Abstracts
The current study aimed to systematically analyze trends and priorities in the theoretical and conceptual approaches and empirical studies on specific health services management modalities in the Brazilian Unified National Health System. A narrative review of the literature identified, in 33 publications, the location and nature of services, management models, methodological procedures, and study outcomes. The research deals mainly with the models’ conceptual and legal characteristics and management practices, in addition to addressing contracts, procurement, human resources, financing, and control mechanisms. In conclusion, the literature is limited and concentrated in the State of São Paulo, showing little theoretical diversity and methodological weaknesses, while it is nonconclusive as to the superiority of one management model over another. New evaluation studies are needed that are capable of comparing different models and assessing their performance and their effects on the quality of health services’ provision, the population’s health, and the health system’s organization.
Keywords:
Health Management; Health Services Administration; Unified Health System
O presente trabalho busca sistematizar tendências e prioridades das abordagens teórico-conceituais e das investigações empíricas sobre modalidades específicas de gestão de serviços no âmbito do Sistema Único de Saúde no Brasil. Foi realizada uma revisão narrativa da literatura que identificou, em 33 publicações, a localização e a natureza dos serviços, os modelos de gestão, os procedimentos metodológicos e os desfechos dos estudos. A produção trata principalmente de aspectos conceituais, legais e práticas gerenciais dos modelos, além de abordar contratos, compras, recursos humanos, financiamento e mecanismos de controle. Concluiu-se que a literatura analisada é restrita, concentrada no Estado de São Paulo, com baixa diversidade de teorias e fragilidades de aportes metodológicos, sendo inconclusiva quanto à superioridade de um modelo de gestão sobre outro. São fundamentais novas pesquisas avaliativas capazes de comparar os diferentes modelos e julgar seus desempenhos e efeitos na qualidade da assistência prestada, na saúde da população e na organização do sistema de saúde.
Palavras-chave:
Gestão em Saúde; Administração de Serviços de Saúde; Sistema Único de Saúde
El presente estudio tuvo como objetivo analizar sistemáticamente las tendencias y prioridades en los enfoques teóricos y conceptuales y estudios empíricos sobre modalidades específicas de gestión de los servicios de salud en el Sistema Único de Salud de Brasil. Una revisión narrativa de la literatura identificó, en 33 publicaciones, la ubicación y la naturaleza de los servicios, los modelos de gestión, los procedimientos metodológicos y los resultados del estudio. La investigación se ocupa principalmente de las características conceptuales y legales y las prácticas de gestión de los modelos, además de abordar los contratos, las adquisiciones, los recursos humanos, el financiamiento y los mecanismos de control. En conclusión, la literatura es limitada y concentrada en el Estado de São Paulo, mostrando poca diversidad teórica y debilidades metodológicas, mientras que no es concluyente en cuanto a la superioridad de un modelo de gestión sobre otro. Se necesitan nuevos estudios de evaluación que sean capaces de comparar diferentes modelos y evaluar su desempeño y sus efectos sobre la calidad de la provisión de servicios de salud, la salud de la población y la organización del sistema de salud.
Palabras-clave:
Gestión en Salud; Administración de los Servicios de Salud; Sistema Único de Salud
Introduction
The states and municipalities that comprise the Brazilian Unified National Health System (SUS) can manage, maintain, and provide health services directly or indirectly, including through complementary participation by the private sector, in order to meet their Constitutional duty to ensure healthcare for the entire population 11. Brasil. Lei Federal nº 8.080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes e dá outras providências. Diário Oficial da União 1990; 20 set..
Healthcare establishments that serve users of the SUS have diverse organizational compositions, administrative formats, and management models, changing over time due to administrative reforms, legal interpretations, political decisions, and complementary federal, state, and municipal legislations.
In addition to health services provided under direct federal, state, and municipal administration, the public sector delegates or transfers the execution of services under the SUS to indirect administration, which can come under various legal formats, including autarquias (independent agencies), foundations, government-owned companies, and semi-public corporations. For the same purpose of providing healthcare services, public administrators can opt for complementary private administration, signing contracts or agreements with social organizations, nonprofit civil society associations, private foundations, and private companies 22. Scheffer MC, Aith FMA. O sistema de saúde brasileiro. Clín Méd 2016; 1:355-65..
Research on health services management in Brazil 33. Paim J, Travassos C, Almeida C, Bahia L, Macinko J. The Brazilian health system: history, advances, and challenges. Lancet 2011; 377:1778-97. has endeavored to orient the management of hospitals and public healthcare units, administrators’ practices, the nature and oversight of agreements, work processes, and users’ perceptions, especially through reports, essays, case studies, and evaluative studies. As for the health system’s management, studies thus far have examined participatory management, financing, regulation, and evaluation of services 44. Santos JS, Teixeira CF. Política de saúde no Brasil: produção científica 1988-2014. Saúde Debate 2016; 40:219-30..
However, there is an important gap related to the characteristics, functioning, and efficacy of the arrangements and models within the public healthcare system.
The current review focuses on the research production in Public Health, in the subarea Health Policy, Planning, and Management, aimed to summarize trends and priorities in the theoretical and conceptual approaches and the empirical studies on specific health services management modalities in the SUS.
The aim is to contribute to the understanding of the current challenges for improving the health services’ management by adding evidence from studies on the dimensions that characterize, compare, or differentiate the models featured in the literature.
Methodology
A narrative literature review was performed, seeking to summarize the research production on this theme (since the topic was not specific enough to address with a systematic review) 55. Green BN, Johnson CD, Adams A. Writing narrative literature reviews for peer-reviewed journals: secrets of the trade. J Chiropr Med 2006; 5:101-17..
We reviewed Brazil’s domestic research in the field of Public Health on health services management modalities in the SUS. In order to increase its reproducibility and transparency, the review used explicit methods and informed the electronic databases with the terms used in the search strategy, screening strategy, eligibility criteria, data extraction, and summary approach.
The literature search was conducted by a reviewer (A.F.R.) from May 1 to 29, 2017, and included MEDLINE (via PubMed), EMBASE, Latin American and Caribbean Health Sciences Literature (LILACS), Scientific Electronic Library Online (SciELO), and Google Scholar and covered studies published from January 2005 to December 2016. Additional relevant studies were identified in other sources, based on the reference lists from the studies obtained in the electronic search.
The start of the study period was set as the date of approval of the legal framework for one of the possible management modalities, Public-Private Partnerships (PPPs), regulated by Law n. 11,079/200466. Brasil. Lei nº 11.079, de 30 de dezembro de 2004. Institui normas gerais para licitação e contratação de parceria público-privada no âmbito da administração pública. Diário Oficial da União 2004; 31 dez.. The period was thus intended to cover research production on the main alternative management models existing in Brazil at the time.
The search strategies used specific indexing terms (Medical Subject Headings - MeSH; and Descritores em Ciências da Saúde - DeCS). For MEDLINE and EMBASE, the following terms were included: “State Reform”, “Reform of State”, “Models of Health Sector Reform”, “Health Sector Reform”, “Organizational Models”, “Health Organizations”, and “Public-Private Partnerships”. The search also used the filter for date of publication from 2005 and 2016 and limited to “Brazil”.
In the LILACS and SciELO databases, the search terms were: “Reforma do Estado”, “Reforma do Setor Saúde”, “Modelos de Reforma em Saúde”, “Modelos Organizacionais”, “Organizações de Saúde”, “Parceria Público-Privada”, “Modelos de Gestão”, “Gestão de Serviços de Saúde”, and “Gestão do Sistema Único de Saúde”. In both databases, after the search, Brazil was selected as the country pertaining to the topic.
For Google Scholar, we used the specific search system for this database. A manual search was also done in the references from the articles selected in the previous databases. Publications were obtained with the following terms (in Portuguese): “Administração Direta”, “Organização Social”, “Fundação Estatal”, “Fundação Pública”, “Parceria Público Privada”, “PPPs”, “Empresa Brasileira de Serviços Hospitalares”. Free terms were included to increase the search strategy’s sensitivity and identify book chapters, in addition to scientific articles.
Two independent reviewers (A.F.R., P.C.D.S.) first read the publications’ titles and abstracts, and then read the full texts in the second stage. Eligibility criteria for analysis of research production were scientific articles, books, book chapters, theses/dissertations, and reports that presented, described, or discussed the characteristics of at least one health services management model or format in the SUS.
The search first eliminated the publications that did not deal with health-related topics. Then it excluded the publications that dealt with the health system, but on topics unrelated to health services management modalities, such as decentralization, planning, clinical protocols, user satisfaction and participation, human resources, and work processes. Articles on supplementary (private) healthcare services or management of health plans and insurance were not included.
Two independent reviewers (A.F.R., P.C.D.S.) extracted the data (object location, management model, outcomes, study design, data source, type of analysis, number of participants) from the selected publications. In case of disagreement, the decision was made by a third reviewer (M.C.S.), and the publications were then grouped and categorized.
Results
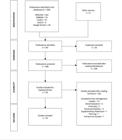
A total of 341 records were identified on the theme, and after exclusion of duplicates, 308 records were screened. At the end of the full reading of 59 publications, 33 were included in the analysis (Figure 1).
The final sample included 27 scientific articles, three reports, two book chapters, and one dissertation. Of the articles, 23 (85%; 23/27) were published in indexed periodicals and four (15%; 4/27) in non-indexed sources. The following indexed periodicals published the most articles included in the review: Ciência & Saúde Coletiva (five articles), Revista de Saúde Pública (four), Cadernos de Saúde Pública (three), and Einstein (two).
Table 1 summarizes the location and types of services, management models analyzed, and study outcomes. The studies that mentioned specific health services management models in the SUS mainly addressed the following: Social Healthcare Organizations - OSS (61%; 20/33), Direct Administration (30%; 10/33), PPPs (30%; 10/33), and Government Foundations (12%; 4/33). Eleven studies (33%; 11/33) examined or compared more than one management model.
Of the 33 selected studies, 18 publications (54%; 16/33) analyzed the management of services located in the State of São Paulo linked to the State Health Secretariat (SES) or some Municipal Health Secretariat. There were two studies (6%; 2/33) on equipment management in the State of Mato Grosso and one (3%; 1/33) that analyzed the PPP model in the following places: Bahia, Ceará, Federal District, Espírito Santo, Mato Grosso, Rio de Janeiro, Roraima, São Paulo, Belo Horizonte (Minas Gerais), Manaus (Amazonas), city of São Paulo, and Sorocaba (São Paulo).
The health services covered in the studies in the literature included public units and hospitals managed by State and Municipal Health Secretariats, besides private and university hospitals. Thirteen articles (39%; 13/33) reported exclusively on hospitals; two articles (6%; 2/33) analyzed hospitals and other health units; one article (3%; 1/33) analyzed a non-hospital health unit. One of the studies (3%; 1/33), with a nationwide scope, addressed both public and private healthcare establishment in general. The other publications (48%; 16/33) did not deal with specific types of health services.
As for the studies’ outcomes, four themes stood out among others in the literature: human resources, contracts and purchases (procurement), control or oversight mechanisms, and financing.
The most frequent study designs were: descriptive (36%; 12/33), qualitative (36%; 12/33), and case studies (33%; 11/33). The most common analytical approaches were comparative (33%; 11/33), descriptive (33%; 11/33), and content analysis (12%; 4/33). As shown in Table 2, some publications used more than one methodology.
Ten articles (30%; 10/33) published comparative analyses, the most frequent of which compared Direct (government) Administration to Social Organizations, addressed in five articles (15%; 5/33).
Sixteen studies (49%; 16/33) used secondary sources, including the scientific literature, documents, and open-access demographic and administrative databases. Three articles (9%; 3/33) only used primary sources, through qualitative approaches, interviews, or focus groups. Another 14 articles (42%; 14/33) included both primary and secondary sources.
Discussion
Part of the literature analyzed here is seeking an explanation for the causes, emergence, and dissemination of alternative management models for public healthcare services. The authors adopted different approaches, including neoliberal premises, state reform, and the presentation of private administrative tools as factors for better or worse health services performance. The management models were presented alternatingly as the modernization or the elimination of the state’s role and responsibilities in health.
The first explanation, exogenous and macropolitical, is situated in the scenario of privatizations 77. Contreiras H, Matta GC. Privatização da gestão do sistema municipal de saúde por meio de Organizações Sociais na cidade de São Paulo, Brasil: caracterização e análise da regulação. Cad Saúde Pública 2015; 31:285-97. and transfer of the government’s responsibilities to the private sector, with a gradual retreat from public policies and dismantlement of the state apparatus 88. Bravo MIS. Política social de saúde no Brasil. In: Mota AES, Bravo MIS, Teixeira M, Uchôa R, Marsiglia RMG, Gomes L, organizadores. Serviço social e saúde: formação e trabalho profissional. São Paulo: Cortez Editora; 2006. p. 1-24.. But the explanation also refers to the management reform scenario, which provided for transferring the supply of public services to social organizations and non-state public providers, which would receive state funding, with their action governed by management contracts. Other objectives included the existence of regulatory agencies, results-based management, and merit-based incentives, under the argument of making public administration more efficient, rationalizing expenditures, and offering citizens services with better quality, assigning greater importance to financial results and the production of services 99. Bresser-Pereira LC. A reforma do estado dos anos 90: lógica e mecanismos de controle. Brasília: Ministério da Administração Federal e Reforma do Estado; 1997.,1010. Bresser-Pereira LC. Reforma gerencial e legitimação do estado social. Rev Adm Pública 2017; 51:147-56..
The second explanation, endogenous to management, was a response to the difficulties encountered by direct government administration in adequately managing health services, due to its low operational capacity, lack of budget financial, and administrative autonomy, low quality control, external political interference, and excessive bureaucracy for hiring staff, making adjustments, and purchasing inputs, medicines, and equipment. Added to the above were the typical rules and procedures of direct government administration and Brazil’s Fiscal Responsibility Law, which limits workforce expansion and qualification 1111. Nogueira RP. O desenvolvimento federativo do SUS e as novas modalidades institucionais de gerência das unidades assistenciais. In: Santos NR, Amarante ODC, organizadores. Gestão pública e relação público privado na saúde. Rio de Janeiro: Centro Brasileiro de Estudos de Saúde; 2011. p. 24-47.,1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.,1313. Couttolenc B, La Forgia G, Matsuda Y. Raising the quality of public spending and resource. Management in the health sector. https://openknowledge.worldbank.org/handle/10986/10292 (acessado em 25/Jun/2017).
https://openknowledge.worldbank.org/hand...
.
The literature reviewed here also addressed the differences between management modalities, based on empirical data produced in the studies and considering the legal configurations and frameworks.
Direct public administration follows the rules governing public service in Brazil, e.g., Art. 37 of the 1988 Federal Constitution and Federal Law n. 8,666 of June 21, 1993 1414. Brasil. Lei nº 8.666, de 21 de junho de 1993. Regulamenta o art. 37, inciso XXI, da Constituição Federal, institui normas para licitações e contratos da Administração Pública e dá outras providências. Diário Oficial da União 1993; 22 jun.. Meanwhile, the so-called Social Organizations, structural entities of the 1995 state administrative reform 1010. Bresser-Pereira LC. Reforma gerencial e legitimação do estado social. Rev Adm Pública 2017; 51:147-56., were regulated by Federal Law n. 9,637 of May 15, 1998 1515. Brasil. Lei nº 9.637, de 15 de maio de 1998. Dispõe sobre a qualificação de entidades como organizações sociais, a criação do Programa Nacional de Publicização, a extinção dos órgãos e entidades que menciona e a absorção de suas atividades por organizações sociais, e dá outras providências. Diário Oficial da União 1998; 18 mai. and state and municipal legislations, and reconfirmed by the Federal Supreme Court in 2015 1616. Supremo Tribunal Federal. Ação Direta de Inconstitucionalidade nº 1.923. http://www.stf.jus.br/portal/processo/verProcessoAndamento.asp?numero=1923&classe=ADI&origem=AP&recurso=0&tipoJulgamento=M (acessado em 25/Jun/2017).
http://www.stf.jus.br/portal/processo/ve...
. PPPs, governed by private law, were established under Federal Law n. 11,079 of December 30, 2004 66. Brasil. Lei nº 11.079, de 30 de dezembro de 2004. Institui normas gerais para licitação e contratação de parceria público-privada no âmbito da administração pública. Diário Oficial da União 2004; 31 dez.. Although there is no specific legislation, there are bills under review 1717. Brasil. Projeto Fundação Estatal - principais aspectos. Brasília: Ministério do Planejamento, Orçamento e Gestão; 2007. in the Brazilian Congress to regulate the Government Foundations as entities of indirect public administration, providing them with greater flexibility and autonomy than the current autarquias and public foundations. The Government Foundations were proposed under Complementary Bill of Law n. 92/2007, which regulates Art. 37, item XIX, of the 1988 Federal Constitution1111. Nogueira RP. O desenvolvimento federativo do SUS e as novas modalidades institucionais de gerência das unidades assistenciais. In: Santos NR, Amarante ODC, organizadores. Gestão pública e relação público privado na saúde. Rio de Janeiro: Centro Brasileiro de Estudos de Saúde; 2011. p. 24-47.,1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40..
The public procurement process is one of the principal elements in the rules governing Public Administration, establishing a series of duties and procedures for signing a contract or making a purchase. For Direct Administration, Law n. 8,666/1993 applies in full, leaving less flexibility 1818. Barbosa NB, Elias PEM. As organizações sociais de saúde como forma de gestão público/privado. Ciênc Saúde Coletiva 2010; 15:2483-95.. Government Foundations, as entities of Indirect Administration, allow more streamlined procedures due to their own specific regulations for public bidding (although still ruled by Law n. 8,666/19931111. Nogueira RP. O desenvolvimento federativo do SUS e as novas modalidades institucionais de gerência das unidades assistenciais. In: Santos NR, Amarante ODC, organizadores. Gestão pública e relação público privado na saúde. Rio de Janeiro: Centro Brasileiro de Estudos de Saúde; 2011. p. 24-47.). Meanwhile, the OSS enjoy some flexibility since they are not subject to government procurement rules; their obligations are set in the form of management contracts 1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.,1919. Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80.. Finally, the purchases made by PPPs are not subject to the restrictions imposed on the other management modalities 2020. Anker T, Pereira BR. O atual cenário das PPPs no setor de saúde pública no Brasil: potencialidades, desafios e as primeiras experiências em âmbito estadual. In: Oliveira G, Oliveira Filho LC, organizadores. Parcerias público-privadas: experiências, desafios e propostas. São Paulo: LTC; 2013. p. 159-80.,2121. Matzuda Y, Rinne J, Shepherd G, Wenceslau J. Enhancing performance in Brazil's health sector: lessons from innovations in the State of São Paulo and the city of Curitiba. http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba (acessado em 25/Jun/2017).
http://documents.worldbank.org/curated/p...
.
The formats for hiring and paying human resources, plus the meritocracy and results-based policies, were addressed by various studies in the current review of management models. In Direct Administration, staff hiring must comply with Art. 37 of the 1988 Federal Constitution, which requires public admissions exams and job stability, with the exception of positions subject to free nomination and dismissal, a situation that sometimes generates difficulties in updating the workforce 2222. André AM, Ciampone MHT, Santelle O. Tendências de gerenciamento de unidades de saúde e de pessoas. Rev Saúde Pública 2013; 47:158-63.,2323. Lorenzetti J, Lanzoni GMM, Assuiti LFCA, Pires DEP, Ramos FRS. Gestão em saúde no Brasil: diálogo com gestores públicos e privados. Texto & Contexto Enferm 2014; 23:417-25.. However, this requirement does not exist in the other models. With some differences, the models allow hiring staff according to Brazil’s Consolidated Labor Laws (CLT) 1818. Barbosa NB, Elias PEM. As organizações sociais de saúde como forma de gestão público/privado. Ciênc Saúde Coletiva 2010; 15:2483-95.,1919. Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80.,2424. Ditterich RG, Moysés ST, Moysés SJ. O uso de contratos de gestão e incentivos profissionais no setor público de saúde. Cad Saúde Pública 2012; 28:615-25.,2525. Quinhões TAT. O modelo de governança das Organizações Sociais de Saúde (OSS) e a qualidade do gasto público hospitalar corrente. In: XIV Prêmio Tesouro Nacional 2009. http://www3.tesouro.fazenda.gov.br/Premio_TN/XIVPremio/qualidade/1qualidadeXIVPTN/Monografia_Tema4_Trajano_Augustus.pdf (acessado em 25/Jun/2017).
http://www3.tesouro.fazenda.gov.br/Premi...
,2626. Barbosa NB. Regulação do trabalho no contexto das novas relações público versus privado na saúde. Ciênc Saúde Coletiva 2012; 15:2497-506.. In addition to the flexibilization, there is a positive result in human resources management under OSS when compared to Direct Administration in cases where a change in organizational culture has been identified, with greater employee participation and accountability 2727. Costa e Silva V, Barbosa PR, Hortale VA. Parcerias na saúde: as Organizações Sociais como limites e possibilidades na gerência da Estratégia Saúde da Família. Ciênc Saúde Coletiva 2016; 21:1365-76..
As for financing of services, the Foundations are paid as a function of production, with payment usually tied to pre-agreed targets 1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.,2828. Lima SML, Rivera FJU. A contratualização nos hospitais de ensino no Sistema Único de Saúde brasileiro. Ciênc Saúde Coletiva 2012; 17:2507-21.. Pay for performance is also a tool used to finance OSS, through management contracts 1919. Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80.,2929. Santos MAB, Madeira FC, Passos SRL, Bakr F, Oliveira KB, Andreazzi MAR. Autonomia financeira em estabelecimentos públicos e privados de saúde no Brasil. Cad Saúde Pública 2014; 30:201-6.. PPPs are also financed according to rules and criteria set during the bidding process 2020. Anker T, Pereira BR. O atual cenário das PPPs no setor de saúde pública no Brasil: potencialidades, desafios e as primeiras experiências em âmbito estadual. In: Oliveira G, Oliveira Filho LC, organizadores. Parcerias público-privadas: experiências, desafios e propostas. São Paulo: LTC; 2013. p. 159-80.,3030. Barbosa AP, Malik AM. Desafios na organização de parcerias público-privadas em saúde no Brasil. Análise de projetos estruturados entre janeiro de 2010 e março de 2014. Rev Adm Pública 2015; 49:1143-65..
Regardless of the management model, formal internal and external control mechanisms are provided for, such as supervision by the Brazilian Ministry of Health, oversight and evaluation by the Federal, State, and Municipal Accounts Courts and Offices of the Public Prosecutors, subordination to social control by the community-based Health Councils, and duties as to publicity of decisions, expenditures, and contracts 1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.. The OSS and PPPs are limited by management contracts and performance measurement. As long as there is agreement on targets, instruments for follow-up, objective criteria to assess production, and budgetary limits, theoretically it is possible to evaluate and demand better performance from the Social Organizations 1919. Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80.. Meanwhile, the PPPs are presented as having a unique oversight model, through the “establishment of output-based performance indicators, that is, based on targets and results (...) measured a posteriori” 2020. Anker T, Pereira BR. O atual cenário das PPPs no setor de saúde pública no Brasil: potencialidades, desafios e as primeiras experiências em âmbito estadual. In: Oliveira G, Oliveira Filho LC, organizadores. Parcerias público-privadas: experiências, desafios e propostas. São Paulo: LTC; 2013. p. 159-80. (p. 163). Payment for the services provided only occurs after ensuring the scope of what was stipulated in the contract.
Despite the formal oversight and performance assessment mechanisms, the literature points to flaws in the delegation of public health services to management not conducted by Direct Administration. In the case of OSS, the rhetoric of the benefits of managerialism may fail to weigh the private interests involved in healthcare management 3131. Puccini PT. As Organizações Sociais e o direito à saúde. http://idisa.org.br/img/File/SUS%20OS%20Paulo%20Puccini%20Fim%206_4_2011.pdf (acessado em 11/Mar/2018).
http://idisa.org.br/img/File/SUS%20OS%20...
. Concerning the PPPs, based on a descriptive and conceptual discussion 3232. Sodré F, Littike D, Drago LMB, Perim MCM. Empresa Brasileira de Serviços Hospitalares: um novo modelo de gestão? Serv Soc Soc 2013; 114:365-80. and interaction with relevant actors in this model’s implementation 3333. Cabral S, Fernandes ASA, Ribeiro DBC. Os papéis dos stakeholders na implementação das parcerias público-privadas no Estado da Bahia. Cadernos EBAPE.BR 2016; 14:325-39., the literature indicated the private sector’s capacity to influence and enable projects in which it has a vested interest, with a view towards obtaining profits.
Even when dealing with real-life cases, the research focused predominantly on the model’s conceptual perspective, normative framework, underlying legislation, management practices, and contractual relations.
A few studies also criticized the OSS’ lack of accounting transparency 3434. Camargo TA, Prado O, Bernardo R, Lara ACHS. Controle e transparência no modelo de organizações sociais de saúde do Estado de São Paulo. In: VI Congresso Consad de Gestão Pública 2013. http://www.escoladegestao.pr.gov.br/arquivos/File/2013/V_CONSAD/VI_CONSAD/050.pdf (acessado em 25/Jun/2017).
http://www.escoladegestao.pr.gov.br/arqu...
, besides exposing the private interests involved in the services’ management 3131. Puccini PT. As Organizações Sociais e o direito à saúde. http://idisa.org.br/img/File/SUS%20OS%20Paulo%20Puccini%20Fim%206_4_2011.pdf (acessado em 11/Mar/2018).
http://idisa.org.br/img/File/SUS%20OS%20...
and questioning the alleged expansion of the population’s access to the services provided by these models 3535. Carneiro Junior N, Elias PEM. Controle público e equidade no acesso a hospitais sob gestão pública não estatal. Rev Saúde Pública 2006; 40:914-20..
There was no consensus among the few comparative studies as to the superiority of one model over another. Public hospitals managed by OSS showed higher economic efficiency and human resources management when compared to Direct Administration 1212. Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.,1919. Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80., in addition to lower expenditure per hospital bed 3636. La Forgia GM, Harding A. Public-private partnerships and public hospital performance in São Paulo, Brazil. Health Aff (Millwood) 2009; 28:1114-26.. Still, services administered by OSS in São Paulo performed similarly to services under Direct Administration in Curitiba (Paraná) 2121. Matzuda Y, Rinne J, Shepherd G, Wenceslau J. Enhancing performance in Brazil's health sector: lessons from innovations in the State of São Paulo and the city of Curitiba. http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba (acessado em 25/Jun/2017).
http://documents.worldbank.org/curated/p...
. As for staff performance, due to greater flexibility in hiring and wage procedures 1818. Barbosa NB, Elias PEM. As organizações sociais de saúde como forma de gestão público/privado. Ciênc Saúde Coletiva 2010; 15:2483-95., the workforce under OSS were more highly qualified, according to one study 2727. Costa e Silva V, Barbosa PR, Hortale VA. Parcerias na saúde: as Organizações Sociais como limites e possibilidades na gerência da Estratégia Saúde da Família. Ciênc Saúde Coletiva 2016; 21:1365-76.. Meanwhile, another study found no difference between OSS and Direct Administration in terms of human resources management 2121. Matzuda Y, Rinne J, Shepherd G, Wenceslau J. Enhancing performance in Brazil's health sector: lessons from innovations in the State of São Paulo and the city of Curitiba. http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba (acessado em 25/Jun/2017).
http://documents.worldbank.org/curated/p...
. PPPs and Government Foundations were not even compared to other models, perhaps because they are still not as common in Brazil.
Studies with comparisons of models were not only few in number, but methodologically limited. Only one study conducted economic assessments comparing two or more alternative models, simultaneously evaluating costs and results 3636. La Forgia GM, Harding A. Public-private partnerships and public hospital performance in São Paulo, Brazil. Health Aff (Millwood) 2009; 28:1114-26.. No quality assessments or comparative analyses were done on health services management under different models, considering characteristics such as accessibility, equity, satisfaction, or efficiency.
Neither were there any studies on possible impasses with the coexistence of different models in the same healthcare network or the repercussions from the coexistence of heterogeneous management models on staff, services, and pay, which can impact the organization and functioning of the health system as a whole or even hinder the configuration of an integrated network of services linked at increasingly complex levels in order to guarantee comprehensive healthcare in each given region.
The review also failed to identify any systematic or narrative literature review or the use of surveys with managers, users, and health professionals, just to mention two examples of methodological procedures that could have been employed to analyze a given model in greater depth or to compare one modality to another.
The review showed a heavy concentration of studies in the State of São Paulo, with 18 publications (55%; 18/33). According to the Brazilian Survey of Medical-Sanitary Assistance (Brazilian Institute of Geography and Statistics. http://www.ibge.gov.br/home/estatistica/populacao/condicaodevida/ams/2009/, accessed on 18/Jun/2017), in 2009, of the 94,070 public and private, for-profit and non-profit, outpatient and inpatient healthcare establishments in Brazil, 15% (14,215) were located in the State of São Paulo. Considering the nationwide presence of alternative (non-Direct Administration) health services management modalities, the concentration of studies in São Paulo does not reflect the establishments’ national distribution and fails explore the models’ diversity of characteristics and outcomes.
With a predominance of qualitative studies, the review showed that most of the selected studies provided weak descriptions of their methodologies, and that some descriptive and content analyses failed to produce conclusions or even interpretative inferences. The theoretical and methodological references used in the articles were limited, corroborating a previous study by Deslandes &Iriart 3737. Deslandes SF, Iriart JAB. Usos teórico-metodológicos das pesquisas na área de Ciências Sociais e Humanas em Saúde. Cad Saúde Pública 2012; 28:2380-6.. The latter authors analyzed the repertoire of methodologies in scientific production on social and human sciences in health and concluded, “there is a monotony and predominance of few analytical modalities and data production techniques, narrowing what would otherwise be a wide range of choices and innovative research approaches” 3737. Deslandes SF, Iriart JAB. Usos teórico-metodológicos das pesquisas na área de Ciências Sociais e Humanas em Saúde. Cad Saúde Pública 2012; 28:2380-6. (p. 2385).
As with non-Brazilian reviews 3838. Basu S, Andrews J, Kishore S, Panjabi R, Stuckler D. Comparative performance of private and public healthcare systems in low- and middle-income countries: a systematic review. PLoS Med 2012; 9:e1001244.,3939. Rao S. Is the private sector more efficient? A cautionary tale. http://www.gsdrc.org/document-library/is-the-private-sector-more-efficient-a-cautionary-tale/ (acessado em 25/Jun/2017).
http://www.gsdrc.org/document-library/is...
, the current review provided little evidence of the real impact of alternative models or public-private arrangements on health services management. It has not been proven that one model is intrinsically more efficient than (or superior to) another, although isolated case studies attribute the results of given services or those in specific contexts to the management modality.
The comparative analyses of the healthcare management models’ efficiency or quality characteristics (public, private, for-profit, non-profit, mixed) concluded that the differences are scarcely significant or nonconclusive 1818. Barbosa NB, Elias PEM. As organizações sociais de saúde como forma de gestão público/privado. Ciênc Saúde Coletiva 2010; 15:2483-95.,2121. Matzuda Y, Rinne J, Shepherd G, Wenceslau J. Enhancing performance in Brazil's health sector: lessons from innovations in the State of São Paulo and the city of Curitiba. http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba (acessado em 25/Jun/2017).
http://documents.worldbank.org/curated/p...
,3636. La Forgia GM, Harding A. Public-private partnerships and public hospital performance in São Paulo, Brazil. Health Aff (Millwood) 2009; 28:1114-26.. Efficiency in services provision, whatever the management model, will depend on the health system’s characteristics and factors such as financing, regulation, external social control, degree of public monitoring of the execution of outsourced or hired services, competition, institutional development, and staff hiring and payment policies.
Conclusion
In conclusion, the Brazilian literature on health services management models in the SUS has produced few articles, geographically concentrated, mainly in the State of São Paulo, with only a handful of studies on the more recently introduced or less widespread modalities. This limited research production is marked by a narrow diversity of theories and weak methodological approaches, emphasizing the legal frameworks and configurations and focusing on the hiring, contractual, procurement, human resources, financing, and control processes.
The review points to the need for more in-depth research in keeping with the system’s complexity and scope, considering that alternative (non-Direct Administration) management models are now hegemonic in most of Brazil’s municipal and state public healthcare networks.
The approaches that call for more studies would include the shareholding formats, the experience with the expansion of coverage and capital accumulation by the organizations, entities, and companies working with services management in the SUS, as well as networks of influence and the mechanisms used by them to defend their vested interests vis-à-vis government policymakers.
The current study also suggests the importance of adopting other methodological approaches in the literature on the issue, in order to produce evaluative studies capable of comparing different models and drawing on research procedures, methods, and instruments by which the management modality can be judged for its performance and its effects on quality of care, the population’s health, and organization of the health system.
Acknowledgments
The authors wish to thank the Director of the Department of Preventive Medicine, School of Medicine, São Paulo University, who approved this research project within the Master’s Program in Health Policy, Planning, and Management, and CNPq for research project grant n. 405077/2013-0.
Referências
-
1Brasil. Lei Federal nº 8.080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes e dá outras providências. Diário Oficial da União 1990; 20 set.
-
2Scheffer MC, Aith FMA. O sistema de saúde brasileiro. Clín Méd 2016; 1:355-65.
-
3Paim J, Travassos C, Almeida C, Bahia L, Macinko J. The Brazilian health system: history, advances, and challenges. Lancet 2011; 377:1778-97.
-
4Santos JS, Teixeira CF. Política de saúde no Brasil: produção científica 1988-2014. Saúde Debate 2016; 40:219-30.
-
5Green BN, Johnson CD, Adams A. Writing narrative literature reviews for peer-reviewed journals: secrets of the trade. J Chiropr Med 2006; 5:101-17.
-
6Brasil. Lei nº 11.079, de 30 de dezembro de 2004. Institui normas gerais para licitação e contratação de parceria público-privada no âmbito da administração pública. Diário Oficial da União 2004; 31 dez.
-
7Contreiras H, Matta GC. Privatização da gestão do sistema municipal de saúde por meio de Organizações Sociais na cidade de São Paulo, Brasil: caracterização e análise da regulação. Cad Saúde Pública 2015; 31:285-97.
-
8Bravo MIS. Política social de saúde no Brasil. In: Mota AES, Bravo MIS, Teixeira M, Uchôa R, Marsiglia RMG, Gomes L, organizadores. Serviço social e saúde: formação e trabalho profissional. São Paulo: Cortez Editora; 2006. p. 1-24.
-
9Bresser-Pereira LC. A reforma do estado dos anos 90: lógica e mecanismos de controle. Brasília: Ministério da Administração Federal e Reforma do Estado; 1997.
-
10Bresser-Pereira LC. Reforma gerencial e legitimação do estado social. Rev Adm Pública 2017; 51:147-56.
-
11Nogueira RP. O desenvolvimento federativo do SUS e as novas modalidades institucionais de gerência das unidades assistenciais. In: Santos NR, Amarante ODC, organizadores. Gestão pública e relação público privado na saúde. Rio de Janeiro: Centro Brasileiro de Estudos de Saúde; 2011. p. 24-47.
-
12Ibañez N, Vecina Neto G. Modelos de gestão e o SUS. Ciênc Saúde Coletiva 2007; 12:1831-40.
-
13Couttolenc B, La Forgia G, Matsuda Y. Raising the quality of public spending and resource. Management in the health sector. https://openknowledge.worldbank.org/handle/10986/10292 (acessado em 25/Jun/2017).
» https://openknowledge.worldbank.org/handle/10986/10292 -
14Brasil. Lei nº 8.666, de 21 de junho de 1993. Regulamenta o art. 37, inciso XXI, da Constituição Federal, institui normas para licitações e contratos da Administração Pública e dá outras providências. Diário Oficial da União 1993; 22 jun.
-
15Brasil. Lei nº 9.637, de 15 de maio de 1998. Dispõe sobre a qualificação de entidades como organizações sociais, a criação do Programa Nacional de Publicização, a extinção dos órgãos e entidades que menciona e a absorção de suas atividades por organizações sociais, e dá outras providências. Diário Oficial da União 1998; 18 mai.
-
16Supremo Tribunal Federal. Ação Direta de Inconstitucionalidade nº 1.923. http://www.stf.jus.br/portal/processo/verProcessoAndamento.asp?numero=1923&classe=ADI&origem=AP&recurso=0&tipoJulgamento=M (acessado em 25/Jun/2017).
» http://www.stf.jus.br/portal/processo/verProcessoAndamento.asp?numero=1923&classe=ADI&origem=AP&recurso=0&tipoJulgamento=M -
17Brasil. Projeto Fundação Estatal - principais aspectos. Brasília: Ministério do Planejamento, Orçamento e Gestão; 2007.
-
18Barbosa NB, Elias PEM. As organizações sociais de saúde como forma de gestão público/privado. Ciênc Saúde Coletiva 2010; 15:2483-95.
-
19Sano H, Abrucio FL. Promessas e resultados da nova gestão pública no Brasil: o caso das organizações sociais de saúde em São Paulo. Revista de Administração de Empresas 2008; 48:64-80.
-
20Anker T, Pereira BR. O atual cenário das PPPs no setor de saúde pública no Brasil: potencialidades, desafios e as primeiras experiências em âmbito estadual. In: Oliveira G, Oliveira Filho LC, organizadores. Parcerias público-privadas: experiências, desafios e propostas. São Paulo: LTC; 2013. p. 159-80.
-
21Matzuda Y, Rinne J, Shepherd G, Wenceslau J. Enhancing performance in Brazil's health sector: lessons from innovations in the State of São Paulo and the city of Curitiba. http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba (acessado em 25/Jun/2017).
» http://documents.worldbank.org/curated/pt/664271468016810488/Brazil-Enhancing-performance-in-Brazils-health-sector-lessons-from-innovations-in-the-state-of-Sao-Paulo-and-the-city-of-Curitiba -
22André AM, Ciampone MHT, Santelle O. Tendências de gerenciamento de unidades de saúde e de pessoas. Rev Saúde Pública 2013; 47:158-63.
-
23Lorenzetti J, Lanzoni GMM, Assuiti LFCA, Pires DEP, Ramos FRS. Gestão em saúde no Brasil: diálogo com gestores públicos e privados. Texto & Contexto Enferm 2014; 23:417-25.
-
24Ditterich RG, Moysés ST, Moysés SJ. O uso de contratos de gestão e incentivos profissionais no setor público de saúde. Cad Saúde Pública 2012; 28:615-25.
-
25Quinhões TAT. O modelo de governança das Organizações Sociais de Saúde (OSS) e a qualidade do gasto público hospitalar corrente. In: XIV Prêmio Tesouro Nacional 2009. http://www3.tesouro.fazenda.gov.br/Premio_TN/XIVPremio/qualidade/1qualidadeXIVPTN/Monografia_Tema4_Trajano_Augustus.pdf (acessado em 25/Jun/2017).
» http://www3.tesouro.fazenda.gov.br/Premio_TN/XIVPremio/qualidade/1qualidadeXIVPTN/Monografia_Tema4_Trajano_Augustus.pdf -
26Barbosa NB. Regulação do trabalho no contexto das novas relações público versus privado na saúde. Ciênc Saúde Coletiva 2012; 15:2497-506.
-
27Costa e Silva V, Barbosa PR, Hortale VA. Parcerias na saúde: as Organizações Sociais como limites e possibilidades na gerência da Estratégia Saúde da Família. Ciênc Saúde Coletiva 2016; 21:1365-76.
-
28Lima SML, Rivera FJU. A contratualização nos hospitais de ensino no Sistema Único de Saúde brasileiro. Ciênc Saúde Coletiva 2012; 17:2507-21.
-
29Santos MAB, Madeira FC, Passos SRL, Bakr F, Oliveira KB, Andreazzi MAR. Autonomia financeira em estabelecimentos públicos e privados de saúde no Brasil. Cad Saúde Pública 2014; 30:201-6.
-
30Barbosa AP, Malik AM. Desafios na organização de parcerias público-privadas em saúde no Brasil. Análise de projetos estruturados entre janeiro de 2010 e março de 2014. Rev Adm Pública 2015; 49:1143-65.
-
31Puccini PT. As Organizações Sociais e o direito à saúde. http://idisa.org.br/img/File/SUS%20OS%20Paulo%20Puccini%20Fim%206_4_2011.pdf (acessado em 11/Mar/2018).
» http://idisa.org.br/img/File/SUS%20OS%20Paulo%20Puccini%20Fim%206_4_2011.pdf -
32Sodré F, Littike D, Drago LMB, Perim MCM. Empresa Brasileira de Serviços Hospitalares: um novo modelo de gestão? Serv Soc Soc 2013; 114:365-80.
-
33Cabral S, Fernandes ASA, Ribeiro DBC. Os papéis dos stakeholders na implementação das parcerias público-privadas no Estado da Bahia. Cadernos EBAPE.BR 2016; 14:325-39.
-
34Camargo TA, Prado O, Bernardo R, Lara ACHS. Controle e transparência no modelo de organizações sociais de saúde do Estado de São Paulo. In: VI Congresso Consad de Gestão Pública 2013. http://www.escoladegestao.pr.gov.br/arquivos/File/2013/V_CONSAD/VI_CONSAD/050.pdf (acessado em 25/Jun/2017).
» http://www.escoladegestao.pr.gov.br/arquivos/File/2013/V_CONSAD/VI_CONSAD/050.pdf -
35Carneiro Junior N, Elias PEM. Controle público e equidade no acesso a hospitais sob gestão pública não estatal. Rev Saúde Pública 2006; 40:914-20.
-
36La Forgia GM, Harding A. Public-private partnerships and public hospital performance in São Paulo, Brazil. Health Aff (Millwood) 2009; 28:1114-26.
-
37Deslandes SF, Iriart JAB. Usos teórico-metodológicos das pesquisas na área de Ciências Sociais e Humanas em Saúde. Cad Saúde Pública 2012; 28:2380-6.
-
38Basu S, Andrews J, Kishore S, Panjabi R, Stuckler D. Comparative performance of private and public healthcare systems in low- and middle-income countries: a systematic review. PLoS Med 2012; 9:e1001244.
-
39Rao S. Is the private sector more efficient? A cautionary tale. http://www.gsdrc.org/document-library/is-the-private-sector-more-efficient-a-cautionary-tale/ (acessado em 25/Jun/2017).
» http://www.gsdrc.org/document-library/is-the-private-sector-more-efficient-a-cautionary-tale/ -
40Pacheco HF, Gurgel Júnior GD, Santos FAS, Ferreira SCC, Leal EMM. Organizações sociais como modelo de gestão da assistência à saúde em Pernambuco, Brasil: percepção de gestores. Interface (Botucatu, Online) 2016; 20:585-95.
-
41Romano CMC, Scatena JHG, Kehrig RT. Articulação público-privada na atenção ambulatorial de média e alta complexidade do SUS: atuação da Secretaria de Estado de Saúde de Mato Grosso. Physis (Rio J.) 2015; 25:1095-115.
-
42Rodrigues CT, Spagnuolo RS. Organizações Sociais de Saúde: potencialidades e limites na gestão pública. Rev Eletrônica Enferm 2014; 16:549-57.
-
43Barata LRB, Mendes JDV. Organizações Sociais de Saúde: a experiência exitosa de gestão pública de saúde do Estado de São Paulo. São Paulo: Secretaria Estadual de Saúde; 2007.
-
44Melo TBN, Almeida MR. Parceria público-privada: a gestão privada em hospitais universitários no Rio Grande do Norte. Revista de Saúde Pública de Santa Catarina 2014; 7:46-62.
-
45Mendes CA, Martins AA, Teivelis MP, Kuzniec S, Wolosker N. Parceria público-privada em cirurgia vascular. Einstein (São Paulo) 2014; 12:342-6.
-
46Kaliks RA, Pontes LB, Bognar CLFB, Santos KCC, Bromberg SE, Amaral PGT, et al. Pacientes com câncer de mama oriundas do Sistema Único de Saúde tratadas no setor privado: custos de um piloto de parceria público-privada em oncologia. Einstein (São Paulo) 2013; 11:216-23.
-
47Andreazzi MFS. Empresa Brasileira de Serviços Hospitalares: inconsistências à luz da reforma do Estado. Rev Bras Educ Méd 2013; 37:275-84.
-
48Maciel BC, Wichert MAAL, Peroni SP, Próspero UOS. Gestão em parceria entre uma fundação de apoio e um hospital público universitário: análise custo-efetividade. Revista de Administração 2005; 40:342-52.
-
49Costa e Silva V, Escoval A, Hortale VA. Contratualização na Atenção Primária à Saúde: a experiência de Portugal e Brasil. Ciênc Saúde Coletiva 2014; 19:3593-604.
-
50La Forgia GM, Couttolenc BF. Hospital performance in Brazil: the search for excellence. https://openknowledge.worldbank.org/handle/10986/10284 (acessado em 25/Jun/2017).
» https://openknowledge.worldbank.org/handle/10986/10284
Publication Dates
-
Publication in this collection
2018
History
-
Received
04 July 2017 -
Reviewed
12 Jan 2018 -
Accepted
26 Jan 2018