Abstracts
PURPOSE: The brachial plexus has a complex anatomical structure since its origin in the neck throughout its course in the axillary region. It also has close relationship to important anatomic structures what makes it an easy target of a sort of variations and provides its clinical and surgical importance. The aims of the present study were to describe the brachial plexus anatomical variations in origin and respective branches, and to correlate these variations with sex, color of the subjects and side of the body. METHODS: Twenty-seven adult cadavers separated into sex and color had their brachial plexuses evaluated on the right and left sides. RESULTS: Our results are extensive and describe a large number of variations, including some that have not been reported in the literature. Our results showed that the phrenic nerve had a complete origin from the plexus in 20% of the cases. In this way, a lesion of the brachial plexus roots could result in diaphragm palsy. It is not usual that the long thoracic nerve pierces the scalenus medius muscle but it occurred in 63% of our cases. Another observation was that the posterior cord was formed by the posterior divisions of the superior and middle trunks in 9%. In these cases, the axillary and the radial nerves may not receive fibers from C7 and C8, as usually described. CONCLUSION: Finally, the plexuses studied did not show that sex, color or side of the body had much if any influence upon the presence of variations.
Anatomy; Axilla; Brachial plexus.; Anatomical variations; Peripheral nerves
OBJETIVOS: O plexo braquial apresenta uma estrutura anatômica complexa, desde sua origem, no pescoço, até sua ramificação terminal, na região axilar. Ele também apresenta relações importantes com outras estruturas anatômicas locais, o que o torna vulnerável ao aparecimento de uma série de variações anatômicas, marcando sua importância clínica e cirúrgica. Os objetivos desse estudo foram de descrever as variações anatômicas do plexo braquial, desde sua origem até seus ramos terminais e correlacionar essas variações com o sexo e a cor dos indivíduos, bem como com o lado do corpo estudado. MÉTODOS: Vinte e sete cadáveres adultos, separados em sexo e cor, tiveram seus plexos braquiais avaliados à direita e à esquerda. RESULTADOS: Nossos resultados são extensos e descrevem um grande número de variações, incluindo algumas ainda não descritas na literatura. Nossos resultados mostram que o nervo frênico apresentou sua origem diretamente no plexo braquial em 20% dos casos. Assim, uma lesão das raízes do plexo braquial poderia resultar em uma inexplicada paralisia diafragmática. Não é esperado que o nervo torácico longo passe através do músculo escaleno médio entretanto, esse fato foi observado em 63% de nossos casos. Outra observaçõa foi a formação do fascículo posterior pelas divisões posteriores dos troncos superior e médio em 9% dos casos. Nesses casos, os nervos axilar e radial poderão não receber fibras de C7 e C8, como normalmente descrito na literatura. CONCLUSÃO: Os plexos braquiais estudados não mostraram que o sexo, a cor ou o lado do corpo influenciam de maneira importante na presença de variações anatômicas dessa estrutura.
Anatomia; Axila; Plexo braquial; Variações anatômicas; Nervos periféricos
ARTIGO ORIGINAL
Brachial plexus variations in its formation and main branches
Valéria Paula Sassoli FazanI; André de Souza AmadeuII; Adilson L. CaleffiII; Omar Andrade Rodrigues FilhoIII
IAssistant Professor, Departament of Surgery and Anatomy, School of Medicine of Ribeirão Preto, University of São Paulo, Ribeirão Preto, São Paulo, Brazil
IIMedical Student, School of Medicine of Triângulo Mineiro, Uberaba, Minas Gerais; Brazil
IIIGraduate Student and Instructor in Anatomy, School of Medicine of Triângulo Mineiro, Uberaba, Minas Gerais; Brazil
Correspondence Correspondence to Valéria Paula Sassoli Fazan, M.D.; Ph.D. Department of Surgery and Anatomy School of Medicine of Ribeirão Preto University of São Paulo Av. Bandeirantes 3900, Ribeirão Preto SP 14049-900 Brazil Phone: + 55 16 602-2407 FAX: + 55 16 633-0017 e-mail: vpsfazan@fmrp.usp.br
ABSTRACT
PURPOSE: The brachial plexus has a complex anatomical structure since its origin in the neck throughout its course in the axillary region. It also has close relationship to important anatomic structures what makes it an easy target of a sort of variations and provides its clinical and surgical importance. The aims of the present study were to describe the brachial plexus anatomical variations in origin and respective branches, and to correlate these variations with sex, color of the subjects and side of the body.
METHODS: Twenty-seven adult cadavers separated into sex and color had their brachial plexuses evaluated on the right and left sides.
RESULTS: Our results are extensive and describe a large number of variations, including some that have not been reported in the literature. Our results showed that the phrenic nerve had a complete origin from the plexus in 20% of the cases. In this way, a lesion of the brachial plexus roots could result in diaphragm palsy. It is not usual that the long thoracic nerve pierces the scalenus medius muscle but it occurred in 63% of our cases. Another observation was that the posterior cord was formed by the posterior divisions of the superior and middle trunks in 9%. In these cases, the axillary and the radial nerves may not receive fibers from C7 and C8, as usually described.
CONCLUSION: Finally, the plexuses studied did not show that sex, color or side of the body had much if any influence upon the presence of variations.
Key Words: Anatomy. Axilla. Brachial plexus. Anatomical variations. Peripheral nerves.
RESUMO
OBJETIVOS: O plexo braquial apresenta uma estrutura anatômica complexa, desde sua origem, no pescoço, até sua ramificação terminal, na região axilar. Ele também apresenta relações importantes com outras estruturas anatômicas locais, o que o torna vulnerável ao aparecimento de uma série de variações anatômicas, marcando sua importância clínica e cirúrgica. Os objetivos desse estudo foram de descrever as variações anatômicas do plexo braquial, desde sua origem até seus ramos terminais e correlacionar essas variações com o sexo e a cor dos indivíduos, bem como com o lado do corpo estudado.
MÉTODOS: Vinte e sete cadáveres adultos, separados em sexo e cor, tiveram seus plexos braquiais avaliados à direita e à esquerda.
RESULTADOS: Nossos resultados são extensos e descrevem um grande número de variações, incluindo algumas ainda não descritas na literatura. Nossos resultados mostram que o nervo frênico apresentou sua origem diretamente no plexo braquial em 20% dos casos. Assim, uma lesão das raízes do plexo braquial poderia resultar em uma inexplicada paralisia diafragmática. Não é esperado que o nervo torácico longo passe através do músculo escaleno médio entretanto, esse fato foi observado em 63% de nossos casos. Outra observaçõa foi a formação do fascículo posterior pelas divisões posteriores dos troncos superior e médio em 9% dos casos. Nesses casos, os nervos axilar e radial poderão não receber fibras de C7 e C8, como normalmente descrito na literatura.
CONCLUSÃO: Os plexos braquiais estudados não mostraram que o sexo, a cor ou o lado do corpo influenciam de maneira importante na presença de variações anatômicas dessa estrutura.
Descritores: Anatomia. Axila. Plexo braquial. Variações anatômicas. Nervos periféricos.
INTRODUCTION
The nerve supply of the upper limb arises from the eleventh cranial nerve, the cervical plexus and through the brachial plexus. At the brachial plexus, nerve fibers are routed from different levels of the spinal cord to enter one of the terminal nerves that supply the upper limb. It must be remembered that the brachial plexus is merely a routing mechanism to get nerves with a common function into the proper terminal nerves and thus errors in distribution may occur that are corrected distally in the arm, forearm or hand, resulting in anatomical variations of the plexus1. Some variations are vulnerable to damage in radical neck dissection and other surgical operations of the axilla and upper arm2. Also, a very close course of an unusual brachial plexus branch with the axillary artery may lessen the blood supply of the upper extremity by compressing the vessel3. Moreover, it seems that certain surgical treatment failures of brachial plexus lesions are related to the presence of anatomical variations. Due to the surgical importance of the brachial plexus, the aims of the present study were to describe its anatomical variations in origin and respective branches, and to correlate these variations with sex, color of the subjects and side of the body.
METHODS
A total of 27 embalmed human cadavers of both sexes (21 males and 6 females) and two distinct colors (12 white and 15 black), in a total of 54 upper extremities were studied (27 from each side). The age of death ranged from 37 to 76 years and all specimens were fixed in 10% formaldehyde solution. The upper limbs have been partially dissected by the School of Medicine of Triângulo Mineiro medical students during the previous years and, the authors did further dissections under magnification, with the aid of a D.F. Vasconcellos M-90 surgical microscope. A classic brachial plexus was defined when the superior trunk was formed by the union of C5 and C6 roots, the middle trunk was the continuation of C7 root and the inferior trunk was formed by the union of C8 and T1 roots4,5. The terminal branches of the brachial plexus were considered as being the axillary, radial, ulnar, median and musculocutaneous nerves. From the supraclavicular part, the origins of the dorsal scapular, long thoracic, suprascapular, subescapular, thoracodorsal, medial pectoral and lateral pectoral nerves were studied. Also, the origins of the phrenic and accessory phrenic nerves were evaluated. From the infraclavicular part, the origins of the medial brachial cutaneous and the medial antebrachial cutaneous nerves were studied. Variations of the trunks, divisions and cords were also explored, as well as the origin of the terminal branches. The obtained results are of a descriptive order and data are presented as absolute numbers and percentage of the total.
RESULTS
From the 54 upper extremities evaluated, 39 (72%) showed normal origin of the brachial plexus. Thirteen plexuses (24%) were prefixed in origin, 2 from male and 11 from female, being 5 in white and 8 in black cadavers (54% on the right and 46% on the left side). Only 3 plexuses were postfixed in origin, being all from male white cadavers, 2 on the right and 1 on the left side. Eleven phrenic nerves (20%) originated entirely from the brachial plexus in 9 male and 2 female, being 6 white and 5 black cadavers (73% on the right and 27% on the left sides). An accessory phrenic nerve was present on 12 plexuses, 50% on each side, in 9 male and 3 female, being 5 in white and 7 in black cadavers. When the nerves arising from the roots of the brachial plexus were evaluated (54 in total), only 45 plexuses presented the dorsal scapular branch, 12 (27%) of which were completely out of the middle scalene muscle during their course (Figure 1).
Thirty-three (73%) dorsal scapular nerves had an intramuscular course in 26 male and 7 female, being 15 in white and 18 in black cadavers. The long thoracic nerve was formed by C5 and C6 in 33% (17 plexuses), by C5, C6 and C7 in 46% (24 plexuses) and by C6 and C7 in 15% (8 plexuses) of the cases. No female cadavers presented a long thoracic nerve formed as the last description. The long thoracic nerve pierced the middle scalene muscle in 63% of the cases.
Variation on the superior trunk was present in 2 plexuses, both on the right side. In both cases, C5 and C6 roots were split in anterior and posterior division (Figure 1). Both anterior divisions joined to give origin to an "anterior superior trunk" and both posterior divisions joined to give origin to a "posterior superior trunk". These trunks joined to give origin to the superior trunk.
The middle trunk received a communicating branch from C8 on the left side in one male white cadaver and a communicating branch from the inferior trunk on the right side in one male black cadaver. The inferior trunk was not variable in our cases.
The posterior cord was formed by the posterior divisions of the superior and middle trunks on 5 plexuses (9%), all from male black cadavers (Figure 2). The lateral and medial cords were not variable in our cases.
Table 1 shows the variations in origin of the lateral pectoral, medial pectoral, suprascapular and thoracodorsal nerves. Table 2 shows the variations in origin of the upper subscapular, lower subscapular, medial brachial cutaneous and medial antebrachial cutaneous nerves. Also, a medial cutaneous trunk, which gave origin to the medial antebrachial cutaneous and medial brachial cutaneous nerves, was present in 36 plexuses (67%), 29 in male and 19 in black cadavers. From these, 2 medial cutaneous trunks, both on the right side from male black cadavers, originated from the inferior trunk of the brachial plexus.
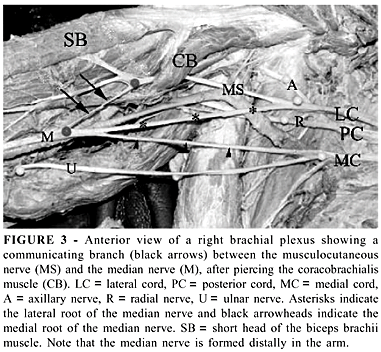
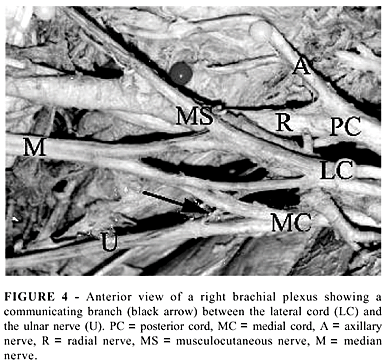
From the terminal branches of the brachial plexus, the axillary and the musculocutaneous nerves were not variable in origin. In 4 male cadavers (2 white and 2 black, 1 one the right and 3 on the left side), the musculocutaneous nerve, after piercing the coracobrachialis muscle, gave off a communicating branch to the median nerve, which was normal in its origin (Figure 3). The radial nerve received a communicating branch from the inferior trunk in 4 cases (7%), all in male black cadavers, 3 on the right and 1 on the left side. The ulnar nerve received a communicating branch from the lateral cord in 16 cases (30%), being 12 male and 4 female cadavers (Figure 4). The median nerve was formed by 2 lateral roots and 1 medial root (from the medial cord) in 28 (52%) cases, being 25 from male and 3 from female, 9 from white and 19 from black cadavers. In 4 cases, one of the two lateral roots came from the anterior division of the middle trunk and 1 from the lateral cord. On the other 24 cases, the two lateral roots came from the lateral cord of the plexus. Four (7%) median nerves were formed distally, in the arm (Figure 3).
DISCUSSION
Knowledge of variations in anatomy is important to anatomists, radiologists, anesthesiologists and surgeons, and has gained more importance due to the wide use and reliance on computer imaging in diagnostic medicine5. Also, the presence of anatomic variations of the peripheral nervous system is often used to explain unexpected clinical signs and symptoms. Descriptions of nerve variations are useful in clinical/surgical practice since an anatomical variation can be the cause of a nerve palsy syndrome due to a different relation of a nerve and a related muscle. In most of these cases, surgery can lead to a rapid recovery of nerve function6. Although a brachial plexus injury during neck surgery is a rare condition, especially due to its protection by a dense layer of deep cervical fascia surrounding the scalenus muscles and also the protection of its roots between the scalenus anterior and scalenus medius muscle, anatomical variations of the brachial plexus may render it vulnerable to injury during routine surgical neck dissection7. In our observations, the dorsal scapular branch was completely out of the scalenus medius muscle during its course in 27%, being vulnerable to injury in neck surgical procedures. Also, because of the relatively large number of prefixed plexuses (24 % in our cases), the phrenic nerve originated entirely from the plexus in 20% of the cases. An injury to the plexus in the neck, in these cases, could result in unexplained diaphragm palsy.
Kerr8 extensively revised the anatomy of the brachial plexus in man and, classified this anatomical structure into 3 groups and 7 sub-groups. Although most of the variations reported in that study were also present in ours, with some differences in the percentages (probably due to the large number of cases studied in that study), some variations remained to be described. In our observations, we found a middle trunk which received a communicating branch from C8 what could be an indicative that the musculocutaneous nerve may receive fibers also from C8, what has not been previously reported. Another observation from our material is that the posterior cord from 5 plexuses was formed by the posterior divisions of the superior and middle trunks. This observation is suggestive that, in some cases, the axillary and the radial nerves may not receive fibers from C7 and C8, as usually described. The origin of the suprascapular nerve from C5 is mentioned by Tountas and Bergman1 and was present in 5.5% of our cases. The origin of the upper subscapular nerve from the axillary nerve and the origin of the lower subscapular nerve from the thoracodorsal nerve were also not described before.
The presence of communicating branches between the terminal branches of the brachial plexus was relatively common in our material. The existence of communicating branches may be of importance in the evaluation of unexplained sensory loss after trauma or surgical intervention in a particular area9.
The absence of the musculocutaneous nerve was described by LeMinor10 and by Nakatani and Tanaka11,12 and in all these cases, the lateral cord pierced the coracobrachialis muscle and inervated the anterior muscles of the arm. In our series, none of the brachial plexuses presented such variation. The formation of the median nerve by three roots was described by Sargon et al.3 on a male cadaver. In this case, the authors reported the presence of two roots coming from the lateral cord, one of them with a very close course over the axillary artery. The same variation was present in 52% of our material and one must be aware that this kind of variation is more prone to injury in surgical operations of the axilla and that, the very close course of the second lateral root of the median nerve to the axillary artery may lessen the blood supply of the upper extremity by compressing the vessel3.
Although some differences were present in our material, a pattern of variations for sex, color or side of the body was not evident. As also described by Kerr8, the plexuses studied did not show that sex, color or side of the body had much if any influence upon the presence of variations.
Conflict of interest: None
Financial Support: FAPEMIG grant nº CBS 8011896, CNPq grant nº 501230/2003-3 and FAPESP grant nº 02/09406-5.
- 1. Tountas CP, Bergman RA. Anatomic Variations of the Upper Extremity. Churchill Livingstone, New York, 1993.
- 2. Uzun A, Seeling LL Jr. A Variation in the Formation of the Median Nerve: Communicating Branch Between the Musculocutaneous and Median Nerves in Man. Folia Morphol 2002; 60: 99-101.
- 3. Sargon MF, Uslu SS, Celik HH, AkÄit D. A Variation of the Median Nerve at the Level of the Brachial Plexus. Bull Assoc Anat 1995; 79: 25-6.
- 4. Agur AMR. Grant's Atlas of Anatomy. 9th Ed. Baltimore: Williams & Wilkins, 1991.
- 5. Harry WG, Bennett JDC, Guha SC. Scalene Muscles and the Brachial Plexus: Anatomical Variations and Their Clinical Significance. Clin Anat 1997; 10: 250-2.
- 6. Megele R. Anterior Interosseus Nerve Syndrome with Atypical Nerve Course in Relation to the Pronator Teres. Acta Neurochir 1988; 91: 144-6.
- 7. Gacek RR. Neck Dissection Injury of a Brachial Plexus Anatomical Variant. Arch Otolaryngol Head Neck Surg 1990; 116: 356-8.
- 8. Kerr AT. The Brachial Plexus of Nerves in Man, the Variations in its Formation and Branches. Am J Anat 1918; 23: 285-395.
- 9. Hoogbergen MM, Kauer JM. An Unusual Ulnar Nerve-Median Nerve Communicating Branch. J Anat 1992; 181: 513-6.
- 10. LeMinor JM. A Rare Variation of the Median Nerve and Musculocutaneous Nerve in Man. Arch Anat Histol Embryol 1990; 73: 33-42.
- 11. Nakatani T, Tanaka S. Absence of the Musculocutaneous Nerve with Innervation of Coracobrachialis, Biceps Brachii, Brachialis and the Lateral Border of the Forearm by Branches from the Lateral Cord of the Brachial Plexus. J Anat 1997; 191: 459-60.
- 12. Nakatani T, Tanaka S. Two Rare Anomalies of the Brachial Plexus. J Anat 1998; 192: 303-4.
Publication Dates
-
Publication in this collection
29 Apr 2004 -
Date of issue
2003