Abstracts
The purpose of this study was to assess the nursing workload at admission to and discharge from intensive care of three groups of patients (i.e., acute coronary syndrome, acute respiratory failure, and sepsis). A prospective, descriptive study was performed over a 27-month period and included 563 patients. The workload was assessed using the Nursing Activities Score scale. Significant differences in the workload were determined on the days of admission and discharge: the workload was higher in both cases for patients with acute respiratory failure and sepsis compared with patients diagnosed with acute coronary syndrome. This difference was maintained over the first seven days of their hospital stay. From day 8 on, the difference disappeared, and a workload balance was achieved in the three groups. Good staffing requires adequate tools for measuring care needs and understanding the workload required in the groups of patients who are most frequently admitted to intensive care.
Workload; Intensive care; Nursing staff, hospital
Se objetivó valorizar la carga de trabajo al ingreso y al alta en tres grupos de pacientes (síndrome coronario agudo, insuficiencia respiratoria aguda y sepsis) en terapia intensiva. Estudio descriptivo, prospectivo, de 27 meses, incluyéndose 563 pacientes, valorando carga de trabajo según Nursing Activities Score. Existieron diferencias significativas en la carga de trabajo al ingreso y en el alta entre los grupos de pacientes, siendo superior en ambos momentos la de pacientes con insuficiencia respiratoria aguda y sepsis frente a pacientes coronarios. Durante los siete primeros días de estancia se mantuvo esta diferencia, desapareciendo a partir del octavo día, equilibrándose la carga de trabajo para los tres grupos. Para conseguir una adecuada dotación de personal es fundamental contar con instrumentos para medir las necesidades de cuidados y conocer la carga de trabajo de los distintos grupos de enfermos que ingresan con mayor frecuencia en las unidades de terapia intensiva.
Carga de trabajo; Cuidados intensivos; Personal de enfermería en hospital
O objetivo deste estudo foi avaliar a carga de trabalho na admissão e alta dos pacientes de três grupos (síndrome coronária aguda, insuficiência respiratória aguda e sepsis) em cuidados intensivos. Trata-se de estudo prospectivo, descritivo, que decorreu durante 27 meses, incluindo 563 pacientes. Para a avaliação da carga de trabalho utilizou-se a escala Nursing Activities Score. A partir dos resultados do estudo parecem existir diferenças significativas na carga de trabalho no dia da admissão e alta entre os grupos de pacientes, sendo a carga maior em ambos os tempos a dos pacientes com insuficiência respiratória aguda e sepsis. Durante os primeiros sete dias de internamento essa diferença manteve-se, desaparecendo no oitavo dia, o que equilibrou a carga de trabalho para os três grupos. Conclui-se que para se conseguir os recursos adequados é essencial dispor de instrumentos para medir as necessidades de cuidados e conhecer a carga de trabalho dos diferentes grupos de pacientes que passam com mais frequência pelas unidades de cuidados intensivos.
Carga de trabalho; Terapia intensiva; Recursos humanos de enfermagem no hospital
ORIGINAL ARTICLE
Assessment of nursing workload in three groups of patients in a Spanish ICU using the Nursing Activities Score scale
Carga de trabajo en tres grupos de pacientes de UTI Española según Nursing Activities Score
Francisco Javier Carmona-MongeI; Ana Jara-PérezII; Cristina Quirós-HerranzIII; Gloria Rollán-RodríguezIV; Isabel Cerrillo-GonzálezV; Sonia García-GómezVI; Montserrat Martínez-LareoVII; Dolores Marín-MoralesVIII
INurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Associate Professor, Nursing Department, Universidad Rey Juan Carlos. Alcorcón, Madrid, Spain. javier.carmona@urjc.es
IINurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Alcorcón, Madrid, Spain. ajara@fhalcorcon.es
IIINurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Alcorcón, Madrid, Spain. cquiros@fhalcorcon.es
IVNurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Alcorcón, Madrid, Spain. gmrollan@fhalcorcon.es
VNurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Alcorcón, Madrid, Spain. icerrillog@fhalcorcon.es
VINurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón. Alcorcón, Madrid, Spain. sgarciag@fhalcorcon.es
VIINurse, Critical Care Unit, Hospital Universitario Fundación Alcorcón, Madrid, Spain. mmartinezl@fhalcorcon.es
VIIIAssociate Professor, Nursing Department, Universidad Rey Juan Carlos. Alcorcón, Madrid, Spain. dolores.marin@urjc.es
Correspondence addressed to
ABSTRACT
The purpose of this study was to assess the nursing workload at admission to and discharge from intensive care of three groups of patients (i.e., acute coronary syndrome, acute respiratory failure, and sepsis). A prospective, descriptive study was performed over a 27-month period and included 563 patients. The workload was assessed using the Nursing Activities Score scale. Significant differences in the workload were determined on the days of admission and discharge: the workload was higher in both cases for patients with acute respiratory failure and sepsis compared with patients diagnosed with acute coronary syndrome. This difference was maintained over the first seven days of their hospital stay. From day 8 on, the difference disappeared, and a workload balance was achieved in the three groups. Good staffing requires adequate tools for measuring care needs and understanding the workload required in the groups of patients who are most frequently admitted to intensive care.
Descriptors: Workload; Intensive care; Nursing staff, hospital
RESUMEN
Se objetivó valorizar la carga de trabajo al ingreso y al alta en tres grupos de pacientes (síndrome coronario agudo, insuficiencia respiratoria aguda y sepsis) en terapia intensiva. Estudio descriptivo, prospectivo, de 27 meses, incluyéndose 563 pacientes, valorando carga de trabajo según Nursing Activities Score. Existieron diferencias significativas en la carga de trabajo al ingreso yen el alta entre los grupos de pacientes, siendo superior en ambos momentos la de pacientes con insuficiencia respiratoria aguda y sepsis frente a pacientes coronarios. Durante los siete primeros días de estancia se mantuvo esta diferencia, desapareciendo a partir del octavo día,equilibrándose la carga de trabajo para los tres grupos. Para conseguir una adecuada dotación de personal es fundamental contar con instrumentos para medir las necesidades de cuidados y conocer la carga de trabajo de los distintos grupos de enfermos que ingresan con mayor frecuencia en las unidades de terapia intensiva.
Descriptores: Carga de trabajo; Cuidados intensivos; Personal de enfermería en hospital
INTRODUCTION
Advances in the treatment of critical diseases in recent years have changed the types of patients admitted in critical care units. There are more therapeutic options for replacing the vital functions of various organs and systems in the human body and for maintaining these functions until the cause of the disorder disappears. Treatment and care create high hospitalization expenses, partially because of the treatments per se but also because of the large number of employees required for these services. Furthermore, because of the complexity of these treatments, patients admitted to Intensive Care Units (ICUs) require increased care. Determining the precise needs of the nursing staff for these highly specialized services is essential to ensure quality nursing care and thus avoid the occurrence of adverse events associated with health care.
Different international organizations note the relevance of having the appropriate nursing staff when attempting to increase patient safety and consequently reduce the potential complications associated with health care(1). Various studies have shown that an adequate number of nurses for the types of patients admitted to the ICU has a positive effect and results in a reduction of hospital-acquired infections, number of skin lesions, time on mechanical ventilation, and stay in the intensive care unit(2-6).
Nursing workload is a fundamental element of establishing the needs of the staff in a specific unit. Over the past 30 years, there have been attempts to measure the real needs of nurses in ICUs. Initially, indirect measuring instruments derived from medical scales were developed. These first tools assessed nursing workload as a result of implementing a series of therapeutic interventions on the patient. However, these scales have many limitations because they do not assess the amount of nursing care administered during routine patient attention that does not originate directly from the therapeutic interventions/treatments(7). The Nursing Activities Score (NAS) scale was developed to try to resolve this(8). This scale consists of 23 items that assess the activities and care that nurses provide to critical patients. Each item has an assigned value, and the total score is the sum of all of the values. The total score represents the percentage of time a nurse spends in direct care of the patient over a 24-hour period of ICU stay. Thus, a total score of 100% indicates the amount of work a nurse can do over a 24-hour period. The sum of the values from the 23 items on the scale can range from 0% to 177%(9).
Several studies using the NAS scale have been conducted, most of them to determine the difference between actual nurse staffing and that estimated by the scale(10-13). Similarly, other studies have compared the values obtained using this scale and the values obtained using other assessment scales regarding the workload in the ICU, such as the Nine Equivalents of Nursing Manpower Use Score (NEMS) or the Therapeutic Intervention Scoring System-28 (TISS-28). The NAS scale provided greater accuracy in assessing the workload(14).
No studies have been found in the literature assessing the workload of nurses while taking care of different sub-groups of patients (different diagnoses at admission to the unit) or assessing the evolution of the workload from the admission day of these patients to the unit. The purpose of this study is to identify differences in the workload at admission and discharge in three groups of patients with the highest percentage of admissions to our unit: acute coronary syndrome (ACS), acute respiratory failure (ARF), and sepsis. The workload in each of these groups for a period of 30 days is also assessed to determine whether there are differences between groups.
METHODS
Design and Setting
A prospective, descriptive study was performed over a 27-month period (October 2007 December 2009). The study was conducted in a university hospital of the Community of Madrid with 450 beds (Spain). Data collection was conducted in the 12-bed adult medical ICU. Most admissions to this unit were because of a medical pathology, and a small percentage of patients were postoperative. The nurse-to-patient-ratio on all shifts was 1:2 or 1:3. The nursing staff worked 12-hour shifts.
Participants
Included in the study were patients admitted to the ICU who were at least 18 years of age,had a minimum hospital stay of 24 hours, and were diagnosed at admission with acute coronary syndrome (ACS), acute respiratory failure (ARF), or sepsis. Of the 913 patients admitted to the unit over the study period, 563 made up the study sample.
Data Collection
Demographic and clinical data of the patients were obtained during the study period. Furthermore, workload information was collected on a daily basis for each of the patients admitted to the unit using the Nursing Activities Score (NAS) scale. Data collection was performed every day at seven o´clock in the morning; all information from the 24 hours prior to the patient´s admission to the unit was also gathered. The NAS scale consists of 23 items that assess the routine activities performed by the nurses while caring for critical patients. Each item has an assigned weight that assesses the amount of time required to perform certain activities during patient care. The scores represent a percentage of the time the nursing staff employ in performing the activities included in the tool over a 24-hour period. Summing the values of the items provides the total time that nurses spend in the ICU performing these tasks on a specific day. The results indicate that the NAS can specify what is being done for 81% of the time that nurses spend in the ICU.
Follow-up of the patients was performed throughout their stay in the unit. However, to analyze the workload differences among the three groups of patients, only the data from the first 30 days of their stays in the unit were used. To analyze the workload differences between patient admission and patient discharge, all patients were included, even if their stay in the unit were longer than 30 days.
The Ethics and Research Committee of the center approved the project (09/68).
Data analysis
Data were analyzed using the Statistical Package for the Social Sciences (SPSS) version 16.0 for Windows (SPSS Inc., Chicago, IL) and are presented as the means (standard deviation) or median (25th percentile - 75th percentile), depending on variable characteristics. One-factor ANOVA was used to analyze the correlation between admission diagnosis and nursing workload as well as the differences between workload at admission and at discharge, using Scheffé's method for post hoc comparisons. Eta-squared was used to measure the effect size. All p values < 0.05 were considered significant (bilateral).
RESULTS
During the study period, 563 admissions met the inclusion criteria; 5704 measurements were obtained using the NAS scale. The mean daily number of patients in the unit was 10.4 (SD = 2.2); bed occupancy during the study period was 91.2%.
Regarding the study sample, most patients were male (72.5%; n = 408), with a mean age of 62.5 years (SD = 14.0). The main cause for admission was coronary disease (58.1%; n = 327), followed by ARF (34.1%; n = 192) and sepsis (7.8%; n = 44). The median stay in the ICU was 3.6 days (2.2 8.2) and ranged between 1 and 139 days. The number of patients in each group admitted to the unit for a period of 30 days is shown in Figure 1. From the 503 studied patients, most were discharged to a conventional ward in the hospital (88.8%; n = 500), 52 patients died during their stay in the ICU (9.2%), and 11 patients were transferred to another center to receive the appropriate treatment for their disease (2.0%). The remaining characteristics of the study sample are shown in Table 1.
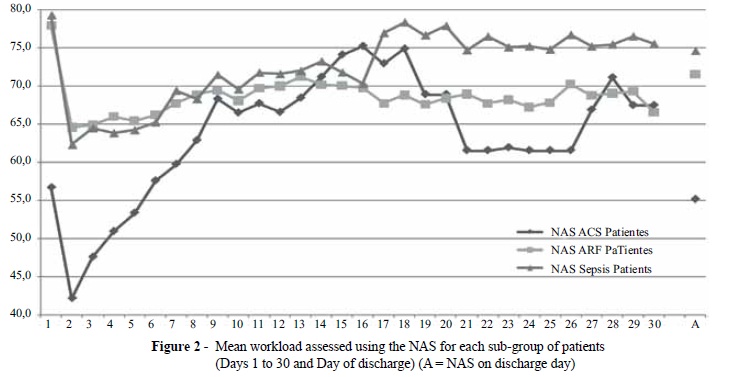
Mean daily workloads on admission and discharge days were analyzed, as was the mean workload during the admission of patients with ACS, patients with ARF, and patients with sepsis. A one-factor ANOVA was used for these analyses. Significant differences were determined for the three assessed variables (Figure 2). On the admission day, the workload for patients with ACS was 56.7 (DT = 9.9); for patients with ARF, the workload was 77.6 (DT = 16.1); and for patients diagnosed with sepsis, the result was 79.2 (SD = 17.9) (F(2, 554) = 179.7; p < .01; ηp2 = .393). Significant differences were observed between the patients with ACS or sepsis and the patients with ARF in the post-hoc analysis. This difference was maintained at discharge; the mean score obtained with the NAS for patients with ACS was 43.0 (SD = 21.0), 55.3 (SD = 15.2) for patients with ARF, and 57.0 (SD = 19.5) for patients with sepsis (F(2, 553) = 29.7; p < .01; ηp2 = .096). Similarly, significant differences were determined between patients with ACS and patients with ARF and sepsis in post-hoc analysis.
Next, the workload over a 30-day follow-up period for each of the indicated diagnostic categories was analyzed (Figures 1 and 2). Another one-factor ANOVA was conducted to compare the mean daily workload for each subgroup of patients. Significant differences were determined from days 1 to 7 post-admission (p < 0.01), and the values were lower for patients with ACS compared with patients with ARF or sepsis; no differences were determined between these two last sub-groups in the post-hoc analysis. From day 8 post-admission and until day 30, no significant differences were observed between the workload and the different types of patients, although the nursing workload for septic patients was higher compared with the other two groups during the 30 analyzed days.
DISCUSSION
The scores from the NAS scale in the three sub-groups of patients with different diagnosed diseases provide information regarding the nursing staffing needs of the groups. This information should be helpful in planning the workforce required in critical care units that admit patients with characteristics similar to the studied sample(15).
First, the workload with ACS patients is lower than that for patients diagnosed with ARF or sepsis. This lower workload is usually reflected during workforce planning; nurse-to-patient ratios are higher in coronary care units than in medical ICU units. A relevant observation in this study is that these differences in workload disappear after day 7 post-admission to the unit. This situation is expected because the care needs of a patient with ACS with a certain degree of complication (i.e., those who will stay in the ICU for longer periods) are similar to those of a patient with ARF or sepsis. These requirements should be considered when calculating staffing for shifts in medical ICUs; both the number of coronary patients who are being admitted to the unit and the number of patients with some type of complication (staying more than 7 days in the unit) are required. A more realistic assessment of the required nursing staff will be possible with this information.
Conversely, the workload at discharge was medium-high for patients with ARF and sepsis. These patients are sent to a conventional care unit and have high care needs. Although their stay in the ICU may not be justified, their needs can be excessive for the staff in a conventional ward because of higher nurse-to-patient ratios on conventional wards.Other studies have previously shown the need for intermediate care units for patients who suffer from a critical disease as an additional step before sending such patients to a conventional ward. The workload results at discharge in this group of patients again reveal the usefulness of units for patients requiring high-intensity care but low-intensity medical treatment(16-17).
The score for the global workload in our sample was 65.9 points, which is quite similar to the score obtained for ICU patients in Brazil (mean NAS of 63.7).(13) This result indicates that for each of the 12-hour shifts in the unit, each of the patients requires a total of 7.91 hours of direct nursing care, which is in line with the results in other studies. Adjustments in the nursing staff have not been evaluated here. However, in other studies in which the NAS scale was applied, overstaffing was determined.
There are some limitations to this study, such as the fact that the data were collected only in one unit. Because of the characteristics of the unit, the workload for post-surgical patients was not assessed. In other studies, the NAS scores for these patients are quite high during the first days of an ICU stay.
CONCLUSIONS
Appropriate staffing in ICUs is essential to ensure quality care for critical patients. Such staffing will increase the patients' safety and reduce the risk of adverse events that may occur while staying in the unit. To achieve adequate staffing, tools to measure the care needs of the patients are necessary, as is knowledge of the workload required for the different groups of patients who are most frequently admitted to these units.
This first analysis of the workload in different sub-groups of patients has provided NAS scores for patients with ACS, ARF, and sepsis. A priori, the workload for coronary patients is lower compared with the other two studied groups. However, when the stay of coronary patients is extended, the workload is comparable to that of any other critical patient, which should be considered during workforce planning in a unit.
Acknowledgements
The Carlos III Health Institute has partially financed this study as part of the support of the Spanish Health Research Funds (project PI10/02198). The authors wish to thank Dr. Katia Grillo Padilha for reading and reviewing the first version of the manuscript and for providing helpful suggestions
REFERENCES
- 1. Bray K, Wren I, Baldwin A, St Ledger U, Gibson V, Goodman S, et al. Standards for nurse staffing in critical care units determined by: the British Association of Critical Care Nurses, The Critical Care Networks National Nurse Leads, Royal College of Nursing Critical Care and In-flight Forum. Nurs Crit Care. 2010;15(3):109-11.
- 2. Aiken LH, Clarke SP, Sloane DM, Sochalski J, Silber JH. Hospital nurse staffing and patient mortality, nurse burnout, and job dissatisfaction. JAMA. 2002;288(16):1987-93.
- 3. Cho SH, Ketefian S, Barkauskas VH, Smith DG. The effects of nurse staffing on adverse events, morbidity, mortality, and medical costs. Nurs Res. 2003;52(2):71-9.
- 4. Lang TA, Hodge M, Olson V, Romano PS, Kravitz RL. Nurse-patient ratios: a systematic review on the effects of nurse staffing on patient, nurse employee, and hospital outcomes. J Nurs Adm. 2004;34(7-8):326-37.
- 5. Estabrooks CA, Midodzi WK, Cummings GG, Ricker KL, Giovannetti P. The impact of hospital nursing characteristics on 30-day mortality. J Nurs Adm. 2011;41(7-8 Suppl):S58-68.
- 6. Blot SI, Serra ML, Koulenti D, Lisboa T, Deja M, Myrianthefs P, et al. Patient to nurse ratio and risk of ventilator-associated pneumonia in critically ill patients. Am J Crit Care. 2011;20(1):e1-9.
- 7. Subirana Casacuberta M, Sola AI. Instrumentos basados en medidas indirectas para UCI: TISS y NEMS. Metas Enferm. 2007;10(1):15-20.
- 8. Miranda DR, Nap R, de Rijk A, Schaufeli W, Iapichino G; TISS Working Group. Therapeutic Intervention Scoring System. Nursing activities score. Crit Care Med. 2003;31(2):374-382.
- 9. Subirana Casacuberta M, Sola AI. Instrumentos basados en medidas directas para UCI: NAS (Nursing Activities Score). Metas Enferm. 2006;9(10):67-71.
- 10. Bernat Adell A, Abizanda Campos R, Cubedo Rey M, Quintana Bellmunt J, Sanahuja Rochera E, Sanchis Munoz J, et al. Nursing Activities Score (NAS). Our experience with a nursing load calculation system based on times. Enferm Intensiva. 2005;16(4):164-73.
- 11. Goncalves LA, Padilha KG, Cardoso Sousa RM. Nursing Activities Score (NAS): a proposal for practical application in Intensive Care Units. Intensive Crit Care Nurs. 2007;23(6):355-61.
- 12. Padilha KG, de Sousa RM, Queijo AF, Mendes AM, Reis Miranda D. Nursing Activities Score in the intensive care unit: analysis of the related factors. Intensive Crit Care Nurs. 2008;24(3):197-204.
- 13. Padilha KG, Sousa RM, Garcia PC, Bento ST, Finardi EM, Hatarashi RH. Nursing workload and staff allocation in an intensive care unit: a pilot study according to Nursing Activities Score (NAS). Intensive Crit Care Nurs. 2010;26(2):108-13.
- 14. Padilha KG, Sousa RM, Kimura M, Miyadahira AM, Cruz DALM, Vattimo MF, et al. Nursing workload in Intensive Care Units: a study using the Therapeutic Intervention Scoring System-28 (TISS-28). Intensive Crit Care Nurs. 2007;23(3):162-69.
- 15. Hickey PA. Increasing nurse staffing levels in cardiac surgery centres appears to be a cost effective patient safety intervention. Evid Based Nurs. 2010;13(4):102.
- 16. Silva MC, Sousa RM, Padilha KG. Patient destination after discharge from intensive care units: wards or intermediate care units? Rev Latino Am Enferm. 2010;18(2):224-32.
- 17. Goncalves LA, Padilha KG. Factors associated with nursing workload in adult intensive care units. Rev Esc Enferm USP. 2007;41(4):645-52.
Correspondência:
Publication Dates
-
Publication in this collection
04 June 2013 -
Date of issue
Apr 2013
History
-
Received
23 Aug 2011 -
Accepted
11 July 2012