Abstracts
Objective - Thoracic lesions and resulting complications have gained increased importance in literature because they present a serious problem despite the generalized use of antibiotic therapy. Our study, therefore, aims at obtaining better estimates regarding the benefits obtained using antibiotic therapy in patients with isolated thoracic trauma and who have undergone closed chest drainage. Methods - Eight prospective and randomized studies were selected and meta-analysis was used to statistically associate the results. Results - The results demonstrated a statistical significance which favored the use of antibiotic therapy in preventing pleural empyema and a 9.25 (IC 95% 2.85 - 30.01) total relative risk for patients who did not receive antibiotic therapy. The total risk regarding all the infectious complications that occurred was 4.29 (IC 95% 2.70 - 8.97). Conclusion - The results of this meta-analysis study showed that antibiotic therapy effectively reduces the incidence of infectious complications in patients with isolated thoracic trauma, who have undergone closed pleural drainage.
Meta-analysis; Drainage; Empyema, pleural; Thoracic injuries
Objetivo - A literatura aponta para a crescente importância das lesões torácicas com sua possíveis complicações e, apesar do uso generalizado da antibioticoterapia, estas continuam a ser um grave problema. Assim, o propósito do presente estudo, foi de desenvolver melhores estimativas da quantidade de benefícios quanto a utilização da antibioticoterapia nos pacientes com trauma isolado do tórax, submetidos, unicamente, à drenagem pleural fechada. Métodos - Através do estudo de meta-análise, oito trabalhos, prospectivos e randomizados, foram selecionados para associação de seus resultados dentro de um modelo de análise estatística quantitativa. Resultados - Os resultados mostraram uma significância estatística favorável ao uso da antibioticoterapia na prevenção do empiema pleural, com risco relativo total de 9,25 (IC 95% 2,85 - 30,01) para os pacientes sem uso do antibiótico. Se consideradas a ocorrência de todas as complicações infecciosas, verifica-se que o risco total foi igual a 4,29 (IC 95% 2,70 - 8.97). Conclusão - Com os resultados do presente estudo de meta-análise, pode-se concluir que, o uso da antibioticoterapia se mostra fortemente favorável em reduzir a incidência de complicações infecciosas nos pacientes acometidos por trauma isolado do tórax e, submetidos à drenagem pleural fechada.
Meta-análise; Drenagem; Empiema pleural; Traumatismos torácicos
2 - ORIGINAL ARTICLE
INCIDENCE OF INFECTIOUS COMPLICATIONS FOLLOWING TUBE THORACOSTOMY WITH AND WITHOUT USE OF ANTIBIOTIC THERAPY: META-ANALYSIS STUDY1 1 . This study has been conducted by the Trauma Surgery Division of the Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas. 2 . Master of Trauma Surgery. 3 . Titular Professor, Chief - Trauma Surgery, Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas.
Mauro José Fontelles2 1 . This study has been conducted by the Trauma Surgery Division of the Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas. 2 . Master of Trauma Surgery. 3 . Titular Professor, Chief - Trauma Surgery, Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas.
Mario Mantovani3 1 . This study has been conducted by the Trauma Surgery Division of the Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas. 2 . Master of Trauma Surgery. 3 . Titular Professor, Chief - Trauma Surgery, Department of Surgery, Faculty of Medical Sciences, UNICAMP - Campinas.
Fontelles MJ, Mantovani M. Incidence of infectious complications following tube thoracostomy with and without use of antibiotic therapy: meta-analysis study. Acta Cir Bras [serial online] 2001 Oct-Dec;16(4). Available from: URL: http://www.scielo.br/acb.
ABSTRACT:Objective - Thoracic lesions and resulting complications have gained increased importance in literature because they present a serious problem despite the generalized use of antibiotic therapy. Our study, therefore, aims at obtaining better estimates regarding the benefits obtained using antibiotic therapy in patients with isolated thoracic trauma and who have undergone closed chest drainage. Methods -Eight prospective and randomized studies were selected and meta-analysis was used to statistically associate the results. Results - The results demonstrated a statistical significance which favored the use of antibiotic therapy in preventing pleural empyema and a 9.25 (IC 95% 2.85 - 30.01) total relative risk for patients who did not receive antibiotic therapy. The total risk regarding all the infectious complications that occurred was 4.29 (IC 95% 2.70 8.97). Conclusion - The results of this meta-analysis study showed that antibiotic therapy effectively reduces the incidence of infectious complications in patients with isolated thoracic trauma, who have undergone closed pleural drainage.
KEY WORDS: Meta-analysis. Drainage. Empyema, pleural. Thoracic injuries.
INTRODUCTION
Despite the generalized use of antibiotic therapy in thoracic trauma, infectious complications are still a serious problem that affect the patients general condition with repercussions in postoperative rates of morbidity and mortality and increase the cost of the treatment because of prolonged hospitalization.
This slow recovery also involves increased costs in relation to the individuals job, as there is a delay in returning to work. Therefore, it is extremely important to define the criteria regarding the use of antibiotics because a great majority of thoracic trauma patients undergo drainage during their treatment.
Although, there is a consensus in literature regarding the indications for a surgical procedure, antibiotic therapy is still a controversial topic because of the difficulties related to risk factor evaluation during the post-operatory of a patient with thoracic trauma lesions (1,2,3). Therefore, various studies have been conducted over the last few decades to try to establish more reliable parameters for the use of antibiotic therapy in cases of thoracic lesions (4,5,6).
Hence, the objective of our study was to use meta-analysis to assess the efficacy of antibiotic therapy in reducing the incidence of infectious complications in patients with isolated chest trauma, who have only undergone closed chest drainage.
METHODS
Meta-analysis is a statistical method which is gaining ground in clinical medicine in relation to quantitative or qualitative assessment of specialized literature that deals with research on defined scientific topics.
Quantitative meta-analysis is a technique, based on the results of previous studies, that is generally applied to synthesize various randomized clinical studies in order to obtain a better estimate of the benefits regarding certain medical procedures. However, it is sometimes more important to check if a clinical or surgical intervention is really beneficial and the technique used here is a qualitative (7,8) .
This method of analysis involves three phases: identifying studies in specialized literature that are related to the topic to be analyzed; analyzing the results of the selected studies; integrating the results within a statistical model.
Identifying studies
There are various studies in specialized literature related to the use of antibiotics in cases of infectious complications resulting from thoracic trauma . Fallon et al.,(9) 1992, conducted a similar research on articles published between 1997 to 1992 regarding thoracic trauma, chest drainage, with and without the use of antibiotic therapy and empyema. He selected six relevant publications and applied meta-analysis. In addition to Fallons study, there are studies by Gonzalez et al.,(10) 1998 and Fontelles et al.,(11) 2000, aimed at perfecting the results obtained (Table 1).
Criteria for inclusion
The selected studies were all prospective and randomized and followed the pre-established criteria. The patients evaluated in this study were isolated thoracic trauma cases, who had undergone closed chest drainage soon after being admitted at the emergency unit and the antibiotic administrated, even in vitro, presented activity against gram-positive bacteria.
Statistical analysis
Relative risk (RR) calculation, according to the Mantel-Haenszel method, was used in this study. Relative risk is also known as risk ratio and is the ratio between the risk of an exposed group and that of a non-exposed group. If the risks are the same the RR will be 1, but if they are not, the RR calculation is a direct manner, in relative terms, of showing the different risks (greater or smaller) for the exposed group 7. This study considered exposure to antibiotic therapy, which meant that the RR was calculated by finding the ratio of chances of an infection or pleural empyema occurring without the use of antibiotics with chances of an infection or pleural empyema occurring with the use of antibiotics. For example, if in table 1 (Grover12), 06 patients in the group without antibiotics and only 1 patient in the group with antibiotics, developed an infection, the RR would be (06/37)/ (01/37) = 6.
The Mantel-Haenszel method gives an estimate of the risk ratio for each study when all the studies are jointly considered. When the values obtained was found to be zero, the RR calculation corrected by approximation13,14. The program SAS System for Windows 6.12 version (SAS Institute Inc, Cary, NC, USA) was used to perform the calculations.
RESULTS
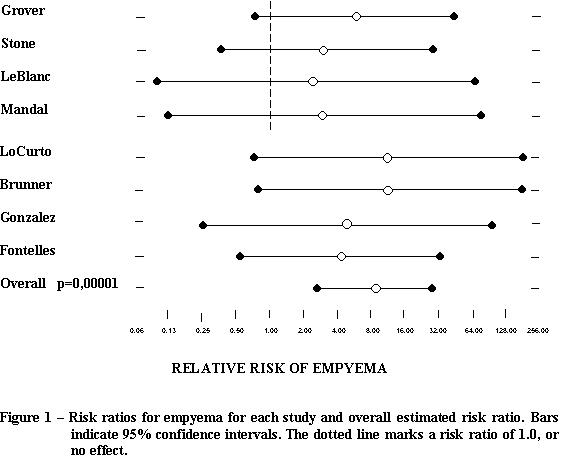
After individually analyzing all the selected studies and, reporting the advantages of antibiotic therapy in preventing complications of pleural empyema, it was observed was that only two (LoCurto01 and Brunner04) out of the eight studies evaluated demonstrated a favorable effect regarding the use of antibiotics for closed chest drainage (Table 1). However, when all the eight studies were considered jointly in relation to pleural empyema, the results showed a favorable statistical significance regarding the use of antibiotic therapy in preventing this complication. The total relative risk in this study was 9.25 (IC 95% 2.85 30.01) and p=0.00001. The overall results showed that those patients who did not undergo antibiotic therapy had nine times more chances of developing postoperative pleural empyema than those who were given antibiotics (Figure 1).
RELATIVE RISK OF EMPYEMA
When considering the use of antibiotics in relation to the occurrence of infectious complications (pneumonia and/or pleural empyema) in the studies analyzed, it was seen that six of the authors who were studied here (Grover12, Stone15, LoCurto01, Brunner04, Gonzalez10 and Fontelles11) showed favorable results regarding the use of antibiotic therapy. In this case the total risk was 4.29 (IC 95% 2.70 8.97) and p < 0.00000001 (Figure 2).
DISCUSSION
One of the first procedures in the area of thoracic surgery was open drainage of the pleural cavity, which was attributed to Hippocrates, the famous Greek physician who conducted pleural empyema drainage using a cautery and a metal tube. On the other hand, the study of thoracic trauma precedes these first historical reports. Three cases with this type of lesion have been described on papyrus and they are attributed to the Egyptian physician Imhotep, who lived between 3000 and 2500 B. C. In all these historical reports, there are references regarding the treatment of patients with thoracic trauma lesions.
At the end of the last century, with the discovery of the infectious nature of many diseases, surgery gained ground in the field of postoperative complications by increasing control through the introduction of new techniques which were performed in aseptic and antiseptic conditions. This significantly reduced the occurrence of postoperative infections. The introduction of antimicrobial drugs in modern medicine resulted in the prophylactic use of these drugs, which radically changed the clinical course of some diseases. However, antibiotics were soon used indiscriminately without any specific criteria or without identifying the cause of the disease or even studying the disease, but used just to prevent infections. This disorderly and aggressive conduct was often practiced in the surgical area. The medical professionals in this area used antibiotics for long periods and often many days before and after the surgery to avoid complications that were not always predictable. Establishing the existence of an infectious process, clinical or surgical, is a fundamental prerequisite for indicating antibiotic therapy. This therapy cannot be used randomly or without guidelines and, the decision to use antibiotics should be related to a good knowledge of the clinical condition and the microbial etiologies commonly related to that type of lesion 16,17.
The main aspect to be resolved is the establishment of criteria to indicate the precise drug to be used for patients with thoracic trauma and who have undergone closed chest drainage. Therefore, over the last few decades, the use of antibiotics in these trauma cases has been a controversial subject among surgeons. These discussions are also due to the fact that the incidence of pleuropulmonary complications resulting from pleural drainage, especially in empyema, are very low about 1% to 16%, and in most of the studies the rates are below 3% 18,19,20. It has been difficult to clarify this aspect through retrospective studies, as these studies indistinctly assess different risk populations without considering how they occur, whether due to sepsis or the trauma itself and if in a precocious or slow manner. On the other hand, randomized prospective studies have not been sufficiently dependable to indicate the use of this conduct, which is probably due to the small casuistic, a faulty interpretation of the results obtained and poor statistical methods used to analyze these studies. The use of meta-analysis in these cases is very efficient, as it not only aggregates the results of selected studies but also individually estimates the effect of each of them and tests the statistical significance of the total result of the studies in association.
Careful selection and posterior association of randomized and prospective studies, as well as the inclusion of studies with patients having lesions restricted to the thoracic segment only, helped in reducing the large variability of the groups studied and as a result eliminated other risk factors such as associated lesions which could compromise the results. On the other hand, studies with both positive and negative results found in literature were included to diminish any possible selection bias 7 .
The table 1 demonstrates that most of the studies analyzed presented results that favored the use of antibiotic therapy in relation to all infectious complications, however, this was not necessarily the case for pleural empyema. Figure 1 compares the risks for pleural empyema, only 4 studies out of 8 studies analyzed demonstrated a tendency to accept the use of antibiotics as beneficial. This was probably due to the resulting large reliability intervals and the small samples used. Nevertheless, when analyzed as a whole, the total risk shown by these studies favored an association of pleural drainage and antibiotic therapy to reduce the incidence of empyema, as those patients who did not receive antibiotic therapy nine times more chances of developing this complication (p=0.00001).
An analysis of figure 2, which lists the relative risk for all infectious complications shows that only two of the eight studies (LeBlanc21 and Mandal22) did not favor the use of antibiotics for preventing complications. In the same way, when the results were studied in conjunction, the inference was that the total relative risk was highly favorable in relation to the use of antibiotic therapy. This result demonstrated that patients who were not given antibiotics had four times the chance of having a postoperative infectious pleuropulmonary complication than the patients who were administered the antibiotics.
Although, the results of the studies that were compared maybe inconclusive or even contrary, individually, meta-analysis proves to be an appropriate method to be used for checking the use of antibiotic therapy in cases of isolated thoracic trauma. However, the risk factors and the indication for associated antibiotic therapy should be studied further with new experimental studies using meta-analysis with a more consistent and objective approach so that more information is obtained regarding the criteria that should regulate the treatment of thoracic trauma.
CONCLUSION
The conclusion reached after comparing the results of this meta-analytical study is that antibiotic therapy has proved to be very effective in reducing the incidence of pleuropulmonary complications in patients with isolated thoracic trauma, who have undergone pleural drainage.
Fontelles MJ, Mantovani M. Incidência de complicações infecciosas pós-drenagem pleural fechada com e sem uso da antibioticoterapia: estudo de meta-análise. Acta Cir Bras [serial online] 2001 Out-Dez;16(4). Disponível em: URL: http://www.scielo.br/acb.
RESUMO:Objetivo - A literatura aponta para a crescente importância das lesões torácicas com sua possíveis complicações e, apesar do uso generalizado da antibioticoterapia, estas continuam a ser um grave problema. Assim, o propósito do presente estudo, foi de desenvolver melhores estimativas da quantidade de benefícios quanto a utilização da antibioticoterapia nos pacientes com trauma isolado do tórax, submetidos, unicamente, à drenagem pleural fechada. Métodos - Através do estudo de meta-análise, oito trabalhos, prospectivos e randomizados, foram selecionados para associação de seus resultados dentro de um modelo de análise estatística quantitativa. Resultados - Os resultados mostraram uma significância estatística favorável ao uso da antibioticoterapia na prevenção do empiema pleural, com risco relativo total de 9,25 (IC 95% 2,85 30,01) para os pacientes sem uso do antibiótico. Se consideradas a ocorrência de todas as complicações infecciosas, verifica-se que o risco total foi igual a 4,29 (IC 95% 2,70 8.97). Conclusão - Com os resultados do presente estudo de meta-análise, pode-se concluir que, o uso da antibioticoterapia se mostra fortemente favorável em reduzir a incidência de complicações infecciosas nos pacientes acometidos por trauma isolado do tórax e, submetidos à drenagem pleural fechada.
DESCRITORES: Meta-análise. Drenagem. Empiema pleural. Traumatismos torácicos .
Conflito de interesses: nenhum
Fontes de financiamento: nenhuma
Address for correspondence:
Dr. Mauro José Fontelles.
Rua Major Solon, 615/62.
Campinas São Paulo
13024-907
Phone: (19) 3294-6850
(19) 3788-7852
Fax: (19) 3788-9446
e-mail: mikefox@uol.com.br
Data do recebimento: 23/03/2001
Data da revisão: 30/04/2001
Data da aprovação: 01/06/2001
- 01 - LoCurto JJ, Tischler CD, Swan KG, Rocko JM, Blackwood JM, Griffin CC, Lazaro EJ, Reiner DS. Tube thoracostomy and trauma: antibiotics or not? J Trauma 1986;26:1067-72.
- 02 - Symbas PN. Chest drainage tubes. Surg Clin North Am 1989;69:41-6.
- 03 - Mattox KL. Indications for thoracotomy: deciding to operate. Surg Clin North Am 1989;69:47-52.
- 04 - Brunner RG, Vinsant GO, Alexander RH, Laneve L, Fallon JR WF. The role of antibiotic therapy in the prevention of empyema in patients with an isolated chest injury (ISS 9 10): a prospective study. J Trauma 1990;30:1148-53.
- 05 - Ashbaugh DG. Empyema thoracis: factor influencing morbidity and mortality. Chest 1991;99:1162-5.
- 06 - Mandal AK, Thadepalli H, Mandal AK, Chettipalli U. Posttraumatic empyema thoracis: a 24 year experience at a major trauma center. J Trauma 1997;5:764-71.
- 07 - Jekel JF, Elmore JG, Katz DL. Epidemiologia, bioestatística e medicina preventiva. Porto Alegre: Artes Médicas Sul; 1999.
- 08 - Gerbarg ZB, Horwitz RI. Resolving conflicting clinical trials: guidelines for meta-analyzis. J Clin Epidemiol 1988;41:503-9.
- 09 - Fallon Jr WF, Wears RL. Prophylatic antibiotics for the prevention of infectious complications including empyema following tube thoracostomy for trauma: result of meta-analysis. J Trauma 1992;33:110-6.
- 10 - Gonzalez RP, Holevar MR. Role of prophylactic antibioctics for tube thoracostomy in chest trauma. Am Surg 1998;64:617-20.
- 11 - Fontelles MJ, Mantovani M. Trauma torácico: fatores de risco de complicaçőes pleuropulmonares pós-drenagem pleural fechada. Rev Col Bras Cir 2000;27:396-403.
- 12 - Grover FL, Richardson JD, Fewel JG, Arom KV, Webb GE, Trinkle JK. Prophylatic antibiotics in the treatment of penetrating chest wounds. J Thorac Cardiovasc Surg 1997;4:52836.
- 13 - Freeman Jr DH. Applied categorical data analysis. New York: Marcel Deker Inc.; 1987.
- 14 - Hosmer DW, Lemeshow S. Applied logistic regression. New York: John Wiley & Sons Inc.; 1989.
- 15 - Stone HH, Symbas PN, Hooper CA. Cefamandole for profilaxis against infection in closed tube thoracostomy. J Trauma 1981;21:9757.
- 16 - Salles JM. Antibióticos: quando indicar como usar. 2ed. Belém: Universitária; 1996.
- 17 - Tavares W. Manual de antibióticos e quimioterápicos antiinfecciosos. 2ed. Săo Paulo: Atheneu; 1996.
- 18 - Eddy AC, Luna GK, Copass M. Empyema thoracis in patients undergoing emergent tube thoracostomy for thoracic trauma. Am J Surg 1989;157:4947.
- 19 - Etoch SW, Bar-Natan MF, Miller FB, Miller FB, Richardson JD. Tube thoracostomy: factors related to complications. Arch Surg 1995;130:5216.
- 20 - Botter M, Saad Jr R, Giannini JA, Neto VD. Drenagem pleural no trauma torácico. J Pneumol 1996;22:5964.
- 21 - LeBlanck KA, Tucker WY. Prophylatic antibiotic and closed tube thoracostomy. Surg Gynecol Obstet 1985;160:25963.
- 22 - Mandal AK, Montano J, Thadepalli H. Prophylactic antibiotics and no antibiotics compared in penetrating chest trauma. J Trauma 1985;25:63943.
Publication Dates
-
Publication in this collection
11 Sept 2003 -
Date of issue
Dec 2001
History
-
Received
23 Mar 2001 -
Reviewed
30 Apr 2001 -
Accepted
01 June 2001