Abstracts
OBJECTIVE: To evaluate the most significant features of parosteal osteosarcoma and to describe the most frequent findings on conventional radiology. MATERIALS AND METHODS: A retrospective study was performed including 26 cases of patients with parosteal osteosarcoma from the archives of "Clube do Osso", Rio de Janeiro, RJ, Brazil, with analysis of main clinical and radiological findings. RESULTS: The disease was prevalent in female patients in the third decade of life. Main clinical findings were the increase in volume on the site of the tumor (77% of cases) and local pain (68% of cases). The most frequent site of tumor was the popliteal fossa (40%), and metaphyseal involvement has occurred in 92% of cases. The most frequent radiological findings were densely mineralized lesions on juxtacortical locations, and irregularly thickened adjacent host cortex (92.3%), with adherence areas being observed in 88.5% of cases, besides lobular (50%) or irregular (38.5%) tumor margins. Also, a radiolucent line between the tumor and the adjacent bone (48%), a denser mineralization on the basis than in the periphery of the tumor (42.3%), and a small rate of periosteal reaction (15.4%) were found. CONCLUSION: Although computed tomography and magnetic resonance imaging are important modalities for identifying some aspects of parosteal osteosarcoma, conventional x-ray is essential in the initial evaluation of this type of lesion, most frequently allowing differential diagnosis with other surface bone lesions.
Parosteal osteosarcoma; Bone radiology
OBJETIVO: Avaliar os achados clínicos mais importantes do osteossarcoma parosteal e descrever os seus aspectos mais comuns na radiologia convencional. MATERIAIS E MÉTODOS: Estudo retrospectivo com 26 pacientes com osteossarcoma parosteal, provenientes do arquivo do Clube do Osso, Rio de Janeiro, RJ, e análise dos principais achados clínicos e aspectos radiológicos. RESULTADOS: A doença predominou em pacientes do sexo feminino e teve idade média de acometimento na terceira década de vida. Os achados clínicos mais freqüentes foram o aumento do volume no local do tumor (77% dos casos) e a dor local (68% dos casos). O local mais comum de tumor foi o oco poplíteo, com 40% dos casos, e houve envolvimento metafisário em 92% dos tumores. O aspecto radiológico mais comumente encontrado foi de lesão bem mineralizada e intimamente justaposta à superfície óssea, com o córtex adjacente irregularmente espessado (92,3% dos casos), observando-se área de adesão a este (88,5% dos casos), além de margens tumorais lobuladas (50% dos casos) ou irregulares (38,5% dos casos). Evidenciaram-se, também, linha radiolucente entre o tumor e o osso adjacente (48% dos casos), padrão de mineralização mais denso na base do que na periferia (42,3% dos casos) e pequena ocorrência de reação periosteal (15,4% dos casos). CONCLUSÃO: Apesar de a tomografia computadorizada e a ressonância magnética serem importantes na identificação de alguns aspectos do osteossarcoma parosteal, a radiologia convencional é altamente sugestiva deste tumor e permite, na maior parte dos casos, o diagnóstico diferencial com outras lesões da superfície óssea.
Osteossarcoma parosteal; Radiologia óssea
ORIGINAL ARTICLE
Parosteal osteosarcoma: conventional radiology findings* * Study developed at Department of Radiology Universidade Federal do Rio de Janeiro (UFRJ) and at Clube do Osso (Bone Club), Rio de Janeiro, RJ, Brazil.
Francisco Nanci NetoI; Edson MarchioriII; Alberto Domingues ViannaIII; Ierecê Lins AymoréIV; Ana Luiza Brito de AlmeidaV; Klaus L. IrionVI; Felipe Birchal CollaresVII
IMD, Radiologist at Clínica de Diagnóstico por Imagem CDPI, Rio de Janeiro, RJ, Brazil
IITitular Professor of Radiology at Universidade Federal Fluminense (UFF), Adjunct Coordinator of Post-graduation Course in Radiology at Universidade Federal do Rio de Janeiro (UFRJ), Rio de Janeiro, RJ, Brazil
IIIAssociate Professor of Radiology at Universidade Federal Fluminense (UFF), Rio de Janeiro, RJ, Brazil
IVPathologist at Hospital de Traumato-Ortopedia, Responsible for the Clube do Osso collection, Rio de Janeiro, RJ, Brazil
VPathologist at Laboratório Cláudio Lemos, Co-responsible for the Clube do Osso collection, Rio de Janeiro, RJ, Brazil
VIConsultant Chest Radiologist at The Cardiothoracic Centre NHS Trust and The Royal Liverpool and Broadgreen University Hospitals, Liverpool, England
VIIVascular and Interventional Radiology Research Fellow of the Beth Israel Deaconess Medical Center (BIDMC) Harvard Medical School, Boston, USA
Mailing address Mailing address: Dr. Francisco Nanci Neto Praia João Caetano, 155, ap. 201, Ingá Niterói, RJ, Brazil, 24210-405 E-mail: francisconanci@predialnet.com.br
ABSTRACT
OBJECTIVE: To evaluate the most significant features of parosteal osteosarcoma and to describe the most frequent findings on conventional radiology.
MATERIALS AND METHODS: A retrospective study was performed including 26 cases of patients with parosteal osteosarcoma from the archives of "Clube do Osso", Rio de Janeiro, RJ, Brazil, with analysis of main clinical and radiological findings.
RESULTS: The disease was prevalent in female patients in the third decade of life. Main clinical findings were the increase in volume on the site of the tumor (77% of cases) and local pain (68% of cases). The most frequent site of tumor was the popliteal fossa (40%), and metaphyseal involvement has occurred in 92% of cases. The most frequent radiological findings were densely mineralized lesions on juxtacortical locations, and irregularly thickened adjacent host cortex (92.3%), with adherence areas being observed in 88.5% of cases, besides lobular (50%) or irregular (38.5%) tumor margins. Also, a radiolucent line between the tumor and the adjacent bone (48%), a denser mineralization on the basis than in the periphery of the tumor (42.3%), and a small rate of periosteal reaction (15.4%) were found.
CONCLUSION: Although computed tomography and magnetic resonance imaging are important modalities for identifying some aspects of parosteal osteosarcoma, conventional x-ray is essential in the initial evaluation of this type of lesion, most frequently allowing differential diagnosis with other surface bone lesions.
Keywords: Parosteal osteosarcoma; Bone radiology.
INTRODUCTION
Osteosarcoma is a tumor arising from the osteogenic matrix, and is the most frequent primary malignant tumor of bone in youngsters(1). It may be localized inside or on the surface of the bone; and in this case it may occur in the cortical bone (intracortical), in adjacent soft tissues (extra-osseous), or in the periosteum (juxtacortical)(2).
Juxtacortical osteosarcomas are rare (8%10% of all osteosarcomas)(1) and can be classified into: parosteal, periosteal and high-grade surface types(3,4). These types are characterized according their origin, respectively from the external periosteal layer, internal periosteal layer, or from any site of the periosteum, but histologically identical to the conventional osteosarcoma(2). On its turn, parosteal osteosarcomas can be subdivided into conventional and dedifferentiated(1,5,6).
Parosteal osteosarcoma is the most common subtype of juxtacortical osteosarcomas, accounting for 75% of them, with a better prognosis(7). The incidence is highest in the third and fourth decades of life(810) most frequently affecting women(7,912). Its most frequent presentation is a mildly painful mass(7,13,14) in the posterior distal region of the femur(12,15,16). Occasionally, areas of dedifferentiation for a high grade sarcoma may arise inside a pre-existent low-grade lesion, both at the tumor presentation (synchronic), and after one or more recurrences (metachronic), in this case with worse prognosis(7,11,1619).
Generally, histological findings associated with conventional x-ray are distinctive, allowing differentiation between parosteal osteosarcoma and other surface osteosarcomas as well as other lesions with which they are frequently confused. Prognosis and management are determined by the extent and histological grade of the tumor(20).
The objective of the present study was to analyze the most significant clinical findings of parosteal osteosarcoma, and to describe the most frequent findings on conventional radiology.
MATERIALS AND METHODS
A retrospective study was performed including 26 cases of patients (nine males, 16 females, one unspecified) diagnosed with parosteal osteosarcoma from the archives of Clube do Osso (Bone Club), in Rio de Janeiro, RJ, Brazil, gathering up radiological and anatomopathological documentation of more than 6,000 cases of bone diseases. The patients came from several public and private hospitals and clinics, in the period between 1960 and 1995, with histopathological confirmation of parosteal osteosarcoma.
The patients' dossiers were reviewed for collection of data such as sex, signs and symptoms, as well as symptoms duration at the moment of the diagnosis.
Plain films of the 26 patients were evaluated, and the following main aspects of the lesion were defined: localization in relation to the affected bone and preferential region; shape; margins; interface with the adjacent cortex, mineralization pattern and presence of medullary invasion, radiolucent line and periosteal reaction.
RESULTS
a) Clinical considerations
The mean age of the patients was approximately 23.6 years, the oldest patient with 47 years and the youngest with six years of age. The peak of incidence occurred in the second and third decades of life, with 17 patients (65.4%) in this age range.
As regards the sex of the patients, 16 were female (61.5%), nine male (34.6%), and in one case this information was unavailable. Therefore, women were preferentially affected with a male-to-female ratio of 1:2.
Information on signs and symptoms were available for 23 cases. The most frequent clinical finding was increase in local volume of the tumor which was visible or palpable in 18 patients (78.3%); in seven patients, the tumor was painless. Pain in the affected site was the second most frequent clinical finding, present in 16 (69.6%) patients; five of these latest presented only pain. Also, limitation of the adjacent joint movement amplitude was observed in four cases (17.4%) and report of a previous trauma in five cases (21.7%).
The duration of symptoms until the moment of the diagnosis was quite variable. Of the 19 patients whose information were available, 11 presented symptoms for one to twelve months, seven for one to five years, and one patient had symptoms for more than five years. No patient presented symptoms for less than one month.
b) Radiological findings
The evaluation of all the 26 patients was based on conventional radiology findings.
As regards the skeletal tumor location, the most frequent site was the distal femur in 16 cases (61.5%), 11 of these cases (68.7%) with involvement of the distal posterior femoral region (popliteal fossa).
The second most frequent site was the proximal tibia, with four cases (15.4%), followed by the middle femur with two cases (7.7%), one of them in the femoral amputation stump, and the proximal humerus, also with two cases (7.7%). The two remaining tumors originated respectively from the distal fibula and proximal femur (7.7%). Therefore, all the tumors occurred in the appendicular skeleton, and 20 patients (76.9%) presented a tumor around the knee.
Twenty-four tumors (92.3%) involved the metaphysis: 11 were metaphyseal and diaphyseal, five affected only the metaphysis, six affected all the regions, and two were metaphyseal and epiphyseal. The two remaining tumors were exclusively epiphyseal.
The typical radiographic finding present in all of the cases was an ovoid or spherical mass, with bone density and in close juxtaposition to the bone surface.
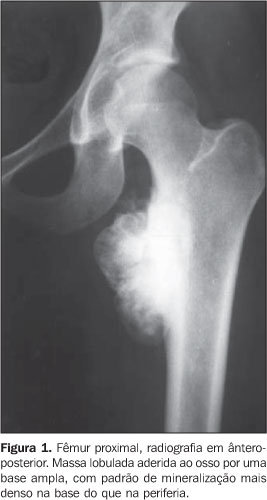
In 13 (50%) cases the tumors were seen as lobular masses (Figures 1 and 2), with irregular margins in ten cases (38.5%) e smooth margins in three cases (11.5%).
The majority of tumors (88.5%) appeared as a mass attached to the underlying cortical bone, and the smallest ones presented with smaller areas of cortical adhesion, but as the tumor grew they also increased. Because of overlapping between tumor and host bone, the adherence areas could not be evaluated in three cases (11.5%).
The small lesions were eccentric and, as the tumor increased, tending to wrap around the host bone (Figures 2 and 3). This has occurred in 20 cases (76.9%). This trend to wrap around the bone led to the radiolucent line obliteration; also, because of structures overlapping, the identification of possible medullary invasion, besides the previously mentioned cortical adhesion by means of conventional x-ray became difficult.
In 24 patients (92.3%) there was reactive sclerosis of the adjacent cortex, resulting in cortical thickening (Figure 4).
A radiolucent line between the tumor and the adjacent cortex, except in the area of the tumor attachment to the cortex, was observed in 13 cases (50%).
The classical pattern of tumor mineralization a denser mineralization on the base than in the periphery of the tumor (Figures 1, 2 e 3) was found in 42.3% of cases. Other mineralization patterns found were: amorphous pattern (23.1%), uniform pattern (23.1%) and lobulated pattern (11.5%).
Periosteal reaction was present in four cases (15.4%) with formation of a Codman's triangle (Figure 4) in two, and periosteal thickening with calcification (Figure 5) in one case.
Finally, it is important to note that although there is no report on follow-up for the majority of patients, three cases corresponded to local recidivation.
DISCUSSION
Osteogenic sarcomas (osteosarcomas) are the most frequent malignant bone tumors in children and young adults, constituting about 15% of primary bone tumors(21). Other most common bone sarcomas are chondrosarcoma and Ewing's sarcoma(2224).
In the present study, the mean age of the patients was approximately 23.6 years, with peak of incidence in the second and third decades of life. This finding was a little different from the majority of published studies, where the peak of incidence occurs ten years latter, in the third and fourth decades of life(2,4,9,11,20,25,26). Schajowicz et al.(4), have studied 64 cases with 81% of the patients with more than 20 years of age, while Jelinek et al.(27) have reported a mean age of 31 years (n = 60). Okada et al.(13), who have presented the largest casuistic in the literature, with 226 cases, reported a mean age of 28 years, similarly to Temple et al.(9), with 38 patients (mean age = 28.9 years), Johnson et al.(25), with 33 patients (mean age = 33 years), and Cassone et al.(26), with 29 patients (mean age = 25.3 years).
As regards the patient's sex, women were preferentially affected 61.5% women (n = 16), 34.6% men (n = 9) and one patient whose sex was not reported , with a 2:3 men/women ratio. This higher female prevalence is in agreement with several authors(2,4,7,9,12,13), with a similar 2:3 men/women ratio reported by Okada et al.(13) (n = 226).
Regarding signs and symptoms, in the present casuistic, the most frequent clinical findings were increase in local volume of the tumor in 18 patients (78.3%), local pain in 16 (69.6%). Also, limitation of the adjacent joint movement amplitude was observed in four cases (17.4%), and report of previous trauma in five cases (21.7%) These clinical findings are similar to those described by several other studies(24,7, 13,14,26). Okada et al.(13) have reported the following symptoms as the most frequently found: localized edema in 54% of patients (n = 102), and pain in 35% (n = 66); the following signs have been observed: a mass in 86% of patients (n = 81), and limitation of the adjacent joint movement amplitude in 33% of cases (n = 31). There was a history of previous trauma in only 19 cases (8.4%). According to Schajowicz et al.(4), a trauma just attracts attention to already existing lesions, rather than causing them to appear.
In the present study, all the tumors were situated in long tubular bones, the popliteal fossa being the most frequent site (40% of cases). This finding is in agreement with all the other series(1,7,12,14,20,2527). Also, 76% of the lesions involved bones around the knee, a rate similar to those reported by Resnick et al.(3) and Spina et al.(1) (70%), and Johnson et al.(25) and Cassone et al.(26) (72%).
The preference of the tumor for a specific site in the bone affected was a remarkable characteristic of parosteal osteosarcoma. The metaphysis was affected by 92.3% of tumors, and 7.7% were restricted to the diaphysis. These percentages are in agreement with the expected ratios; Partovi et al.(16) have reported 90% of lesions involving the metaphysis, and 10% involving only the diaphysis, while Okada et al.(13) have found respectively 91% and 9%. Both the present study and other studies in the literature, have found no tumor restricted to the epiphyseal region.
Temple et al.(9), with a 38-patient casuistic, have radiographically described all the lesions as densely mineralized and in close juxtaposition to the bone surface. These features we also observed in all the cases in the present study.
Okada et al.(13), evaluating 226 patients, demonstrated that the most frequently found external edge of tumors was the lobulated one (60%), followed by irregular edges (17%) and smooth edges (16%). In the present study, similar results were found, the lobulated edge being the most frequently found (50%), irregular (38.5%), and smooth (11,5%), less frequently found. These results are in agreement with other studies in the literature(1,4,11,15,27), generally describing these tumors with lobulated or irregular margins.
Twenty-three of the 26 tumors (88.5%) were attached to the bone cortex; and in three of them (11.5%) the adhesion could not be evaluated because of overlapping between the lesion and the host bone. Okada et al.(13) have reported 70% of tumors attachment to the underlying bone cortex, and in 24% of tumors this attachment could not be evaluated due the same above mentioned reasons.
In 76% of cases, the tumor involved the bone as its size increased, likewise in several other studies(3,11,15,20,27).
Hudson et al.(28) and Pérez et al.(11) have reported an irregular thickening of the adjacent cortex, which was also observed in 92.3% of patients in the present study. Okada et al.(13), with 226 patients, have reported cortical thickening in only 29% of cases.
In the present study, intramedullary extension of the tumor could not be found. In their study, Okada et al.(13) mentioned that the medullary involvement was more clearly seen on computed tomography or magnetic resonance imaging, evidenced in 37 (22%) patients evaluated in transverse sections.
In the present casuistic, a radiolucent line between the tumor and the adjacent bone was observed in 13 cases (50%), with a tendency to obliteration in tumors involving the bone. This fact has been reported by several authors(3,11,15,20,27); Okada et al.(13) have observed this radiolucent line in 58% of 226 lesions, with difficulty in identifying it by conventional radiology in the remaining lesions because of structures (tumor and adjacent bone) overlapping.
Some authors(2,3,18) have described a classical lesion mineralization pattern, denser on the base than in the periphery; in the present study this pattern was found in 42.3% of cases (n = 11). Also, an amorphous pattern of mineralization was found in 23.1% of patients, a uniform pattern in 23.1%, and a lobulated pattern in 11.5%. Okada et al.(13) have observed this classical pattern of mineralization in a still lower percentage, only 15%.
The periosteal reaction, absent in the majority of cases according to some authors(2,11,26), was observed in only four cases in the present study (15.4%). A similarly low rate was reported by Okada et al.(13), with only 6% of tumors presenting periosteal reaction.
In summary, the main findings of conventional radiology in all of the cases were a densely mineralized lesion in close juxtaposition to a bone surface, with the adjacent cortex irregularly thickened, besides areas of cortical attachment and irregular and lobulated margins. Also, a radiolucent line between the tumor and the adjacent bone was typically evidenced, besides a denser mineralization pattern on the base than in the periphery, and a mild periosteal reaction.
REFERENCES
Received May 5, 2006.
Accepted after revision June 30, 2006.
- 1. Spina V, Montanari N, Romagnoli R. Malignant tumors of the osteogenic matrix. Eur J Radiol 1998;27(Suppl 1):S98109.
- 2. Kenan S, Abdelwahab IF, Klein MJ, Hermann G, Lewis MM. Lesions of juxtacortical origin (surface lesions of bone). Skeletal Radiol 1993;22: 337357.
- 3. Resnick D. Diagnosis of bone and joint disorders. 3rd ed. Philadelphia: WB Saunders, 1996;36623697.
- 4. Schajowicz F. Neoplasias ósseas e lesões pseudotumorais. 2Ş ed. Rio de Janeiro: Revinter, 2000;71130.
- 5. Sheth DS, Yasko AW, Raymond AK, et al. Conventional and dedifferentiated parosteal osteosarcoma. Diagnosis, treatment, and outcome. Cancer 1996;78:21362145.
- 6. David A, Rios RA, Tarragô RP, et al. Indicação de ressecção radical em sarcoma parosteal. Rev Bras Ortop 1995;30:801804.
- 7. Abdelwahab IF, Kenan S, Hermann G, Klein MJ. Dedifferentiated parosteal osteosarcoma of the radius. Skeletal Radiol 1997;26:242245.
- 8. Lin J, Yao L, Mirra JM, Bahk WJ. Osteochondroma-like parosteal osteosarcoma: a report of six cases of a new entity. AJR Am J Roentgenol 1998; 170:15711577.
- 9. Temple HT, Scully SP, O'Keefe RJ, Katapurun S, Mankin HJ. Clinical outcome of 38 patients with juxtacortical osteosarcoma. Clin Orthop Relat Res 2000;(373):208217.
- 10. Meohas W, Smith J, Aymoré IL, et al. Osteossarcoma parosteal de escápula. Rev Bras Ortop 2003;38:561566.
- 11. Pérez MG, Peinador AM, Moya AB, et al. Osteosarcoma yuxtacortical. Rev Clín Esp 1990;187189.
- 12. Picci P, Campanacci M, Bacci G, Capanna R, Ayala A. Medullary involvement in parosteal osteosarcoma. A case report. J Bone Joint Surg Am 1987;69:131136.
- 13. Okada K, Frassica FJ, Sim FH, Beabout JW, Bond JR, Unni KK. Parosteal osteosarcoma. A clinicopathological study. J Bone Joint Surg Am 1994; 76:366378.
- 14. Wines A, Bonar F, Lam P, McCarthy S, Stalley P. Telangiectatic dedifferentiation of a parosteal osteosarcoma. Skeletal Radiol 2000;29:597600.
- 15. Edeiken J, Farrell C, Ackerman LV, Spjut HS. Parosteal sarcoma. Am J Roentgenol Radium Ther Nucl Med 1971;111:579583.
- 16. Partovi S, Logan PM, Janzen DL, O'Connel JX, Connel DG. Low grade parosteal osteosarcoma of the ulna with dedifferentiation into high-grade osteosarcoma. Skeletal Radiol 1996;25:497500.
- 17. Haeckel C, Ayala AG, Radig K, Raymond AK, Roessner A, Czerniak B. Protease expression in dedifferentiated parosteal osteosarcoma. Arch Pathol Lab Med 1999;123:213221.
- 18. Shuhaibar H, Friedman L. Dedifferentiated parosteal osteosarcoma with high-grade osteoclast-rich osteogenic sarcoma at presentation. Skeletal Radiol 1998;27:574577.
- 19. Bertoni F, Bacchini P, Staals EL, Davidovitz P. Dedifferentiated parosteal osteosarcoma: the experience of the Rizzoli Institute. Cancer 2005; 103:23732782.
- 20. Levine E, De Smet AA, Huntrakoon M. Juxtacortical osteosarcoma: a radiologic and histologic spectrum. Skeletal Radiol 1985;14:3846.
- 21. Pinho MC, Lima GAF, Rodrigues MB. Osteossarcoma periosteal (Qual o seu diagnóstico?). Radiol Bras 2005;38(6):VIIIX.
- 22. Oliveira GA, Werlang HZ, Bergoli PM, Frechiani M, Oliveira F. Tomografia computadorizada na análise dos padrões de calcificação nos tumores ósseos da bacia em pediatria: nova abordagem. Radiol Bras 2006;39:413418.
- 23. Gomes ACN, Silveira CRS, Paiva RGS, Aragão Jr AGM, Castro Jr JRC. Condrossarcoma em paciente com osteocondromatose múltipla: relato de caso e revisão da literatura. Radiol Bras 2006;39: 449451.
- 24. Catalan J, Fonte AC, Lusa JRB, Oliveira AD, Melo ES, Gonçalves CM. Sarcoma de Ewing: aspectos clínicos e radiográficos de 226 casos. Radiol Bras 2005;38:333336.
- 25. Johnson K, Davies AM, Evans N, Grimer RJ. Imaging recurrent parosteal osteosarcoma. Eur Radiol 2001;11:460466.
- 26. Cassone AE, Camargo PO, Croci AT, Oliveira CRGMC. Osteossarcoma parosteal: avaliação clínica, radiográfica, anatomopatológica e fatores de prognóstico em 29 casos operados. Rev Bras Ortop 1998;33:867875.
- 27. Jelinek JS, Murphey MD, Kransdorf MJ, Shmookler BM, Malawer MM, Hur RC. Parosteal osteosarcoma: value of MR imaging and CT in the prediction of histologic grade. Radiology 1996; 201:837842.
- 28. Hudson TM, Springfield DS, Benjamin M, Bertoni F, Present DA. Computed tomography of parosteal osteosarcoma. AJR Am J Roentgenol 1985;144:961965.
Publication Dates
-
Publication in this collection
21 May 2007 -
Date of issue
Apr 2007
History
-
Accepted
30 June 2006 -
Received
15 May 2006