Abstracts
Asthma results from a combination of three essential features: airflow obstruction, hyperresponsiveness of airways to endogenous or exogenous stimuli and inflammation. Inadequacy of the techniques to use different inhalation devices is one of the causes of therapeutic failure. The main purpose of this study was to evaluate how 20 medical students, 36 resident physicians of Internal Medicine/Pediatrics, and 40 asthma patients used three devices for inhalation therapy containing placebo. All patients were followed at the Pulmonary Outpatient Service of Botucatu Medical School and had been using inhaled medication for at least six months. The following devices were evaluated: metered dose inhalers (MDI), dry powder inhalers (DPI), and MDI attached to a spacer device. A single observer applied a protocol containing the main steps necessary to obtain a good inhaler technique to follow and grade the use of different devices. Health care professionals tested all three devices and patients tested only the device being used on their management. MDI was the device best known by doctors and patients. MDI use was associated with errors related to the coordination between inspiration and device activation. Failure to exhale completely before inhalation of the powder was the most frequent error observed with DPI use. In summary, patients did not receive precise instruction on how to use inhaled medication and health care professionals were not well prepared to adequately teach their patients.
Asthma; Administration, inhalation; Techniques; Students, medical; Medical Staff, hospital
A asma resulta da combinação de três características essenciais: obstrução das vias aéreas, hiper-responsividade brônquica e inflamação. O uso dos inalantes com técnica inadequada tem sido apontado como um dos responsáveis pelo fracasso terapêutico. O objetivo deste estudo foi avaliar o domínio da técnica de uso das medicações inalatórias de 20 estudantes do 6º ano médico, 36 médicos residentes em Clínica Médica/Pediatria e de 40 pacientes. Os pacientes eram acompanhados no Ambulatório de Pneumologia do HC/Unesp e estavam em uso de medicação inalatória durante pelo menos seis meses. Os dispositivos avaliados foram: nebulímetros pressurizados (NEPS), nebulímetros com espaçadores (ESP) e inaladores de pó seco (IPS). A técnica foi observada e pontuada por examinador único, de acordo com protocolo apropriado. Os profissionais de saúde demonstraram a técnica com os três tipos de inalantes citados, enquanto os pacientes foram avaliados somente nos que faziam parte do seu tratamento. O NEP foi o dispositivo mais conhecido tanto por médicos quanto por pacientes. Para o NEP, os erros mais comuns, em todos os grupos estudados, foram os relacionados com a coordenação entre a inspiração e o acionamento do dispositivo. Para o IPS, foi a não realização da expiração máxima antes da inalação do medicamento. Foi observado que os pacientes apresentavam grande carência de informações precisas quanto ao uso dos dispositivos e que os profissionais desconheciam a técnica ou sentiam-se inseguros quanto à melhor forma de ensinar seus pacientes, optando, muitas vezes, por não orientá-los.
Asma; Administração por inalação; Técnicas; Estudantes de medicina; Médicos residentes
ORIGINAL ARTICLE
Inhaled medication for asthma management: evaluation of how asthma patients, medical students, and doctors use the different devices* Correspondence to Rua João Carmelo,185 A, Jardim Paraíso Botucatu, SP Phones. (14) 6824-7779/(14) 9798-7773
Inalantes no tratamento da asma: avaliação do domínio das técnicas de uso por pacientes, alunos de medicina e médicos residentes
Janaína Barbosa MunizI; Carlos Roberto PadovaniII; Irma GodoyIII
ISenior graduate student of Medicine of the Medical School of Botucatu/Unesp
IIFull Professor of the Department of Statistics of Bioscience Institute /Unesp
IIIAssociate Professor of Pneumology and of Internal Medicine, Medical School of Botucatu/Unesp
Correspondence Correspondence to Rua João Carmelo,185 A, Jardim Paraíso Botucatu, SP Phones. (14) 6824-7779/(14) 9798-7773
ABSTRACT
Asthma results from a combination of three essential features: airflow obstruction, hyperresponsiveness of airways to endogenous or exogenous stimuli and inflammation. Inadequacy of the techniques to use different inhalation devices is one of the causes of therapeutic failure. The main purpose of this study was to evaluate how 20 medical students, 36 resident physicians of Internal Medicine/Pediatrics, and 40 asthma patients used three devices for inhalation therapy containing placebo. All patients were followed at the Pulmonary Outpatient Service of Botucatu Medical School and had been using inhaled medication for at least six months. The following devices were evaluated: metered dose inhalers (MDI), dry powder inhalers (DPI), and MDI attached to a spacer device. A single observer applied a protocol containing the main steps necessary to obtain a good inhaler technique to follow and grade the use of different devices. Health care professionals tested all three devices and patients tested only the device being used on their management. MDI was the device best known by doctors and patients. MDI use was associated with errors related to the coordination between inspiration and device activation. Failure to exhale completely before inhalation of the powder was the most frequent error observed with DPI use. In summary, patients did not receive precise instruction on how to use inhaled medication and health care professionals were not well prepared to adequately teach their patients.
Key words: Asthma. Administration, inhalation. Techniques. Students, medical. Medical Staff, hospital.
RESUMO
A asma resulta da combinação de três características essenciais: obstrução das vias aéreas, hiper-responsividade brônquica e inflamação. O uso dos inalantes com técnica inadequada tem sido apontado como um dos responsáveis pelo fracasso terapêutico. O objetivo deste estudo foi avaliar o domínio da técnica de uso das medicações inalatórias de 20 estudantes do 6º ano médico, 36 médicos residentes em Clínica Médica/Pediatria e de 40 pacientes. Os pacientes eram acompanhados no Ambulatório de Pneumologia do HC/Unesp e estavam em uso de medicação inalatória durante pelo menos seis meses. Os dispositivos avaliados foram: nebulímetros pressurizados (NEPS), nebulímetros com espaçadores (ESP) e inaladores de pó seco (IPS). A técnica foi observada e pontuada por examinador único, de acordo com protocolo apropriado. Os profissionais de saúde demonstraram a técnica com os três tipos de inalantes citados, enquanto os pacientes foram avaliados somente nos que faziam parte do seu tratamento. O NEP foi o dispositivo mais conhecido tanto por médicos quanto por pacientes. Para o NEP, os erros mais comuns, em todos os grupos estudados, foram os relacionados com a coordenação entre a inspiração e o acionamento do dispositivo. Para o IPS, foi a não realização da expiração máxima antes da inalação do medicamento. Foi observado que os pacientes apresentavam grande carência de informações precisas quanto ao uso dos dispositivos e que os profissionais desconheciam a técnica ou sentiam-se inseguros quanto à melhor forma de ensinar seus pacientes, optando, muitas vezes, por não orientá-los.
Descritores: Asma. Administração por inalação. Técnicas. Estudantes de medicina. Médicos residentes.
Abbreviations used in this paper
FRC Forced residual capacity
RV Residual volume
MDI metered dose inhaler
ESP MDI attached to a spacer device
DPI Dry powder inhaler
INTRODUCTION
Asthma is defined as an "chronic inflammatory disease of the upper airways, in which several cells play an important role, especially mast cells, eosinophils and T lymphocytes. In susceptible individuals, this inflammation causes recurrent episodes of hissing, dyspnea, chest weight and cough, especially at night and/or when waking up, besides increasing the resistance of the upper airways to several stimuli. These symptoms are usually associated with a wide but variable obstruction of the airflow, which is, at least partially, possible of being reversed spontaneously or after the treatment" (1).
In Brazil, ISAAC's data (International Study of Asthma and Allergies in Childhood) show a prevalence of asthma between 4.7 and 20.7% for the age range of six to seven years, and between 4.8 and 21%, for the age range of 13 to 14 years. International and national studies show the general trend of increasing asthma prevalence, morbidity and mortality in Occidental countries, in the last 30 years or more (2).
Asthma treatment can be divided in two different categories: medications for relief and for control of the disease. Therapeutic recommendation is based on differential actions according to severity of the basic disease and crisis (3). Use of inhalant medication is essential for the treatment.
Inhalant therapy is not simple and is highly dependent on the devices. To be effective, the inhalation device must produce spray with the largest amount of particles at the breathing range, to penetrate and to lodge in the lower airways. Moreover, the ideal device must result in a small amount to lodge in the oropharynx, not producing systemic effects; it must be simple, portable, durable and cost-effective. The efficacy and side effects of inhalant medication depend on the device, on the medication it contains and on the adequate use (coordination, adherence, respiratory pattern), so the response can be highly variable. Dose meter inhalers are the most commonly used; however, even with the best inhalation technique, only 10 to 15% of the spray reach the lungs (4). The studies have shown that 30 to 89% of the patients use the inhalers inadequately (5-11). Some of them relate this fact to the low intellectual level of the patients and to the lack of adequate orientation to manage the technique(6,7, 12-15). Nonetheless, the technical mistakes are not limited to the patients; some data indicate that doctors cannot identify either the factors responsible for the satisfactory effect of sprays (6,16,17).
To solve this problem, it would be necessary that the patients master the technique better as well as a clearer theoretical instruction about asthma, without the prejudice and myth surrounding it. But, in order to accomplish this, doctors and health professionals must also become aware of the need to be qualified and willing to teach adequately, for no one teaches what one does not know.
Based on the literature available, we can hypothesize that in Brazil and in other countries, a significant amount of patients and doctors do not know nor use adequately the technique for use of inhalant medication. Therefore, the objective of the present study is to evaluate the performance of asthma patients, medical students and doctors to master the inhalation technique.
METHODS
This study was approved by the Ethics Research Committee of the Medical School of Botucatu. All participants were informed about the study and signed a consent form of participation. Forty patients were interviewed, 16 (40%) males older than 18 years, with average age of 45.3 (S.D. 14.9) years, attended at the Ambulatory of Pneumology of the HC of the Medical School of Botucatu UNESP, who had been using inhalant medication for at least six months. Health professionals were also interviewed, including a group of 36 resident doctors of the Internal Medicine/Pediatrics and 20 senior students of Medicine. The devices evaluated included: metered dose inhalers (MDI), MDI attached to a spacer device and dry powder inhalers (DPI). The participants did not have access to the content of this study until the time of the interview and did not receive previous instructions about the correct technique of using them.
To test the technique of use, spray devices containing placebo were used. The health care professionals demonstrated the inhalation techniques with each type of inhaler mentioned, whereas the patients were evaluated only on the type of inhaler that was part of their treatment. The interviews were made by a single examiner, qualified to observe and score the technique according to the number of steps correctly taken, using the protocol specifically developed for this purpose (summarized on Table 1).
The statistical analysis of the association between the devices and the adequacy of the technique of use was done by the Goodman Contrast Test among and within multinomial populations (18,19). The comparison of percentage of the steps correctly taken in the three populations and three types of devices was performed by the Spearman Coefficient Correlation, with the association (two by two) between the types of inhalers and the percentage of correct answers of residents and students (20).
RESULTS
The inhaling technique was evaluated by means of two different methods, established arbitrarily by the researchers, based on clinical experience. On the first one, the population was divided in groups according to the number of correct steps taken, as shown on Table 2. In the second one, the percentage of correct steps was evaluated, with the objective of getting information on which are the most frequent wrong steps or the ones not accomplished at all.
Of a total of 40 patients, 35 (87.5%) used MDI; five (12.5%), MDI with spacer device; and 16 (40%), DPI; 14 patients (35%) used two types and one (2.5%), the three types. Due to the small number of patients using MDI with spacer device, evaluation of this device was not performed.
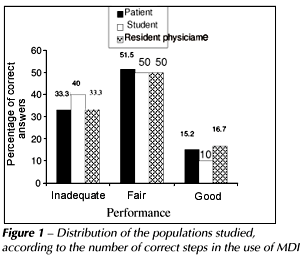
The results obtained when the population was divided according to the number of correct steps are shown in Figures 1, 2 and 3. The Goodman Test showed that among residents and patients the percentage of inadequate use was significantly higher for MDI. The same trend took place among the students; however, the difference did not reach statistical significance. A significantly higher proportion of patients using DPI performed better than those who used MDI. During the study we observed that patients who used MDI and DPI presented and reported easier management of the second device. Moreover, three students (15%) and 13 resident doctors (36.1%) did not know DPI and refused to demonstrate the technique of use, which also happened with two students and three residents regarding MDI with spacer device.
When the percentage of correct steps for MDI, we observed that the lower values in the three populations occurred in steps 2 (vigorous shaking), 6 (expire until residual volume RV) and 8 (inspire until CPT and hold the breath). For DPI, the lowest percentage took place with step 6 (expire until RV) for the three populations and step 5 (press the lateral buttons and release them) for patients and students. MDI with spacer device was evaluated in students and residents; in the two populations the lowest percentages of correct use occurred in step 3 (expire until RV) and 10 (wait 20 to 30 seconds before the second step); the students presented low percentage of correct use (< 28%) in steps 7 (inspire until CPT), 8 (hold the breath for 5 to 10 sec) and 9 (let go the air).
The results of the two most frequently incorrect steps considered important for an efficient treatment with the three devices are presented in Figures 4 and 5. The statistical analysis showed that a significantly higher proportion of individuals in the three groups studied did not performed the expiration before operating the device for all types of inhalers. Regarding the breathing in until CPT and holding the breath, the analysis showed that a higher proportion of individuals using MDI did not do the maneuver correctly in the three populations. In this step, a higher proportion of patients who did the correct maneuver was among DPI users.
The statistical analysis of the average percentage of correct use, for all steps together showed an association among inhalers, i.e., the performance of one kind of device was associated to the performance of the other device, indicating that the knowledge is not limited only to a technical difficulty.
DISCUSSION
The population studied is representative of adult asthma patients followed in the Ambulatory of Pneumology of MSB/UNESP and, in agreement with the literature, there was a predominance of females (21). In the present study, we chose not to perform this investigation by means of a questionnaire because the visual observation may provide more reliable data, evidencing more clearly the difficulties at the time of use. The patient often knows what to do in theory, but in practice, he/she has difficulties that make the satisfactory use of the technique impossible. Other times, the patient develops inadequate habits during the time because they are easier to follow; the doctor may not know about them, and therefore they are not appropriately corrected.
Most of the patients used MDI (87.5%), probably due to its more affordable cost. DPI was used by 40% of the patients. Among those who used both types, there was a clear preference for DPI due to easier inhalation technique, as well as the esthetics. These data are in accordance with the findings described by Interiano and Guntupalli (12).
Patients, doctors and students had a similar performance regarding the inadequate use of the MDI inhalation technique. There was also a high correspondence among the three populations regarding the percentage of correct steps considered individually. According to the available data in the literature, we observed that there is a clear difficulty in the simultaneous coordination of respiratory and motor movements to handle MDI (12,16). Moreover, especially among doctors and students, we noticed a lack of concern for the real importance of respecting the interval between puffs.
Regarding the DPI, the most frequently incorrect step taken by the three populations was the same, step 6 (exhale as much as possible). Data from recent studies show that the handling of DPI favors the respiratory and mechanical coordination when compared with MDI (8-10). In our study, 33 to 40% of the individuals of each group performed inadequately for MDI against 4.4 to 12% for DPI. We also noticed that many health care professionals did not know the mechanism of powder release from the capsule, i.e., they put the mouthpiece between the lips, pushed the lateral buttons and waited for the powder to be released as if they were using a pressurized device such as MDI.
At the time of evaluation we found out that MDI was the best known device both by students and resident doctors and, therefore, the most prescribed. This finding is in accordance with a study carried out in the early 90's in Europe, before the development of new devices (13). Although a large number of devices had recently been introduced in Brazil, their high cost hinders their general use. Thus, especially among low income patients in public hospitals, MDI is still the best known and used device.
Comparing Figures 1 and 2 among patients, we can notice that the number of correct steps for DPI is quite higher, where 50% of the patients had a good performance, whereas for MDI it is limited to 15.2%. When questioned about the reason of such difficulty, some patients referred not being adequately oriented by their physicians in the beginning of the treatment; others, on the other hand, although properly instructed, forgot some steps.
The fact that DPI device is put inside the mouth makes it easier to coordinate the respiratory movements more efficiently than the MDI, whose handling requires notion of distance, motor coordination and enough training to start the inhalation and activate the device almost simultaneously, without forgetting that, although slow, inhalation must be deep. The patients often did not shake the MDI (step 2: 25.7% of accuracy), claiming that they were not appropriately warned about the importance of this movement. Other studies show similar findings (8,10,22).
It is noticed that, despite the difficulties, the technique of DPI use is more specific for the patients, basically focusing on two steps (5 and 6) which may simplify the correction of the mistakes. For MDI, despite some percentage of correct steps being considerably lower, there is a larger dispersion of mistakes.
Both students and resident doctors had a better performance with DPI and MDI with spacer device, although few were familiar with this device and prescribed it to their patients (13). The mistake was concentrated on step 6 of DPI and step 3 of the MDI with spacer device, whereas there was no dispersion on MDI, similarly for the patients.
During this study, we noticed the patients' need for more precise information, which transmitted safety and reliability, since part of the success of this treatment is embedded in the technique. These people are eager to learn, without the opportunity to look for other sources of knowledge, except for our institution. On the other hand, we also found professionals with deficits in their academic background, who do not know the technique or are insecure about the best way to teach their patients, often choosing not to instruct them. It is the doctor's responsibility to teach them with patience, perseverance and confidence. In order to make it a reality in the Medical School of Botucatu, in 2002we proposed to give classes on the subject as well as to enable the students (interns) to adequately instruct their patients by performing the technique during the appointments.
In face of such results and, in agreement with the literature, we can conclude that doctors are potentially responsible for their patients' performance in the use of the inhalation technique (6,8,12,17).
Received for publication on 8/ 7/02
Approved after revision on 12/18/02
* Work carried out at the Department of Internal Medicine of Medical School of Botucatu Unesp, Botucatu, SP.
Supporting agency: Graduate Fellowship from FAPESP, grant # 99/11842-3.
- 1. Busse WW, Lemanske RF. Advances in immunology Asthma. N Engl J Med 2001;344:350-62.
- 2.Sociedades Brasileiras de Alergia e Imunopatologia, Pediatria e Pneumologia e Tisiologia. II Consenso Brasileiro no Manejo da Asma. J Pneumol 1998;24:173-276.
- 3.Sociedades Brasileiras de Alergia e Imunopatologia, Pediatria e Pneumologia e Tisiologia. III Consenso Brasileiro de Asma. J Pneumol 2002; 28(Supl 1).
- 4.Yeats DB, Mortensen J. Depositon and clearance. In: Murray JF, Nadel JA, Mason RJ, Boushey HA, editors. Textbook of respiratory medicine. Philadelphia: WB Saunders, 2000;349-84.
- 5.Gergen PJ. Epidemiology of asthma. In: Busse WW, Holgate ST, editors. Asthma and rhinitis. Oxford: Blackwell Science, 1995;15-25.
- 6.Jones JS, Holstege CP, Riekse R, White L, Bergquist T. Metered-dose inhalers: do emergency health care providers know what to teach? Ann Emerg Med 1995;26:308-11.
- 7.Kelly HW. Correct aerosol medication use and the health professions: who will teach the teachers? Chest 1993;104:1648-9.
- 8.Godoy DV, Barbieri R, Perin FA. Avaliação da técnica de utilização de nebulímetros pressurizados para terapêutica tópica. J Pneumol 2000; 26(Supl 3):90.
- 9.Lenney J, Innes JA, Crompton GK. Inappropriate inhaler use: assessment of use and patient preference of seven inhalation devices. Respir Med 2000;94:496-500.
- 10.Van der Palen J, Klein JJ, Van Herwaarden CLA, Zielhuis GA, Seydel ER. Multiple inhalers confuse asthma patients. Eur Resp J 1999;14: 1034-7.
- 11.Sandrini A, Jacomossi A, Farensin SM, Fernandes ALG, Jardim JR. Aprendizado do uso do inalador dosimetrado após explicação por pneumologista. J Pneumol 2001;27:7-10.
- 12.Interiano B, Guntupalli KK. Metered-dose inhalers: do health care providers know what to teach? Arch Intern Med 1993;153:81-5.
- 13. Crompton GK. The adult patient's difficulties with inhalers. Lung 1990; (Suppl):658-62.
- 14.Wilson SR, Scamagas P, German D, Hughes GW, Lulla S, Coss S. A controlled trial of two forms of self-management education for adults with asthma. Ann Intern Med 1993;94:564-75.
- 15.Williams MV, Baker DW, Honig EG, Lee TM, Nowlan A. Inadequate literacy is a barrier to asthma knowledge and self-care. Chest 1998; 114:1008-14.
- 16.Amiravi I, Goren A, Pawlowski NI. Clinical aspects of allergic disease: what do pediatricians in training know about the correct use of inhalers and spacer devices? J Allergy Clin Immunol 1994;94:669-75.
- 17. Hanania NA, Wittman R, Kesten S, Chapman KR. Medical personnel's knowledge of and ability to use inhaling devices. Chest 1994; 105:111-6.
- 18.Goodman LA. Simultaneous confidence intervals for contrasts among multinomial populations. Ann Math Stat 1964;35:716-25.
- 19.Goodman LA. Simultaneous confidence intervals for multinomial proportions. Technometrics 1965;7:247-54.
- 20. Streiner DL, Norman GR. Biostatistics The bare essentials. St. Louis: Mosby-Year Book, 1994;260.
- 21.Burney P. Asthma. In: Maseano A, Gusvik A, Viegi G. Respiratory epidemiology in Europe. Eur Respir Soc Monogr 2000;5:48-56.
- 22.Cochrane GM, Bala MV, Downs KE, Mauskopf J, Ben-Joseph RH. Inhaled corticosteroids for asthma therapy. Chest 2000;117(Suppl 2):542-50.
Publication Dates
-
Publication in this collection
23 June 2003 -
Date of issue
Apr 2003
History
-
Accepted
07 Aug 2003 -
Received
07 Aug 2002