Abstracts
BACKGROUND: Obesity is linked to high blood pressure (HBP) in childhood. However, the role of fat as a predictor of HBP in adolescents remains unknown. OBJECTIVE: To investigate the association between general and abdominal obesity with HBP and to identify the sensitivity and specificity of these indicators to detect HBP in adolescents. METHODS: The sample was composed of 1,021 adolescents aged 10-17 years. Subjects were classified as normal, overweight/obese, according to BMI measurements, and as non-obese and with abdominal obesity, according to waist circumference (WC) measurements. Systolic (SBP) and diastolic (DBP) blood pressure were assessed using an oscillometric device. Logistic regression and ROC curves were used in the statistical analysis. RESULTS: The overall prevalence of HBP was 11.8% (13.4% in boys and 10.2% in girls). The prevalence of HBP among general overweight/obese boys and girls was 10% and 11.1%, respectively. The prevalence of HBP among boys with abdominal obesity was 28.6%. For both genders, the odds ratio (OR) for HBP was higher in abdominal obesity than in general overweight/obesity (4.09 [OR95%CI = 2.57-6.51]) versus 1.83 [OR95%CI = 1.83-4.30]). The OR for HBP was higher when general overweight/obesity and abdominal obesity were clustered (OR = 4.35 [OR95%CI = 2.68-7.05]), than when identified by either general overweight/obesity or abdominal obesity alone (OR = 1.32 [OR95%CI = 0.65-2.68]). However, both types of obesity had low predictive power in HBP detection. CONCLUSION: General and abdominal obesity were associated to HBP, however, the sensitivity and specificity of these variables to detect HBP are low in Brazilian adolescents.
Blood pressure; obesity, abdominal; overweight; waist circumference; adolescent
FUNDAMENTO: A obesidade está ligada à hipertensão arterial (HA) na infância. Entretanto, o papel da gordura como preditor de HA em adolescentes permanece desconhecido. OBJETIVO: Investigar a associação entre obesidade geral e abdominal com HA e identificar a sensibilidade e especificidade desses indicadores para detectar HA em adolescentes. MÉTODOS: A amostra consistiu em 1.021 adolescentes com idade de 10-17 anos. Os indivíduos foram classificados como normal, sobrepeso/obesidade, de acordo com as medidas do IMC, e como não-obeso com obesidade abdominal, de acordo com as medidas da circunferência da cintura (CC). A pressão arterial sistólica (PAS) e diastólica (PAD) foi avaliada através de um dispositivo oscilométrico. Regressão logística e curvas ROC foram usadas na análise estatística. RESULTADOS: A prevalência geral de HA foi 11,8% (13,4% em meninos e 10,2% em meninas). A prevalência de HA em meninos e meninas com sobrepeso/obesidade foi 10% e 11,1%, respectivamente. A prevalência de HA em meninos com obesidade abdominal foi 28,6%. Para ambos os sexos, o odds ratio (OR) para HA foi mais alto na obesidade abdominal do que no sobrepeso/obesidade geral (4,09 [OR IC95% = 2,57-6,51]) versus 1,83 [OR IC95% = 1,83-4,30]). O OR para HA foi mais alto quando sobrepeso/obesidade geral e obesidade abdominal estavam agrupados (OR = 4,35 [OR IC95% = 2,68 -7,05]), do que quando identificados como sobrepeso/obesidade geral ou obesidade abdominal apenas (OR = 1,32 [OR IC95% = 0,65- 2,68]). Entretanto, ambos os tipos de obesidade apresentavam baixo poder preditivo na detecção de HA. CONCLUSÃO: Obesidade geral e obesidade abdominal foram associadas com HA; entretanto, a sensibilidade e especificidade dessas variáveis na detecção de HA são baixas em adolescentes brasileiros.
Pressão arterial; obesidade abdominal; sobrepeso; circunferência da cintura; adolescente
Universidade Estadual Paulista, Presidente Prudente, SP; Universidade Estadual de Londrina, Londrina, PR; Universidade de Pernambuco, Recife, PE; Universidade Estadual Paulista, Rio Claro, SP - Brazil
Mailing address
ABSTRACT
BACKGROUND: Obesity is linked to high blood pressure (HBP) in childhood. However, the role of fat as a predictor of HBP in adolescents remains unknown.
OBJECTIVE: To investigate the association between general and abdominal obesity with HBP and to identify the sensitivity and specificity of these indicators to detect HBP in adolescents.
METHODS: The sample was composed of 1,021 adolescents aged 10-17 years. Subjects were classified as normal, overweight/obese, according to BMI measurements, and as non-obese and with abdominal obesity, according to waist circumference (WC) measurements. Systolic (SBP) and diastolic (DBP) blood pressure were assessed using an oscillometric device. Logistic regression and ROC curves were used in the statistical analysis.
RESULTS: The overall prevalence of HBP was 11.8% (13.4% in boys and 10.2% in girls). The prevalence of HBP among general overweight/obese boys and girls was 10% and 11.1%, respectively. The prevalence of HBP among boys with abdominal obesity was 28.6%. For both genders, the odds ratio (OR) for HBP was higher in abdominal obesity than in general overweight/obesity (4.09 [OR95%CI = 2.57-6.51]) versus 1.83 [OR95%CI = 1.83-4.30]). The OR for HBP was higher when general overweight/obesity and abdominal obesity were clustered (OR = 4.35 [OR95%CI = 2.68-7.05]), than when identified by either general overweight/obesity or abdominal obesity alone (OR = 1.32 [OR95%CI = 0.65-2.68]). However, both types of obesity had low predictive power in HBP detection.
CONCLUSION: General and abdominal obesity were associated to HBP, however, the sensitivity and specificity of these variables to detect HBP are low in Brazilian adolescents.
Keywords: Blood pressure; obesity, abdominal; overweight; waist circumference; adolescent.
Introduction
Cardiovascular diseases are the leading cause of death in the world1,2. High blood pressure (HBP) is one of the major risk factors for cardiovascular disease, and when present in childhood, it predicts cardiovascular mortality in adulthood3. This is an important issue since the prevalence of HBP in pediatric populations is high in developed and developing countries, ranging from 3.6% to 19.4%4,5.
Childhood obesity is also highly prevalent in developed6,7 and in developing countries8 and has been considered the best predictor of childhood hypertension9. Moreover, higher body mass index (BMI) in infancy is positively and significantly related to triglycerides and systolic blood pressure at 23 years of age10. Therefore, the diagnosis of childhood obesity can provide an early identification of the risk of HBP and other chronic diseases.
Obesity has been identified in clinical setting using two practical, cost-effective and feasible methods: waist circumference (WC) and BMI. Although abdominal obesity is more often associated with cardiovascular risk than with general obesity in adults, this association in pediatric populations is yet to be clarified. A previous study that analyzed the association between fat distribution and cardiovascular risk in children showed that both types of obesity are linked to HBP in childhood11, however, the best predictor of HBP in adolescents remains uncertain.
Recently, Genovesi et al11 observed that WC improves the ability of BMI to detect HBP in Italian children aged 5 to 11 years, suggesting that the evaluation of both types of obesity is better for screening children at risk of HBP. Nevertheless, since this study was performed in children from a specific country, its results may not be generalized to adolescents from other nations12, which are known to have different lifestyle habits.
Thus, the purposes of this study were (i) to investigate the association of general and abdominal obesity with HBP and (ii) to identify the sensitivity and specificity of these indicators to detect HBP in Brazilian adolescents.
Methods
Sample
This cross-sectional study was carried out in Londrina, Southern Brazil. The sample was composed of 1,021 adolescents enrolled in either private or public schools, aged 10 to 17 years. A sample size of 1,021 subjects was estimated by means of an expected HBP prevalence of 10%, error of 3%, power of 80%, confidence interval of 95%, and additional data for losses of 15% (based on a pilot study that found 10.2% of losses). Sampling was performed by means of a random multistage based on all regions of the city (east, west, north, south, and center) and on the total number of schools (respecting the proportion of public and private students in each region of the city). Informed consent was obtained from each volunteer's parent or guardian. This study was approved by the Ethics Committee on Human Experimentation of the State University of Londrina.
Anthropometric variables
All anthropometric measurements were performed by trained technicians in a reserved room at school. Body weight was measured using a mobile digital scale accurate to 0.1 kg and with maximum capacity of 150 kg. Subjects were asked to wear light clothes and to stand barefoot in the center of the platform scale. Height was measured using a portable stadiometer accurate to 0.1 cm and with a maximum length of 2.0 meters. Adolescents were required to stand barefoot, turned back to the stadiometer with the head positioned in the Frankfurt plane. The mobile part of the stadiometer was conducted by touching the vertex, with the compression of the hair according to the procedures described by Gordon et al13. BMI was calculated as weight (kg)/height squared (m). WC was determined by the mean of two measurements of the minimum circumference between the iliac crest and rib cage, using a metal tape with the accuracy in millimeters (mm).
General and abdominal obesity
General overweight/obesity was classified according to the cutoff points suggested by Cole et al14, while abdominal obesity was identified according to the criteria proposed by Taylor et al15. Additionally, based on both adiposity indexes, the sample was stratified in: (i) neither general overweight/obesity nor abdominal obesity, (ii) only general overweight/obesity, (iii) only abdominal obesity, and (iv) both general overweight/obesity and abdominal obesity.
Blood pressure measures
Systolic (SBP) and diastolic (DBP) blood pressure were assessed using an oscillometric device Omron HEM 742-E, which was calibrated and previously validated for adolescents16. For blood pressure measurements, the cuff was adjusted to the arm circumference (9 x 18 cm and 12 x 23 cm), following the recommendations of the American Heart Association (AHA)17. After the assessment of arm circumference, a 9x 18-cm-width cuff was used for the assessment of subjects with arm circumference between 16 to 22 cm, while a 12 x 23 cm width cuff was employed for the assessment of subjects with arm circumference between 23 and 34 cm, respectively.
One day prior blood pressure assessment, subjects were asked not to practice physical activity18 and avoid caffeinated beverages19. Blood pressure measurement was performed in a quiet room. After a 5-minute rest in the sitting position, a single previously trained evaluator performed two blood pressure measurements (with a 2-minute interval between them) and the mean of both was used for the analysis. If blood pressure differed more than 5 mmHg between measurements, two more measurements were performed and the mean of these measures were used for analysis (this event occurred in less than 1% of the sample).
HBP was defined as blood pressure > percentile 95, adjusted by age and height according to the National High Blood Pressure Education Program20 criteria. Subjects with HBP received a counseling feedback that included increase in physical activity levels, as previously suggested21. Moreover, adolescents were advised to visit a physician in a Basic Health Unit (Public Health System).
Statistical procedures
Descriptive statistics were expressed as mean, standard deviation (SD), minimum and maximal for age, weight, height, BMI, WC, SBP and DBP. Differences between genders in the continuous variables were analyzed using Student t test for independent samples. Chi-square test was used to assess the association between categorical variables, while binary logistic regression, represented by odds ratio values (OR) and 95% confidence intervals (OR95%CI), was used to determine the magnitude of these associations. ROC curve and its parameters (sensitivity, specificity, area under curve [AUC], positive predictive value [PPV], and negative predictive value [NPV]) were applied to assess general overweight/obesity and abdominal obesity diagnosis characteristics. Statistical analyses were conducted in SPSS software (version 13.0) and the significance level was set at 0.05.
Results
Most of the sample was composed of females (52%). Sixty-five percent of the sample was aged 11 to 13 years and the mean age of all adolescents was 12.3 ± 1.5. BMI and WC values were higher in males than in females (p < 0.05). There were no significant differences in any other variables (Table 1).
The prevalence of general overweight/obesity was 21.9% and 14.8% for males and females (p = 0.004), respectively. The prevalence of abdominal obesity was 15.2% and 8.5% in males and females (p = 0.001), respectively. Considering the subjects who had general overweight/obesity and abdominal obesity, the prevalence was 13.8% and 8.0% in males and females, respectively. In the overall sample, 76 subjects (7.4% [40 boys and 36 girls]) had general overweight/obesity, but not abdominal obesity, 10 subjects (1% [7 boys and 3 girls]) had abdominal obesity, but not general overweight/obesity and 110 subjects (10.8% [68 boys and 42 girls]) had both outcomes.
The overall prevalence of HBP was 11.8% (CI = 7-13%) and the prevalence of overweight and obesity was 18.2% (CI = 14.2-20.1%). The prevalences of HBP among boys and girls that had only general overweight/obesity were 10% and 11.1%, respectively. The prevalence of HBP among boys with only abdominal obesity was 28.6% (n = 2). Considering the subjects who had general overweight/obesity and abdominal obesity, the prevalence of HBP in boys and girls was 30.9% and 28.6%, respectively. In our pediatric sample, only 2% (n = 20) of the overall sample had systolic or diastolic blood pressure higher than 139 mmHg and 89 mmHg, respectively.
The OR of HBP was higher in abdominal obesity than in general overweight/obesity (4.09 [OR95%CI = 2.57-6.51]) versus 1.83 [OR95%CI = 1.83-4.30]). The OR of HBP was higher when general overweight/obesity and abdominal obesity were clustered (OR = 4.35 [OR95%CI = 2.68-7.05]), than when identified as either general overweight/obesity or abdominal obesity alone (OR = 1.32 [OR95%CI = 0.65-2.68]) (table 2).
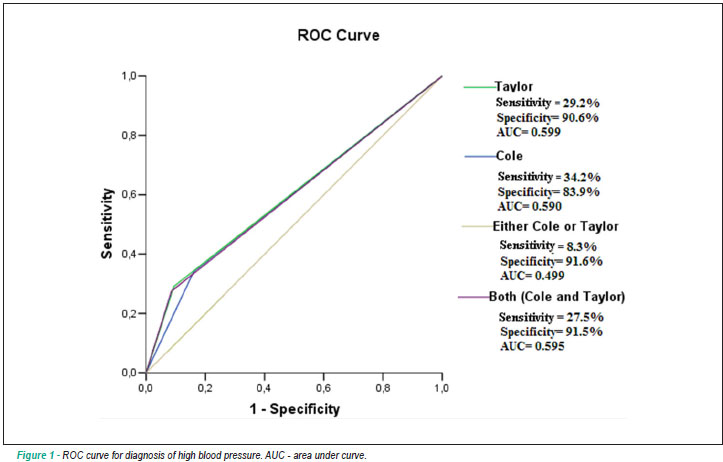
General overweight/obesity criteria showed higher sensitivity (34.2%), while abdominal obesity criteria showed higher AUC (0.599 ± 0.030) to detect HBP. PPV values were low in all analyzes, but the clustered use of both obesity indicators slightly improved the scores (Figure 1).
Paired comparisons of AUC indicated that the mean differences were similar between general overweight/obesity and abdominal obesity (mean differences = 0.0083 ± 0.021 [95%CI = -0.034; 0.051]; p = 0.703), and between both obesity indicators clustered and general overweight/obesity (mean differences = 0.0044 ± 0.020 [95%CI = -0.034; 0.043]; p = 0.826) or abdominal obesity (mean differences = 0.0038 ± 0.009 [95%CI = -0.014; 0.021]; p = 0.671) alone. The general overweight/obesity or abdominal obesity presented lower accuracy than both indicators clustered (p = 0.012).
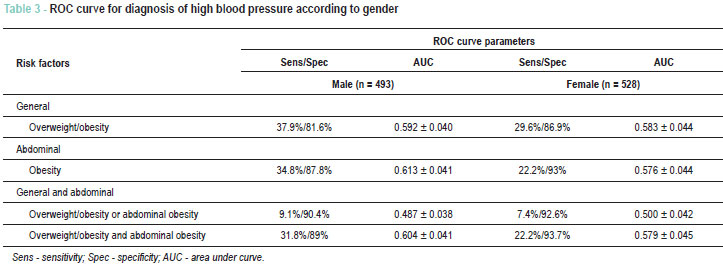
In both genders, abdominal obesity presented a higher sensitivity. The sensitivity scores were higher in boys than in girls, while the specificity was higher in girls than in boys. In the general analysis, anthropometric indexes were more accurate in boys than in girls (Table 3).
Discussion
The main results of this cross-sectional study were: (i) abdominal obesity and general overweight/obesity are associated with HBP in Brazilian adolescents; (ii) the diagnostic properties of general overweight/obesity or abdominal obesity are low; and (iii) the clustered use of both general overweight/obesity and abdominal obesity improved the sensitivity to detect HBP.
The link between hypertension and obesity is not completely understood. Several factors, such as an increase in the secretion of angiotensinogen, renin, and other substances by adipocytes, as well as the increase in tumor necrosis factor-α levels has been suggested to be the factors that link obesity and hypertension. Moreover, the increase in visceral fat leads to insulin resistance22 and vasoconstriction23,24. In fact, childhood BMI is a powerful predictor of cardiovascular disease, since it is positively related to increased values of fasting insulin, triglycerides and systolic blood pressure, as well as decreased high density lipoprotein scores in adulthood10. Thus, the adiposity indexes seem to screen children and adolescents at increased risk of hypertension and other chronic diseases.
However, the role of fat distribution in cardiovascular risk in children and adolescents remains inconclusive. In the present study, neither general overweight/obesity nor abdominal obesity, when analyzed alone was associated with HBP. These results are different from a previous study, which identified an association between general overweight/obesity or abdominal obesity and HBP among adolescents11. The main reason for this controversy is that the previous studies did not describe how many subjects had both types of obesity. In the present study, approximately 28% of the adolescents with HBP had general and abdominal obesity, whereas only a few adolescents had only general overweight/obesity (6.6%) or abdominal obesity (1.6%).
The results of the present study showed that simultaneous general overweight/obesity and abdominal obesity were associated with HBP in adolescents. These results are in agreement with Genovesi et al11 that observed, in 4,177 children, that the association of general and abdominal obesity indicators are better to predict HBP than the use of only one indicator alone. The association between general and abdominal obesity has been previously described25, suggesting that central and general obesity act together in the development of HBP in this population.
Although the assessment of blood pressure is the best way to identify subjects with HBP, it is still poorly performed in clinical practice due to several reasons. First, it is time-consuming, as subjects need to rest for a period and blood pressure must be assessed at least three times in both arms. Second, to perform blood pressure measurements, subjects have to follow several recommendations that include avoiding caffeine and alcohol19 and not performing physical activity on the day before the assessment, as post-exercise hypotension might last for several hours18. Thus, these recommendations need to be given to subjects at least one day before the measurement. Third, the assessment of blood pressure depends on an adequate device. Finally, the interpretation of blood pressure measurements is very difficult, since it involves the analysis of several tables. Therefore, the results of this study have important practical applications. Based on our results, the measurement of general and abdominal obesity might be useful for screening children with increased risk of HBP. Thus, in settings with a large number of children (e.g. schools) in which the measurement of blood pressure is not feasible, the use of anthropometric measurements might be considered. Moreover, as this study was performed in a developing country in which the assessment of blood pressure is not common, especially in the public health system, the results obtained might be easily incorporated into clinical practice, strengthening the practical application of the results.
This study presents several limitations that should be considered in the interpretation of the results. It was limited by the cross-sectional design, which does not allow us to analyze a causality effect. The measurements of other indicators of cardiovascular risk, such as glucose tolerance, body composition and physical activity were not performed. In fact, it is an important issue, as previous studies have reported that these factors are also associated with HBP26. The lack of body composition measurements limited our understanding as to whether the classification provided by BMI reflected adiposity in the adolescents. Maturation indicators were not collected and inferences regarding the association between anthropometric indicators and HBP according to maturational status were not possible to be established.
In addition, this study has limitations regarding blood pressure assessment. Blood pressure was obtained using two cuff sizes, which are adequate to assess subjects with arm circumferences between 16 and 22 cm and between 27 and 34 cm. Thus, the assessment of blood pressure in subjects with an arm circumference between 23 and 26 cm was performed using the largest cuff size, which might have underestimated the blood pressure levels of these subjects. The assessment of auscultatory blood pressure in subjects who have HBP according to the automatic device has been recommended19. In this study, this procedure was not performed due to the high number of subjects studied. Therefore, although the equipment used to assess blood pressure showed high sensitivity and specificity, some false positive cases might have occurred. Finally, in this study, data regarding parental obesity and hypertension were not assessed. Considering that genetics seems to play an important role in the occurrence of obesity and HBP in children and adolescents27,28, it might be a potential variable for screening adolescents at risk of HBP, and should be investigated in future studies.
In conclusion, general and abdominal obesity are associated to HBP; however, the sensitivity and specificity of these variables to detect HBP is low in Brazilian adolescents.
References
- 1. Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension. 2003;42(6):1206-52.
- 2. Van den Hoogen PC, Feskens EJ, Nagelkerke NJ, Menotti A, Nissinen A, Kromhout D. The relation between blood pressure and mortality due to coronary heart disease among men in different parts of the world. N Eng J Med. 2000;342(1):1-8.
- 3. Lauer RM, Clarke WR, Witt J. Childhood risk factors for high adult blood pressure: the Muscatine study. Pediatrics. 1989;84(4):633-41.
- 4. Oliveira AM, Oliveira AC, Almeida MS, Almeida FS, Ferreira JB, Silva CE, et al. Environmental and anthropometric factors associated with childhood arterial hypertension. Arq Bras Endocrinol Metab. 2004;48(6):849-54.
- 5. Sorof JM, Lai D, Turner J, Poffenbarger T, Portman RJ. Overweight, ethnicity, and the prevalence of hypertension in school-aged children. Pediatrics. 2004;113(3):475-82.
- 6. Reich A, Muller G, Gelbrich G, Deutscher K, Godicke R, Kiess W. Obesity and blood pressure-results from the examination of 2365 schoolchildren in Germany. Int J Obes. 2003;27(12):1459-64.
- 7. Hedley AA, Ogden CL, Johnson CL, Carroll MD, Curtin LR, Flegal KM. Prevalence of overweight and obesity among US children, adolescents, and adults, 1999-2002. JAMA. 2004;16(23):2847-50.
- 8. Abrantes MM, Lamounier JA, Colosimo EA. Overweight and obesity prevalence among children and adolescents from Northeast and Southeast regions of Brazil. J Pediatr (Rio J). 2002;78(4):335-40.
- 9. Ostchega Y, Carroll M, Prineas RJ, McDowell MA, Louis T, Tilert T. Trends of elevated blood pressure among children and adolescents: data from the National Health and Nutrition Examination Survey1988-2006. Am J Hypertens. 2009;22(1):59-67.
- 10. Sinaiko AR, Donahue RP, Jacobs DR Jr, Prineas RJ. Relation of weight and rate of increase in weight during childhood and adolescence to body size, blood pressure, fasting insulin, and lipids in young adults. The Minneapolis Children's Blood Pressure Study. Circulation. 1999;99(11):1471-6.
- 11. Genovesi S, Antolini L, Giussani M, Pieruzzi F, Galbiati S, Valsecchi MG, et al. Usefulness of waist circumference for the identification of childhood hypertension. J Hypertens. 2008;26(8):1563-70.
- 12. Rosa ML, Mesquita ET, da Rocha ER, Fonseca Vde M. Body mass index and waist circumference as markers of arterial hypertension in adolescents. Arq Bras Cardiol. 2007;88(5):573-8.
- 13. Gordon CC, Chumlea WC, Roche AF. Stature, recumbent length and weight. In: Lohman TG, Roche AF, Martorel R, editors. Anthropometric standardization reference manual. Champaign: Human Kinetics Books; 1988. p. 3-8.
- 14. Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320(7244):1240-3.
- 15. Taylor RW, Jones JE, Williams SM, Goulding A. Evaluation of waist circumference, waist-to-hip, and the conicity index as screening tools for high trunk fat mass, as measured by dual-energy X-ray absorptiometry, in children aged 3-19y. Am J Clin Nutr. 2000;72(2):490-5.
- 16. Christofaro DG, Casonatto J, Polito MD, Cardoso JR, Fernandes R, Guariglia DA, et al. Evaluation of the Omron MX3 Plus monitor for blood pressure measurement in adolescents. Eur J Pediatr. 2009;168(11):1349-54.
- 17. Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves J, Hill MN, et al. Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Hypertension. 2005;45(1):142-61.
- 18. Mota MR, Padorno E, Lima LC, Arsa G, Bottaro M, Campbell CS, et al. Effects of treadmill running and resistance exercises on lowering blood pressure during the daily work of hypertensive subjects. J Strength Cond Res. 2009; 23(8):2331-8.
- 19. Sociedade Brasileira de Cardiologia / Sociedade Brasileira de Hipertensão / Sociedade Brasileira de Nefrologia. VI Diretrizes brasileiras de hipertensão. Arq Bras Cardiol. 2010;95(1 supl.1):1-51
- 20. National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 114(2 Suppl 4th Report):555-76.
- 21. Leary SD, Ness AR, Smith GD, Mattocks C, Deere K, Blair SN, et al. Physical activity and blood pressure in childhood: findings from a population-based study. Hypertension. 2008;51(1):92-8.
- 22. Mattinson R, Jensen M. The adipocyte as an endocrine cell. Curr Opin Endocrinol Diabetes and Obesity. 2003;10(5):317-21.
- 23. Sinaiko A. Obesity, insulin resistance and the metabolic syndrome. J Pediatr (Rio J). 2007;83(1):3-5.
- 24. Mlinar B, Marc J, Janez A, Pfeifer M. Molecular mechanisms of insulin resistance and associated diseases. Clin Chim Acta. 2007;375(1):20-35.
- 25. Fernandes RA, Christofaro DG, Buonani C, de Araújo LR, Kassab YK, Cardoso JR, et al. The accuracy of national body fat cutoff levels in the prediction of elevated blood pressure among Brazilian male adolescents. J Trop Pediatr. 2009;56(3):208-9.
- 26. Eisenmann JC, Welk GJ, Ihmels M, Dollman J. Fatness, fitness, and cardiovascular disease risk factors in children and adolescents. Med Sci Sports Exerc. 2007;39(8):1251-6.
- 27. Ramos de Marins VM, Almeida RM, Pereira RA, de Azevedo Barros MB. The relationship between parental nutritional status and overweight children/adolescents in Rio de Janeiro, Brazil. Public Health. 2004;118(1):43-9.
- 28. Elias MC, Bolivar MS, Fonseca FA, Martinez TL, Angelini J, Ferreira C, et al. Comparison of the lipid profile, blood pressure, and dietary habits of adolescents and children descended from hypertensive and normotensive individuals. Arq Bras Cardiol. 2004;82(2):139-42.
High blood pressure detection in adolescents by clustering overall and abdominal adiposity markers
Publication Dates
-
Publication in this collection
29 Apr 2011 -
Date of issue
June 2011
History
-
Accepted
09 Dec 2010 -
Reviewed
30 Nov 2010 -
Received
28 May 2010