Abstracts
PURPOSE: To compare morphologically three different types of tracheotomy in growing rats, applying microsurgical technique. METHODS: EPM-1 Wistar growing rats (n=57) weighing 88gm and aged 35 days were randomized in four groups, according tracheotomy incision type (longitudinal, transverse and tracheal segment excision), and sham group. Following intramuscular anesthesia with ketamine and xylazine, the trachea was exposed and incised, according to the group, and a hand-made endotracheal cannula was inserted into the organ, under sterile conditions. This cannula was removed after 7 days, and animals have been sacrificed 30 days later. Tracheas samples were submitted to histological study, stained by hematoxylin-eosin and Masson trichrome, evaluating fibrosis, inflammatory infiltrate and epidermoid metaplasia. RESULTS: There was more frequency of inflammatory infiltrate at the tracheal epithelium in the tracheal segment excision group (87%) compared to the longitudinal (40%) and transverse (36%) incision groups (p=0.009). Evaluating epidermoid metaplasia, tracheal segment excision and the longitudinal groups presented 33% and 40%, respectively, compared to 0% of the transverse group (p=0.03). Concerning to fibrosis, in a global comparison (p=0.1) among the three groups there was no difference, however, compared to the longitudinal group the transverse group showed lower level of fibrosis (p=0.04). Sham group did not present any relevant morphologic alterations and it was used as reference pattern. CONCLUSION: Taken together, our data show that tracheal segment excision promotes more epithelium aggression and transverse tracheal incision shows less morphologic alterations.
Tracheotomy; Models, animal; Rats,Wistar; Growing
OBJETIVO: Comparar os aspectos histológicos da cicatrização traqueal após diferentes tipos de traqueotomia nos ratos em crescimento, usando técnica microcirúrgica. MÉTODOS: Ratos EPM-1 Wistar (n=57), em crescimento, com peso médio de 88g e idade de 35 dias foram distribuídos randomicamente em quatro grupos de acordo com o tipo de incisão traqueal (longitudinal, transversa e com retirada de fragmento de anel cartilaginoso) e grupo simulado. Sob anestesia intramuscular (cetamina/xilazina), usando técnica asséptica, a traquéia era exposta e aberta, de acordo com o grupo, sendo introduzida uma cânula confeccionada em silicone. Esta cânula foi removida no 7º dia e após 30 dias os animais foram submetidos à eutanásia. As traquéias retiradas foram submetidas a estudo histológico, nas colorações H-E e tricrômico de Masson, avaliando-se fibrose, infiltrado inflamatório no epitélio traqueal e metaplasia epidermóide. RESULTADOS: Houve mais infiltrado inflamatório ao epitélio traqueal no grupo em que se retirou um segmento traqueal um (87%) comparado aos das incisões longitudinal (40%) e transversa (36%)(p=0,009). Avaliando a metaplasia epidermóide, os grupos com excisão de segmento traqueal e da incisão longitudinal apresentaram 33% e 40%, respectivamente, comparado a 0% do grupo com incisão transversa (p=0,03). No que se refere à fibrose, numa comparação entre os três tipos de incisão não houve diferença significante (p=0,1), entretanto, ao se comparar ao grupo de incisão longitudinal, o grupo da incisão transversa mostrou menor nível de fibrose (p=0,04). O grupo simulado não apresentou qualquer alteração histológica e foi utilizado como padrão de referência. CONCLUSÃO: Nossos dados mostraram que a incisão com excisão de segmento traqueal promove maior agressão epitelial e a incisão transversa apresenta menor grau de alterações histológicas.
Traqueotomia; Modelos animais; Ratos Wistar; Crescimento
ORIGINAL ARTICLE
Tracheotomy in growing rats. Histological aspects1 Correspondence to Mônica Cecília Bochetti Manna Rua José Antônio Coelho, 603/32B 04011-061 São Paulo SP E-mail: manna@uol.com.br
Traqueostomia no rato em crescimento: aspectos histológicos
Mônica Cecília Bochetti MannaI; Edna Frasson de Souza MonteroII; Maria Antonieta Longo Galvão da SilvaIII; Yara JulianoIV
IMaster in Medicine - Operative Technique and Experimental Surgery - UNIFESP EPM. Brazil
IIAfiliated Professor, MD, PhD - Operative Technique and Experimental Surgery Division Department of Surgery - UNIFESP EPM. Brazil
IIIAssistant Professor, MD, PhD - Department of Pathology, Medical Sciences Faculty of Santa Casa. São Paulo - Brazil
IVProfessor, MD, PhD - Department of Epidemiology - UNIFESP EPM. Brazil
Correspondence Correspondence to Mônica Cecília Bochetti Manna Rua José Antônio Coelho, 603/32B 04011-061 São Paulo SP E-mail: manna@uol.com.br
ABSTRACT
PURPOSE: To compare morphologically three different types of tracheotomy in growing rats, applying microsurgical technique.
METHODS: EPM-1 Wistar growing rats (n=57) weighing 88gm and aged 35 days were randomized in four groups, according tracheotomy incision type (longitudinal, transverse and tracheal segment excision), and sham group. Following intramuscular anesthesia with ketamine and xylazine, the trachea was exposed and incised, according to the group, and a hand-made endotracheal cannula was inserted into the organ, under sterile conditions. This cannula was removed after 7 days, and animals have been sacrificed 30 days later. Tracheas samples were submitted to histological study, stained by hematoxylin-eosin and Masson trichrome, evaluating fibrosis, inflammatory infiltrate and epidermoid metaplasia.
RESULTS: There was more frequency of inflammatory infiltrate at the tracheal epithelium in the tracheal segment excision group (87%) compared to the longitudinal (40%) and transverse (36%) incision groups (p=0.009). Evaluating epidermoid metaplasia, tracheal segment excision and the longitudinal groups presented 33% and 40%, respectively, compared to 0% of the transverse group (p=0.03). Concerning to fibrosis, in a global comparison (p=0.1) among the three groups there was no difference, however, compared to the longitudinal group the transverse group showed lower level of fibrosis (p=0.04). Sham group did not present any relevant morphologic alterations and it was used as reference pattern.
CONCLUSION: Taken together, our data show that tracheal segment excision promotes more epithelium aggression and transverse tracheal incision shows less morphologic alterations.
key words:Tracheotomy. Models, animal. Rats,Wistar. Growing.
RESUMO
OBJETIVO: Comparar os aspectos histológicos da cicatrização traqueal após diferentes tipos de traqueotomia nos ratos em crescimento, usando técnica microcirúrgica.
MÉTODOS: Ratos EPM-1 Wistar (n=57), em crescimento, com peso médio de 88g e idade de 35 dias foram distribuídos randomicamente em quatro grupos de acordo com o tipo de incisão traqueal (longitudinal, transversa e com retirada de fragmento de anel cartilaginoso) e grupo simulado. Sob anestesia intramuscular (cetamina/xilazina), usando técnica asséptica, a traquéia era exposta e aberta, de acordo com o grupo, sendo introduzida uma cânula confeccionada em silicone. Esta cânula foi removida no 7o dia e após 30 dias os animais foram submetidos à eutanásia. As traquéias retiradas foram submetidas a estudo histológico, nas colorações H-E e tricrômico de Masson, avaliando-se fibrose, infiltrado inflamatório no epitélio traqueal e metaplasia epidermóide.
RESULTADOS: Houve mais infiltrado inflamatório ao epitélio traqueal no grupo em que se retirou um segmento traqueal um (87%) comparado aos das incisões longitudinal (40%) e transversa (36%)(p=0,009). Avaliando a metaplasia epidermóide, os grupos com excisão de segmento traqueal e da incisão longitudinal apresentaram 33% e 40%, respectivamente, comparado a 0% do grupo com incisão transversa (p=0,03). No que se refere à fibrose, numa comparação entre os três tipos de incisão não houve diferença significante (p=0,1), entretanto, ao se comparar ao grupo de incisão longitudinal, o grupo da incisão transversa mostrou menor nível de fibrose (p=0,04). O grupo simulado não apresentou qualquer alteração histológica e foi utilizado como padrão de referência.
CONCLUSÃO: Nossos dados mostraram que a incisão com excisão de segmento traqueal promove maior agressão epitelial e a incisão transversa apresenta menor grau de alterações histológicas.
Descritotores:Traqueotomia. Modelos animais. Ratos Wistar. Crescimento.
Introduction
Complications related to pediatric tracheotomies constitute an important clinical problem, and it is controversial the role exert by tracheotomy incision type (1-7). Studies showing that this operation is safe and effective, with minimum morbidity. However, this is still a controversial subject, mainly the type of tracheal incision and which one is the best type(7).
In a review about tracheotomy techniques, Hotaling et al.(8)showed that the inferior-based tracheal flap was the best incision because it created a secure stoma, minimizing postoperative complications.
The traditional approach, which uses a midline vertical incision in the anterior tracheal wall, is associated with relatively high rates of complications when it is used on a long-term basis. Alternative approaches, such as removing tracheal window or creating tracheal flaps, have been avoided in the pediatric patient because of the risk of tracheal stenosis and the potential for the subsequent effect on tracheal growth. Rhee et al.(9) in a study in children showing that was safe, useful, and advantageous used the superiorly based flap tracheotomy.
There are few researches concerning to pediatric experimental models, using dogs, ferrets and rabbits(10-12), despite several experimental studies about tracheotomy complications(14-22). Evaluating tracheal growth in tracheotomized dogs, aged eight to ten weeks old, Mendez-Picon et al.(10) showed that both longitudinal and transverse incisions could be performed with minimal postoperative distortion and no functional consequence in immature growing animals. However, the experiment suggested that a transverse intercartilaginous incision heals with less scarring and deformity than the longitudinal one. It suggested that since both can be made equally easily, the incision of choice is clearly the transverse one. Fry et al.(11) have studied tracheotomy incisions in ferrets aged eight to nine weeks old, and they concluded that the longitudinal tracheal incision was the incision of choice in infantile trachea, with less incidence of stenosis. Emphasizing post-tracheotomy tracheal stenosis in rabbits aged ten weeks old, using a vertical and a superiorly-based flap, Miller et al.(12). concluded that despite the potential adverse effects on the trachea, the superiorly flap tracheotomy did not seem to impair normal tracheal growth and development and the procedure seemed to be well tolerated in children that needed long-term control of the upper airways.
Previously, we described a microsurgical tracheotomy pediatric model in growing rats(13), and this paper aims to evaluate morphologically three types of incision and its healing repercussions, 30 days after cannula removal.
Methods
This work was approved by the Ethics Committee on Animal Research.of HSP/UNIFESP-EPM and it was done at the Laboratory of Microsurgery of the Operative Technique and Experimental Surgery Division, UNIFESP-EPM.
Fifty-seven EPM-1 Wistar female rats aged 35 days and weighing 88gm were obtained for this experiment from CEDEME, UNIFESP-EPM and the animals were randomized into four groups, according to the tracheotomy incision type as follow:
Longitudinal Group: (n=15) midline longitudinal incision including second and third tracheal rings; Transverse Group: (n=14) transverse intercartilaginous incision between the second and the third tracheal rings; Window Group: (n=15)segment excision of the third tracheal ring (window incision); Sham Group: (n=13) dissection and exposition of the trachea without incision.
All the operative procedures were performed with sterile technique under intramuscular anesthesia with ketamine(60mg.kg-1) associate to xylazine (10mg.kg-1). Next, they were immobilized in supine position on the surgical table. After the hair had been clipped from the anterior neck, the skin was prepared with povidone-iodine solution, midline longitudinal cervical skin incision was made, and the cervical trachea was exposed by separation of the muscles.
The tracheal incision chosen for the study was made on the anterior tracheal wall, depending on the group, using microsurgical instruments and D.F. Vasconcellos microscopy, with 10x and 16x magnification. The cannula was assembled by using a 1.5cm long segment of 3Fr silicone catheter passed through an hexagonal-shaped silicone screen, as described elsewhere(13). The skin was sutured, exteriorizing approximately 5mm of the tip of the tracheal cannula, and the animals were kept in individual cages for observation, warmed under incandescent light source, from early after surgery to anesthetic recovery. Following, they were taken to the sector of animal laboratory and provided water and food ad libitum.
The tracheotomy cannula was removed on the 7th postoperative day, after the animals had been anesthetized and weighed, and we made a new longitudinal incision in the anterior cervicall wall, exposing the subcutaneous screen by cutting the stitch that had fixated the cannula and removing it. On the 30th day after removal cannula, all animals had been weighed, anesthetized and sacrificed. Then, trachea was carefully removed, since the larynx to bronchial bifurcation.
The tracheas were fixed in formalin solution 10% and submitted to histological study, staining by hematoxylin-eosin and Masson trichrome. It was analyzed inflammatory infiltrate, epithelium and corium thickness (fibrosis), utilizing 40X and 400X magnifications. For the fibrosis evaluation, it was used a 20 millimeter ruler superposed to the lamina and observed with 40X magnification and the measurement was done since the basal membrane of the epithelium to the cartilage. The tracheal epithelium aggressions by the inflamatory infiltrate as well as the epidermoid metaplasia were evaluated with 40 and 400X magnifications.
Data were submitted to statistical studies by Kruskal-Wallis variance analysis to compare groups submitted to different types of tracheal incision and Mann-Whitney to compare the groups in pairs, concerning to the fibrosis measurement. Chi-square test for the contingency tables, in order to compare these groups concerning to the presence or absence of epithelium aggression and epidermoid metaplasia. We determined the null hypothesis rejection level as 0.05 or 5%, and marked with an asterisk the significant values.
Results
There was more frequency (p=0.009) of inflammatory infiltrate at the tracheal epithelium in the window group (87%) compared to the longitudinal (40%) and transverse (36%) incision groups (Figure 1). At the sham group, it was observed some mononuclear cells but without aggression of the epithelium (Figure 2A), and as did not present any relevant morphologic alterations it was used like reference pattern. That inflammatory infiltrate occurred at the anterior tracheal wall, where it was performed the tracheal incision (Figure 2B).
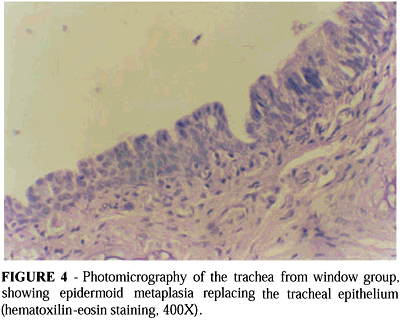
Evaluating epidermoid metaplasia, tracheal segment excision and longitudinal groups presented 33% and 40%, respectively, compared to 0% of the transverse group (p=0.03) (Figure 3). It was observed that in some cases from window and longitudinal groups occurred partial replacement of the ciliate cylindrical stratified epithelium by metaplasic pavement stratified epithelium, focally in the site of the previous tracheal incision (Figure 4). It was not found it in the transverse group, but it occurred similarly in both longitudinal and window groups.
Concerning to fibrosis (corium thickness), in a global comparison among the three groups there was no difference (p=0.1). However, compared to the longitudinal group, the transverse group showed lower level of fibrosis (p=0.04), despite the comparison of these groups to the window group did not show difference (LongxWind - p=0.29 and TransxWind - p=0.28) (Table 1).
Discussion
Tracheotomy in children is not a difficult procedure to be performed, but it is controversial according to the choice of incision adopted and its correlations with the surgical complications.
Since it is still a controversial topic, owing to the related morbidity and mortality rates, the types of tracheal incision have been studied in some animal models (14-22). However, among the experimental studies about tracheotomy incisions, little has been done using growing animals (10-12), in an attempt to translate a pediatric model. Thus, we used growing rats to investigate the heal consequences post-tracheotomy as a pediatric experimental model, since they are small, easy to handle and accessible. The cost of the animals is affordable, besides they are frequently studied and their healing process is well known. In addition, the biological time of rats, as equivalent to humans, would be of 1day/30 days, which results in a very appropriate animal for long-term studies (23). In order to prevent respiratory epithelium abnormalities in the rat using inhalation anesthetic, we decided to use injecting drugs, which enable 2 to 4-hour anesthetic plans (24).
At the sham group, there was not a tracheal incision to promote alterations in the revetment epithelium. However, the respiratory epithelium of the rat presents sub epithelial lymphoid follicles, which explains the inflammatory infiltrate observed at this group (25). In some cases, it was observed the inflammatory infiltrate provoking aggression to the tracheal epithelium mainly at the window group. In the longitudinal and transverse groups also occurred aggression to the epithelium, but less frequently. These findings suggest that resection of a cartilage segment led to a more intense inflammatory reaction at the tracheal anterior wall. In the literature, there was not found any research studying this morphologic alteration.
Concerning to epidermoid metaplasia, it could be noticed that occurred the replacement of the tracheal epithelium by metaplasic pavement stratified localized in the site of the incision. The transverse group did not show this replacement, but it occurred in both longitudinal and window groups, similarly. Probably, because in the transverse group it was done only intercartilaginous membrane incision, without injuring the tracheal cartilage, suggesting the superiority of this incision. It was not observed in the literature any study concerning to this kind of epithelium tracheal alteration.
The effect of tracheotomy incisions on tracheal growth was studied in dogs aged 8 to 10 weeks old by Mendez-Picon et al. (10) The experiment was designed to compare two incisions: longitudinal and transverse between two rings on tracheal growth and development in the immature growing animal, maintaining the cannula for five days and sacrificing the animals six months later. In a group with transverse incision, a gross examination of the trachea at the level of the tracheotomy demonstrated a normal configuration without visible scare externally and a smooth epithelial surface internally. The tracheas in the longitudinal incision group were, on a gross inspection, deformed and narrowed in the transverse plane at the level of the tracheotomy incision with external scarring but smooth epithelial surface. Microscopically they referred that the respiratory epithelium was normal. They suggested that a transverse intercartilaginous healed with less scarring and deformity than longitudinal one.
Also comparing tracheotomy incisions in a pediatric model, Fry at al. (11) developed a study in ferrets, comparing three types of incisions: inferiorly based trapdoor, horizontal H and longitudinal. Recommendations for pediatric tracheal incisions are made on the basis of this study since they concluded that the longitudinal was the best incision after endoscopic, radiographic and airflow evaluation as well as cross-section tracheal areas analyzed by computerized program. Tracheal cannulation was kept for eight days and the sacrifice was done seven days later. This study can not be compared to our results, because they evaluated different parameters.
To investigate the short and long-term complications of pediatric tracheotomy, emphasizing post-tracheotomy tracheal stenosis in an animal model, Miller et al. (12) developed a research in rabbits aged 10 weeks old. They compared two incisions: a longitudinal, considered the traditional, and a superiorly based flap tracheotomy. They found no significant risk of tracheal stenosis or adverse effects on tracheal growth for the flap tracheotomy in a developing animal model. They concluded that this tracheotomy technique might be useful in the management of pediatric patients who require long-term bypass of the upper airway.
In our data we can assert which was the best tracheotomy incision, but the transverse incision did not cause epidermoid metaplasia in any animal studied, as well as showed few aggression to the epithelium by inflammatory infiltrate. We can say that the incision where we removed a tracheal fragment, the aggression to the epithelium was present in almost the majority of the animals.
Conclusion
Tracheal segment excision promotes more epithelium aggression and transverse tracheal incision shows less morphologic alterations.
Data do recebimento: 18/02/2003
Data da revisão: 01/03/2003
Data da aprovação: 12/03/2003
Conflict of interest: none
Financial source: CNPq
1. Operative Technique and Experimental Surgery Division Department of Surgery Federal University of de São Paulo - Paulista School of Medicine (UNIFESP EPM). Brazil.
- 1. Wetmore RF, Handler SD, Potsic WP. Pediatric tracheostomy: experience during the past decade. Ann Otol Rhinol Laryngol 1982; 91:628-32.
- 2. Kenna MA, Reilly JS, Stool SE. Tracheostomy in the preterm infant. Ann Otol Rhinol Laryngol 1987; 96:68-71.
- 3. Gianoli GJ, Miller RH, Guarisco JL. Tracheotomy in the first year of life. Ann Otol Rhinol Laryngol 1990; 99:896-901.
- 4.Ward RF. Current trends in pediatric tracheotomy. Pediatr Pulmonol 1997; 16:290-1.
- 5. Dubey SP, Garap JP. Paediatric tracheostomy: an analysis of 40 cases. J Laryngol Otol 1999; 113:645-51.
- 6. Carron JD, Derkay CS, Strope GL, Nosonchuk JE, Darrow DH. Tracheostomies: changing indications and outcomes. Laryngoscope 2000; 110:1099-104.
- 7. Carter P, Benjamin BV. Ten-year review of pediatric tracheotomy. Ann Otol Rhinol Laryngol 1983; 92:398-400.
- 8. Hotaling AJ, Robbins WK, Madgy DN, Belenky WM. Pediatric tracheotomy: a review of technique. Am J Otolaryngol 1992; 13(2):115-9.
- 9. Rhee CK, Miller FR, Tucker HM, Eliachar I. The superiorly based flap long-term tracheostomy in pediatric patients. Am J Otol 1996; 17(4):251-6.
- 10. Mendez-Picon G, Elvilich FE, Salzberg AM. The effect of tracheostomy incisions on tracheal growth. J Pediatr Surg 1976; 11(5):681-5.
- 11. Fry TL, Jones RO, Fischer ND, Pillsbury HC. Comparisons of tracheostomy incisions in a pediatric model. Ann Otol Rhinol Laryngol 1985; 94:450-3.
- 12. Miller FR, Guay ME, Bauer T, Tucker HM. Long-term flap tracheostomy in a pediatric animal model. Arch Otol Head Neck Surg 1995; 121:743-8.
- 13. Manna MCB, Montero EFS, Leão JQS, Novo NF. Microsurgical tracheotomy: a pediatric model in growing rats. Microsurgery, in press.
- 14. Nelson TG. Tracheostomy: a clinical and experimental study. Part I Am Surg 1957a; 23:669-94.
- 15. Nelson TG. Tracheostomy: a clinical and experimental study. Part II. Am Surg 1957b; 23:750-84.
- 16. Nelson TG. Tracheostomy: a clinical and experimental study. Part III. Am Surg 1957c; 23:841-90.
- 17. Bardin J, Boyd AD, Hirose H, Engelman RM. Tracheal healing following tracheostomy. Surg Forum 1974; 25:210-3.
- 18. Lulenski GC, Batsakis JG. Tracheal incisions as a contributing factor to tracheal stenosis. Ann Otol Rhinol Laryngol 1975; 84:871-6.
- 19. Bryant LR, Mujia D, Greenberg S, Huey JM, Schechter FG, Albert HM. Evaluation pf tracheal incisions for tracheostomy. Am J Surg 1978; 135:675-9.
- 20. Eliachar I, Goldsher M, Joachims HZ, Mordechovich D, Shohat S. Superiorly based tracheostomal flap to counteract tracheal stenosis: experimental study. Laryngosope 1981; 91:976-81.
- 21. Smith MM, Saunders GK, Leib MS, Simmons EJ. Evaluation of horizontal and vertical tracheotomy healing after short-duration tracheostomy in dogs. J Oral Maxillofac Surg 1995; 53:289-94.
- 22. Silva GS. Comparação entre os três tipos de incisões para traqueostomia: estudo experimental em coelhos [Tese - Mestrado] Universidade Federal de São Paulo - Escola Paulista de Medicina; 1995.
- 23. Donaldson HH. The rat: data and references tables for the Albino rat (mus norvegius albinus) and the Norway rat (mus norvegius). 2ed. Philadelphia; 1924. p 1-33.
- 24. Wixson SF, White WJ, Hughes HC, Labg CM, Marshall WK. A comparison of Pentobarbital, Fentanyl-Droperidol, Ketamine-Xylazine and Ketamine-Diazepam anesthesia in adult rats. Lab Anim Sci 1987; 37(6):726:30.
- 25. Hebel R, Stromberg MW. Respiratory system: anatomy of the laboratory rat. 1ed. Baltimore: The Williams&Wilkins Company; 1976. p 55-61.
- 26. Wyatt ME, Barley B, Whiteside JC. Update on pediatric tracheostomy tubes. J Laryngol Otol 1999; 113:35-40.
Publication Dates
-
Publication in this collection
08 Oct 2003 -
Date of issue
June 2003
History
-
Accepted
12 Mar 2003 -
Reviewed
01 Mar 2003 -
Received
18 Feb 2003