Abstract
INTRODUCTION
Infrared imaging (IR) is a noninvasive technique that quantifies body surface temperature, producing a digital color image. IR has been used to study diseases in which skin temperature can reflect the presence of inflammation.
METHODS
This was an observational pilot study of eight patients envenomed by snakes, spiders, and scorpions. All patients were examined using a thermal camera.
RESULTS
In all cases, we obtained infrared images that corroborated clinical findings indicating localized effects of venom, specifically inflammation.
CONCLUSIONS
IR has potential for use as a research, diagnostic, and monitoring tool for localized effects of animal venoms.
Keywords:
Infrared thermography; Envenomation; Venomous animals
Infrared imaging (IR) is a noninvasive technique that quantifies body surface temperature by capturing the thermal radiation emitted and producing a high-resolution digital image called a thermogram11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35.. The information is made visible via a color scale where the warmest areas are depicted as white or red, while the coolest areas appear blue or black22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46.. IR has been used to study diseases in which skin temperature can reflect the presence of inflammation in underlying tissues, or those in which blood flow is increased or decreased because of a clinical abnormality11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35.,22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46..
It is widely known that animal venoms are capable of inducing localized reactions involving inflammation and pain33. Farsky SH, Antunes E, Mello SB. Pro and anti-inflammatory properties of toxins from animal venoms. Curr Drug Targets Inflamm Allergy. 2005;4(3):401-11.. One of the challenges that clinicians face when treating patients envenomed by venomous animals is a lack of suitable clinical tools for accurate assessment of the localized effects caused by different venoms in order to provide refined criteria for choosing the best therapeutic option, especially the most efficacious use of antivenom. IR has great potential for use as such a clinical tool because it is a non-invasive method that has no biological side effects, requires no sedation or anesthesia, and can be repeated as desired for follow-ups11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35. 22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46.. To the best of our knowledge, no study has investigated the use of IR with high-resolution thermograms for assessing the local effects of envenomation by venomous animals. The aim of this observational pilot study was to evaluate the feasibility of this new potential clinical application of IR for the diagnosis and management of venomous animal bites and stings.
Eight patients envenomed by snakes (three cases), spiders (three cases), and scorpions (two cases) were studied. The study sample represents a convenience sample where a research investigator was present and the equipment was available. Only cases in which the causative animal was identified (Laboratório Especial de Coleções Zoológicas, Instituto Butantan, São Paulo, Brazil) were included.
Infrared imaging examinations were conducted in compliance with international recommendations22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46. by using a FLIR T650sc camera (FLIR Systems AB, Taby, Sweden). This infrared system has an image resolution of 640×480 pixels and thermal sensitivity of <20mK at 30ºC. The camera produced quantitative and qualitative temperature maps of surface temperature (thermograms), and results were analyzed using the rainbow palette, with white/red as hot and blue/black as cold. Image acquisition and storage was carried out with the Flir Tools® software (V 5.3.15320.1002, 2015, FLIR Systems AB, Danderyd, Sweden). Emissivity of the skin was assumed to be 0.98±0.0122. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46.. Before thermographic measurements were obtained, patients spent 15 minutes in an acclimatization room within a temperature-controlled environment (23°C), which allows the measurement of skin temperature variations within a range of 0.05-0.1ºC from the affected region to the surrounding body region, or the contralateral region of the body22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46..
Once the qualitative thermal images were captured, we outlined regions of interest (ROI) according to anatomical references by using the polygon drawing tool embedded in the camera software with the intention of comparing the quantitative data of the affected areas with those of normal or contralateral areas44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55.. Thermal data of each ROI (ellipses or circles) were calculated as the arithmetic mean of the temperature values of all the pixels inside the ROI44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55.. Using these data, we could quantitatively evaluate temperature asymmetries (ΔT values) between areas affected by venom and the surrounding body region, or the corresponding area on the opposite side of the body44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55..
The physiological foundation for using IR in medicine resides in the fact that the skin temperature distribution of the human body depends on complex relationships that define heat exchange processes between local vasculature, metabolic activity, skin tissue, inner tissues, and the regulation of sympathetic and parasympathetic activity in the maintenance of homeostasis55. Merla A, Romani GL. Functional infrared imaging in medicine: a quantitative diagnostic approch. Conf Proc IEEE Eng Med Biol Soc. 2006;1:224-7. ID: 17946387.. The presence of a disease interferes locally with the heat balance, resulting in an increase or decrease of skin temperature, with respect to the surrounding regions or the unaffected contralateral region. A diagnostic approach based on infrared imagery consists of searching for hyper-radiation or hypo-radiation areas and/or asymmetric thermal patterns in contralateral regions44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55.,55. Merla A, Romani GL. Functional infrared imaging in medicine: a quantitative diagnostic approch. Conf Proc IEEE Eng Med Biol Soc. 2006;1:224-7. ID: 17946387.. A degree of thermal asymmetry between opposite sides of the body (ΔT) up to 1ºC has been considered indicative of dysfunction44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55..
Snakebites
We studied three cases of snake bites (Figures 1A, B, C, D, E, F, G, H and I). IR performed on the patient bitten by Bothrops moojeni (case 1) showed significant asymmetry between the temperatures observed in both the bitten and the healthy upper limbs (Figure 1C). The temperature increase observed in the bitten limb provides an image of the extent of the inflammatory process attributed to the localized venom inoculation. It is well known that Bothrops snake venom elicits, among other alterations, a pronounced local inflammatory response66. Teixeira C, Cury Y, Moreira V, Picolob G, Chaves F. Inflammation induced by Bothrops asper venom. Toxicon. 2009;54(1):67-76..
Snakebites. Case 1: A 28-year-old man was bitten on his right middle finger by a lance-headed viper identified as Bothrops moojeni (A) 15 minutes prior to arrival at the hospital. Erythema, marked edema, and two fang marks could be observed at the bite site (B). Infrared imaging (IR) conducted one day after the snakebite showed a significant asymmetry between the temperatures observed in both the bitten and the healthy upper limbs (ΔT=1.8ºC) (C). Case 2: A 28-year-old healthy man was bitten by a rattlesnake (Crotalus durissus terrificus) (D) on his right index finger an hour and a half prior to arriving at the hospital. On arrival, he reported mild pain at the bite site, generalized myalgia, and visual impairment. He had a small erythematous lesion on his right index finger without swelling, (E) and pronounced ptosis. The IR conducted ten hours after the snakebite showed a significant temperature rise at the bite site, as confirmed by the difference between the temperatures of the fingertips of the index and little fingers (ΔT=3.6ºC) (F). Case 3: A 27-years-old woman was bitten on her left fourth toe by a lance-headed viper identified as Bothrops jararaca (G) about two hours prior to admission to the hospital. On arrival, she reported only pain at the bite site, with two localized fang marks, but without localized erythema, edema, ecchymosis, or systemic symptoms (H). Results of routine laboratory tests, including her coagulation profile, were normal. After 18 hours of observation, the patient showed no other symptoms, the diagnosis was considered to be dry bite, and she was discharged without the use of antivenom. The IR performed at admission showed no asymmetry between the temperatures observed in both lower limbs (ΔT=0 ºC) (I).
In case 2, we present a patient bitten by a rattlesnake on the right index finger (Figure 1E). A significant increase in temperature in the affected finger, extending throughout the palm, was noticeable (Figure 1F). Although clinical studies have demonstrated that Crotalus durissus venom does not induce a significant inflammatory reaction at the bite site77. Bucaretchi F, Herrera SRF, Hyslop S, Baracat ECE, Vieira RJ. Snakebites by Crotalus durissus ssp in children in Campinas, São Paulo, Brazil. Rev Inst Med Trop São Paulo. 2002;44(3):133-8., the local inflammatory process detected by thermography is in agreement with the findings of Toyama et al., who observed that phospholipase A2 isolated from Crotalus durissus collilineatus venom markedly increased vascular permeability in rat skin88. Toyama DO, Marangoni S, Diz-Filho EB, Oliveira SC, Toyama MH. Effect of umbelliferone (7-hydroxycoumarin, 7-HOC) on the enzymatic, edematogenic and necrotic activities of secretory phospholipase A2 (sPLA2) isolated from Crotalus durissus collilineatus venom. Toxicon. 2009;53(4):417-26..
In case 3, we describe a patient who suffered a dry bite by Bothrops jararaca. The diagnosis of dry bite was only confirmed after several hours of observation and repeated laboratory tests, but there is still no consensus as to the observation time necessary for the diagnosis of non-envenomation. However, the IR performed on admission showed no thermal changes in the affected limb (Figure 1I). In a retrospective study of 792 patients bitten by Bothrops jararaca who were treated at the Hospital Vital Brazil, São Paulo, Brazil, Nicoleti et al. identified 117 (14,8%) cases of dry bite99. Nicoleti AF, Medeiros CR, Duarte MR, França FOS. Comparison of Bothropoides jararaca bites with and without envenoming treated at the Vital Brazil Hospital of the Butantan Institute, State of São Paulo, Brazil. Rev Soc Bras Med Trop. 2010;43(6):657-61.. In this study, the authors did not cite the observation time required for this diagnosis. Therefore, our results suggest the possibility of protocols that can be used to verify whether IR can present an alternative method for early diagnosis of dry bite.
Scorpion stings
Tityus serrulatus and Tityus bahiensis are among the main species of scorpions associated with envenomation in Brazil1010. Cupo P. Clinical update on scorpion envenoming. Rev Soc Bras Med Trop . 2015;48(6):64-9.. The venom of these scorpions contains neurotoxins that act mainly on ion channels (sodium and potassium voltage-gated channels), leading to intense and prolonged depolarization and neuronal excitation. This in turn induces the release of mediators such as acetylcholine, adrenaline, and noradrenaline, which are responsible for the onset of clinical manifestations1010. Cupo P. Clinical update on scorpion envenoming. Rev Soc Bras Med Trop . 2015;48(6):64-9.. Although systemic signs and symptoms such as cardiac arrhythmias and acute pulmonary edema can occur in cases of severe envenoming, 85-90% of cases are classified as mild, with only localized manifestations observed, particularly pain with variable intensity1010. Cupo P. Clinical update on scorpion envenoming. Rev Soc Bras Med Trop . 2015;48(6):64-9.. In addition, recent studies have shown that scorpion venom can induce the production of inflammatory mediators and inflammatory reactions1111. Petricevich VL. Scorpion venom and the inflammatory response. Mediators Inflamm. 2010;2010:903295..
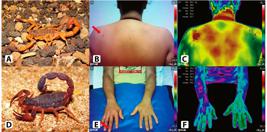
Herein, we present two cases of scorpion stings (Figures 2A, B, C, D, E and F). In both cases, the patients did not present systemic symptoms, referring mainly to pain at the bite site. In case 4, IR showed a significant temperature rise at the sting site, reflecting the localized action of the venom (Figure 2C). Infrared imaging has been used as a diagnostic and monitoring prognostic tool for pain in many clinical situations22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46.. Future studies may clarify whether IR can also be a useful tool for monitoring local manifestations of scorpion envenomation, mainly pain. This may be particularly important in pediatric patients stung by scorpions, where it is often difficult to assess pain intensity and response to treatment.
Scorpion stings. Case 4: A 16-year-old girl was stung by a scorpion identified as Tityus serrulatus (A) about two hours prior to admission to the hospital. Clinical examination on admission revealed a severe, localized, burning pain with a small area of erythema on the left scapular region (B). The infrared imaging (IR) performed on admission showed a significant temperature rise at the sting site (ΔT=1.5ºC) (C). Case 4: A 49-year-old man was admitted with a Tityus bahiensis (D) scorpion sting on his right middle finger one hour before admission. He complained of local pain radiating to the whole forearm. He had a small area of erythema on the distal phalanx of the affected finger (E). The IR performed on admission showed a region with decreased temperature extending from the sting site to the elbow (ΔT=-1.8ºC) (F).
In case 5, IR showed a region with decreased temperature extending from the sting site to the patient’s elbow (Figure 2F). What drew our attention in this case was the finding of decreased local temperature, unlike the increase seen in the previous case. A closer look revealed a thin layer sweat throughout this area, which justifies the heat loss by convection. Interestingly, the patient experienced referred pain radiating all the way to this area, where heat loss was observed. Obviously, further studies will be needed in order to define the real value of IR as a non-invasive method for the analysis of local manifestations and prognosis of scorpion stings.
Spider bites
We studied three cases of spider bites (Figures 3A, B, C, D, E, F, H and H). In case 6, IR showed a region with increased temperature, extending from the bite site to the knee (Figure 3C). Although the clinical examination showed only a small area with erythema involving the bite site, this patient had reported localized pain radiating out to his knee, which was compatible with the images obtained by IR. Experimental studies have indicated that the intense localized pain reported after most Phoneutria nigriventer bites involves peripheral (tachykinin NK1 and NK2, and glutamate receptors) and central (spinal) mechanisms (neurokinins, excitatory amino acids, NO, proinflammatory cytokines, and prostanoids), which all probably act synergistically1212. Zanchet EM, Longo I, Cury Y. Involvement of spinal neurokinins, excitatory amino acids, proinflammatory cytokines, nitric oxide and prostanoids in pain facilitation induced by Phoneutria nigriventer spider venom. Brain Res. 2004;1021(1):101-11.. These mechanisms may explain the thermal alterations observed in IR, which showed a region with increased temperature extending from the bite site to the knee (Figure 3C). Similar to IR use in scorpion stings, the utility of IR as a tool for prognosis and monitoring of local manifestations of armed spider envenomation, mainly pain, may be clarified in future studies.
Spider bites. Case 6: A 56-year-old man was admitted to our hospital two hours and a half after being bitten on his right hallux by a Brazilian wandering spider identified as Phoneutria nigriventer (A). Clinical examination showed local severe burning pain radiating to the knee and a small area with erythema involving his right hallux (B). The infrared imaging (IR) performed on admission showed a region with increased temperature extending from the bite site to the knee (ΔT=7.4ºC) (C). Case 7: A 71-year-old woman was bitten on her neck by a brown spider identified as Loxosceles gaucho (D). She visited the hospital about 19 hours after being bitten. She presented with an erythematous area of 4×2cm in the right cervical region (E). There was no local necrosis. The IR performed on admission showed a significant increase in temperature at the bite region (ΔT=2.2ºC) (F). Case 8: A 32-year-old man visited the hospital three days after being bitten by a brown spider (Loxosceles sp) on his right popliteal region. Clinical examination showed an erythematous area of approximately 8×4 cm with a central brownish-crimson area of 5×6 cm with thin dark blisters (G). After 21 days of evolution, the wound had become a well-defined ulcer (H). The IR carried out at this time (I) showed significant asymmetry between the temperatures observed in both lower limbs (ΔT=1.2ºC). In the affected leg, a central area with decreased temperature was observed, corresponding to the necrotic wound.
Loxoscelism is caused by Loxosceles spp., and the cutaneous form manifests as pain and erythema that can develop into a necrotic ulcer1313. Isbister GK, Fan HW. Spider bite. Lancet. 2011;378(9808):2039-47.. The pathogenesis of this lesion involves a complex inflammatory response including the release of pro-inflammatory cytokines and lipid mediators1414. Gremski LH, Trevisan-Silva D, Ferrer VP, Matsubara FH, Meissner GO, Wille AC, et al. Recent advances in the understanding of brown spider venoms: From the biology of spiders to the molecular mechanisms of toxins. Toxicon. 2014;83:91-120.. We performed IR in two patients bitten by brown spiders, with both patients experiencing only cutaneous manifestations (cases 7 and 8), but in different stages of evolution. None of these patients presented clinical signs of systemic loxoscelism, which is characterized by intravascular hemolysis and renal failure1313. Isbister GK, Fan HW. Spider bite. Lancet. 2011;378(9808):2039-47..
In case 7, the patient was seen at the beginning of the initial skin changes attributed to local venom inoculation, still without evident necrosis (Figure 3E). IR showed a significant increase in temperature at the bite site, providing an image of the extent of the local inflammatory process (Figure 3F). In case 8, the marble plaque observed on admission (Figure 3G) developed into a well-defined ulcer that we observed after 21 days of evolution (Figure 3H). The IR performed at this time showed a region with increased temperature, denoting a local inflammatory process, and a colder central area corresponding to the necrotic area (Figure 3I). This temperature decrease can be attributed to the impairment of the local microcirculation.
Some important questions to be answered are whether the use of IR in the early stages of cutaneous loxoscelism could predict the formation of necrosis or its extension, and whether the thermographic monitoring of necrotic ulcers could have some utility in monitoring the healing process. Thermography has been used with some success in preventing foot ulcers11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35., preventing the formation of venous ulcers in patients with chronic venous disease11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35., and in assessing the depth of burns11. Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35. 22. Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46. 44. Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55.. In a study of 35 patients with pressure ulcers, Nakagami et al. concluded that using thermography to classify pressure ulcers according to temperature could be a useful predictor of healing at 3 weeks1515. Nakagami G, Sanada H, Iizaka S, Kadono T, Higashino T, Koyanagi H, et al. Predicting delayed pressure ulcer healing using thermography: a prospective cohort study. J Wound Care. 2010;19(11):465-6..
Obviously, further studies are needed to define the real value of IR in patients bitten by Loxosceles. We intend to advance this line of research because we believe that the use of IR to monitor the onset and healing of ulcers could provide a valuable tool in the analysis of indications for antivenom administration and the timing of administration, which remains a controversial issue1313. Isbister GK, Fan HW. Spider bite. Lancet. 2011;378(9808):2039-47. 1414. Gremski LH, Trevisan-Silva D, Ferrer VP, Matsubara FH, Meissner GO, Wille AC, et al. Recent advances in the understanding of brown spider venoms: From the biology of spiders to the molecular mechanisms of toxins. Toxicon. 2014;83:91-120..
In conclusion, although this was a pilot study that analyzed a small group of patients, and a large sample size would be required to extract definitive conclusions, it can be affirmed that IR has great potential for use as a diagnostic, monitoring, and research tool for evaluating the effects of localized envenomation by venomous animals.
Ethical considerations
This project was approved by the Ethics and Research Committee of Universidade Anhanguera de São Paulo (UNIAN), São Paulo, SP, Brazil, (number: 55382416.8.0000.5493), and all patients signed a consent form for the conduct of IR examinations and the publication of images. Full details of the IR were specified in this consent form.
Acknowledgments
We wish to thank Giuseppe Puorto and Rafael P. Indicatti for having kindly provided the photos of the animals.
REFERENCES
-
1Lahiri BB, Bagavathiappan S, Jayakumar T, Philip J. Medical applications of infrared thermography: a review. Infrared Phys Technol. 2012;55(4):221-35.
-
2Ring EF, Ammer K. Infrared thermal imaging in medicine. Physiol Meas. 2012;33(3):R33-46.
-
3Farsky SH, Antunes E, Mello SB. Pro and anti-inflammatory properties of toxins from animal venoms. Curr Drug Targets Inflamm Allergy. 2005;4(3):401-11.
-
4Fernández-Cuevas I, Bouzas Marins JC, Arnáiz-Lastras J, Gómez Carmona PM, Piñonosa Cano S, García-Concepción MA, et al. Classification of factors influencing the use of infrared thermography in humans: a review. Infrared Phys Technol . 2015;71:28-55.
-
5Merla A, Romani GL. Functional infrared imaging in medicine: a quantitative diagnostic approch. Conf Proc IEEE Eng Med Biol Soc. 2006;1:224-7. ID: 17946387.
-
6Teixeira C, Cury Y, Moreira V, Picolob G, Chaves F. Inflammation induced by Bothrops asper venom. Toxicon. 2009;54(1):67-76.
-
7Bucaretchi F, Herrera SRF, Hyslop S, Baracat ECE, Vieira RJ. Snakebites by Crotalus durissus ssp in children in Campinas, São Paulo, Brazil. Rev Inst Med Trop São Paulo. 2002;44(3):133-8.
-
8Toyama DO, Marangoni S, Diz-Filho EB, Oliveira SC, Toyama MH. Effect of umbelliferone (7-hydroxycoumarin, 7-HOC) on the enzymatic, edematogenic and necrotic activities of secretory phospholipase A2 (sPLA2) isolated from Crotalus durissus collilineatus venom. Toxicon. 2009;53(4):417-26.
-
9Nicoleti AF, Medeiros CR, Duarte MR, França FOS. Comparison of Bothropoides jararaca bites with and without envenoming treated at the Vital Brazil Hospital of the Butantan Institute, State of São Paulo, Brazil. Rev Soc Bras Med Trop. 2010;43(6):657-61.
-
10Cupo P. Clinical update on scorpion envenoming. Rev Soc Bras Med Trop . 2015;48(6):64-9.
-
11Petricevich VL. Scorpion venom and the inflammatory response. Mediators Inflamm. 2010;2010:903295.
-
12Zanchet EM, Longo I, Cury Y. Involvement of spinal neurokinins, excitatory amino acids, proinflammatory cytokines, nitric oxide and prostanoids in pain facilitation induced by Phoneutria nigriventer spider venom. Brain Res. 2004;1021(1):101-11.
-
13Isbister GK, Fan HW. Spider bite. Lancet. 2011;378(9808):2039-47.
-
14Gremski LH, Trevisan-Silva D, Ferrer VP, Matsubara FH, Meissner GO, Wille AC, et al. Recent advances in the understanding of brown spider venoms: From the biology of spiders to the molecular mechanisms of toxins. Toxicon. 2014;83:91-120.
-
15Nakagami G, Sanada H, Iizaka S, Kadono T, Higashino T, Koyanagi H, et al. Predicting delayed pressure ulcer healing using thermography: a prospective cohort study. J Wound Care. 2010;19(11):465-6.
Publication Dates
-
Publication in this collection
Mar-Apr 2017
History
-
Received
20 Sept 2016 -
Accepted
06 Dec 2016