Abstracts
OBJECTIVE: To describe the different tomographic findings in hypodense hepatic lesions in children and its differential diagnosis. MATERIALS AND METHODS: Computed tomographic studies were obtained from 50 patients (age range: 0-16 years) with low-density liver lesions previously diagnosed by ultrasound. Images were made before and after administration of intravenous contrast medium. Image findings were analyzed and afterwards correlated with anatomopathological diagnosis. RESULTS: Forty-seven of 50 cases were confirmed, 30 by anatomopathological diagnosis. Most of then were benign lesions, hemangioma in 20%. Such lesions presented a homogeneous contrast absorption, mainly at the delayed phase, differing from malignant lesions. Metastasis was the most frequently found malignant lesion (18%). CONCLUSION: Computed tomographic study is of great value in complementing the diagnosis of hypodense hepatic lesions in children, and must follow ultrasound diagnosis as a routine procedure.
Hypodense hepatic injuries; Computed tomography; Childhood
OBJETIVO: Relatar os diferentes aspectos tomográficos das lesões hepáticas hipodensas na infância, orientando às diferentes possibilidades diagnósticas. MATERIAIS E MÉTODOS: Foram realizados estudos tomográficos de lesões hipodensas hepáticas previamente diagnosticadas à ultra-sonografia em 50 pacientes pediátricos (0-16 anos). As imagens foram obtidas antes e após a administração de contraste venoso. Os aspectos de imagem foram analisados e correlacionados posteriormente com o diagnóstico anatomopatológico. RESULTADOS: Dos 50 casos estudados, 47 foram confirmados, 30 destes por estudo anatomopatológico. A maioria das lesões era benigna, sendo o hemangioma o mais freqüente (20% dos casos). Tais lesões apresentaram captação homogênea do meio de contraste, principalmente na fase tardia, diferenciando assim das malignas. As lesões malignas mais freqüentes foram as metástases (18%). CONCLUSÃO: O presente estudo constatou que o exame tomográfico, antes e após a administração do contraste venoso, dinâmico e/ou helicoidal, foi de grande valia para a complementação da hipótese diagnóstica nas lesões hipodensas hepáticas na infância, devendo ser rotina após diagnóstico ultra-sonográfico.
Lesão hipodensa hepática; Tomografia computadorizada; Infância
ORIGINAL ARTICLE
Computed tomographic study of 50 patients with hypodense hepatic injuries in childhood* * Study developed at the Department of Radiology at Faculty of Medical Sciences, Universidade Estadual de Campinas, Campinas, SP.
Inês Minniti Rodrigues PereiraI; Beatriz Regina ÁlvaresI; Jamal BaracatII; Daniel Lahan MartinsII; Ricardo Minniti Rodrigues PereiraIII
IDoctors-Professors at the Department of Radiology, Universidade Estadual de Campinas
IIMD, Residents at the Department of Radiology, Universidade Estadual de Campinas
IIIGraduate Student at Faculty of Medical Sciences, Universidade Estadual de Campinas
Mailing address Mailing address: Profa. Dra. Inês Minniti Rodrigues Pereira Departamento de Radiologia, FCM-Unicamp Rua Tessália Vieira de Camargo, 126 Campinas, SP, Brasil 13083-970 Caixa Postal: 6111 E-mail: iminniti@fcm.unicamp.br
ABSTRACT
OBJECTIVE: To describe the different tomographic findings in hypodense hepatic lesions in children and its differential diagnosis.
MATERIALS AND METHODS: Computed tomographic studies were obtained from 50 patients (age range: 016 years) with low-density liver lesions previously diagnosed by ultrasound. Images were made before and after administration of intravenous contrast medium. Image findings were analyzed and afterwards correlated with anatomopathological diagnosis.
RESULTS: Forty-seven of 50 cases were confirmed, 30 by anatomopathological diagnosis. Most of then were benign lesions, hemangioma in 20%. Such lesions presented a homogeneous contrast absorption, mainly at the delayed phase, differing from malignant lesions. Metastasis was the most frequently found malignant lesion (18%).
CONCLUSION: Computed tomographic study is of great value in complementing the diagnosis of hypodense hepatic lesions in children, and must follow ultrasound diagnosis as a routine procedure.
Keywords: Hypodense hepatic lesion; Computed tomography; Childhood.
INTRODUCTION
Hepatic tumors account for 5% to 6% of all abdominal tumors in children. Primary hepatic neoplasms are the third cause of malignancy in the childhood after Wilms' tumor and neuroblastoma, and are the most usual malignancy of the gastrointestinal tract in children(1).
Such tumors remain a challenge both for the radiologist and the clinician. Many times, benign tumors mimic expansive malignant lesions or metastases, leading to wrong therapeutic decisions. Therefore, it is important that the radiologist familiarizes himself/herself with the different diagnosis techniques and characteristics of the hepatic tumors(2).
The ultrasound (US) frequently is the initial imaging modality of choice for evaluation of the child suspect for expansive abdominal lesion. When the US confirms the hepatic origin of the tumor, additional examinations are performed with computed tomography (CT) or magnetic resonance imaging (MRI). The choice between CT and MRI is controversial and depends upon the experience of the institution and techniques available.
The CT is an appropriate technique for liver imaging. The rapid acquisition of images, makes it possible to evaluate the hepatic parenchyma in two phases (immediate and delayed), considering that the liver has a double blood supply. This improves the detection and characterization of the tumor(3).
The authors' purpose is to report the different tomographic aspects of hypodense hepatic lesions in childhood, providing guidance for different diagnostic possibilities.
MATERIALS AND METHODS
Enhanced spiral and/or dynamic tomographic studies of hypodense hepatic lesions previously diagnosed by US were performed in 50 patients with ages ranging up to 16 years, before and after intravenous contrast (weight-based dose = 1,5 ml/kg).
The study was performed with 35 mm thick slicing in a first non-contrast-enhanced phase, and, in a second phase, with the same slicing, immediately after contrast medium intravenous injection (immediate phase). After 1520 minutes of the initial injection (delayed phase) the same slicing was performed, observing the behavior of the lesions in both immediate and delayed phases.
Aspects of the lesion were analyzed and later some of them were correlated with the anatomopathological diagnosis.
RESULTS
Of the 50 cases studied, 30 were confirmed by means of anatomopathological study of the liver. The non-biopsied cases were lesions related to hemangiomas, hemangioendotheliomas and hepatic cysts, with diagnoses based on clinical history, US and CT scans and later control follow-up.
For the most part, the lesions were benign, and hemangioma was the more frequent lesion (20% of the cases). Such lesions have presented a more homogeneous captation of contrast medium, principally at the delayed phase (Table 1).
The most frequent malignant lesions were the metastases (18%). Its contrast impregnation is irregular at the immediate phase and remains unchanged at the delayed phase (Table 1).
DISCUSSION
As in the literature, the benign hepatic lesions were the most frequent in this study, in the majority of the cases, hemangiomas(4,5) that are mesenchymal tumors and symptomatic vascular lesions more usual in the childhood(6,7). They may present as expansile abdominal lesions associated with high-output heart failure. At CT scan it appears as a hypodense lesion with or without calcification and, after administration of intravenous contrast, there is peripheral captation in the immediate phase, and in the delayed phase there is homogenization of the lesion (Figure 1).
The infant hemangioendothelioma is the most common benign tumor of the liver in the first six months of life(8,9). Before intravenous contrast, one observes hepatic lesions showing well-defined borders with low-density central areas and internal septations % the same behavior of hemangiomas in the post-contrast phase (Figure 2).
Mesenchymal hamartoma is a rare and benign lesion, most frequently appearing in children less than 2 years old. It is considered mostly as a failure in development than a true neoplasia. It appears as a multiloculated cystic hepatic lesion, with fine internal septations.
Simple hepatic cysts are found incidentally, appearing at CT scan as low density images, with well defined borders, thickened walls, usually solitary and peripheral. They do not present enhancement after contrast(10,11).
Congenital hepatic fibrosis usually complicates with portal hypertension and, at CT scan, multiple low density lesions are observed with calcifications of the walls, with possibility of hemorrhage(12).
The most frequent causes of hepatic abscesses in the childhood are a result of perforated appendicitis or granulomatous disease. They present as hypodense areas with heterogeneous captation after intravenous contrast injection (Figure 3).
As far as malignant lesions are concerned, the most common are metastatic ones. They vary in size and shape and are hypodense, well-defined and multiple in the phase before contrast. Due its low vascularization, they become irregular, with different degrees of impregnation or keep themselves hypodense (Figure 4). The most common hepatic metastasis in the childhood is that by neuroblastoma(13,14).
The hepatoblastoma is the most common tumor of the liver in infants before one year of age(6,15). It presents itself as a hypodense, solid and central lesion, possibly containing calcifications and areas of hemorrhage. Intense enhancement is present following contrast, showing the internal lobulation and the nodularity (Figure 5).
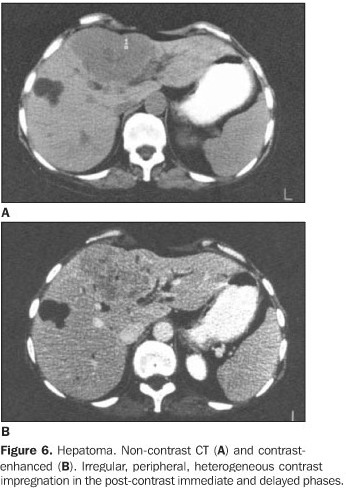
The hepatocellular carcinoma (hepatoma) has a high incidence in young adults, but, when it appears in the childhood, it is more usual in infants(16). At the CT scan it appears as a solitary lesion, large or hypodense multinodular and, frequently, presents itself with a central and hemorrhagic area of necrosis. Post-contrast phase shows enhancement in the non-necrotic areas (Figure 6).
The undifferentiated sarcoma of the liver has an embryonal origin and represents the fourth most common neoplasia in childhood(17,18). It presents itself as a hypodense mass with cystic or heterogeneous aspect, depending upon the degree of necrosis and areas of hemorrhage, seeming septate and solid areas. The impregnation is irregular following contrast.
One observes that benign lesions present a more homogeneous contrast captation, principally in the delayed phase, so the malignant lesions are differentiated. The diagnostic hypothesis is generated by associating the clinic findings with tomographic characteristics of the hepatic lesions,
CONCLUSION
The present study has testified that the dynamic and/or spiral tomographic examination, before and after intravenous contrast medium administration, was invaluable for the completion of the diagnostic hypothesis of hypodense hepatic lesions in the childhood, and must become a routine after US diagnosis.
REFERENCES
Received June 24, 2004.
Accepted after revision July 4, 2005.
- 1. Donnelly LF, Bisset GS. Pediatric hepatic imaging. Radiol Clin North Am 1998;36:413427.
- 2. Horton KM, Bluemke DA, Hruban RH, Soyer P, Fishman EK. CT and MR imaging of benign hepatic and biliary tumors. RadioGraphics 1999;19:431451.
- 3. Quiroga S, Sebastià C, Pallisa E, Castellà E, Pérez-Lafuente M, Alvarez-Castells A. Improved diagnosis of hepatic perfusion disorders: value of hepatic arterial phase imaging during helical CT. RadioGraphics 2001;21:6581.
- 4. Smith WL, Franken EA, Mitros FA. Liver tumors in children. Semin Roentgenol 1983;18:136148.
- 5. Yandza T, Valayer J. Benign tumors of the liver in children: analysis of a series of 20 cases. J Pediatr Surg 1986;21:419423.
- 6. Dachman AH, Lichtenstein JE, Friedman AC, et al Infantile hemangioendothelioma of the liver. A radiologic-pathologic-clinical correlation. AJR 1983;140:10911096.
- 7. Kirchner SG, Heller RM, Kasselberg AG, et al Infantile hepatic hemangioendothelioma with subsequent malignant degeneration. Pediatr Radiol 1981;11:4245.
- 8. Brunelle F, Chaumont P. Hepatic tumors in children: ultrasonic differentiation of malignant from benign lesions. Radiology 1984;150:695700.
- 9. Mahboubi S, Sunaryo FP, Glassman MS, et al Computed tomography, management, and follow-up in infantile hemangioendothelioma of the liver in infants and children. J Comput Tomogr 1987;11: 370375.
- 10. Anand SK, Chan JC, Lieberman E. Polycistic disease and hepatic fibrosis in children. Renal function studies. Am J Dis Child 1975;129:810813.
- 11. Johnston PW. Congenital cysts of the liver in infancy and childhood. Am J Surg 1968;116:184191.
- 12. Bianchi E, Magrini U, Severi F. Congenital hepatic fibrosis. Lancet 1973;1:489.
- 13. Bernardino ME, Erwin BC, Steinberg HV, et al Delayed hepatic CT scanning: increased confidence and improved detection of hepatic metastases. Radiology 1986;159:7174.
- 14. de Campo M, de Campo JF. Ultrasound of primary hepatic tumors in childhood. Pediatr Radiol 1988; 19:1924.
- 15. Amendola MA, Blane CE, Amendola BE, et al CT findings in hepatoblastoma. J Comput Assist Tomogr 1984;8:11051109.
- 16. Soyer P, Roche A, Levesque M, et al CT of fibrolamellar hepatocellular carcinoma. J Comput Assist Tomogr 1991;15:533538.
- 17. Rummeny E, Weissleder R, Stark DD, et al Primary liver tumors: diagnosis by MR imaging. AJR 1989;152:6372.
- 18. Finn JP, Hall-Craggs MA, Dicks-Mireaux C, et al Primary malignant liver tumors in childhood: assessment of resectability with high-field MR and comparison with CT. Pediatr Radiol 1990;21:3438.
Publication Dates
-
Publication in this collection
25 May 2006 -
Date of issue
Apr 2006
History
-
Accepted
04 July 2005 -
Received
24 June 2004