Abstract
OBJECTIVE: To use published Hypertension Optimal Treatment (HOT) Study data to evaluate changes in cardiovascular mortality in nondiabetic hypertensive patients according to the degree of reduction in their diastolic blood pressure. METHODS: In the HOT Study, 18,700 patients from various centers were allocated at random to groups having different objectives of for diastolic blood pressure: <=90 (n=6264); <=85 (n=6264); <=80mmHg (n=6262). Felodipine was the basic drug used. Other antihypertensive drugs were administered in a sequential manner, aiming at the objectives of diastolic blood pressure reduction. RESULTS: The group of nondiabetic hypertensive subjects with diastolic pressure<=80mmHg had a cardiovascular mortality ratio of 4.1/1000 patients/year, 35.5% higher than the group with diastolic pressure <=90mmHg (cardiovascular mortality ratio, 3.1/1000 patients/year). In contrast, diabetic patients allocated to the diastolic pressure objective group of <=80mmHg had a 66.7% reduction in cardiovascular mortality (3.7/1000 patients/year) when compared with the diastolic pressure group of <=90mmHg (cardiovascular mortality ratio, 11.1/1000 patients/year). CONCLUSION: The results indicate that in hypertensive diabetic patients reduction in diastolic blood pressure to levels <=80mmHg decreases the risk of fatal cardiovascular events. It remains necessary to define the level of diastolic blood pressure <=90mmHg at which maximal reduction in cardiovascular mortality is obtained for nondiabetics.
arterial hypertension; HOT Study; diabetes mellitus
Original Article
Reduction in Diastolic Blood Pressure and Cardiovascular Mortality in Nondiabetic Hypertensive Patients. A Reanalysis of the HOT Study
Antonio Alberto Lopes, Jadelson Andrade, Antonio Carlos Beisl Noblat, Marco Antonio Silveira
Salvador, BA - Brazil
OBJECTIVE: To use published Hypertension Optimal Treatment (HOT) Study data to evaluate changes in cardiovascular mortality in nondiabetic hypertensive patients according to the degree of reduction in their diastolic blood pressure.
METHODS: In the HOT Study, 18,700 patients from various centers were allocated at random to groups having different objectives of for diastolic blood pressure: £90 (n=6264); £85 (n=6264); £80mmHg (n=6262). Felodipine was the basic drug used. Other antihypertensive drugs were administered in a sequential manner, aiming at the objectives of diastolic blood pressure reduction.
RESULTS: The group of nondiabetic hypertensive subjects with diastolic pressure £80mmHg had a cardiovascular mortality ratio of 4.1/1000 patients/year, 35.5% higher than the group with diastolic pressure £90mmHg (cardiovascular mortality ratio, 3.1/1000 patients/year). In contrast, diabetic patients allocated to the diastolic pressure objective group of £80mmHg had a 66.7% reduction in cardiovascular mortality (3.7/1000 patients/year) when compared with the diastolic pressure group of £90mmHg (cardiovascular mortality ratio, 11.1/1000 patients/year).
CONCLUSION: The results indicate that in hypertensive diabetic patients reduction in diastolic blood pressure to levels £80mmHg decreases the risk of fatal cardiovascular events. It remains necessary to define the level of diastolic blood pressure £90mmHg at which maximal reduction in cardiovascular mortality is obtained for nondiabetics.
Key words - arterial hypertension, HOT Study, diabetes mellitus
Hypertension is an important risk factor in fatal cardiovascular events 1. Furthermore, the difference in risk of these events in patients with or without hypertension has not been fully eliminated by antihypertensive treatment 2. A possible explanation for this finding is that hypertensive patients, in general, have not been maintained under adequate control 3,4. It is not easy, however, to define what is meant by "adequate control" of arterial pressure in hypertensive subjects. In addition, the concern exists that in certain patients a reduction below certain limits raises the risk of complications, in particular ischemic events in the heart 5,6. The need to determine to which level arterial pressure in a hypertensive patients should be lowered to obtain maximal reduction in unfavorable events was one of the reasons for the development of the Hypertension Optimal Treatment (HOT) Study 7. This study showed evidence of benefits acquired by a more accentuated reduction in diastolic blood pressure in diabetic hypertensive patients in regards to major cardiovascular events and cardiovascular mortality. However, the publication of the HOT Study findings did not include nondiabetic patients. We, therefore, decided to evaluate the cardiovascular mortality trends in this group, in terms of the level of diastolic blood pressure reduction goal.
Methods
Details of the HOT study have been described 7,8. In our study, hypertensive patients were randomly allocated to different groups with differing goals for diastolic blood pressure: £90, £85, £80mmHg. The basic drug used was felodipine, initiated at 5mg, titrated up to 10mg. When necessary, low doses of angiotensin converting enzyme inhibitors, or beta-blockers followed by hydrochlorothiazide, were additionally administered in a sequential manner. Patient ages ranged between 50 and 80 years, averaging 61.5 years. Hypertensive patients were allocated as follows into the 3 study groups: <90mmHg, 6264 patients; <85mmHg, 6264 patients; <80mmHg, 6262 patients. Approximately 8% of the patients had diabetes mellitus.
Estimated values used in the present reanalysis were based on data presented in tables in one of the HOT study publications 7. The number of fatal cases due to cardiovascular disease occurring in nondiabetic patients was determined by subtracting the number of such events in diabetic patients from those occurring in the total number of cases. The mortality per year for diabetic patients was obtained by multiplying the number of their fatal cases by 1000 and dividing the results by the totality of cases. To determine the number of nondiabetic patients/year (NNDPY), the number of diabetic patients/year (NDPY) was subtracted from the total group (NTPY), that is, NNDPY = NTPY-NDPY. Relative risk modifications (reduction or increase) and their respective P values were determined by the RATES2 module of Software Computer Programs for Epidemiologists (PEPI), 3.01 version 9.
Results
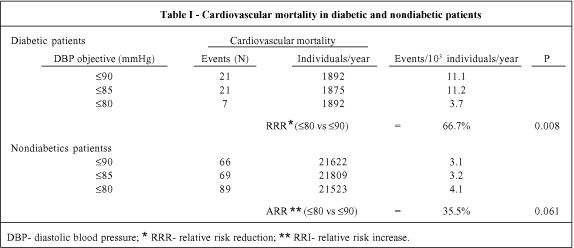
Table I shows cardiovascular mortality ratios in diabetic patients and the corresponding estimates for nondiabetic patients. Among diabetic patients, the group with a diastolic blood pressure goal of £80mmHg had the lowest level of cardiovascular mortality. A reduction in risk of death due to a cardiovascular event of approximately 66.7% (P=0.008) was observed following the comparison of the £90mmHg group (cardiovascular mortality ratio=11.1/1000) with the £80mmHg group (cardiovascular mortality ratio=3.7/1000). In contrast, in nondiabetic subjects, cardiovascular mortality was greater in the group with the diastolic blood pressure objective of £80mmHg. The relative increase in risk was approximately 35.5% (P=0.061) when the £90mmHg group (cardiovascular mortality ratio=4.1/1000 patients/year) was compared with the £80mmHg group (cardiovascular mortality ratio=3.1/1000 patients/year).
Discussion
The results for diabetic patients here presented are consistent with those of the earlier HOT Study publication 7. They show that a more intense reduction diastolic blood pressure is accompanied by a decreased occurrence in fatal cardiovascular events in this group of patients. It is important to note that in the HOT study, the average diastolic blood pressure reached in the groups with the objective of £90 and £85mmHg were 85 and 83mmHg, respectively 7. On the other hand, in the group for the objective of £80, the average diastolic blood pressure reached was around 81mmHg, higher therefore, than desired. This proximity of the averages of the diastolic blood pressure values certainly could decrease the ability of the study to demonstrate differences between the groups. Despite this, in the diabetes mellitus group, a statistically significant reduction in cardiovascular mortality was observed following the comparison of the £80 with the £90mmHg group.
It is worth noting that the results for nondiabetic subjects were not presented in the original HOT publication. According to the present analysis, in the non-diabetic hypertensive group, an inverse tendency toward cardiovascular mortality relative to diastolic blood pressure was apparent, because an increased mortality in groups with lower levels of diastolic blood pressure was observed. Although the difference in cardiovascular mortality in nondiabetic patients was found to be slightly above the conventional limit for statistical significance, the clinical significance and, above all, the implication of this finding in the public health context should be taken into consideration. It alerts to the possibility that the level of diastolic blood pressure below which risk overcomes benefit is higher in nondiabetic compared with diabetic subjects.
To apply the results of the HOT Study to medical practice, some aspects should be taken into consideration. In the HOT Study, the number of events was lower than that observed in previous published clinical reports 1. For this reason, the study was extended, resulting in an average follow-up of 3.8, rather than 2.5 years, a period not foreseen in the initial project. This is evidence that the results obtained from the various groups were better than those occurring in medical practice. The better results relative to those of other analyses from the HOT Study may be related to the fact that only 8.5% of the patients remained with a diastolic blood pressure above 90mmHg.
The HOT study brings additional evidence showing that it is beneficial to maintain the hypertensive patients under rigorous arterial pressure control. Yet, to define the ideal diastolic blood pressure interval to be maintained in hypertensive patients, it is necessary to separately analyze data from patients with or without a diabetic condition. Although the former represented 8% of the patients selected for the HOT Study, the good results associated with a more marked reduction in diastolic blood pressure observed in this group contributes greatly to the results shown by the group in general. According to the present reanalysis, it appears required to define the level below 90mmHg at which maximal reduction in cardiovascular mortality is obtained among nondiabetic patients. Studies to evaluate this question seem necessary considering the relatively high costs of antihypertensive therapy, the adverse effects of drugs, and the relevance of arterial hypertension in the public health context.
Hospital Universitário Professor Edgar Santos ¾ Universidade Federal da Bahia
Mailing address: Antonio Alberto Lopes - Rua Marechal Floriano, 448/1301 ¾ 40110-010, Salvador, BA - E-mail: aaslopes@ufba.br
-
1Collins R, Peto R, MacMahon S, et al. Blood pressure, stroke, and coronary heart disease. Part 2, Short-term reductions in blood pressure: overview of randomised drug trials in their epidemiological context. Lancet 1990; 335: 827-38.
-
2Lindholm L, Ejlertsson G, Schersten B. High risk of cerebro-cardiovascular morbidity in well treated male hypertensives. A retrospective study of 40-59-year-old hypertensives in a Swedish primary care district. Acta Med Scand 1984; 216: 251-9.
-
3Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. The sixth report. Arch Intern Med 1997; 157: 2413-46.
-
4Burt VL, Culter JA, Higgins M, et al. Trends in the prevalence, awareness, treatment, and control of hypertension in the adult US population. Data from the health examination surveys, 1960 to 1991. Hypertension 1995; 26: 60-9.
-
5Hansson L. How far should blood pressure be lowered? What is the role of the J-curve? Am J Hypertens 1990; 3: 726-9.
-
6Fletcher AE, Bulpitt CJ. How far should blood pressure be lowered? N Engl J Med 1992; 326: 251-4.
-
7Hansson L, Zanchetti A, Carruthers SG, et al. Effects of intensive blood-pressure lowering and low-dose aspirin in patients with hypertension: principal results of the Hypertension Optimal Treatment (HOT) randomised trial. HOT Study Group. Lancet 1998; 351: 1755-62.
-
8Hansson L, Zanchetti A. The Hypertension Optimal Treatment (HOT) Study-patient characteristics: randomization, risk profiles, and early blood pressure results. Blood Press 1994; 3: 322-7.
-
9Abramson JH, Gahlinger PM. Computer Programs for Epidemiologists: PEPI. USD Inc. Stone Mountain, GA, 1999.
Publication Dates
-
Publication in this collection
21 Aug 2001 -
Date of issue
Aug 2001