Abstracts
INTRODUCTION: The patients suffering heart failure develop an increase in pulmonary pressure because of a retrograde mechanism. The pulmonary hypertension is a prognostic marker. OBJECTIVE: The aim of this study is to correlate pulmonary hypertension measured by echocardiogram versus catheterization in pre-heart transplant patients on waiting list. METHODS: Data from 90 patients of the Clinical Hospital UFMG were collected between 2004 and 2009. All the patients took an echo and catheterization as an integral part of pre-heart transplant. Mean age was 45.5 years old, 68 (75.6%) male. Fourty-two (46.7%) were Chagas' disease patients, 32 (35.6%) presented idiopathic dilated cardiomyopathy, 10 (11.1%) had ischemic cardyomiopathy. RESULTS: The mean eco-PASP was 45 ± 12mmHg). The mean cat-PASP was 47 ±14mmHg. The eco-PASP-Chagas was 41.7 ±12,5 mmHg and non-Chagas 47.6 ±12.8 mmHg P=0.04. The cat-PASP-Chagas was 46 ±12.1 mmHg and non-Chagas 48.7 ±12.8 mmHg P=0.43. Eight patients had cat-PASP>60. The correlation between eco-PASP and cat-PASP in Chagas' patients was r=0.45; P=0.008 and in the non-Chagas was r=0.66; P<0.001. The eco-PASP-Chagas>32,5mmHg has a sensitivity of 79% and specificity of 75% to diagnose PH, with an area under the curve of 0.819. The eco-PASP-non-Chagas>35.5 mmHg has a sensitivity of 82% and a specificity of 70% to diagnose PH, with an area under the curve of 0.776. CONCLUSIONS: There is a good correlation between eco-PASP and cat-PASP (r=0.54) in pre-heart transplant patients. The eco-PASP was lower in the Chagas' group. The echocardiogram is an important method to diagnosis and control pulmonary pressure in pre-heart transplant, specifically in Chagas' patients. The catheterization is still important to evaluate pulmonary reactivity during vasodilation test.
Pulmonary artery, pathology; Heart transplantation; Catheterization
INTRODUÇÃO: O paciente com insuficiência cardíaca desenvolve aumento da pressão pulmonar por mecanismo retrógrado e a hipertensão arterial pulmonar (HP) é um marcador de mau prognóstico. OBJETIVO: Correlacionar pressão pulmonar ao ecogardiograma (eco) e ao cateterismo, em pacientes em lista de espera para transplante cardíaco (TC), especialmente nos chagásicos. MÉTODOS: Avaliamos 90 pacientes no HC-UFMG entre 2004 e 2009. Todos realizaram cateterismo e eco no pré-transplante. A idade média foi de 45,5 anos, sendo 68(75,6%) homens, 42(46,7%) chagásicos, 32(35,6%) portadores de miocardiopatia dilatada e 10(11,1%) isquêmicos. RESULTADOS: A eco-PSAP (pressão sistólica arterial pulmonar) média foi de 45 ± 12mmHg. A cat-PSAP média foi de 47 ± 14mmHg. A eco-PSAP-chagásicos foi 41,7 ±12,5 mmHg e não-chagásicos, 47,6 ±12,8 mmHg P=0,04. A cat-PSAP-chagásicos foi de 46 ±12,1 mmHg e não-chagásicos 48,7±12,8mmHg; P=0,43. Oito pacientes apresentavam cat-PSAP>60. A correlação entre a eco-PSAP e o cat-PSAP nos chagásicos foi r=0,45, P=0,008 e nos não-chagásicos de r=0,66, P<0,001. A eco-PSAP-chagásico >32,5mmHg tem uma sensibilidade de 79% e especificidade de 75% para diagnosticar HP, com área sob a curva ROC de 0,819. A eco-PSAP-não chagásico>35,5 mmHg tem sensibilidade de 82% e especificidade de 70% para HP, com área sob a curva ROC de 0,776. CONCLUSÕES: Há boa correlação entre a eco-PSAP e a cat-PSAP (r=0,54) entre os pacientes em fila de espera. A eco-PSAP foi menor no grupo dos chagásicos. O ecocardiograma é um método útil para diagnosticar e monitorar a pressão pulmonar previamente ao TC, especialmente em pacientes chagásicos. Entretanto, não é possível prescindirmos do cateterismo para avaliar a reatividade pulmonar com o teste com vasodilatador e indicar com segurança o TC mesmo nos pacientes chagásicos.
Hipertensão Pulmonar; Transplante de coração; Cateterismo Cardíaco
ORIGINAL ARTICLE
Pulmonary pressure checked by echocardiography in chagasic patients on the heart transplant waiting list
Cláudio Léo GelapeI; Maria do Carmo Pereira NunesII; Renato BráulioIII; Paulo Henrique NogueiraIV; Silvio Amadeu de AndradeV; Paula Athayde Braga MachadoVI; Piero Menoti OrlandiVI; Maria da Consolação Vieira MoreiraVII
IDoctorate Degree; Cardiovascular Surgeon; Hospital das Clínicas; UFMG; Assistant Professor; Department of Surgery, Federal University of Minas Gerais - UFMG
IIDoctorate Degree; Assistant Professor; Department of Clinical Medicine; UFMG
IIIMaster Degree; Cirurgião do Hospital das Clínicas da UFMG
IVCardiovascular Surgeon; Surgeon; Hospital das Clínicas da UFMG
VPhysician specializing in cardiology; Physician of the Heart Transplant Staff; Hospital das Clínicas; UFMG
VIUndergaduate Medical Student; UFMG
VIIDoctorate Degree (Assistant Professor; Department of Clinical Medicine; UFMG
Corresponding Author
ABSTRACT
INTRODUCTION: Patients with heart failure develop an increase in pulmonary pressure because of a retrograde mechanism. Pulmonary hypertension is a prognostic marker.
OBJECTIVE: The aim of this study is to correlate pulmonary hypertension measured by echocardiogram versus catheterization in pre-heart transplant patients on the waiting list. Methods: Data from 90 patients of the UFMG Clinical Hospital was collected between 2004 and 2009. All the patients took an echo and catheterization as an integral part of pre-heart transplant. The mean age of the patients was 45.5 years, and 68 (75.6%) were male. Forty-two (46.7%) presented with Chagas' disease, 32 (35.6%) presented idiopathic dilated cardiomyopathy, and 10 (11.1%) had ischemic cardiomyopathy.
RESULTS: The mean eco-PASP was 45 (±12mmHg). The mean cat-PASP was 47 (±14mmHg). The eco-PASP-Chagas was 41.7 (±12.5) mmHg and non-Chagas 47.6 (±12.8) mmHg; P = 0.04. The cat-PASP-Chagas was 46 (±12.1) mmHg and non-Chagas 48.7 (±12.8) mmHg; P=0.43. Eight patients had cat-PASP > 60. The correlation between eco-PASP and cat-PASP in Chagas' patients was r=0.45; P=0.008 and in the non-Chagas was r = 0.66; P < 0.001. The eco-PASP-Chagas > 32.5 mmHg have a sensitivity of 79% and specificity of 75% to diagnose PH, with an area under the curve of 0.819. The eco-PASP-non-Chagas > 35.5 mmHg have a sensitivity of 82% and a specificity of 70% to diagnose PH, with an area under the curve of 0.776.
CONCLUSION: There is a good correlation between eco-PASP and cat-PASP (r=0.54) in pre-heart transplant patients. The eco-PASP was lower in the Chagas' group. The echocardiogram is an important method to diagnosis and control pulmonary pressure in pre-heart transplant, specifically in Chagas' patients. The catheterization is still important to evaluate pulmonary reactivity during the vasodilation test.
Descriptors: Pulmonary Hypertension, Pathology. Heart transplantation. Catheterization.
INTRODUCTION
The patient with end-stage heart failure (HF) often develops increased pulmonary pressure by a retrograde mechanism. Left ventricular dysfunction causes increased end-diastolic pressure that is transmitted to the pulmonary vascular bed by increasing venous pressure. As time passed, vascular vasoconstriction and subsequent restructuring occur, with pathological cellular proliferation and intimal hypertrophy associated with fibrosis. Up to one third of patients develop pulmonary arterial hypertension [1].
Pulmonary hypertension (PH) is a marker of poor prognosis in patients with HF. There is an increased mortality in cases of heart transplant (HT) recipients. The donated heart cannot tolerate the right pressure overload, developing right ventricular dysfunction in the postoperative period [1].
The evaluation of candidates for a heart transplant is a rigorous process involving laboratory tests, echocardiography (ECHO), and right cardiac catheterization (cat), among others. PH, especially when irreversible, is associated with increased morbidity and mortality after heart transplant. Therefore, it is appropriate to identify and exclude such individuals in the pre-transplant [2].
The heart failure clinical setting is more serious and present a poor prognosis, especially in the context of Chagas' patients [3,4]. Pulmonary hypertension has been often associated with pulmonary and left ventricular dysfunction in approximately 35% of the cases. The right ventricular function, frequently compromised in patients in functional class IV, is extremely dependent on the afterload and not only of its own contractility [5]. Yock & Popp [6] demonstrated the utility of the echocardiography in the assessment of systolic pulmonary artery pressure in patients with PH.
In the present study, we evaluated the correlation between measures of pulmonary pressure recorded by transthoracic echocardiogram and the same measures taken obtained by right heart catheterization performed on patients on waiting lists for heart transplantation. Nesse estudo, avaliamos a correlação entre as medidas da pressão pulmonar aferidas pelo ecocardiograma transtorácico e as mesmas medidas realizadas pelo cateterismo cardíaco direito realizado nos pacientes em lista de espera para transplante cardíaco. A subgroup analysis of possible recipients with Chagas' disease was particularly accomplished.
Objectives
The aim of this study was to determine the correlation between measurements of pulmonary artery pressure by transthoracic echocardiography performed in relation to the hemodynamic study in patients who were candidates to heart transplant and to verify the diagnostic accuracy of the estimate pulmonary artery pressure by echocardiography performed in patients with Chagas' disease compared to other etiologies of HF.
METHODS
From 2004 to 2009, 90 eligible consecutive patients on the waiting list for a heart transplant were selected at the Heart Failure Unit from the UFMG Clinics Hospital (Hospital das Clínicas). All the patients underwent right heart catheterization and echocardiography as a pre-transplant assessment protocol for analysis of hemodynamic parameters. These exams were performed with clinically stable patients in use of oral medications to treat heart failure. The clinical characteristics of the study population are shown in Table 1.
Right Heart Catheterization
The hemodynamic study was carried out according to the American Heart Association Guidelines [7]. The Swan-Ganz catheter was introduced via a major peripheral vein, usually left subclavian or left jugular vein and floated under pressure waveform guidance with fluoroscopy, sequentially through the superior vena cava, right atrium, and tricuspid valve to reach the pulmonary artery. In this position, the systolic, diastolic, and mean pressures were measured, as well as the pulmonary capillary pressure, the cardiac output and cardiac index, and the systemic and pulmonary resistances. Pulmonary hypertension was defined as cat-PASP > 30 mmHg or PVR > 3.5 UW. The reversibility of the pulmonary hypertension was confirmed with the use of nitroglycerin, at doses between 2 to 6 mg/h, which was administered intravenously. Pulmonary hypertension is considered fixed when the PVR does not fall, at least, less than 20% of the baseline after the test with the vasodilator [8].
Transthoracic Echocardiogram (Transthoracic Echodopplercardiogram)
The images were obtained through an HP Sonos 5500 (Hewlett-Packard, Andover, MA, USA), with a 2.5 to 3.5 MHz transducer at the Hospital das Clínicas from the UFMG. As imagens foram obtidas por intermédio do aparelho Sonos 5500 (Hewlett-Packard, Andover, MA, USA), com transdutor de 2,5 a 3,5 MHz, no Hospital das Clínicas da UFMG. As previously established, the echocardiograms were performed using the following techniques: one-dimensional and two-dimensional echocardiographies, pulsed and continuous Doppler guided by color flow mapping [9,10].
At the two-dimensional study, the end-systolic and end-diastolic volumes of the left ventricle and the ejection fraction were calculated by the two- and four-chambers apical section using the modified Simpson's method, as recommended by the American Society of Echocardiography. This method consists in dividing the left ventricle in multiple cylinders within known dimensions. The total volume of the ventricle is obtained by summing the volumes of the segments, without interference of the ventricular contour changes, such as aneurysms, or in face of segmental alterations of contractility [11].
The right ventricle was evaluated mostly by the two-dimensional echocardiography and its size expressed in relation to the left ventricle. The presence of dilatation and hypocontractility were evaluated through visual analysis by the two-dimensional echocardiography [12].
The presence of tricuspid regurgitation was determined by the Doppler color flow mapping. The measurement of the maximum velocity of tricuspid regurgitation was used to obtain the gradient between the right atrium and the right ventricle through the modified Bernoulli equation (pressure gradient = 4 x V2). The gradient thus obtained estimated PASP using the formula: (PASP = 4 V2 + right atrial pressure). For this calculation, the pressure in the right atrium was considered in all the patients as being 10 mmHg [13].
Statistical Analysis
Continuous variables are presented as mean ± SD and categorical variables are presented as frequencies and proportions.
Comparison between patients with Chagasic cardiomyopathy with the other patients was assessed using the Fisher's exact test. The categorical variables were compared using the chi-square test. Continuous variables were tested with the Student's t test or the Wilcoxon test. To establish the correlation between pulmonary arterial pressure measured by catheterization and echocardiography was used Pearson correlation coefficient or Spearman, as appropriate.
The diagnostic accuracy of echocardiography in identifying PH was measured by the length of the area under the ROC curve (receiver-operating characteristic), by calculating the sensitivity and specificity. Statistical analysis was performed using SPSS for Windows version 17 (SPSS Inc., Chicago, Illinois). We considered P < 0.05 statistically significant.
RESULTS
The mean age of the patients was 45.5 ± 12.07 yrs old (interquartile range from 17 to 68), 75.6% (68) were male. According to the etiology that led to heart failure, it was observed that 42 (46.7%) patients had Chagas disease, 32 (35.6%) had idiopathic dilated cardiomyopathy, 10 (11.1%) had ischemic cardiomyopathy and 6 patients presented other diagnoses. Five of these patients had already had one episode of pulmonary venous thromboembolism. All the patients were in New York Heart Association functional class III or IV, despite the optimized treatment for HF, according to the guidelines of the Brazilian Society of Cardiology [14].
Twenty-nine (32%) patients had some type of cardiac pacing device. Eighteen patients underwent an insertion of a conventional pacemaker and 11 patients who underwent insertion of an implantable cardiac (cardioverter) defibrillator (ICD). A total of 29 patients had electrodes in the right chambers. Of these 29 patients with an intracardiac device, 11 (38%) had moderate or severe tricuspid insufficiency compared with 31 patients without the device (51%), P = 0.082. Eco-PASP was 43.8 ± 11.1 mmHg in patients with the device and 48.1 ± 14.8 mmHg in the patients without the device (P = 0.201).
The mean ejection fraction was 23.12 (± 7.6%) with a left ventricular diameter in diastole of 71 (± 10 mm) and a left ventricular diameter in systole of 63 (± 10 mm). The mean systolic pulmonary artery pressure by the echocardiography (echo-PASP) was 45 ± 12 mmHg. The average cat-PASP was 47 ± 14 mmHg.
The average eco-PASP in chagasic patients was 41.7 ± 12.5 mmHg and in group II was 47.6 ± 12.8 mmHg, P = 0.04. The average cat-PASP in chagasic patients was 46 ± 12.1 mmHg and without Chagas' disease was 48.7 ± 12.8 mmHg, P = 0.43. Eight patients had cat-PASP > 60 (severe PH). Eco-PASP could be measured in 79 patients (87.7%).
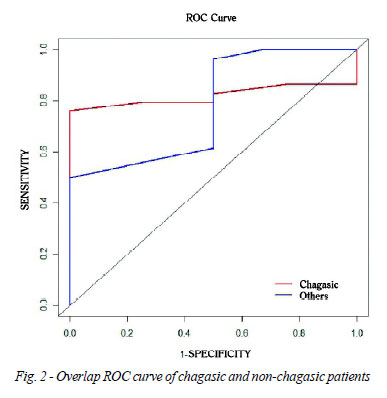
The correlation between the eco- and cat-PASP in the chagasic group was r = 0.45, P = 0.008 (Figure 1) and of the non-chagasic r = 0.66, P < 0.001. Sixty-three patients (70%) had HP defined as PASP > 30 mmHg at the catheterization. To set the value of eco-PASP that identifies patients with HP, we used the ROC curve. A value of 32.5 mmHg PASP estimated by echo had a sensitivity of 79% with a specificity of 75% to diagnose HP, with an area under the ROC curve of 0.819 (Figure 2), which was obtained by stratifying patients according to etiology of HF in patients with Chagas disease. In the other patients, a value of 35.5 mmHg PASP estimated by echo had a sensitivity of 82% with a specificity of 70% to diagnose HP, with an area under the ROC curve of 0.776.
DISCUSSION
Increased pulmonary pressure is one of the most important predictors of death after a heart transplant. This determines the importance of analyzing the pulmonary arterial pressure and its reactivity in the pre-lung transplantation period. Invasive studies of pulmonary pressure are constituent of several research protocols at different institutions. There are several methods available that use Doppler in order to measure pulmonary artery pressure. Although the hemodynamic study plays a major confirmatory role in the diagnosis of PH, the disadvantages of catheterization include high cost, its invasive nature and not being free of risks [5,15].
Several studies have been designed to establish a correlation between echocardiographic and invasive pulmonary parameters. It would be highly desirable to perform a noninvasive exam to diagnose and to follow up of patients in the pre-HT, especially in patients with Chagas disease, since this disease has a high percentage of HT performed in Brazil, and it is increasing in numbers around the world [16,17]. In our study, a value of echo-PASP of 32.5 mmHg had a sensitivity of 79% with a specificity of 75% to diagnose PH, with an area under the ROC curve of 0.819. Therefore, transthoracic echocardiography seems to be a useful method to diagnose and specifically to monitor pulmonary pressure prior to HT, particularly in patients with Chagas disease.
There was good correlation between the echo- and cat-PASP (r = 0.54) when considering all patients in the waiting list (chagasic and non-chagasic) (Figure 3). Echo-PASP was lower in the chagasic group. This fact could be explained by the most likely occurrence of right ventricular dysfunction in chagasic cardiomyopathy, which could underestimate the pulmonary pressure [18].
Conflicting results can be observed. The findings of this study, however, contrast with those observed in other studies. Given that both tests are typically conducted at different times, hemodynamic changes may considerably occur. According to Attaran [2] and Fisher [19], even when echocardiography and hemodynamic studies were performed in a period of 24 hours and in one hour, respectively, there was a poor correlation between its results.
The Study Group for PH reported a correlation of 0.57 between echocardiography and hemodynamics to check PH, which was similar to our findings [20]. The Group could measure pulmonary pressure by tricuspid regurgitant jet in 86% of the patients. In our study, it was possible to perform the measurement of pulmonary pressure by this method in 87.7% of the cases. We must stress that the right atrial pressure is estimated by clinical assessment of jugular venous pulse, which can bring out a potential source of error, especially in patients with Chagas disease, once they have special characteristics of the right ventricle [21-23]. In spite of many of these patients present some type of cardiac pacing device, this seems not affect the prevalence of tricuspid insufficiency and pulmonary pressure measurement [21].
The study carried out by Attaran [2] evaluated the pulmonary artery systolic pressure measured by transesophageal echocardiography and compared with the measurements obtained by hemodynamic pathway through the catheterization of the right heart. This author found a low correlation between these measures in patients with ischemic and non-ischemic cardiomyopathy. On some occasions, a difference of up to 20 mmHg is reported.
Fisher et al. [19] concluded in their study that transthoracic echocardiography is often ineffective in estimating pulmonary pressure. There was a statistically significant difference (> 10 mmHg) between echocardiographic and hemodynamic measurements in 48% of patients.
This study has some limitations. It is a retrospective study. The echocardiogram and hemodynamic assessment were performed at different times. However, our observations regarding the patients with Chagas disease had not yet been described.
We must stress the importance of the hemodynamic study, and we identified as many other authors had, the limitations related to the echocardiogram in the setting of HF and the measurement of PH, especially in Chagas patients who seem to present right ventricular dysfunction more frequently. It has been reported in the literature several measurements using the Doppler effect to assess the pulmonary artery hemodynamics. According to some authors in the future there will be the replacement of the cardiac catheterization by echocardiographic measurements [24].
Many patients cannot tolerate the hemodynamic examination due to arterial hypotension and arrhythmias. Besides, they may be in oral anticoagulant for atrial fibrillation and/or embolic events, which could increase the morbidity of catheterization. Despite these facts, it is not yet possible to leave this exam aside, because it is vital to assess the pulmonary reactivity by testing it with the vasodilator and take the patient safely to heart transplant.
REFERENCES
- 1. Mogollón MV, Laje Gallé E, Hinojosa Pérez R, Herruzo Avilés A, Sobrino Márquez JM, Romero Rodriguez N, Martínez MA. Prognosis after heart transplant in patients with pulmonary hypertension secondary to cardiopathy. Transplant Proc. 2008;40(9):3031-3.
- 2. Attaran RR, Ramaraj R, Sorrell VL, Movahed MR. Poor correlation of estimated pulmonary artery systolic pressure between echocardiography and right heart catheterization in patients awaiting cardiac transplantation: results from the clinical arena. Transplant Proc. 2009;41(9):3827-30.
- 3. Bestetti RB, Muccillo G. Clinical course of Chaga's heart disease: a comparison with dilated cardiomyopathy. Int J Cardiol. 1997;60(2):187-93.
- 4. Freitas HF, Chizzola PR, Paes AT, Lima AC, Mansur AJ. Risk stratification in a Brazilian hospital-based cohort of 1220 outpatients with heart failure: role of Chaga's heart disease. Int J Cardiol. 2005;102(2):239-47.
- 5. Nunes MCP, Barbosa MM, Brum VA, Rocha MO. Morphofunctional characteristics of the right ventricle in Chagas' Cardiomyopathy. Int J Cardiol. 2004;94(1):79-85.
- 6. Yock PG, Popp RL. Noninvasive estimation of right ventricular systolic pressure by Doppler ultrasound in patients with tricuspid regurgitation. Circulation. 1984;70(4):657-62.
- 7. Tonelli AR, Alnuaimat H, Mubarak K. Pulmonary vasodilator testing and use of calcium channel blockers in pulmonary arterial hypertension. Respir Med. 2010;104(4):481-96.
- 8. Zimpfer D, Zrunek P, Roethy W, Czerny M, Schima H, Huber L, et al. Left ventricular assist devices decrease fixed pulmonary hypertension in cardiac transplant candidates. J Thorac Cardiovasc Surg. 2007;133(3):689-95.
- 9. Tajik AJ, Seward JB, Hagler DJ, Mair DD, Lie JT. Two-dimensional real-time ultrasonic imaging of the heart and great vessels. Technique, image orientation, structure, identification and validation. Mayo Clin Proc. 1978;53(5):271-303.
- 10. Sahn DJ, DeMaria A, Kisslo J, Weyman A. Recommendations regarding quantification in M-mode echocardiography: results of a survey of echocardiographic measurements. Circulation 1978;58(6):1072-83.
- 11. Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, et al; Chamber Quantification Writing Group; American Society of Echocardiography's Guidelines and Standards Committee; European Association of Echocardiography. Recommendations for chamber quantification: a report from the American Society of Echocardiography's Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 2005;18(12):1440-63.
- 12. Tei C, Dujardin KS, Hodge DO, Bailey KR, McGoon MD, Tajik AJ, Seward SB. Doppler echocardiographic index for assessment of global right ventricular function. J Am Soc Echocardiogr. 1996;9(6):838-47.
- 13. Currie PJ, Seward JB, Chan KL, Fyfe DA, Hagler DJ, Mair DD, et al. Continuous wave Doppler determination of right ventricular pressure -a simultaneous Doppler catheterization study in 127 patients. J Am Coll Cardiol. 1985;6 (4):750-6.
- 14. Bocchi EA, Braga FGM, Ferreira SMA, Rohde LEP, Oliveira WA, Almeida DR, et al. III Diretriz Brasileira de Insuficiência Cardíaca Crônica. Arq Bras Cardiol. 2009; 93(1 supl.1):1-71.
- 15. Tei C, Dujardin KS, Hodge DO, Bailey KR, McGoon MD, Tajik AJ, et al. Doppler echocardiographic index for assessment of global right ventricular function. J Am Soc Echocardiogr. 1996;9:838-47.
- 15. Bestetti RB, Theodoropoulos TA. A systematic review of studies on heart transplantation for patients with end-stage Chagas' heart disease. J Card Fail. 2009;15(3):249-55.
- 16. Blanche C, Aleksic I, Takkenberg JJ, Czer LS, Fishbein MC, Trento A. Heart transplantation for Chagas' cardiomyopathy. Ann Thorac Surg. 1995;60(5):1406-8.
- 17. Bacal F, de Freitas AF Jr, Moreira LF, Fiorelli AI, Mangini S, Abuhab A, et al. Validation of a cutoff value on echo Doppler analysis to replace right heart catheterization during pulmonary hypertension evaluation in heart transplant candidates. Transplant Proc. 2010;42(2):535-8.
- 18. Fisher MR, Forfia PR, Chamera E, Housten-Harris T, Champion HC, Girgis RE, et al. Accuracy of Doppler echocardiography in the hemodynamic assessment of pulmonary hypertension. Am J Respir Crit Care Med. 2009;179(7):615-21.
- 19. Hoeper MM, Barberà JA, Channick RN, Hassoun PM, Lang IM, Manes A, et al. Diagnosis, assessment, and treatment of non-pulmonary arterial hypertension pulmonary hypertension. J Am Coll Cardiol. 2009;54(1 Suppl):S85-96.
- 20. Nunes MC, Rocha MO, Ribeiro AL, Colosimo EA, Rezende RA, Carmo GA, et al. Right ventricular dysfunction is an independent predictor of survival in patients with dilated chronic Chagas' cardiomyopathy. Int J Cardiol. 2008;127(3):372-9.
- 21. Lanzarini L, Fontana A, Campana C, Klersy C. Two simple echo-Doppler measurements can accurately identify pulmonary hypertension in the large majority of patients with chronic heart failure. J Heart Lung Transplant. 2005;24(6):745-54.
- 22. Selimovic N, Rundqvist B, Bergh CH, Andersson B, Petersson S, Johansson L, et al. Assessment of pulmonary vascular resistance by Doppler echocardiography in patients with pulmonary arterial hypertension. J Heart Lung Transplant. 2007;26(9):927-34.
Publication Dates
-
Publication in this collection
21 June 2011 -
Date of issue
Mar 2011
History
-
Received
23 Aug 2010 -
Accepted
16 Jan 2011