Abstracts
The objective of this study was to evaluate the prevalence and risk factors associated with HCV infection in a group of HIV seropositive patients. We analyzed the medical records of 1,457 patients. All patients were tested for HCV infection by third generation ELISA. Whenever possible, a sample of the positive patients was also tested for HCV by PCR. HCV positive patients were analyzed according to their risk factors for both infections. The prevalence of anti-HCV positive patients was 17.7% (258 patients). Eighty-two (82) of these patients were also tested by PCR and 81 were positive for HCV virus (98%). One hundred fifty-one (58.5%) were intravenous drug users (IDU); 42 (16.3%) were sexual partners of HIV patients; 23 (8.9%) were homosexual males; 12 (4.7%) had received blood transfusion; 61 (17.5%) had promiscuous sexual habits; 14 (5.4%) denied any risk factor; 12 (4.7%) were sexual partners of IDU. Two hundred four patients mentioned only one risk factor. Among them, 28 (10.9%) were sexual partners of HIV-positive patients. Although intravenous drug use was the most important risk factor for co-infection, sexual transmission seemed to contribute to the high HCV seroprevalence in this group of patients.
HIV-HCV; Viral Hepatitis; Epidemiology; Seroprevalence; Brazil
O objetivo do presente estudo foi avaliar a prevalência e os fatores de risco associados à infecção pelo vírus da hepatite C (VHC) em um grupo de pacientes soropositivos para o HIV. Analisamos os prontuários médicos de 1.457 pacientes. O diagnóstico laboratorial de infecção pelo VHC foi feito utilizando-se ELISA de terceira geração. Uma parte dos pacientes soropositivos para VHC foram também submetidos à realização de PCR. Os pacientes soropositivos para VHC foram analisados em relação aos fatores de risco para ambas as infecções. A prevalência de pacientes soropositivos para VHC foi de 17,7% (258 pacientes). 82 desses pacientes foram testados para VHC por PCR e 81 (98%) apresentaram-se com resultado positivo. 151 (58,5%) referiram uso de drogas endovenosas (UDE), 42 (16,3%) eram parceiros sexuais de pacientes infectados pelo HIV, 23 (8,9%) eram homossexuais masculinos, 12 (4,7%) tinham recebido transfusão sanguínea, 61 (17,5%) referiram promiscuidade sexual, 14 (5,4%) negaram qualquer fator de risco, 12 (4,7%) eram parceiros sexuais de UDE. 204 pacientes referiram apenas um fator de risco, 51 referiram dois diferentes fatores de risco e três referiram três diferentes fatores de risco. Entre os pacientes que referiram apenas um fator de risco, 28 em 204 (10,9%) eram parceiros sexuais de pacientes infectados pelo HIV. Embora o uso de drogas endovenosas tenha sido o fator de risco mais importante na determinação da co-infecção, a transmissão sexual parece ter contribuído para a alta soroprevalência do VHC nesse grupo de pacientes.
HEPATITIS C VIRUS SEROPREVALENCE AND RISK FACTORS AMONG PATIENTS WITH HIV INFECTION
Maria Cássia J. MENDES-CORRÊA(1 This work was supported by grants from Fundação Zerbini, São Paulo. Presented in part at the 38 th Interscience Conference on Antimicrobial Agents and Chemotherapy, San Diego, California, U.S.A.,1998. ), Antonio Alci BARONE(2 This work was supported by grants from Fundação Zerbini, São Paulo. Presented in part at the 38 th Interscience Conference on Antimicrobial Agents and Chemotherapy, San Diego, California, U.S.A.,1998. ) & Cristina GUASTINI(3 This work was supported by grants from Fundação Zerbini, São Paulo. Presented in part at the 38 th Interscience Conference on Antimicrobial Agents and Chemotherapy, San Diego, California, U.S.A.,1998. )
SUMMARY
The objective of this study was to evaluate the prevalence and risk factors associated with HCV infection in a group of HIV seropositive patients. We analyzed the medical records of 1,457 patients. All patients were tested for HCV infection by third generation ELISA. Whenever possible, a sample of the positive patients was also tested for HCV by PCR. HCV positive patients were analyzed according to their risk factors for both infections. The prevalence of anti-HCV positive patients was 17.7% (258 patients). Eighty-two (82) of these patients were also tested by PCR and 81 were positive for HCV virus (98%). One hundred fifty-one (58.5%) were intravenous drug users (IDU); 42 (16.3%) were sexual partners of HIV patients; 23 (8.9%) were homosexual males; 12 (4.7%) had received blood transfusion; 61 (17.5%) had promiscuous sexual habits; 14 (5.4%) denied any risk factor; 12 (4.7%) were sexual partners of IDU. Two hundred four patients mentioned only one risk factor. Among them, 28 (10.9%) were sexual partners of HIV-positive patients. Although intravenous drug use was the most important risk factor for co-infection, sexual transmission seemed to contribute to the high HCV seroprevalence in this group of patients.
KEYWORDS: HIV-HCV; Viral Hepatitis; Epidemiology; Seroprevalence; Brazil
INTRODUCTION
Hepatitis C virus (HCV) and HIV share the same parenteral, sexual and vertical routes of transmission. Hepatitis C is primarily spread by parenteral or blood borne exposures, such as transfusion of blood products or intravenous drug use. Sexual transmission, however, can occur, occupational exposures have been reported, and perinatal transmission has been documented. This common epidemiology explains the high frequency of combined infections by this virus and HIV.
Hepatitis C virus (HCV) infection occurs throughout Brazil and until the recent introduction of serological tests for HCV, the prevalence of this infection was not known. The use of screening assays for HCV in blood banks has uncovered a large population of asymptomatic carriers. Among blood donors the prevalence of antibody to HCV (anti-HCV) varies between 0.84% to 3.4% in different parts of Brazil. In São Paulo, where this study was conducted, the prevalence of antibody to HCV in blood donors is 0.84%2 .
Populational studies on the prevalence of virus C infection are not common in Brazil. Three different studies have shown it to vary between 0 to 3%6,10,16 . Patients co-infected with both HIV and HCV have a higher risk of progression to chronic liver disease than those infected with HCV alone15,17,19. However, little is known about the effect of co-infection on the progression of HIV disease4,14,21.
Limited information is available about hepatitis C virus infection in patients with HIV infection in Brazil11,12. This study was designed as part of a protocol of treatment of patients with chronic hepatitis C and HIV infections in our department. The objective was to evaluate: 1) the prevalence of HCV, 2) the risk factors and the association among them, in a group of HIV/HCV patients, followed at our institution from January to December, 1996.
PATIENTS AND METHODS
This study was conducted at an AIDS Outpatient Clinic, which belongs to the Department of Infectious Diseases, São Paulo University School of Medicine.
From January 1996 through December 1996, 1457 patients (1009 male, 448 female), were attended at the AIDS Outpatient Clinic and were tested for HCV infection.
Laboratory data was extracted from a data base used in the follow up of these patients.
Tests for anti-HCV were done by ELISA (Abbott HCV EIA second generation and third generation) according to the manufacturer's instructions. HCV RNA was investigated by the "nested" polymerase chain reaction (PCR) using two sets of oligonucleotide primers derived from 5' non-coding region. All serologic studies were performed at the Central Laboratory of Hospital das Clinicas.
PCR tests were performed at the Laboratório de Investigação Médica em Hepatites da Faculdade de Medicina da Universidade de São Paulo. Medical records from 258 patients, co-infected by HIV and HCV were reviewed.
Demographic data, risk behaviors and clinical information were obtained from medical records and the data base used in follow up of these patients. Ninety five out of these 258 patients were also interviewed by one of the authors, comprising questions involving identification, demographic characteristics, AIDS/hepatitis knowledge, AIDS treatment, risk factors (use of intravenous illegal drugs, blood transfusion, sexual behavior, possible sexual contact with someone seropositive for either HIV or HCV, use of inhaled drugs, body piercing, tattooing). When answering the questions, the patients were asked about their sexual habits and could choose between the following categories: heterosexual, bisexual, male or female homosexual. All patients were also asked about the frequency of their sexual practice. Sexual promiscuity was defined as more than two different sexual partners during the last six months.
Statistical analysis of risk factors was performed using correspondence analysis technique8. This is an exploratory multivariate analysis that represents each level of categorical variables in a two-dimensional plan. The association between two factors may be interpreted by the size of the angles formed between vectors from the origin to each point. The smaller the angle between two levels of different factors, the stronger is the association between them.
RESULTS
The estimated prevalence of anti-HCV antibodies among the 1,457 patients tested for HCV was 17.7% with 95% confidence interval of [15.8%; 19.8%]. Among the 258 anti-HCV positive patients, 82 were also tested by HCV-RNA by "nested" polymerase chain reaction ("nested" PCR) and 81 were positive for HCV virus (98%).
Two hundred and two (82.2%) anti-HCV positive patients were male and age varied from 20 to 61 years, with mean of 34.08 and standard-deviation of 7.19 years.
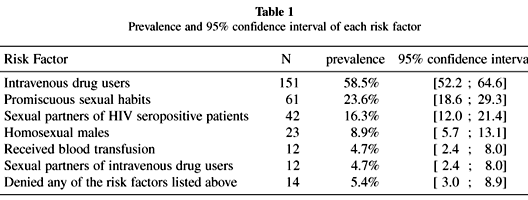
The frequency of each risk factor in these patients can be seen on Table 1.
One single factor was mentioned by 204 (79.1%) patients; two combined factors, by 51 (19.8%) patients and three combined factors, by 3 (1.2%) patients.
Among those patients who mentioned only one risk factor: 106 (41.1%) were intravenous drug users; 29 (11.2%) had more than 2 sexual partners; 28 (10.9%) were sexual partners of HIV patients (without any other risk factor for HCV); 14 (5.4%) were homosexual males; 7 (2.7%) were sexual partners of intravenous drug users; 6 (2.3%) had received blood transfusion and 14 (5.4%) denied any of the risk factors cited above. Table 2 shows the associations of risk factors.
Through correspondence analysis it was possible to infer which risk factors were more associated to each other. Figure 1 shows the vectors representing the positive status of each risk factor. It may be observed that the vectors representing the risk factors sexual partner of HIV seropositive patients and sexual partner of intravenous drug users, have small angles between them, indicating association between these risk factors.
DISCUSSION
The prevalence of antibodies to HCV in HIV infected patients varies according to the risk factor for HCV and HIV infection and to the serological assay used. Among HIV/hemophiliacs the prevalence of anti-HCV varies between 60% to 95%, and, among HIV/IDU, it may be around 70%19.
The prevalence of anti-HCV may also be underestimated by fluctuations or spontaneous disappearance of antibodies to HCV in HIV seropositive patients. WOOLEY et al.20 found out that 18 out of 52 HIV-positive patients, negative for anti-HCV, had HCV-RNA in plasma by polymerase chain reaction test.
Our study has shown that among 1,457 HIV-infected patients, 17.7% were co-infected by HCV. This seroprevalence is much higher than the prevalence among blood donors or the seroprevalence obtained through populational studies in Brazil. Such high seroprevalence is easy to understand when we analyze the epidemiology of HIV infection in Brazil.
An evolving pattern in the epidemiology of this infection has become evident in most countries of the Americas, including Brazil. Substantial differences in the distribution of cases, according to exposure category, have been noted in the present decade when compared to the early 1980s. Initially, the epidemic predominated in the male homosexuals or bisexuals, hemophiliacs and others who had received blood products. However, within the past few years, there has been an increase of HIV among IDUs and heterosexuals18.
The first registered case of HIV infection in an intravenous drug user in Brazil was in 1982. This category is responsible at present for about 20% of accumulated AIDS cases in this country7.
In Brazil, the HIV epidemics among cocaine injectors, and more recently among heroin injectors, are compounded by the association of crack cocaine use and the practice of unsafe sexual behaviors. HCV infection is more rapidly acquired after initiation of intravenous drug use than other viral infections (hepatitis B virus and HIV). Also, rates of HCV infection among young intravenous drug users are four times higher than rates of HIV infection. More rapid acquisition of HCV infection compared with other viral infections among IDUs is likely to be caused by high prevalence of chronic HCV infection among IDUs, which results in a greater likelihood of exposure to an HCV infected person3.
Intravenous drug use was the most frequent risk factor involved in our study, which is in agreement with the epidemiology for HIV infection observed in Brazil, as exposed above.
It was also very interesting to observe that the second largest risk factor for HCV acquisition (16.3%) was being a sexual partner of an HIV seropositive person.
Among the patients who mentioned only one risk factor, 28 out of 204 (10.9%) were sexual partners of HIV-positive patients and denied any other risk factor for HIV/HCV infection. The proportion of the different risk factors involved in the groups analyzed was maintained.
Through correspondence analysis it was also possible to infer an association between the risk factors: sexual partner of HIV seropositive patients and sexual partner of intravenous drug users. This association could easily be explained by the fact that these groups may have similar exposures and are frequently compounded by the same persons.
Sexual transmission of HCV has been a matter of important controversy in literature. Case-control studies have reported an association between exposure to a sex contact with a history of hepatitis or exposure to multiple sex partners and the acquisition of hepatitis C.
In contrast, a low prevalence of HCV infection has been reported by different studies of long term spouses of patients with chronic HCV infection. The average prevalence of HCV infection in this situation is 1.5% (range: 0% to 4.4%)3.
Although there are important differences among different studies on this subject, there are sufficient data to indicate that sexual transmission of HCV may occur, but that this virus is probably inefficiently spread through this route.
A more precise way to examine the issue of sexual transmission is to test the monogamous sexual partners of HCV-infected individuals. LISSEN et al.9 examined 147 such heterosexual partners, who denied intravenous drug use or blood transfusion. According to this study the anti-HCV prevalence in stable heterosexual partners of HCV/HIV index cases was 2.2 times higher than in stable heterosexual partners of index cases reactive for anti-HCV only (9.2% vs. 4.1%).
Among partners of hemophilics co-infected with HCV/HIV, BRETTLER et al. reported an average prevalence of HCV infection of 3%1.
EYSTER et al. also studied female sexual partners of anti-HCV positive hemophiliacs5. According to this study, female sexual partners of anti-HCV positive hemophiliacs were found to be at four times greater risk of acquiring HCV if the hemophiliac was co-infected with HIV.
Our study has shown a significant proportion of HCV/HIV patients who mentioned, as their only risk factor, the fact of being sexual partners of HIV-positive patients.
Although we do not know the HCV status of those HIV partners, it is possible that most of them were probably HCV positive, as well. It would be interesting to suppose that HIV infection could increase the chances of sexual HCV transmission.
Some studies have suggested that the level of HCV viremia is higher in HIV-infected patients when compared to HIV-negative patients19. Higher HCV replication is suggested by the more frequent vertical transmission of HCV to newborns from HIV-infected mothers than from HIV-negative mothers. In HIV-negative mothers the risk of transmission is clearly related to the level of viremia13.
Eighty-two of our 258 anti-HCV positive patients were tested by HCV-RNA by "nested" PCR and 81 were positive (98%). This data could suggest that patients with HIV and HCV are more likely to have active HCV infections with persistent viremia.
It is possible that sexual transmission of HCV could be enhanced in HIV-positive patients due to higher HCV viremia and also due to more active HCV infection with persistent viremia.
RESUMO
Prevalência e fatores de risco da hepatite C em pacientes infectados pelo vírus da imunodeficiência humana
O objetivo do presente estudo foi avaliar a prevalência e os fatores de risco associados à infecção pelo vírus da hepatite C (VHC) em um grupo de pacientes soropositivos para o HIV. Analisamos os prontuários médicos de 1.457 pacientes. O diagnóstico laboratorial de infecção pelo VHC foi feito utilizando-se ELISA de terceira geração. Uma parte dos pacientes soropositivos para VHC foram também submetidos à realização de PCR. Os pacientes soropositivos para VHC foram analisados em relação aos fatores de risco para ambas as infecções. A prevalência de pacientes soropositivos para VHC foi de 17,7% (258 pacientes). 82 desses pacientes foram testados para VHC por PCR e 81 (98%) apresentaram-se com resultado positivo. 151 (58,5%) referiram uso de drogas endovenosas (UDE), 42 (16,3%) eram parceiros sexuais de pacientes infectados pelo HIV, 23 (8,9%) eram homossexuais masculinos, 12 (4,7%) tinham recebido transfusão sanguínea, 61 (17,5%) referiram promiscuidade sexual, 14 (5,4%) negaram qualquer fator de risco, 12 (4,7%) eram parceiros sexuais de UDE. 204 pacientes referiram apenas um fator de risco, 51 referiram dois diferentes fatores de risco e três referiram três diferentes fatores de risco. Entre os pacientes que referiram apenas um fator de risco, 28 em 204 (10,9%) eram parceiros sexuais de pacientes infectados pelo HIV. Embora o uso de drogas endovenosas tenha sido o fator de risco mais importante na determinação da co-infecção, a transmissão sexual parece ter contribuído para a alta soroprevalência do VHC nesse grupo de pacientes.
ACKNOWLEDGMENT
We thank Dr. Maria Aparecida Shikanai Yasuda, Professor of Infectious Diseases, School of Medicine, University of São Paulo. We also thank Professor David Uip, Chief, AIDS Outpatient Clinic, University of São Paulo.
Received: 17 August 2000
Accepted: 31 October 2000
(1) AIDS Outpatient Clinic, Hospital das Clínicas, School of Medicine, Infectious Diseases Department, University of São Paulo, SP, Brazil.
(2) Hospital das Clínicas, School of Medicine, Infectious Diseases Department, University of São Paulo. Laboratório de Investigação Médica em Hepatites (LIM-47), School of Medicine , University of São Paulo, SP, Brazil.
(3) AIDS Outpatient Clinic, Hospital das Clínicas, School of Medicine, Infectious Diseases Department, University of São Paulo, SP, Brazil.
Correspondence to: Maria Cassia Jacintho Mendes Corrêa, Praça Vicentina de Carvalho 84, 05447-050 São Paulo, SP, Brazil. tel: 5511-91622498, 5511-38199242 Fax: 5511-30821555, 5511 30851755, e-mail: cassiamc@uol.com.br
- 1. BRETTLER, D.B.; MANNUCCI, P.M.; GRINGERI, A. et al. - The low risk of hepatitis C virus transmission among sexual partners of hepatitis C-infected hemophilic males: an international, multicenter study. Blood, 80: 540-543,1992.
- 2. CARRILHO, F.J. & MENDES CORRĘA, M.C.J. - The magnitute of hepatitis B and C in Latin America. In: SCHINAZI, R.F.; SOMMADOSSI, J.P. & THOMAS, H.C.,ed. Therapies for viral hepatitis London, International Medical Press, 1998. p.25-34.
- 3. CENTERS FOR DISEASE CONTROL AND PREVENTION - Recommendations for prevention and control of hepatitis C virus (HCV) infection and HCV-related chronic disease. M.M.W.R., 47: 1-39, 1998.
- 4. DORRUCI, M.; PEZZOTTI, P.; PHILLIPS, A.N.; LEPRI, A.C. & REZZA, G. - Coinfection of hepatitis C virus with the human immunodeficiency virus and progression to AIDS. Italian seroconversion study. J. infect. Dis., 172: 1503-1508, 1995.
- 5. EYSTER, M.E.; ALTER, H.J.; ALEDORT, L.M. et al - Heterosexual co-transmission of hepatitis C virus (HCV) and human immunodeficiency virus (HIV). Ann. intern. Med., 115: 764-768, 1991.
- 6. FOCACCIA, R. - Prevalęncia das hepatites virais A, B, C e E. Estimativa de prevalęncia na populaçăo geral da cidade de Săo Paulo, medida por marcadores séricos, em amostragem populacional estratificada com sorteio aleatório e coleta domiciliar Săo Paulo, 1998. (Tese de Livre Docęncia - Faculdade de Medicina da Universidade de Săo Paulo).
- 7. FONSECA, M.G.P. & CASTILHO, E.A. - Os casos de AIDS entre usuários de drogas injetáveis. Brasil, 1980-1997. Semana Epidemiológica 23 a 25, junho/agosto. Bol. Epidem. AIDS, 10(3): 6-14, 1997.
- 8. GREENACRE, M.J. - Theory and applications of correspondence analysis London, Academic Press, 1984.
- 9. LISSEN, E.; ALTER, H.J. & ABAD, M.A. - Hepatitis C virus infection among sexually promiscous groups and the heterosexual partners of hepatitis C virus infected index cases. Europ. J. clin. Microbiol. infect. Dis., 12: 827-831, 1993.
- 10. MARTINS, R.M.B.; PORTO S.O.B.; VANDERBORGHT, B.O.M. et al. - Short report: prevalence of hepatitis C viral antibody among Brazilian children, adolescents, and street youths. Amer. J. trop. Med. Hyg., 53: 654-655, 1995.
- 11. MENDES CORRĘA, M.C.J.; DUARTE, M.I.S.; GUASTINI, C. et al - Hepatitis C in patients with the immunodeficiency virus. In: CONFERENCE ON RETROVIRUS AND OPPORTUNISTIC INFECTIONS, 5., Chicago, 1998. Abstract. p. 494.
- 12. MENDES CORRĘA, M.C.J. - Hepatitis C in patients with the immunodeficiency virus, in Săo Paulo, Brazil. In: ANNUAL MEETING OF THE INFECTIOUS DISEASES SOCIETY OF AMERICA, 36., Denver, 1998. Abstract. p. 412 .
- 13. OHTO, H.; TERAZAWA, S.; SASAKI, N. et al - Transmission of hepatitis C virus from mother to infants. The vertical transmission of hepatitis C virus collaborative study group. New Engl. J. Med., 330: 744-750, 1994.
- 14. PIROTH, L.; DUONG, M.; QUANTIN, C. et al. - Does hepatitis C virus co-infection accelerate clinical and immunological evolution of HIV-infected patients? AIDS, 12: 381-388, 1998.
- 15. SABIN, C.A.; TELFER, P.; PHILLIPS, N.A; BHAGANI, S. & LEE, C.A.. - The association between hepatitis C virus genotype and human immunodeficiency virus disease progression in a cohort of hemophilic men. J. infect. Dis., 175: 164-168, 1997.
- 16. SILVA, L.; PARANA, R.; MOTA, E. et al - Prevalence of hepatitis C virus in urban and rural population of Northeast Brazil: pilot study. Arq. Gastroent., 32: 168-171, 1995.
- 17. SOTO, B.; SANCHEZ-QUIJANO, A.; RODRIGO, L. et al - Human immunodeficiency virus infection modifies the natural history of chronic parenterally-acquired hepatitis C with an unusually rapid progression to cirrhosis. J. Hepat., 26: 1-5, 1997.
- 18. SZWARCWALD, C.L.; BASTOS, F.I. & CASTILHO, E.A. - The dynamics of the AIDS epidemic in Brazil: a space-time analysis in the period 1987-1995. Braz. J. infect. Dis., 2: 175-186, 1998.
- 19. ZYLBERBERG, H. & POL, S. - Reciprocal interations between human immunodeficiency virus and hepatitis C virus infections. Clin. infect. Dis., 23: 1117-1125, 1996.
- 20. WOOLEY, I.; VALDEZ, H.; HORSCH, A. et al. - Prevalence of unrecognized hepatitis B and C infections in AIDS patients with abnormal liver function tests. In: CONFERENCE ON RETROVIRUS AND OPPORTUNISTIC INFECTIONS, 6., Chicago, 1999. Abstract. p. 189.
- 21. WRIGHT, T.; HOLLANDER, H.; PU, X. et al - Hepatitis C in HIV-infected patients with and without AIDS: prevalence and relationship to patient survival. Hepatology, 20: 1152-1155, 1994.
Publication Dates
-
Publication in this collection
09 Mar 2001 -
Date of issue
Feb 2001
History
-
Accepted
31 Oct 2000 -
Received
17 Aug 2000