Abstracts
PURPOSE: To compare the effectiveness of intraperitoneally administered vitamin E with the sodium hyaluronate/carboxymethylcellulose membrane (HA/CBMC) in preventing postoperative intraperitoneal adhesion formation. METHODS: Sixty Wistar rats underwent a laparotomy and adhesions were induced (IA). The animals were divided into four groups: group 1, control (IA); group 2 (IA + Vitamin E): group 3 (IA+HA/CBMC) and group 4 (IA+ Vitamin E + HA/CBMC). The Vitamin E (groups 2 and 4) and HA/CBMC (groups 3 and 4) were administered intraperitoneally before the abdominal wall was closed. After 30 days, adhesions were classified by an independent surgeon. RESULTS: Three animals died; one from group 3 and two from group 4. All control animals had substantial adhesions compared with unsubstantial adhesions observed in 11/15 in group 2 (P = 0.000), 11/14 in group 3 (P = 0.001), and 10/13 in group 4 (P = 0.000). CONCLUSION: Vitamin E, administered intraperitoneally, is as effective as HA/CBMC in preventing postoperative adhesions.
Adhesions; Vitamin E; Carboxymethylcellulose; Rats
OBJETIVO: Comparar a efetividade da Vitamina E e da membrana de Carboximetilcelulose/Hialuronato de Sódio (CBMC/HA) na prevenção da formação de aderências intraperitoneais pós-operatórias. MÉTODOS: Sessenta ratos Wistar foram submetidos à laparotomia para indução de aderências (IA) com abrasão do ceco seguido de aplicação de álcool absoluto e sutura com fio de seda no peritônio parietal. Os animais foram divididos em quatro grupos: 1 controle ( IA ); 2 ( IA + Vitamina E ); 3( IA + CBMC/HA ) e 4 ( IA + Vitamina E + CBMC/HA ). A Vitamina E ( grupos 2 e 4 ) e CBMC/HA ( grupos 3 e 4 ) foram administrados intraperitonealmente antes do fechamento da parede. Os ratos foram sacrificados em 30 dias e as aderências foram classificadas por cirurgião independente. Resultados: Três animais morreram, sendo um do grupo 3 e dois do grupo 4. Todos os animais do grupo controle ( 1 ) tiveram aderências substanciais, comparados com aderências insubstanciais em 11/15 no grupo 2 ( p = 0,000 ), 11/14 no grupo 3 ( p = 0,001 ) e 10/13 no grupo 4 ( p = 0,000 ). CONCLUSÃO: A Vitamina E administrada de maneira intraperitoneal é tão eficaz quanto a CBMC/HA na prevenção da formação de aderências pós-operatórias.
Aderências; Vitamina E; Carboximetilcelulose; Ratos
ORIGINAL ARTICLE
PERITONEUM
Preventing intraperitoneal adhesions with vitamin E and sodium hyaluronate/carboxymethylcellulose. A comparative study in rats1 1 Research performed at Department of Surgery, Clinical Hospital of Porto Alegre (HCPA), General Hospital of Caxias do Sul (HG), University of Caxias do Sul (UCS), Rio Grande do Sul, Brazil.
Prevenção de aderências intraperitoneais com vitamina E e hialuronato de sódio/carboximetilcelulose. Estudo comparativo em ratos
Fredy CorralesI; Marcelo CorralesII; Carlos Cauduro SchirmerIII
IMS, Digestive System Surgeon, HG UCS, Caxias do Sul, Brazil
IIVascular surgeon, HG, Caxias do Sul, Brazil
IIIPhD, Digestive System Surgeon, HCPA, Porto Alegre, Brazil
Correspondence Correspondence: Fredy Corrales R. 20 de setembro, 2430/31 95020-450 Caxias do Sul RS Brazil Phone: (55 54)3223-0108 clindig@uol.com.br
ABSTRACT
PURPOSE: To compare the effectiveness of intraperitoneally administered vitamin E with the sodium hyaluronate/carboxymethylcellulose membrane (HA/CBMC) in preventing postoperative intraperitoneal adhesion formation.
METHODS: Sixty Wistar rats underwent a laparotomy and adhesions were induced (IA). The animals were divided into four groups: group 1, control (IA); group 2 (IA + Vitamin E): group 3 (IA+HA/CBMC) and group 4 (IA+ Vitamin E + HA/CBMC). The Vitamin E (groups 2 and 4) and HA/CBMC (groups 3 and 4) were administered intraperitoneally before the abdominal wall was closed. After 30 days, adhesions were classified by an independent surgeon.
RESULTS: Three animals died; one from group 3 and two from group 4. All control animals had substantial adhesions compared with unsubstantial adhesions observed in 11/15 in group 2 (P = 0.000), 11/14 in group 3 (P = 0.001), and 10/13 in group 4 (P = 0.000).
CONCLUSION: Vitamin E, administered intraperitoneally, is as effective as HA/CBMC in preventing postoperative adhesions.
Key words: Adhesions. Vitamin E. Carboxymethylcellulose. Rats.
RESUMO
OBJETIVO: Comparar a efetividade da Vitamina E e da membrana de Carboximetilcelulose/Hialuronato de Sódio (CBMC/HA) na prevenção da formação de aderências intraperitoneais pós-operatórias.
MÉTODOS: Sessenta ratos Wistar foram submetidos à laparotomia para indução de aderências (IA) com abrasão do ceco seguido de aplicação de álcool absoluto e sutura com fio de seda no peritônio parietal. Os animais foram divididos em quatro grupos: 1 controle ( IA ); 2 ( IA + Vitamina E ); 3( IA + CBMC/HA ) e 4 ( IA + Vitamina E + CBMC/HA ). A Vitamina E ( grupos 2 e 4 ) e CBMC/HA ( grupos 3 e 4 ) foram administrados intraperitonealmente antes do fechamento da parede. Os ratos foram sacrificados em 30 dias e as aderências foram classificadas por cirurgião independente.
Resultados: Três animais morreram, sendo um do grupo 3 e dois do grupo 4. Todos os animais do grupo controle ( 1 ) tiveram aderências substanciais, comparados com aderências insubstanciais em 11/15 no grupo 2 ( p = 0,000 ), 11/14 no grupo 3 ( p = 0,001 ) e 10/13 no grupo 4 ( p = 0,000 ).
CONCLUSÃO: A Vitamina E administrada de maneira intraperitoneal é tão eficaz quanto a CBMC/HA na prevenção da formação de aderências pós-operatórias.
Descritores: Aderências. Vitamina E. Carboximetilcelulose. Ratos.
Introduction
Postoperative adhesions are a common complication following a variety of surgical procedures. In most cases they are clinically asymptomatic. However, following a laparotomy, adhesion formation is associated with serious postoperative complications, including chronic pelvic pain¹,², infertility³, and intestinal obstruction4. The risk of an inadvertent enterotomy is about 19% higher in those patients who have previously undergone abdominal surgery. Peritoneal ischemia, abrasive manipulation of tissues, infection and inadequate hemostasis, are the most frequent causes of intraperitoneal adhesion formation6, which in turn is the most significant cause of intestinal obstruction7. During re-operation, dissection between the adhesion and tissue can cause intra-operative complications and lead to longer surgical times5. This may lead to further hospitalizations and the need for intensive care and associated higher costs. In light of this, various agents have been studied to prevent the formation of postoperative adhesions, but without proper verification of their effectiveness.
The peritoneum is a membrane of mesodermic origin, covering the abdominal and pelvian cavities and the organs within, and is divided into the parietal and visceral peritoneum. Microscopically, it presents as a layer of flaccid conjunctive tissue, covered by only one layer of cells, the mesothelium8
Peritoneal inflammation (peritonitis) occurs in response to a variety of infectious (bacteria, virus, fungus, and parasite), and non-infectious stimuli (trauma, surgery, chemical agents, and neoplasia)9.10. In the inflamed peritoneum exacerbated permeability results in an increase in volume of the peritoneal fluid and the concentration of proteins, with the subsequent release of chemotactic agents and the migration of leukocytes to the site of inflammation. It is currently presumed that reduced fibrinolytic activity in the peritoneal cavity alters the balance between coagulation and fibrinolytic activity, and is the key-mechanism for the formation of peritoneal adhesions 11
Sodium hyaluronate/carboxymethylcellulose (HA/CBMC) (Seprafilm, Genzyme, MA) is a bio-reabsorbable membrane that has been shown to reduce the formation of adhesions in animal models and in human studies, and has been approved for clinical use12,13,14,15 Vitamin E, administered intraperitoneally, has also been shown to be an effective adhesion inhibitor16, without promoting adverse systemic effects17.
We therefore aimed to compare the use of intraperitoneal vitamin E with HA/CBMC in the prevention of postoperative adhesion formation.
Methods
This study was submitted and approved by the Committee of Ethics in Research of the University of Caxias do Sul.
Sixty Wistar male rats, weighing from 450 to 550 g, were used. They were accommodated in boxes with four animals in each, arranged in their own stand (Alesco®) with an exhaust and an ammonia filter, a temperature of 20º to 22ºC, and a light/dark cycle alternating every 12 hours. All rats received ration (Nuvilab®) and water ad libitum. The surgical treatment was carried out under a general anesthesia inhalant containing halothane, and intraperitoneal tiletamine-zolazapam (Zoletil®). All animals received a prophylactic dose of ampicillin (50 mg/kg) subcutaneously immediately prior to the procedure. Postoperative analgesia was obtained with the use of intramuscular butorphanol tartrate (Turbogesic®).
The animals were divided into four groups of 15 according to the treatment:
Group 1: induction of adhesions (IA).
Group 2: IA + intraperitoneal administration of vitamin E (Sigma Chemical Co, St. Louis, MO) (10 mg/5 mL olive oil, autoclaved prior to use).
Group 3: IA + insertion of the HA/CBMC membrane (measuring 30 mm × 30 mm) between the cecum and the parietal peritoneum.
Group 4: IA + insertion of the HA/CBMC membrane + intraperitoneal administration of vitamin E.
Surgical technique
We used the adhesion induction model described by Hemadeh et al.30 which resulted in a 100% incidence of adhesions in our controls. The surgeon used talc-free gloves. After anesthesia, a trichotomy was made aseptically with a povidine-iodine solution, followed by an abdominal incision 4 cm, exposing the wall of the cecum. This was rubbed with gauze until the serosa lost its shine and hemorrhagic points appeared. One drop of absolute alcohol was applied to the cecum wall in the area where the wound was provoked, and the cecum was returned to its anatomical position. The parietal peritoneum was clamped with a fine hemostat and a 3-0 silk suture ligature was placed. Before closing the wound, 5 mL of vitamin E dissolved in olive oil was applied to the animals in groups 2 and 4. In groups 3 and 4, a thin plate of HA/CBMC measuring 3 x 3 cm, was placed between the cecum and the abdominal wall. The abdominal cavity was then closed in two layers with simple, continuous sutures of silk 3-0. The animals were euthanized with halothane 30 days post surgery. A surgeon, who did not perform the initial surgery, inspected the cavity and noted the formation of adhesions based on a scale described by Nair et al.18 (Table 1).
Statistical analysis
We calculated that a sample size of 12 animals per group would provide a statistical power greater than 95% for detecting differences in the averages of at least two units of the score (assuming that the standard-deviation of the variable of the result (score) was not greater than 1.3 units).
A comparison of the groups was carried out using the non-parametric Kruskal-Wallis H test followed by the post-hoc procedure on ranks, to detect statistically significant differences among the groups. The level of significance was set to 5%. Analysis was performed using SPSS version 12.0.
Results
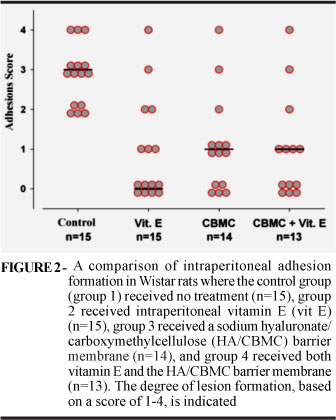
During the study, three animals died: one in group 3 (anesthetic induction), and two in group 4 (4th day post surgery) In group 1 (control group), five animals developed degree 2 adhesions, seven animals developed degree 3 adhesions, and three animals developed degree 4 adhesions. All of these are classified as substantial adhesions. A statistically significant difference was observed in the other groups, relative to the control group. In group 2 (vitamin E), eight animals did not develop adhesions (degree 0) (Figure 1a), three animals developed degree 1 adhesions (Figure 1b), two animals developed degree 2 adhesions, and one animal developed both degree 3 and degree 4 (Figure 1c) adhesions, respectively (P < 0.001). In group 3 (HA/CBMC), five animals did not develop adhesions (degree 0), six animals developed degree 1 adhesions, and one animal developed degree 2, 3 and 4 adhesions, respectively (P = 0.001). In group 4 (vitamin E + HA/CBMC) six animals did not develop adhesions (degree 0), four animals developed degree 1 adhesions and one animal developed degree 2, 3 and 4 adhesions, respectively (P > 0.001) (Figure 2). The comparison between groups 2, 3 and 4 showed no statistically significant difference in adhesion formation (Figure 2).
Discussion
Intraperitoneal adhesions are a major complication of abdominal surgery. They can result in intestinal o bstruction, in turn leading to the need for further complicated interventions with increased surgical time, the increased possibility of lesions in other organs7, and the consequent increase of the morbid-mortality of these patients. Nearly 40% of intestinal obstructions19, and nearly 70% of small intestine obstructions in Western countries occur due to postoperative adhesions.
Various agents have been studied to prevent the formation of adhesions, including the use of anti-inflammatories, antioxidants, anti-coagulants and fibrinolytics20,21,22,23,24. However, bioreabsorbable physical barriers such as sodium hyaluronate carboxymethyl-cellulose25 (Seprafilm, Genzyme, MA), polylactic acid26 (SurgiWrap, MAST ) and cellulose27 (Interceed, Johnson) are the most utilized methods in clinical practice. These barriers reduce the formation of adhesions by limiting contact of the tissues post surgery, and particularly during the period in which they are formed28, namely between the seventh and tenth postoperative day. It has been shown that this period is crucial in preventing adhesion formation29. Although these barriers are currently the most utilized methods in clinical practice, their use is limited in our setting due to their high cost.
Vitamin E presents interesting biological proprieties and activities for preventing intraperitoneal adhesions. It demonstrates numerous in vitro effects such as (1) acting as an anti-oxidant by cleaning the free radicals created locally and inhibiting the enzymatic peroxidase and non-enzymatic lipids, thus protecting the cell membranes from oxidative degradation30,31, (2) acting as an anti-inflammatory agent due to the inhibition of cyclooxygenase-2 (COX-2) and endogen conversion of the arachadonic acid in PGE2 and PGF2"16, and (3) acting as an anticoagulant by inhibiting the aggregation of platelets and maintaining their stability. Vitamin E inhibits the formation of thrombus, and consequently reduces the formation of fibrin, which is thought to play an important role in the formation of peritoneal adhesions30,32, and has an anti-fibroblastic effect, inhibiting the action of TGF-beta, a powerful fibrosis inductor, while still playing a role in diminishing the production of collagen16.
The oral and intramuscular administration of vitamin E in the prevention of adhesions has produced conflicting results30,31,33,34. However, the intraperitoneal administration of vitamin E, has proved to be a safe and efficient means of preventing intraperitoneal adhesions16, and its cost is much lower than that of the bioreabsorbable barriers.
This study shows that the intraperitoneal administration of vitamin E is as efficient as the CBMC/HA membrane in reducing the formation of postoperative adhesions, confirming the results of a previous study16. We showed that vitamin E, using olive oil as a diluting vehicle, reduced adhesion formation by 80% compared with other groups, including the group where only olive oil was used intraperitoneally.
Conclusion
The intraperitoneal use of vitamin E is as efficient as the bioreabsorbable barrier, HA/CBMC, in inhibiting the formation of postoperative adhesions. A notable advantage of this, particularly in our setting, is the cost of the vitamin E, which is much lower than the HA/CBMC barrier.
Received: August 21, 2007
Review: October 17, 2007
Accepted: November 14, 2007
Conflict of interest: none
Financial source: none
- 1. Sulamain H, Gabella G, Davis C, Mutsaers SE, Boulos P, Laurent GJ et al Growth of nerve fibres into murine peritoneal adhesions. J Pathol. 2000;192(3):396-403.
- 2. Howard FM. The role of laparoscopy in the chronic pelvic patient. Clin Obstet Gynecol. 2003;46(4):749-66.
- 3. Kavic SM, Kavic SM. Adhesions and adhesiolysis: the role of laparoscopy. J Soc Laparoendosc Surg. 2002;6:99-109.
- 4. Menzies D. Peritoneal adhesions: incidence, causes and prevention. Surg Annu. 1992;24:27-45.
- 5. Van Der Krabben AA, Dijkstra FR, Nieuwennhuijzen M, Reijnen MM, Schaalpveld M, Van Goor H. Morbidity and mortality of inadvertent enterotomy during adhesiotomy. Br J Surg. 2000;87:467-71.
- 6. Wilson MS, Hawkswell J, McCloy RF. Natural history of adhesions small bowel obstruction: counting the cost. Br J Surg. 1998;85:12948.
- 7. Ellis H. The causes and prevention of intestinal adhesions. Br J Surg. 1982;69:241-3.
- 8. Crowe DT, Bjorling DE. Peritoneum and peritoneal cavity. In: Slatter DH, editor. Textbook of small animal surgery. 2ed. Philadelphia: W. B. Saunders; 1993. p.407-30.
- 9. Ellis H. The clinical significance of adhesions: focus on intestinal obstruction. Eur J Surg. Suppl 1997;577:5-9.
- 10. Santschi EM, Grindem CB, Tate LP Jr, Corbett WT. Peritoneal fluid analysis in ponies after abdominal surgery. Vet Surg. 1988;17:6-9.
- 11. Baxter GM. Intraabdominal adhesions in horses. Compend Contin Edu Pract Vet. 1991;13:1587-97.
- 12. Oncel M, Feza H, Remzi, MD, Senagore AJ, Connor JT, Fazio VW. Application of Adcon-P or Seprafilm in consecutive laparotomies using a murine model. Am J Surg. 2004;187:3048.
- 13. Kutlay J, Ozer Y, Isik B, Kargici H. Comparative effectiveness of several agents for preventing postoperative adhesions. World J Surg. 2004;28(7):662-5.
- 14. Kusunoki M, Ikeuchi H, Yanagi H, Noda M, Tonouchi H, Mohri Y, et al Bioresorbable hyaluronate-carboxymethylcellulose membrane (Seprafilm) in surgery for rectal carcinoma: a prospective randomized clinical trial. Surg Today. 2005;35(11):940-5.
- 15. Fazio VW, Cohen Z, Fleshman JW, van Goor H, Bauer JJ, Wolff BG et al. Reduction in adhesive small-bowel obstruction by Seprafilm adhesion barrier after intestinal resection. Dis Colon Rectum 2006;49(1):1-11.
- 16. De la Portilla F, Ynfante I, Bejarano D, Conde J, Fernández A, Ortega JM et al. Prevention of peritoneal adhesions by intraperitoneal administration of vitamin E: an experimental study in rats. Dis Colon Rectum. 2005;47:2157-61.
- 17. McGee CD, Greenwood CE, Jeejeebhoy KN. Blood and tissue tocopherol levels in rats following intraperitoneally administered alpha-tocopheryl acetate. J Parenter Enteral Nutr. 1990;14(1):74-8.
- 18. Nair SK, Bath IK, Aurora AL. Role of proteolytic enzymes in the prevention of post-operative intraperitoneal adhesions. Arch Surg. 1974;11:273-80.
- 19. Menzies D. Peritoneal adhesions: incidence, cause, and prevention. Surg Ann. 1992;24:27-45.
- 20. Jackson EK. Intraperitoneal administration of adenosine inhibits formation of abdominal adhesions. Dis Colon Rectum. 2004;47:1390-6.
- 21. Guvenal T, Cetin A, Ozdemir H, Yanar O, Kaya T. Prevention of postoperative adhesion formation in a rat uterine horn model by nimesulide: a seletive COX-2 inhibitor. Hum Reprod. 2001;16:1732-5.
- 22. Kappas AM, Barsoum GH, Ortiz JB, Keighley MR. Prevention of peritoneal adhesions in rats with verapamil, hydrocortisone sodium succinate, and phosphatidylcholine. Eur J Surg. 1992;158(1):33-5.
- 23 Belluco C, Meggiolaro F, Pressato D, Pavesio A, Bigon E, Donà M et al Prevention of postsurgical adhesions with an autocrosslinked hyaluronan derivative gel. J Surg Res. 2001;100(2):217-21.
- 24. Watson A, Vandekerckhove P, Lilford R. Liquid and fluid agents for preventing adhesions after surgery for subfertility. Cochrane Database Syst Rev. 2000;3:CD001298.
- 25. Yoldemir T, Sagol S, Adakan S, Oztekin K, Ozsener S, Karadadas N. Comparison of the reduction of postoperative adhesions by two barriers, one solution, and two pharmacological agents in the rat uterine model. Fertil Steril. 2002;78(2):335-9.
- 26 Avital S, Bollinger TJ, Wilkinson JD, Marchetti F, Hellinger M, Sands LR. Preventing intra-abdominal adhesions with polylactic acid film: an animal study. Dis Colon Rectum. 2005;48:153-7.
- 27. Wiseman DM, Trout JR, Franklin RR, Diamond MP. Metaanalysis of the safety and efficacy of an adhesion barrier (Interceed TC7) in laparotomy. J Reprod Med. 1999;44(4):325-31.
- 28. Hellebrekers BW, Trimbos-Kemper GC, van Blitterswijk CA, Bakkum EA, Trimbos JB. Effects of five different barrier materials on postsurgical adhesion formation in the rat. Hum Reprod. 2000;15(6):1358-63.
- 29. Gomel V, Urman B, Gurgan T. Pathophysiology of adhesion formation and strategies for prevention. J Reprod Med. 1996;41:35-41.
- 30. Hemadeh O, Chilokuri S, Bonet V, Hussein S, Chaudry IH. Prevention of peritoneal adhesions by administration of sodium carboxymethyl cellulose and oral vitamin E. Surgery. 1993;114:907-10.
- 31. Kagoma P, Burger SN, Seifter E, Levenson SM, Demetriou AA. The effect of vitamin E on experimentally induced peritoneal adhesions in mice. Arch Surg. 1985;120(8):949-51.
- 32. Dereska N, McLemore EC, Tessier DJ, Bash DS, Brophy CM. Short-term, moderate dosage vitamin E supplementation may have no effect on platelet aggregation, coagulation profile, and bleeding time in healthy individuals. J Surg Res. 2006;132:121-9.
- 33. Uzunköy A, Akinci OF, Coskun A, Aslan O, Kocyigit A. Effects of antiadhesive agents on the healing of intestinal anastomosis. Dis Colon Rectum. 2000;43(3):370-5.
- 34. Sanfilippo JS, Booth RJ, Burns CD. Effect of vitamin E on adhesion formation. J Reprod Med. 1995;40(4):278-82.
Publication Dates
-
Publication in this collection
27 Mar 2008 -
Date of issue
Feb 2008
History
-
Accepted
14 Nov 2007 -
Reviewed
17 Oct 2007 -
Received
21 Aug 2007