Abstracts
PURPOSE: To evaluate the inflammatory response of potentially infected wounds treated with isotonic saline solution, chlorhexidine and PVP-I, seven days after surgery. METHODS: Thirty-two male rats were used, divided into 4 groups. All animals had their surgical wounds infected with a standard bacterial inoculum. Control group (A): animals had their surgical wounds sutured without any kind of cleaning. Saline solution group (B): animals had their wounds cleaned with saline solution. Chlorhexidine group (C): animals had their wounds cleaned with chlorhexidine. PVP-I group (D): animals had their wounds cleaned with PVP-I. Seven days after surgery, all the animals had their skin submitted to microscopic and macroscopic evaluation. RESULTS: Edema was found on all histological slices analyzed, as well as vascular proliferation and congestion. Groups A and D showed presence of mild neutrophilic infiltrate, and moderate lymphocytic and macrophage infiltrate. Group B showed severe neutrophilic, macrophage, and lymphocytic infiltrate. Group C showed moderate neutrophilic, macrophage, and lymphocytic infiltrate. CONCLUSION: Group D was the group which showed inflammatory infiltrate most similar to the group that was not submitted to treatment.
Antisepsis; Chlorhexidine; Povidone-Iodine; Wounds and Injuries
OBJETIVO: Avaliar a resposta inflamatória da limpeza de feridas potencialmente infectadas tratadas com PVP-I, clorexidina e solução salina isotônica, no sétimo dia de pós-operatório, em ratos Wistar. MÉTODOS: Utilizou-se 32 ratos distribuídos em quatro grupos. Os animais tiveram suas feridas operatórias infectadas com um inóculo bacteriano padrão. Grupo controle (A): os animais tiveram suas feridas operatórias suturadas sem a limpeza com qualquer substância. Grupo solução salina (B): os animais tiveram suas feridas operatórias lavadas com solução salina. Grupo Clorexidina (C): os animais tiveram suas feridas operatórias lavadas com clorexidina. Grupo PVP-I (D): os animais tiveram suas feridas operatórias lavadas com PVP-I. Após sete dias foi realizada a avaliação morfológica da pele. RESULTADOS: Em todos cortes histológicos observou-se a presença de edema, proliferação e congestão vascular. O grupo A e D mostraram a presença de um infiltrado neutrofílico discreto, macrofágico e linfocítico moderados. O grupo B, um infiltrado neutrofílico, macrofágico e linfocítico severos. O grupo C, um infiltrado de neutrófilos, macrófagos e linfócitos em moderada quantidade. CONCLUSÃO: O grupo D foi o grupo que apresentou o infiltrado inflamatório mais semelhante com o grupo que não recebeu nenhum tratamento.
Anti-Sepsia; Clorexidina; Povidina-Iodo; Ferimentos e Lesões
ORIGINAL ARTICLE
Morphological analysis of three wound-cleaning processes on potentially contamined wounds in rats1 1 Research performed at Surgical Technique and Experimental Surgery of the Federal University of Santa Catarina (UFSC), Brazil.
Análise morfológica de três tipos de limpeza em feridas cutâneas potencialmente infectadas em ratos
Armando José d'AcamporaI; Daniella Serafin Couto VieiraII; Marcos Túlio SilvaIII; Débora Cadore de FariasIV; Ricardo TramonteV
IAssociate Professor, PhD, Department of Surgery, UFSC, Brazil
IIAssistant Professor, MSc, Department of Pathology, UFSC, Brazil
IIIAssistant Professor, MSc, Department of Anatomy, UFSC, Brazil
IVGraduate Student, UFSC, Brazil
VAssociate Professor, PhD, Department of Morphological Sciences, UFSC, Brazil
Correspondence Correspondence: Armando José d'Acampora Condomínio San Diego, casa 9 88024-420 Florianópolis SC Brazil Phone: (55 48)9961-0316 dacampora@gmail.com
ABSTRACT
PURPOSE: To evaluate the inflammatory response of potentially infected wounds treated with isotonic saline solution, chlorhexidine and PVP-I, seven days after surgery.
METHODS: Thirty-two male rats were used, divided into 4 groups. All animals had their surgical wounds infected with a standard bacterial inoculum. Control group (A): animals had their surgical wounds sutured without any kind of cleaning. Saline solution group (B): animals had their wounds cleaned with saline solution. Chlorhexidine group (C): animals had their wounds cleaned with chlorhexidine. PVP-I group (D): animals had their wounds cleaned with PVP-I. Seven days after surgery, all the animals had their skin submitted to microscopic and macroscopic evaluation.
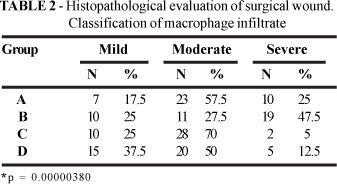
RESULTS: Edema was found on all histological slices analyzed, as well as vascular proliferation and congestion. Groups A and D showed presence of mild neutrophilic infiltrate, and moderate lymphocytic and macrophage infiltrate. Group B showed severe neutrophilic, macrophage, and lymphocytic infiltrate. Group C showed moderate neutrophilic, macrophage, and lymphocytic infiltrate.
CONCLUSION: Group D was the group which showed inflammatory infiltrate most similar to the group that was not submitted to treatment.
Key words: Antisepsis. Chlorhexidine. Povidone-Iodine. Wounds and Injuries.
RESUMO
OBJETIVO: Avaliar a resposta inflamatória da limpeza de feridas potencialmente infectadas tratadas com PVP-I, clorexidina e solução salina isotônica, no sétimo dia de pós-operatório, em ratos Wistar.
MÉTODOS: Utilizou-se 32 ratos distribuídos em quatro grupos. Os animais tiveram suas feridas operatórias infectadas com um inóculo bacteriano padrão. Grupo controle (A): os animais tiveram suas feridas operatórias suturadas sem a limpeza com qualquer substância. Grupo solução salina (B): os animais tiveram suas feridas operatórias lavadas com solução salina. Grupo Clorexidina (C): os animais tiveram suas feridas operatórias lavadas com clorexidina. Grupo PVP-I (D): os animais tiveram suas feridas operatórias lavadas com PVP-I. Após sete dias foi realizada a avaliação morfológica da pele.
RESULTADOS: Em todos cortes histológicos observou-se a presença de edema, proliferação e congestão vascular. O grupo A e D mostraram a presença de um infiltrado neutrofílico discreto, macrofágico e linfocítico moderados. O grupo B, um infiltrado neutrofílico, macrofágico e linfocítico severos. O grupo C, um infiltrado de neutrófilos, macrófagos e linfócitos em moderada quantidade.
CONCLUSÃO: O grupo D foi o grupo que apresentou o infiltrado inflamatório mais semelhante com o grupo que não recebeu nenhum tratamento.
Descritores: Anti-Sepsia. Clorexidina. Povidina-Iodo. Ferimentos e Lesões.
Introduction
Wound healing consists of a perfect and coordenate cascade of cellular and molecular events which interact to promote the repavement and reconstitution of the damaged tissue.1 Since the origins of medicine there has been a concern about the healing of wounds in general, considered to be essential to life, as it has always been known that infections acquired through wounds might lead to death.2 A great example of such ancient concern is Edwin Smith's papyrus, the oldest medical document ever known (Egypt, 5000 b.C.), which is famous for providing guidance on the treatment of infections contained therein.3,4 During the Second World War, the treatment and healing of wounds focused on the utilization of antiseptic and topical agents with antimicrobial action and protection with dry covers, a result of Pasteur's findings on the Theory of Germs. These were the golden years with regards to the utilization of antiseptics such as Dakin, Eusol, iodine, mercury and aluminum products.1 Nowadays, infection continues to be a major concern . The solution of skin continuity caused by the injury allows for both residing and transitory microorganisms to multiply, duplicating themselves every two hours after the injury, thus causing a local infection. There are also the microorganisms of the surfaces which the wound came in contact with, which may also infect it5, becoming one more interference that is likely to delay the scarring process. Based on these findings, some authors propose a didatic classification to healing, dividing the process into five main stages1:
On a routine basis, an adequate and careful mechanical cleaning of the wound is done prior to any necessary problem-solving procedure. The way in which such cleaning is to be done, however, still remais controversial among emergency professionals and the same holds true for the availabe literature.4,5,6,7,8,9,10,11,12,13,14 The routine cleaning procedure of any wound prior to suture varies from hospital to hospital. Most medical services use a chlorhexidine or a poplyvinylpyrrolidine (PVP-I) solution for wound-cleaning9,10,11,12 while others use only a saline solution at 0.9% to do the cleaning. In our service, cleaning with soap and water is thought to be the simplest, most inexpensive and rather efficient way to do it, which any service can afford. In the consulted literature on substances used in the antisepsis of wounds, contradictory results were found, mainly with regards to the use of chlorhexidine and PVP-I. De Wet et al15 verified the bactericidal effect of PVP-I in the form of ointment in the treatment of burns and concluded that it had not been satisfactory in the group studied.15 Molloy and Brady10 stated that the use of PVP-I inhibits wound healing in an experimental rat model, but does not mention the inflammatory reaction and the presence of tissue necrosis.10 In a similar line of investigation, Kjolseth et al11 proved that PVP-I delays wound epithelialization when compared to sodium hypochlorite, silver sulphadiazine, bacitracine and silver nitrate. However, these researchers did not comparatively study chlorhexidine, which is widely used in Brazilian hospitals.11 Kashyap et al12 concluded that PVP-I reduces wound strength12 and, in an experimental study, could not demonstrate its superior action when compared to an isotonic saline solution.16 More recently, Souza Filho et al2, using an animal model, evaluated the use of the isotonic saline solution compared to agar in the treatment of wounds infected with Staphylococcus aureus, in which the latter proved to be more regular and efficient than the saline solution. Most authors agree that PVP-I reduces wound infection and also that it delays healing, but no comparative experimental histological study could be found on chlorhexidine, PVP-I and the saline solution which showed the tissue reactions resulting from their individualized utilization on wounds.2,10,11,12,17,18
Several products have been experimentally tested in order to obtain the ideal substance to reduce tissue infection without altering the healing process, but there is still no consensus in the literature on this matter.7,9,10,11,12,13, 14,18,19,20,21,22,23 Therefore, this experimental study has been proposed with the purpose of comparing both macroscopically and microscopically the inflammatory reactions caused by each of the substances being studied on the cleaning of potentially infected wounds, in order to evaluate the inflammatory response of their treatment with polyvynilpyrrolidine (PVP-I), chlorhexidine and isotonic saline solution, in the seventh day post-operatory, on Wistar rats.
Methods
The experiment was conducted in the Operatory Technique and Experimental Surgery Laboratory of the Clinical Surgery Department at the Federal University of Santa Catarina. This research was approved to Ethical Animal Committee of UFSC. Thirty-two male rats of the Rattus norvergiccus species, Wistar strain, with the average age of 120 days, coming from the Central Vivarium of the Federal University of Santa Catarina. The animals were fed appropriately for the species, having free access to food and water throughout the experiment, being kept under ambient temperature, light and noise, maintaining the day-night cycle in plastic cages. Each cage contained only one animal, isolated from the forrage by a stainless steel screen, without any contact with its physiological secretions (urine and feces). The animals were distributed into four groups:
1. Control group Group A (n=8)
The animals in this group had a wound produced on their dorsal region and infected with the standard inoculum and, after 15 minutes, had the incision sutured without any wound cleaning. After seven days, they were submitted to euthanasia and a skin fragment was collected, as will be described later, and sent for a morphological analysis.
2. Saline solution group Group B (n=8)
The animals in this group had a wound produced on their dorsal region and infected with the standard inoculum and, after 15 minutes, had the incision washed with 100 ml isotonic saline solution at 0.9% and sutured with a monofilament thread. After seven days, they were submitted to euthanasia and a skin fragment was collected, as will be described later, and sent for a morphological analysis.
3. Chlorhexidine group - Group C (n=8)
The animals in this group had a wound produced on their dorsal region and infected with the standard inoculum and, after 15 minutes, had the incision washed with five ml chlorhexidine in degerming solution at 2% and 100 ml saline solution at 0.9% and sutured with a monofilament thread. After seven days, they were submitted to euthanasia and a skin fragment was collected, as will be described later, and sent for a morphological analysis.
4. PVP-I group Group D (n=8)
The animals in this group had a wound produced on their dorsal region and infected with the standard inoculum and, after 15 minutes, had the incision washed with five ml polyvinylpylorridine in a degerming solution at 10% and 100 ml saline solution at 0.9% and sutured with a monofilament thread. After seven days, they were submitted to euthanasia and a skin fragment was collected, as will be described later, and sent for a morphological analysis. The cages had alpha numeric identification, the animals being numbered one-eigth in each group.
Procedures
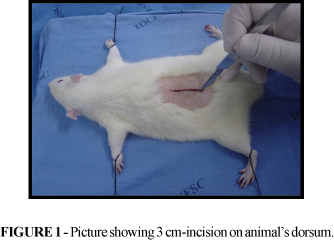
The inoculum was obtained from Staphylococcus aureus and Streptococcus pyogenes colonies provided by Santa Luzia Medical Laboratory, obtained from microbiological examinations carried out by this laboratory. These cultures were transferred to a culture environment called Miller-Hinton, placed on Petry dishes and kept in the laboratory by successive striking for suspension in a Sodium Chloride aqueous solution at 0.9%, in the amount of 109 bacteria per ml of suspension, amount considered to be infectant in 100% of cases, measured by means of a Mac Farland scale, read against the light collorimeter. The bottles were individualized with one ml of suspension each, and frozen at 70° C. The bottles were defrosted in the immediate pre-operatory in boiling water at 37° C. All animals, already identified and weighed, were submitted to anesthesia with a solution containing Ketamine Hydrochloride and aqueous solution at 2% of 2-Hydrochloride -(2, 6-xylidine)- 5, 6- dihydro-4-H-1,3-tiazine at the rate of 5:1, 0,5 ml of the solution being injected in the intramuscular way, on the inside of the animal's left leg, previously chosen by drawing. Following anesthesia, the animals were immobilized and placed on a 30x35 cm wooden board, protected by a one cm-thick styrofoam sheet and tied on their paws and legs with rubber bands in the horizontal position lying on their bellies. Depilation was done by means of pulling on the animal's dorsal region, in an area of approximately eigth cm2, without any chemical antisepsis, only washing with two ml saline solution at 0.9%. Every animal was submitted to a tree cm-incision in the median dorsal region and had the full-thickness wound produced, sectioning full corium and subcutaneous cellular tissue, later infected with one ml of each bacterial inoculum already described24,25, first Streptococcus pyogenes and then Staphylococcus aureus, such sequence being defined by drawing (Figures 1 a 4). The same bacterial strains were used for all animals in the experiment. The inoculum was previously tested and the preliminary study showed that infection occured in 100% of untreated wounds after five days.24,25 Surgical procedures were carried out with aseptic technique and at an average temperature of 28 degrees centigrade, with the support of an air conditioner.
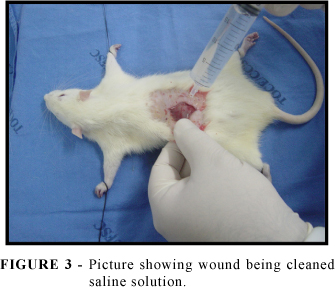
Fifteen minutes after the wound was infected by the described bacterial strain, the animals had their wounds washed by one of the substances being studied, which have been previously described, followed by wound synthesis with Mononylon® 4-0 thread in separate stitches on a single plan, comprising subcutaneous cellular tissue and skin. As to the animals in the control group, they only had their wounds sutured in the manner described above, but without any prior washing. All animals in all groups had the same number of stitches done, two stitches. No occlusive dressing was placed on the surgical wound. A daily follow-up was conducted in the post-operatory with the purpose of indentifying probable inflammatory and infectious reactions. The following parameters were used for wound analysis:
a. Alteration on skin color. b. Observation and note-taking of secretion present in the wound as to type, odor, color, and presence or not of purulent material.
No analgesia and no dressing was used in the post-operatory of the animals being srudied. Animals were submitted to euthanasia by a lethal dose of ethylic ether and were placed on a 35x30 cm wooden board lying on their bellies. A 4x2 cm skin sample was taken from the region where the procedure had been done, which was then sent for a hystopathological analysis. The skin fragments were fixed in an aqueous formaldehyde solution at 10% and sent to the Anatomico-Pathological Diagnostic Institute IDAP Pathology Laboratory at the Caridade Hospital in Florianópolis, SC. The specimens were submitted to the usual hystological processing with dehydration and clarification in a tissue processor (PT MONO 200®),being later included in paraffin blocks, identified and sectioned in microtome with five semi-seriate slices with a thickness of tree micrometers (mm). The slide blades obtained were indentified with the protocol number and stained with Hematoxilin-Eosin. All slide blades were evaluated by the same researcher in a Nikon Elipse 200® microscope with 4X e 40X lenses, with enlargements of 40X and 400X respectively. The parameters used for microscopic evaluation were:
The data obtained were submitted to statistical analysis employing EpiData and EpiInfo programs and considered to be significant when p < 0,05.
Results
Out of the 32 animals in the experiment, none came to die within seven days following the first surgical procedure. Wound examination with unarmed eye, which took place from the first to the seventh postoperative day, showed partial dehyscence of the suture in the third postoperative day in one animal of group C and on the fourth postoperative day in two animals (groups A and D). The presence of infection on the skin adjacent to the incision, with the presence of purulent and fetid odor, was seen on the seventh postoperative day in two animals of group D, characterizing pyodermatitis. Abcess formation was identified under unarmed eye on the seventh postoperative day in six animals of group A, eigth animals of group B and four animals of group D. No animal in group C presented abcess formation visible to the unarmed eye. For microscopic analysys, five histological slices of each animal were analyzed, totalling 40 slices per group and a total of 160 histological slices in this study (Figures 5 to 9). All animals in all groups presented edema, vascular proliferation and congestion upon microscopic examination of the skin.
Discussion
Wound healing is a dynamic process involving biochemical and physiological phenomena which behave in a harmonious way in order to ensure tissue restoration. The main factor which triggers healing is the local lesion with or without tissue loss, from which physiological events completely turn towards repairing that which caused damage to the integrity of the organism.1 Tissue loss may completely or incompletely affect the corium, or the whole organ, reaching subcutaneous cellular tissue. That is what wound definition stems from. In partial-thickness wounds - incomplete corium - repair takes place through the reepithelialization of epithelial annexes or epithelium originated from the unaffected adjacent skin, resulting in an almost imperceptible scar. On the other hand, full-thickness wounds - complete corium or extended to subcutaneous cellular tissue - require the formation of new tissue, called granulation tissue. Epithelialization, basis for the healing of partial-thickness wounds, takes place only on the wound edges. In this case, scarring is totally perceptible and, many times, strongly marked.1 In a clean surgical incision, neutrophils appear within 24 hours. There is thickening of the epidermis on the incisional edge, resulting from basal cell mitosis. Within 24 to 48 hours, a continuous thin epithelial layer is formed right under the superficial crust, resulting from the migration and growth of epithelial cells. Up until the third day neutrophils are, in their majority, replaced by macrophages which will reach their peak at 10 days. Granulation tissue invades the incision, with the appearance of collagen fibers on the incisional edges. By the fiveth day the incisional space is filled by granulation tissue.26 From the seventh day on there is fibroblast proliferation and continuous accumulation of collagen, with the disappearance of most of the leucocyte infiltrate, the edema and the increased vascularization. The scar becomes pale due to the presence of collagen. In the clean surgical wound, maximum neovascularization takes place at five days. Collagen becomes abundant and epidermial architecture is recovered, with superficial keratinization. At the end of the first month the scar is represented by connective tissue free of inflammatory infiltrate. Many variables, both general as well as local, influence the long and complex healing process. With the evolution of hospital infection control studies, the role of endogenous and exogenous factors which lead to such problem has become evident, which caused antisepsis to become a rational measure rather than a questionable one.17 Out of the general factors which interfere in healing some may be highlighted, such as age, nutritional status, the existence of disease (such as diabetes), cardiocirculatory and coagulation alterations, systemic infectious conditions and the use of systemic drugs. Some of the local factors which interfere in healing are the surgical technique, the formation of hematomas, reaction to foreign bodies, infection and the use of topical drugs.1,26 In this study we have tried to standardize the animal samples in such a way that the variables which might interfere with the healing process would be the same. All animals had approximately the same age, were fed the same diet, operated on by the same researcher, exposed to the same quantity and quality of inoculum, with the surgical wound being sutured with the same type thread and equal number of stitches. The use of different topical agents to clean the wounds was the only variable under study. The resulting slides were analyzed by the same researcher who did not know which experimental group they belonged to, thus avoiding variations in their result. The rat was the experimental animal of choice because of factors such as easy obtention, handling and maintenance aside from a lesser morbidity and mortality, as they are animals of proven strength, even in an adverse environment.27 Another advantage in the use of rats is the smaller amount of elastic fibers found on the corium28, since there was no interest in the study of collagen, allowing researchers to study the greater or lesser inflammatory process depending on the antisseptic agent envolved. In this experimental model the choice was to conduct the suture in all animals, in order to protect the spot from other bacteria which the wound might get in contact with otherwise, and to have a better correlation with what happens in the daily routine of human emergency wards. Nevertheless, the suture is known to contribute with the appearance of infection. It serves as a mechanical deposit for bacteria and also as an irritating factor. The mechanical aspect of suture strain also favors the onset of infection.2 The presence of a foreign body, in this case the suture, significantly decreases the number of germs causing local infection, a fact which has been proven by Elek.24 The standard inoculum used in this study has been previously tested. Preliminary studies carried out by Elek24 and Roettinger et al25 showed that the inoculation of 109 bacteria per ml of suspension, done on the dorsum of laboratory animals, causes the appearance of 100% infection. Both PVP-I and chlorhexidine have different antisseptic properties. Saline solution, however, despite not being an antisseptic, shows to be efficient in the treatment of the infected wound. This leads us to believe that, whatever solution is employed, the main thing is to allow for a good irrigation with enough volume and pressure to cause the mechanical removal of fibrin, debris, bacteria and secretion from the wound surface.29 The PVP-I and the chlorhexidine used in this study were aquous solutions, known as degerming solutions. The presence of alcohol in the composition of these products would interfere negatively in tissue regeneration since, when applied locally, it promotes cell damage, precipitating and dehydrating its protoplasm.17 Contact between surgery and these antiseptic agents takes place in a direct and indirect way, as both PVP-I and chlorhexidine have residual action following antisepsis.17 PVP-I has been synthetized in 1953, being broadly used as a surgical antisseptic, at the concentration of 1%, since then called povidine®. Its active principle is free iodine, presenting bacteriostatic action at the concentration of 6.4% and bactericide action at 9.6%, with regards to Staphylococcus aureus. The concentration used in this study was 10%, aquous solution, avoiding the citotoxic effects presented by alcohol.30 Many authors agree that the use of iodine substances causes tissue damage and question their indication in the prophylaxis of wound infection. This is due to the fact that the PVP-I solution has, in its composition, a non-ionic surfactant which provides more adherence to the surface on which it is employed, allowing for the release of iodine during a longer period, which increases the length of its antimicrobial action.17 With the wide use of PVP-I in the treatment of contaminated wounds, results as to its influence on healing and antibacterial effect are still controversial. We have tried to evaluate its effect on wounds contaminated with Staphylococcus aureus and Streptococcus pyogenes as compared to the utilization of chlorhexidine and saline solution, on lab rats. Macroscopic evaluation of surgical wounds, conducted on the seventh postoperative day, under unarmed eye, showed the formation of abcesses in 75% of untreated animals, 100% of animals treated with saline solution and 50% of those treated with chlorhexidine. Abcess formation in the animals treated with PVP-I was not verified under unarmed eye on the seventh postoperative day. This suggests that the group treated with PVP-I had greater protection against bacteria or had a slower inflammatory process, thus delaying the organization of collections. Nevertheless, this was the group which, on the seventh postoperative day, presented two animals (25%) with purulent secretion of fetid odor on the skin adjacent to the surgical incision, characterizing pyodermatitis (folliculitis?). This was not observed in any other animal in this study. In all histological slices analyzed in this study, out of all groups, the presence of edema, vascular proliferation and congestion was observed, important events in the inflammatory response and wound healing, be they contaminated or not. Upon analyzing the group which did not undergo any type of treatment, the presence of a mild neutrophilic infiltrate is observed, as well as moderate macrophage and lymphocytic infiltrate. This characterizes an inflammatory process which is becoming chronic, most likely due to the infection which perpetuates cell damage. This is the representaion of the natural evolution of an untreated infected wound in Wistar rats. Group B, on the other hand, treated only with saline solution, shows a severe neutrophilic, macrophage and lymphocytic infiltrate. Saline solution certainly influences the healing process somehow, perhaps due to the mechanical action caused by its pressure and volume which ends up dragging off debris and cells, but basically diluting and distributing the inoculum inside the wound. The group of animals treated with chlorhexidine presented a moderate neutrophilic infiltrate, accompanied by macrophages and lymphocytes in moderate quantity as well. The animals treated with PVP-I showed a predominantly mild neutrophilic infiltrate, accompanied by macrophages and lymphocytes in moderate quantity. This was the group which was closer to the outcome observed on the animals which had no substance interfering on the healing process other than the infection itself. The presence of a moderate to mild lymphocytic infiltrate in all slices studied, in all groups, leads us to think about a chronification of the inflammatory process, problably due to the infection present in all animals, which perpetuates cell damage. Edema did not disappear in the slices studied. After seven days, it was observed that groups A (untreated) and D (treated with PVP-I) were the ones which presented a healing outcome which was most similar to the natural history, with a predominance of a mild neutrophilic infiltrate, moderate macrophage and lymphocytic infiltrate and presence of granulation tissue. The healing of full-thickness wounds, produced in this study, requires the formation of new tissue, the granulation tissue, and re-epithelization occurs from the edges to the center of the wound. On all slices analyzed, after the seventh day, there was presence of granulation tissue, except for one slice from group A. Nevertheless, the absence of granulation tissue in only one slice, out of the 160 total, was not statistically significant, p > 0.05. Several authors demonstrate the citotoxic effect of PVP-I at 10% over fibroblasts.17,30 In this study there was fibroblast proliferation in all slices analyzed, except for one slice in group D, treated with PVP-I.. However, this piece of data was not statistically significant, p > 0.05. These authors have demonstrated a more intense inflammatory process and a slower regeneration when PVP-I is used as compared to saline solution and chlorhexidine.17,30 The result of the present study demonstrates that tissue repair and healing took place more rapidly in the untreated group, folloswed by the group treated with PVP-I, then saline solution and lastly the group treated with chlorhexidine. The parameter used to determine the speed of healing was the presence of young fibrosis. Its absence was considered to be a delay in the healing process. In all slides studied there is fibroblast proliferation. The presence of foreign body granuloma was most observed in the slides feom group B (85%), followed by group C (72.5%), D (55%) and A (47.5%), a result considered to be statistically significant (p=0.00168107). This foreign body granuloma formed around the suture thread and was present in all surgical wounds studied. However, this result is pure chance. All animals had the same number of stitches with the same type thread. The formation of this granuloma around the suture thread is known to be inevitable. The fact that this granuloma was not observed on some slides was due to their section levels which, by chance, may or may not go over the exact spot where the suture thread was present.
Conclusions
1. Groups A e D showed, on the seventh postoperative day, an inflammatory infiltrate with neutrophils (polymorphonuclear) in mild quantity and an infiltrate with macrophages and lymphocytes (mononuclear) in moderate quantity;
2. Group B showed, on the seventh postoperative day a severe infiltrate of neutrophils, macrophages and lymphocytes;
3. Group C showed, on the seventh postoperative day a moderate infiltrate of neutrophils (polymorphonuclear), macrophages and lymphocytes (mononuclear);
4. Group D was the one which showed an inflammatory infiltrate that was most similar to that of the untreated group. This suggests that PVP-I was the substance which least interfered with the natural evolution of the inflammatory process.
Received: April 04, 2006
Review: May 09, 2006
Accepted: June 06, 2006
Conflict of interest: none
Financial source: none
- 1. Mandelbaum SH, Santis EPD, Mandelbaum MHS. Cicatrização: conceitos atuais e recursos auxiliares. An Bras Dermatol. 2003; 8(4): 8-18.
- 2. Souza Filho ZA, Repka JC, Appel L, Canelo G, Fonseca O. Estudo comparativo do ágar com a solução salina isotônica no tratamento de feridas infectadas, em cobaias. Acta Cir Bras. 1997; 12(3): 169-72.
- 3. Knutson RA. Merbitz LA. Creekmore MA. Snipes HG. Use of sugar and povidone-iodine to enhance wound healing: five year's experience. South Med J. 1981; 74(11):1329-35.
- 4. d'Acampora AJ, Ortellado DK, Schemes KE, Cútulo LRA. Um pouco da história e evolução da medicina. Rev Ciênc Saúde. 2002; 20(1): 65-7.
- 5. d'Acampora, A.J. Infecção em cirurgia. Arq Cat Med. 1994; 23(1): 55-7.
- 6. Kaysinger KK. Nicholson NC. Ramp WK. Kellam JF. Toxic effects of wound irrigation solutions on cultured tibiae and osteoblasts. J Orthop Trauma. 1995; 9(4):303-11.
- 7. Serikawa S. Ito S. Hatta T. Kusakari N. Senna K. Hiramune T. Kikuchi N. Yanagawa R. Protection from caseous lymphadenitis in sheep by spraying iodine tincture on shearing wounds. J Vet Med Sci. 1994; 56(2):411-2.
- 8. Swaim SF. Bandages and topical agents. Vet Clin North Am. 1990; 20(1):47-65.
- 9. Rashidy AA. Fox LK. Gay JM. Diagnosis of Staphylococcus aureus intramammary infection by detection of specific antibody titer in milk. J Dairy Sci. 1992; 75(6):1430-5.
- 10. Molloy RG. Brady MP. A modified technique of delayed primary closure using a povidone iodine wick: influence on wound healing in an experimental model. Ir J Med Sci. 1993; 162(8):297-300.
- 11. Kjolseth D. Frank JM. Barker JH. Anderson GL. Rosenthal AI. Acland RD. et al. Comparison of the effects of commonly used wound agents on epithelialization and neovascularization. J Am Coll Surg. 1994; 179(3):305-12.
- 12. Kashyap A. Beezhold D. Wiseman J. Beck WC. Effect of povidone iodine dermatologic ointment on wound healing. Am Surg. 1995; 61(6):486-91.
- 13. Reid AB. Stranc MF. Healing of infected wounds following iodine scrub or CO2 laser treatment. Lasers Surg Med. 1991; 11(5):475-80.
- 14. Goebel ME. Drez D Jr. Heck SB. Stoma MK. Contaminated rabbit patellar tendon grafts. In vivo analysis of disinfecting methods. Am J Sports Med. 1994; 22(3):387-91.
- 15. De Wet PM. Rode H. Cywes S. Bactericidal efficacy of 5 per cent povidone iodine cream in Pseudomonas aeruginosa burn wound infection. Burns. 1990; 16(4):302-6.
- 16. Kai MS. Comparação dos efeitos do uso do Povidine 10% e da solução salina isotônica no tratamento de feridas contaminadas: estudo experimental [Mestrado]. Curitiba: Universidade Federal do Paraná; 1993.
- 17. Filho OM, Okamoto T, Garcia IG, Aranega A, Dezan E. Biocompatibilidade das soluções de iodo polivinilpirrolidona (PVP-I) e clorexidina: estudo histológico em ratos. Rev Odontol. UNESP 1998; 5(3): 9-16.
- 18. Howell JM. Dhindsa HS. Stair TO. Edwards BA. Effect of scrubbing and irrigation on staphylococcal and streptococcal counts in contaminated lacerations. Antimicrobi Agents Chemother. 1993; 37(12):2754-5.
- 19. Archer HG. Barnett S. Irving S. Middleton KR. Seal DV. A controlled model of moist wound healing: comparison between semi-permeable film, antiseptics and sugar paste. J Exp Pathol. 1990; 71(2):155-70.
- 20. Swaim SF. Riddell KP. Geiger DL. Hathcock TL. McGuire JA. Evaluation of surgical scrub and antiseptic solutions for surgical preparation of canine paws. J Am Vet Med Assoc. 1991; 198(11):1941-5.
- 21. Taylor GJ. Leeming JP. Bannister GC. Effect of antiseptics, ultraviolet light and lavage on airborne bacteria in a model wound. J Bone Joint Surg Am. 1993; 75(5):724-30.
- 22. Severyns AM. Lejeune A. Rocoux G. Lejeune G. Non-toxic antiseptic irrigation with chlorhexidine in experimental revascularization in the rat. J Hosp Infect. 1991; 17(3):197-206.
- 23. Osuna DJ. DeYoung DJ. Walker RL. Comparison of an antimicrobial adhesive drape and povidone-iodine preoperative skin preparation in dogs. Vet Surg.1992; 21(6):458-62.
- 24. Elek SD. Experimental staphylococcal infections in the skin of man. Ann N Y Acad Sci. 1956; 65: 85-90.
- 25. Roeitinger W, Edgerion M, Kurtz LD. Role of inoculation site as a determinant of infection in soft tissue wounds. Am J Surg. 1973; 126: 354-8.
- 26. Cotran RS, Kumar V, Collins T. Patologia estrutural e functional. 6Ş ed. Rio de Janeiro: Guanabara Koogan; 2000.
- 27. d'Acampora AJ. Modelo de sepse experimental em ratos: estudo clínico e histológico [Doutorado]. São Paulo: Universidade Federal de São Paulo; 1996.
- 28. Noronha L, Chin EWK, Kimura LY, Graf R. Estudo morfométrico e morfológico da cicatrização após uso de laser erbium: YAG em tecidos cutâneos de ratos. J Bras Patol Med Lab. 2004; 40(1): 41-8.
- 29. Torres AM, Cisterna MS, Vargas G, Cosignani M, Oporto V, Fuentes N, et al. Antisepticos y solucion salina en el manejo de herida operatória infectada. Bol Hosp Viña Del Mar 1986; 42(3): 164-7.
- 30. Ribeiro RC, Santos OLR, Moreira AM, Bacellar C, Aboim E. Interferência do uso de soluções de polivinil-pirrolidona-iodo no processo cicatricial: estudo experimental em camundongos. Folha Med. 1995; 111(1): 61-5.
Publication Dates
-
Publication in this collection
11 May 2007 -
Date of issue
Oct 2006
History
-
Reviewed
09 May 2006 -
Received
04 Apr 2006 -
Accepted
06 June 2006