Abstracts
PURPOSE: To investigate the effects of l-alanyl-glutamine (Ala-Gln) intragastric administration upon blood and kidney metabolic parameters alterations in rats subjected to ischemia/reperfusion of hind limb. METHODS: Forty-eight male rats were randomized in 2 groups offered via gavage either saline 2.0 mL (G-1) or Ala-Gln solution 0.75 mgKg-1(G-2) once a day at 7 AM during 7 days. One-hour after the last gavage (Day 7) all rats were submitted to ether anesthesia, laparotomy and clamping of the left iliac artery for 3 h. Kidney and blood samples were collected at the end of ischemic period (3h) and at 1-3-6h during reperfusion period for metabolites (pyruvate, lactate, glucose and ketone bodies) enzymatic analysis. ATP was also assayed in kidney samples. RESULTS: Lactacemia and ketonemia were significantly increased in Ala-Gln treated rats during reperfusion. Kidney pyruvate concentrations were significantly decreased and tissue lactate concentrations were significantly increased during reperfusion (1h and 3h) in G-2 rats compared with respective controls. Glucose, ATP and ketone bodies concentrations were significantly increased in the kidney in L-Ala-Gln treated rats at 3 hours after reperfusion as compared to respective controls. CONCLUSIONS: Unilateral hind limb ischemia in L-Ala-Gln pre-treated rats may induce increased lactacemia and increased kidney lactate concentrations, indicating increased glycolytic activity in renal medulla and in other peripheral tissues. Higher ketonemia during reperfusion may reflect a possible increase in ketogenesis due to lower insulin plasma concentration hepatic signaling as a result of increased glucose oxidation in peripheral tissues, caused by the intra-gastric administration of glutamine dipeptide, suggesting also decreased insulin resistance.
Ischemia; Reperfusion; Kidney; Metabolism; Rats; Wistar
OBJETIVO: Investigar alterações dos parâmetros metabólicos no sangue e rim de ratos submetidos à isquemia/reperfusão do membro pélvico. MÉTODOS: Quarenta e oito ratos machos foram distribuídos aleatoriamente em 2 grupos pré-tratados com administração intragástrica de solução salina 2,0 mL (G-1) ou L-alanil-glutamina 0,75 mgKg-1(G-2), uma vez ao dia (7:00h) durante 7 dias. Uma hora após a última gavagem todos os ratos foram anestesiados com éter dietílico, laparotomizados e submetidos ao pinçamento da artéria de ilíaca esquerda, durante 3 horas. Amostras foram coletadas ao término de isquemia e durante a reperfusão (1-3-6h) para determinação das concentrações in vivo de piruvato, lactato, glicose e corpos cetônicos (rim e sangue) e ATP (rim). RESULTADOS: Lactacemia e cetonemia aumentaram no grupo G-2 quando comparadas às aferidas em ratos não-tratados, durante a reperfusão. As concentrações de piruvato diminuíram e de lactato aumentaram significativamente no rim, durante a reperfusão (1h, 3h) em ratos do G-2 comparados aos respectivos controles. Houve um aumento significante nas concentrações renais de glicose, ATP e corpos cetônicos nos ratos tratados com L-alanil-glutamina durante a reperfusão (3h). CONCLUSÕES: A isquemia do membro pélvico em ratos pré-tratados com L-alanil-glutamina induz aumento da lactacemia e da concentração de lactato renal, indicando atividade glicolítica aumentada na medula renal. A hipercetonemia induzida pela oferta do dipeptídeo sugere cetogênese elevada, sinalizada por possível queda nas concentrações plasmáticas de insulina resultante da maior oxidação de glicose e utilização desse hormônio em tecidos periféricos.
Isquemia; Reperfusão; Rim; L-Alanil-glutamina; Metabolismo; Ratos Wistar
9 - ORIGINAL ARTICLE
Effects of L-alanyl-glutamine upon the blood and kidney biochemical parameters in the rat hind limb model of ischemia/reperfusion1 1 . From the Department of Surgery, Post-graduation Program ( Stricto Sensu), Faculty of Medicine, Federal University of Ceará (UFC), Brazil.
Efeitos da L-alanil-glutamina sobre os parâmetros bioquímicos do sangue e do rim no rato submetido à isquemia/reperfusão do membro pélvico
Marcos Antonio AlvesI; Sérgio Botelho GuimarãesII; Daniel Aguiar DiasIII; Paulo Roberto Cavalcante de VasconcelosIII; Vicente de Paulo Martins CoelhoIII; Paulo Roberto Leitão de VasconcelosIV
IPost-Graduate Student (UFC)
IIMaster in Surgery, Associate Professor, Faculty of Medicine (UFC) Fortaleza, CE
IIIMedical students (UFC)
IVProfessor of Surgery (Ph.D.), Coordinator, Post-graduation Program (Stricto Sensu), Faculty of Medicine (UFC), Fortaleza, CE
Correspondence Correspondence to Paulo Roberto Leitão de Vasconcelos Departamento de Cirurgia Rua Prof. Costa Mendes, 1608/3º andar 60430-140 FortalezaCE Brazil Phone: (55 85)288-8063 Fax: (55 85)288-8064 mcirur@npd.ufc.br
ABSTRACT
PURPOSE: To investigate the effects of l-alanyl-glutamine (Ala-Gln) intragastric administration upon blood and kidney metabolic parameters alterations in rats subjected to ischemia/reperfusion of hind limb.
METHODS: Forty-eight male rats were randomized in 2 groups offered via gavage either saline 2.0 mL (G-1) or Ala-Gln solution 0.75 mgKg-1(G-2) once a day at 7 AM during 7 days. One-hour after the last gavage (Day 7) all rats were submitted to ether anesthesia, laparotomy and clamping of the left iliac artery for 3 h. Kidney and blood samples were collected at the end of ischemic period (3h) and at 1-3-6h during reperfusion period for metabolites (pyruvate, lactate, glucose and ketone bodies) enzymatic analysis. ATP was also assayed in kidney samples.
RESULTS: Lactacemia and ketonemia were significantly increased in Ala-Gln treated rats during reperfusion. Kidney pyruvate concentrations were significantly decreased and tissue lactate concentrations were significantly increased during reperfusion (1h and 3h) in G-2 rats compared with respective controls. Glucose, ATP and ketone bodies concentrations were significantly increased in the kidney in L-Ala-Gln treated rats at 3 hours after reperfusion as compared to respective controls.
CONCLUSIONS: Unilateral hind limb ischemia in L-Ala-Gln pre-treated rats may induce increased lactacemia and increased kidney lactate concentrations, indicating increased glycolytic activity in renal medulla and in other peripheral tissues. Higher ketonemia during reperfusion may reflect a possible increase in ketogenesis due to lower insulin plasma concentration hepatic signaling as a result of increased glucose oxidation in peripheral tissues, caused by the intra-gastric administration of glutamine dipeptide, suggesting also decreased insulin resistance.
Key words: Ischemia. Reperfusion. Kidney. Metabolism. Rats, Wistar.
RESUMO
OBJETIVO: Investigar alterações dos parâmetros metabólicos no sangue e rim de ratos submetidos à isquemia/reperfusão do membro pélvico.
MÉTODOS: Quarenta e oito ratos machos foram distribuídos aleatoriamente em 2 grupos pré-tratados com administração intragástrica de solução salina 2,0 mL (G-1) ou L-alanil-glutamina 0,75 mgKg-1(G-2), uma vez ao dia (7:00h) durante 7 dias. Uma hora após a última gavagem todos os ratos foram anestesiados com éter dietílico, laparotomizados e submetidos ao pinçamento da artéria de ilíaca esquerda, durante 3 horas. Amostras foram coletadas ao término de isquemia e durante a reperfusão (1-3-6h) para determinação das concentrações in vivo de piruvato, lactato, glicose e corpos cetônicos (rim e sangue) e ATP (rim).
RESULTADOS: Lactacemia e cetonemia aumentaram no grupo G-2 quando comparadas às aferidas em ratos não-tratados, durante a reperfusão. As concentrações de piruvato diminuíram e de lactato aumentaram significativamente no rim, durante a reperfusão (1h, 3h) em ratos do G-2 comparados aos respectivos controles. Houve um aumento significante nas concentrações renais de glicose, ATP e corpos cetônicos nos ratos tratados com L-alanil-glutamina durante a reperfusão (3h).
CONCLUSÕES: A isquemia do membro pélvico em ratos pré-tratados com L-alanil-glutamina induz aumento da lactacemia e da concentração de lactato renal, indicando atividade glicolítica aumentada na medula renal. A hipercetonemia induzida pela oferta do dipeptídeo sugere cetogênese elevada, sinalizada por possível queda nas concentrações plasmáticas de insulina resultante da maior oxidação de glicose e utilização desse hormônio em tecidos periféricos.
Descritores: Isquemia. Reperfusão. Rim. L-Alanil-glutamina. Metabolismo. Ratos Wistar.
Introduction
Ischemia leads to muscle cell energy failure and biochemical alterations. Skeletal muscle represents 70 to 75% of the whole mass of the inferior members and 80% of the active metabolism of the organism. Skin, bones and tendons are quite resistant to the hypoxia compared with the skeletal muscle that exhibits an intermediate resistance under the same condition. That relative tolerance to the ischemia is largely owed, not only the low metabolic activity in rest, as well as to the great glycogen and high energy phosphates storage. Under these conditions basic cellular functions are maintained via anaerobic glycolysis.1 As early as 1941 investigators have described a renal complex metabolic syndrome secondary to ischemia and reperfusion of lower limbs.2 It is well established that exposure to hypoxia results in local tissue injury. The ischemic lesion may be aggravated by the return of fresh blood flow to the ischemic muscle originating the so-called reperfusion syndrome. The ill effects of this syndrome affect not just the local tissues. Remote organs such as the heart, kidneys, liver and lungs may be affected.3 The search for efficient substances to revert or attenuate the ischemia/reperfusion injury has been pursued extensively and new drugs are continually being added to the already extensive list of compounds. Glutamine is considered a conditionally essential amino acid, since endogenous glutamine production may be insufficient to meet the increased requirements during catabolic stress conditions.4 In addition, glutamine is the most abundant free amino acid in the extra and intracellular compartments, contributing to more than 50% of the body free amino acid pool and may it may play a significant role in the biochemical changes that occur during ischemia.4,5 The aim of this study is to examine the effect of L-alanyl-glutamine intra-gastric pre-treatment in rats subjected to 3-hour hind limb ischemia upon blood and kidney biochemical parameters by assaying in vivo concentrations of pyruvate, lactate, glucose, ketone bodies and ATP (only in kidney tissue).
Methods
Forty-eight healthy male albino Wistar (Mammalia Rodentia, Muridae, Rattus Norvegicus Albinus) rats obtained from Faculty of Medicine (Federal University of Ceará) Small Animals Laboratory. Rats weighing 400-450 g (average 420 g) were used in this study. All animals were of the same breed and raised in controlled environment for research use only. All rat procedures and handling were in compliance with the University of Ceará ethical guidelines for handling and care of experimental animals and the Council for International Organization of Medical Sciences (CIOMS) ethical code for animal experimentation (WHO Chronicle 1985; 39(2):51-6). Approval for experimental use of laboratory animals was obtained from the Commission of Ethics in Animal Research, Federal University of Ceará. The design of the experiment is depicted in Figure 1. All procedures were performed under inhalatory diethyl ether anesthesia. After each surgical intervention rats were allowed to recover from anesthesia and were left free in their cages.
Blood and muscle samples
Samples from arterial blood and kidney were collected at the end of ischemia and 1, 3 and 6 hours later, during reperfusion of the muscle. Kidney samples were obtained from each rat and immediately freeze-clamped in liquid nitrogen for posterior biochemical analysis. Blood samples were placed in glass vials containing perchloric acid and deep frozen until utilized.
Biochemical analysis
Pyruvate, lactate, glucose and ketone bodies concentrations were assayed in blood and kidney samples according to biochemical methods published elsewhere.6-9 Kidney ATP was determined according to Lamprecht & Trautschold's method.10
Statistical analysis
Metabolites concentrations were calculated as µmol/g of fresh tissue or µmol/ml blood and the results were expressed as mean ± SEM (Standard Error of the Mean). Mann-Whitney and Kruskal-Wallis/Dunn non-parametric tests were used for statistical analysis. Statistical significance was accepted as p<0.05.
Results
Blood concentrations of pyruvate and lactate were similar in control and experiment groups (Table 1). Lactacemia was significantly increased at 1h (3.21±0.25 vs. 1.63±0.13) and at 3h post-revascularization (2.57±0.66 vs. 0.49±0.17) in Ala-Gln treated rats (G-2) compared with respective controls. Blood lactate levels were significantly decreased in G-1 rats at 6h compared with 0h (0.49±0.17 vs. 2.17±0,33) and at 3h post-revascularization (0.49±0.17 vs. 1.63±0.13) (Figure 2). Ketonemia was significantly increased in Ala-Gln treated rats during reperfusion (1h: 0.67±0.11 vs. 0,37±0.06), (3h: 0.89±0.22 vs. 0.37±0.06) and (6h: 1.33±0.11 vs. 0.54±0.01). There was also an increase in blood ketone body concentrations at the end of the study (6h of reperfusion) compared with 0h (maximal isquemia) (1.33±0.11 vs. 0.55±0.04). (Figure 3).
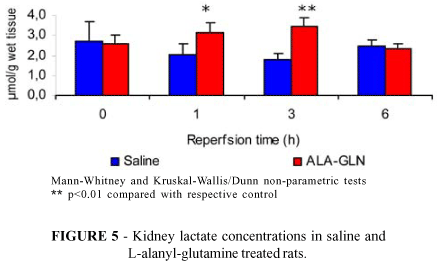
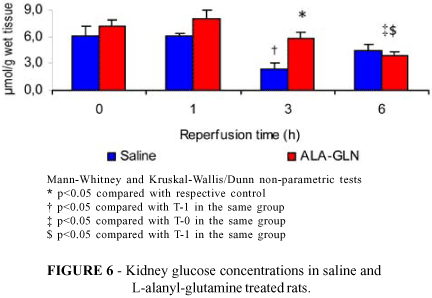
Kidney pyruvate concentrations were significantly decreased (1h: 0.33±0.08 vs. 1.01±0.19 and 3h: 0.37±0.08 vs. 1.03±0.11) and lactate concentrations were significantly increased (1h: 3.13±0.49 vs. 2.03±0.55 and 3h: 3.46±0.42 vs. 1.81±0.26) after revascularization in G-2 rats compared with respective controls (Figures 4 and 5). Glucose (Figure 6), ATP (Figure 7) and ketone bodies (Figure 8) concentrations in the kidney were increased at 3h of reperfusion (glucose: 5.76±0.75 vs. 2.40±0.68 / ATP: 0.75±0.06 vs. 0.45±0.05 / ketone bodies: 1.03±0.11 vs. 0.42±0,05 as compared to those found in non-treated rats. There was also a significant increase in ATP concentrations (0.89±0.06 vs. 0.45±0.05) in G-1 rats at the end of the reperfusion period (6h) compared with 3h post-revascularization (Figure 7). G-1 rats presented a significant decrease in ketone bodies concentrations at 3h, compared with 0h (0.42±0.05 vs. 1.43±0.17) and 1h(0.42±0.05 vs.1.64±0.29) of reperfusion (Figure 8).
Discussion
Glutamine free form (L-glutamine) is poorly soluble in aqueous solution, highly unstable in low pH and high temperatures. Due to such limitations it has been recommended the administration of glutamine precursors, such as glycil-glutamine (Gly-Gln) or L-alanyl-glutamine (Ala-Gln) for their high solubility in water and stability during preparation, storage and administration of nutritional solutions when nutritional therapy is required. Hydrolysis occurs as soon as the dipeptide Ala-Gln is introduced into the blood stream, releasing alanine and glutamine.10 The increased blood lactate concentrations in Ala-Gln treated rats points out to an increase in the anaerobic glycolysis in the peripheral tissues. This increased lactacidemia is related to the pro-glycolytic activity of Ala-Gln (Figure 2). This may occur via conversion of glutamine to glutamate in rich glutaminase tissues, activation of the malate/aspartate shuttle and increased availability of NAD+ at citosol, which in turn, enhances the conversion of one molecule of glucose into two molecules of pyruvate (glycolitic first step).11,12 It has been shown in glutamate pre-treated rabbits a significant improvement of myocardial function along with elevation of lactate levels due possibly to increased anaerobic production of ATP.13 Recent studies have demonstrated that glycolysis may be glutamate-mediated, increasing lactate concentrations in head-injured patients.14 In the present study exogenous offer of l-alanyl-glutamine may have led to increased availability of glutamate to glutaminase rich tissues such as kidney medulla. Glutamate in turn stimulates the malate-aspartate shuttle leading to a redox state, rich in NAD+, favorable to glycolytic pathway activation.15 Increased blood ketone bodies levels during reperfusion in G-2 as compared to G-1 may be related to increased ketogenesis (Figure 3). The signal to activate ketogenesis is lower plasma insulin. Increased glycolysis in peripheral tissues indicates higher insulin utilization (decreased insulin resistance) and may have an impact in lowering plasma insulin concentrations. The significant decrease in renal pyruvate concentrations during reperfusion (1h and 3h) suggests greater utilization of this metabolite in the anaerobic glycolysis pathway (increased activity of the Krebs cycle in the renal cortex) resulting in decreased total renal pyruvate levels (Figure 4). Kidney medulla metabolic activity is primarily glycolytic, resulting in increased lactate levels due to utilization of glucose for energy production. This activity may explain the significant increase in kidney lactate concentrations during reperfusion (1h, 3h) in rats pre-treated with Ala-Gln (Figure 5). Also, there was increased renal glucose concentration in G-2 animals (3h) may be related to increased uptake of glucose. The same phenomenon was not observed in saline treated rats despite glycemia levels being similar in both groups (Figure 6). The apparent increase in renal ATP (Figure 7) and ketone bodies (Figure 8) in G-2 compared with G-1 during reperfusion (3h) was probably due to a decrease in the concentration of ATP and ketone bodies in G-1. As the concentrations of those metabolites remained similar during the reperfusion period one may believe that this finding could be related to Ala-Gln activity.
Conclusions
This study has shown that the enteral offer of glutamine dipeptide to animals subjected to unilateral hind limb ischemia, caused by clamping of the left iliac artery, may induce increased lactacemia and distant metabolic alterations in renal biochemical parameters expressed by increased kidney lactate concentrations, indicating elevation of glycolytic activity in renal medulla. The elevation in ketonemia may reflect enhanced ketogenesis, possibly due lower plasma insulin as a result of increased insulin utilization (lower insulin resistance) as a consequence of augmented activation of glucose utilization in peripheral tissues, induced by the intra-gastric administration of L-alanyl-glutamine, via activation of malate/aspartate shuttle.
Received: May 7, 2005
Review: June 9, 2005
Accepted: July 13, 2005
Conflict of interest: none
Financial source: none
- 1. Perry MO. Compartment syndromes and reperfusion injury. Surg Clin North Am. 1998; 68:853-64.
- 2. Bywaters EGL, Beall D. Crush injuries with impairment of renal function. Br Med J. 1941;1:427-32.
- 3. Grace PA. Ischaemia-reperfusion injury. Brit J Surg. 1994;81:637-47.
- 4. Souba WW. Nutritional support. N Engl J Med. 1997;336:418.
- 5. Furst P, Pogan K, Stehle P: Glutamine dipeptides in clinical nutrition. Nutrition 1997;13:731-7.
- 6. Hohorst HJ, Kreutz FH, Bütcher TH. On the metabolite content and the metabolite concentration in the liver of the rat. Biochemische Zeitschrift 1959;332:18-46.
- 7. Williamson DH, Mellanby J, Krebs HA. Enzymic determinations of the D-(-) â-hydroxybutyric acid and acetoacetic acid in blood. Biochem J. 1962;82:90-6.
- 8. Hohorst HJ. D-Glucose-6-phosphate and D-fructose-6-phosphate: determination with glucose-6-phosphate dehydrogenase and phosphoglucose isomerase. In: Bergmeyer HU. Methods of enzymatic analysis. London: Weinheim/Academic Press;1963. p.134-8.
- 9. Slein MW. Determination with hexokinase and glucose-6-phosphate dehydrogenase. In: Bergmeyer HU. Methods of enzymatic analysis. London: Weinheim/Academic Press; 1963. p.117-23.
- 10. Lamprecht, W.;Trautschold, I. Determination with hexokinase and glucose-6-phosphate dehydrogenase. In: Bergmeyer HU. (Ed). Methods of enzymatic analysis. London: Weinheim/Academic Press; 1963. p. 543-51.
- 11. Souba WW. Intestinal glutamine metabolism and nutrition. J Nutr Biochem. 1993;4:2-9.
- 12. Bezerra Filho JE, Guimarães SB, Chaves CR, Queiroz DF, Vasconcelos PRC, Vasconcelos PRL. Effects of L-alanyl-glutamine on in vivo kidney and blood concentrations of glucose, pyruvate and lactate in rats subjected to unilateral renal ischemia and reperfusion. Rev Bras Nutr Clin. 2002;17:122-5.
- 13. Torres, JMS, Guimarães SB, Vasconcelos PRL.; Martins MCR, Chaves CR, Vasconcelos PRC. Efeitos metabólicos da L-Alanil-Glutamina em ratos submetidos à isquemia da pata traseira esquerda, seguida de reperfusão. Acta Cir Bras. 2003;18:39-44.
- 14. Bittl JA, Shine KI: Protection of ischemic rabbit myocardium by glutamic acid. Am J Physiol. 1983;245:406-12.
- 15. Alessandri B, Doppenberg E, Zauner A, Woodward J, Choi S, Bullock R. Evidence for time-dependent glutamate-mediated glycolysis in head-injured patients: a microdialysis study. Acta Neurochir. 1999;75:25-8.
- 16. Garcia C, Pithon-Curi CT, Firmano ML, Melo MP, Newsholme P, Curi R. Effects of adrenaline on glucose and glutamine metabolism and superoxide production by rat neutrophils. Clin Sci. 1999;96:549-55.
Publication Dates
-
Publication in this collection
08 Nov 2005 -
Date of issue
Dec 2005
History
-
Reviewed
09 June 2005 -
Received
07 May 2005 -
Accepted
13 July 2005