Abstract
Abdominal ultrasound (US) has been widely used in the evaluation of patients with schistosomiasis mansoni. It represents an important indirect method of diagnosis and classification of the disease, and it has also been used as a tool in the evaluation of therapeutic response and regression of fibrosis. We describe the case of a man in whom US showed solid evidence of schistosomal periportal fibrosis and magnetic resonance imaging revealed that periportal signal alteration corresponded to adipose tissue which entered the liver togheter with the portal vein.
schistosomiasis; Schistosoma mansoni; ultrasound; magnetic resonance imaging
Disagreement between ultrasound and magnetic resonance imaging in the identification of schistosomal periportal fibrosis
Luciana CS SilvaI,1 1 Corresponding author: lucristina@medicina.ufmg.br ; Ana CF PereiraI; Leonardo C QueirozII; Luciene M AndradeIII; Carlos MF AntunesI; José R LambertucciI
IServiço de Doenças Infecciosas e Parasitárias, Faculdade de Medicina
IIServiço de Radiologia, Hospital das Clínicas, Universidade Federal de Minas Gerais, Av. Alfredo Balena 190, sala 3035, 30130-100 Belo Horizonte, MG, Brasil
IIIDepartamento de Diagnóstico por Imagem, Instituto Hermes Pardini, Belo Horizonte, MG, Brasil
ABSTRACT
Abdominal ultrasound (US) has been widely used in the evaluation of patients with schistosomiasis mansoni. It represents an important indirect method of diagnosis and classification of the disease, and it has also been used as a tool in the evaluation of therapeutic response and regression of fibrosis. We describe the case of a man in whom US showed solid evidence of schistosomal periportal fibrosis and magnetic resonance imaging revealed that periportal signal alteration corresponded to adipose tissue which entered the liver togheter with the portal vein.
Key words: schistosomiasis - Schistosoma mansoni - ultrasound - magnetic resonance imaging
Abdominal ultrasound (US) has been widely used in the evaluation of patients with schistosomiasis mansoni. It represents an important indirect method of diagnosis and classification of the disease (Abdel-Latif et al. 1981, Hussain et al. 1984, Fataar et al. 1984, Cerri et al. 1984, Homeida et al. 1988a, b, Abdel-Wahab et al. 1989, Pinto-Silva et al. 1994, Gerspacher-Lara et al. 1998, Gerspacher-Lara 1999, Niamey Working Group 2000, Ritcher et al. 2001, Lambertucci et al. 2001). US has also been used as a tool in the evaluation of therapeutic response and regression of fibrosis in schistosomiasis (Massoud et al. 1986, Homeida et al. 1988c, Homeida et al. 1991, Doehring-Schwerdtfeger et al. 1992, Boisier et al. 1998, Frenzel et al. 1999, De Jesus et al. 2000, Cota et al. 2006). Ultra-sonographic examination of subjects with hepatosplenic schistosomiasis has detected a characteristic pattern of abnormalities, quite different from the aspects observed in liver cirrhosis (Homeida et al. 1988a, Abdel-Wahab et al. 1989) and in acute schistosomiasis (Barata et al. 1999, Lambertucci et al. 1994, 1997). The most important finding was echogenic thickening of the walls of the portal vein and its branches. Field studies in endemic areas have shown that the sum of total thickening of three peripheral branches of the portal vein, thickening of gall-bladder wall, enlargement of the left lobe of the liver, and thickening of the portal vein in its bifurcation are the best variables for ultrasonographic diagnosis of schistosomiasis mansoni (Gerspacher-Lara 1999).
Magnetic resonance imaging (MRI) has been described in four cases of hepatosplenic schistosomiasis mansoni (Patel et al. 1993, Willemsen et al. 1995, Lambertucci et al. 2002, 2004). The first two studies used US, computed tomography (CT) and MRI in the evaluation of a patient with hepatosplenic schistosomiasis mansoni. The findings of the different methods were in agreement in both studies. Periportal echogenic thickening on US, suggestive of fibrosis, and low attenuation bands about the portal vessels, which markedly enhanced with contrast CT were described. MRI demonstrated the same periportal bands that were seen on liver US and CT scans. These bands showed hiperintense signal on T2-weighted sequences, and were isointense in T1-weighted sequences, with enhancement after contrast administration. The studies of Lambertucci et al. (2002, 2004) evaluated patients with advanced forms of hepatosplenic schistosomiasis by US and MRI. Both methods were again in agreement with respect to the presence of intense periportal fibrosis. Once more, MRI demonstrated broad periportal bands hypointense to the liver on T1-weighted sequences, while they had increased signal on T2-weighted images. Thickening of the gallbladder wall, enlargement of spleen, splenic and portal veins and collateral vessels were detected. After contrast administration, T1-weighted images revealed enhancement of the gallbladder wall and periportal space.
We describe the case of a man in whom the results of US and MRI were not in agreement with respect to the identification of periportal fibrosis.
PATIENTS AND METHODS
A 59-year-old man was referred to the Hospital of the Federal University of Minas Gerais, in Brazil, for the evaluation of schistosomal periportal fibrosis, suggested by an abdominal US performed elsewhere. He was a resident of Belo Horizonte, a city where schistosomiasis is not endemic, but informed previous contact with stream waters in areas were transmission of the disease is known to occur. Examination of nine stool samples did not disclose eggs of Schistosoma mansoni, and no eggs or granulomas were detected by a rectal biopsy. The patient denied previous episodes of digestive bleeding, ascitis or jaundice, as well as chronic prescribed drugs use or alcohol abuse. His clinical examination revealed no abnormalities: liver and spleen were non palpable, and no signs of portal hypertension of hepatic dysfunction were found. Blood counts also revealed no alterations: 6.28 ´ 106 red cells/mm3, hemoglobin 16.7 g/dl, 149 ´ 103 platelets/mm3, 6.1 ´ 103 white cells/mm3. Serological investigation for hepatitis B and C were negative and blood chemistry and coagulation were unremarkable (albumin 4.5 g/dl, ASAT 29 g/dl, ALAT 39 g/dl, GGT 31 g/dl).
A new US examination of the abdomen was performed using real-time ALOKA SSD 1700 device (Japan) with electronic linear 3.5 MHz transducers. Additional imaging was obtained using a GE 1.5 T Sigma unit (General Eletric, New Jersey, US). Axial and coronal 5 mm slice thickness images were performed in T1 and T2-weighted sequences, before and after contrast administration.
RESULTS
US of the abdomen showed enlarged central periportal bands with increased echogenicity, suggesting intense central fibrosis (Fig. 1). Echogenic thickening of the gallbladder wall was also detected (Fig. 2). The image pattern was characteristic of hepatic fibrosis produced by S. mansoni. No evidence of portal hypertension, such as portal vein or spleen enlargement and collateral veins, was noticed.
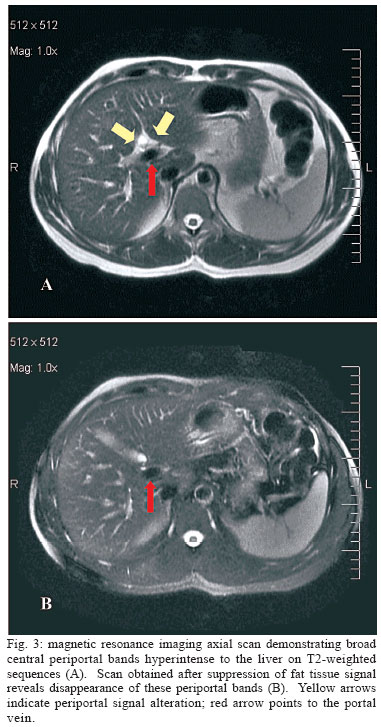
MRI demonstrated broad central periportal bands hypointense to the liver on T1-weighted sequences, and with increased signal on T2-weighted images. However, after suppression of fat tissue signal, these periportal bands disappeared (Fig. 3). This finding shows that US periportal thickening suggestive of schistosomal fibrosis corresponded in fact to adipose tissue. Like US, MRI did not detect any evidence of portal hypertension.
DISCUSSION
MRI was decisive to put away the diagnosis of schistosomal periportal fibrosis suggested by US in the patient described above. All clinical and laboratory aspects of the case reported suggested absence of schistosomiasis, and there were no evidences of the hepatosplenic form of the disease. However, US images in this patient showed solid evidence of schistosomal periportal fibrosis, since characteristic periportal thickening was observed. The hypothesis of schistosomiasis was then made, since periportal fibrosis can occur without enlarged liver or spleen, or without portal hypertension. Surprisingly MRI revealed that periportal signal alteration corresponded to adipose tissue which entered the liver surrounding the portal vein.
Up to 20 years ago, field studies would distinguish hepatosplenic schistosomiasis from other chronic forms of the disease by detecting a palpable spleen on physical examination (Kloetzel 1962, Barreto et al. 1985, Lambertucci & Barravieira 1994, Prata 2002). Liver and spleen enlargement in a person eliminating S. mansoni eggs in stool was indicative of Symmers fibrosis in both epidemiological studies and in those involving hospitalized patients. In the last two decades, studies comparing spleen palpation with more accurate methods for detecting spleen enlargement, such as ultrasound, have shown serious limitations on abdominal physical examination (Sullivan & Williams 1976, Barkun et al. 1991). These studies have established that some spleens of normal size are palpable, and have confirmed that many enlarged spleens are non palpable. Studies comparing abdominal physical examination with US have established that spleen palpation is not precise for the diagnosis of spleen enlargement and for the identification of severe cases in endemic areas of schistosomiasis (Homeida et al. 1988b, Abdel-Wahab et al. 1992, Lambertucci et al. 1996, Gerspacher-Lara et al. 1998).
Lambertucci et al. (2001) have studied 741 subjects with schistosomiasis in an endemic area of Minas Gerais. US examination identified 15 patients (2%) with intense periportal thickening without spleen enlargement, showing that intense periportal fibrosis can occur without splenomegaly, and that subjects with severe forms of the disease could have not been included in previous studies evaluating morbidity. Symmers fibrosis in patients without spleen enlargement has also been described previously by one US study in Africa (Homeida et al. 1988b) and by one autopsy study in Brazil (Prata & Andrade 1963).
These are examples of how new techniques allow us to better access and comprehend the morbidity in schistosomiasis (Barbosa et al. 1996). MRI has been established as a very sensitive image method in various diseases and, different from US, is not a dynamic study and can be less examiner-dependent. Disagreement between US and MRI (in favor of the second) in the identification of schistosomal periportal fibrosis was found in this case. Studies of series of cases are necessary to compare these image methods and to define the role of MRI in the diagnosis and evaluation of morbidity in schistosomiasis mansoni.
Niamey Working Group 2000. Ultrasound in schistosomiasis. A practical guide to the standardized use of ultrasonography for the assessment of schistosomiasis-related morbidity. World Health Organization/TDR/SCH/ULTRASON/document. Geneva.
Received 25 May 2006
Accepted 26 June 2006
Partial financial support: CNPq
- Abdel-Latif Z, Abdel-Wahab MF, El-Kady NM 1981. Evaluation of portal hypertension in cases of hepatosplenic schistosomiasis using ultrasound. J Clin Ultrasound 9: 409-412.
- Abdel-Wahab MF, Esmat G, Milad M, Abdel-Razek S, Strickland GT 1989. Characteristic sonographic pattern of schistosomal hepatic fibrosis. Am J Trop Med Hyg 40: 72-76.
- Abdel-Wahab MF, Esmat G, Farrag A, El-Boraey YA, Strickland GT 1992. Grading of hepatic schistosomiasis by the use of ultrasonography. Am J Trop Med Hyg 46: 403-408.
- Barata CH, Pinto-Silva RA, Lambertucci JR 1999. Abdominal ultrasound in acute schistosomiasis mansoni. Br J Randiol 72: 949-952.
- Barbosa MM, Lamounier JA, Oliveira EC, Souza MV, Marques DS, Silva AA, Lambertucci JR 1996. Pulmonary hypertension in schistosomiasis mansoni. Trans R Soc Trop Med Hyg 90: 663-665.
- Barkun NA, Camus M, Green L, Meagher T, Coupal L, De Stempel J, Grover AS 1991. The bedside assessment of splenic enlargement. Am J Med 91: 512-518.
- Barreto ML, Loureiro S, Melo AS, Anjos CFD 1985. The effect of Schistosoma mansoni infection on child morbidity in the state of Bahia, Brazil. Rev Inst Med Trop São Paulo 27: 167-171.
- Boisier P, Ramarokoto CE, Ravaoalimalala VE, Rabarijaona L, Serieye J, Roux J, Esterre P 1998. Reversibility of Schistosoma mansoni-associated morbidity after yearly mass praziquantel therapy: ultrasonographic assessment. Trans R Soc Trop Med Hyg 92: 451-453.
- Cerri GG, Alves VAF, Magalhães A 1984. Hepatosplenic schistosomiasis mansoni: ultrasound manifestations. Radiology 153: 777-780.
- Cota GF, Pinto-Silva RA, Antunes CMF, Lambertucci JR 2006. Ultrasound and clinical investigation of hepatosplenic schistosomiasis: evaluation of splenomegaly and liver fibrosis four years after mass chemotherapy with oxamniquine. Am J Trop Med Hyg 74: 103-107.
- De Jesus AR, Miranda DG, Miranda RG, Araújo I, Magalhães A, Bacellar M, Carvalho EM 2000. Morbidity associated with Schistosoma mansoni infection determined by ultrasound in an endemic area of Brazil, Caatinga do Moura. Am J Trop Med Hyg 63: 1-4.
- Doehring-Schwerdtfeger E, Abdel-Rahim IM, Kardorff R, Kaiser C, Franke D, Schlake J, Richter J, Elsheikh M, Mohamed-Ali Q, Ehrich JHH 1992. Ultrasonographical investigation of periportal fibrosis in children with Schistosoma mansoni infection: reversibility of morbidity twenty-three months after treatment with praziquantel. Am J Trop Med Hyg 46: 409-415.
- Fataar S, Bassiony H, Satyanath S, Vassileva J, Hanna RM 1984. Characteristic sonographic features of schistosoma periportal fibrosis. Am J Roent 143: 69-71.
- Frenzel K, Grigull L, Odongo-Aginya E, Ndugwa CM, Loroni-Lakwo T, Schweigmann U, Vester U, Spannbrucker N, Doehring E 1999. Evidence for a long-term effect of a single dose of praziquantel on Schistosoma mansoni-induced hepatosplenic lesions in northern Uganda. Am J Trop Med Hyg 60: 927-31.
- Gerspacher-Lara R 1999. Parâmetros Quantitativos para o Diagnóstico Ultra-sonográfico da Esquistossomose Mansônica, PhD Thesis, Faculdade de Medicina da UFMG, Belo Horizonte: 114 pp.
- Gerspacher-Lara R, Pinto-Silva RA, Serufo JC, Rayes AAM, Drummond SC, Lambertucci JR 1998. Splenic palpation for the evaluation of morbidity due to schistosomiasis mansoni. Mem Inst Oswaldo Cruz 93: 245-248.
- Homeida M, Abdel-Gadir AF, Cheever AW, Bennett JL, Arbab BMO, Ibrahium SZ, Abdel-Salam IM, Dafalla AA, Nash TE 1988a. Diagnosis of pathologically confirmed Symmers' periportal fibrosis by ultrasonography: a prospective blinded study. Am J Trop Med Hyg 38: 86-91.
- Homeida M, Ahmed S, Dafalla A, Suliman S, El Tom I, Nash T, Bennett JL 1988b. Morbidity associated with Schistosoma mansoni infection as determined by ultrasound: a study in Gezira, Sudan. Am J Trop Med Hyg 39: 196-201.
- Homeida M, El Tom I, Nash T, Bennett JL 1988c. Association of the therapeutic activity of praziquantel with the reversal of Symmers' fibrosis induced by Schistosoma mansoni Am J Trop Med 45: 360-365.
- Homeida MA, Tom IE, Nash T, Bennett JL 1991. Association of the therapeutic activity of praziquantel with the reversal of Symmers' fibrosis induced by Schistosoma mansoni. Am J Trop Med Hyg 45: 360-365.
- Hussain S, Hawass ND, Zaidi AJ 1984. Ultrasonographic diagnosis of schistosomal periportal fibrosis. J Ultrasound Med 3: 449-452.
- Kloetzel K 1962. Splenomegaly in schistosomiasis mansoni. Am J Trop Med Hyg 11: 472-476.
- Lambertucci JR, Barravieira B 1994. Esquistossomose mansônica. Estudo clínico. JBM 67: 59-100.
- Lambertucci JR, Andrade LM, Pinto-Silva RA 2002. Magnetic resonance imaging of the liver in hepatosplenic schistosomiasis mansoni. Rev Soc Bras Med Trop 35: 679-680.
- Lambertucci JR, Cota GF, Pinto-Silva RA, Serufo JC, Gerspacher-Lara R, Drummond SC, Antunes CM, Nobre V, Rayes AAM 2001. Hepatosplenic schistosomiasis in field-bases studies: a combined clinical and sonografic definition. Mem Inst Oswaldo Cruz 96:147-150.
- Lambertucci JR, Gerspacher-Lara R, Pinto-Silva RA, Barbosa MM, Teixeira R, Barbosa HF, Serufo JC, Rezende DF, Drummond SC, Rayes AAM 1996. O projeto Queixadinha: a morbidade e o controle da esquistossomose em área endêmica no nordeste de Minas Gerais, Brasil. Rev Soc Bras Med Trop 29: 127-135.
- Lambertucci JR, Pinto-Silva RA, Gerspacher-Lara R, Barata CH 1994. Acute Manson's schistosomiasis: sonographic features. Trans R Soc Trop Med Hyg 88: 76-77.
- Lambertucci JR, Rayes AAM, Barata CH, Teixeira R, Gers-pacher-Lara R 1997. Acute schistosomiasis: report on five singular cases. Mem Inst Oswaldo Cruz 92: 631-635.
- Lambertucci JR, Silva LCS, Andrade LM, Queiroz LC, Pinto-Silva RA 2004. Magnetic resonance imaging and ultrasound in hepatosplenic schistosomiasis mansoni. Rev Soc Bras Med Trop 37: 333-337.
- Massoud AM, Ghoneem M, Massoud M 1986. Effect of oxamniquine and praziquantel on intrasplenic pressure and portal vein diameter in hepatosplenic schistosomiasis. J Egypt Soc Parasitol 16: 427-37.
- Patel AS, Castillo DF, Hibbeln JF, Watkins JL 1993. Magnetic resonance imaging appearance of hepatic schistosomiasis, with ultrasound and computed tomography correlation. Am J Gastroenterol 88: 113-116.
- Pinto-Silva RA, Abrantes WL, Antunes CM, Lambertucci JR 1994. Sonographic features of portal hypertension in schistosomiasis mansoni. Rev Inst Med Trop São Paulo 36: 355-361.
- Prata A 2002. Esquistossomose mansoni. In R Veronesi, R Focaccia (eds), Tratado de Infectologia, 2nd ed., v. 2, Atheneu, São Paulo, p. 1374-1392.
- Prata A, Andrade ZA 1963. Fibrose hepática de Symmers sem esplenomegalia. O Hospital 63: 617-623.
- Richter J, Domingues ALC, Barata CH, Prata AR, Lambertucci JR 2001. Report on the second satellite symposium on ultrasound in schistosomiasis. Mem Inst Oswaldo Cruz 96: 151-156.
- Sullivan S, Williams R 1976. Reliability of clinical techniques for detecting splenic enlargement. Brit Med J 2: 1043-1044.
- Willemsen UF, Pfluger TH, Zoller WG, Kueffer G, Hahn K 1995. MRI of hepatic schistosomiasis mansoni. J Comput Assit Tomogr 19: 811-813.
Publication Dates
-
Publication in this collection
12 Feb 2007 -
Date of issue
Oct 2006
History
-
Accepted
26 June 2006 -
Received
25 May 2006