Abstracts
The authors report a case of bilateral Tinea nigra plantaris treated through a double-blind study with the topical antifungal agents Isoconazole and Terbinafine. The objective of the study was to clinically compare the efficacy of these two topical antifungal agents on days 10, 20 and 30 of the treatment. No significant clinical differences were found, as all the plantar lesions regressed completely by the end of the treatment. Our conclusion was that in the case reported, the topical antifungal agents Isoconazole and Terbinafine demonstrated identical efficacy as a clinical cure. We also suggest the inclusion of injuries caused by arthropods of the Diplopoda Class in the differential diagnosis of Tinea nigra plantaris, due to the persistent acral hyperpigmentation.
Antifungal agents; Dermatomycoses; Mycoses; Tinea
Os autores relatam um caso de Tinea nigra plantaris bilateral tratado através de um estudo duplo cego com os antifúngicos tópicos isoconazol e terbinafina. O objetivo do estudo foi comparar clinicamente a eficácia entre esses dois antifúngicos tópicos aos dias 10, 20 e 30 do tratamento, sendo que não foram observadas diferenças clínicas significativas, uma vez que todas as lesões plantares regrediram completamente no final do tratamento. Nossa conclusão foi que os antifúngicos tópicos isoconazol e terbinafina demonstraram a mesma eficácia na cura clínica do caso relatado. Adicionalmente, é sugerida a inclusão dos acidentes causados por artrópodos da Classe Diplopoda no diagnóstico diferencial com a Tinea nigra plantaris devido a hiperpigmentação acral persistente.
INTRODUCTION
Tinea nigra (TN) is a dermatomycosis caused by the fungus Hortaea werneckii 44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,88. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.,99. Rossetto AL, Cruz RCB. Tinea nigra nas formas geográficas em “coração” e “bico do papagaio”. An Bras Dermatol. 2011;86:389-90.,1010. Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2.. It is a cosmopolitan disease which is common in the coastal areas of tropical and subtropical regions22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.. It generally affects young people below the age of 20 years, particularly females22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.. Clinically, it manifests as a single, asymptomatic macule, ranging from dark brown to black in color, located on the palm of the hand. In rare instances it is bilateral22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,1111. Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62.. Sometimes it is located on the soles, or even in atypical areas11. Aguiar C. Um caso interessante de “ceratomicose nigricans palmar” ou “Tinea nigra”. Bahia Med. 1937;8(1):137-40.,22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,88. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.,1212. Silva F, Mendonça AB. Sobre um caso interessante de Tinea nigra. Gaz Med Bahia. 1932;591-3.. The differential diagnosis is made with melanocytic lesions and exogenous pigmentations22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,66. Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.,1111. Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62..
The fungus is sensitive to treatment with various topical antifungal drugs44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,66. Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.,88. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.,99. Rossetto AL, Cruz RCB. Tinea nigra nas formas geográficas em “coração” e “bico do papagaio”. An Bras Dermatol. 2011;86:389-90.,1010. Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2.. The objective of this communication, carried out as a double-blind study with Isoconazole and Terbinafine, was to clinically compare the efficacy of these two topical antifungal agents. The small number of reports of TN prompted the authors to carry out a review of cases with bilateral involvement published in Brazil. Additionally, we suggest the inclusion of injuries caused by arthropods of the Diplopoda Class in the differential diagnosis of Tinea nigra plantaris, due to the persistent acral hyperpigmentation.
CASE REPORT
Male patient, 19 years-old, student, living in Itajaí Town in Santa Catarina State (SC), Brazil. Two years prior to the examination, he noticed the appearance of small, black, itchy spots on the plantar regions. He associated the spots with the fact that he had been walking barefoot on Cassino Beach in the state of Rio Grande do Sul, where he lived for six months. He reported no other symptoms, contact with insects or previous treatments.
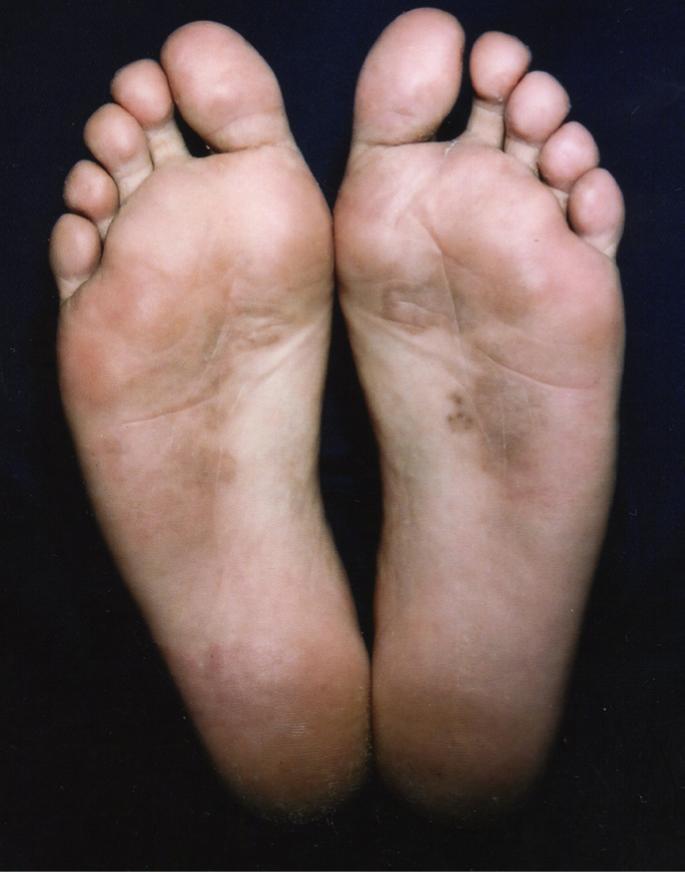
On dermatological examination, the patient presented black macules with superficial fine peeling and irregular, poorly-defined edges. The macules ranged from 1 cm to 5 cm in diameter, and covered approximately two thirds of the plantar region (Fig. 1 and Fig. 2).
Black macules with fine desquamation and irregular, poorly-defined edges, ranging in size from 1 cm to 5 cm in diameter, covering approximately two thirds of the plantar regions.
Detail of the hyperchromic macules with fine desquamation, located on the left plantar region.
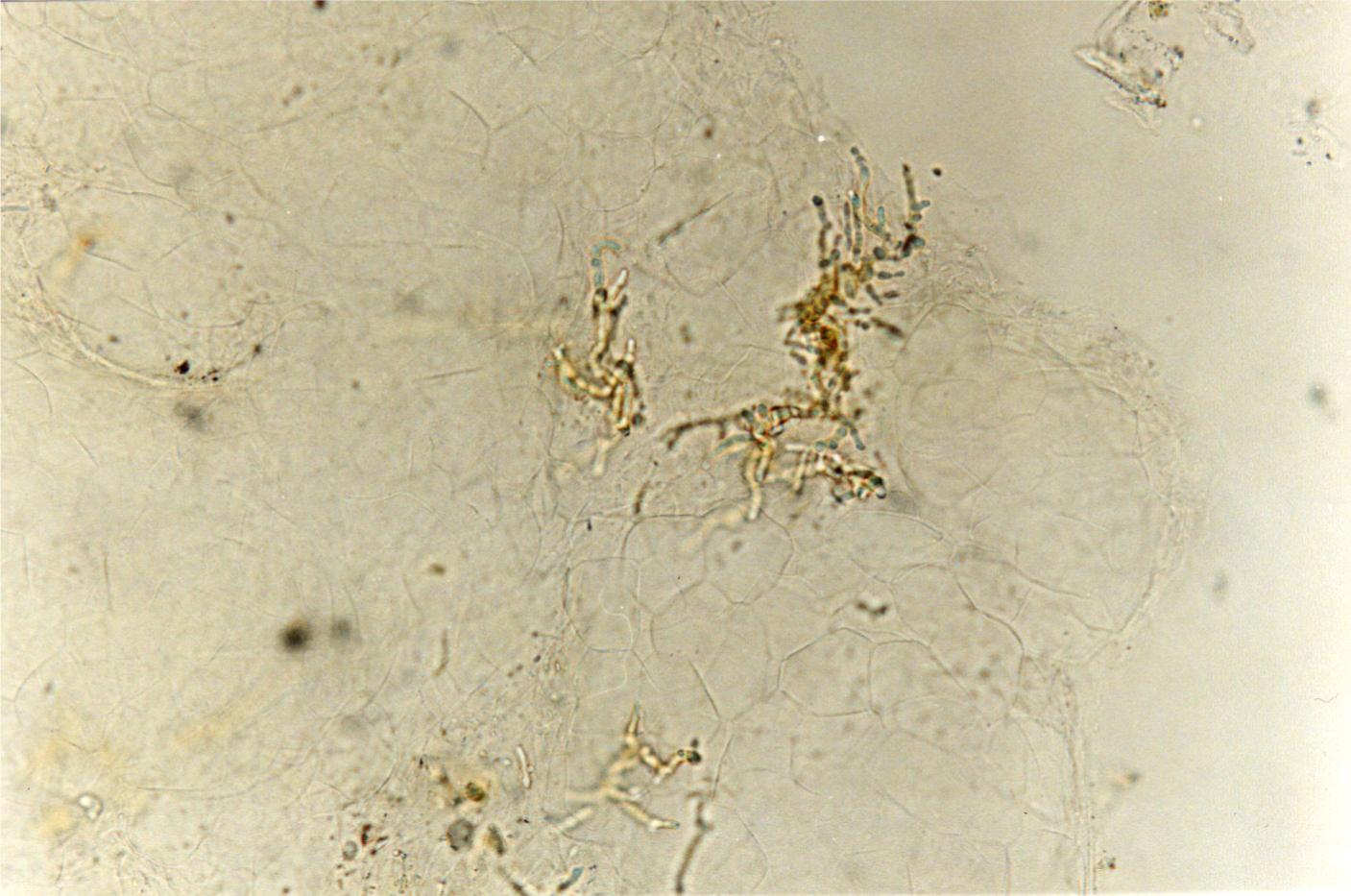
A direct mycological exam showed irregular, branching, septate, dematiaceous hyphae and the presence of yeast-like cells with spores (Fig. 3). Cultures were grown in Sabouraud agar medium on two separate occasions and once again before the treatment, with negative results.
Direct, clarified mycological exam with 20% potassium hydroxide, showing irregular, branching, septate dematiaceous hyphae, and the presence of yeast-like cells with spores.
Treatment was proposed with the topical antifungal agents Isoconazole and Terbinafine, through a double-blind study. The antifungal agents were poured separately into identical tubes by a pharmaceutical biochemist, with each tube containing the same amount of antifungal agent. The two tubes were labeled with the patients name, the doctors name, and the indication for topical use on the plantar regions - right or left. The topical treatments were applied by the patient twice a day for 30 days. The patient was clinically evaluated by the same dermatologist at days 10, 20 and 30 of the treatment. At the end of the treatment period, the professional responsible for the tubes revealed that the tube used on the right sole had contained Isoconazole, and the one used on the left sole had contained Terbinafine. All the lesions regressed and disappeared completely by the end of the treatment. No clinically significant differences were noted in the appearance of the regression of the lesions on the right and left plantar regions. The patient was followed up for 10 years, without any reappearance of the lesions.
DISCUSSION
Reports of TN in Brazil have been rare since the 1916 publication in Bahia by Cerqueira22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,66. Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.,1010. Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2.,1111. Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62.. The bibliographic review carried out for this study found eight cases published in Brazil with bilateral involvement, shown in Table 1 11. Aguiar C. Um caso interessante de “ceratomicose nigricans palmar” ou “Tinea nigra”. Bahia Med. 1937;8(1):137-40.,22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,66. Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.,77. Ramos e Silva J. Caso de Tinea nigra. An Bras Dermatol. 1958;33(4):84.,1111. Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62.,1212. Silva F, Mendonça AB. Sobre um caso interessante de Tinea nigra. Gaz Med Bahia. 1932;591-3.. Of these, there was only one case of bilateral plantar involvement, also in a young patient aged 19 years, but this time female22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.. In the case of bilateral nail location1212. Silva F, Mendonça AB. Sobre um caso interessante de Tinea nigra. Gaz Med Bahia. 1932;591-3., the presence of black spots was limited to the nails of the index fingers and left little beyond the hyperchromic macules on the right palmar area, the cultures of nail and scarce material were negative due to pretreatment performed by the patient, fact that made it impossible to claim certainty the diagnosis of TN. The nail lesions, despite the dematiaceous fungi, were probably not Tinea nigra but onychomycosis, due to non-dermatophyte fungi.
Since 1995, the authors have frequently observed TN on the north coast of Santa Catarina88. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.,99. Rossetto AL, Cruz RCB. Tinea nigra nas formas geográficas em “coração” e “bico do papagaio”. An Bras Dermatol. 2011;86:389-90.,1010. Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2.. During the 60th Congress of the SBD (Brazilian Dermatological Society) in 2005, twenty-seven cases were reported occurring over a 10-year period88. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.. Recently, we described a case which evolved to a spontaneous cure and was confirmed by a mycological exam99. Rossetto AL, Cruz RCB. Tinea nigra nas formas geográficas em “coração” e “bico do papagaio”. An Bras Dermatol. 2011;86:389-90., and two cases with curious forms analogous to formations in nature called “Heart” and “Parrot Beak”1010. Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2..
The present case affects a male patient, the involvement is bilateral and the location of the lesions differs from the typical clinical manifestations of TN. The prolonged period of evolution before diagnosis may have contributed to the involvement of more extensive regions of the plantar areas than is usual.
We emphasize the importance of the differential diagnosis of melanocytic lesions, especially dysplastic nevi and malignant melanoma. The knowledge of dermatomycoses and dermoscopy may avoid surgical procedures in cases where melanocytic lesions lead to the misdiagnosis of TN. With pityriasis versicolor, the differentiation diagnostic occurs in the clinic according to the location, blackish color and usually absence of scaling lesions seen with TN. In our case we ruled out the diagnosis of fixed pigmented erythema. On top of the fact that the patient denied the use of systemic drugs, an increase in the size of the lesions was clinically observed once established. Cases of exogenous pigmentation blemishes varying from a shade of brown to a blackish color were due to impregnations by chemical dyes, grease or tar. Even though the patient had been walking barefoot in the sand, these cases were discarded because the spontaneous regression of such lesions occurs after several weeks of development.
Apart from Tinea pedis, another differential diagnosis to be remembered in this case is the injuries caused by arthropods of the Diplopoda Class. Commonly known as millipedes, they release quinones and other irritative and pigmentary substances when threatened or crushed55. Lima CAJ, Cardoso JLC, Magela A, Oliveira FGM, Talhari S, Haddad V Jr. Pigmentação exógena em pododáctilos simulando isquemia de extremidades: um desafio diagnóstico provocado por artrópodos da classe Diplopoda (“piolhos-de-cobra”). An Bras Dermatol. 2010;85:391-2.. When the liquids and vapors expelled come into contact with human skin, they cause a burning sensation55. Lima CAJ, Cardoso JLC, Magela A, Oliveira FGM, Talhari S, Haddad V Jr. Pigmentação exógena em pododáctilos simulando isquemia de extremidades: um desafio diagnóstico provocado por artrópodos da classe Diplopoda (“piolhos-de-cobra”). An Bras Dermatol. 2010;85:391-2.. The site of contact instantly becomes hyperchromic, ranging in color from light yellow to dark brown, and lasting up to several months (Fig. 4). In the present case, the persistence of hyperpigmentation of the cutaneous lesions, with evolution of two years, which is considered prolonged; itching as the only symptom described; the absence of a sensation of burning in the plantar regions, and the lack of reported contact with insects; rules out a clinical diagnosis of accidents by arthropods. However, the persistent hyperpigmentation in accidents caused by Diplopoda in the plantar regions may be included as part of the differential diagnosis with plantar TN.
Detail of an area of black-colored exogenous pigmentation on the plantar region of the hallux, caused by a millipede inside his shoe in an accident that occurred as a child, simulating the clinical diagnosis of Tinea nigra plantaris.
As for the differential diagnosis cited, the presence of scaly lesions on the plantar regions may in this case suggest a hypothesis of Tinea pedis, which could be confirmed by a mycological exam. In the case reported here, the culture was performed twice even with scaly lesions, both times with a negative result. On both occasions, the direct mycological exam revealed a finding of dematiaceous hyphae, reaffirming through laboratory tests the clinical diagnosis of TN.
In the treatment of bilateral TN, all the cases revised used various topical antifungal agents, always applying the same topical antifungal agent to all the cutaneous lesions11. Aguiar C. Um caso interessante de “ceratomicose nigricans palmar” ou “Tinea nigra”. Bahia Med. 1937;8(1):137-40.,22. Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.,33. Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.,44. Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.,66. Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.,77. Ramos e Silva J. Caso de Tinea nigra. An Bras Dermatol. 1958;33(4):84.,1111. Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62.,1212. Silva F, Mendonça AB. Sobre um caso interessante de Tinea nigra. Gaz Med Bahia. 1932;591-3.. The treatment with topical Isoconazole and Terbinafine demonstrated the efficacy of both antifungal agents in the clinical cure of bilateral Tinea nigra plantaris, as well as enabling a comparative study of the efficacy of the two treatments in cases of bilateral Tinea nigra.
Although the study was limited and restricted to clinical evaluations during the physical examination, the medical literature reviewed did not find any reports of the use of the two topical antifungal agents, either simultaneously or separately, in the treatment of lesions with bilateral involvement of TN.
The authors conclude that future studies in cases of bilateral TN, whether plantar or palmar, as well as clinical evaluations, mycological exams and dermatoscopy, can be of use in making the comparative results of efficacy between various topical antifungal agents more quantifiable. Additionally, cases of bilateral TN must undergo a rigorous diagnostic process and new differential diagnoses of bilateral lesions are suggested in this communication.
REFERENCES
-
1Aguiar C. Um caso interessante de “ceratomicose nigricans palmar” ou “Tinea nigra”. Bahia Med. 1937;8(1):137-40.
-
2Giraldi S, Marinoni LP, Bertogna J, Abbage KT, Oliveira VC. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.
-
3Gondim-Gonçalves HM, Mapurunga ACP, Diógenes MJN. Tinha negra palmar bilateral. An Bras Dermatol. 1991;66:37-8.
-
4Larangeira de Almeida H Jr, Dallazem RN, Dossantos LS, Hallal SA. Bilateral Tinea nigra in temperate climate. Dermatol Online J. 2007;13:25.
-
5Lima CAJ, Cardoso JLC, Magela A, Oliveira FGM, Talhari S, Haddad V Jr. Pigmentação exógena em pododáctilos simulando isquemia de extremidades: um desafio diagnóstico provocado por artrópodos da classe Diplopoda (“piolhos-de-cobra”). An Bras Dermatol. 2010;85:391-2.
-
6Purim KSM, Telles Filho FQ, Serafini SZ. Feohifomicose superficial (Tinea nigra): relato de dois casos no Paraná. An Bras Dermatol. 1990;65:178-80.
-
7Ramos e Silva J. Caso de Tinea nigra. An Bras Dermatol. 1958;33(4):84.
-
8Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.
-
9Rossetto AL, Cruz RCB. Tinea nigra nas formas geográficas em “coração” e “bico do papagaio”. An Bras Dermatol. 2011;86:389-90.
-
10Rossetto AL, Cruz RCB. Cura espontânea em um caso de Tinea nigra. An Bras Dermatol. 2012;87:160-2.
-
11Severo LC, Bassanesi MC, Londero AT. Tinea nigra: report of four cases observed in Rio Grande do Sul (Brazil) and review of Brazilian literature. Mycopathologia. 1994;126:157-62.
-
12Silva F, Mendonça AB. Sobre um caso interessante de Tinea nigra. Gaz Med Bahia. 1932;591-3.
Publication Dates
-
Publication in this collection
Apr 2013
History
-
Received
6 May 2012 -
Accepted
17 Sept 2012