ABSTRACT
This communication is a retrospective epidemiological study of the scorpion sting cases recorded from 2007 to 2014 in the Rio Grande do Norte State, Northeastern Brazil. The data was collected from the Injury Notification Information System database of the Health Department of Rio Grande do Norte State. A total of 20,555 cases were studied. The cases were distributed over all months of the period studied and occurred mainly in urban areas. Victims were predominantly 20-29 year-old women. Most victims were stung on the foot and received medical care within 1-3 h after being stung. The cases were mostly classified as mild and progressed to cure. Scorpion stings in Rio Grande do Norte State are an environmental public health problem that needs to be monitored and controlled throughout the year.
Arachnids; Envenomation; Public health
INTRODUCTION
Scorpion stings are a public health problem in many tropical and subtropical countries, due to its high incidence and the ability of some species to induce severe clinical symptoms, fatal at times 11. Chippaux JP, Goyffon M. Epidemiology of scorpionism: A global appraisal. Acta Trop. 2008;107:71-9.,22. Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual de controle de escorpiões. Brasília: Ministério da Saúde; 2009. . Several species may induce envenomation, including Centruroides genus in North and Central America, Colombia; Tityus in South America; Androctonus and Buthus in North Africa; Buthotus and Leiurus in the Middle East and Mesobuthus tamulus in India 11. Chippaux JP, Goyffon M. Epidemiology of scorpionism: A global appraisal. Acta Trop. 2008;107:71-9. . The Brazilian scorpion fauna is large, consisting of about 131 species, 23 genera and 4 families 33. Brazil TK, Porto TJ. Os escorpiões. Salvador: EDUFBA; 2010. . In Brazil, scorpion species of the genus Tityus have been responsible for envenomation of medical importance: T. serrulatus and T. bahiensis in the Southeast, T. obscurus, silvestris and metuendus in North and T. stigmurus and pusillus in Northeast. T. serrulatus may be the main responsible for severe cases, with high lethality, especially in children 44. Albuquerque CM, Santana Neto PL, Amorim ML, Pires SC. Pediatric epidemiological aspects of scorpionism and report on fatal cases from Tityus stigmurus stings (Scorpiones: Buthidae) in State of Pernambuco, Brazil. Rev Soc Bras Med Trop. 2013;46:484-9.
5. Cardoso JL, França FS, Wen FH, Malaque CM, Haddad Júnior V. Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. 2ª ed. São Paulo: Sarvier; 2009.
6. Coelho JS, Ishikawa EA, Santos PR, Pardal PP. Scorpionism by Tityus silvestris in eastern Brazilian Amazon. J Venom Anim Toxins Incl Trop Dis. 2016;22. In Press.
7. Albuquerque CM, Porto TJ, Amorim ML, Santana Neto PL. Escorpionismo por Tityus pusillus Pocock, 1893 (Scorpiones; Buthidae) no Estado de Pernambuco. Rev Soc Bras Med Trop. 2009;42:206-8.-88. Wen FH, Monteiro WM, Silva AM, Tambourgi DV, Silva IM, Sampaio VS, et al. Snakebites and scorpion stings in the Brazilian Amazon: identifying research priorities for a largely neglected problem. PLoS Negl Trop Dis. 2015;9:e0003701. .
The toxicity of the scorpion venom varies between different species and between a same species from different regions 33. Brazil TK, Porto TJ. Os escorpiões. Salvador: EDUFBA; 2010.,55. Cardoso JL, França FS, Wen FH, Malaque CM, Haddad Júnior V. Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. 2ª ed. São Paulo: Sarvier; 2009.,99. Brazil TK, Lira-da-Silva RM, Porto TJ, Amorim AM, Silva TF. Escorpiões de importância médica do estado da Bahia, Brasil. Gaz Med Bahia. 2009;79 Supl 1:38-42. . Scorpion venoms contain proteins and peptides that block and/or modulate different types of ion channels (e.g. sodium, potassium, chlorine and calcium), mainly in the autonomic nervous system. At the nerve terminals of such a system, the scorpion venom induces the release of acetylcholine and/or catecholamines (adrenaline and/or noradrenaline), leading to clinical symptoms 55. Cardoso JL, França FS, Wen FH, Malaque CM, Haddad Júnior V. Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. 2ª ed. São Paulo: Sarvier; 2009. . Scorpion stings may lead to immediate local pain only, but they may also be followed by other local symptoms, such as swelling, hyperemia, paresthesia, and piloerection. The development of systemic symptoms (gastrointestinal, respiratory, cardiovascular and/or neurological disorders) indicate an increase in the severity of envenomation 22. Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual de controle de escorpiões. Brasília: Ministério da Saúde; 2009. . The severity of the cases depends on the scorpion and/or the victim. Factors related to the scorpions include the species and size of the animal, the content of the venom glands, the status of the venom ducts of the telson, the number of stings, and the amount of venom inoculated. The victim factors are age, part of the body stung, body mass, health status, sensitivity to venom, time elapsed between sting and treatment, and the maintenance of the vital functions 55. Cardoso JL, França FS, Wen FH, Malaque CM, Haddad Júnior V. Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. 2ª ed. São Paulo: Sarvier; 2009.,1010. Brasil. Ministério da Saúde. Fundação Nacional de Saúde. Manual de diagnóstico e tratamento de acidentes por animais peçonhentos. 2 a ed. Brasília: Ministério da Saúde; 2001. . The treatment of scorpion envenomation aims to decrease the clinical symptoms by using analgesics and antivenom. The effectiveness of the treatment may be related to the time elapsed between the incident and the medical care, mainly by the use of the antivenom 22. Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual de controle de escorpiões. Brasília: Ministério da Saúde; 2009. .
Globally, the epidemiology of the scorpion envenomation is poorly known due to underreporting of the cases and insufficiency of studies devoted to the scorpionism. Two factors may explain the information deficiency; the generally reduced severity of scorpion envenomation in adults, and the organization of health services, which do not require very precise information 11. Chippaux JP, Goyffon M. Epidemiology of scorpionism: A global appraisal. Acta Trop. 2008;107:71-9. . There are considerable geographical variations, at the level of both the incidence and severity. However, at least 1,200,000 cases of envenomation and 3,250 deaths by scorpion stings may occur in the world annually 11. Chippaux JP, Goyffon M. Epidemiology of scorpionism: A global appraisal. Acta Trop. 2008;107:71-9. . In Brazil, the Ministry of Health implemented the National Program for Snakebites Control in 1986, extended to other poisonous animals in 1988. This program made the records by health providers of epidemiological and clinical data of the scorpion sting cases mandatory 88. Wen FH, Monteiro WM, Silva AM, Tambourgi DV, Silva IM, Sampaio VS, et al. Snakebites and scorpion stings in the Brazilian Amazon: identifying research priorities for a largely neglected problem. PLoS Negl Trop Dis. 2015;9:e0003701. . Since then, the number of cases reported in Brazil has significantly increased in all regions of country. The number of scorpion sting cases increased from 12,552 in 2000 to 74,598 in 2015 1111. Brasil. Ministério da Saúde. Sistema de Informação de Agravos de Notificação. Secretaria de Vigilância à Saúde. Incidência (100.000 hab) de casos de acidentes por escorpiões. Brasil, Grandes Regiões e Unidades Federadas. 2000 a 2013. [cited 2015 Mar 13]. Available from: http://u.saude.gov.br/images/pdf/2014/julho/10/Tabela-10---INCIDENCIA-CASOS---escorpiao---2000-a-2013---21-05-2013.pdf
http://u.saude.gov.br/images/pdf/2014/ju...
. The number of deaths also increased from 13 to 119 during this period. The Brazilian Northeast has been having the highest incidence of cases and of deaths followed by the Southeast, Central-West, North, and South 1111. Brasil. Ministério da Saúde. Sistema de Informação de Agravos de Notificação. Secretaria de Vigilância à Saúde. Incidência (100.000 hab) de casos de acidentes por escorpiões. Brasil, Grandes Regiões e Unidades Federadas. 2000 a 2013. [cited 2015 Mar 13]. Available from: http://u.saude.gov.br/images/pdf/2014/julho/10/Tabela-10---INCIDENCIA-CASOS---escorpiao---2000-a-2013---21-05-2013.pdf
http://u.saude.gov.br/images/pdf/2014/ju...
. Despite its medical importance, the epidemiological profile of scorpion stings in the Northeastern Brazil has not been conclusively determined. Moreover, social and environmental changes occurring in this region during recent decades demand new research on this topic. To address this shortcoming, the current study analyzed epidemiological data regarding scorpion stings between 2007 and 2014 in the Rio Grande do Norte State, Northeastern Brazil.
MATERIALS AND METHODS
Study area
The Rio Grande do Norte State, whose capital is Natal, is a federal unit that integrates the Northeast region of Brazil. It is composed of 167 municipalities, covering an area of 52,811,126 km 2 . These municipalities are distributed in four regions: Oeste Potiguar, Central Potiguar, Agreste Potiguar and Leste Potiguar. According to the Instituto Brasileiro de Geografia e Estatística (IBGE), the total resident population of the State is 3,168,027 inhabitants, with 2,464,991 living in urban areas and 703,036 in rural areas. The population density is of 60 inhabitants/km 2 . Regarding gender, its population consists about 1,548,887 men and 1,619,140 women 1212. Instituto Brasileiro de Geografia e Estatística. Censo 2010. [cited 2017 May 11]. Available from: http://censo2010.ibge.gov.br/
http://censo2010.ibge.gov.br/...
. In Rio Grande do Norte, there are two climate types: tropical and semiarid. The first takes place on the East Coast, with more abundant rainfall, while the latter dominates almost all areas of the State, including the North Coast. In the region of semiarid climate, rainfall is scarce and irregular. The majority of the Rio Grande do Norte territory (98%) is located within the “Drought Polygon”, an area that is affected annually by prolonged periods of drought. Almost the entire region has a low rainfall rate, high average temperatures, acute water deficits, generally thin and often salty soils, and caatinga vegetation. The average annual temperature in the State is 26 °C, with a maximum of 31 ºC and minimum of 21°C. The rainy season occurs between the months of April to July and rainfall is below 600 mm annually 1313. Brasil. Ministério do Meio Ambiente. Secretaria de Recursos Hídricos. Atlas das áreas susceptíveis à desertificação do Brasil. Brasília: Ministério do Meio Ambiente; 2007. .
Data collection
Scorpion sting cases are mandatorily recorded by the National System for Notifiable Diseases (SINAN) based on medical records used in the investigation and follow-up of injury cases by poisonous animals. The SINAN is a national electronic surveillance system that contains a variety of diseases in an integrated database that also includes scorpion sting cases 1414. Bochner R, Struchiner CJ. Acidentes por animais peçonhentos e sistemas nacionais de informação. Cad Saude Publica. 2002;18(3):735-46. . All scorpion envenomation cases in the Rio Grande do Norte State recorded to SINAN from 2007 to 2014 were included in the current study. Demographic and population data from the Brazilian Institute of Geography and Statistics were used to calculate the incidence rates for scorpion stings.
Spatial distribution
The map was prepared with the software QGIS 2.8 using estimates of the average incidence by municipality. The incidence rate was calculated as the ratio of cases by the population of each municipality estimated for every 100,000 inhabitants. Spatial interpolation of the incidence of cases was mapped using data from 167 municipalities was performed by the Inverse Distance Weight method.
Statistical analysis
Statistical analyses were performed using the Chi-square (Likelihood Ratio Chi-Square) test and Correspondence Analysis (ANACOR), Mann-Whitney and Kruskal-Wallis and Odds Ratio tests. The level of significance was P<0.05. All statistical analyses were performed using the software SPSS ® version 22.0 (Statistical Package for Social Sciences) for Windows.
Ethical approval
This study was approved by the Ethics Research Committee of the Federal University of Campina Grande (Protocol Nº 1.331.330/2015) and followed the guidelines established by the Declaration of Helsinki.
RESULTS
Spatial distribution
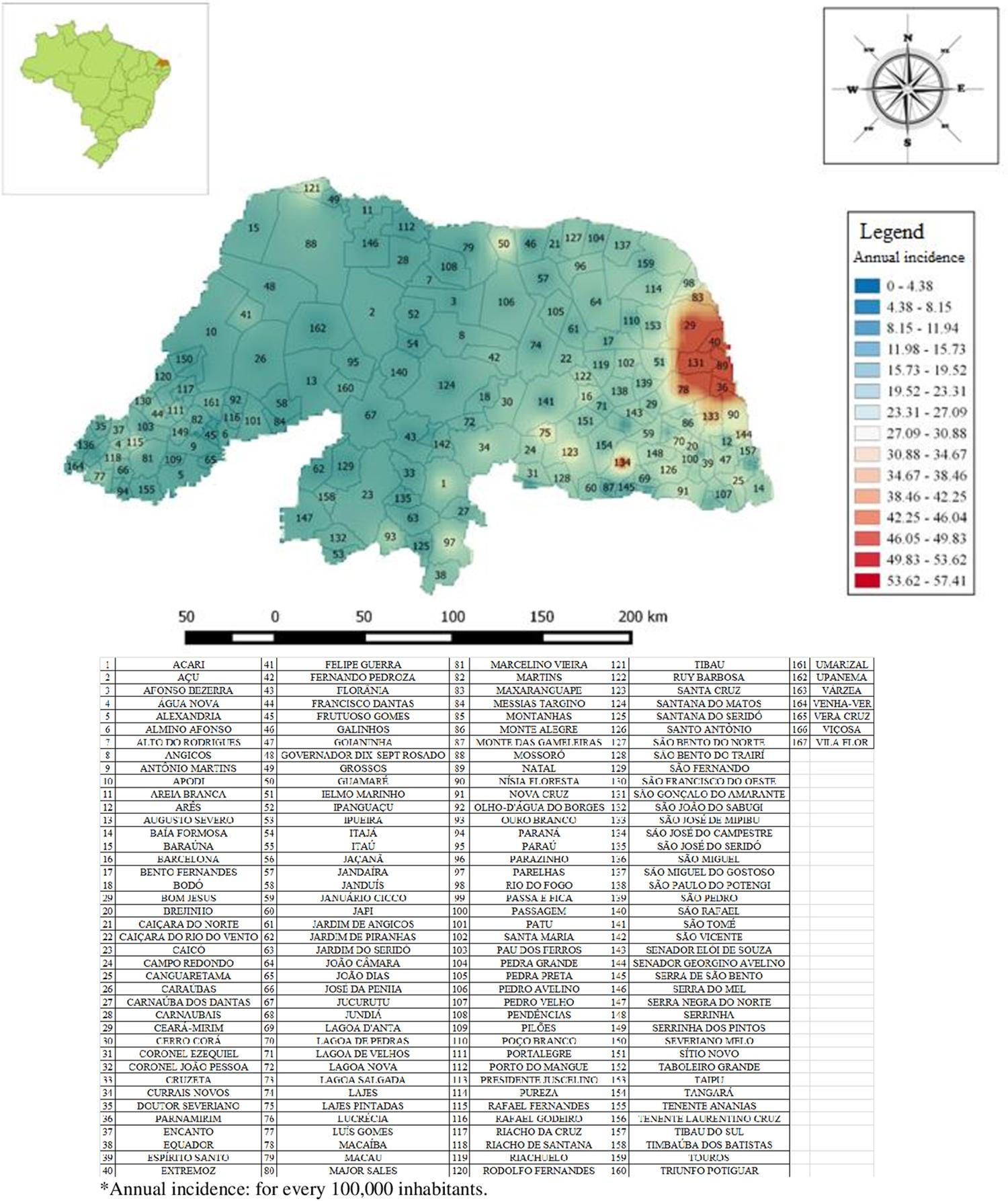
Incidence rates were unevenly distributed across the Rio Grande do Norte State, although there were scorpion sting cases reported in the 150 municipalities. Mapping showed a large area with high incidence rate in Eastern region of the State, in the vicinity of the capital (Natal), near the coast. In this region, the incidence rate was higher than 50 cases/100,000 inhabitants/year. The municipality of São José do Campestre , located in the South region of the State, has also exhibited a high incidence rate, of 50 cases/100,000 inhabitants/year. The incidence rate by municipality is presented in Figure 1 .
Spatial distribution of the scorpion stings cases in the Rio Grande do Norte State, from 2007 to 2014. *Annual incidence: for every 100,000 inhabitants.
Study population
A total of 20,555 scorpion sting cases were recorded by the Health Department of Rio Grande do Norte from January/2007 to December/2014. There was a gradual increase in the number of cases during the investigated period: from 1,280 in 2007 to 3,803 cases in 2014 (Figure 2A). The average incidence rates per 100,000 inhabitants were 41.50; 46.32; 70.69; 75.13; 91.16; 96.37; 101.01 and 111.57 cases from 2007 to 2014, respectively. Figure 2B shows that the scorpion sting cases were distributed in all months of the years studied, with higher frequencies in September (n=1,858; 9.04%), March (n=1,841; 8.96%) and May (n=1,825; 8.88%). No significant differences were observed among the months. Table 1 shows that the frequency of cases involving women (n=12,069; 61.19%) was higher than in men (n=7,423; 38.08%) (p<0.01). Regarding the age range of the victims, the largest number of cases was reported by individuals between 20 and 29 years old (n=3,983; 19.38%), followed by the age range between 30 and 39 years (n=3,307; 16.09%) (p<0.05). The frequency of cases was higher in urban (n=18,571; 90.35%) than in rural areas (n=1,175; 5.72%) (p<0.01). The body parts mostly stung were the foot (n=5,463; 26.58%), finger (n=5,087; 24.75%), toe (n=2,794; 13.59%) and hand (n= 2,411; 11.73%). There was significant difference when compared with other body parts (p<0.01). The most frequent time interval elapsed between sting and medical assistance was from 0 to 1 hour (n=7,894; 38.41%), followed by 1 to 3 hours (n=5,682; 27.64%). There was significant difference between time intervals, as well as between other intervals (p<0.01). Table 2 shows that the majority of cases were classified as mild (n=19,762; 96.15%), while few cases were classified as moderate (n=260; 1.26%) or severe (n=18; 0.09%). There was predominance of cases progressing to healing (n=19,332; 94.05%), 16 deaths were recorded and the average lethality rate was of 0.06%. Antivenom was used in 139 patients and the mean number of ampoules used was 2.6 per case. Table 3 shows that the most frequent local symptoms were pain (n=18,720; 96.04%), swelling (n=5,982; 30.69%), hyperemia (n=4,111; 21.09%), paresthesia (n=1,855; 9.52%), punctiform lesion (n=476; 2.44%) and erythema (n=266; 1.36%), whereas the most frequent systemic clinical symptoms were headache (n=376; 28.55%), sweating (n=233; 17.69%), fever (n=157; 11.92%), shivering (n=111; 8.43%), dizziness (n=107; 8.12%), vagal (n=98; 7.44%), chills (n=85; 6.45%), cramps (n=57; 4.33%), nervousness (n=50; 3.80%) and vomiting (n=47; 3.57%). Other local and systemic symptoms were also reported ( Table 3 ).
Distribution by year and month of scorpion sting cases in the Rio Grande do Norte State, from 2007 to 2014.
Epidemiological characteristics of scorpion sting cases in the Rio Grande do Norte State, from 2007 to 2014
Distribution of scorpion sting cases in Rio Grande do Norte State, from 2007 to 2014, according to the severity and progression of the case
Distribution of scorpion sting cases in Rio Grande do Norte , from 2007 to 2014, according to the local and systemic manifestations
DISCUSSION
A total of 20,555 scorpion sting cases were recorded in the Rio Grande do Norte State from 2007 to 2014. The cases increased from 1,280 in 2007 to 3,803 in 2014 (p <0.05) (Figure 2A). The incidence of cases also increased, from 41.50 in 2007 to 111.57 cases in 2014, with an average annual incidence of 79.22 cases/100,000 inhabitants. According to data from the Ministry of Health of Brazil, the Northeast and Southeast regions are those most affected by the injury, respectively. In the Northeast, the State of Alagoas exhibits the highest incidence rate, followed by Rio Grande do Norte 1111. Brasil. Ministério da Saúde. Sistema de Informação de Agravos de Notificação. Secretaria de Vigilância à Saúde. Incidência (100.000 hab) de casos de acidentes por escorpiões. Brasil, Grandes Regiões e Unidades Federadas. 2000 a 2013. [cited 2015 Mar 13]. Available from: http://u.saude.gov.br/images/pdf/2014/julho/10/Tabela-10---INCIDENCIA-CASOS---escorpiao---2000-a-2013---21-05-2013.pdf
http://u.saude.gov.br/images/pdf/2014/ju...
,1515. Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46. . Other epidemiological studies carried out in Northeastern Brazilian States also show an expressive increase in cases 1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.
17. Mesquita FN, Nunes MA, Santana VR, Machado Neto J, Almeida KB, Lima SO. Acidentes escorpiônicos no estado do Sergipe - Brasil. Rev Fac Ciênc Méd Sorocaba. 2015;17:15-20.-1818. Barbosa IR. Aspectos do escorpionismo no estado do Rio Grande do Norte. Rev Saúde.com. 2014;10:43-53. . The significant incidence of envenomation by scorpions suggests that the Rio Grande do Norte State may be considered an endemic area. The cases occurred in all months of the years investigated, with little variation among months (Figure 2B). This uniform monthly distribution of the cases may be related to the stable climate conditions of the studied region, which is characterized by high temperatures in all months of the year and a low rainfall index 1818. Barbosa IR. Aspectos do escorpionismo no estado do Rio Grande do Norte. Rev Saúde.com. 2014;10:43-53. . Stable climate conditions favor the activity and reproduction of scorpions, which can contribute to increase the number of cases in Northeastern Brazil 1919. Barros RM, Pasquino JA, Peixoto LR, Targino IT, Sousa JA, Leite RS. Clinical and epidemiological aspects of scorpion stings in the northeast region of Brazil. Cien Saude Colet. 2014;19:1275-82. . On the other hand, in the South and Southeast of Brazil, the incidence of stings seems to be related to seasonal factors. The highest frequency of cases occurs between the months of September and January, which are commonly the hottest and wettest 2020. Guerra CM, Carvalho LF, Colosimo E, Freire HB. Analysis of variables related to fatal outcomes of scorpion envenomation in children and adolescents in the state of Minas Gerais, Brazil, from 2001 to 2005. J Pediatr (Rio J). 2008;84:509-15. .
The distribution of cases in 150 counties indicates that scorpions are widely dispersed in the State. These municipalities make up the metropolitan region of Natal, suggesting that this region may be a high-risk area for scorpion poisoning 1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.,2121. Brites-Neto J, Brasil J. Estratégias de controle do escorpionismo no municipio de Americana, SP. Bol Epidemiol Paulista. 2012;9:4-15. . The high incidence of cases in Natal and neighboring municipalities may be explained by the physiognomic and socioeconomic characteristics of the large urban regions of Brazil 2222. Alves RS, Martins RD, Souza DF, Alves CD, Barbosa PS, Queiroz MG, et al. Aspectos epidemiológicos dos acidentes escorpiônicos no estado do Ceará no período de 2003 a 2004. Rev Eletrônica Pesq Méd. 2007;1:14-20.,2323. Lira-da-Silva RM, Amorim AM, Carvalho FM, Brazil TK. Acidentes por escorpião na cidade do Salvador, Bahia, Brasil (1982-2000). Gaz Méd Bahia. 2009;79 Supl 1:43-9. . Several authors have described the increase of scorpions in large Northeastern urban areas 1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.,1717. Mesquita FN, Nunes MA, Santana VR, Machado Neto J, Almeida KB, Lima SO. Acidentes escorpiônicos no estado do Sergipe - Brasil. Rev Fac Ciênc Méd Sorocaba. 2015;17:15-20.,2424. Biondi-de-Queiroz I, Santana VP, Rodrigues DS. Estudo retrospectivo do escorpionismo na Região Metropolitana de Salvador (RMS) - Bahia, Brasil. Sitientibus. 1996;15:273-85. . In a study carried out in Natal, it was reported that the most affected neighborhoods by scorpion sting are those with higher population density and disordered growth. In these districts, basic sanitation is deficient and there is accumulation of garbage and waste of construction materials 2525. Lima AL, Lima JA, Souto MC, Lopes TF, Torres UP, Maciel AC. Spatial distribution and epidemiological profile of scorpion accidents in Natal/RN. ConScientiae Saúde. 2011;10:627-33. . The difference between female (62%) and male (38%) cases shows that women are more exposed to the risk of envenomation than men. However, the risk of death was 1.39 times higher (0.868-2.238; p> 0.05) in men. The more regularly search for medical assistance by women may be related to the lower risk of death in cases of scorpion envenomation 2626. Almeida TS, Fook SM, França FO, Monteiro TM, Silva EL, Gomes LC, et al. Spatial distribution of scorpions according to the socioeconomic conditions in Campina Grande,State of Paraíba, Brazil. Rev Soc Bras Med Trop. 2016;49:477-85. . The highest frequency of cases involving the female gender was also reported in other States in the Northeast of Brazil 1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.,1717. Mesquita FN, Nunes MA, Santana VR, Machado Neto J, Almeida KB, Lima SO. Acidentes escorpiônicos no estado do Sergipe - Brasil. Rev Fac Ciênc Méd Sorocaba. 2015;17:15-20.,2727. Santos JM, Croesy GS, Marinho LF. Perfil epidemiológico dos acidentes escorpiônicos em crianças, no estado da Bahia, de 2007 a 2010. Rev Enferm Contemp. 2012;1:118-29. . In the Southeastern and Northern regions of Brazil, the male gender has been affected more frequently and the incidence is related to the professional activity performed by the individual 2828. Quadros RM, Varela AR, Cazarin MG, Marques SM. Acidentes escorpiônicos notificados pelo SINAN na Região Serrana de Santa Catarina, Brasil, 2000-2010. Rev Eletrônica Biol. 2014;7:96-108.,2929. Queiroz AM, Sampaio VS, Mendonça I, Fé NF, Sachett J, Ferreira LC, et al. Severity of scorpion stings in the Western Brazilian Amazon: a case-control study. PLoS One. 2015;10:0128819. . The cases are more frequent among men working in sawmills, wood warehouses, construction sites, ceramics, quarries, among others 3030. Nunes CS, Bevilacqua PD, Jardim CC. Aspectos demográficos e espaciais dos acidentes escorpiônicos no Distrito Sanitário Noroeste, Município de Belo Horizonte, Minas Gerais, 1993 a 1996. Cad Saude Publica. 2000;16:213-23. . On the other hand, the greater number of envenomation in women in the Northeast may be related to a greater exposure to scorpions in home environments, especially when performing domestic work activities. The majority of cases involved individuals aged between 20 and 49 years, indicating that the economically active population is the most affected by the stings. However, the risk of death is 4.23 times higher in individuals aged 0 and 9 years (p < 0.05) and 3.1 times higher in individuals aged 10 to 19 years (p < 0.05) when compared to other age groups. It was also observed that cases involving individuals older than 50 years are strongly associated with the development of moderate clinical symptoms (χ 2 = 13,256; p > 0.05). Our results are similar to those reported by Alves et al.2222. Alves RS, Martins RD, Souza DF, Alves CD, Barbosa PS, Queiroz MG, et al. Aspectos epidemiológicos dos acidentes escorpiônicos no estado do Ceará no período de 2003 a 2004. Rev Eletrônica Pesq Méd. 2007;1:14-20. in Ceará, Guerra et al.2020. Guerra CM, Carvalho LF, Colosimo E, Freire HB. Analysis of variables related to fatal outcomes of scorpion envenomation in children and adolescents in the state of Minas Gerais, Brazil, from 2001 to 2005. J Pediatr (Rio J). 2008;84:509-15. in Minas Gerais and Albuquerque et al.44. Albuquerque CM, Santana Neto PL, Amorim ML, Pires SC. Pediatric epidemiological aspects of scorpionism and report on fatal cases from Tityus stigmurus stings (Scorpiones: Buthidae) in State of Pernambuco, Brazil. Rev Soc Bras Med Trop. 2013;46:484-9. in Pernambuco. The highest risk in children and young people is possibly due to the highest amount of venom in the blood according to body surface, the species and the size of the scorpion, the amount of venom inoculated, the anatomical part of the body, the sensitivity of the victim to the venom, the immune system in formation and the greater permeability of the blood-brain barrier 3131. Oliveira HF, Costa CF, Sassi R. Relatos de acidentes por animais peçonhentos e medicina popular em agricultores de Cuité, região do Curimataú, Paraíba, Brasil. Rev Bras Epidemiol. 2013;16:633-43.
32. Benmosbah M, Guegueniat P, Mayence C, Egmann G, Narcisse E, Gonon S, et al. Epidemiological and clinical study on scorpionism in French Guiana. Toxicon. 2013;73:56-62.-3333. Soares MR, Azevedo CS, Maria M. Escorpionismo em Belo Horizonte , MG : um estudo retrospectivo. Rev Soc Bras Med Trop. 2002;35:359-63. . The highest toxicity in the elderly may be due to the decrease in the biotransformation intensity, in addition to its low renal excretion capacity, as well as the reduction of immunological activity 3333. Soares MR, Azevedo CS, Maria M. Escorpionismo em Belo Horizonte , MG : um estudo retrospectivo. Rev Soc Bras Med Trop. 2002;35:359-63.,3434. Maestri Neto A, Guedes AB, Carmo SF, Chalkidis HM, Coelho JS, Pardal PP. Aspectos do escorpionismo no Estado do Pará-Brasil. Rev Para Med. 2008;22:49-55. .
The disordered urban growth and high ecological plasticity of some scorpion species has altered the epidemiological profile of the cases in Brazil 1515. Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46. . The Northeast and Southeast regions are the most populous in the country, with about 70% of the population and degree of urbanization of 65% and 90%, respectively 1414. Bochner R, Struchiner CJ. Acidentes por animais peçonhentos e sistemas nacionais de informação. Cad Saude Publica. 2002;18(3):735-46. . Such socio-demographic characteristics associated with the scorpion adapted to the anthropic environment and the improvement in the notification system of the cases can explain the high incidence rates found in the urban area of these regions 3535. Bucaretchi F, Fernandes LC, Fernandes CB, Branco MM, Prado CC, Vieira RJ, et al. Clinical consequences of Tityus bahiensis and Tityus serrulatus scorpion stings in the region of Campinas, southeastern Brazil. Toxicon. 2014;89:17-25. . In our study, the majority of cases occurred in the urban area; however, the risk of death in the rural area was 6.27 times higher when compared to the other areas of occurrence (2,099-11,289; p <0,05), confirming the results reported by Guerra et al . 2020. Guerra CM, Carvalho LF, Colosimo E, Freire HB. Analysis of variables related to fatal outcomes of scorpion envenomation in children and adolescents in the state of Minas Gerais, Brazil, from 2001 to 2005. J Pediatr (Rio J). 2008;84:509-15. , Reckzigel and Pinto Júnior 1515. Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46. , and Queiroz et al . 2929. Queiroz AM, Sampaio VS, Mendonça I, Fé NF, Sachett J, Ferreira LC, et al. Severity of scorpion stings in the Western Brazilian Amazon: a case-control study. PLoS One. 2015;10:0128819. . The greater risk of death in rural areas may be related to the difficulty of the population in accessing health care centers 1515. Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46. and the lack of antivenom in hospitals and health services in smaller and municipalities distant from large urban centers 3636. Oliveira HF, Lopes YA, Barros RM, Vieira AA, Leite RS. Epidemiologia dos acidentes escorpiônicos na Paraiba - Nordeste do Brasil. Rev Biol Farm. 2012;8:86-96. . In this sense, it would be important to decentralize the distribution of antivenom in order to facilitate the access and improve the patient’s treatment 3737. Horta FM, Caldeira AP, Sares JA. Escorpionismo em crianças e adolescentes : aspectos clínicos e epidemiológicos de pacientes hospitalizados. Rev Soc Bras Med Trop. 2007;40:351-3. .
In our study, 60% of the cases received medical care up to 3 hours after the sting. In addition, from the 139 cases that performed the antivenom therapy, 64.75% received medical care up to 3 hours after the sting. These results indicate that the population is enlightened about the importance of seeking prompt medical care in case of scorpion sting. In addition, the manifestation of immediate acute pain at the site of the sting is an essential factor for the rapid search of medical care 3838. Ribeiro LA, Rodrigues L, Jorge MT. Aspectos clínicos e epidemiológicos do envenenamento por escorpiões em São Paulo e municípios próximos. Rev Patol Trop. 2001;30:83-92. . The rapid search for medical care may also be related to the greater occurrence of cases close to the medical service which is a determining factor in the ease of access to it 2323. Lira-da-Silva RM, Amorim AM, Carvalho FM, Brazil TK. Acidentes por escorpião na cidade do Salvador, Bahia, Brasil (1982-2000). Gaz Méd Bahia. 2009;79 Supl 1:43-9. . A strong association was observed among cases attended up to 3 hours after the sting with mild severity, indicating that early medical care may be an important factor for the patient’s clinical evolution (χ 2 = 86.797; p <0.05). In fact, patients who took 3 to 6 hours to receive medical care had a 1.67-fold higher risk of progression to a serious clinical condition; 6 to 12 hours had a 1.97-fold higher risk, and patients seen after 24 hours had a risk 2.51 times higher risk. These results show that the delay in medical care increases the risk of death, possibly due to the greater binding of the venom to the action sites 2020. Guerra CM, Carvalho LF, Colosimo E, Freire HB. Analysis of variables related to fatal outcomes of scorpion envenomation in children and adolescents in the state of Minas Gerais, Brazil, from 2001 to 2005. J Pediatr (Rio J). 2008;84:509-15. . Stings usually occur at a time when the victim performs activities such as putting on their shoes, wearing clothes, handling construction materials without gloves, and so on. This may explain the greater frequency of envenomation affecting the extremities of the victim’s body. In the present study, the body areas most affected by the stings were the foot and the hand, totaling 76.65% of the cases, confirming the results reported by other authors 1919. Barros RM, Pasquino JA, Peixoto LR, Targino IT, Sousa JA, Leite RS. Clinical and epidemiological aspects of scorpion stings in the northeast region of Brazil. Cien Saude Colet. 2014;19:1275-82.,2828. Quadros RM, Varela AR, Cazarin MG, Marques SM. Acidentes escorpiônicos notificados pelo SINAN na Região Serrana de Santa Catarina, Brasil, 2000-2010. Rev Eletrônica Biol. 2014;7:96-108.,3939. Pardal PP, Castro LC, Jennings E, Pardal JS, Monteiro MR. Aspectos epidemiológicos e clínicos do escorpionismo na região de Santarém, Estado do Pará, Brasil. Rev Soc Bras Med Trop. 2003;36:349-53. . However, the sting in the torso area has a risk of death 6.56 times higher than the other anatomical regions (1,848-23,300; p <0.05), showing that the anatomical region of the body affected by the sting may be an important factor for the severity and progression of the case. In fact, the closer to the vital organs, the greater the severity of the envenoming 4040. Nodari FR, Leite MD, Nascimento E. Aspectos demográficos, espaciais e temporais dos acidentes escorpiônicos ocorridos na área de abrangência da 3 a Regional de Saúde – Ponta Grossa, PR, no período de 2001 a 2004. Publication UEPG Cien Biol Saúde. 2006;12:15-26. . The transport velocity of the toxins depends on their physicochemical properties, on the constant rate of distribution and blood flow 4141. Winter ME. Basic clinical pharmacokinetics. 5ª ed. Baltimore: Lippincott Williams & Wilkins; 2010. . Tityus stigmurus has been referred to as the most involved species in envenomation in the Northeastern States of Brazil 99. Brazil TK, Lira-da-Silva RM, Porto TJ, Amorim AM, Silva TF. Escorpiões de importância médica do estado da Bahia, Brasil. Gaz Med Bahia. 2009;79 Supl 1:38-42.,4242. Lira-da-Silva RM, Amorim AM, Brazil TK. Envenenamento por Tityus stigmurus (Scorpiones; Buthidae) no Estado da Bahia, Brasil. Rev Soc Bras Med Trop. 2000;33:239-45. . Some local symptoms are characteristic of T. stigmurus envenoming, although the local clinical picture may show similarities with other species ( T. serrulatus and T. bahiensis ) 4343. Albuquerque IC, Albuquerque HN, Albuquerque EF, Nogueira AD, Cavalcanti ML. Escorpionismo em Campina Grande-PB. Rev Biol Cien Terra. 2004;4:1-8. . Local and systemic symptoms of injury by scorpion are similar regardless of the zoological differences among these arachnids 4343. Albuquerque IC, Albuquerque HN, Albuquerque EF, Nogueira AD, Cavalcanti ML. Escorpionismo em Campina Grande-PB. Rev Biol Cien Terra. 2004;4:1-8. . In our study, local symptoms were reported in 94.82% of the cases, which have also been reported in studies in the North 3939. Pardal PP, Castro LC, Jennings E, Pardal JS, Monteiro MR. Aspectos epidemiológicos e clínicos do escorpionismo na região de Santarém, Estado do Pará, Brasil. Rev Soc Bras Med Trop. 2003;36:349-53. , Northeast 1919. Barros RM, Pasquino JA, Peixoto LR, Targino IT, Sousa JA, Leite RS. Clinical and epidemiological aspects of scorpion stings in the northeast region of Brazil. Cien Saude Colet. 2014;19:1275-82.,2626. Almeida TS, Fook SM, França FO, Monteiro TM, Silva EL, Gomes LC, et al. Spatial distribution of scorpions according to the socioeconomic conditions in Campina Grande,State of Paraíba, Brazil. Rev Soc Bras Med Trop. 2016;49:477-85. and other regions of Brazil 66. Coelho JS, Ishikawa EA, Santos PR, Pardal PP. Scorpionism by Tityus silvestris in eastern Brazilian Amazon. J Venom Anim Toxins Incl Trop Dis. 2016;22. In Press.,4343. Albuquerque IC, Albuquerque HN, Albuquerque EF, Nogueira AD, Cavalcanti ML. Escorpionismo em Campina Grande-PB. Rev Biol Cien Terra. 2004;4:1-8. . Systemic symptoms were observed in 6.0% of the cases. The main systemic symptoms were: gastrointestinal, respiratory, neurological and cardiovascular. These systemic symptoms were also reported in studies conducted in the Northeastern 44. Albuquerque CM, Santana Neto PL, Amorim ML, Pires SC. Pediatric epidemiological aspects of scorpionism and report on fatal cases from Tityus stigmurus stings (Scorpiones: Buthidae) in State of Pernambuco, Brazil. Rev Soc Bras Med Trop. 2013;46:484-9.,1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.,1919. Barros RM, Pasquino JA, Peixoto LR, Targino IT, Sousa JA, Leite RS. Clinical and epidemiological aspects of scorpion stings in the northeast region of Brazil. Cien Saude Colet. 2014;19:1275-82. and Southeastern Brazil 3838. Ribeiro LA, Rodrigues L, Jorge MT. Aspectos clínicos e epidemiológicos do envenenamento por escorpiões em São Paulo e municípios próximos. Rev Patol Trop. 2001;30:83-92. . The mild severity and progression to cure in the majority of cases reported in the present study are in agreement with the data of the Ministry of Health and other authors 1818. Barbosa IR. Aspectos do escorpionismo no estado do Rio Grande do Norte. Rev Saúde.com. 2014;10:43-53.,2222. Alves RS, Martins RD, Souza DF, Alves CD, Barbosa PS, Queiroz MG, et al. Aspectos epidemiológicos dos acidentes escorpiônicos no estado do Ceará no período de 2003 a 2004. Rev Eletrônica Pesq Méd. 2007;1:14-20.,4444. Santos PL, Martins FJ, Vieira RC, Ribeiro LC, Barbosa NR. Características dos acidentes escorpiônicos em Juiz de Fora - MG. Rev APS. 2010;13:164-9. . Our results show that the incidence of cases in Rio Grande do Norte State is high, but the number of deaths is low. The average lethality found was 0.06%, which can be considered low when compared to data from the North, Southeast and Central-West region of Brazil 1515. Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46. . However, this lethality is similar to the one found in Ceará (0.07%) 1616. Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15. and in Sergipe (0.06%) 1717. Mesquita FN, Nunes MA, Santana VR, Machado Neto J, Almeida KB, Lima SO. Acidentes escorpiônicos no estado do Sergipe - Brasil. Rev Fac Ciênc Méd Sorocaba. 2015;17:15-20. States. In our study, it was observed that the majority of the cases were attended up to 3 hours after the sting. In addition, 64.75% of the cases, in which the antivenom therapy was performed, were treated within the first 3 hours after the sting. Despite the high number of cases, rapid therapeutic interventions and treatment efficiency appear to have contributed to the low lethality.
CONCLUSIONS
The high incidence of scorpion sting cases suggests that the Rio Grande do Norte State may be considered an endemic area. The occurrence of cases in 150 municipalities indicates the wide dispersion of scorpions in the State. Most cases occurred in urban areas throughout the year, with little variation between months. Cases were more frequent in young women, and the extremities of the limbs (foot and hand) are the body parts most affected by the stings. Medical care has been performed at the appropriate time. Local symptoms are more frequent than systemic symptoms and cases predominantly exhibit mild severity and progress to cure. The high incidence of cases in Rio Grande do Norte State suggests that the scorpion sting may be considered a public health problem that must be monitored and controlled throughout the year. Future studies on the species and community structure of those scorpions existing in the Northeast region are necessary to better understand the species involved in the scorpion envenomation.
ACKNOWLEDGEMENTS
This study was supported by the Instituto Nacional de Ciência e Tecnologia em Toxinas (INCTTOX). The authors are grateful to the workers of the Health Department of the Rio Grande do Norte State for kindly providing us with the epidemiological data. The authors thank Luis Fernando Lunardello Casado for the English review.
REFERENCES
-
1Chippaux JP, Goyffon M. Epidemiology of scorpionism: A global appraisal. Acta Trop. 2008;107:71-9.
-
2Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual de controle de escorpiões. Brasília: Ministério da Saúde; 2009.
-
3Brazil TK, Porto TJ. Os escorpiões. Salvador: EDUFBA; 2010.
-
4Albuquerque CM, Santana Neto PL, Amorim ML, Pires SC. Pediatric epidemiological aspects of scorpionism and report on fatal cases from Tityus stigmurus stings (Scorpiones: Buthidae) in State of Pernambuco, Brazil. Rev Soc Bras Med Trop. 2013;46:484-9.
-
5Cardoso JL, França FS, Wen FH, Malaque CM, Haddad Júnior V. Animais peçonhentos no Brasil: biologia, clínica e terapêutica dos acidentes. 2ª ed. São Paulo: Sarvier; 2009.
-
6Coelho JS, Ishikawa EA, Santos PR, Pardal PP. Scorpionism by Tityus silvestris in eastern Brazilian Amazon. J Venom Anim Toxins Incl Trop Dis. 2016;22. In Press.
-
7Albuquerque CM, Porto TJ, Amorim ML, Santana Neto PL. Escorpionismo por Tityus pusillus Pocock, 1893 (Scorpiones; Buthidae) no Estado de Pernambuco. Rev Soc Bras Med Trop. 2009;42:206-8.
-
8Wen FH, Monteiro WM, Silva AM, Tambourgi DV, Silva IM, Sampaio VS, et al. Snakebites and scorpion stings in the Brazilian Amazon: identifying research priorities for a largely neglected problem. PLoS Negl Trop Dis. 2015;9:e0003701.
-
9Brazil TK, Lira-da-Silva RM, Porto TJ, Amorim AM, Silva TF. Escorpiões de importância médica do estado da Bahia, Brasil. Gaz Med Bahia. 2009;79 Supl 1:38-42.
-
10Brasil. Ministério da Saúde. Fundação Nacional de Saúde. Manual de diagnóstico e tratamento de acidentes por animais peçonhentos. 2 a ed. Brasília: Ministério da Saúde; 2001.
-
11Brasil. Ministério da Saúde. Sistema de Informação de Agravos de Notificação. Secretaria de Vigilância à Saúde. Incidência (100.000 hab) de casos de acidentes por escorpiões. Brasil, Grandes Regiões e Unidades Federadas. 2000 a 2013. [cited 2015 Mar 13]. Available from: http://u.saude.gov.br/images/pdf/2014/julho/10/Tabela-10---INCIDENCIA-CASOS---escorpiao---2000-a-2013---21-05-2013.pdf
» http://u.saude.gov.br/images/pdf/2014/julho/10/Tabela-10---INCIDENCIA-CASOS---escorpiao---2000-a-2013---21-05-2013.pdf -
12Instituto Brasileiro de Geografia e Estatística. Censo 2010. [cited 2017 May 11]. Available from: http://censo2010.ibge.gov.br/
» http://censo2010.ibge.gov.br/ -
13Brasil. Ministério do Meio Ambiente. Secretaria de Recursos Hídricos. Atlas das áreas susceptíveis à desertificação do Brasil. Brasília: Ministério do Meio Ambiente; 2007.
-
14Bochner R, Struchiner CJ. Acidentes por animais peçonhentos e sistemas nacionais de informação. Cad Saude Publica. 2002;18(3):735-46.
-
15Reckzigel GC, Pinto Júnior VL. Scorpionism in Brazil in the years 2000 to 2012. J Venom Anim Toxins Incl Trop Dis. 2014;20:46.
-
16Furtado SS, Belmino JF, Diniz AG, Leite RS. Epidemiology of scorpion envenomation in the state of Ceará, Northeastern Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:15.
-
17Mesquita FN, Nunes MA, Santana VR, Machado Neto J, Almeida KB, Lima SO. Acidentes escorpiônicos no estado do Sergipe - Brasil. Rev Fac Ciênc Méd Sorocaba. 2015;17:15-20.
-
18Barbosa IR. Aspectos do escorpionismo no estado do Rio Grande do Norte. Rev Saúde.com. 2014;10:43-53.
-
19Barros RM, Pasquino JA, Peixoto LR, Targino IT, Sousa JA, Leite RS. Clinical and epidemiological aspects of scorpion stings in the northeast region of Brazil. Cien Saude Colet. 2014;19:1275-82.
-
20Guerra CM, Carvalho LF, Colosimo E, Freire HB. Analysis of variables related to fatal outcomes of scorpion envenomation in children and adolescents in the state of Minas Gerais, Brazil, from 2001 to 2005. J Pediatr (Rio J). 2008;84:509-15.
-
21Brites-Neto J, Brasil J. Estratégias de controle do escorpionismo no municipio de Americana, SP. Bol Epidemiol Paulista. 2012;9:4-15.
-
22Alves RS, Martins RD, Souza DF, Alves CD, Barbosa PS, Queiroz MG, et al. Aspectos epidemiológicos dos acidentes escorpiônicos no estado do Ceará no período de 2003 a 2004. Rev Eletrônica Pesq Méd. 2007;1:14-20.
-
23Lira-da-Silva RM, Amorim AM, Carvalho FM, Brazil TK. Acidentes por escorpião na cidade do Salvador, Bahia, Brasil (1982-2000). Gaz Méd Bahia. 2009;79 Supl 1:43-9.
-
24Biondi-de-Queiroz I, Santana VP, Rodrigues DS. Estudo retrospectivo do escorpionismo na Região Metropolitana de Salvador (RMS) - Bahia, Brasil. Sitientibus. 1996;15:273-85.
-
25Lima AL, Lima JA, Souto MC, Lopes TF, Torres UP, Maciel AC. Spatial distribution and epidemiological profile of scorpion accidents in Natal/RN. ConScientiae Saúde. 2011;10:627-33.
-
26Almeida TS, Fook SM, França FO, Monteiro TM, Silva EL, Gomes LC, et al. Spatial distribution of scorpions according to the socioeconomic conditions in Campina Grande,State of Paraíba, Brazil. Rev Soc Bras Med Trop. 2016;49:477-85.
-
27Santos JM, Croesy GS, Marinho LF. Perfil epidemiológico dos acidentes escorpiônicos em crianças, no estado da Bahia, de 2007 a 2010. Rev Enferm Contemp. 2012;1:118-29.
-
28Quadros RM, Varela AR, Cazarin MG, Marques SM. Acidentes escorpiônicos notificados pelo SINAN na Região Serrana de Santa Catarina, Brasil, 2000-2010. Rev Eletrônica Biol. 2014;7:96-108.
-
29Queiroz AM, Sampaio VS, Mendonça I, Fé NF, Sachett J, Ferreira LC, et al. Severity of scorpion stings in the Western Brazilian Amazon: a case-control study. PLoS One. 2015;10:0128819.
-
30Nunes CS, Bevilacqua PD, Jardim CC. Aspectos demográficos e espaciais dos acidentes escorpiônicos no Distrito Sanitário Noroeste, Município de Belo Horizonte, Minas Gerais, 1993 a 1996. Cad Saude Publica. 2000;16:213-23.
-
31Oliveira HF, Costa CF, Sassi R. Relatos de acidentes por animais peçonhentos e medicina popular em agricultores de Cuité, região do Curimataú, Paraíba, Brasil. Rev Bras Epidemiol. 2013;16:633-43.
-
32Benmosbah M, Guegueniat P, Mayence C, Egmann G, Narcisse E, Gonon S, et al. Epidemiological and clinical study on scorpionism in French Guiana. Toxicon. 2013;73:56-62.
-
33Soares MR, Azevedo CS, Maria M. Escorpionismo em Belo Horizonte , MG : um estudo retrospectivo. Rev Soc Bras Med Trop. 2002;35:359-63.
-
34Maestri Neto A, Guedes AB, Carmo SF, Chalkidis HM, Coelho JS, Pardal PP. Aspectos do escorpionismo no Estado do Pará-Brasil. Rev Para Med. 2008;22:49-55.
-
35Bucaretchi F, Fernandes LC, Fernandes CB, Branco MM, Prado CC, Vieira RJ, et al. Clinical consequences of Tityus bahiensis and Tityus serrulatus scorpion stings in the region of Campinas, southeastern Brazil. Toxicon. 2014;89:17-25.
-
36Oliveira HF, Lopes YA, Barros RM, Vieira AA, Leite RS. Epidemiologia dos acidentes escorpiônicos na Paraiba - Nordeste do Brasil. Rev Biol Farm. 2012;8:86-96.
-
37Horta FM, Caldeira AP, Sares JA. Escorpionismo em crianças e adolescentes : aspectos clínicos e epidemiológicos de pacientes hospitalizados. Rev Soc Bras Med Trop. 2007;40:351-3.
-
38Ribeiro LA, Rodrigues L, Jorge MT. Aspectos clínicos e epidemiológicos do envenenamento por escorpiões em São Paulo e municípios próximos. Rev Patol Trop. 2001;30:83-92.
-
39Pardal PP, Castro LC, Jennings E, Pardal JS, Monteiro MR. Aspectos epidemiológicos e clínicos do escorpionismo na região de Santarém, Estado do Pará, Brasil. Rev Soc Bras Med Trop. 2003;36:349-53.
-
40Nodari FR, Leite MD, Nascimento E. Aspectos demográficos, espaciais e temporais dos acidentes escorpiônicos ocorridos na área de abrangência da 3 a Regional de Saúde – Ponta Grossa, PR, no período de 2001 a 2004. Publication UEPG Cien Biol Saúde. 2006;12:15-26.
-
41Winter ME. Basic clinical pharmacokinetics. 5ª ed. Baltimore: Lippincott Williams & Wilkins; 2010.
-
42Lira-da-Silva RM, Amorim AM, Brazil TK. Envenenamento por Tityus stigmurus (Scorpiones; Buthidae) no Estado da Bahia, Brasil. Rev Soc Bras Med Trop. 2000;33:239-45.
-
43Albuquerque IC, Albuquerque HN, Albuquerque EF, Nogueira AD, Cavalcanti ML. Escorpionismo em Campina Grande-PB. Rev Biol Cien Terra. 2004;4:1-8.
-
44Santos PL, Martins FJ, Vieira RC, Ribeiro LC, Barbosa NR. Características dos acidentes escorpiônicos em Juiz de Fora - MG. Rev APS. 2010;13:164-9.
Publication Dates
-
Publication in this collection
2017
History
-
Received
2 Apr 2017 -
Accepted
11 May 2017