Abstracts
INTRODUCTION: The Amazon region has extensive forested areas and natural ecosystems, providing favorable conditions for the existence of innumerous arboviruses. Over 200 arboviruses have been isolated in Brazil and about 40 are associated with human disease. Four out of 40 are considered to be of public health importance in Brazil: Dengue viruses (1-4), Oropouche, Mayaro and Yellow Fever. Along with these viruses, about 98% of the malaria cases are restricted to the Legal Amazon region. METHODS: This study aimed to investigate the presence of arboviruses in 111 clinical serum samples from patients living in Novo Repartimento (Pará), Plácido de Castro (Acre), Porto Velho (Rondônia) and Oiapoque (Amapá). The viral RNA was extracted and RT-PCR was performed followed by a Multiplex-Nested-PCR, using Flavivirus, Alphavirus and Orthobunyavirus generic and species-specific primers. RESULTS: Dengue virus serotype 2 was detected in two patients living in Novo Repartimento (Pará) that also presented active Plasmodium vivax infection. CONCLUSIONS: Despite scant data, this situation is likely to occur more frequently than detected in the Amazon region. Finally, it is important to remember that both diseases have similar clinical findings, thus the diagnosis could be made concomitantly for dengue and malaria in patients living or returning from areas where both diseases are endemic or during dengue outbreaks.
Arboviruses; Coinfection; Flaviviruses; Dengue; Malaria; Amazon region
INTRODUÇÃO: A região Amazônica possui extensas áreas florestadas e ecossistemas naturais, provendo condições favoráveis para a existência de diversos arbovírus. Aproximadamente, 200 arbovírus foram isolados no Brasil, e 40 estão associados com doenças em humanos. Quatro destes 40 são considerados ser de importância para a saúde pública no Brasil: vírus da dengue (1-4), Oropouche, Mayaro e febre amarela. Juntamente com estes vírus, aproximadamente 98% dos casos de malária estão restritos à região da Amazônia Legal. MÉTODOS: O objetivo deste estudo foi investigar a presença de arbovírus em 111 amostras clínicas de sangue de pacientes que residiam em Novo Repartimento (Pará), Plácido de Castro (Acre), Porto Velho (Rondônia) and Amapá (Macapá). O RNA viral foi extraído, RT-PCR foi realizada seguida de uma Multiplex-Nested-PCR, usando primers genéricos e espécie-específicos para Flavivirus, Alphavirus and Orthobunyavirus. RESULTADOS: Detectamos o vírus da dengue, sorotipo 2, em dois pacientes que residiam em Novo Repartimento (Pará), que também tinham infecção por Plasmodium vivax. CONCLUSÕES: Apesar de dados escassos, esta situação, provavelmente, ocorre mais frequência que a detectada na região Amazônica. Definitivamente, é importante lembrar que ambas as doenças possuem achados clínicos similares, assim o diagnóstico deveria ser feito concomitantemente para dengue e malária em pacientes que residem ou estão voltando de áreas onde ambas as doenças são endêmicas.
Arbovírus; Co-infecção; Flavivírus; Dengue; Malária; Região Amazônica
ARTICLE ARTIGO
Concurrent dengue and malaria in the Amazon region
Co-infecção por dengue e malária na região Amazônica
Vinícius dos Santos SantanaI,II; Lígia Carolina LavezzoI,II; Adriano MondiniI; Ana Carolina Bernardes TerzianI; Roberta Vieira de Moraes BronzoniI; Andrea Regina Baptista RossitIII; Ricardo Luiz Dantas MachadoIII; Paula RahalII; Mara Correa Lelles NogueiraIII; Maurício Lacerda NogueiraI,III
ILaboratory of Virology, São José do Rio Preto Medical School, São José do Rio Preto, SP, Brazil
IIGraduated Program in Microbiology, São Paulo State University, São José do Rio Preto, SP, Brazil
IIIDepartment of Dermatology and Infectious Diseases, São José do Rio Preto Medical School, São José do Rio Preto, SP, Brazil
Address to Address to: Prof. Maurício Lacerda Nogueira Laboratório de Pesquisa em Virologia/FAMERP Av. Brigadeiro Faria Lima 5416, Vila São Pedro 15090-000 São José do Rio Preto, SP, Brazil Phone: 55 17 3201-5731 e-mail: mauricio.nogueira@pq.cnpq.br
ABSTRACT
INTRODUCTION: The Amazon region has extensive forested areas and natural ecosystems, providing favorable conditions for the existence of innumerous arboviruses. Over 200 arboviruses have been isolated in Brazil and about 40 are associated with human disease. Four out of 40 are considered to be of public health importance in Brazil: Dengue viruses (1-4), Oropouche, Mayaro and Yellow Fever. Along with these viruses, about 98% of the malaria cases are restricted to the Legal Amazon region.
METHODS: This study aimed to investigate the presence of arboviruses in 111 clinical serum samples from patients living in Novo Repartimento (Pará), Plácido de Castro (Acre), Porto Velho (Rondônia) and Oiapoque (Amapá). The viral RNA was extracted and RT-PCR was performed followed by a Multiplex-Nested-PCR, using Flavivirus, Alphavirus and Orthobunyavirus generic and species-specific primers.
RESULTS: Dengue virus serotype 2 was detected in two patients living in Novo Repartimento (Pará) that also presented active Plasmodium vivax infection.
CONCLUSIONS: Despite scant data, this situation is likely to occur more frequently than detected in the Amazon region. Finally, it is important to remember that both diseases have similar clinical findings, thus the diagnosis could be made concomitantly for dengue and malaria in patients living or returning from areas where both diseases are endemic or during dengue outbreaks.
Key-words: Arboviruses. Coinfection. Flaviviruses. Dengue. Malaria. Amazon region.
RESUMO
INTRODUÇÃO: A região Amazônica possui extensas áreas florestadas e ecossistemas naturais, provendo condições favoráveis para a existência de diversos arbovírus. Aproximadamente, 200 arbovírus foram isolados no Brasil, e 40 estão associados com doenças em humanos. Quatro destes 40 são considerados ser de importância para a saúde pública no Brasil: vírus da dengue (1-4), Oropouche, Mayaro e febre amarela. Juntamente com estes vírus, aproximadamente 98% dos casos de malária estão restritos à região da Amazônia Legal.
MÉTODOS: O objetivo deste estudo foi investigar a presença de arbovírus em 111 amostras clínicas de sangue de pacientes que residiam em Novo Repartimento (Pará), Plácido de Castro (Acre), Porto Velho (Rondônia) and Amapá (Macapá). O RNA viral foi extraído, RT-PCR foi realizada seguida de uma Multiplex-Nested-PCR, usando primers genéricos e espécie-específicos para Flavivirus, Alphavirus and Orthobunyavirus.
RESULTADOS: Detectamos o vírus da dengue, sorotipo 2, em dois pacientes que residiam em Novo Repartimento (Pará), que também tinham infecção por Plasmodium vivax.
CONCLUSÕES: Apesar de dados escassos, esta situação, provavelmente, ocorre mais frequência que a detectada na região Amazônica. Definitivamente, é importante lembrar que ambas as doenças possuem achados clínicos similares, assim o diagnóstico deveria ser feito concomitantemente para dengue e malária em pacientes que residem ou estão voltando de áreas onde ambas as doenças são endêmicas.
Palavras-chaves: Arbovírus. Co-infecção. Flavivírus. Dengue. Malária. Região Amazônica.
INTRODUCTION
Every year, thousands cases of malaria are diagnosed and about 98% of them are restricted to the Legal Amazon region1. However, in the Brazilian Amazon region, approximately 200 arboviruses have been isolated and about 40 have been associated with human disease. Among these viruses, dengue viruses are the most important flavivirus causing human disease and outbreaks of important public health impact2.
Recently, concurrent dengue and malaria was reported in the Amazon region of French Guiana3. Altogether, there are few reports concerning dengue and malaria coinfection and all of them were isolated cases4-10.
In the Brazilian Amazon region, concomitant infection with malaria and arbovirus was reported in 1990, though the first detection was in 1971. Five other incidences were identified in 1974, 1983, 1984 and 1987. These cases of fever of unknown origin were previously diagnosed as malaria and despite treatment, the symptoms remained. The agents identified were Catu, Guaroa and Tacaiuma viruses, all belonging to the genus Orthobunyavirus, family Bunyaviridae11. Since the 1980s dengue has become a major public health issue in Brazil and has become more frequent in the Amazon region. Thus, the aim of this study was to investigate the presence of arboviruses (especially dengue virus) in clinical samples from patients with malaria residing in the Amazon region.
METHODS
Study areas
Oiapoque (03º50'35" S; 51º50'06" W) is 560km from the capital of State of Amapá, and is located on the Amazon River within tropical forest. Its estimated population is 20,962 inhabitants and its Annual Parasitic Index (API) was 6.0 in 2009. Porto Velho (-8º45' 43" S; 63º54'14"W) is the capital of State of Rondônia in the upper Amazon River basin, with 383,425 inhabitants and an API of 53.7 in 2009. Plácido de Castro (10º16'33" S; 67º09'00"W) is located at the border of the country Bolivia as well as Rondonia and Amazonas States, it has a population of 18,235 inhabitants and its API was 20.6 in 2009. Novo Repartimento (04º19' 50" S; 49º47' 47"W) is a gold mining area in southeastern State of Pará. Its population is estimated at 55,759 habitants and it had an API of 15.4 in 2009. The climate in these areas is characterized as tropical with no dry season; the mean monthly precipitation level is at least 60mm.
Clinical samples
Male and female malaria patients (n=111) from four regions of the Brazilian Amazon were enrolled in this study: 40 samples from Novo Repartimento, 29 samples from Porto Velho and 30 samples from Plácido de Castro were obtained from May 2003 to August 2005. Additionally, 12 samples from the municipality of Oiapoque, State of Amapá were obtained in 2009 (Figure 1). These individuals sought attendance on their own initiative and were invited to participate in this study at the public healthcare clinics in each study area. They were all over 18 years-old and had positive thick blood film results for P. falciparum or P. vivax single infection. Pregnant women, patients under 18 years-old and those with no other concomitant illness were excluded from the study. Participants were asked to sign a written free informed consent form before blood samples were collected. The consent form was cosigned by a staff member of the clinic. Clinical and epidemiological data such as age, sex, past history of malaria and current infection information were obtained during a specific interview conducted by the physicians and also from medical records.
Clinical evaluation
All patients voluntarily sought medical assistance presenting with uncomplicated clinical malaria symptoms, as determined by the physicians and/or nurses enrolled in the malaria diagnosis and treatment routine of the Brazilian government national program. Individuals who presented at least one of the following symptoms: fever, headache, and shivering, in addition to microscopic positivity, were included in the post diagnostic medical evaluation. Likewise, symptoms were defined as present or absent by the medical staff according to the temperature measurements performed by the nurses and also by a detailed, specific interview, regarding unusual and/or previously experienced clinical malaria manifestation. Of all the clinical aspects recorded during the 111 malaria attacks, a typical febrile paroxysm was the most frequent clinical symptom, observed in 97.4% of cases, as a single or an associated manifestation. Associations between the three clinical aspects assessed (fever, headache and shivering) showed fever plus headache in 85.2% of cases, while fever plus shivering was reported in 88.7%.
Study strategy
The sera were stored at -80ºC. Viral RNA was extracted from 140µl of each serum with the QIAamp viral RNA Mini kit (QIAGEN, Inc.) in accordance with the manufacturer's instructions and yielded a final volume of 60µl.
Initially, clinical samples were tested for the presence of flavivirus and alphavirus, as described by Bronzoni et al12. A Dulplex-RT-PCR (D-RT-PCR) was performed using Flavivirus and Alphavirus universal primers simultaneously. After, three Multiplex-Nested-PCR (M-N-PCR) were performed using specie-specific primers to detect and identify dengue virus (DENV1-3), yellow fever virus (YFV) and Saint Louis Encephalitis virus (SLEV); another to detect DENV-4, Rocio virus (ROCV), Ilhéus virus (ILHV) and West Nile virus (WNV); and a third to detect Eastern Equine Encephalitis virus (EEEV), Venezuelan Equine Encephalitis virus (VEEV), Western Equine Encephalitis virus (WEEV), Mayaro virus (MAYV) and Aura virus (AURAV). Finally, a RT-PCR with primers that anneal to the 5' and 3' extremities of the genome segments of bunyaviruses and internal primers that anneal to the S segment of Simbu serogroup viruses in a Nested PCR was used to amplify the Oropouche virus genome, as described by Morelli et al13. The amplicons were loaded into a 1% agarose electrophoresis gel and visualized under ultraviolet light. Amplicon sizes were determined by comparison with a 100bp DNA ladder (Promega). Precautions to avoid contamination were followed; positive and negative controls were used in all reactions. All amplicons were also sequenced in order to confirm the specificity of the amplification using the PCR primers Big Dye v3.1 (Applied Biosytems, CA) in a ABI3130 automated sequencer.
Ethical
The protocol for this study was reviewed and approved by the Research Board of the Faculty of Medicine from São José do Rio Preto.
RESULTS
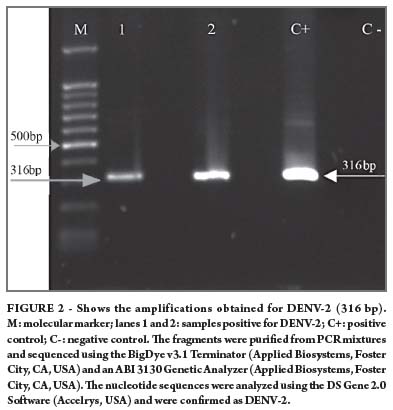
Of the total of 111 malaria-positive patients that were tested for arboviral detection, 80 presented Plasmodium vivax and 31 presented Plasmodium falciparum infections. Concurrent dengue virus serotype 2 and malaria were confirmed in 2 of the 111 patients (Figure 2), who possessed prior laboratorial diagnosis of malaria before molecular screening for arboviruses. These patients were a 57 year-old male and a 20 year-old female living in Novo Repartimento (Pará) and both had active Plasmodium vivax infections.
Virus isolation was attempted but was unsuccessful, because it is very difficult to isolate arboviruses and the blood samples have to be collected when the viremia is occurring, which means during the first 5 days of the disease.
DISCUSSION
The Brazilian Amazon region has extensive forested areas, natural ecosystems and a large diversity of animals that provide a suitable environment for arbovirus transmission. Currently, 99.8% percent of malaria cases are restricted to the Legal Amazon region1, where approximately 40 arboviruses considered to be of importance to public health cocirculate14.
In Brazil, 54 species of Anopheles mosquitoes are currently known and 33 of these occur in the Brazilian Amazon region15,16. An darlingi, An nuneztovari and An albitarsis are considered of special interest, because they have been detected with Plasmodium infection near human habitations15. Nowadays, An darlingi is the main vector, because it is highly antrophofilic. An nuneztovari, An triannulatus and An albitarsis are considered to be secondary vectors, since they are detected with Plasmodium infection only in areas where An darlingi initiated an outbreak16.
However, some arboviruses isolated in the Amazon region have Anopheles sp mosquitoes as their vectors, including: the widely spread Guaroa virus that is associated with sporadic cases in the rural area, isolated from An triannulatus and An nuneztovari; and Tacaiuma virus, associated with sporadic cases in enzootic foci, isolated from An Triannulatus17.
Despite these reports, the concomitance of dengue and malaria reported here is merely incidental, because this arbovirus has Aedes aegypti and Aedes albopictus mosquitoes as vectors18, which are not considered to be vectors of Plasmodium sp protozoans.
Mixed infections with many etiologic agents are not uncommon in malaria19. Despite scant data, dengue and malaria coinfection should be common in areas where both diseases are co-endemic in many places of the world10. In the Amazon region of Brazil, this situation is likely to occur more frequently than detected, considering that malaria is the most prevalent disease1 and dengue is endemic to this region as well20. In this context,  coninfection with malaria and dengue cannot be ruled out and should be suspected in patients living or returning from areas where both diseases are endemic.
coninfection with malaria and dengue cannot be ruled out and should be suspected in patients living or returning from areas where both diseases are endemic.
The most common clinical findings for dengue are fever (100%), myalgia (79%), rash (79%), headache (68%), nausea (37%) and diarrhea (37%)21. Similarly, the typical clinical findings for malaria are high-grade fever followed by chills, profuse sweating and headache that occur intermittently depending on the infecting Plasmodium species. However, in some patients prodromal symptoms appear some days before disease paroxysms, including nausea, vomiting, asthenia, fatigue and anorexia1. In the Brazilian Amazon region, malaria predominates in Mesoendemic conditions with wide variations in transmission, as can be observed by the nonimmune or semi-immune status of the adult population, as well as by asymptomatic carriers. An explanation for the reduction in symptoms in mixed infection carriers could be the mean age of the affected patients and time of residence in the endemic area, since it is well documented by different authors that immunity can play an important role in malaria symptom relief22,23. Consequently, minor clinical evidence for malaria was noted by the patients studied once a reduction in the severity of malaria symptoms was reported in individuals with limited preexposure to different species24. Nevertheless, it is not a general consensus that higher fevers, per se, are the consequence of greater clinical severity or more effective immune response25.
In a recent study regarding diagnostic techniques and management of dengue and malaria coinfection, all patients with dual infection presented prolonged fever for more than seven days, myalgia, bleeding manifestations, rash and anemia26. Moreover, according to Vasconcelos et al, the continuous fever caused by arboviral infection can mask the periodic fever associated with malarial parasites11.
Although a reduced sample number was assessed in this study, a limitation that we acknowledge, it is important to remember that dengue and malaria coinfection requires special attention because delayed diagnosis and appropriated treatment can result in fatal complications6,10. Both diseases cause similar symptoms and simultaneous infections with two different infectious agents may result in overlapped symptoms4, diagnosis of malaria and dengue based purely on clinical grounds may become difficult for physicians10 and it is possible that either clinical spectrum of the disease or treatment may also be affected9. Finally, it is important to remember that both diseases have similar clinical findings, thus the diagnosis could be made concomitantly for dengue and malaria in patients living or returning from areas where both diseases are endemic or during dengue outbreaks.
ACKNOWLEDGMENTS
The authors would like to thank all the individuals enrolled in this study; Aline Barroso, Maria Cristina Figueredo and Mauro Tada for their assistance during the malaria field work; and Prof. Luiz Hildebrando Pereira da Silva for permission to use the facilities at CEPEM.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
FINANCIAL SUPPORT
This work was supported by the Fundação de Amparo à Pesquisa no Estado de São Paulo (FAPESP, Grant # 08/03828-1 to MLN and Grant # 02/0946-1 to ARBR; CNPq, Grant # 302353/03-8 to RLDM) and the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES). MLN, PR, ARBR and RLDM are supported by a CNPq Fellowship.
Received in 19/01/2010
Accepted in 26/03/2010
- 1. Sistema de Vigilância em Saúde. Situação Epidemiológica da Malária no Brasil. Ministério da Saúde; 2008.
- 2. Figueiredo LTM. Emergent arboviruses in Brazil. Rev Soc Bras Med Trop 2007; 40:224-229.
- 3. Carme B, Matheus S, Donutil G, Raulin O, Nacher M, Morvan J. Concurrent Dengue and Malaria in Cayenne Hospital, French Guiana. Emerg Infect Dis 2009; 15:668-671.
- 4. Bhalla A, Sharma N, Sharma A, Suri V. Concurrent infection with Dengue and Malaria. Indian J Med Sci 2006; 60:330-331.
- 5. Chander J, Singla N, Singh R. Concurrent Presence of Dengue and Plasmodium falciparum Trop Med Health 2009; 37:69-70.
- 6. Charrel RN, Brouqui P, Foucault C, Lamballerie X. Concurrent Dengue and Malaria. Emerg Infect Dis 2007; 11:1153-1154.
- 7. Deresinski S. Concurrent Plasmodium vivax Malaria and Dengue. Emerg Infect Dis 2006; 12:1802-1803.
- 8. Kaushik RM, Varma A, Kaushik R, Gaur, KJBS. Concurrent dengue and malaria due to Plasmodium falciparum and P. vivax Trans R Soc Trop Med Hyg 2007; 101:1048-1050.
- 9. Tangaratham PS, Jeevan MK, Rajendran R, Samuel PP, Tyagi BK. Dual Infection by Dengue Virus and Plasmodium vivax in Alappuzha District, Kerala, India. Jpn J Infect Dis 2006; 59:211-212.
- 10. Ward DI. A case of fatal Plasmodium falciparum malaria complicated by acute dengue fever in East Timor. Am J Trop Med Hyg 2006; 75:182-185.
- 11. Vasconcelos PFC, Rosa APAT, Rosa JFST, Dégallier N. Concomitant Infections by Malaria and Arboviruses in the Brazilian Amazon Region. Rev Latinoam Microbiol 1990; 32:291-294.
- 12. Bronzoni RVM, Baleotti FG, Nogueira RMR, Nunes M, Figueiredo LTM. Duplex Reverse Transcription-PCR followed by Nested PCR assays for detection and identification of Brazilian Alphaviruses and Flaviviruses. J Clin Microbiol 2005; 43:696-702.
- 13. Morelli ML, Aquino VH, Cruz ACR, Figueiredo LTM. Diagnosis of Oropouche Virus Infection by RT-Nested-PCR. J Med Virol 2002; 66:139-142.
- 14. Rosa JFST, Rosa APAT, Vasconcelos PFC, Pinheiro FP, Rodrigues SG, Rosa EST, et al. Arboviruses isolated in the Evandro Chagas Institute, including some described for the first time in the Brazilian Amazon region, their known hosts and their pathology for man. In: Rosa APAT, Vasconcelos PFC, Rosa JFST, editors. An overview of arbovirology in Brazil and neighboring countries. Instituto Evandro Chagas, Belém; 1998. p. 19-31.
- 15. Tadei WP, Thatcher BD, Santos JMM, Scarpassa VM, Rodrigues IB, Rafael MS. Ecologic observations on anopheline vectors of malaria in the Brazilian Amazon. Am J Trop Med Hyg 1998; 59:325-335.
- 16. Tadei WP, Thatcher BD. Malaria vectors in the Brazilian Amazon. Anopheles of the subgenus Nyssorhynchus (1). Rev Inst Med Trop Sao Paulo 2000; 42:87-94.
- 17. Vasconcelos PFC, Rosa APAT, Pinheiro FP, Shope RE, Rosa JFST, Rodrigues SG, et al. Arboviruses pathogenic for man in Brazil. In: Rosa APAT, Vasconcelos PFC, Rosa JFST, editors. An overview of arbovirology in Brazil and neighbouring countries. Instituto Evandro Chagas, Belém; 1998. p. 72-99.
- 18. Figueiredo LTM. The Brazilian flavivirus. Microbes Infect 2000; 2:1643-1649.
- 19. Singhsilarak T, Phongtananant S, Jenjittikul M, Watt G, Tangpakdee N, Popak N, et al. Possible acute coinfections in Thai malaria patients. Southeast Asian J Trop Med Public Health 2006; 37:1-4.
- 20. Penna G, Pinto LF, Soranz D, Glatt R. High Incidence of Diseases Endemic to the Amazon Region of Brazil, 2001-2006. Emerg Infect Dis 2009; 15: 626-632.
- 21. Sung V, O'Brien DP, Matchett E, Brown GV, Torresi J. Dengue fever in Travelers Returning from Southeast Asia. J Travel Med 2003; 10:208-213.
- 22. Alves FP, Durlacher RR, Menezes MJ, Krieger H, Silva LHP, Camargo EP. High prevalence of asymptomatic Plasmodium vivax and Plasmodium falciparum infections in native Amazonian populations. Am J Trop Med Hyg 2002; 66: 641-648.
- 23. Coura JR, Suarez-Mutis M, Ladeia-Andrade S. A new challenge for malaria control in Brazil: asymptomatic Plasmodium infection -a review. Mem Inst Oswaldo Cruz 2006; 101: 229-237.
- 24. Gunewardena DM, Carter R, Mendis KN. Patterns of acquired anti-malarial immunity in Sri Lanka. Mem Inst Oswaldo Cruz 1994; 89:63-65.
- 25. McKenzie FE, Smith DL, O'Meara WP, Forney JR, Magil AJ, Permpanich B, Erhart LM, Sirichaisinthop J, Wongsrichanalai C, Gasser Jr RA. Fever in patients with mixed-species malaria. Clin Infect Dis 2006; 42: 1713-1718.
- 26. Abbasi A, Butt N, Sheikh QH, Bhutto AR, Munir SM, Ahmed SM. Clinical Features, Diagnostic Techniques and Management of Dual Dengue and Malaria Infection. J Coll Physicians Surg Pak 2009; 19:25-29.
Address to:
Publication Dates
-
Publication in this collection
05 Nov 2010 -
Date of issue
Oct 2010
History
-
Accepted
26 Mar 2010 -
Received
19 Jan 2010