Abstracts
Lymphogranuloma venereum (LGV) is an uncommon, contagious, sexually transmitted disease (STD). We report a case of a 17-year-old teenager who presented with a 2-month-old ulcerous vegetant lesion in the right inguinal region. The patient was diagnosed with LGV and received erythromycin treatment. Three months after treatment, he presented with a new ulcerous lesion, very similar to the previous one, in the right supraclavicular region. He was diagnosed with a diffuse large B-cell non-Hodgkin lymphoma. Both diseases are rare in Rio de Janeiro City, Brazil, and physicians should not neglect the possibility of STDs in such cases.
Lymphogranuloma venereum; Non-Hodgkin lymphoma; STD
Linfogranuloma venéreo (LGV) é uma doença sexualmente transmissível e de ocorrência pouco frequente. Relatamos um caso de um adolescente com 17 anos de idade que apresentou uma lesão ulcerativa vegetante a cerca de dois meses na região inguinal direita. Foi diagnosticado como LGV e o paciente foi tratado com eritromicina. Três meses após o tratamento o paciente apresentou uma nova lesão ulcerativa, muito semelhante à anterior, na região supraclavicular direita. O diagnóstico desta lesão foi de linfoma difuso de células B do tipo não-Hodgkin. Ambas as patologias não são comuns na Cidade do Rio de Janeiro, Brasil e um médico não deve negligenciar a possibilidade da ocorrência de uma doença sexualmente transmissível (DST).
Linfogranuloma venéreo; Linfoma não Hodgkin; DST
CASE REPORT RELATO DE CASO
Lymphogranuloma venereum and non-Hodgkin lymphoma: a case report
Linfogranuloma venéreo e linfoma não Hodgkin: um relato de caso
Mauro Romero Leal PassosI; Wilma Nancy Campos ArzeI; Felipe Dinau Leal PassosII; Priscilla Frauches Madureira de FariaIII; Renata Queiroz VarellaIII; Mariana Dinau Leal PassosIV; Dennis de Carvalho FerreiraI,V
ISetor de Doenças Sexualmente Transmissíveis, Universidade Federal Fluminense, Niterói, RJ
IIFaculdade de Biologia, Universidade Santa Úrsula, Rio de Janeiro, RJ
IIIFaculdade de Medicina, Universidade Federal Fluminense, Niterói, RJ
IVFaculdade de Medicina, Universidade Estácio de Sá, Rio de Janeiro, RJ
VDepartamento de Microbiologia Médica, Instituto de Microbiologia Paulo de Góes, Universidade Federal do Rio de Janeiro, Rio de Janeiro, RJ
Address to Address to: Dr. Mauro Romero Leal Passos Setor de DST/UFF. Outeiro São João Batista s/nº, Campus do Valonguinho Centro, 24210-150 Niterói, RJ, Brasil e-mail: mauroromerodst@hotmail.com; maurodst@gmail.com
ABSTRACT
Lymphogranuloma venereum (LGV) is an uncommon, contagious, sexually transmitted disease (STD). We report a case of a 17-year-old teenager who presented with a 2-month-old ulcerous vegetant lesion in the right inguinal region. The patient was diagnosed with LGV and received erythromycin treatment. Three months after treatment, he presented with a new ulcerous lesion, very similar to the previous one, in the right supraclavicular region. He was diagnosed with a diffuse large B-cell non-Hodgkin lymphoma. Both diseases are rare in Rio de Janeiro City, Brazil, and physicians should not neglect the possibility of STDs in such cases.
Keywords: Lymphogranuloma venereum. Non-Hodgkin lymphoma. STD.
RESUMO
Linfogranuloma venéreo (LGV) é uma doença sexualmente transmissível e de ocorrência pouco frequente. Relatamos um caso de um adolescente com 17 anos de idade que apresentou uma lesão ulcerativa vegetante a cerca de dois meses na região inguinal direita. Foi diagnosticado como LGV e o paciente foi tratado com eritromicina. Três meses após o tratamento o paciente apresentou uma nova lesão ulcerativa, muito semelhante à anterior, na região supraclavicular direita. O diagnóstico desta lesão foi de linfoma difuso de células B do tipo não-Hodgkin. Ambas as patologias não são comuns na Cidade do Rio de Janeiro, Brasil e um médico não deve negligenciar a possibilidade da ocorrência de uma doença sexualmente transmissível (DST).
Palavras-chaves: Linfogranuloma venéreo. Linfoma não Hodgkin. DST.
INTRODUCTION
Venereal lymphogranuloma (LGV), also known as Nicolas-Favre-Durand disease, is a contagious, systemic, sexually transmitted disease (STD) that is caused by Chlamydia trachomatis L1, L2, and L3 serovars. It is rare in industrialized countries, and has been found more frequently in underdeveloped countries. In such countries, it has been reported that members of the lower social and economic classes who indulge in promiscuous sexual relations frequently become infected13. However, in recent years there has been a greater occurrence of LGV in Europe, North America, and Australia, mainly among male homosexuals, and predominately those co-infected with the human immunodeficiency virus (HIV)4. Its incidence is higher in men, especially those aged between 20-30 years.
Venereal lymphogranuloma is a chronic disease with late and acute symptoms1,5,6. Rectal involvement is rare in LGV, but the pararectal lymph nodes can get affected in the chronic stage, causing rectal stenosis. In the genitals, the disease can evolve to esthiomene (i.e., elephantiasis with fistula and ulcer)3,7,8.
The disease can be clinically diagnosed by the identification of C. trachomatis at the infection site with enzyme-linked immunosorbent assay (ELISA), immunofluorescence, polymerase chain reaction (PCR), or serology9. Differential diagnoses should mainly consider chancroid and primary syphilis in an early stage. In the bubo stage, ganglionar/vulvar tuberculosis, cat-scratch disease, paracoccidioidomycosis, and Hodgkin disease should be considered810.
Venereal lymphogranuloma is not a common disease, and physicians are not familiar with its signs and symptoms; therefore, its recognition and the differential diagnosis of neoplastic diseases are confounding11.
CASE REPORT
The patient was a 17-year-old male high school student from São Gonçalo City (municipality of the State of Rio de Janeiro, at a distance of 25 km from the capital; 22º49'37"S, 43º03'14"W; altitude, 19m), Rio de Janeiro, Brazil. He was single, heterosexual, and had only 1 sexual partner. He became sexually active at 14 years of age and did not use condoms. After consultation at a general clinic of a public hospital, he was transferred to the STD Division of the Federal Fluminense University due to the presence of a 2-month-old unilateral inguinal painless lesion. The patient described the initial sign as a small papule draining a purulent liquid, which evolved into an ulcerated node. He reported general discomfort from 1 week before his examination at the STD clinic. During the examination, a 10-cm ulcerated tumor with raised surfaces in the right inguinal region and necrotic areas was observed (Figure 1).
The following laboratory tests were carried out at the STD Division: serology tests for Chlamydia trachomatis, which showed reactivity at 1:32; smear cytopathology tests of the inguinal lesion, were inconclusive morphology for malignancy; venereal disease research laboratory (VDRL) test, which showed non-reactivity; and anti-HIV test, which showed non-reactivity.
From the clinical laboratory data, LGV was diagnosed, and the treatment recommended was oral erythromycin (500 mg, 6/6 h, for 21 days).
A complete regression of the clinical symptoms occurred after the treatment. It should be observed that the symptoms started to decline rapidly during the antibiotic therapy.
Three months after the first examination, the patient returned to the STD Division with a new ulcerous lesion, similar to the first one, in the right supraclavicular region. The patient reported a right clavicular fracture due to a fall 70 days earlier, which caused pain and local edema. Thoracic X-rays showed a lytic lesion in the right clavicle and a morphostructural alteration of an insufflated lesion with dense soft tissue.
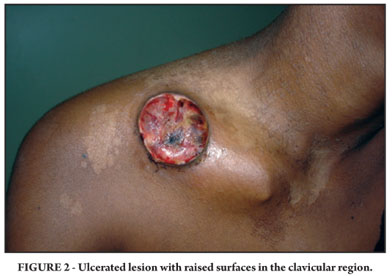
A physical examination showed a 5-cm ulcerous lesion in the clavicular region with raised surfaces, a vegetant bottom layer, purulent secretion, and painless to touch (Figure 2). The inguinogenital region had no lesion and showed complete cicatrization.
Considering this new lesion, the hypothesis of systemic disease was reinforced. Therefore, the patient was sent to the Instituto Nacional do Câncer (INCA; National Cancer Institute), in the City of Rio de Janeiro, for clinical investigation and monitoring.
The following tests were performed at the INCA: thoracic computer tomography (CT) scan revealed a bone lesion in the right clavicle, i.e., a small node with the density of soft tissue in the lung periphery of the right superior lobe (sarcoma). Normal results were obtained in the pelvic and abdominal CT scans. Bone scintigraphy performed at 2 h after the intravenous administration of 99mTc-MDP revealed hyperfixation of the radioisotope during full extension of the right clavicle, in the sixth costovertebral articulation, and with regular distribution in the remaining skeleton. Negative serological results were obtained for hepatitis viruses A, B, and C. Negative results were obtained for anti-human T lymphotropic virus type 1 and anti-HIV. The right shoulder X-rays showed an important lytic insufflating lesion in the right clavicle. The laboratory results were as follows: glutamic oxaloacetic transaminase level, 16mg/dL; beta 2-microglobulin level, 2.24; alkaline phosphatase level, 120g/dL; lactate dehydrogenase level, 260; gamma-T level, 46. No alterations were observed in the total bilirubin levels or in the results for the hemogram and clinical urine tests. Incisional biopsy of the right clavicle revealed granulomatous tissue without malignancy; bone marrow biopsy showed 70% cellularity, represented by elements for which serovars showed maturation; and incisional biopsy of the ulcerous vegetant supraclavicular wound revealed a high-grade non-Hodgkin lymphoma. Immunohistochemical analysis showed diffuse non-Hodgkin lymphoma of large B-cells.
Chemotherapy was the treatment of choice after the diagnosis was confirmed, and the patient is now being monitored after completion of chemotherapy.
DISCUSSION
The incidence of LGV worldwide reduced considerably after antibiotics were discovered12. However, there are studies showing that there is a resurgence of LGV, mainly in the homosexual male population4,7,12. Patients practicing anal sex could develop proctitis or proctocolitis because of the direct implantation of the bacteria in the anal-rectal mucosa.
The importance of this report is due to the rarity of the pathological features and the challenge of its diagnosis. Although B-cell extracutaneous lymphomas are generally more common than T-cell extracutaneous lymphomas, the opposite finding is observed in the skin, where T-cell lymphomas are more common. B-cell cutaneous lymphomas show a discrete prevalence in males, with the main incidence at ~59 years of age; therefore, its occurrence in this young patient shows the rarity of this case.
Despite the clinical evidence, confirmation of the diagnosis is always important to distinguish it from other pathologies with similar characteristics, e.g., cutaneous tuberculosis, paracoccidioidomycosis, Jessner lymphocytic infiltrate, insect sting, tegumentary leishmaniasis, drug eruption (e.g., diphenylhydantoin, salicylates, nitrofurantoin, and cyclosporine) and lymphocytoma cutis9,11.
There were several similarities between the first lesion described and treated as LGV (inguinal lesion) and the second lesion (clavicular), and although there was a rapid regression with the specific treatment for LGV, it should be observed that a B-cell cutaneous lymphoma can also regress or recur. It is unknown whether the 2 lesions had the same cause, since no biopsy was carried out on the inguinal lesion, and only cytological analysis was performed, which showed no malignancy.
We would also like to report another case examined by the authors in the same STD clinic. The patient was from the State of São Paulo and presented with a large inguinal mass (bubo); doxycycline and tetracycline had been previously administered, with no results. In this case, paracoccidioidomycosis was the final diagnosis11.
In the presence of a patient with any inguinogenital lesion, the physician should consider that many systemic diseases show localized symptoms, suggesting classic STD. Conversely, concomitant STD with other contagious or non-contagious diseases is not an uncommon observation.
FINANCIAL SUPPORT
Felipe Dinau Leal Passos has a scholarship from the Fundação Oswaldo Cruz (FIOCRUZ), Rio de Janeiro, Brazil.
Received in 02/03/2011
Accepted in 03/11/2011
- 1. Mabey D, Peeling RW. Lymphogranuloma venereum. Sex Transm Infect 2002; 78:90-92.
- 2. Simms I, Ward H, Martin I, Alexander S, Ison C. Lymphogranuloma venereum in Australia. Sex Health 2006; 3:131-133.
- 3. Collins L, White JA, Bradbeer C. Lymphogranuloma venereum. BMJ 2006; 332:366.
- 4. Van de Laar M. The emergence of LGV in Western Europe: what do we know, what can we do? Euro Surveill 2006; 11:146-148.
- 5. McLean CA, Stoner BP, Workowski KA. Treatment of lymphogranuloma venereum. Clin Infect Dis 2007; 44: (suppl 3):147-152.
- 6. Vall-Mayans M, Noguer I. Brotes de linfogranuloma venéreo entre hombres homosexuales em Europa, 2003-2004. Enferm Infecc Microbiol Clin 2006; 24:137-138.
- 7. Azulay RD. Linfogranuloma venéreo (doença de Nicolas Favre). Dermatologia. Rio de Janeiro: Guanabara Koogan; 2008.
- 8. Passos MRL. Linfogranuloma venéreo. In: Editor. Deessetologia, editor. DST 5. Rio de Janeiro: Cultura Médica; 2005. p. 299-303.
- 9. Passos MRL, Almeida G. Atlas de DST e diagnóstico diferencial. Revinter: Rio de Janeiro; 2002.
- 10. Van de Laar M, Fenton K, Ison C, European Surveillance of Sexually Transmitted Infections (ESSTI). Update on the European lymphogranuloma venereum epidemic among men who have sex with men. Euro Surveill 2005; 10:E050602.1.
- 11. Passos MRL, Martins ECS, Barreto NA, Pinheiro VMS, Varella RQ. Diagnóstico diferencial em DST: adenopatia inguinal. J Bras Doenças Sex Transm 1999; 11:34-35.
- 12. Nieuwenhuis RF. Ossewaarde JM, Götz HM, Dees J, Thio HB, Thomeer MG, e t al. Resurgence of lymphogranuloma venereum in Western Europe: An outbreak of Chlamydia trachomatis serovar L2 proctitis in the Netherlands among men who have sex with men. Clin Inf Dis 2004; 39:996-1003.
Publication Dates
-
Publication in this collection
27 June 2012 -
Date of issue
June 2012
History
-
Received
02 Mar 2011 -
Accepted
03 Nov 2011