Abstract
Cytomegalovirus (CMV) is the most common congenital viral infection, causing hearing, visual and psychomotor impairment. Preexisting maternal CMV immunity substantially reduces, but not eliminates, the risk of fetal infection and affectation. This article is about a case of nonprimary maternal CMV infection during pregnancy, with vertical transmission, resulting in severe fetal affectation. Preconceptional analysis indicated maternal CMV past infection. Pregnancy progressed uneventfully until the 20th week ultrasound (US), which revealed cerebral abnormalities: thin and hyperechogenic cerebral cortex with prominent lateral ventricles, bilateral periventricular hyperechogenicities, cerebellar vermis hypoplasia and absent corpus callosum. The MRI suggested these findings were compatible with congenital infection rather than primary brain malformation.
The fetal karyotype was normal. The title of CMV's IgG antibodies almost tripled. Since the first semester,analysisof the polymerasechainreaction(PCR)forCMVDNAintheamniotic fluid was negative. The pregnancy was terminatedat 23weeks. Neuropathologicalfindings at autopsy showed severe brain lesions associated with CMV infection.
Keywords
cytomegalovirus fetal infection; nonprimary infection; lissencephaly
Resumo
O citomegalovírus (CMV) é a infeção viral congénita que mais comumente causa deficiência auditiva, visual e psicomotora. A preexistência de imunidade materna reduz substancialmente, mas não elimina, o risco de infeção e afetação fetal. Trata-se de um caso de infeção materna não primária por CMV durante a gravidez, com transmissão vertical, resultando em afetação fetal severa. As análises preconcepção indicavam infecção passada por CMV. A gravidez decorreu sem intercorrências até a ecografia efetuada na 20ª semana, que revelou alterações cerebrais: córtex cerebral fino e hiperecogénico com ventrículos laterais proeminentes, hiperecogenecidades periventriculares bilaterais, hipoplasia do vérmis cerebeloso e ausência de corpo caloso. A ressonância magnética sugeriu que estes achados eram mais favoráveis a uma infeção congénita do que com uma malformação cerebral primária. O cariótipo fetal era normal. O título de anticorpos IgG para CMV havia triplicado desde a dosagem do primeiro trimestre. O PCR para o DNA do CMV no líquido amniótico foi negativo. A gravidez foi interrompida na 23ª semana. Os achados neuropatológicos na autópsia mostraram lesões cerebrais severas associadas a infeção por CMV.
Palavras-chave
infeção fetal por citomegalovírus; infeção não primária; lisencefalia
Introduction
Cytomegalovirus (CMV) is the most common congenital viral infection, with a birth prevalence of 0,2 to 2,2%, 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 causing hearing and visual impairment and delay of psychomotor development. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354
Primary CMV infection during pregnancy has an incidence of 1 to 4%, 22 Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599 and the global risk of transplacental infection is ∼ 40%. 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 44 Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758 The risk of fetal infection increases with the gestational age 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 22 Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599 55 Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214 (according to a study involving 508 pregnancies, vertical CMV transmission rate by gestational age at the time of maternal infection was 0% in the pregestation group, 4.6% in the periconception group, 34.8, 42 and 58.6% respectively in the first, second and third trimester groups). 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 Severe disease may affect fetuses infected during the first trimester as well as the second, but rarely affects fetuses infected later on in pregnancy. 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 55 Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214 Also, congenital infection impairs placental development and functions, and should be considered as an underlying cause of intrauterine growth restriction (IUGR), regardless of virus transmission to the fetus. 66 Pereira L, Petitt M, Fong A, et al. Intrauterine growth restriction caused by underlying congenital cytomegalovirus infection. J Infect Dis 2014;209(10):1573-1584
Ten to 15% of congenitally infected newborns are overtly symptomatic at birth and will present neurodevelopmental damage within the first three years. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 From those, 20 to 30% die, mostly of disseminated intravascular coagulation, hepatic dysfunction, or bacterial superinfection; severe neurologic morbidity occurs in 50 to 60% of survivors. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 55 Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214 77 Ornoy A, Diav-Citrin O. Fetal effects of primary and secondary cytomegalovirus infection in pregnancy. Reprod Toxicol 2006 ; 21(4):399-409 Of the asymptomatic infants at birth (85 to 90%), 5 to 15% will develop long-term neurodevelopmental morbidity, such as sensorial hearing loss, delay of psychomotor development and visual impairment. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354
The criteria necessary to recommend universal screening for CMV infection in pregnant women haven't yet been met, and are not recommended by the Centers for Disease Control and Prevention or the American College of Obstetricians and Gynecologists. 22 Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599 88 Walker SP, Palma-Dias R, Wood EM, Shekleton P, Giles ML. Cytomegalovirus in pregnancy: to screen or not to screen. BMC Pregnancy Childbirth 2013;13:96 Prenatal diagnosis is mainly performed when US abnormalities are observed. 44 Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758
Nonprimary maternal CMV infection (reactivation or reinfection with a different strain) occurs more rarely, with less probability of fetal infection (1,5% in a study with 543 cases of suspected maternal nonprimary infection) 99 Yoeli-Ullman R, Lipitz S, Schiff E, Feldman B. 216: Prenatal diagnosis of fetal cytomegalovirus infection in 543 cases of suspected maternal non-primary infection. Am J Obstet Gynecol 2007;197(6, Suppl)S71 and only 0.2 to 2% of newborns will develop a symptomatic disease, 66 Pereira L, Petitt M, Fong A, et al. Intrauterine growth restriction caused by underlying congenital cytomegalovirus infection. J Infect Dis 2014;209(10):1573-1584 which indicates a minor fetal affectation in these cases.
This case draws attention to the gravity of a nonprimary CMV infection.
Case Description
The patient is 37 years old, with irrelevant personal and family medical histories, and in her fourth spontaneous pregnancy. The patient has a history of two spontaneous abortions and a term vaginal delivery, which resulted in a healthy child. The spouse is healthy; the couple is not consanguineous.
Preconceptional analysis indicated maternal immunity to Rubella, Toxoplasmosis and CMV. First trimester routine analysis at the 11th week of pregnancy indicated CMV IgG and IgM of respectively 848.9 Ul/mL (positive threshold ≥ 1) and 0.379 Ul/mL (negative threshold < 0,8). The first trimester US did not show fetal anomalies, and the combined prenatal screening for chromosomal abnormalities was negative.
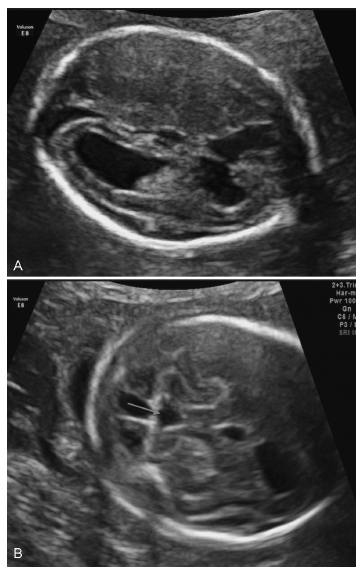
At 20 weeks of gestation, US revealed cerebral abnormalities: thin and hyperechogenic cerebral cortex with prominent lateral ventricles, bilateral periventricular hyperechogenicities, cerebellar vermis hypoplasia and absent corpus callosum ( Fig. 1 ). Amniocentesis was performed and the karyotype was normal (46, XY).
(A) Ultrasound at 20 weeks of gestation – thin and hyperechogenic cerebral cortex with prominent lateral ventricles and bilateral periventricular hyperechogenicities. (B) Ultrasound at 20 weeks of gestation – cerebellar vermis hypoplasia (arrow).
An extended serology study was then performed, and it showed no immunity to Herpes simplex virus type 2 and immunity to Toxoplasmosis, Herpes simplex virus type 1, Parvovirus and CMV. However, CMV IgG title increased almost three times since the first trimester analysis, and CMV IgM kept negative (IgG 2695.0 Ul/mL and IgM 0.333 Ul/mL) – these serologic tests were performed in the same laboratory as the first trimester tests. IgG avidity testing was high.
When asked about flu–like symptoms, the patient mentions an episode during the second trimester of pregnancy; however, as it was mild, it was difficult to precise the time of it.
Magnetic resonance imaging (MRI) at 22 weeks of gestation confirmed US findings and raised the hypothesis of fetal infection: “[…] enlargement of the cerebrospinal fluid circulation spaces at the expense of marked reduction in the thickness of the cerebral parenchyma of both hemispheres of lissencephalic appearance [...] suggesting serious sequelae of brain infection (group TORCH? other?) rather than primary malformative injury of the central nervous system” ( Fig. 2 ).
Outcome and Follow-up
The pregnancy was terminated at 23 weeks.
At this time, a new sample of amniotic fluid was collected to perform PCR for CMV DNA. The result was negative. Pathologic examination study of fetal and placental tissues revealed cerebral ventricular dilation with necro-hemorrhagic and calcified periventricular lesions, necro-hemorrhagic lesions also at the level of the basal ganglia, hippocampus, periventricular regions of brainstem and cerebellar hemispheres. There were areas of four-layer polymicrogyria and frequent cellular viral inclusions (cytomegalic cells), particularly in the germinal matrix and near the necrotic lesions. These cells tested positive for CMV immunohistochemistry ( Figs. 3 , 4 and 5 ). Immunohistochemical detection of CMV DNA was found not only in the fetus brain, but also in his liver, heart and in the placenta.
Macroscopical findings – coronal section at the level of the hippocampus showing dilation of lateral ventricles, extensive white matter periventricular lesions with focal necro-hemorrhagic lesions at this level and also at the level of the amygdala/hippocampus and thalamus.
(A) Histopathological findings – neurons of germinal matrix with some viral inclusions (arrow), with the typical aspect of cytomegalic cells (HE). Magnification, 630x. (B) Histopathological findings – cells positive for CMV immunohistochemistry (some showing colocation with the viral inclusions). Magnification, 100x.
Discussion
All the investigation and outcomes in this case suggest a probable CMV secondary infection, which can be due to a reactivation or reinfection with a different strain. According to the maternal serology and the morphologic US performed, the maternal CMV secondary infection must have occurred between 11 and 20 weeks of pregnancy.
The preferred approach for diagnosing fetal infection is PCR testing for DNA virus in the amniotic fluid, 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 44 Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758 which has a sensitivity of 75–100%. 44 Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758 Gestational age at amniocentesis and the time elapsed since the suspicion of infection are critical factors for the sensitivity of the method. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 44 Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758
The PCR for CMV DNA negative result was indeed a false negative. Although this method is recognized as the gold standard for prenatal diagnosis of fetal CMV infection, the gestational age and the time lag between maternal infection and amniocentesis is a critical factor influencing sensitivity. To achieve the highest sensitivity, amniocentesis should be performed after 21 weeks of gestation and at least 6 to 7 weeks after the onset of maternal infection reflecting the time it takes for placental infection, transmission to the fetus, viral replication in the fetal kidney, and excretion into amniotic fluid. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 33 Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6 88 Walker SP, Palma-Dias R, Wood EM, Shekleton P, Giles ML. Cytomegalovirus in pregnancy: to screen or not to screen. BMC Pregnancy Childbirth 2013;13:96 In spite of having fulfilled the first prerequisite, the time lag might not have been achieved. Nevertheless, we were reaching the legal limit for terminating the pregnancy, and even without a prenatal diagnosis, the US findings foretold a poor outcome for the offspring.
The idea that nonprimary CMV maternal infection will not result in severe fetal sequelae and congenital disease has been proved different in several published cases. 55 Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214 1010 Boppana SB, Fowler KB, Britt WJ, Stagno S, Pass RF. Symptomatic congenital cytomegalovirus infection in infants born to mothers with preexisting immunity to cytomegalovirus. Pediatrics 1999 ; 104(1 Pt 1):55-60 1111 Stagno S, Pass RF, Dworsky ME, et al. Congenital cytomegalovirus infection: The relative importance of primary and recurrent maternal infection. N Engl J Med 1982;306(16):945-949 The preexisting maternal CMV seropositivity substantially reduces, but not eliminates, the risk of fetal infection and affectation; therefore, the use of prenatal invasive methods for the detection of fetal infection in nonprimary maternal infections may be justified.
Neurons migrate from the areas where they are born to the areas where they will settle into their proper neural circuits. Neuronal migration starts in the second month of gestation and is controlled by a complex assortment of chemical guides and signals. When these signals are absent or incorrect, neurons do not end up where they belong, resulting in a primary malformative injury called lissencephaly. The lack of gyral development after a defective neuronal migration in the developing brain can be associated with the agenesis of the corpus callosum or cerebellar hypoplasia, and is also due to some genetic syndromes. 1212 Cheeran MC, Lokensgard JR, Schleiss MR. Neuropathogenesis of congenital cytomegalovirus infection: disease mechanisms and prospects for intervention. Clin Microbiol Rev 2009;22(1): 99-126
Neuropathological studies of brains infected prenatally by CMV show evidence of lissencephaly, polymicrogyria, cerebellar hypoplasia and ventricular dilation in consequence of loss of volume (atrophy), 77 Ornoy A, Diav-Citrin O. Fetal effects of primary and secondary cytomegalovirus infection in pregnancy. Reprod Toxicol 2006 ; 21(4):399-409 1212 Cheeran MC, Lokensgard JR, Schleiss MR. Neuropathogenesis of congenital cytomegalovirus infection: disease mechanisms and prospects for intervention. Clin Microbiol Rev 2009;22(1): 99-126 findings suggestive of the severity and risk of neurological and motor sequelae. Still, a normal US examination cannot exclude neonatal or long-term morbidity. 11 YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354 1313 Picone O, Teissier N, Cordier AG, et al. Detailed in utero ultrasound description of 30 cases of congenital cytomegalovirus infection. Prenat Diagn 2014;34(6):518-524 Mild ventriculomegaly, cerebellar vermis hypoplasia and lissencephaly can also be associated with extra central nervous system abnormalities, chromosomal aberration and other fetal infections like rubella and toxoplasmosis. 1313 Picone O, Teissier N, Cordier AG, et al. Detailed in utero ultrasound description of 30 cases of congenital cytomegalovirus infection. Prenat Diagn 2014;34(6):518-524 In this case, no other abnormalities were found beyond the fetal central nervous system; the karyotype was normal and the other fetal infections were excluded.
There is insufficient evidence to support the use of passive immunization to prevent congenital infection, 22 Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599 and the only known means of reducing the risk of congenital CMV is by reducing exposure to the virus through hygiene measures. 22 Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599 55 Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214
Therapies for treatment of congenital CMV are in the experimental stage. In an uncontrolled study published in 2005, administration of CMV-specific hyperimmune globulin to pregnant women with primary CMV infection significantly reduced the rate of intrauterine transmission, from 40 to 16%. 1414 Nigro G, Adler SP, La Torre R, Best AM; Congenital Cytomegalovirus Collaborating Group. Passive immunization during pregnancy for congenital cytomegalovirus infection. N Engl J Med 2005 ; 353(13):1350-1362 A 2014 randomized placebo-controlled phase 2 trial of virus-specific hyperimmune globulin for the prevention of congenital CMV infection, involving 124 women with primary CMV infection from 5 to 26 weeks of gestation, showed that the treatment with hyperimmune globulin did not significantly modify the course of primary CMV infection during pregnancy. 1515 Revello MG, Lazzarotto T, Guerra B, et al; CHIP Study Group. A randomized trial of hyperimmune globulin to prevent congenital cytomegalovirus. N Engl J Med 2014;370(14):1316-1326 Other phase 3 studies are under way to further our understanding of the efficacy and safety of hyperimmune globulin administration as a means of preventing congenital CMV infection.
Although it is still not recommended, our institution offers pregnant women systematic screening for CMV infection, as well as education about hygienic measures. However, we do not provide any therapy for pregnant women with suspicious or confirmed CMV primary or nonprimary infections.
Nevertheless, the US and MRI findings in this case suggested the presence of severe advanced disease and high risk of long-term neurodevelopmental impairment, so the option of pregnancy termination was obviously raised.
This article is about a rare case of nonprimary maternal CMV infection during pregnancy, with vertical transmission, resulting in severe fetal affectation. The preexisting maternal CMV seropositivity substantially reduces, but not eliminates, the risk of fetal infection and affectation. This article highlights the importance of clinical suspicion and the difficulty of prenatal confirmation of a CMV infection.
References
-
1YinonY,FarineD,YudinMH,etal;FetalMedicineCommittee,Society of Obstetricians and Gynaecologists of Canada. Cytomegalovirus infection in pregnancy. J Obstet Gynaecol Can 2010;32(4):348-354
-
2Johnson J, Anderson B. Screening, prevention, and treatment of congenital cytomegalovirus. Obstet Gynecol Clin North Am 2014; 41(4):593-599
-
3Feldman B, Yinon Y, Tepperberg Oikawa M, Yoeli R, Schiff E, Lipitz S. Pregestational, periconceptional, and gestational primary maternal cytomegalovirus infection: prenatal diagnosis in 508 pregnancies. Am J Obstet Gynecol 2011;205(4):342.e1-342.e6
-
4Picone O, Vauloup-Fellous C, Cordier AG, et al. A series of 238 cytomegalovirus primary infections during pregnancy: description and outcome. Prenat Diagn 2013;33(8):751-758
-
5Benoist G, Leruez-Ville M, Magny JF, Jacquemard F, Salomon LJ, Ville Y. Management of pregnancies with confirmed cytomegalovirus fetal infection. Fetal Diagn Ther 2013;33(4): 203-214
-
6Pereira L, Petitt M, Fong A, et al. Intrauterine growth restriction caused by underlying congenital cytomegalovirus infection. J Infect Dis 2014;209(10):1573-1584
-
7Ornoy A, Diav-Citrin O. Fetal effects of primary and secondary cytomegalovirus infection in pregnancy. Reprod Toxicol 2006 ; 21(4):399-409
-
8Walker SP, Palma-Dias R, Wood EM, Shekleton P, Giles ML. Cytomegalovirus in pregnancy: to screen or not to screen. BMC Pregnancy Childbirth 2013;13:96
-
9Yoeli-Ullman R, Lipitz S, Schiff E, Feldman B. 216: Prenatal diagnosis of fetal cytomegalovirus infection in 543 cases of suspected maternal non-primary infection. Am J Obstet Gynecol 2007;197(6, Suppl)S71
-
10Boppana SB, Fowler KB, Britt WJ, Stagno S, Pass RF. Symptomatic congenital cytomegalovirus infection in infants born to mothers with preexisting immunity to cytomegalovirus. Pediatrics 1999 ; 104(1 Pt 1):55-60
-
11Stagno S, Pass RF, Dworsky ME, et al. Congenital cytomegalovirus infection: The relative importance of primary and recurrent maternal infection. N Engl J Med 1982;306(16):945-949
-
12Cheeran MC, Lokensgard JR, Schleiss MR. Neuropathogenesis of congenital cytomegalovirus infection: disease mechanisms and prospects for intervention. Clin Microbiol Rev 2009;22(1): 99-126
-
13Picone O, Teissier N, Cordier AG, et al. Detailed in utero ultrasound description of 30 cases of congenital cytomegalovirus infection. Prenat Diagn 2014;34(6):518-524
-
14Nigro G, Adler SP, La Torre R, Best AM; Congenital Cytomegalovirus Collaborating Group. Passive immunization during pregnancy for congenital cytomegalovirus infection. N Engl J Med 2005 ; 353(13):1350-1362
-
15Revello MG, Lazzarotto T, Guerra B, et al; CHIP Study Group. A randomized trial of hyperimmune globulin to prevent congenital cytomegalovirus. N Engl J Med 2014;370(14):1316-1326
Publication Dates
-
Publication in this collection
Apr 2016
History
-
Received
02 Sept 2015 -
Accepted
11 Jan 2016