Abstracts
There is increasing interest in the early years as a focus for reducing health inequalities as well as one that is important for the children themselves. This paper describes the introduction in England of Sure Start Local Programmes, which included home visiting within a community development approach, and an intensive home visiting programme, the Nurse-Family partnership, for disadvantaged teenage mothers. It reflects on changes and challenges in service provision to mothers and their pre-school children in England, explaining that a long tradition of home visiting was, paradoxically, reduced as attention focused on the newer initiatives. This is now being addressed, with attention to a range of evidence based programmes and a specific focus on heath visitor provision.
Child care; Child health; Home visit; Health inequalities
Há um crescente interesse, nos últimos anos, objetivando reduzir as desigualdades na área da saúde, bem como uma desigualdade específica infantil. Este artigo descreve a introdução, na Inglaterra, de programas locais chamados Sure Start, que incluem visitação domiciliar, dentro de uma abordagem de desenvolvimento da comunidade, e um programa intensivo de visitas domiciliares, a parceria com a Nurse-Family, para mães adolescentes em condições desfavoráveis. Isso reflete nas mudanças e desafios da provisão de serviço as mães e filhos em idade pré-escolar, na Inglaterra, explicando que uma longa tradição de visitas domiciliares foi, paradoxalmente, reduzida, conforme a atenção concentrava-se em novas iniciativas. Isso está sendo, agora, tratado, atentando para uma variedade de evidências com base nos programas e com um foco específico na provisão de visitantes da área da saúde.
Cuidado da criança; Saúde da criança; Visita domiciliar; Desigualdades em saúde
Existe un creciente interés en los años tempranos de la infancia para reducir inequidades de salud, tratándose de algo de alto impacto para los propios niños. Este artículo describe la introducción en Inglaterra de los Sure Start Local Programmes (Programas Locales de Inicio Seguro), los cuales incluyen visitas domiciliarias insertas en una aproximación al desarrollo comunitario, y un programa intensivo de visitas, el Nurse-Family partnership (Asociación Enfermera-Familia), para madres adolescentes en situación desventajosa. Se reflexiona acerca de cambios y desafíos en provisión de atención a madres y sus hijos en edad preescolar en Inglaterra, explicando que una larga tradición en visitas domiciliarias fue reducida, paradójicamente, por enfocarse la atención en las iniciativas más actuales. Todo esto está siendo direccionado, atendiendo a una serie de programas basados en la evidencia y a un foco específico en la percepción del visitante de campo.
Cuidado del niño; Salud del niño; Visita domiciliaria; Desigualdades en la salud
REFLECTION
Home visitors and child health in England: advances and challenges
Visitadores domiciliares e saúde infantil na Inglaterra: avanços e desafios
Visitantes domiciliarios y salud infantil en Inglaterra: avances y desafíos
Sarah Cowley
Nurse. Professor of Community Practice Development, Florence Nightingale School of Nursing and Midwifery King's College London. sarah.cowley@kcl.ac.uk
Correspondence addressed to Correspondence addressed to: Sara Cowely 27 Swiss Avenue City: Chelmsford Zip Code: CM1 2AD Essex - UK - Reino Unido
ABSTRACT
There is increasing interest in the early years as a focus for reducing health inequalities as well as one that is important for the children themselves. This paper describes the introduction in England of Sure Start Local Programmes, which included home visiting within a community development approach, and an intensive home visiting programme, the Nurse-Family partnership, for disadvantaged teenage mothers. It reflects on changes and challenges in service provision to mothers and their pre-school children in England, explaining that a long tradition of home visiting was, paradoxically, reduced as attention focused on the newer initiatives. This is now being addressed, with attention to a range of evidence based programmes and a specific focus on heath visitor provision.
Descriptors: Child care; Child health; Home visit; Health inequalities
RESUMO
Há um crescente interesse, nos últimos anos, objetivando reduzir as desigualdades na área da saúde, bem como uma desigualdade específica infantil. Este artigo descreve a introdução, na Inglaterra, de programas locais chamados Sure Start, que incluem visitação domiciliar, dentro de uma abordagem de desenvolvimento da comunidade, e um programa intensivo de visitas domiciliares, a parceria com a Nurse-Family, para mães adolescentes em condições desfavoráveis. Isso reflete nas mudanças e desafios da provisão de serviço as mães e filhos em idade pré-escolar, na Inglaterra, explicando que uma longa tradição de visitas domiciliares foi, paradoxalmente, reduzida, conforme a atenção concentrava-se em novas iniciativas. Isso está sendo, agora, tratado, atentando para uma variedade de evidências com base nos programas e com um foco específico na provisão de visitantes da área da saúde.
Descritores: Cuidado da criança; Saúde da criança; Visita domiciliar; Desigualdades em saúde
RESUMEN
Existe un creciente interés en los años tempranos de la infancia para reducir inequidades de salud, tratándose de algo de alto impacto para los propios niños. Este artículo describe la introducción en Inglaterra de los Sure Start Local Programmes (Programas Locales de Inicio Seguro), los cuales incluyen visitas domiciliarias insertas en una aproximación al desarrollo comunitario, y un programa intensivo de visitas, el Nurse-Family partnership (Asociación Enfermera-Familia), para madres adolescentes en situación desventajosa. Se reflexiona acerca de cambios y desafíos en provisión de atención a madres y sus hijos en edad preescolar en Inglaterra, explicando que una larga tradición en visitas domiciliarias fue reducida, paradójicamente, por enfocarse la atención en las iniciativas más actuales. Todo esto está siendo direccionado, atendiendo a una serie de programas basados en la evidencia y a un foco específico en la percepción del visitante de campo.
Descriptores: Cuidado del niño; Salud del niño; Visita domiciliaria; Desigualdades en la salud
INTRODUCTION
Child health has risen higher on the political agenda over the last two decades, largely as a result of scientific advances in two fields, which both emphasise the early years. First, there has been an exponential increase in understanding about neurological and genetic development during pregnancy and the very early weeks and months of life. This has brought about a realisation that an infant's future physical and mental health, as well as their social and cognitive development and later economic position in life, is strongly affected by the way he or she is fed, nurtured and cared for during this critical period(1).
Second, this knowledge of the early years has influenced understanding of the interactions across the lifecourse of social determinants on health and health inequalities(2). There is a growing realisation that the social determinants and health inequalities are important to the whole population, not only those experiencing the worst conditions and poverty(3). This is particularly the case in countries, including both Brazil and England, which have passed what has been called the epidemiological transition' where long term conditions (cancer, heart and circulatory disease, diabetes, mental health problems) are more prevalent and the cause of more deaths than those from infectious diseases(4). Lack of food, shelter and access to adequate medical care explains inequalities in countries where malnutrition and infectious disease are the major causes of death. Once those basic requirements are met, differences in income no longer explain major differences in mortality or morbidity across social groups: nor, as Wilkinson put it, does having one fewer car to wash at the weekend, or a smaller lawn to mow, provide a plausible explanation for different levels of mortality across the entire social spectrum(5)
Britain is amongst the most unequal of developed countries and a recent review(6) identified examples to illustrate the way inequalities show across a gradient encompassing the whole population. This gradient is clearly seen in Figure 1, which shows deaths that would be avoided among infants born in England and Wales in 2005-6, if they all had the same chance of survival as those in the highest quintile(7). Infants in the worst off 20% are most likely to be affected, but the gradient runs from bottom to top. Figure 2 shows the gradient in issues related to school readiness and young children's capacity to learn, including birth weight, maternal post-natal depression, child being read to every day and regular bedtimes(8).
In both examples, the differences are most stark between the top and the bottom, but they run through the whole population, so that each socio-economic step, up or down, affects the child's life chances. Infants who reach school less able to learn, are then disadvantaged throughout their school years, then more likely to become involved with criminal justice systems or be at risk of experiencing violence or being violent in their teens, more likely to engage in risky behaviour like smoking, drug and alcohol misuse, less likely to obtain gainful employment and therefore to be in the lower social group that is likely to die young. Along the way, they will have children who enter the same cycle of missed opportunities and poor health chances, in the absence of intervention to change the situation.
Targeted interventions
Evidence about potentially effective interventions initially emphasised the importance of targeting those who were worst off, and also highlighted home visiting as a useful way to deliver programmes(9-10). The then New Labour government invested huge sums of money in Sure Start Local Programmes (SSLPs), which ran for around 10 years from 1999, with a view to improving the life chances for children living in disadvantaged areas(11). SSLPs were based on ideas of community development, but also included a home visiting component. Each local area was encouraged to plan the kind of service that would help children in their area and to bid for funds to develop it, so each local programme was unique, although there were key principles that had to be met and a clear, centrally-driven, framework of performance management to drive forward the multi-agency activity(12).
The huge variability between local programmes was a major challenge for evaluation, but a quasi-experimental approach was developed, to compare children in Sure Start areas with those in the longitudinal Millenium Cohort Study. At first, differences between Sure Start children and those in the matched areas seemed minimal(13), but gradually improvements(14). Sure Start has been considered generally successful, particularly where the local programmes were led by the health sector, a difference attributed to better engagement in these areas with the pre-existing health visiting service, because of their knowledge of local needs and the local population, and their ability to carry out the home visits in a way that engaged the mothers in the Sure Start programme.
However, a major criticism and challenge was the fact that the most needy and deprived families seemed not to make full use of the Sure Start Local Programmes, possibly becoming even more disadvantaged as a result, in comparison with their neighbours(13). The Nurse-Family Partnership intensive home visiting programme was seen as the solution to this problem and it was implemented after 2007, being funded, managed and run directly from central government(15). It was relabeled the Family-Nurse Partnership (FNP), ostensibly to place interest in families first, and focused upon unmarried, first time teenaged mothers, as this group encompasses a large proportion of the most needy and excluded families who had shunned the SSLPs.
Evidence base comes from three trials of his programme, which is fully manualised and clearly structured, with frequent (weekly to fortnightly) home visits from early pregnancy until the child is two years old(15). All three trials show benefits for mothers and children, and despite the heavy initial outlay, the consistently positive results lead to a convincing cost-benefit overall, based on a fifteen year follow up of the first cohort. Each FNP nurse visitor has a caseload of 25 families, and requires continuing support in the form of clinical supervision and training, which is managed from a central government department to ensure consistency and fidelity to the programme.
The third trial compared delivery of the programme by professionals, who were nurses with additional training, and by paraprofessionals who had the same programme-specific training, but who did not start out with professional education(16). Results for families who received the programme from the paraprofessionals were far less effective, being only about half as good in most instances as those who received it from the professionals. Many of the long-term benefits are derived from avoidance of the criminal justice system, which also accounts for much of the economic benefit(17). A large trial is underway, to assess whether the programme delivers the same level of benefit in England as that found in the original, in the USA.
Universal services
Whilst these two major initiatives were being developed, less attention was paid to the pre-existing services for pre-school children. In England, health visitors have traditionally provided a proactive, universal child and family public health service, which is essentially preventive in nature. The service has been in existence for 150 years and has always used a combination of home visiting and different forms of community outreach, like group or community development activities. It is similar to community or public health nursing, or child and family health nursing in other countries, and operates in conjunction with the midwifery service, which is concerned with pregnancy and birth. Both health visitors and midwives are funded from national taxation and delivered through the National Health Service, which are free at point of delivery. However, between 2000 and 2010, whilst SSLPs and FNP sites flourished, there was a fall of around 20% in the number of health visitors employed 10,046 to 8125 full time equivalents, being approximately one health visitor per 7500 population, or 85 new births per year(18).
In a bid to clarify the function and purpose of health visitors, the government-sponsored Healthy Child Programme (HCP) was updated(19). That guidance takes account of the evidence about infant neurodevelopment and the increasing knowledge about activities that support parenting and help to promote healthy development. It focused on effective interventions identified in a large review of reviews and introduced the idea of progressive universalism, suggesting that everyone needs some support, but that more should be available for those in greatest need(20).
There is increasing awareness within the scientific world that, however excellent they are, highly targeted and selective programmes will not reduce health inequalities, because they can only reach the tip of the iceberg of need. Health needs are distributed throughout the population, and the majority of cases are likely to be found outside selected groups or areas, because of the greater numbers in the general population(21) . Bearing this in mind, called for what he dubbed a second revolution in the early years, which would involve increasing the proportion of overall expenditure allocated for this age group, and to focus attention proportionately across the social gradient to ensure effective support to all new parents(6). He used the phrase proportionate universalism, which describes the complexity of these activities more accurately than the linear continuum implied in the term progressive universalism.
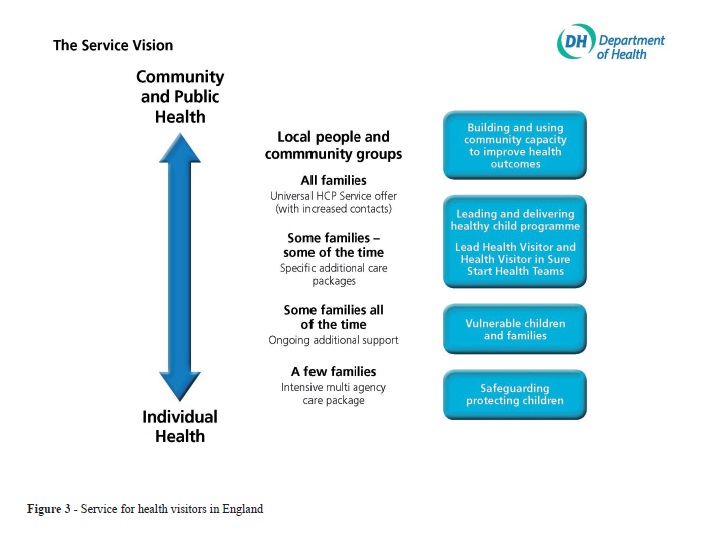
Faced with this evidence, and the sharp downturn in provision of health visitors who had previously delivered the universal service, the new Coalition government in 2010 embarked upon a programme to restore and reinvigorate health visiting(22). They set out a new service vision, which cannot be delivered within current existing resources, but which will be developed over the next four years, as new staff qualify and come on stream (Figure 3)(23).
The whole service is set within a multi-agency, community-wide context and the way health visitors operate across communities, families and individuals is summarised in the four straightforward descriptions. These aim to make a very complex service understandable by everyone, including the families who use the services, stating that:
-
all families get some universal support, particularly at the start of life around breast feeding, early attachment and early development
-
specific additional care packages are available for help with everyday problems such as for behaviour problems, crying babies, feeding queries and health worries, that is for
some families some of the time,
-
some families have an ongoing need for support, particularly if they are vulnerable for any reason, or where a child has long term condition or disability, that is
some people all of the time
-
for a
few all of the time who are the extremely vulnerable families, there is the kind of intensive service provided by the FNP
Strengthening all provision
Call for both universal and targeted services is a new challenge, which should avoid the potentially negative effect of concentrating on either one type of provision or another(6). However, achieving this requires evaluators to concentrate on developing the context, or service setting, for programmes, as well as the programmes themselves. An example of one such initiative is the recently developed maternal and early childhood sustained home visiting (MECSH) programme, developed in Australia(24). The MECSH programme, which was trialled in a deprived suburb of Sydney, aims to shift the curve of health inequalities by targeting the worst-off 20%, including multiparous women, not just first time mothers. This brings a sustained home visiting programme to a far larger and more heterogeneous group than that targeted by the nurse-family partnership programme, and results of the initial trial were equally impressive(15,24).
MECSH was designed to capitalise on what is known about successful home visiting programmes(10,25) allowing sufficient intensity and duration (from pregnancy until the child is 2 years old), and focusing on parent and child. To encompass the range of needs encountered, it is broad based and multi-faceted, and also aims to exploit and integrate with any resources available in the wider community(24). As well as home visiting, the programme includes group activities for MECSH families, and encourages engagement with and referral to other services, assisting and facilitating the transition of families as their involvement in the MECSH programme comes to an end.
Early childhood services in England and Australia are similar in many respects, but there are some key differences. MECSH was explicitly designed to make use of the highly skilled Australian child and family health nurses, who are all trained in strengths-based practice using the family partnership model(26). In England, not all health visitors have this training. Also, MECSH needs to be integrated with the existing general resource system, which in England include Sure Start Children's Centres and the Family Nurse Partnership pilot sites, which differ from provision in Australia. So, transfer and implementation requires initial service mapping and piloting, which is underway before a full trial and wider implementation of the full MECSH programme. Instead of viewing these differences and requirements as a barrier, they are being used as an opportunity to develop new services across the spectrum of need, in line with the new service vision for health visiting(23).
CONCLUSION
It is both an exciting and a daunting time for anyone interested in child health and health inequalities. Global economic conditions threaten to create new waves of social injustice and future challenges across the world. Yet, we have an opportunity to ameliorate these threats, because of the increasing knowledge about how early life conditions affect later health and resilience, and also about the forms of service provision and programmes that can help to change those early life conditions, for the sake of future generations.
Recebido: 30/10/2011
Aprovado: 29/11/2011
-
1Harvard University. Center on the Developing Child; National Scientific Council on the Developing Child. National Forum on Early Childhood Policy and Programs. The foundations of lifelong health are built in early childhood [Internet]. Cambridge; 2010 [cited 2011 Nov 21]. Available from: http://developingchild.harvard.edu/resources/reports_and_working_papers/foundations-of-lifelong-health/
- 2. Graham H, Power C. Childhood disadvantage and health inequalities: a framework for policy based on lifecourse research. Child Care Health Dev. 2004;30(6):671-8.
- 3. Wilkinson R, Marmot M. Social determinants of health: the solid facts. Denmark: WHO Regional Office for Europe; 2003.
- 4. Wilkinson R. Unhealthy societies: the afflictions of health inequality. London: Routledge; 1996.
- 5. Wilkinson R. The impact of inequality: empirical evidence. Renewal. 2006;14(1):20-6.
- 6. Marmot M. Strategic review of health inequalities in England post-2010: the Marmot Review [Internet]. London; 2010 [cited 2011 Nov 24]. Available from: http://www.instituteofhealthequity.org/projects/fair-society-healthy-lives-the-marmot-review
- 7. Oakley L, Maconochie N, Doyle P, Dattani N, Moser K. Multivariate analysis of infant death in England and Wales in 2005-6, with focus on socioeconomic status and deprivation. Health Statist Quart. 2009;42(1):22-39.
- 8. Goodman A, Gregg P. Poorer children's educational attainment: how important are attitudes and behaviours. New York: Joseph Rowntree Foundation; 2010.
- 9. Karoly LA, Kilburn MR, Cannon JS. Early childhood interventions: proven results, future promise. Santa Monica: Rand Corporation; 2005.
-
10Harvard University. Center on the Developing Child; National Scientic Council on the Developing Child. National Forum on Early Childhood Policy and Programs. A science-based framework for early childhood policy: using evidence to improve outcomes in learning, behavior, and health for vulnerable children [Internet]. Cambridge; 2007 [cited 2011 Nov 24]. Available from: http://developingchild.harvard.edu/resources/reports_and_working_papers/policy_framework/
- 11. Glass N. Sure start: the development of an early intervention programme for young children in the United Kingdom. Children Soc. 1999;13(2):257-64.
- 12. Bagley C, Ackerley CL, Rattray J. Documents and debates Social exclusion, sure start and organizational social capital: evaluating inter-disciplinary multi-agency working in an education and health work programme. J Educ Policy. 2004;19(5):595-607.
- 13. Belsky J, Melhuish E, Barnes J, Leyland AH, Romaniuk H. Effects of Sure Start Local Programmes on children and families from a quasi-experimental, cross-sectional study. BMJ. 2006;332(7556):1476-8.
- 14. Melhuish E, Belsky J, Leyland AH, Barnes J; National Evaluation of Sure Start Research Team. Effects of fully-established Sure Start Local Programmes on 3-year-old children and their families living in England: a quasi-experimental observational study. Lancet. 2008;372(9650):1641-7.
- 15. Olds DL. The nurse-family partnership: an evidence based preventive intervention. Infant Mental Health J. 2006;27(1):5-25.
- 16. Olds DL, Robinson J, O'Brien R, Luckey DW, Pettitt LM, Henderson CR Jr, et al. Home visiting by nurses and by paraprofessionals: a randomized controlled trial. Pediatrics. 2002;110(3):486-96.
- 17. Olds D, Henderson CR Jr, Cole R, Eckenrode J, Kitzman H, Luckey D, et al. Long-term effects of nurse home visitation on children's criminal and antisocial behavior: 15-year follow-up of a randomized trial. JAMA. 1998;280(14):1238-44.
- 18. United Kingdom. The Health and Social Care Information Centre. NHS Hospital and Community Health Services Non-Medical Staff England 2010. London: Department of Health; 2010.
- 19. United Kingdom. Department of Health; Department for Children, Schools and Families. The Health Child Programme: pregnancy and the first five years of life. London: Department of Health; 2009.
- 20. Barlow J, Schrader McMillan A, Kirkpatrick S, Ghate D, Smith M, Barnes J. Health-led parenting interventions in pregnancy and the early years. London: Department for Children, Schools and Families; 2008.
- 21. Rose G. Rose's strategy of preventive medicine. Oxford: Oxford University Press; 2008.
- 22. United Kingdom. Department of Health. Health Visitor Implementation Plan 2011-2015: a call to action. London: Department of Health; 2011a.
- 23. United Kingdom. Department of Health. Service vision for health visiting in England. London: Department of Health; 2011b
- 24. Kemp L, Harris E, McMahon C, Matthey S, Vimpani G, Anderson T, et al. Child and family outcomes of a long-term nurse home visitation program: a randomised controlled trial. Arch Dis Child. 2011;96(6):533-40.
- 25. Macleod J, Nelson G. Programs for the promotion of family wellness and the prevention of child maltreatment: a meta-analytic review. Child Abuse Negl. 2000;24(9):1127-49.
- 26. Davis H, Day C. Working in partnership: the family partnership model. London: Pearson Education; 2010.
Correspondence addressed to:
Publication Dates
-
Publication in this collection
04 May 2012 -
Date of issue
Dec 2011
History
-
Received
30 Oct 2011 -
Accepted
29 Nov 2011