Abstracts
Criss-cross heart is an extremely rare anomaly, characterized by an abnormal rotation of the ventricular mass along its major axis. It may be associated with any malformation of the heart segments and connections. Due to the complex structural changes and rarity of the anomaly, the rotation of ventricular axis is often misdiagnosed. In this paper, two cases of criss-cross heart are reported, with emphasis on diagnostic and surgical techniques used to corrected the main defects. A literature review on the subject is also presented which, although sparse, emphasized on the morphologic, diagnostic and surgical aspects of the anomaly.
Congenital abnormalities; Cardiac surgical procedures; Crisscross heart
Coração entrecruzado (criss-cross heart) é uma anomalia extremamente rara, caracterizada por rotação anormal da massa ventricular ao longo do seu eixo maior e pode estar associada com qualquer malformação dos segmentos e das conexões entre as câmaras cardíacas. Devido às alterações estruturais complexas e à raridade da anomalia, essa anomalia de rotação é muitas vezes mal diagnosticada. Neste trabalho são relatados dois casos de coração entrecruzado com ênfase no diagnóstico morfológico e nas técnicas cirúrgicas utilizadas. Foi também realizada revisão da literatura sobre o assunto, que, embora escassa, foi enfatizada quanto à morfologia, diagnóstico, abordagem cirúrgica e possíveis complicações.
Anormalidades congênitas; Procedimentos cirúrgicos cardíacos; Coração entrecruzado
REVIEW ARTICLE
Criss-cross heart: report of two cases, anatomic and surgical description and literature review
Coração entrecruzado (Criss-cross heart): relato de dois casos, descrição anatomocirúrgica e revisão de literatura
Ítalo Martins de OliveiraI; Vera Demarchi AielloII; Marcela Maria Aguiar MindêlloIII; Yasmin de Oliveira MartinsIV; Valdester Cavalcante Pinto JrV
IPhD in Cardiology at Faculty of Medicine in the University of São Paulo, Research Coordinator at Hospital de Messejana Dr. Carlos Alberto Studart Gomes, Fortaleza, Ceará
IIPathologist-in-chief, Surgical Pathology Section, Laboratory of Pathology at the Heart Institute of Sao Paulo University School of Medicine
IIIPhysician, graduated at State University of Ceará
IVMedicine Student at Fortaleza University
VMaster's Degree in Public Politics Assessment at Federal University of Ceará, Head of the Pediatric Cardiac Surgery Service at Hospital de Messejana Dr. Carlos Alberto Studart Gomes, Fortaleza, Ceará
Correspondence address Correspondence address: Ítalo Martins de Oliveira Av. Frei Cirilo, 3480 - Messejana Fortaleza, CE, Brazil. Zip code: 60846-190 E-mail: italomartins@cardiol.br
ABSTRACT
Criss-cross heart is an extremely rare anomaly, characterized by an abnormal rotation of the ventricular mass along its major axis. It may be associated with any malformation of the heart segments and connections. Due to the complex structural changes and rarity of the anomaly, the rotation of ventricular axis is often misdiagnosed. In this paper, two cases of criss-cross heart are reported, with emphasis on diagnostic and surgical techniques used to corrected the main defects. A literature review on the subject is also presented which, although sparse, emphasized on the morphologic, diagnostic and surgical aspects of the anomaly.
Descriptors: Congenital abnormalities. Cardiac surgical procedures. Crisscross heart.
RESUMO
Coração entrecruzado (criss-cross heart) é uma anomalia extremamente rara, caracterizada por rotação anormal da massa ventricular ao longo do seu eixo maior e pode estar associada com qualquer malformação dos segmentos e das conexões entre as câmaras cardíacas. Devido às alterações estruturais complexas e à raridade da anomalia, essa anomalia de rotação é muitas vezes mal diagnosticada. Neste trabalho são relatados dois casos de coração entrecruzado com ênfase no diagnóstico morfológico e nas técnicas cirúrgicas utilizadas. Foi também realizada revisão da literatura sobre o assunto, que, embora escassa, foi enfatizada quanto à morfologia, diagnóstico, abordagem cirúrgica e possíveis complicações.
Descritores: Anormalidades congênitas. Procedimentos cirúrgicos cardíacos. Coração entrecruzado.
INTRODUCTION
Congenital heart defects are present in about 8 cases per 1000 newborns at term. This index increases if premature and stillbirths were considered. Criss-cross heart anomaly is extremely rare, accounting for less than 0.1% of all congenital heart defects, not exceeding 8 per 1,000,000 births [1].
The morphological essence of the criss-cross heart is a rotation of the ventricular mass along its major axis [1]. This conformational change may be associated with any malformation described in cardiac segments, resulting in different relationships and connections between the atria, ventricles and great vessels (Figure 1)[2].
Although translated by Health Sciences Descriptors (MeSH) as "criss-cross heart", there is no fully accepted and standardized translation to Portuguese for this word from the English language, which is why we use it in its original form throughout this study[3]. In French, some authors refer to this anomaly as "coeur croisé" or as "coeur avec ventricules entrecroisés" [4].
Due to the complex structural changes and the rarity of the disease, this anomaly of rotation is often misdiagnosed due to lack of awareness of the medical team, bringing potential harm to appropriate surgical approach [5]. Depending on the associated anomalies, surgical treatment includes from palliative correction to definitive anatomic correction.
In this study, we performed a literature review, based on the report of two cases of criss-cross heart where the pulmonary and systemic circulations intersect at the atrioventricular level. Both present situs solitus or usual arrangement of the organs. In one of them the right atrium was morphologically connected to the right ventricle with most of the mass placed on the left, with transposition of the great vessels. In the other case the right atrium was connected to the morphologically left ventricle, with discordant atrioventricular connection as will be described below.
This study was approved by the Research Ethics Committee of the institution, case number 473/07 on 25/09/2007.
CASE REPORT
Case 1
Clinical data
A 12-day-old male newborn presented with progressive dyspnea and acrocyanosis from the first day of life. On examination, he presented severe dyspnea with retraction of sternal notch, subcostal and intercostal indrawing and nasal flaring, diaphoresis, cyanosis ++/4+, afebrile, with a heart rate of 140 beats per minute, respiratory rate of 120 breaths per minute. Cardiac auscultation showed systolic murmur ++/6+ at the left sternal edge and accentuated P2 heart sound. His abdomen presented palpable liver two inches below the right costal margin. Peripheral pulses were present and symmetric and the saturation was 85.5% in oxihood (oxygen hood or helmet). Clinical evaluation started from birth at neonatal Intensive Care Unit (ICU).
Tests
The transthoracic echocardiography showed situs solitus. There were concordant atrioventricular connections and most of the morphologically left ventricle mass stood on the right. There was transposition of great arteries with a left-sided and anterior aorta originating from the morphologically right ventricle. The posterior pulmonary trunk was located at right and posteriorly to the aortic root. There was a significant gradient in the right ventricular outflow tract (RVOT), and at the left ventricular outflow tract (LVOT) we observed the presence of mild posterior deviation of the infundibular portion of the interventricular septum without evidence of LVOT obstruction (subpulmonary). There was no significant atrioventricular valve regurgitation. Presence of muscular ventricular septal defect (VSD) of 3.6 mm with right ventricle (RV) flow to left ventricle (LV) (aortopulmonary), and large atrial septal defect (ASD) of ostium secundum type, measuring about 7mm with flow from left to right (L-R) and arterial channel of 4.5 mm with L-R continuous flow. Biventricular systolic function was qualitatively normal.
Diagnosis
This is a case of criss-cross heart with concordant atrioventricular connections, ventriculo-arterial discordance, large ASD, VSD and patent ductus arteriosus (PDA) with continuous flow predominantly L-R.
Approach
The presence of associated malformations and the patient's clinical outcome characterize the severity of the condition. Jatene's surgical technique was indicated due to the patient's age at the time of diagnosis.
Surgical procedure
The proposed surgery was performed in March 2007. We performed the switch operation, sectioning just above the arterial valves, and thecoronary arteries were reimplanted in the new aorta, associated with correction of septal defects. In the immediate postoperative period, the patient developed systemic inflammatory response syndrome, reversed by standard therapy. During postoperative period he also presented the following complications: respiratory infection associated with prolonged mechanical ventilation and atelectasis of the left upper lobe.
He was discharged on the thirty-sixth day postoperatively using furosemide and amiodarone. Discharge echocardiogram showed the criss-cross heart and post-Jatene's correction condition. There was no evidence of dysfunction of the neopulmonary or the neoaorta. It was also observed a foramen ovale with left-right shunt, small perimembranous VSD and preserved contractile function in both ventricles.
After six months of correction, another evaluation showed that the patient presented pulmonary branches supravalvular stenosis, confirmed by cardiac catheterization. At the age of one year and ten months, the patient underwent atrioventriculosseptoplastia and expansion of the right ventricular outflow tract using valved tube. Clinical follow-up was performed every six months and the patient remained asymptomatic, without drugs. New hemodynamic study performed at five years of age, indicated supravalvular stenosis in neopulmonary artery with RV- pulmonary artery (PA) gradient of 38 mmHg.
Case 2
Clinical data
A seven year-and-11-month-old female child, 19kg, with a history of progressive exertional dyspnea and cyanosis of the extremities since the age of three. On physical examination, the patient was afebrile and mildly cyanotic, with systolic murmur ++/6+ in the lower left sternal border and presence of digital clubbing.
Tests
A transthoracic echocardiogram showed discordant atrioventricular connections, double outlet right ventricle (DORV), large VSD, criss-cross heart, and pulmonary valve stenosis (PVS) with a peak gradient of 96 mmHg.
Hemodynamic study was performed which showed double outlet right ventricle with mild infundibular stenosis, discordant atrioventricular connections, perimembranous VSD, and well developed pulmonary branches and right ventricle decreased in size. Oximetry showed blood oxygen saturation in LV of 87%, aorta (Ao) 91% and right ventricle of 100%, 10mmHg RA pressure, LV 107x15mmHg and AO 107x65x81mmHg.
Diagnosis
Criss-cross heart with discordant atrioventricular connections, DORV, large VSD and VPS. The presence of associated malformations characterized the severity of the cardiac defect.
A Fontan procedure was indicated, obeying the following criteria: age above 2 years, absence of pulmonary stenosis, mean pulmonary artery pressure less than 15 mmHg, pulmonary vascular resistance below 4 Wood units, preserved left atrioventricular valve and ventricular function. The biventricular repair was contraindicated due to the small size of the right ventricle.
Surgical procedure
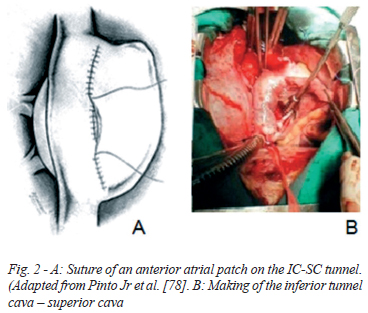
The surgical procedure was performed starting the right atriotomy approximately 1 cm above the insertion of the superior vena cava extending to the inferior cava. Thus, it was possible to make the tunnel, suturing the patch to the interatrial septum leaving the coronary sinus to the left and performing tunnel fenestration. After the completion of the tunnel, suture of the anterior patch over this was performed (Figure 2). Postoperatively, the patient presented as complications: heart failure (HF) and right pleural effusion, resolved using increased diuretic use. Later, she remained unchanged, with no other complications. He was discharged by making use of digoxin, furosemide, captopril and spironolactone.
A transthoracic echocardiogram 3 months after surgery showed left ventricle with good contractility and venous connections (cavopulmonary) with fair functioning, ejection fraction (EF) of 71%, LV diastolic diameter of 21mm and 13mm systolic.
Clinical follow-up was performed every six months for 11 years. At the last visit, the patient was asymptomatic, with normal psychomotor development, without changes in physical examination and under no drug therapy. The last echocardiogram showed mild mitral regurgitation, hypertrophy and mild RV dilatation, cavo-pulmonary connections with diameters and normal flows, with an EF of 69%.
DISCUSSION
Description and anatomy
The criss-cross heart is an extremely rare malformation but well described morphologically. In descriptive report of a collection of 81 hearts with congenital malformations collected over two decades and published in 1999, only one specimen with criss-cross was found, representing only 1.2% of cases [6].
This congenital defect was first described by Lev & Rowlatt [7] in 1961, but it was only in 1974 that Anderson et al. [4] first used the term criss-cross heart. From this publication, about 300 cases of the anomaly have been reported in articles cited in Pubmed to date (2012) [8-43].
The diagnosis of criss-cross heart is based on the intersection of the axes of the ventricular entries. In a normal heart these axes are virtually parallel. This condition is characterized by a spatial change of the ventricular mass that guides or appears to guide, each ventricle in a contralateral position in relation to the corresponding atrium. While the base of the heart remains unchanged in its spatial position, the ventricles appear to have been twisted along their longitudinal axis. This promotes a change in hemodynamics characterized by crossing flows through the atrioventricular valves, resulting in the false impression that each atrium is being directed to the contralateral ventricle [1]. (Figure 1)
The criss-cross heart may present with concordant or discordant atrioventricular connections (Figure 3). These connections were demonstrated in 1961 by Lev & Rowlatt [7] through the study of the anatomy of two hearts presenting atria in solitus position communicating with morphologically discordant ventricles in normal position.- a morphologically right atrium draining to the morphologically left ventricle situated to the left. Another case of criss-cross heart was described by Van Praagh in 1962 [43], in which the morphologically right atrium connected to the morphologically right ventricle on the left side, in a case example with concordant atrioventricular connections.
There are cases of criss-cross heart described in the literature with discordant atrioventricular connections associated with transposition of the great vessels which results in a corrected physiological circulation, since the presence of "double mismatch" results in the direction of venous blood to the lungs and arterial blood into the systemic circulation. Patients with this type of anomaly, which represents 0.05% of congenital heart diseases [44] may be symptomatic not because of the criss-cross heart, but by the presence of other associated anomalies such as VSD, pulmonary outflow obstruction, tricuspid valve abnormalities [45].
Often the criss-cross heart is associated with other cardiac malformations. A review of the literature revealed no cases of of this anomaly occurring in isolation. Most patients have ventricular septal defects, transposition of the great arteries, double-outlet right ventricle, hypoplastic right ventricle, pulmonary stenosis and tricuspid hypoplasia, the latter present in most patients. Other associated defects, although less frequent, are straddling mitral or tricuspid valve, subaortic stenosis, aortic arch obstruction and mitral stenosis [1,45-47]. Anomalies of the coronary circulation may be present and usually related to the ventricular position, and in these cases, magnetic resonance image (MRI) and angiography are useful tools in the diagnosis and approach [47]. In literature there are some studies linking the Cx43 gene mutation to pathogenesis of the criss-cross heart. Deletion of gene would result in a delay in establishing heart dextroposition, which makes the right ventricle to maintain a craniomedial position, resulting in a 90º rotation of the atrioventricular mass [48].
The Cx43 gene is responsible for the production of a type of the protein connexin. These proteins are known to compose gap junctions, and the decrease in their expression has been associated with various genetic alterations, with increased cell proliferation and carcinogenesis [49]. Reaume et al. [50] in 1995 reported that animals with deletions in both alleles of Cx43 died shortly after birth, with no major phenotypic differences compared to controls, except for cyanotic appearance. Necropsy revealed cardiac defects, thereby revealing vital importance of this protein in cardiac development during embrionary development. Ya et al. [48] in 1998 reported that, on the 9th day of development, animals with deletion of Cx43 showed delayed development of the ascending looping of the heart tube, causing malformation of the tricuspid valve patch and changes in conformation and cardiac death of animals shortly after birth with cyanotic appearance.
Clinical, supplementary and differential diagnosis
Due to the complex structural changes, this anomaly is often not recognized. The diagnosis becomes more difficult due to the similarity of the clinical presentation of the different connections abnormalities [51,52].
The anatomic and physiologic diagnosis of this anomaly can be established by echocardiography, along with other diagnostic methods, such as MRI and cardiac catheterization if necessary [53].
The transthoracic echocardiography can be used to identify the position and morphology of all cardiac chambers, AV valves, in addition to the connections between chambers and vessels. The subcostal window will determine the location of the heart apex and assess mainly the ventricles characteristics. The trabeculae morphological features, will determine the morphologic ventricle characteristics [51]. The great arteries connections are better visualized in the paraesternal window [54,55].
MRI, when showing the heart in the axial, coronal and sagital planes makes such additional examination an important tool for diagnosis of complex congenital heart diseases [56].
MRI, when compared to other imaging tests, has the advantage of providing a wide field of vision and the ability to reconstruct the image in 3 dimensions [57]. The images acquired with the MRI show in detail all the heart components and simultaneously clarifies the changes in the AV connections by being able to diagnose abnormalities of heart rotation [58].
The indications for cardiac catheterization are currently limited, since the images obtained with echocardiography and magnetic resonance imaging better delimit the anatomy, ventricular function and atrioventricular relationships [51]. Cardiac catheterization may be necessary only to obtain pressure and oximetry data and discard additional septal ventricular defects [53]. Some indications for the invasive study were assessment of pulmonary vascular resistance, angiographic analysis of coronary arteries, presence of pulmonary valve atresia or pulmonary anomalous veins [53].
The differential diagnosis of criss-cross heart should include straddling atrioventricular valve, double atrial outlet where an outlet orifice apparently crosses the other valve, and severe forms of Ebstein anomaly on which the tricuspid valve opens to the infundibulum, giving the appearance of crossing the valves [54].
Surgical treatment
The natural history of patients is unfavorable without surgical treatment, 64% of deaths occurring in childhood, with 50% still in the neonatal period [58,59]. The surgical management of patients with criss-cross heart consists of the repair of major and limiting malformation, not being ventricular rotation itself the reason for the correction.
The initial management is determined by the presence or absence of pulmonary stenosis, and its severity. On those where the pulmonary flow is inadequate, early intervention with prostaglandin E1 is indicated for maintaining the patency of the ductus arteriosus. When anatomic correction fails, balance in pulmonary flow can be achieved with the construction of systemic-pulmonary shunt.
The corrective surgery is determined by the potential use of both ventricles. Only some patients are candidates for biventricular repair, due to hypoplasia of the tricuspid valve and right ventricle, atrioventricular valve straddling [60-62]. In these cases the Fontan correction is indicated as a palliative repair option.
The case studies reflect the size of the treatment of structural abnormalities associated with the criss-cross heart. In the first, the association with transposition of the great arteries, VSD, ASD and PDA, was defined as a surgical option the Jatene's operation. The surgery is usually performed in the neonatal period and may be performed in patients with VSD and maintains left ventricular mass characteristics compatible to support the systemic resistance.
Several factors may contribute to the loss of left ventricular mass, and the reduction of pulmonary arteriolar resistance, the most important. Echocardiographic selection is the primary method for defining the surgical treatment. With this assessment, the size of the atrial septal defect, the presence of flow through the ductus arteriosus and the LV outflow tract obstructions can be assessed, in addition to the determination of the ventricles mass [63]. For cases of dTGA and IAC, according to most authors, the primary anatomic correction should be performed until the 15th day of life, and this period may be extended with relative safety until the end of the 1st month [64]. The approach after the neonatal period is controversial and published experiences generally have a small number of patients. Lacourt-Gayet et al. [65] and Lyer et al. [66] advocate for clinical and echocardiographic selection correction in 1 or 2 stages in these cases. Davis et al. [67] and Ducan et al. [68] indicate primary anatomic correction in all patients until the 2nd month of life, based on an aggressive vasodilator therapy and occasional use of ventricular assistance postoperatively. Yacoub et al. [69] in 1980 reported 20 cases who had undergone late staging, with an immediate mortality of three patients, and 14 of them directed to the 2nd stage, when there were four deaths (29%). The main advantage of the ventricular preparation would be related to better LV conditioning, which could provide better long term outcomes. Moreover, the long interval between stages can be a source of problems related to the presence of pulmonary artery banding, such as distortions of the trunk and branches of the pulmonary artery and an increased incidence of late aortic insufficiency and fibroelastosis [63]. The difficulty of proper control after discharge of some patients also contributes to early correction with rapid preparation.
Most children who underwent Jatene's operation have normal physical, psychomotor and cardiovascular development. However, some problems can be found in late development. Among these, pulmonary or RVOT stenoses are the most common and can be directly related to surgical technique and patient's age at the time of correction. The incidence of RVOT obstruction varies from 7%-40% [70], and is the main cause of reoperation after discharge [70,71]. The obstructive process may occur in the infundibular or annular region (proximal obstructions) or supravalvular region (distal obstructions). In the first case described here, the patient developed supra-valvular stenosis in neopulmonary and in pulmonary branches after six months postoperatively, being treated with implantation of a valved tube.
In the second case, due to right ventricular hypoplasia the choice was for the Fontan procedure which, over the past 40 years, goes through technical enhancements to the optimization of hemodynamic status. Studies show lack of atrial contractility, over time, since it tends to dilation, turning the flow turbulent with consequent arrhythmia and thrombosis [72]. The use of prosthetic material as part of the tunnel excludes pulsatile mobility of the conduit. Several authors [73,74] have shown that TCP anastomosis, because it excludes the right atrium and makes the inferior cava flow occurs through a tunnel, avoids turbulence, thus reducing the risk of thrombosis and arrhythmias. The use of bovine pericardium for the atrial level tunneling is worrisome because retractions with minimal obstructions can cause significant hemodynamic effects. Rossi et al. [75] in 1986 and Arbustini et al. [76] in 1983 showed calcification in thistype of graft, with a clear relation with time.
In 1997, Pires et al. [77] demonstrated that bovine pericardial tissue implanted in the atrium calcifies, retracts and promotes thrombus formation. The variation proposed by Van De Wal et al, without the use of prosthetic material, using the retail from the own right atrial wall by confection of the tunnel [72], aimed to improve the outcome in the short term, because it keeps the tunnel contraction, allowing improved systemic venous drainage. On the other hand, in the long-term, as a prosthetic material was not used, a proper growth of this conduit was obtained, without calcification, resulting in lower risk of retraction, embolization and anti-coagulation problems [59].
CONCLUSION
The study of these two cases and the extensive literature review on the subject show that the rotation anomalies of the ventricular mass are associated with changes in general connections between the cameras and large arteries and that the surgical approach depends on the morphology of the main defect. The presence of crossed ventricles in the reported cases had no impact alone on the surgical intervention.
REFERENCES
1. Sanders, S. Crisscross Heart. Orphanet encyclopedia, Feb 2003. Disponível em <http://www.orpha.net/data/patho/Pro/en/CrissCrossHeart-FRenPro8602.pdf> Acesso em 29 de fevereiro de 2012.
2. Cavellucci PMSM, Suaide CE, Ferreira LDC, Tandrafilov MD, Pimentel BDPA, Lerner M, et al. Entrecruzamento das vias de entrada ventriculares (criss-cross heart) e transposição ana-tomicamente corrigida das grandes artérias: relato de caso e revisão de literatura. Rev Bras Ecocardiogr Imagem Cardiovasc. 2012;25(4):292-7.
3. Aiello VD, Caneo LF, Jatene MB, Riso AA, Atik E, Afiune JY, et al. Uma proposta para nomenclatura dos defeitos congênitos do sistema cardiovascular. Rev Bras Cir Cardiovasc. 2002;17(1):1-5.
4. Anderson RH, Shinebourne EA, Gerlis LM. Criss-cross atrioventricular relationships pro-ducing paradoxical atrioventricular concordance or discordance. Their significance to nomen-clatura of congenital heart disease. Circulation. 1974;50(1):176-80.
5. Symons JC, Shinebourne EA, Joseph MC, Lincoln C, Ho Y, Anderson RH. Criss-cross heart with congenitally corrected transposition: report of a case with d-transposed aorta and ventricu-lar preexcitation. Eur J Cardiol. 1977;5(6):493-505.
6. Van Praagh R. Segmental approach to diagnosis. In: Nadas' Pediatric Cardiology. Philadel-phia: Saunders, Fyler. Hanley & Belfus;2006. p.39-49.
7. Lev M, Rowlatt VF. The pathologic anatomy of mixed levocardia. Am J Cardiol. 1961;8:250-5.
8. Fang F, Li ZA, Yang Y, Zheng CH, Lam YY. Deciphering the mysteries of crisscross heart by transthoracic echocardiography. Echocardiography. 2011;28(1):104-8.
9. Yang YL, Wang XF, Cheng TO, Xie MX, Lü Q, He L, et al. Echocardiographic characteris-tics of the criss-cross heart. Int J Cardiol. 2010;140(2):133-7.
10. Rubensfigueroa J, Erdmenger Orellana J, Muñoz Castellanos L, Vázquez Antona C, Buendía Hernández A, Vargas Barrón J. Echocardiographic segmental analysis in patients with an atrioventricular criss-cross. Rev Esp Cardiol. 2009;62(9):1055-9.
11. Hoffman P, Szymański P, Lubiszewska B, Rózański J, Lipczyńska M, Klisiewicz A. Criss-cross hearts in adults: echocardiographic evaluation and natural history. J Am Soc Echocardiogr. 2009;22(2):134-40.
12. Del PasquaA, Sanders SP, Rinelli G. Images in cardiovascular medicine. Three-dimensional echocardiography in crisscross heart: could a specimen be better? Circulation. 2007;116(17):e414-5.
13. Ming Z, Yumin Z. Magnetic resonance evaluation of criss-cross heart. Pediatr Cardiol. 2008;29(2):359-65.
14. Cantinotti M, Bell A, Hegde S, Razavi R. A segmental approach to criss-cross heart by car-diac MRI. Int J Cardiol. 2007;118(3):e103-5.
15. Nielsen JC, Parness IA. Anatomy of a criss-cross heart. Circulation. 2002;106(9):e41.
16. Araoz PA, Reddy GP, Thomson PD, Higgins CB. Images in cardiovascular medicine. Mag-netic resonance angiography of criss-cross heart. Circulation. 2002;105(4):537-8.
17.Alva C, Jiménez S, David F, Ortegón J, Sánchez A, Jiménez D, et al. Atrioventricular dis-cordance. Clinico-surgical experience 1990-2000. Arch Inst Cardiol Mex. 2000;70(6):561-8.
18. Gerlis LM, Ho SY, Anderson RH, Branfoot AC. The anatomy of a collection. Cardiovasc Pathol. 1999;8(2):103-7.
19. Choe YH, Kim YM, Han BK, Park KG, Lee HJ. MR imaging in the morphologic diagnosis of congenital heart disease. Radiographics. 1997;17(2):403-22.
20. Morelli PJ, Kimball TR, Witt SA, Meyer RA. Echocardiographic considerations in demon-strating complex anatomy of crisscross atrioventricular valves and discordant atrioventricular and ventriculoarterial relations. J Am Soc Echocardiogr. 1996;9(5):727-9.
21. Nagatsu M, Harada Y, Takeuchi T, Goto H, Ota Y. Can concordant criss-cross heart be ameliorated by hemodynamic changes? Ann Thorac Surg. 1995;60(3):699-701.
22. Vargas-Barron J, Rijlaarsdam M, Romero-Cardenas A, Keirns C, Diaz-Moncada S. Transesophageal echocardiography in adults with congenital cardiopathies. Am Heart J. 1993;126(2):426-32.
23. Yoo SJ, Seo JW, Lim TH, Park IS, Hong CY, Song MG, et al. < Hearts with twisted atrioven-tricular connections: findings at MR imaging. Radiology. 1993;188(1):109-13.
24. Geva T, Van Praagh S, Sanders SP, Mayer JE Jr, Van Praagh R. Straddling mitral valve with hypoplastic right ventricle, crisscross atrioventricular relations, double outlet right ventricle and dextrocardia: morphologic, diagnostic and surgical considerations. J Am Coll Cardiol. 1991;17(7):1603-12.
25. Sreeram N, Stümper OF, Kaulitz R, Hess J, Roelandt JR, Sutherland GR. Comparative value of transthoracic and transesophageal echocardiography in the assessment of congenital abnor-malities of the atrioventricular junction. J Am Coll Cardiol. 1990;16(5):1205-14.
26. Myers JL, Waldhausen JA, Weber HS, Arenas JD, Cyran SE, Gleason MM. A reconsidera-tion of risk factors for the Fontan operation. Ann Surg. 1990;211(6):738-43.
27.Battistessa S, Soto B. Double outlet right ventricle with discordant atrioventricular connex-ion: an angiographic analysis of 19 cases. Int J Cardiol. 1990;27(2):253-63.
28. Igarashi H, Kuramatsu T, Shiraishi H, Yanagisawa M. Criss-cross heart evaluated by colour Doppler echocardiography and magnetic resonance imaging. Eur J Pediatr. 1990;149(8):523-5.
29. Héry E, Jimenez M, Didier D, van Doesburg NH, Guérin R, Fouron JC,. Echocardiographic and angiographic findings in superior-inferior cardiac ventricles. Am J Cardiol. 1989;63(18):1385-9.
30. Anderson RH, Smith A, Wilkinson JL. Disharmony between atrioventricular connections and segmental combinations: unusual variants of "crisscross" hearts. J Am Coll Cardiol. 1987;10(6):1274-7.
31. Carminati M, Valsecchi O, Borghi A, Balduzzi A, Bande A, Crupi G, et al. Cross-sectional echocardiographic study of criss-cross hearts and superoinferior ventricles. Am J Cardiol. 1987;59(1):114-8.
32. Marino B, Sanders SP, Pasquini L, Giannico S, Parness IA, Colan SD. Two-dimensional echocardiographic anatomy in crisscross heart. Am J Cardiol. 1986;58(3):325-33.
33. Nakada I, Nakamura T, Matsumoto H, Sezaki T. Successful repair of criss-cross heart using modified Fontan operation.Chest. 1983;83(3):569-70.
34. Dunn JM, Donner R, Black I, Balsara RK. Palliative repair of transposition of the great ar-teries with criss-cross heart: ventricular septal defect and hypoplastic right (systemic) ventricle. J Thorac Cardiovasc Surg. 1982;83(5):755-60.
35. van Mill G, Moulaert A, Harinck E, Wenink A, Oppenheimer-Dekker A. Subcostal two-dimensional echocardiographic recognition of a criss-cross heart with discordant ventriculoarterial connection. Pediatr Cardiol. 1982;3(4):319-23.
36. Tadavarthy SM, Formanek A, Castaneda-Zuniga W, Moller JH, Edwards JE, Amplatz K. The three types of criss-cross heart: a simple rotational anomaly. Br J Radiol. 1981;54(645):736-43.
37. Marcelletti C, Mazzera E, Olthof H, Sebel PS, Düren DR, Losekoot TG, et al. Fontan's op-eration: an expanded horizon. J Thorac Cardiovasc Surg. 1980;80(5):764-9.
38. Danielson GK, Tabry IF, Ritter DG, Fulton RE. Surgical repair of criss-cross heart with straddling atrioventricular valve. J Thorac Cardiovasc Surg. 1979;77(6):847-51.
39. Freedom RM, Culham G, Rowe RD. The criss-cross and superoinferior ventricular heart: an angiocardiographic study. Am J Cardiol. 1978;42(4):620-8.
40. Anderson KR, Lie JT, Sieg K, Hagler DJ, Ritter DG, Davis GD. A criss-cross heart. De-tailed anatomic description and discussion of morphogenesis. Mayo Clin Proc. 1977;52(9):569-75.
41. Anderson RH, Shinebourne EA, Gerlis LM. Criss-cross atrioventricular relationships pro-ducing paradoxical atrioventricular concordance or discordance. Their significance to nomen-clature of congenital heart disease. Circulation. 1974;50(1):176-80.
42. Atik E. Caso 3/2007: lactente de três meses com criss-cross heart, discordância atrioventri-cular e dupla via de saída de ventrículo direito, sem estenose pulmonar. Arq Bras Cardiol. 2007;88(6):693-5.
43. VanPraagh R, VanPraagh S, Vlad P, Keith JD. Anatomic types of congenital dextrocardia: diagnostic and embryologic implications. Am J Cardiol. 1964;13:510-31.
44. Wallis GA, Debich-Spicer D, Anderson RH. Congenitally corrected transposition. Orphanet J Rare Dis. 2011;6:22.
45. Croti UA, Mattos SS, Pinto Jr VC, Aiello VD. Cirurgia cardiovascular pediátrica. 1ª ed. São Paulo:Roca;2008.
46. Gatzoulis MA, Webb G, Broberg C, Uemura H. Cases in adult congenital heart disease. Complex congenital heart conditions. 2010;1:278-80.
47. Angelini P, Lopez A, Lufschanowski R, Nemeth MA, Flamm SD. Coronary arteries in crisscross heart. Tex Heart Inst J. 2003;30(3):208-13.
48. Ya J, Erdtsieck-Ernste EBHW, Boer PAJ, Van Kempen MJA, Jongsma H, Gros D, et al. Heart defects in connexin 43-deficient mice. Circulation Research 1998, 82:360-6.
49. Chaible LM. Efeitos da deleção do gene Cx43 sobre o desenvolvimento fetal de camundon-gos de diferentes backgrounds genéticos: ênfase na osteogênese [Dissertação de mestrado]. São Paulo:Universidade de São Paulo; 2009.
50. Reaume AG, Sousa PA, Kulkarni S, Langille BL, Zhu D, Davies TC, et al. Cardiac mal-formation in neonatal mice lacking connexin43. Science. 1995;267(5205):1831-4.
51. Wallis GA, Debich-Spicer D, Anderson RH. Congenitally corrected transposition. Orphanet J Rare Dis. 2011;6:22.
52. Valenzuela JMB, Lucas E, Bomfin Jr EJ. Criss-cross heart: diagnóstico fetal. Rev Bras Ecocardiogr Imagem Cardiovasc. 2009;22(2):51-6.
53. Robinson PJ, Kumpeng V, Macartney FJ. Cross sectional echocardiographic and angiocar-diographic correlation in criss cross hearts. Br Heart J. 1985;54(1):61-7.
54. Carminati M, Valsecchi O, Borghi A, Balduzzi A, Bande A, Crupi G, et al. Cross-sectional echocardiography study of criss-cross heart and superoinferior ventricles. Am J Cardiol. 1987:59(1):114-8.
55. Attie F, Zabal C, Buendia A. Cardiologia pediátrica diagnóstico y tratamiento. México. 1993;1:353-62.
55. Link KM, Weesner KM, Formanek AG. MR imaging of the criss-cross heart. AJR Am J Roetgenol. 1989;152(4):809-12.
57. Araoz PA, Reddy GP, Thomson PD, Higgins CB. Images in cardiovascular medicine. Magnetic resonance angiography of criss-cross heart. Circulation. 2002;105(4):537-8.
58. Fantini FA, Gontijo B, Martins C, et al. Operação de Fontan: uma técnica em evolução. Rev Bras Cir Cardiovasc 2009;24(4):463-9.
59. Carotti A, Iorio FS, Amodeo A, Giamberti A, Marianeschi S, Nava S, et al. Total cavopul-monary direct anastomosis: a logical approach in selected patients. Ann Thorac Surg. 1993;56(4):963-4.
60. Sato K, Ohara S, Tsukaguchi Yyasui K, Nakata T, Tamai M, et al. A criss-cross heart with concordant atrioventriculo-arterial connection. Report of case. Circulation. 1978;57(2):396-400.
61. Danielson GK, Tabry IF, Ritter DG, Fulton RE. Surgical repair of criss-cross heart with straddling atrioventricular valve. J Thorac Cardiovasc Surg. 1979;77(6):847-51.
62. Kashiwagi J, Imai Y, Aoki M, Shin'oka T, Hagino I, Nakazawa M. An arterial switch oper-ation for a concordant crisscross heart with the complete transposition of the great arteries. J Thorac Cardiovasc Surg. 2002;124(1):176-8.
63. Gontijo Filho B, Fantini FA, Martins C, Lopes RM, Pereira RST, Rabelo SM, et al. Estra-tégia cirúrgica na transposição das grandes artérias com septo interventricular intacto após pe-ríodo neonatal. Arq Bras Cardiol. 2005;85(1):39-44.
64. Plaché C, Bruniaux J, Lacour-Gayet F, Kachaner J, Binet JP, Sidi D, et al. Switch operation for transposition of the great arteries in neonates. A study of 120 patients. J Thorac Cardiovasc Surg. 1988;96(3):354-63.
65. Lacourt-Gayet F, Piot D, Zoghbi, Serraf A, Gruber P, Macé L, et al. Surgical management and indication of left ventricular retraining in arterial switch for transposition of the great arteries with intact ventricular septum. Eur J Cardiothoracic Surg. 2001;20(4):824-9.
66. Iyer KS, Sharma R, Kumar K, Bhan A, Kothari SS, Saxena A, et al. Serial echocardiog-raphy for decision making in rapid two-stage arterial switch operation. Ann Thorac Surg. 1995;60(3):658-64.
67. Davis AM, Wilkinson JL, Karl TR, Mee RB. Transposition of the great arteries with intact ventricular septum. Arterial switch repair in patients 21 days of age or older. J Thoracic Cardi-ovasc Surg. 1993;106(1):111-5.
68. Ducan BW, Poirier NC, Mee RB, Drummond-Webb JJ, Qureshi A, Mesia CI, et al. Selec-tive timing for the arterial switch operation. Ann Thorac Surg. 2004;77(5):1691-6.
69. Yacoub MH, Radley-Smith R, Maclaurin R. Two-stage operation for anatomical correction of transposition of the great arteries with intact interventricular septum. Lancet. 1977;1(8025):1275-8.
70. Williams WG, Quaegebeur JM, Kirklin JW, Blackstone EH. Outflow obstruction after the arterial switch operation: a multiinstitutional study. Congenital Heart Surgeons Society. J Thorac Cardiovasc Surg. 1997;114(6):975-87.
71. Nogi S, McCrindle BW, Boutin C, Williams WG, Freedom RM, Benson LN. Fate of the neopulmonary valve after the arterial switch operation in neonates. J Thorac Cardiovasc Surg. 1998;115(3):557-62.
72. van de Wal HJ, Tanke RF, Roef MJ. The modified Senning operation for cavopulmonary connection with autologous tissue. J Thorac Cardiovasc Surg. 1994;108(2):377-80.
73. Björk VO, Olin CL, Bjarke BB, Thorén CA. Right atrial-right ventricular anastomosis for correction of tricuspid atresia. J Thorac Cardiovasc Surg. 1979;77(3):452-8.
74. Kreutzer J, Kaene JF, Lock JE, Walsh EP, Jonas RA, Castañeda AR, et al. Conversion of modified Fontan procedure to lateral atrial tunnel cavopulmonary anastomosis. J Thorac Cardiovasc Surg. 1996;111(6):1169-76.
75. Rossi MA, Braile DM, Teixeira MD, Carrilo SV. Calcific degeneration of pericardial val-vular xenografts implanted subcutaneously in rats. Int J Cardiol 1986;12(3):331-9.
76. Arbustini E, Jones M, Ferrans VJ. Formation of cartilage in bioprosthetic cardiac valve im-planted in sheep: a morphologic study. Am J Cardiol. 1983;52(5):632-6.
77. Pires AC, Saporito WF, Leão LEV, Forte V, Cardoso SH, Ramaciotti O. Pericárdio bovino utilizado como remendo no sistema cardiovascular. Rev Bras Cir Cardiovasc. 1997;12(2):176-87.
78. Pinto Jr. VC, Carvalho Jr. W, Barroso HB, Mejia JAC, Mesquita FA, Sardenberg CRC, et al. Anastomose cavo-pulmonar total sem uso de material protético. Rev Bras Cir Cardiovasc. 1998;13(3):234-8.
Article received on May 9th, 2012
Article accepted on December 26th, 2012
Work carried out at: Hospital de Messejana Dr. Carlos Alberto Studart Gomes. Fortleza, CE, Brazil.
- 1. Sanders, S. Crisscross Heart. Orphanet encyclopedia, Feb 2003. Disponível em <http://www.orpha.net/data/patho/Pro/en/CrissCrossHeart-FRenPro8602.pdf> Acesso em 29 de fevereiro de 2012.
- 2. Cavellucci PMSM, Suaide CE, Ferreira LDC, Tandrafilov MD, Pimentel BDPA, Lerner M, et al. Entrecruzamento das vias de entrada ventriculares (criss-cross heart) e transposição ana-tomicamente corrigida das grandes artérias: relato de caso e revisão de literatura. Rev Bras Ecocardiogr Imagem Cardiovasc. 2012;25(4):292-7.
- 3. Aiello VD, Caneo LF, Jatene MB, Riso AA, Atik E, Afiune JY, et al. Uma proposta para nomenclatura dos defeitos congênitos do sistema cardiovascular. Rev Bras Cir Cardiovasc. 2002;17(1):1-5.
- 4. Anderson RH, Shinebourne EA, Gerlis LM. Criss-cross atrioventricular relationships pro-ducing paradoxical atrioventricular concordance or discordance. Their significance to nomen-clatura of congenital heart disease. Circulation. 1974;50(1):176-80.
- 5. Symons JC, Shinebourne EA, Joseph MC, Lincoln C, Ho Y, Anderson RH. Criss-cross heart with congenitally corrected transposition: report of a case with d-transposed aorta and ventricu-lar preexcitation. Eur J Cardiol. 1977;5(6):493-505.
- 6. Van Praagh R. Segmental approach to diagnosis. In: Nadas' Pediatric Cardiology. Philadel-phia: Saunders, Fyler. Hanley & Belfus;2006. p.39-49.
- 7. Lev M, Rowlatt VF. The pathologic anatomy of mixed levocardia. Am J Cardiol. 1961;8:250-5.
- 8. Fang F, Li ZA, Yang Y, Zheng CH, Lam YY. Deciphering the mysteries of crisscross heart by transthoracic echocardiography. Echocardiography. 2011;28(1):104-8.
- 9. Yang YL, Wang XF, Cheng TO, Xie MX, Lü Q, He L, et al. Echocardiographic characteris-tics of the criss-cross heart. Int J Cardiol. 2010;140(2):133-7.
- 10. Rubensfigueroa J, Erdmenger Orellana J, Muñoz Castellanos L, Vázquez Antona C, Buendía Hernández A, Vargas Barrón J. Echocardiographic segmental analysis in patients with an atrioventricular criss-cross. Rev Esp Cardiol. 2009;62(9):1055-9.
- 12. Del PasquaA, Sanders SP, Rinelli G. Images in cardiovascular medicine. Three-dimensional echocardiography in crisscross heart: could a specimen be better? Circulation. 2007;116(17):e414-5.
- 13. Ming Z, Yumin Z. Magnetic resonance evaluation of criss-cross heart. Pediatr Cardiol. 2008;29(2):359-65.
- 14. Cantinotti M, Bell A, Hegde S, Razavi R. A segmental approach to criss-cross heart by car-diac MRI. Int J Cardiol. 2007;118(3):e103-5.
- 15. Nielsen JC, Parness IA. Anatomy of a criss-cross heart. Circulation. 2002;106(9):e41.
- 16. Araoz PA, Reddy GP, Thomson PD, Higgins CB. Images in cardiovascular medicine. Mag-netic resonance angiography of criss-cross heart. Circulation. 2002;105(4):537-8.
- 17.Alva C, Jiménez S, David F, Ortegón J, Sánchez A, Jiménez D, et al. Atrioventricular dis-cordance. Clinico-surgical experience 1990-2000. Arch Inst Cardiol Mex. 2000;70(6):561-8.
- 18. Gerlis LM, Ho SY, Anderson RH, Branfoot AC. The anatomy of a collection. Cardiovasc Pathol. 1999;8(2):103-7.
- 19. Choe YH, Kim YM, Han BK, Park KG, Lee HJ. MR imaging in the morphologic diagnosis of congenital heart disease. Radiographics. 1997;17(2):403-22.
- 20. Morelli PJ, Kimball TR, Witt SA, Meyer RA. Echocardiographic considerations in demon-strating complex anatomy of crisscross atrioventricular valves and discordant atrioventricular and ventriculoarterial relations. J Am Soc Echocardiogr. 1996;9(5):727-9.
- 21. Nagatsu M, Harada Y, Takeuchi T, Goto H, Ota Y. Can concordant criss-cross heart be ameliorated by hemodynamic changes? Ann Thorac Surg. 1995;60(3):699-701.
- 22. Vargas-Barron J, Rijlaarsdam M, Romero-Cardenas A, Keirns C, Diaz-Moncada S. Transesophageal echocardiography in adults with congenital cardiopathies. Am Heart J. 1993;126(2):426-32.
- 23. Yoo SJ, Seo JW, Lim TH, Park IS, Hong CY, Song MG, et al. < Hearts with twisted atrioven-tricular connections: findings at MR imaging. Radiology. 1993;188(1):109-13.
- 24. Geva T, Van Praagh S, Sanders SP, Mayer JE Jr, Van Praagh R. Straddling mitral valve with hypoplastic right ventricle, crisscross atrioventricular relations, double outlet right ventricle and dextrocardia: morphologic, diagnostic and surgical considerations. J Am Coll Cardiol. 1991;17(7):1603-12.
- 25. Sreeram N, Stümper OF, Kaulitz R, Hess J, Roelandt JR, Sutherland GR. Comparative value of transthoracic and transesophageal echocardiography in the assessment of congenital abnor-malities of the atrioventricular junction. J Am Coll Cardiol. 1990;16(5):1205-14.
- 26. Myers JL, Waldhausen JA, Weber HS, Arenas JD, Cyran SE, Gleason MM. A reconsidera-tion of risk factors for the Fontan operation. Ann Surg. 1990;211(6):738-43.
- 27.Battistessa S, Soto B. Double outlet right ventricle with discordant atrioventricular connex-ion: an angiographic analysis of 19 cases. Int J Cardiol. 1990;27(2):253-63.
- 28. Igarashi H, Kuramatsu T, Shiraishi H, Yanagisawa M. Criss-cross heart evaluated by colour Doppler echocardiography and magnetic resonance imaging. Eur J Pediatr. 1990;149(8):523-5.
- 29. Héry E, Jimenez M, Didier D, van Doesburg NH, Guérin R, Fouron JC,. Echocardiographic and angiographic findings in superior-inferior cardiac ventricles. Am J Cardiol. 1989;63(18):1385-9.
- 30. Anderson RH, Smith A, Wilkinson JL. Disharmony between atrioventricular connections and segmental combinations: unusual variants of "crisscross" hearts. J Am Coll Cardiol. 1987;10(6):1274-7.
- 31. Carminati M, Valsecchi O, Borghi A, Balduzzi A, Bande A, Crupi G, et al. Cross-sectional echocardiographic study of criss-cross hearts and superoinferior ventricles. Am J Cardiol. 1987;59(1):114-8.
- 32. Marino B, Sanders SP, Pasquini L, Giannico S, Parness IA, Colan SD. Two-dimensional echocardiographic anatomy in crisscross heart. Am J Cardiol. 1986;58(3):325-33.
- 33. Nakada I, Nakamura T, Matsumoto H, Sezaki T. Successful repair of criss-cross heart using modified Fontan operation.Chest. 1983;83(3):569-70.
- 34. Dunn JM, Donner R, Black I, Balsara RK. Palliative repair of transposition of the great ar-teries with criss-cross heart: ventricular septal defect and hypoplastic right (systemic) ventricle. J Thorac Cardiovasc Surg. 1982;83(5):755-60.
- 35. van Mill G, Moulaert A, Harinck E, Wenink A, Oppenheimer-Dekker A. Subcostal two-dimensional echocardiographic recognition of a criss-cross heart with discordant ventriculoarterial connection. Pediatr Cardiol. 1982;3(4):319-23.
- 36. Tadavarthy SM, Formanek A, Castaneda-Zuniga W, Moller JH, Edwards JE, Amplatz K. The three types of criss-cross heart: a simple rotational anomaly. Br J Radiol. 1981;54(645):736-43.
- 37. Marcelletti C, Mazzera E, Olthof H, Sebel PS, Düren DR, Losekoot TG, et al. Fontan's op-eration: an expanded horizon. J Thorac Cardiovasc Surg. 1980;80(5):764-9.
- 38. Danielson GK, Tabry IF, Ritter DG, Fulton RE. Surgical repair of criss-cross heart with straddling atrioventricular valve. J Thorac Cardiovasc Surg. 1979;77(6):847-51.
- 39. Freedom RM, Culham G, Rowe RD. The criss-cross and superoinferior ventricular heart: an angiocardiographic study. Am J Cardiol. 1978;42(4):620-8.
- 40. Anderson KR, Lie JT, Sieg K, Hagler DJ, Ritter DG, Davis GD. A criss-cross heart. De-tailed anatomic description and discussion of morphogenesis. Mayo Clin Proc. 1977;52(9):569-75.
- 41. Anderson RH, Shinebourne EA, Gerlis LM. Criss-cross atrioventricular relationships pro-ducing paradoxical atrioventricular concordance or discordance. Their significance to nomen-clature of congenital heart disease. Circulation. 1974;50(1):176-80.
- 42. Atik E. Caso 3/2007: lactente de três meses com criss-cross heart, discordância atrioventri-cular e dupla via de saída de ventrículo direito, sem estenose pulmonar. Arq Bras Cardiol. 2007;88(6):693-5.
- 43. VanPraagh R, VanPraagh S, Vlad P, Keith JD. Anatomic types of congenital dextrocardia: diagnostic and embryologic implications. Am J Cardiol. 1964;13:510-31.
- 44. Wallis GA, Debich-Spicer D, Anderson RH. Congenitally corrected transposition. Orphanet J Rare Dis. 2011;6:22.
- 45. Croti UA, Mattos SS, Pinto Jr VC, Aiello VD. Cirurgia cardiovascular pediátrica. 1Ş ed. São Paulo:Roca;2008.
- 46. Gatzoulis MA, Webb G, Broberg C, Uemura H. Cases in adult congenital heart disease. Complex congenital heart conditions. 2010;1:278-80.
- 47. Angelini P, Lopez A, Lufschanowski R, Nemeth MA, Flamm SD. Coronary arteries in crisscross heart. Tex Heart Inst J. 2003;30(3):208-13.
- 48. Ya J, Erdtsieck-Ernste EBHW, Boer PAJ, Van Kempen MJA, Jongsma H, Gros D, et al. Heart defects in connexin 43-deficient mice. Circulation Research 1998, 82:360-6.
- 49. Chaible LM. Efeitos da deleção do gene Cx43 sobre o desenvolvimento fetal de camundon-gos de diferentes backgrounds genéticos: ênfase na osteogênese [Dissertação de mestrado]. São Paulo:Universidade de São Paulo; 2009.
- 50. Reaume AG, Sousa PA, Kulkarni S, Langille BL, Zhu D, Davies TC, et al. Cardiac mal-formation in neonatal mice lacking connexin43. Science. 1995;267(5205):1831-4.
- 51. Wallis GA, Debich-Spicer D, Anderson RH. Congenitally corrected transposition. Orphanet J Rare Dis. 2011;6:22.
- 52. Valenzuela JMB, Lucas E, Bomfin Jr EJ. Criss-cross heart: diagnóstico fetal. Rev Bras Ecocardiogr Imagem Cardiovasc. 2009;22(2):51-6.
- 53. Robinson PJ, Kumpeng V, Macartney FJ. Cross sectional echocardiographic and angiocar-diographic correlation in criss cross hearts. Br Heart J. 1985;54(1):61-7.
- 54. Carminati M, Valsecchi O, Borghi A, Balduzzi A, Bande A, Crupi G, et al. Cross-sectional echocardiography study of criss-cross heart and superoinferior ventricles. Am J Cardiol. 1987:59(1):114-8.
- 55. Attie F, Zabal C, Buendia A. Cardiologia pediátrica diagnóstico y tratamiento. México. 1993;1:353-62.
- 55. Link KM, Weesner KM, Formanek AG. MR imaging of the criss-cross heart. AJR Am J Roetgenol. 1989;152(4):809-12.
- 57. Araoz PA, Reddy GP, Thomson PD, Higgins CB. Images in cardiovascular medicine. Magnetic resonance angiography of criss-cross heart. Circulation. 2002;105(4):537-8.
- 58. Fantini FA, Gontijo B, Martins C, et al. Operação de Fontan: uma técnica em evolução. Rev Bras Cir Cardiovasc 2009;24(4):463-9.
- 59. Carotti A, Iorio FS, Amodeo A, Giamberti A, Marianeschi S, Nava S, et al. Total cavopul-monary direct anastomosis: a logical approach in selected patients. Ann Thorac Surg. 1993;56(4):963-4.
- 60. Sato K, Ohara S, Tsukaguchi Yyasui K, Nakata T, Tamai M, et al. A criss-cross heart with concordant atrioventriculo-arterial connection. Report of case. Circulation. 1978;57(2):396-400.
- 61. Danielson GK, Tabry IF, Ritter DG, Fulton RE. Surgical repair of criss-cross heart with straddling atrioventricular valve. J Thorac Cardiovasc Surg. 1979;77(6):847-51.
- 62. Kashiwagi J, Imai Y, Aoki M, Shin'oka T, Hagino I, Nakazawa M. An arterial switch oper-ation for a concordant crisscross heart with the complete transposition of the great arteries. J Thorac Cardiovasc Surg. 2002;124(1):176-8.
- 63. Gontijo Filho B, Fantini FA, Martins C, Lopes RM, Pereira RST, Rabelo SM, et al. Estra-tégia cirúrgica na transposição das grandes artérias com septo interventricular intacto após pe-ríodo neonatal. Arq Bras Cardiol. 2005;85(1):39-44.
- 64. Plaché C, Bruniaux J, Lacour-Gayet F, Kachaner J, Binet JP, Sidi D, et al. Switch operation for transposition of the great arteries in neonates. A study of 120 patients. J Thorac Cardiovasc Surg. 1988;96(3):354-63.
- 65. Lacourt-Gayet F, Piot D, Zoghbi, Serraf A, Gruber P, Macé L, et al. Surgical management and indication of left ventricular retraining in arterial switch for transposition of the great arteries with intact ventricular septum. Eur J Cardiothoracic Surg. 2001;20(4):824-9.
- 66. Iyer KS, Sharma R, Kumar K, Bhan A, Kothari SS, Saxena A, et al. Serial echocardiog-raphy for decision making in rapid two-stage arterial switch operation. Ann Thorac Surg. 1995;60(3):658-64.
- 67. Davis AM, Wilkinson JL, Karl TR, Mee RB. Transposition of the great arteries with intact ventricular septum. Arterial switch repair in patients 21 days of age or older. J Thoracic Cardi-ovasc Surg. 1993;106(1):111-5.
- 68. Ducan BW, Poirier NC, Mee RB, Drummond-Webb JJ, Qureshi A, Mesia CI, et al. Selec-tive timing for the arterial switch operation. Ann Thorac Surg. 2004;77(5):1691-6.
- 69. Yacoub MH, Radley-Smith R, Maclaurin R. Two-stage operation for anatomical correction of transposition of the great arteries with intact interventricular septum. Lancet. 1977;1(8025):1275-8.
- 70. Williams WG, Quaegebeur JM, Kirklin JW, Blackstone EH. Outflow obstruction after the arterial switch operation: a multiinstitutional study. Congenital Heart Surgeons Society. J Thorac Cardiovasc Surg. 1997;114(6):975-87.
- 71. Nogi S, McCrindle BW, Boutin C, Williams WG, Freedom RM, Benson LN. Fate of the neopulmonary valve after the arterial switch operation in neonates. J Thorac Cardiovasc Surg. 1998;115(3):557-62.
- 72. van de Wal HJ, Tanke RF, Roef MJ. The modified Senning operation for cavopulmonary connection with autologous tissue. J Thorac Cardiovasc Surg. 1994;108(2):377-80.
- 73. Björk VO, Olin CL, Bjarke BB, Thorén CA. Right atrial-right ventricular anastomosis for correction of tricuspid atresia. J Thorac Cardiovasc Surg. 1979;77(3):452-8.
- 74. Kreutzer J, Kaene JF, Lock JE, Walsh EP, Jonas RA, Castañeda AR, et al. Conversion of modified Fontan procedure to lateral atrial tunnel cavopulmonary anastomosis. J Thorac Cardiovasc Surg. 1996;111(6):1169-76.
- 75. Rossi MA, Braile DM, Teixeira MD, Carrilo SV. Calcific degeneration of pericardial val-vular xenografts implanted subcutaneously in rats. Int J Cardiol 1986;12(3):331-9.
- 76. Arbustini E, Jones M, Ferrans VJ. Formation of cartilage in bioprosthetic cardiac valve im-planted in sheep: a morphologic study. Am J Cardiol. 1983;52(5):632-6.
- 77. Pires AC, Saporito WF, Leão LEV, Forte V, Cardoso SH, Ramaciotti O. Pericárdio bovino utilizado como remendo no sistema cardiovascular. Rev Bras Cir Cardiovasc. 1997;12(2):176-87.
- 78. Pinto Jr. VC, Carvalho Jr. W, Barroso HB, Mejia JAC, Mesquita FA, Sardenberg CRC, et al. Anastomose cavo-pulmonar total sem uso de material protético. Rev Bras Cir Cardiovasc. 1998;13(3):234-8.
Correspondence address:
Publication Dates
-
Publication in this collection
28 May 2013 -
Date of issue
Mar 2013
History
-
Received
09 May 2012 -
Accepted
26 Dec 2012