Abstracts
PURPOSE: Peripherally inserted central catheters (PICC) have been extensively used in neonates. However, insertion of these thinnest catheters is a very delicate procedure associated with a high failure rate. In our Neonatal Surgical Intensive Care Unit, we developed a very easy new PICC insertion and evaluated the neonates treated with PICCs which were inserted by using our technique as well as catheter features such as success rate, number of insertion attempts, reason for removal and complications. METHODS: Information was retrospectively collected on all 40 PICCs inserted at Kutahya Evliya Celebi Goverment Hospital and Dicle University Hospital during a 6-years period from September 2004 to September 2010. RESULTS: A total of 40 PICCs were inserted in 37 patients (26, 70% males, 11, 30% females) by using new technique. The median age of patients was 8.3 days (range 1 to 66 days) and the median weight of patients was 2365 g (range 600 to 5000 g). The vein most commonly accessed was long saphenous vein (85%). The length of PICCs in the body was 19.6 cm (range 5 cm to 30 cm). The tip was located in a central vein in all patients. Surgical abdomen was the most common cause for PICC insertion (38%). Duration of catheterization was 7.7±5.6 days (1-F 5.5 days, 2-F 8.6 days). Almost all of the PICCs were inserted successfully (40/42, success rate 95%) and in the first venipucture (36/42, 86%). Completion of therapy and removed after death were achieved with 87% of PICCs. Three minor complications were noted. Minor bleeding in the insertion site which was stopped via compression occurred in two neonates. Major complication was not seen. No deaths were directly attributed to PICCs use. CONCLUSION: The new insertion technique of the neonatal peripherally inserted central catheters may be one of the easiest and safest techniques, in comparison to previous techniques reported in the literature.
Catheterization; Peripheral; Techniques; Infant; Newborn
OBJETIVO: Cateteres centrais de inserção periférica (PICC) têm sido usados extensivamente em neonatos. Entretanto, a inserção destes cateteres tão finos é um procedimento muito delicado associado a uma elevada taxa de falha. Em nossa Unidade de Cuidado Intensivo Neonatal, nós desenvolvemos uma técnica muito fácil de inserção de PICC e avaliamos os neonatos tratados com PICCs que foram inseridos usando nossa técnica assim como características relacionadas ao cateter tais como taxa de sucesso, número de tentativas de inserção, razão de remoção e complicações. MÉTODOS: Informações foram coletadas retrospectivamente de todos os 40 PICCs inseridos no Kutahya Evliya Celebi Goverment Hospital e Dicle University Hospital durante um período de seis anos, desde Setembro de 2004 até Setembro de 2010. RESULTADOS: Um total de 40 PICCs foi inserido em 37 pacientes (26 homens, 70%, 11 mulheres, 30%) usando a nova técnica. A idade media dos pacientes foi de 8,3 dias (variando entre 1 e 66 dias) e a mediana do peso dos pacientes foi 2365g (variando entre 600g e 5000g). A veia mais comumente acessada foi a veia safena magna (85%). O comprimento mediano do PICC no corpo foi 19,6 cm (variando entre 5 cm e 30 cm). A ponta foi alocada em uma veia central em todos os pacientes. Cirurgia abdominal foi a causa mais comum de uso do PICC (38%). A duração do cateterismo foi 7,7±5,6 dias. Quase todos os PICCs foram inseridos com sucesso (40/42, taxa de sucesso de 95%) e na primeira venopunção (36/42, 86%). O término da terapia e a remoção após morte ocorreu em 87% dos PICCs. Foram observadas três complicações menores. Pequeno sangramento no local da inserção, que parou com compressão, ocorreu em dois neonatos. Complicações importantes não foram observadas. Nenhuma morte foi diretamente atribuída ao uso do PICC. CONCLUSÃO: A nova técnica de inserção periférica de cateteres centrais em neonatos pode ser um procedimento seguro e fácil, comparando com as técnicas previamente relatadas na literatura.
Cateterismo Periférico; Técnicas; Recém-Nascido
14 - ORIGINAL ARTICLE
TECHNICAL SKILL
Peripherally inserted central catheters in the neonatal period1 1 Research performed at Department of Pediatric Surgery, Kutahya Evliya Celebi Goverment Hospital and Dicle University Hospital, Turkey.
Cateteres centrais de inserção periférica no período neonatal
Ibrahim UygunI; Mehmet Hanifi OkurII; Selcuk OtcuIII; Hayrettin OzturkIV
IAssistant Professor, Department of Pediatric Surgery, Dicle University, Medical School, Diyarbakir, Turkey. Main author. Responsible for conception, design, intellectual and scientific content of the study. Surgical procedures and manuscript writing
IIAssistant Professor, Department of Pediatric Surgery, Dicle University, Medical School, Diyarbakir, Turkey. Acqusition and interpretation of data
IIIFull Professor, Department of Pediatric Surgery, Dicle University, Medical School, Diyarbakir, Turkey. Critical revision
IVFull Professor, Department of Pediatric Surgery, Abant Izzet Baysal University, Medical School, Bolu, Turkey. Manuscript writing. Responsible for conception and critical revision of the study
Correspondence Correspondence: Hayrettin Ozturk Abant Izzet Baysal University, Medical School, Department of Pediatric Surgery 14280 BOLU, Turkey Phone: 90 374 2534656-3220 Fax: 90 374 2534615 (hospital) ozturkhayrettin@hotmail.com
ABSTRACT
PURPOSE: Peripherally inserted central catheters (PICC) have been extensively used in neonates. However, insertion of these thinnest catheters is a very delicate procedure associated with a high failure rate. In our Neonatal Surgical Intensive Care Unit, we developed a very easy new PICC insertion and evaluated the neonates treated with PICCs which were inserted by using our technique as well as catheter features such as success rate, number of insertion attempts, reason for removal and complications.
METHODS: Information was retrospectively collected on all 40 PICCs inserted at Kutahya Evliya Celebi Goverment Hospital and Dicle University Hospital during a 6-years period from September 2004 to September 2010.
RESULTS: A total of 40 PICCs were inserted in 37 patients (26, 70% males, 11, 30% females) by using new technique. The median age of patients was 8.3 days (range 1 to 66 days) and the median weight of patients was 2365 g (range 600 to 5000 g). The vein most commonly accessed was long saphenous vein (85%). The length of PICCs in the body was 19.6 cm (range 5 cm to 30 cm). The tip was located in a central vein in all patients. Surgical abdomen was the most common cause for PICC insertion (38%). Duration of catheterization was 7.7±5.6 days (1-F 5.5 days, 2-F 8.6 days). Almost all of the PICCs were inserted successfully (40/42, success rate 95%) and in the first venipucture (36/42, 86%). Completion of therapy and removed after death were achieved with 87% of PICCs. Three minor complications were noted. Minor bleeding in the insertion site which was stopped via compression occurred in two neonates. Major complication was not seen. No deaths were directly attributed to PICCs use.
CONCLUSION: The new insertion technique of the neonatal peripherally inserted central catheters may be one of the easiest and safest techniques, in comparison to previous techniques reported in the literature.
Keywords: Catheterization, Peripheral. Techniques. Infant, Newborn.
RESUMO
OBJETIVO: Cateteres centrais de inserção periférica (PICC) têm sido usados extensivamente em neonatos. Entretanto, a inserção destes cateteres tão finos é um procedimento muito delicado associado a uma elevada taxa de falha. Em nossa Unidade de Cuidado Intensivo Neonatal, nós desenvolvemos uma técnica muito fácil de inserção de PICC e avaliamos os neonatos tratados com PICCs que foram inseridos usando nossa técnica assim como características relacionadas ao cateter tais como taxa de sucesso, número de tentativas de inserção, razão de remoção e complicações.
MÉTODOS: Informações foram coletadas retrospectivamente de todos os 40 PICCs inseridos no Kutahya Evliya Celebi Goverment Hospital e Dicle University Hospital durante um período de seis anos, desde Setembro de 2004 até Setembro de 2010.
RESULTADOS: Um total de 40 PICCs foi inserido em 37 pacientes (26 homens, 70%, 11 mulheres, 30%) usando a nova técnica. A idade media dos pacientes foi de 8,3 dias (variando entre 1 e 66 dias) e a mediana do peso dos pacientes foi 2365g (variando entre 600g e 5000g). A veia mais comumente acessada foi a veia safena magna (85%). O comprimento mediano do PICC no corpo foi 19,6 cm (variando entre 5 cm e 30 cm). A ponta foi alocada em uma veia central em todos os pacientes. Cirurgia abdominal foi a causa mais comum de uso do PICC (38%). A duração do cateterismo foi 7,7±5,6 dias. Quase todos os PICCs foram inseridos com sucesso (40/42, taxa de sucesso de 95%) e na primeira venopunção (36/42, 86%). O término da terapia e a remoção após morte ocorreu em 87% dos PICCs. Foram observadas três complicações menores. Pequeno sangramento no local da inserção, que parou com compressão, ocorreu em dois neonatos. Complicações importantes não foram observadas. Nenhuma morte foi diretamente atribuída ao uso do PICC.
CONCLUSÃO: A nova técnica de inserção periférica de cateteres centrais em neonatos pode ser um procedimento seguro e fácil, comparando com as técnicas previamente relatadas na literatura.
Descritores: Cateterismo Periférico. Técnicas. Recém-Nascido.
Introduction
Central venous access is essential in neonatal intensive care units for drug administration or parenteral nutrition. Peripherally inserted central catheters (PICC) have been extensively used in neonates since 19731-6. The insertion technique of PICCs is through-the-introducer catheter technique. In this technique, butterfly needle, splitting needle, peelable cannula, split cannula or peripheral venous cannula (PVC) are used as an introducer6-11. Peripheral insertion is safer than direct central venous puncture. However, insertion of these thinnest catheters is a very delicate procedure associated with a high failure rate in neonates especially in low birth weight infants because the diameter of the vessel is smaller than the introducer and stabilization of the introducer is too difficult6-11.
In our Neonatal Surgical Intensive Care Unit, we developed a very easy new insertion technique of the PICCs in neonates. The purpose of the present study is to evaluate the neonates treated via new insertion technique of the PICCs as well as catheter features such as average catheter life, success rate, number of insertion attempts, reasons for removal and complications.
Methods
Information was retrospectively collected on all PICCs inserted at Kutahya Evliya Celebi Goverment Hospital and Dicle University Hospital during a 6-years period from September 2004 to September 2010. PICCs were inserted primarily by the one Pediatric Surgeon (Dr. Uygun).
All insertions of PICCs were done by using our new technique which described below. In our new insertion technique is used a PICC, two PVCs and a scalpel.
PICCs insertions were attempted in neonates who at least one appropriate peripherally vein were well. Percutaneously femoral vein catheterization initially was preferred for the neonates whose peripherally vein were not well12. Before insertion of the PICCs, analgesic treatment with a local anesthesia, sedation or general anesthesia were not carried out routinely because our technique is similar to PVCs insertion. But all producers are carried out under strict sterile technique.
Technique
A) Equipment and insertion technique for 2-french (F) PICC:
1- A 2-F PICC (Nutriline, Vygon GmbH, Aachen, Germany, product code: 1252.31). The lengths available are 15 or 30 cm. This catheter is packaged with a 20-gauge (G) splitting needle, 20-G peelable cannula or without introducer. We prefer its 30 cm length and without introducer.
2- A 20- and 24-G PVC (B-Cat IV Cannula, Bicakcilar AS, Istanbul, Turkey)
3- A sterile surgical blade No.11 (Beybi AS, Istanbul, Turkey)
Introducer was prepared under sterile conditions (Figure 1). First of all, the 20-G PVC was splitted from approximately 12 mm distal to proximal and cut from the bottom by using sliding blade technique (Figure 1 A-E). In this technique, previously the anterior (Figure 1 A-C) then posterior walls of PVC (Figure 1 D-E) were punctured by the sharp end of the blade No.11 with 45-degree angle on the sharp point hole of the needle style that removed to 1/3 proximal end (Figure 1B) and was slided and splitted approximately 20 mm to the bottom. Then the PVC was cut from the bottom (Figure 1F). The cut proximal end was divided into two wings (Figure 1G) and was placed over the 24-G PVC as a dilator and an introducer (Figure 1 H-I). Finally, the pre-cutsemi-split introducer (PSI) is prepared (Figure 1J).
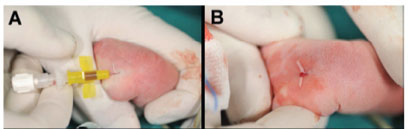
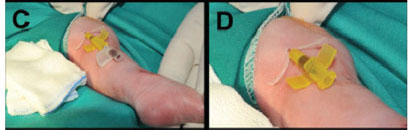
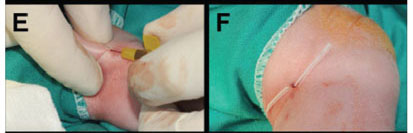
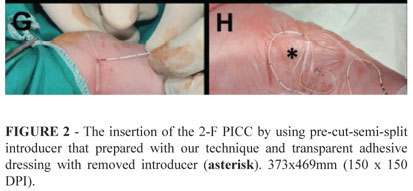
The appropriate vein whose planned insertion and distal regions have not got any venipuncture was selected. Our first preference most commonly was the long saphenous vein at the ankle because of it was the large vein and has easily cannulation, dressing, stabilization and accessing to Vena Cava (Figure 2A). Extremity of insertion side was fully prepared with povidoneiodine three times and fully inserted to hole of the sterile wrap (Figure 2A). Tourniquet was applied to distend the selected vein and immobilize extremity by assistant hand (Figure 2B). Povidone-iodine in the insertion region was cleaned with alcohol to view the selected vessel (Figure 2A). The skin slightly distal or lateral to the side of the proposed venipuncture site was punctured using an 18- or 20-G syringe needle to facilitate entry of the PSI through the skin especially in the over 2000 gr neonates. PSI was inserted through the puncture site and slowly advanced into the vein until blood flows back freely (Figure 2B). PSI was advanced a few millimeters further to ensure that the distal end is in the vein. The needle style was withdrawed a few millimeters for avoid piercing back wall of vein (Figure 2C). The PSI was advanced further until it dilated the skin and placed inside the vein fully up to PSI's wings. The needle style was removed wholly (Figure 2D). The 24-G PVC was also removed wholly while the wings of the PSI was grasped with thumb to avoid back (Figure 2E). The PSI was confirmed free backflow of the blood through it (Figure 2F). Tourniquet was removed. Then, 2-F PICC was opened, flushed with saline and advanced to the central vein through-the-PSI up to predetermined length (Figure 2G). The PSI was certainly removed wholly from the skin approximately 2-4 cm (Figure 2H). The gauze compression was applied a few minutes for the stop of the bleeding from the venipuncture site. After bleeding control, a mini gauze dressing for tamponated addictional minimal bleeding was mostly applied to venipuncture site (Figure 2H). Insertion region with the PICC, mini gauze and removed PSI was covered with a transparent adhesive dressing under strict sterile technique (Figure 2H) and inspected daily, but the dressing was not changed routinely. The catheter position was confirmed by X-Ray.
B) Equipment and insertion technique for 1-F PICCs:
1- A 1-F PICC (Premicath, Vygon GmbH, Aachen, Germany, product code: 1261.201). The lengths available are 8, 15, 20 or 30 cm. This catheter is packaged with a 24-G splitting needle, 24-G PVC, 22-G split cannula, 20-G peelable cannula or without introducer. We prefer its 20 cm length and without introducer.
2- Two 24-G PVCs (B-Cat IV Cannula, Bicakcilar AS, Istanbul, Turkey)
3- A sterile surgical blade No.11 (Beybi AS, Istanbul, Turkey)
Insertion technique for 1-F PICCs is the same for 2-F PICC's that was described above except the preparation of introducer (Figure 2, 3A-3D). Introducer was prepared using two 24-G PVC. The first PVC that needle style's removed was cut prior to 7-8 mm of the bottom as the-pre-hemi-cut PVC. Then the needle style was inserted again. The second PVC was splitted approximately 7-8 mm from distal to proximal and cut from the bottom by using sliding blade technique that described above. The cut proximal end was divided into two wings and was placed overthe-needle style in atop of the first PVC as a PSI (Figure 1J). The skin was not needed puncture to facilitate entry of the introducer through the skin (Figure 3A). After insertion of the PSI up to its wings, the needle style and also the-pre-hemi-cut PVC together was removed wholly while the wings of the PSI was grasped with thumb to avoid back (Figure 3B). Finally, 1-F PICC was opened and advanced to the vein like insertion 2-F PICC that described above (Figure 3 C-D).
At insertion, patient demographic information was recorded on a log sheet by surgeon or residents inserting the catheter. The residents monitored these catheters closely and recorded complications for the duration of catheter use on the log sheet. PICCs were used for IV fluid therapy, administration of medication, TPN solutions and blood products.
Data of the neonatal patients with PICCs which were inserted by using our new technique were collected prospectively from the log sheets and included patient age, weight, catheter features, success rate, number of insertion attempts, reason for removal and complications.
Results
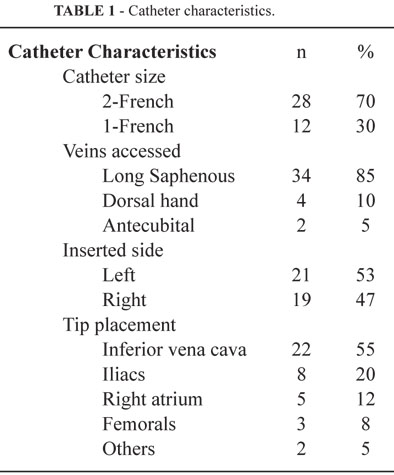
A total of 40 PICCs were inserted in 37 patients (26, 70% males, 11, 30% females) during the 6-years period by using new our insertion technique (37, 93%). The median age of patients was 8.3 days (range 1 to 66 days) and the median weight of patients was 2365 g (range 600 to 5000g). PICC size ranged from 1- to 2-F (Table 1).
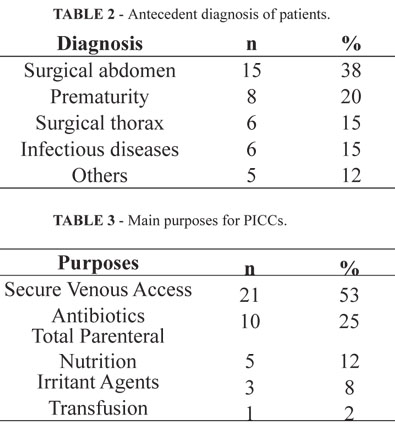
2-F PICCs were most frequently used in all ages (70%). The vein most commonly accessed was long saphenous vein (85%). The side most commonly inserted was left (53%). The length of PICCs in the body was 19.6 cm (range 5 cm to 30 cm). The tip was located in a central vein in all patients. Antecedent diagnosis and main purposes are outlined in Tables 2 and 3.
Surgical abdomen was the most common cause for PICC insertion (38%). Duration of catheterization was 7.7±5.6 days (1-F 5.5 days, 2-F 8.6 days). Almost all of the PICCs were inserted successfully (40/42, success rate 95%) and in the first venipucture (36/42, 86%). Reasons for removal of PICCs are presented in Table 4. Completion of therapy and removed after death were achieved with 87% of PICCs.
Three minor complications were noted. Minor bleeding in the insertion site which was stopped via compression and removing the PSI from the skin occurred in two neonates. In one premature, the difficulty occurred as a result of an unknown cause in the popliteal region during the removal of 1-F PICC that was inserted from the ankle long saphaneous vein and the PICC was completely removed by Cardiovascular surgeon via severe traction. Major complication was not seen. No deaths were directly attributed to PICCs use.
Discussion
PICCs are a safe and reliable vascular access device in neonates4-7. However, insertion of the PICC is a very delicate procedure associated with a high failure rate6-9. The insertion technique of PICCs is through-the-introducer catheter technique. The features of all introducers for the neonatal PICCs are presented in Chart 16-11. Our study demonstrated that our new insertion techniques of the PICCs are seemed to be one of the easiest and safest techniques in neonates.
As an introducer, the butterfly needles and splitting needles are rough and thick for insertion of the PICC. 19-G butterfly needle are needed for insertion of the 2-F PICC. 20-G and 24-G splitting needles are needed for insertion of the 2- and 1-F PICCs. Although the 24-G splitting needle is appropriate size for 1-F PICC, it has thick tip than 24-G PVC tip. These needles can become occluded with skin and subcutaneous tissue. Their sharp and thick points can cause extreme trauma to the vein that lead to bleeding and failing insertion of the PICC. Their handle and stabilization during the insertion of the PICC are also difficult6-8,11.
As also an introducer, the peelable cannula, split cannula or PVC are gentle than the needles and the 19- or 20-G size is appropriate for insertion of the 2-F PICC. They are easy handle, but they can thick for the neonates. 20-G peelable cannula and 22-G split cannula are also appropriate for insertion of the 1-F PICC, but they can also thick for the premature. 24-G PVC is also very appropriate for insertion of the 1-F PICC, but it is non-peelable and not totally withdrawn after insertion and so transparent dressing and stabilization become difficult.
The authors developed the most techniques to facilitate insertion of PICC6-9,13-15. Fischer described an easy method for the insertion 2-F PICC that are based on through the cut tip of the 20-G PVC as an introducer that over the 24-G PVC7. The 2-F PICC can be inserted by using this technique into the vein which the 24-G PVC can be inserted into. The Townsville method which is an alternative technique of the inserting 1-F PICC was described by Gandini8. This technique is also based on through the cut off the 24-G PVC as an introducer. Not only in Fischer's method, but also in the Townsville method are not very safe and very easy. In two methods, during the advancing the PICC, the introducer which is the cut off the PVC can be squeezed by grasper, can be removed or can be escaped into the skin. Finally, failed attempts and complications can be seen. We used to utilize previously Fischer's and the Townsville techniques for 1- and 2-F PICCs when we were residents. We always frightened from the introducer escaping into the skin. Then, we discovered and started to utilize the new our insertion technique for 2-F PICCs. We continued to use the Townsville technique to insertion of the 1-F PICCs until the major complication which was the migration and possible embolism of the introducer that was cut off 24-G PVC tip was seen in one premature who has multiple severe anomalies and after died of another reason. Then, we also discovered and started to utilize the other new our insertion technique for 1-F PICCs.
We successfully inserted 40 neonatal PICCs by using our techniques. Our techniques are very high success rate, very safe and very easy than the others insertion techniques of the neonatal PICCs6-10. While the success rate of neonatal PICCs in Fischer's technique was 83%, it was 95% in our technique7. Only three minor complication and no major complication were seen in our currently patients. Minor bleeding occurred in two neonates. They were through-the-PSI and were stopped via compression and removing the PSI from the skin. Initially, we were leaving the PSI in the skin and also vein, then not. In one premature, the difficulty occurred as a result of an unknown cause during the removal of the PICC. But, the cut off introducers without wings in Fischer's and the Townsville methods can migrate and can cause introducer embolism such as it previously was occurred in our one premature. The PSI in our technique has two wings which certainly prevent to migration into skin and embolism all the time. In addition, its wings also strongly prevent to accidental dislodgement by secured with finger during insertion. After easily insertion of PICC, the PSI was certainly removed wholly from the skin. Then, the PICC and the PSI both easily were dressed with sterile transparent dressing. All experience hands with peripheral vascular access were easily inserted the PICCs in all neonates who have well peripherally vein by using our techniques.
Our technique is very cheaper than the other techniques that required special introducer. Because, in our techniques, the only PICC line without introducer which sold cheaper than the PICC with introducer (approximately $10) and two PVC which were cheap, easy obtained and also mostly compatible with each other brands was used. We do not open the PICC until the PSI is in place within the vein because of previously opening of the PICC is already not necessary. This means that a PICC is not wasted if the vein cannot be cannulated and lower cost. In addition, our new insertion techniques are also very simplier and very cheaper than the other complex insertion of the PICCs which required additional instruments as a guide-wire, arterial or venous catheter sets, introducers or dilators6,9,10,13-15.
Conclusion
The technique of the neonatal peripherally inserted central catheters may be one of the easiest and safest techniques, in comparison to previous techniques reported in the literature.
References
1. Shaw JCL. Parenteral nutrition in the management of sick low birthweight infants. In: Gluck L, ed. Philadelphia: WB Saunders Company; 1973.
2. Puntis JW. Percutaneous insertion of central venous feeding catheters. Arch Dis Child. 1986;61(11):1138–40.
3. Soong WJ, Jeng MJ, Hwang B. The evaluation of percutaneous central venous catheters-a convenient technique in pediatric patients. Intensive Care Med. 1995;21(9):759-65.
4. Thiagarajan RR, Ramamoorthy C, Gettmann T, Bratton SL. Survey of the use of peripherally inserted central venous catheters in children. Pediatrics. 1997;99(2):E4.
5. Janes M, Kalyn A, Pinelli J, Paes B. A randomized trial comparing peripherally inserted central venous catheters and peripheral intravenous catheters in infants with very low birth weight. J Pediatr Surg. 2000;35(7):1040-4.
6. Bayley G. Technique for insertion of percutaneous central venous catheters in the newborn period. Arch Dis Child Fetal Neonatal Ed. 2003;88(3):F256-7.
7. Fischer JE, Fanconi S. Percutaneous central venous catheterization in premature infants: a method for facilitating insertion of silastic catheters via peripheral veins. Pediatrics. 1998;101(3 Pt 1):477-9.
8. Gandini D, Koh TH. A novel, simple way to insert percutaneous central venous catheters in newborn babies. J Perinatol. 2003;23(2):162-3.
9. Wald M, Happel CM, Kirchner L, Jeitler V, Sasse M, Wessel A. A new modified Seldinger technique for 2- and 3-French peripherally inserted central venous catheters. Eur J Pediatr. 2008;167(11):1327-9.
10. Pettit J. Technological advances for PICC placement and management. Adv Neonatal Care. 2007;7(3):122-31.
11. Stringer MD. Vascular access. In: Spitz L, Coran AG, eds. Rob and Smith's Operative surgery: concise pediatric surgery. London: Chapman and Hall Medical Publishers; 1999. p.1-13.
12. Wardle SP, Kelsall AW, Yoxall CW, Subhedar NV. Percutaneous femoral arterial and venous catheterisation during neonatal intensive care. Arch Dis Child Fetal Neonatal Ed. 2001;85(2):F119-22.
13. Galloway M. Using the microintroducer technique for PICC placement. Nursing. 2003;33(2):24.
14. Michel F, Dejode JM, Vialet R, Nicaise C, Thomachot L, Di Marco JN, Lagier P, Martin C. Tunneled central venous catheter for neonates: a simple technique for prolonged indwelling central catheters in intensive care. Pediatr Crit Care Med. 2007;8(1):37-9.
15. Stephenson T, Khan J. A new technique for placement of central venous catheters in small infants. J Parenter Enteral Nutr. 1993;17(5):479-80.
Received: February 10, 2011
Review: April 12, 2011
Accepted: May 16, 2011
Conflict of interest: none
Financial source: none
- 1. Shaw JCL. Parenteral nutrition in the management of sick low birthweight infants. In: Gluck L, ed. Philadelphia: WB Saunders Company; 1973.
- 3. Soong WJ, Jeng MJ, Hwang B. The evaluation of percutaneous central venous catheters-a convenient technique in pediatric patients. Intensive Care Med. 1995;21(9):759-65.
- 4. Thiagarajan RR, Ramamoorthy C, Gettmann T, Bratton SL. Survey of the use of peripherally inserted central venous catheters in children. Pediatrics. 1997;99(2):E4.
- 5. Janes M, Kalyn A, Pinelli J, Paes B. A randomized trial comparing peripherally inserted central venous catheters and peripheral intravenous catheters in infants with very low birth weight. J Pediatr Surg. 2000;35(7):1040-4.
- 6. Bayley G. Technique for insertion of percutaneous central venous catheters in the newborn period. Arch Dis Child Fetal Neonatal Ed. 2003;88(3):F256-7.
- 7. Fischer JE, Fanconi S. Percutaneous central venous catheterization in premature infants: a method for facilitating insertion of silastic catheters via peripheral veins. Pediatrics. 1998;101(3 Pt 1):477-9.
- 8. Gandini D, Koh TH. A novel, simple way to insert percutaneous central venous catheters in newborn babies. J Perinatol. 2003;23(2):162-3.
- 9. Wald M, Happel CM, Kirchner L, Jeitler V, Sasse M, Wessel A. A new modified Seldinger technique for 2- and 3-French peripherally inserted central venous catheters. Eur J Pediatr. 2008;167(11):1327-9.
- 10. Pettit J. Technological advances for PICC placement and management. Adv Neonatal Care. 2007;7(3):122-31.
- 11. Stringer MD. Vascular access. In: Spitz L, Coran AG, eds. Rob and Smith's Operative surgery: concise pediatric surgery. London: Chapman and Hall Medical Publishers; 1999. p.1-13.
- 12. Wardle SP, Kelsall AW, Yoxall CW, Subhedar NV. Percutaneous femoral arterial and venous catheterisation during neonatal intensive care. Arch Dis Child Fetal Neonatal Ed. 2001;85(2):F119-22.
- 13. Galloway M. Using the microintroducer technique for PICC placement. Nursing. 2003;33(2):24.
- 14. Michel F, Dejode JM, Vialet R, Nicaise C, Thomachot L, Di Marco JN, Lagier P, Martin C. Tunneled central venous catheter for neonates: a simple technique for prolonged indwelling central catheters in intensive care. Pediatr Crit Care Med. 2007;8(1):37-9.
- 15. Stephenson T, Khan J. A new technique for placement of central venous catheters in small infants. J Parenter Enteral Nutr. 1993;17(5):479-80.
Publication Dates
-
Publication in this collection
08 Sept 2011 -
Date of issue
Oct 2011
History
-
Received
10 Feb 2011 -
Reviewed
12 Apr 2011 -
Accepted
16 Apr 2011