Abstract
To monitor the evolution of anastomoses performed on the distal colon in a situation of experimental peritonitis, 37 Wistar-Tecpar male rats aged 114 to 130 days and weighing on avarage 298 g were divided into two lots: group S (control, N = 18) and group P (experimental, N = 19). P rats were submitted to laparotomy and peritonitis was induced by perforating the cecum with a needle, and S rats were only submitted to manipulation of the cecum. Twenty-four hours later animals were resubmitted to laparotomy and distal colectomy was performed 1.5 cm to the peritoneal reflection. End-to-end anastomosis was performed on a single extramucosal plane using 8 separate stitches with 5-0 polypropylene sutures. The anastomoses were checked on the 3rd and 7th postoperative day. Upon opening the peritoneal cavity, the presence of alterations such as peritonitis or abscesses, adhesions, organs involved, fistulas or dehiscences was reorded. A 4.0 cm segment of the colon containing the anastomosis was resected and rupture pressure was measured. Epithelialization of the mucosal wound was evaluted and the material was studied histopathologically for inflammatory reaction and scar condition. Upon relaparotomy, peritonitis was detected in all P animals and fibrin was observed in the cavity of all animals. Adhesions were present in 2 groups, without significant differences between them. Mean rupture pressure was 108.7 mm Hg in group S and 112.0 mm Hg in group P on the 3rd day and 205.0 mm Hg in group S and 206.6 mm Hg in group P on the 7th day, with no significant difference between groups. Microscopic evolution was similar in the two groups. These results permit us to conclude that peritonitis induced by this method does not modify the healing process of distal colon anastomoses in rats.
Surgical anastomosis; Infection; Colon
4 ORIGINAL ARTICLE
Evaluation of the cicatrization of left colon anastomoses in the presence of peritonitis. an experimental study on rats1 1 Article from Discipline of Scientific Methodology on Clinical and Surgical Experimentation - Faculdade de Medicina do Paraná (FEMPAR).
Maria de Lourdes Pessole Biondo-SimõesI; Lucilea dos Santos CanalliII; Cristiane FerreiraII; Renata MeschinoII; Ticyane KaimotoII; Luiz Martins CollaçoIII
IProfessor of the Discipline
IIStudents of the FEMPAR
IIIAssistant Professor of Pathology of the FEMPAR
Address reprint request Address reprint request: Maria de Lourdes Pessole Biondo-Simões Rua Ari José Valle, 1987, Santa Felicidade 82030-000 Curitiba, Paraná Telephone (041) 273.51.17
SUMMARY
To monitor the evolution of anastomoses performed on the distal colon in a situation of experimental peritonitis, 37 Wistar-Tecpar male rats aged 114 to 130 days and weighing on avarage 298 g were divided into two lots: group S (control, N = 18) and group P (experimental, N = 19). P rats were submitted to laparotomy and peritonitis was induced by perforating the cecum with a needle, and S rats were only submitted to manipulation of the cecum. Twenty-four hours later animals were resubmitted to laparotomy and distal colectomy was performed 1.5 cm to the peritoneal reflection. End-to-end anastomosis was performed on a single extramucosal plane using 8 separate stitches with 5-0 polypropylene sutures. The anastomoses were checked on the 3rd and 7th postoperative day. Upon opening the peritoneal cavity, the presence of alterations such as peritonitis or abscesses, adhesions, organs involved, fistulas or dehiscences was reorded. A 4.0 cm segment of the colon containing the anastomosis was resected and rupture pressure was measured. Epithelialization of the mucosal wound was evaluted and the material was studied histopathologically for inflammatory reaction and scar condition. Upon relaparotomy, peritonitis was detected in all P animals and fibrin was observed in the cavity of all animals. Adhesions were present in 2 groups, without significant differences between them. Mean rupture pressure was 108.7 mm Hg in group S and 112.0 mm Hg in group P on the 3rd day and 205.0 mm Hg in group S and 206.6 mm Hg in group P on the 7th day, with no significant difference between groups. Microscopic evolution was similar in the two groups. These results permit us to conclude that peritonitis induced by this method does not modify the healing process of distal colon anastomoses in rats.
Subject headings: Surgical anastomosis. Infection. Colon.
INTRODUCTION
In view of the high incidence of infection of the peritoneal cavity in surgical practice, many investigators have the relationship between peritonitis and healing of intestinal anastomoses. Contradictory results have been obtained in studies of the influence of infection on the development of colon anastomoses healing in experimental animals, with some investigators reporting high rates of dehiscense and mortality6,8,21 and others reporting little or no effect of infection on the anastomotic lesion12,18,20
Thus, the present study was conducted to determine the effect of peritonitis on the healing of experimentally induced colon anastomoses in rats.
METHOD
The study was conducted on 40 male rats (Rattus norvegicus albinus, Rodentia mammalia) of the Wistar-Tecpar strain aged 114 to 130 days and weighing on average 298 g. The animals were divided in two groups S (control) and P (experimental).
The animals were anesthetized with ether, weighed and identified. The ventral abdominal wall was shaved and a median 4 cm laparotomy was performed. In P animals, the induction of peritonitis consisted of partial ligation of the cecum immediately below the ileocecal triangular fold with 5-0 polypropylene sutures in order to increase pressure inside this portion of the intestine without provoking ischemia, and also to permit at the same time the free transit of the fecal bolus from the small intestine to the large bowel. The cecum was then perforated at 10 random points with a 40 x 13 venipuncture needle. The abdominal wall was closed with continuous 4-0 coton sutures on two planes , i.e., peritoneum-muscle-aponeurosis and skin. After recovery from anesthesia the rats were returned to their cages where they had free acces to water and ration.
In group S animals the first procedure consisted of manipulation of the cecum passing 5-0 polypropylene suture through its base without performing ligation. Laparorrhaphy was the same as performed in P rats.
Twenty-four after the first surgery, the animals were anesthetized and resubmitted to laparotomy. Total left transverse colotomy was performed 1.5 cm from the peritoneal reflection, followed by end-to-end anastomosis on a single extramucosal plane with 8 separate stitches using 5-0 propylene sutures, Laparorrhaphy was performed on two planes as done in the first surgery, and the animals were allowed to recover from anesthesia and returned to their cages with free acces to water and ration until the day for verification.
The animals were sacrified with a lethal dose of sulfuric ether on the 3rd and 7th day. Changes in the peritoneal cavity, such as presence of purulent or fibrinoid secretion indicating the presence of peritonitis, adhesions and organs involved, fistulas or dehiscences, were recorded. A 4-cm colon fragment containing the anastomosis was removed and submitted to a measurement of rupture pressure by the method of CRONIN, JACKSON and DUNPHY (1968). The surgical piece was opened along the antimesentery border and the epithelialization of the mucosal wound was evaluted. We also determined the possible presence of a mucosal ucler (term used to define the anastomosis line still without reeptheli and covered with fibrin), an internal spur and surgical sutures in the mucosa.
The colon segments were stretched out on filter paper, fixed in 10% formalin and submitted to histopathological study by the hematoxylin and eosin and Mallory trichrome methods.
The inflammatory reaction was scored as acute-chronic and chronic according to the predominance of cell types and according to scar organization in terms of the arrangement of the tunicae as disorganized, organizing and organized.
The presence of mucosal reepithelialization, mural abscess, necrosis and granulation tissue was determined microscopically.
Data was analyzed statistically by the Mann-Whitney test for analysis of the means and by the exact Fisher test for 2 x 2 tables, with the level of significance set at 0.05 or 5.00%.
RESULTS
Two animals from the 3 day control and 1 animal from the 7-day experimental group were excluded due to technical problems, so that 37 rats were left in the experiment.
MACROSCOPIC FINDINGS
PERITONEAL CAVITY
Peritonitis was absent in all S animals and present in 100.0% of P animals on the day of the second intervention and at both evaluation times.
Adhesions were present in 100.0% of the animals of both groups on the 3rd and 7th days, involving fat of the spermatic funiculus, seminal vesicle, posterior paretietal peritoneum, intestinal loops and mesentery of the small intestine. In both groups, adhesions involved 3/4 to 4/4 of the circumference on the 3rd day, and 1/4, 3/4 or 4/4 on the 7th day.
No fistulas or deiscences were observed in either group at any time studied.
Figure 1 shows details of the abdominal cavity and adhesions in the animals of the two groups at the two evaluation times.
SURGICAL PIECE
On the 3rd and 7th day the outer surface presented adhesions, as descibed earlier.
Analysis of the mucosal surface revealed the presence of an internal spur in al surgical pieces from groups S and P.
Mucosal ulcer was identified in 100.0% of the pieces from group S an 90.0% of the pieces from group P on the 3rd (p = 0.3573) and in 60.0% of the pieces from group S and in 100.0% of the pieces from group P on the 7th (p = 0.0376).
Sutures turned towards the mucosa were detected in 25% of the pieces from group S and in 30.0% of those from group P on the 3rd day (p = 0.6176) and in 70.0% of the pieces from group S and 77.7% of those group P on the 7th day (p = 0.5557).
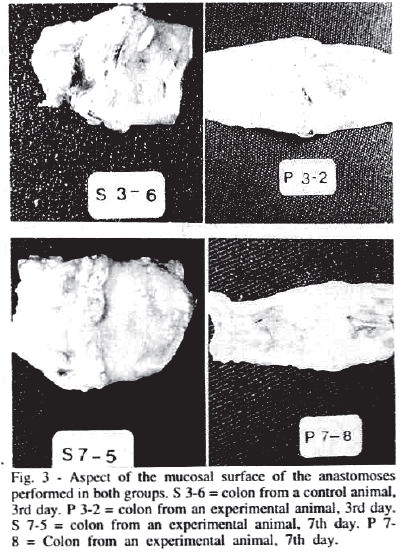
Figure 3 illustrates aspecs of the mucosal surface of the anastomoses of the animals in both groups at the two evaluation times.
RUPTURE PRESSURE
According to SMITH, COMMOLY and GILMORE (1982), anastomoses that rupture at pressures of less than 60.0mm Hg have flaws, even though these are undetectable by being blocked by nearby structures. If we consider this statement to be correct, no detectabel flaws were present in the pieces from the two groups submitted to measurement of rupture pressure.
On the 3rd postoperative day, pressures of 70.0 to 150.0 mm Hg (mean = 108.75 mm Hg) were obtained for group S and pressures of 60 to 150 mm Hg (mean = 112.0 mm Hg) were obtained for group P (Table I).
On the 7th day, rupture pressure ranged from 90.0 to 270.0 mm Hg (mean = 205.0 mm Hg) for group S and from 140.0 to 240.0 mm Hg (mean = 206.6 mm Hg) for group P (Table II).
MICROSCOPIC FINDINGS
On the 3rd and 7th day, microscopic analysis revealed the presence of polymorphonuclear cells, vascular congestion, macrophages, lymphocytes and monocytes, characterizing an inflammatory reaction of the acute-chronic type in all histological sections examined.
On the 3rd day the tunicae of the wall were disroganized in 75.0% of the histological sections in group S and in 80.0% of those of group P (p = 0.6176). On the 7th day, they were organizing in 70.0% of group S animals and in 56.0% of group P animals (p = 0.4299). Figures 4 and 5 presents photomicrographs of the histological sections.
A mural abscess was identified in 30.0% of the histological sections from group S and in 62.5% of the sections from group P on the 3rd day (p = 0.1842). On the 7th day, amural abscess was observed in 40.0% of the histological sections from group P and no abscesses were observed in group S (p = 0.0542).
Necrosis was observed in 10.0% of the histological sections from group S and in 11.0% of the sections from group P on the 3rd day (p<0.7059). On the 7th day there was no necrosis in either group.
Granulation tissue was detected in 100% of the histological sections both on the 3rd and on the 7th day.
DISCUSSION
Several authors consider infection to be one of the major causes of failure of colon anastomoses. COHN Jr. (1970) emphasized the role of infection in anastomosis dehiscence. DUNPHY (1970) and MASTBOOM et al. (1989) suggested that the presence of bacteria on the surface of the anastomosis promotes collagenolytic activy and accelerates dehiscence. HAWLEY et al. (1970), in a study on rats and rabbits, demonstrated a higher collagenase concentration near the infected intestinal sutures and in the mucosa of the colon and rectum. In study on the effect of infection on colon anastomoses in the rat, IRVIN (1976) demonstrated increased intracellular collagen lysis during the early phases of healing. According to YAMAKAWA et al. (1971), there was a decrease in collagen in dors with simulated diverticulitis. MORGENSTERN et al. (1972) reported a decrease in collagen synthesis in contaminated dog anastomoses. IRVIN and HUNT (1974), in an investigation of the cause of dehiscence in traumatized rats, concluded that infection is the immediate cause of anastomosis failure. NAHAI et al. (1977), in a study on dogs, observed that infection of the peritoneal surface along the suture line precedes dehiscence.
TORNQVIST et al. (1990), demonstrated in rats that infection is less important in terms of simulation of collagen metabolism and that the mechanical factor of obstruction d\has a greater effect in this situation. In the present study, although peritoneal infection was present it was not sufficient to promote fistulae or dehiscences, in agreement with data reported by RYAN (1970) and IRVIN and GOLIGHER (1973) who observed that gross infection did not prevent healing.
However, CLEAVER et al. (1974) reported delayed healing in the presence of peritoneonitis. HESP et al. (1984), in a study of infected intestinal anastomosis healing, concluded that infection reduced the hydroxyproline content at the site of anastomosis leading to a delay in recovery of local resistance.
The infection induced the resistance of anastomosis, as demonstrated by the measurement of rupture pressure, which was higher than 60.0 mm Hg in both control and experimental groups. This permitted us tp propose that there was no damage at the level of the anastomoses since, according to SMITH, WEHE, BADGER and PIRKLE (1974), above this pressure limit the anastomoses do not present healing failure. Wowever, mucosal reepithelialization was delayed in the peritonitis group compared to the control on the 7th day (p = 0.0376).
After inducing peritinitis by cecal perforation, BERMAN et al. (1974) reported 79.4% mortality within 24 hours and ALMDAL et al. (1985) reported 100% mortality after 3.0 mm perforations. LAZAR Jr. et al. (1987), CASTILLO et al. (1991) and ZALOGA et al. (1992), using combined perforation an ligation of the cecum below the ileocecal triangular fold reported mortality rates ranging from 34 to 100%.
MASRSHALL et al. (1988), using ligation and needle perforations, obtained peritonitis with edema and a 14% death rate. In the present study carried out using the same methodology there were no animal deaths, although the method proved to be efficient for obtaining peritonitis.
CONCLUSION
Analisys of the results obtained permits us to concluded that the course of healing of distal colon anastomoses in the presence of peritonitis is not significantly altered in rats.
Accepted for publication on march, 1997.
- 1. ALMDAHL, S.M; NORDTRAND, K.; MELBY, K.; OSTERUD, B.; GIECKSKY, K.E. - Faecal peritonitis in the rat, an experimental model for evaluation of surgical and adjuvant therapies. Acta Chir. Scand., 151:213-16, 1995.
- 2. BERMAN, I.R.; GROSFELD, J.L.; ADELMAN, B.A.; RAPP, R.J. - Influence of local and systemic factors on suvival with faecal peritonitis. Surg. Forum, 25:367-9, 1974.
- 3. CASTILLO, M.; PEREIRA, L.H.T.; GUTIERREZ, R.; PROUG, D.; SHAPIRO, E. - Peritonitis after cecal perfuration, an experimental model to suty the therapeutic role of antibiotics associated with Allopurinol and Catalase. Am. Surg.57:313-6, 1991.
- 4. CHON JR, I. - Intestinal antisepsis. Surg. Gynecol. Obstet., 130:1006-14, 1970.
- 5. CLEAVER, C.L.T.; HOPKINS, A.D.; KWONG, K.C.; RAFTERY, A.T. - The effect of postoperative peritoneal lavage on survival, peritoneal wound healing and adhesion formation following daecal peritonitis: an experimental study in teh rat. Br. J. Surg., 61:601-4, 1974.
- 6. DUNPHY, J.E. - The cut. Am. J. Surg, 119:1-8, 1970.
- 7. HAWLEY, P.R. - Causes and prevention of colonic anastomotic breakdown. Dis. Colon Tectum, 16:272-6, 1973.
- 8. HAWLEY, P.R.; FAULK, W.P.; HUNT, T.K.; DUNPHY, J.E. - Collagenase activy in gastrointestinal tract. Br.J. Surg, 896-900, 1970.
- 9. HESP, F.L.E.M.; HENDRIKS, T.L.; LUBBERS, E.C.; DeBOER, H.H.M. - Wound healing in the intestinal wall. Effects of inffection on experimental ileal and colonic anastomoses. Dis. Colon Rectum, 27:462-7, 1984.
- 10. IRVIN, T.T. - Collgen metabolism in efected anastomoses. Surg. Gynecol. Obstet., 143:220-4, 1976.
- 11. IRVIN, T.T. & HUNT, T.K. - Pathogenesis and prevention of discruption of colonic anastomoses in traumatized rats. Br. J. Surg., 61:437-9, 1974.
- 12. IRVIN, T.T. & C\GOLIGHER J.C. - Etiology of disruption of intestinal anastomoses. Br. J. Surg., 60:461-4, 1973.
- 13. LÁZAR J.R.; HUSZTIK, E.; LÁZÁR, G. - Effects of gadolinium chloride on acute septic peritonitis and septic shock in rats. Prog. Clin. Biol. Res, 236B:323-8, 1987.
- 14. MARSHALL, J.C.; CHRISTOU, N.V.; MEAKINS, J.L. - Small bowel basterial overgrowth an systemic immunosuppression in experimental peritiniris. Surgery, 104:404-11, 1988.
- 15. MASTBOOM, W.J.; HENDRIKS, T.; DeBOER, H.H - Collagen changes around intestinal anastomoses in germ-free rats. Br. J. Surg., 76:797-801, 1989.
- 16. MORGENSTERN, L.; YAMAKAWA, T.; BENSHOSHAN, M.; LIPPMAN, H. - Anastomotic leakage after low colonic anastomosis. Clinical and experimental aspects. Am. J. Surg., 123"104-8, 1972.
- 17. NAHAI, F.; LAMB, J.M.; HAVICAN, R.G.; STONE, H.H. - Factors involved in disruption of intestinal anastomoses. Am. Surg., 43:45-51, 1977.
- 18. RYAN, G.P. - Th effect of surronding infection upon the healing of colonic wounds. Experimental studies and clinical experiences. Dis. Colon Rectun, 13:124-6, 1970.
- 19. SCHROCK, T.R.; DEVENEY, C.W.; DUNPHY, J.E. - Factors contributing to leakage of colonic anastomoses. Ann. Surg., 137:13-8, 1973.
- 20. TÖRNQVIST, A.; BLOMQUIST, P.; JIBORN, H.; ZEDERFELDT, B.; SKOVAARD-JENSEN, H. - Impact of bacteria on metabolism of collagen in colonic obstruction in rats. Surg. Gynecol. Obstet, 171:5-8, 1990.
- 21. YAMAKAWA, T.; PATIN, C.S.; SOBEL, S.; MORGENSTERN, L. Healing of colonic anastomosis following resection for experimental "diverticulites". Arch. Surg 103:17-20, 1971.
- 22. ZALOGA, G.P.; SAGER, A.; BLACK, K.W.; PRIELIPP, R. - Low dose calcium administration increases mortality during septic peritonitis in rats. Circulatory Shock, 37:226-9, 1992.
Publication Dates
-
Publication in this collection
19 Nov 2010 -
Date of issue
June 1997