Abstract
In spite of the grate experience accumulated in vascular repairing, the ideal number of sutures for vascular anastomosis remains controversial. It is generally thought that the more stitches applied in a vascular anastomosis, the lesser resistant the anastomosis will be. The purpose of this study was to test this hypothesis in 20 rabbits, in which both carotid arteries were cross sectioned and repaired by end-to-end anastomosis with 8 interrupted sutures in one side (G1) and 16 in the other side (G2). After 3 and 15 days, the animals were randomly allocated for tensile strength, hydroxyproline determination (7 animals) and for histologic analysis of the anastomosis (3 animals). Conventional staining procedures (hematoxylin-eosin and Masson methods) and the picrosirius red polarization (PSP) technique for collagen type determination were used. From 3 to 15 days, the tensile strength increased in both groups, from 265.0±-44.4g to 391.2±-49.0g in G1 and from 310.0±-71.5g to 348.7±-84.0g in G2 (p<0.005), with no statistical difference between the groups in each period of study. The hydroxyproline content, expressed as hydroxyproline/protein ratio, varied from 0.04±-0.01 to 0.05±-0.02 in G1 and from 0.05±-0.01 to 0.05±-0.02 in G2, with no significant difference between periods and groups. The histology showed similar inflammatory and reparative aspects in both groups. In both groups and periods the PSP technique demonstrated predominantly type I collagen in relation to type III collagen in the anastomosis. We concluded that even doubling the number of stitches, the healing process and strength did not change in the arterial anastomosis.
Arteries; Surgical anastomosis; Wound healing; Collagen
3 ORIGINAL ARTICLE
The relationship between suture number and the healing process of end-to-end arterial anastomosis1 1 Article the State University of São Paulo - Botucatú (UNESP).
Winston B. YoshidaI; Luiz E. NaresseI; Aparecida Y. O. AngeleliII; Sidnei LastoriaI; Júlio DefaveriIII; Paulo R. CuriIV; Antonio RodriguesV
IAssistant Professor, Doctor of the Dept. of Surgery and Orthopedics
IIAssistant Professor, Doctor of the Dept. of Medicine
IIIAssistant Professor, Doctor of the Dept. of Pathology
IVFull Professor of the Dept. of Bioestatistics-Faculty of Veterinary Medicine
VAssistant Professor, Doctor of the Dept. of Anathomy-Bioscience Institute
Addres reprint request
SUMMARY
In spite of the grate experience accumulated in vascular repairing, the ideal number of sutures for vascular anastomosis remains controversial. It is generally thought that the more stitches applied in a vascular anastomosis, the lesser resistant the anastomosis will be. The purpose of this study was to test this hypothesis in 20 rabbits, in which both carotid arteries were cross sectioned and repaired by end-to-end anastomosis with 8 interrupted sutures in one side (G1) and 16 in the other side (G2). After 3 and 15 days, the animals were randomly allocated for tensile strength, hydroxyproline determination (7 animals) and for histologic analysis of the anastomosis (3 animals). Conventional staining procedures (hematoxylin-eosin and Masson methods) and the picrosirius red polarization (PSP) technique for collagen type determination were used. From 3 to 15 days, the tensile strength increased in both groups, from 265.0±-44.4g to 391.2±-49.0g in G1 and from 310.0±-71.5g to 348.7±-84.0g in G2 (p<0.005), with no statistical difference between the groups in each period of study. The hydroxyproline content, expressed as hydroxyproline/protein ratio, varied from 0.04±-0.01 to 0.05±-0.02 in G1 and from 0.05±-0.01 to 0.05±-0.02 in G2, with no significant difference between periods and groups. The histology showed similar inflammatory and reparative aspects in both groups. In both groups and periods the PSP technique demonstrated predominantly type I collagen in relation to type III collagen in the anastomosis. We concluded that even doubling the number of stitches, the healing process and strength did not change in the arterial anastomosis.
Subject headings: Arteries. Surgical anastomosis. Wound healing. Collagen.
INTRODUCTION
Continuou and interrupted sutures are the most commonly used techniques for vascular anastomosis. Continuous suture the advantages of economy of time and material, and interrupted suture is prefered for microcurgery and for growing patients6,8,17. Previous paper showed no histologic or tensile strength difference between these two techniques6.
In sipte of the vast experience accumulated in vascular repairing, the ideal number of stitches required for vascular anastomosis remains controversial18. In general, there is a feeling that additional stitches on some arbitrary optimum number of sutures, would inherently weaken the anastomosis, because of further vessel disruption caused by the needle holes, and necrosis which may occur between stitches7. In the order hand, the more stitches applied in the anastomosis, the more hemostatic it will be.
Previous articles dealing with patency rates, resistance to traction, and histology of microvascular anastomosis, suggest the ideal number of sutures ranging from 85,7,18 to 1415. However, no comparative study was done considering all those above parameters in one single experiment.
The purpose of this study was to verify whether or not increasing the number of interrupted sutures in the carotid end-to-end anastomosis in rabbits, would lead to any alteration in the healing process of the vascular anastomosis.
METHOD
Twenty two NORFOLK rabbits, weighing from 2000 to 2500g were anesthetized with intravenous pentobarbital (30mg per kg), with additional 5mg per kg pentobarbital given as needed to maintain anesthesia. The animals were operated on in a supine position, attached on a Claude Berbard board. Proper oxygenation was insured by placing a small tubing in the oral cavity, carrying oxygen at 1 liter per minute.
The carotid arteries of both sides were approached by a midline cervical incision, and were encircled with vessel loops. Each artery was clamped and divided using microvascular instruments and surgical loupes magnification of 2.5 times. The arterial stumps were irrigated with heparinized saline (100 USP units/ml) and the adventitia was excised. The diameter of carotid arteries varied from 2.0 to 2.5 mm after local lidocaine application.
Using standart microvascular technique, each carotid artery was reconstrusted by end-to-end anastomosis with 8 (Group 1) or 16 (Group 2) interrupted sutures with 7-0 ProleneR (Ethicon Inc, SP, Brazil) on a 10 mm needle. The artery, right or left, which would receive 8 or 16 sutures, was randomly chosen. After the completion of the anastomosis, gentle local digital pressure was applied for hemostasis. All the anastomosis were performed by the same surgeon (WBY). After wound closure, the animals received 600 units of benzatin penicilin intramuscularly. No anticoagulant, antiplatelet or vasodilator agents were used.
The animals were allowed to recover from anesthesia and then replaced to their individual cages, with standart rabbit chow and water ad libitum. Dipirone was diluted in the water of the animals in the first postoperative day for analgesia.
After 3 and 15 days, 8 animals per period, chosen at random, were anesthetized and studied angiographically to determine the patency of the anastomosis. Five milliliters of ditriazoate-meglumine (Schering Ltd, SP, BRAZIL) contrast were injected through a 23 scalp needle in each proximal carotid artery, and serial pictures were taken. The animals with carotid thrombosis, even in one side, were excluded from the study. Immediately following angiographic evaluation, both carotid arteries were ligated proximally and distally and were excised in block, including the anastomotic site. The animals were then killed with pentobarbital overdose.
The arteries were immersed in a saline solution of papaverine (0.25 mg/ml) at 37º C to relax muscle bundles and to unify the state of muscle tension in all samples. Tensile strength was measured by one of the authors (LEN) blindly, in a tensiometer developed in the author's laboratory. Briefly, the equipament was fitted with a transducer on its top, where one of the extremities of the arterial segment was attached. The other extremity was connected to a vertical moving plataform, driven by a vertical rotating screw, driven in turn by a synchronous elestrical motor at a controlled velocity. The tensile strength was displayed digitally on the monitor and recorded on a strip chart recorder. The extremities of the carotid arteries were stretched longitudinally to the point of vessel rupture (tensile strenght values were expressed in gram).
Following tensile strenght measurement, the ruptured arterial segments were weighted and the content of hydroxyproline determined by the method of BERGMAN & LOXLEY4, modified by ANGELELI2. Briefly, each carotid artery was homogenized and submitted to acid hydrolysis with HCI 6N for 24 hours, neutralization with saturated LiOH (pH=7.0), oxidation with chloramine T (7% w/v in H2O), and reading in the spectrophotometer with the EHRLICH reagent. The total protein content in the specimen was also determined using a modification of the method of LOWRY et al12. Briefly, the acid hydrolysate was trated with alkaline cupper solution (1% w/v in H2O) and then allowed to react with Folin phenol reagent. The results were expressed as hydroxyproline/protein ratio.
Tensile strength values and hydroxyproline/protein ratio were statistically analyzed by two-way analysis of variance16. The level of significance adopted was 5%.
Three animals per period of experiment were chosen at random for histologic study. After angiography, their carotid arteries were excised and fixed in 10% formalin solution and sent for histologic processing. Hematoxilin-eosin and thrichromic Masson staining methods were used for conventional histology. Collagen types determination in the anastomosis was performed by the picrosirius polarization (PSP) method13. Briefly, 5 mm sections of isotonic 10% formalin fixed material were deparaffinized, hydrated to water, and stained during one hour in a 0.1% solution of Sirius Red (Sirius Red F3 B 200, Mobay Chemical Co. Union, New Jersey, USA) dissolved in aqueous satured picric acid. The sections were rapidly washed in running tap water and counterstained with fresh Harris hematoxylin for 6 hours. A conventional optical microscope with a strong light source and two polaroid filters was used to study the birefringency of the collagen.
RESULTS
The angiographic appearance of the two anastomosis was similar (Fig. 1) and no difference was demonstrated between the two groups related to stenosis. Two animals were excluded from the study, one with bilateral thrombosis and the other with thrombosis only in the convetional suture side.
Tensile strength increased significantly in both groups from the 3rd to the 15th postoperative day (p<0,05). However, there was no statistical difference between the groups in each period of study (Fig.2).
Hydroxyproline/protein ratio did not change along the periods of the study and no significant difference was demonstrated between the groups in each period (Fig.3).
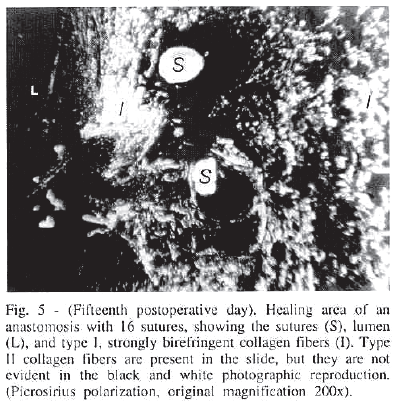
In the third postoperative day, conventional histology showed no relevant difference between the groups regarding inflammatory reaction and necrosis. In almost all slides, there was mural platelet thrombus with fibrin and few erythrocytes over deendothelized luminal surface near the anastomosis. Slight edema and fibrin - leukocyte exudate was also seen in this area (Fig. 4A). In the fifteenth day, both types of suture caused similar intensive reparative process, with granulomas and giant cells around the suture holes and intimal hyperplasia near the anastomosis site (Fig. 4B). Interruption of the elastic laminae was always seen (Fig. 4C). In both groups and periods, the PSP technique demonstrated predominantly type I collagen and lesser amount of type III collagen in the anastomosis (Fig. 5).
DISCUSSION
The healing process of blood vessels is not extensively studied in the literature, but there is an agreement that follows the usual inflammatory and reparative sequence of other surgically tissues1,3,9,10. This sequence was, in general, reproduced in the present study. In the initial period (3 days), the inflammatory reaction was predominant, with necrosis and endothelial loss restricted to the suture site. After 15 days, reparative phenomena were evident, with granulomatous, foreign body type reaction, fibroplasia filling the injured area, and intimal hyperplasia covering the inner surface of the vessel. The placement of 16 interrupted sutures apparently did not cause further necrotic, inflammatory or reparative reaction compared to the standart 8 interrupted sutures.
Intimal hyperplasia is probaly consequence of trauma of the vessel wall. Miointimal cells are supposed to be involved in this process, with its capabilities of collagen, elastic and muscle fibers synthesis, depending on the local demand11. These cells reach the intimal layer through fractures of internal elastic laminae and proliferate generally after 10 or 15 days of surgery3 concomitant with the new endothelial paving of the anastomosis5. In the present study, intimal hyperplasia was similar in both groups, although more surgical trauma was supposed to occur in the anastomosis with more stitches. Comparing to other authors3,11,17, we have found less foreign body granuloma around the suture holes, maybe because we have used polypropylene, which is known to be more biocompatible than the nylon, used by those authors.
Collagen is one of the main components of the structural skeleton of the tissues and plays an important role in the healing process, giving tensile strength to the scar10. Previous studies with the PSP method in normal arteries showed that collagen type I appears as thick, bright, strongly birefringent yellow or red fibers in the tunica adventitia; in contrast, type III collagen appars as thin, pale, weakly birefringent, greenish fibers in the tunica media14. In the present study, these characteristics were also observed in normal areas of the arteries, far from the anastomotic site. At the healing area, however, there was predominantly type I collagen in the whole width of the arterial wall of both goups and periods.
Besides this qualitative analysis, the collagen was quantified by hydroxyproline determination, which estimates new synthesized, mature and lysed collagens2. The hydroxyproline/total protein ratio was utilized to eliminate errors, due to dilution of collagen caused by local edema, which is present mainly in the inflammatory phase. The hydroxyproline/protein ratio did not change from 3rd to 15th postoperative day. However, tensile strength increased in both groups along this same period. Tensile strength is a physical measurement which reflects the degree of intermolecular collagen cross-linking, rather than its biosynthesis10. Tensile strength increase in this study is problaly due to the formation of further collagen cross-links and a change to a more stable forms which lead to reorientation of the direction of the bundles.
In the literature, there is not a consensus on the number of stitches to apply in a small artery anastomosis. Robertson & Robertson15, by only inspecting the anastomosis under the surgical microscope, sugested 12 or 14 sutures in end-to-end anastomosis, because they found more stenosis and thrombosis only in anastomosis performed with a lesser number of sutures. Wang et al.18 did not find difference in patency rates or aneurysm formation varying the number of sutures, but concluded that 8 sutures were ideal because the completion time in this group was lower. Colen et al.7 using a spring scale for tensile stregth measurements of the anastomosis, concluded that 8 was the best number of sutures for an arterial anastomosis. Calvo & Purriel5 comparing histologically 11 sutures with 11-0 nylon and 8 sutures of 10-0 nylon in end-to-side anastomosis did not find any histological difference. Even utilizing different diamates of suture threads, they suggested that 8 sutures were better, because they considered them enough for an anastomosis.
The present work, besides employing some parameters utilized by previous authors, was also completed by qualitative and quantitative collagen analysis, Therefore, our data suggest that even doubling the number of stitches, the healing process and the strength does not change in the arterial anastomosis. So, at least in a short-term (15 days) follow-up, for hemostatic purposes or according to personal preferences, applying additional stitches in an arterial anastomosis or using more stitches than the habitual for a particular artery, will not interfere in its healing process. However, more studies are necessary to know the influence of the number of stitches on long-term patency rates.
ACKNOWLEDGEMENTS
The authors thank to Dr. Edevar Mombrum for his help in PSP processing and to Mrs. Maria Helena Spadot and Sonia Regina Correa for technical assistance.
Addres reprint request:
Winston Bonetti Yoshida
Depto. de Cirurgia e Ortopedia
Faculdade de Medicina de Botucatu
Universidade Estadual Paulista
18618-000 - Botucatu - SP
Brazil
Accepted for publication on march, 1997.
- 1. ACLAND, R.D. & TRACHEMBERG, L. - The histopathology of small arteries following experimental microvascular anastomosis. Plast. Reconst. Surg., 60:868-75, 1977.
- 2. ANGELELI, A.Y.O., BURINI, R.C., OLIVEIRA, J.E.D. - Padronização da metodologia para determinações das frações da hidroxiprolina urinária. Rev. Bras. Patol. Clín., 18:124-7, 1982.
- 3. BAXTER, T.J., O'BRIEN, B.M.C.C., HENDERSON, P.N., BENNET, R.C. - The histopathology of small vessels following microvascular repair. Br. J. Surg., 59:617-22, 1972.
- 4. BERGMAN, I. & LOXLEY, R. - The determination of hydroxyproline in urine hydrolysates. Clin. Chim. Acta, 27:347-9, 1970.
- 5. CALVO, A. & PURRIEL, J.A. - Microanastomosis terminolateral en la carótida de la rata: valoración histolóica de la permabilidad en relación al número de puntos de la sutura y al hilo utilizado. Acta Neurol. Latinoamer., 26:215-22, 1980.
- 6. CARVALHO, I., YOSHIDA, W.B., NARESSE, L.E., ANGELELI, A.Y., CURY, P.R. FABRIS, V.E., MAFFEI, F.H.A. - Estudo comparativo da cicatrização de anastomoses término-terminais em artérias carótidas de coelho, com sutura contínua e sutura com pontos separados: avaliação anatomopatológica e da força de ruptura. Cir. Vasc. Angiol., 92:6-12, 1993.
- 7. COLEN, L.B., GONZALES, F.P., BUNCKLE, H.J. - the relationship between the number of sutures and the strength of microvascular anastomosis. Plast. Reconst. Surg., 64:325-9, 1979.
- 8. COURMIER, J.M. & FLORENT, J. - Técnicas generales de cirugía arterial. In: COURMIER, J.M.- Tratado de técnicas cirúrgicas. V. Artérias-venas-linfáticos Barcelona, Toray-Mason, p.3-39, 1973.
- 9.KOLB, S., WRAY, R.C., WEEKS, P.M. - Bursting strength of microarterial repair. Surg. Forum, 30:531-3, 1979.
- 10. LEAPER, D.F. - Blood Vessels. In: BUCKNALL & ELLIS, ed. - Wound healing for surgerons London, Bailleri Tindall, p. 221-40, 1984.
- 11. LINDMAN, D. & DANIEL, R.K. - The normal healing process of microvascular anastomoses. Scand. Reconst. Surg., 15:103-10, 1981.
- 12. LOWRY, O.H., ROSENBROUGH, N.J. FARR, A.L. - Protein measurement with Folin phenol reagent. J. Biol. Chem, 193:265-75, 1951.
- 13. MONTES, G.S. & JUNQUEIRA, L.C.U. - The use of picrosirius-polarization method for the study of biopathology of collagen. Mem. Inst. Oswaldo Cruz, 86 (suppl. III): 1-11, 1991.
- 14. MONTES, G.S., NICOLELIS, M.A.L, BRENTANI-SAMAIA, H.P., FURVIE, S.S. - Collagen fibril diameters in arteries of mice: a comparison of manual and computed-aided morphometrc analyses. Acta Anat., 135:57-61, 1989.
- 15. ROBERTSON, J.H. & ROBERTSON, J.T. - The relationship between suture number and quality of anastomoses in macrvascular procedures. Surg. Neurol, 10:241-5, 1978.
- 16. SNEDCOR, G.W. & COCHRAN, W.S. - Statistical methods. Iwoa State University Press; AMES, 505 p, 1980.
- 17. STEEN, S., ANDERSSON, L., LOWENHIELM, P., STRIDBECK, H., WALTHER, B., HOLMIO, T. - Comparison between absorbable and nonabsorbable monofilament sutures for end-to-end arterial anastomosis in growing pigs. Surgery, 95:202-8, 1984.
- 18. WANG, S., MARINI, C.P., BASO, S., MAUGHAN, R.E., CUNNINGHAM, J.N., JACOBITZ, I.J. - Optimal number of sutures for microvascular anastomosis. Microsurgery, 13: 161, 1992.
Publication Dates
-
Publication in this collection
19 Nov 2010 -
Date of issue
June 1997