24.
The first case of eumycetoma by M. grisea occurred in the Southernmost state of Brazil will be herein reported. In addition comments on the geographic distribution of this type of eumycetoma and on reported Brazilian cases will be presented.
CASE REPORT
On Jan/86, a 33 year-old white man, mechanic, resident in Esteio (RS) sought for medical attention due to a tumefaction of his right foot. The patient was submitted to a biopsy and, with the diagnosis of actinomycetoma, he was treated with clotrimoxazole.
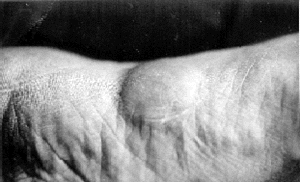
On Mar/94, the patient was admitted to our hospital complaining of the tumefaction on his right foot and pain on walking. Physical examination revealed a tumefaction (3.0 x 3.5 cm) on the plantar arch of his right foot. The skin over the lesion was slightly erythematous, but no crusts were seen neither nodules were palpated (Fig. 1).
A biopsy was then performed, part of which was preserved in formalin for hystological examination, another part was crushed and cultured.
Microbiological findings. Cut sections of biopsied tissue, stained by H&E, revealed a granulomatous lesion, productive fibrosis, and necrotic focus containing small dark brown grains. The grains, varying in size and shape, were composed of an interwoven septate hyphae (3.5 µm). In the central portion of the grain a loose network of hyaline or slightly brown hyphae were seen. The periphery was composed of a dense network of dark brown hyphae and chlamydoconidia (Fig. 2).
Slow growing colonies were obtained on Sabouraud dextrose agar, incubated at 25°C. The colonies were grayish, leathery folded and, later on, covered by a short gray aerial mycelium. Microscopic examination revealed only dematiaceous septate hyphae. Based on these findings M. grisea was identified.
Treatment and evolution. The patient was treated with itraconazole (200 mg twice a day). With the improvement of the lesion the doses was reduced to 200 mg/day.
On Oct/95 the patient returned for consultation. He had discontinued the treatment and his lesions had increased in size. Examination revealed a 3.0 x 4.0 cm tumefaction, draining a whitish secretion from the scar of the biopsy. No grains were obtained. Itraconazole was reintroduced (400 mg/day), and, on Feb/97 reduced to 200 mg/day.
After one year and five months of treatment a superficial tumefaction (3.5 cm in diameter) was still present. The tumefaction was well delimited and covered by a slightly erythematous skin. On account of the poor response to antifungal drug the patient was submitted to surgery (Jun 98).
The excised tumor measured 4.0 x 3.5 x 1.5 cm, and was composed of derma and hypoderma. Four coalescent hypodermal nodules were observed in cut section of the mass. The nodules were dun-colored, had a suppurative or purulent center containing small black grains (Fig. 3). Histologic sections of the nodules, stained by H&E, revealed that they were surrounded by a thick fibrous capsule. Inside the capsule, a granulomatous tissue, infiltrate by lymphocytes and plasma cell, in the midst of which coalescent cavities were observed. These cavities contained a neutrophilic infiltrate and black grains. Some grains were surrounded by foreign body giant cells.
About 4 months (Oct 98) after the surgery, the patient was free of pain on walking. Physical examination showed only the surgical scar in his right foot.
COMMENTARIES
Mackinnon et al16, in 1949, described M. grisea as new species based on cultures obtained from black grain eumycetoma occurred in Argentina, Chile, Paraguay, and Venezuela. Since then eumycetoma by M. grisea have been reported or recorded in the following countries of the Americas: Argentina21, Brazil13, Chile16, El Salvador14, Guatemala20, Mexico6, Paraguay21, United States6, and Venezuela22. Cases occurred also in Caribbean Islands: Curaçao4, Grenade8, and St. Christopher1. In Asia cases seems to be limited to India10, Malay19 and Philippines23. In Africa they occurred sporadically in Chad9, Madagascar18, Sudan17, and Zaire25.
Nine cases of eumycetoma by M. grisea have been related in Brazil. Patient's data, duration and localization of the lesion as well as treatment are shown in Table 1.
Five of the Brazilian cases occurred in individual5 coming from the Northeastern Region (cases 1, 2, 5, 7, and 8), a recognized endemic area of eumycetoma7. In the Centralwestern, eastern, and southern regions occurred one case each. All patients presented pedal lesions. Osseous involvement were observed in 6 of the 7 patients submitted to x-ray examination. Draining sinuses were not seen in two patients (case 5 and the present one). Both patients were submitted to two biopsies. The grain was not identified in the first biopsied tissue from patient case 5, and, in our patient it was misdiagnosed as an actinomycotic granule.
It may be presumed that eumycetoma caused by M. grisea must be more frequent in Brazil, because, at least, one case was not reported and many black grains eumycetomata have been recognized only histopathologically7.
Mycetoma by M. grisea seems to be refractory to treatment. However, proper management with antifungal drug, improving and delimiting the size of the lesion, allows to its surgical excision.
Finally, the world distribution of eumycetoma due to M. grisea resembles that of Exophiala jeanselmei. Both these diseases have been prevalent in countries of the Americas.
RESUMO
Eumicetoma por Madurella grisea. Relato do primeiro caso observado na Região Sul do Brasil
É relatado o primeiro caso de eumicetoma por Madurella grisea ocorrido na Região Sul (Brasil). Além disso, a literatura brasileira correspondente foi revisada e a distribuição geográfica deste tipo de eumicetoma é apresentada.
Correspondence to: Dr. L. C. Severo, Laboratório de Microbiologia Clínica, IPD - Santa Casa, Annes Dias 285, 90020-090 Porto Alegre, RS, Brazil. Fax (55 51) 214 8435. E-mail: severo@santacasa.tche.br
Received: 10 November 1998.
Accepted: 12 December 1998.
- 1. ANNING, S.T.; La TOUCHE, C.J. & HUNTER, G. - Madura foot (Mycetoma). Brit. J. Derm., 70: 301, 1958.
- 2. ARRUDA NETO, E.; PIGNATARI, A.C.C.; CASTELO FILHO, A.; COLOMBO, A.L. & LONGO, J.C. - Micetoma eumicótico. Relato de um caso por Madurella grisea Rev. Microbiol. (S. Paulo), 20: 495-500, 1989.
- 3. BELDA Jr., W.; CUCÉ, L.C.; DIAS, M.C. & LACAZ, C.S. - Eumicetoma de grăos pretos por Madurella grisea Rev. Inst. Med. trop. S. Paulo, 31: 195-199, 1989.
- 4. BORELLI, D. - Ceni di micopathologia venezuelana. G. ital. Derm. Sif., 5: 507-526, 1956.
- 5. BUOT, G.; LAVALLE, P.; MARIAT, F. & SUGUIL, P. - Étude épidemiologique des mycetomas au Mexique. Bull. Soc. Path. exot., 80: 329-339, 1987.
- 6. BUTZ, W.C. & AJELLO, L. - Black grain mycetoma. A case due to Madurella grisea Arch. Derm., 104: 197-201, 1971.
- 7. CASTRO, L.G.M.; BELDA Jr., W.; SALEBIAN, A. & CUCÉ, L.C. - Mycetoma: a retrospective study of 41 cases seen in Săo Paulo, Brazil, from 1978 to 1989. Mycoses, 36: 89-95, 1993.
- 8. CHADFIELD, J.W. - Mycetoma of the foot. Mycopathologia (Den Haag), 24: 130-136, 1964.
- 9. DESTOMBES, P.; RAVISSE, P. & NAZZIMOFF, O. - Bilan des mycoses profondes établi en vingt années d'histopathologie a l'Institut Pasteur de Brazzaville. Bull. Soc. Path. exot., 63: 315-324, 1970.
- 10. GOKHALAY, B.B.; PADHYE, A.A. & THIRUMALACHAR, M.J. - Madura foot in India caused by Madurella grisea Sabouraudia, 6: 305-306, 1968.
- 11. HEINS-VACCARI, E.M.; TAKAHASHI, N.; OLIVEIRA, N.R.B.; LACAZ, C.S. & PORTO, E. - Eumicetoma de grăos pretos por Madurella grisea Registro de um caso. Rev. Inst. Med. trop. S. Paulo, 24: 116-123, 1982.
- 12. LACAZ, C.S. & BELFORT, A.E. - Maduromicose podal de grăos pretos, por Madurella grisea Hospital (Rio de J.), 60: 367-374, 1961.
- 13. LACAZ, C.S. & FAVA NETTO, C. - Contribuiçăo para o estudo dos agentes etiológicos de maduromicose. Folia. clin. biol. (S. Paulo), 22: 303-337, 1954.
- 14. LLERENA, J. - Micosis subcutaneas en el Salvador. Esporotricosis, cromoblastomicosis, micetomas. Rev. Inst. Invest. med., 4: 83-97, 1975.
- 15. MACHADO, L.A.P.; RIVITTI, M.C.M.; CUCE, L.C. et al. - Eumicetoma de grăos pretos por Madurella grisea Registro de dois casos. Rev. Inst. Med. trop. S. Paulo, 34: 569-580, 1992.
- 16. MACKINNON, J.E.; FERRADA-URZUA, L.V & MONTEMAYOR, L. - Madurella grisea n. sp. A new species of fungus producing black variety of maduromycosis in South America. Mycopathologia (Den Haag), 4: 384-392, 1949.
- 17. MAHGOUB, E.l.S. - Mycetomas caused by Curvalaria lunata, Madurella grisea, Aspergillus nidulans and Nocardia brasiliensis in Sudan. Saboraudia, 11: 179-182, 1973.
- 18. MARIAT, F. - Sur la distribution geographic et la répartition des agents de mycetomes. Bull. Soc. Path. exot., 56: 35-45, 1963.
- 19. MARIAT, F. - Notes epidemiologiques a propos de mycetomes. Recent Progr. Microbiol., 8: 668-684, 1963.
- 20. MAYORGA, R.P. & CLOSE de LEON, J.E. - Sur une souche de Madurella grisea sporifera isolée d'un mycetome guatemalteque a grains boire. Sabouraudia, 4: 210-214, 1966.
- 21. NEGRONI, R. - Contribución al estudio de los micetomas en la Republica Argentina. Med cut. ibero lat. amer., 5: 353-363, 1974.
- 22. REYES, C. & BORELLI, D. - Un caso de micetoma podal por Madurella grisea Rev. Sanid. Asist. soc., 22: 445, 1957.
- 23. REYES, A.C.; TANGCO, F. & PUNSALANG Jr., A.P. - Maduromycosis. (maduromycotic mycetoma) in the Philippines caused by Madurella grisea Southeast Asian. J. trop. Med. publ. Hlth., 2: 17-21, 1971.
- 24. SILVA, M.R.R.; FERNANDES, O.F.L.; OLIVEIRA, L.M.; COSTA, M.B. & CASTRO, L.C. - Eumycetoma por Madurella grisea Relato de caso. Rev. Soc. bras. Med. trop., 24: 51-54, 1991.
- 25. VANDERPITTE, J.; BECKMAN, G. & NINANE, J. - Premier cas de pied de Madura par Madurella grisea au Congo Belge. Ann. Soc. belge. Méd. trop., 36: 493-497, 1956.
Publication Dates
-
Publication in this collection
02 July 1999 -
Date of issue
Mar 1999
History
-
Accepted
12 Dec 1998 -
Received
10 Nov 1998