Abstracts
BACKGROUND: Pharyngoesophageal diverticulum presents itself as an uncommon disorder. Thus, choosing the most effective treatment method may be challenging. Surgical treatment remains as the main option. However, establishing the best surgical technique is still controversial. AIM: To evaluate the results of diverticulecomy with chricopharyngeal miotomy and linear stapler closure of the pharynx in a patient sample with Zenker`s diverticulum regarding local and systemic complications. METHODS: Nineteen patients with pharyngoesophageal diverticulum were admitted. All of them presented the clinical conditions required to indicate the surgical procedure. Patients were evaluated with regard to any post-operative complications. This study was conducted retrospectively with patients' data analysis. RESULTS - Patients showed satisfactory results, with no evidence of fistula at the level of the pharyngeal suture. Two out of 19 lost post-operative follow-up and one of them had pharyngeal stenosis reverted with endoscopic dilation. The entire sample reported being satisfied with the procedure emphasizing improvement of the quality of life mainly due to the return of physiological deglutition. CONCLUSION: The diverticulectomy with myotomy and posterior pharyngeal closure with linear surgical stapler proved to be an effective technique, offering a lower risk of post-operative complications and improving the overall quality of life.
Esophagopharyngeal diverticulum; Zenker's diverticulum; Surgical stapler
RACIONAL: O divertículo faringoesofágico apresenta-se como distúrbio pouco frequente e é provável que este fato seja responsável pela dificuldade encontrada na escolha do método terapêutico mais eficaz. O tratamento cirúrgico ainda é a principal opção terapêutica. No entanto, há controvérsias quanto à técnica cirúrgica que garante melhores resultados. OBJETIVO - Avaliar a eficácia da diverticulectomia com miotomia do músculo cricofaríngeo pela sutura mecânica linear no tratamento cirúrgico do divertículo faringoesofágico em uma série de pacientes no tocante às suas complicações locais e sistêmicas. MÉTODO: Foram atendidos 19 pacientes com divertículo de Zenker. Todos apresentavam as condições clínicas necessárias e preenchiam os critérios de elegibilidade para realização do procedimento cirúrgico. Após a diverticulectomia com sutura mecânica todos foram submetidos a avaliação pós-operatória no sentido de identificar a manifestação de qualquer tipo de complicação. Os pacientes foram estudados retrospectivamente através da análise de prontuários e descrição da internação hospitalar realizada no momento da operação e da evolução ambulatorial. RESULTADOS: A totalidade apresentou resultados satisfatórios, sem evidência de fístula ao nível da sutura da faringe no período pós-operatório precoce. Somente dois indivíduos perderam seguimento na avaliação tardia e um desenvolveu estenose faríngea revertida com dilatação endoscópica. Todos referiram estar satisfeitos com o procedimento empregado e relataram melhora na qualidade de vida ao final do seguimento, proporcionada pelo retorno da deglutição. CONCLUSÃO: A diverticulectomia com a miotomia do músculo cricofaríngeo e posterior fechamento da faringe com sutura mecânica linear mostrou-se técnica eficaz, com poucas complicações pós-operatórias e melhora significativa na qualidade de vida.
Divertículo faringoesofágico; Divertículo de Zenker; Suturas mecânicas
ORIGINAL ARTICLE
Pharyngoesophageal diverticulum surgical therapy using linear stapling device
José Luis Braga de Aquino; Marcelo Manzano Said; José Francisco Salles Chagas; Vânia Aparecida Leandro-Merhi; Eusébio José Gallo-Junior; Gustavo Nardini Cecchino; Mayra Todeschini Assunção
Department of Thoracic Surgery and Department of Head and Neck Surgery of the Celso Pierro Maternity and Hospital, Faculty of Medicine - Pontifícia Universidade Católica de Campinas, São Paulo, Brazil
Correspondence Correspondence: José Luis Braga de Aquino, e-mail: jlaquino@sigmanet.com.br
ABSTRACT
BACKGROUND: Pharyngoesophageal diverticulum presents itself as an uncommon disorder. Thus, choosing the most effective treatment method may be challenging. Surgical treatment remains as the main option. However, establishing the best surgical technique is still controversial.
AIM: To evaluate the results of diverticulecomy with chricopharyngeal miotomy and linear stapler closure of the pharynx in a patient sample with Zenker`s diverticulum regarding local and systemic complications.
METHODS: Nineteen patients with pharyngoesophageal diverticulum were admitted. All of them presented the clinical conditions required to indicate the surgical procedure. Patients were evaluated with regard to any post-operative complications. This study was conducted retrospectively with patients' data analysis.
RESULTS: Patients showed satisfactory results, with no evidence of fistula at the level of the pharyngeal suture. Two out of 19 lost post-operative follow-up and one of them had pharyngeal stenosis reverted with endoscopic dilation. The entire sample reported being satisfied with the procedure emphasizing improvement of the quality of life mainly due to the return of physiological deglutition.
CONCLUSION: The diverticulectomy with myotomy and posterior pharyngeal closure with linear surgical stapler proved to be an effective technique, offering a lower risk of post-operative complications and improving the overall quality of life.
Headings: Esophagopharyngeal diverticulum. Zenker's diverticulum. Surgical stapler.
INTRODUCTION
The pharyngoesophageal diverticulum was first described by Abraham Ludlow in 176415, but only in 1877 it was thoroughly studied by the German pathologist Albert Zenker24, who correlated the clinical and anatomopathological aspects of this disease and known with his name. Nevertheless, the first successfully diverticulectomy was only performed by Whealer in 18861.
The Zenker`s diverticulum is a saccular deformity located in the inferoposterior wall of the pharynx mucosa, just above the upper esophageal sphincter, over a region in between the inferior pharyngeal constrictor muscle and the cricopharynx muscle, known as Killian`s triangle, which is the weakest area. When there is excessive pressure within the distal pharynx, its wall herniates through the triangle forming the diverticulum1,24.
It has low frequency responding for 1-3% of all the dysphagia complaints and up to 4% of the patients with esophageal diseases1,18. There is insufficient data regarding the actual number of cases in South America, including Brazil1,18. It prevails among the sixth and eighth decades of life with the highest incidence around 70 years old due to the aging process of loss of muscular tonus and less resistance of the posterior wall, being therefore rare before the forties,1,18. It affects more males than females with a proportion of 3:1 and occurs more often in the Northern countries of Europe, being uncommon in the Middle East region1,2,18.
The main symptoms are dysphagia and regurgitation, but secondary symptoms such as weight loss and halitosis may occur with bad effect on the quality of life18,20,22.
The diagnosis depends on the ability of history taking and is complemented by contrasted radiographic studies of the pharynx and esophagus as well as upper digestive endoscopy. Some cases require esophageal manometry1,16.
Even thought some authors recommend endoscopic techniques, different surgical approaches are described as treatment, like diverticulectomy or diverticulopexy with cricopharyngeal myotomy 1,14,16,19. In spite of being a standardized surgery, the diverticulectomy is not exempt of complications. The most important is the cervical fistula with dehiscence of the pharynx' suture, which has impact on the patients` quality of life since it may compromise their nutritional state. Fortunately it is reverted with conservative treatment13,18.
Since the invention of the linear stapling device, this method has become widely used once it was demonstrated to be secure and precise over different segments of the gastrointestinal tract4,5. This kind of technique minimizes the development of complications in the anastomotic line because of the double-stapling inverted feature, which lessens ischemia and tissue necrosis5.
Due to the modest highlight attributed to the linear stapling device for the pharynx' suture in diverticulectomy, the authors chose to use this method in a series of patients who underwent surgical diverticulectomy with cricopharyngeal myotomy. The main objective was to evaluate the frequency of local and systemic complications attributed to this surgical modality.
METHODS
During the period of June 1999 to December 2010 the Department of Thoracic Surgery of the Celso Pierro Maternity and Hospital PUC-Campinas admitted 19 patients with pharyngoesophageal diverticulum eligible for diverticulectomy with cricopharyngeal myotomy and suture with linear stapling device. All the patients were instructed regarding the surgical procedure and the informed consents were obtained.
This is a retrospective case series with a predominance of men (16 cases 84,2%) over three women (15,8%). Age varied from 62 to 77 year-old patients (median 69.5). Fifteen patients (79%) were smokers of nearly 20 cigarettes/day varying the period of smoking from 35 to 54 years. Thirteen patients (68.4%) referred to be alcohol consumers of one shot of distilled spirits through a period varying from 25 to 47 years.
Preoperative evaluation
The pharyngoesophageal diverticulum diagnosis was performed through clinical, radiologic and endoscopic examination. All the patients had mild intermittent dysphagia to solids during a period from two to five years. Eight patients (42.1%) had regurgitation associated with cough and three of them (15.7%) reported frequent belching as well as loss of 5% of their body weight.
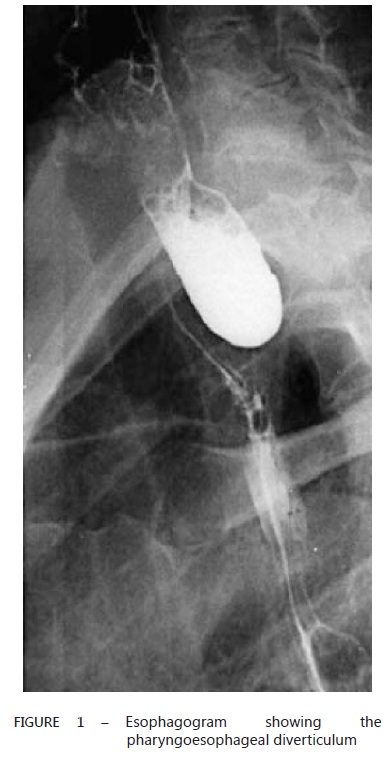
Contrasted radiographic study settled the presence of pharyngoesophageal diverticulum in all of the patients (Figure 1).
The upper digestive endoscopy confirmed pharyngoesophageal diverticulum of big dimensions varying from 5-9 cm of diameter. There were no evidences of associated diseases.
Clinical and nutritional evaluations were satisfactory.
Surgical technique and postoperative evaluation
The surgical procedure performed was the diverticulectomy with cricopharyngeal myotomy according to the following steps: a) left supraclavicular cervical incision and skin detachment; b) left sternocleidomastoid muscle exposure and dissection of its medial portion for pharynx and esophagus exposure; c) isolation of the pharyngoesophageal diverticulum; d) diverticulectomy and pharynx' closure with 45 mm linear stapling device; e) three centimeters cricopharyngeal myotomy; f) nasogastric tube insertion to deliver substances directly into the stomach during the postoperative period; g) insertion of laminar drain and skin suture by planes.
The main focus of the postoperative evaluation was to detect systemic (cardiovascular, respiratory or infectious) and local complications (stenosis and dehiscence of the pharynx' suture). For this reason, daily clinical examination was performed and all the laboratory data were registered as well as the image findings.
The fistulization secondary to dehiscence of the pharynx was diagnosed during the clinical examination by direct visualization of saliva excretion through the incision until the fifth postoperative day. In the absence of this clinical finding, an esophagogram was performed in the fifth postoperative day to evaluate contrast extravasation. A normal result of this image exam was sufficient to introduce liquid oral diet followed by the introduction of the solids diet depending on the patient´s acceptance.
Concerning the stenosis of the pharynx' suture, the diagnosis was based on the clinical presentation, which included dysphagia after the thirtieth postoperative day and decreased diameter of the anastomosis over the contrasted radiography and upper endoscopy.
The overall quality of life perspective was analyzed mainly regarding the return of physiologic deglutition after the surgical procedure.
RESULTS
Short-term evaluation
In the short-term evaluation of the first 30 days of postoperative period two patients (10.5%) presented pulmonary infection, resolved with adequate antibiotic therapy. These patients were the eldest and long-term smokers with chronic obstructive pulmonary disease.
Once no patients developed clinical manifestations of fistulization, an esophagogram was performed on the fifth day to analyze the anastomosis integrity. This exam did not show contrast extravasation at the suture site, reassuring the absence of fistula. Therefore liquid oral diet was introduced at first, followed by solids according the patients' acceptance.
There were no deaths in this case series.
Long-term evaluation
The long-term evaluation was performed on 17 patients since two dropout occurred.
The timing of follow-up varied from two months to nine years (median 4.9). The patients were examined every three months in the first year and every six months from the second year on. Only one patient developed dysphagia to solids after the second month of postoperative observation. The upper digestive endoscopy and the esophagogram revealed stenosis at the level of the suture of the pharynx resolved with three sessions of endoscopic dilation. The entire sample reported be satisfied with the procedure, emphasizing improvement of the quality of life mainly due to the return of physiological deglutition.
DISCUSSION
Due to the low frequency of the pharyngoesophageal diverticulum its clinical management and the definitive treatment are still controversial. This fact also explains this limited case series.
Regarding the treatment, most authors advocate the diverticulectomy with cricopharyngeal myotomy to be the best option1,8,9,23, whereas others suggest the diverticulopexy with cricopharyngeal myotomy, demonstrating similar results12,1318. A less common indication for the Zenker`s diverticulum resection is based on preventing its malignization and taking the opportunity to establish an early diagnosis of a carcinoma in situ3.
Recently the indication of diverticulopexy is restricted to selected patients such as the elderly with high-risk clinical comorbidities and with diverticulum of less than three centimeters 10,12,13.
After a detailed review of the literature and due to the dimensions of the diverticula (greater than five centimeters in all sample), this team opted to indicate the diverticulum resection associated with cricopharyngeal myotomy followed by suture with the linear stapling device. Even though the median age was high (69.5 years old) none of the patients presented with relevant clinical comorbidities.
Lately some authors prefer the endoscopic approach that consists in dividing the septum between the diverticulum and the esophagus 7,21. Van Overbeek21 demonstrated in his 545 case series of endoscopic treatment along thirty years that 91% of the patients' dysphagia symptoms improved with a low rate of morbidity. Ishioka et al.11 also demonstrated their experience with fiberendoscopy to divide the septum in 42 patients, obtaining satisfactory results with only 7.1% of dysphagia recurrence among them.
Concerning the complications of the diverticulectomy, the cervical fistula secondary to the dehiscence of the pharynx' suture has been reported with a frequency of 5-35%1,13,17,18,22. Even though this complication is resolved by conservative treatment in most cases by local care and nutritional support though nasoenteric catheter, it compromises the patient's quality of life for it delays the return to oral deglutition.
For these reasons, there is much advantage in using the mechanic suture with the linear stapling device, mainly because it offers a better coaptation of the borders of the tissues being sutured favoring less dehiscence as demonstrated along the follow-up of these patients. Bonavina et al.6, also emphasized the advantage of using the linear stapling device in their series of 116 cases, in which none of the patients evolved with cervical fistula.
Systemic and predominantly cardiopulmonary complications may be expected in the postoperative period when dealing with older patients potentially with other comorbidities. This fact is present in 10.5% of this series, with a similar rate in other publications 1,13,17,18,23. Smoking is a very relevant aspect in the prognosis as it was a common factor for the only two patients who presented with pulmonary infection after surgery.
In the long-term evaluation, many authors have evidenced that the diverticulectomy with cricopharyngeal myotomy usually vanishes the dysphagia symptoms in most cases 1,10,12,14,17,18,20,23. Andreollo et al.1 in their series of 38 patients with Zenker`s diverticulum and a medium of 14 months of follow-up, also highlight the success rate of 84.6% of individuals submitted to this same surgical technique comparing to 66.6% of success in the group submitted to a diverticulopexia and myotomy.
During the longterm follow-up of this series (medium of 4.8 years) it was reassured that this specific surgical procedure indeed offered benefits once only one patient presented with a minor stenosis at the level of the pharynx resolved precisely after three sessions of dilation. Furthermore, every single patient reestablished adequately their deglutition, obtaining a significant betterment in their quality of life.
CONCLUSION
The diverticulectomy with cricopharyngeal myotomy and mechanical suture with linear stapling device for diverticula of medium and large dimensions determined a successful treatment with very low morbidity, providing improvement in the patients' quality of life after restoring their normal deglutition.
REFERENCES
Financial source: none
Conflicts of interest: none
Received for publication: 13/09/2011
Accepted for publication: 07/02/2012
From Department of Thoracic Surgery and Department of Head and Neck Surgery of the Celso Pierro Maternity and Hospital, Faculty of Medicine - Pontifícia Universidade Católica de Campinas, São Paulo, Brazil.
- 1. Andreollo NA, Lopes LR, Brandalise NA, Camargo MA, Coelho Neto JS. Tratamento cirurgico do divertículo de Zenker: Diverticulopexia versus Diverticulectomia. ABCD Arq Bras Cir Dig 2007;20(4):245-9
- 2. Andreollo NA, Lopes LR, Brandalise NA. Distúrbios motores do esôfago.In : Endoscopia digestiva .1ª Edição. Rio de Janeiro: Sobed, Medsi 1994, p 58-68
- 3. Aquino JLB, Said MM, Bordalo R. Carcinoma in situ em Diverticulo Faringo Esofagico. Rev Col Bras Cir. 2005;32(2):106-107
- 4. Aquino JLB, Said MM, Brandi LA, Oliveira JMP, Maziero D, Leandro Merhi V. Tubo gástrico isoperistaltico de grande curvatura gástrica com sutura mecânica no tratamento cirurgico do câncer de esôfago irressecavel. ABCD Arq Bras Cir Dig 2009;229(3):147-52
- 5. Aquino JLB. Avaliação da anastomose esofagogástrica cervical com sutura mecânica em pacientes com megaesôfago avançado. Rev Col Bras Cir 2005;3:143-146
- 6. Bonavina L, Bona D, Abraham M, Saino G, Abate E. Long term results of endosurgical and open surgical aprroach for Zenker diverticulum. World j Gastroenterl 2007;13(8):2568-9
- 7. Dohlman G, Mattson O. The endoscopic operation for hypopharingeal diverticula. A roentgencinematografic study. Arch Otolaryngol 1960;71:744-52
- 8. Ellis FH, Schlegel JF, Lynch VP, Payne WS. Crycopharyngeal myotomy for Pharyngoesophageal diverticulum. Ann Surg 1969;170:340-9
- 9. Gullane PJ, Willet JM, Heeneman H. Zenker's diverticulum. J Otolaryngol 1983; 12:53-57
- 10. Gutschow CA, Hamoir M, Rombaux P, Otte JB, Goncette L, Collard JM. Management of pharyngoesophageal (Zenker's) diverticulum: which technique? Ann Thorac Surg 2002;74(5): 1677-82
- 11. Ishioka I, Sakai P, Maluf Filho F. Endoscopic incision of Zenker's diverticula. Endoscopy 1995;27:433-37
- 12. Laccourreye O, Menard M, Cauchois R, Huart J, Jouffre V, Brasnu D et al. Esophageal diverticulectomy. Laryngoscope 1994;104:889-92
- 13. Leporrier J, Salame E, Gignoux M, Segol P. Zenker's diverticulum:diverticulopexy versus diverticulectomy. Ann Chir 2001;126(1):42-5
- 14. Lerut T, Van Raemdonck D, Guelinckx P, Dom R, Geboes K. Zenker's diverticulum: is amyotomy of the crycopharyngeus useful? How long should it be? Hepatogastroenterology 1992;39:127-31
- 15. Ludlow A. A case of obstructed deglutition, from a preter natural dilatation of and bag formed in the pharynx. Med Soc Phys 1767;3:35-101
- 16. Migliore M, Payne H, Jeyasingham K. Pathophysiologic Basis for peration on Zenker's Diverticulum. Ann Thorac Surg 1994;57:1616-21
- 17. Okano N, Vargas EC, Moriya T, Carneiro JJ, Elias-Junior AM. Diverticulo do esôfago: analise de 24 pacientes portadores do divertículo de Zenker. Acta Cir Bras 2000;15(2):45-49
- 18. Ribeiro GBS, Mielke F, Volkweis BS, Schirmer CC, Kruel CDP, Morellato G. Tratamento cirurgico do diverticulo de Zenker. ABCD Arq Bras Cir DIG 2008;21(3):110-3
- 19. Sakai P. Endoscopic treatment of Zenker's diverticulum. Gastrointest Endosc 2007;65(7):1054-5
- 20. Simic A, Radovanovic N, Stojakov D, Bjelovic M, Kotarac M, Sabljak P. Surgical experience of the national institution in the treatment of Zenker's diverticula. Acta Chir Iugosl 2009; 56(1):25-33
- 21. Van Overbeek JJM . Meditation on the pathogenesis of hypoharyngeal( Zenker's) diverticulum and a report of endoscopic treatment in 545 patients.Ann Otol Rhinol Laryngol 1994;103:178-185
- 22. Villasennor G, Lorenzo L. Tratamiento quirúrgico de los transtornos motores Del esôfago. Cir Gen 2007;29:253-9
- 23. Wittrick IJ, Gullane PJ, Yeung E. Outcome analysis of Zenker's diverticulectomy and cricopharyngeal myotomy. Head & Neck 1995;17:382-88
- 24. Zenker FA, Von Ziemssen H. Krankheiten des Oesophagus.. In: Von Ziemssen H, ed Hankbuch der Speciellen Pathologie und Therapie, vol 7(suppl). Leipzig: FCW Vogel, 1877: 1-87
Correspondence:
Publication Dates
-
Publication in this collection
01 Feb 2013 -
Date of issue
June 2012
History
-
Received
13 Sept 2011 -
Accepted
07 Feb 2012