Abstracts
PURPOSE: To study the intraperitoneal use of polyester with collagen and polytetrafluoroethylene meshes in the correction of total ventral wall defects in rats. METHODS: Thirty two rats were evaluated and divided randomly into four groups and underwent laparotomy and preparation of total defects of the abdominal wall. Next, the correction of the defect with the intraperitoneal placement of the chosen mesh was performed. The rats were submitted to euthanasia at 30 and 90 days after surgery. Were analyzed the macroscopic adhesions and microscopic aspects, and applied stress rupture test RESULTS: All animals showed intraperitoneal adhesions in varying degrees, with no statistical significance difference. There was no difference also between groups in the evaluation of stress rupture tests. On the microscopic aspect, the A30 group had less inflammatory reaction and less formation of granulomas and foreign body reaction that the B30 group, with significant difference. CONCLUSIONS: There was no difference in intraperitoneal adhesion and tensile rupture strength among groups. Group B30 presented granulomatous inflammatory reaction at the site of mesh attachment to the wall significantly higher than the A30.
Surgical Mesh; Polyesters; Collagen; Polytetrafluoroethylene; Tensile Strength; Wound Healing; Histology; Rats
OBJETIVO: Estudar comparativamente o uso intraperitoneal das telas de poliéster com colágeno e politetrafluoretileno na correção de defeitos totais da parede ventral em ratos. MÉTODOS: Foram avaliados 32 ratos distribuídos em quatro grupos aleatórios e submetidos à laparotomia e confecção de defeitos totais da parede abdominal. Em seguida, foi realizada a correção do defeito com a colocação intraperitoneal das telas. A eutanásia ocorreu aos 30 e 90 dias do pós-operatório. Foram analisadas as aderências macroscópicas, aspectos microscópicos e aplicado teste de tensão de ruptura. RESULTADOS: Todos os animais apresentaram aderências abdominais intraperitoneais em vários graus, sem significância estatística. Não houve diferença entre os grupos na avaliação dos testes de tensão de ruptura. Na análise microscópica o grupo A30 teve menor reação inflamatória e formação de granulomas, e menor reação do tipo corpo estranho quando comparado ao grupo B30, com resultados significativos. CONCLUSÕES: Não houve diferença significativa entre os grupos tanto em relação à formação de aderências intraperitoneais quanto à tensão de ruptura. O grupo B30 apresentou reação inflamatória e formação granulomatosa no local de fixação na parede significativamente maior que o grupo A30.
Telas Cirúrgicas; Poliésteres; Colágeno; Politetrafluoretileno; Resistência à Tração; Cicatrização; Histologia; Ratos
4 - ORIGINAL ARTICLE
WOUND HEALING
Comparative study between meshes of polyester with collagen and polytetrafluoroethylene in the repair of defects produced in abdominal wall of rats1 Correspondence: Andrea Mendes de Oliveira Naufel Av. Visconde de Guarapuava, 4125/202 80250-220 Curitiba - PR Brasil andrem.oliveira@hotmail.com
Estudo comparativo entre as telas de poliéster com colágeno e politetrafluoretileno no reparo de defeitos produzidos na parede abdominal de ratos
Andrea Mendes de Oliveira NaufelI; Nicolau Gregori CzeczkoII; Osvaldo MafafaiaIII; Jurandir Marcondes Ribas-FilhoIV; Carlos Roberto Naufel-JuniorV; Ulrich Andreas DietzVI; Carlos Hespanha Marinho-JúniorVII; Enéas Eduardo SucharskiVIII
IMaster in Surgery; Department of Surgery, FEPAR, Curitiba-PR, Brazil. Main author, conception, design and critical review of the study
IIPhD in Surgery and Associate Professor, Department of Surgery, FEPAR and Federal University of Parana (UFPR), Curitiba-PR, Brazil. Supervised all phases of the study, manuscript writing and critical revision
IIIFull Professor, Head, Department of Surgery FEPAR and UFPR, Coordinator of Principles of Surgery Postgraduate Program of FEPAR, Curitiba-PR, Brazil. Supervised all phases of the study, manuscript writing and critical revision
IVPhD in Surgery, Department of Surgery, UFPR, Parana, Brazil. Conception, design, intellectual and scientific content of the study
VMD, Surgeon, Division of Gastroenterology Surgery, University Evangelic Hospital of Curitiba (HUEC), Curitiba-PR, Brazil. Surgical technical procedures and animals care
VIPhD in Surgery and Associate Professor, Department of Surgery, FEPAR and UFPR, Curitiba-PR, Brazil. Manuscript writing and critical revision
VIIFellow Master degree, Postgraduate Program in Principles of Surgery, FEPAR, Parana, Brazil. Involved in technical procedures
VIIIGraduate student, FEPAR, Paraná, Brazil. Involved in technical procedures
Correspondence Correspondence: Andrea Mendes de Oliveira Naufel Av. Visconde de Guarapuava, 4125/202 80250-220 Curitiba - PR Brasil andrem.oliveira@hotmail.com
ABSTRACT
PURPOSE: To study the intraperitoneal use of polyester with collagen and polytetrafluoroethylene meshes in the correction of total ventral wall defects in rats.
METHODS: Thirty two rats were evaluated and divided randomly into four groups and underwent laparotomy and preparation of total defects of the abdominal wall. Next, the correction of the defect with the intraperitoneal placement of the chosen mesh was performed. The rats were submitted to euthanasia at 30 and 90 days after surgery. Were analyzed the macroscopic adhesions and microscopic aspects, and applied stress rupture test
RESULTS: All animals showed intraperitoneal adhesions in varying degrees, with no statistical significance difference. There was no difference also between groups in the evaluation of stress rupture tests. On the microscopic aspect, the A30 group had less inflammatory reaction and less formation of granulomas and foreign body reaction that the B30 group, with significant difference.
CONCLUSIONS: There was no difference in intraperitoneal adhesion and tensile rupture strength among groups. Group B30 presented granulomatous inflammatory reaction at the site of mesh attachment to the wall significantly higher than the A30.
Key words: Surgical Mesh. Polyesters. Collagen. Polytetrafluoroethylene. Tensile Strength. Wound Healing. Histology. Rats.
RESUMO
OBJETIVO: Estudar comparativamente o uso intraperitoneal das telas de poliéster com colágeno e politetrafluoretileno na correção de defeitos totais da parede ventral em ratos.
MÉTODOS: Foram avaliados 32 ratos distribuídos em quatro grupos aleatórios e submetidos à laparotomia e confecção de defeitos totais da parede abdominal. Em seguida, foi realizada a correção do defeito com a colocação intraperitoneal das telas. A eutanásia ocorreu aos 30 e 90 dias do pós-operatório. Foram analisadas as aderências macroscópicas, aspectos microscópicos e aplicado teste de tensão de ruptura.
RESULTADOS: Todos os animais apresentaram aderências abdominais intraperitoneais em vários graus, sem significância estatística. Não houve diferença entre os grupos na avaliação dos testes de tensão de ruptura. Na análise microscópica o grupo A30 teve menor reação inflamatória e formação de granulomas, e menor reação do tipo corpo estranho quando comparado ao grupo B30, com resultados significativos.
CONCLUSÕES: Não houve diferença significativa entre os grupos tanto em relação à formação de aderências intraperitoneais quanto à tensão de ruptura. O grupo B30 apresentou reação inflamatória e formação granulomatosa no local de fixação na parede significativamente maior que o grupo A30.
Descritores: Telas Cirúrgicas. Poliésteres. Colágeno. Politetrafluoretileno. Resistência à Tração. Cicatrização. Histologia. Ratos.
Introduction
Hernias are common complications after abdominal surgical procedures, with a prevalence of 11% to 20% and complications can arise from their presence, such as incarceration (6% to 15%) or strangulation of intestinal contents (2%)1.
The treatment of incisional hernias is with surgery. The use of synthetic prostheses in the repair of hernias began a new chapter in surgical treatment, and can serve both, as reinforcement of a suture or as a substitute for deficient tissues2.
Currently, the most commonly used prostheses are made of polypropylene. They have some disadvantages, such as the formation of intraperitoneal adhesions3,4, obstructions and intestinal fistulas5.
The ventral hernia repair with meshes has resulted in a low rate of recurrences, but when contact with the viscera with the prosthesis can not be avoided, there is a large inflammatory response with peritoneal complications. In order to minimize adhesions and maintain resistance, alternatives have been developed for polypropylene, with the introduction of polytetrafluoroethylene, polypropylene/poligalactina, double side polypropylene/carboxymethyl cellulose and polyester/polyethylene glycol-glycerol collagen meshes6.
Prior experimental study in the research line of substitute to abdominal wall in Principles of Surgery Postgraduate Program compared Parietex® and Surgisis®7, the one of polyester and absorbable collagen-elastin/polipropilene8, the polyester with collagen and polypropylene with polyglycolic acid9. One study used the meshes of polipropilene/poliglecaprone and polypropylene/polydioxanone/oxidized regenerated cellulose10.
The objective of this study was to compare the use of intraperitoneal meshes of polyester with collagen and polytetrafluoroethylene in total correction of ventral wall defects in rats, evaluating macroscopically the wound; the presence of intraperitoneal adhesions and complications in wound healing; the maximum breakdown of tissue; the evolution of the microscopic wound healing.
Methods
This is an experimental, prospective and comparative study conducted at the Postgraduate Program in Principles of Surgery, Evangelic Faculty of Parana/ University Evangelic Hospital of Curitiba and was approved by the Research Ethics Committee in Animals of the institution.
Were used 32 Wistar rats (Rattus Norvegicus) males with 90 days old and weight ranging between 350g and 450g. In this period they received food ration for the species and had free access to water.
The meshes used were: 1) polyester-collagen-polietilenoglicoglicerol (Parietex Covidien, USA) composed of two layers, one measuring 2 mm in thickness, nonabsorbable reticular and pore size of 3 mm madeof polyester, and another thin laminar layer, absorbable, gelatin, hydrophilic and comprised of collagen-polietilenoglicoglicerol to be in contact abdominal viscera, and two of polytetrafluoroethylene (Gore Infinit®, WL Gore & Associates, United States) macroporous, non-absorbable, and consisting of flat monofilament fibers of expanded polytetrafluoroethylene (PTFE).
The animals were divided in four random groups named: 1) Group A30, in which was used to polyester with collagen mesh and euthanized at day 30 after surgery; 2) Group B30, in which was used polytetrafluoroethylene and euthanasia on the 30th postoperative day; 3) Group A90, in which was used the polyester mesh with collagen and euthanasia on day 90 after surgery; 4) Group B90, in which was used to mesh of polytetrafluoroethylene and euthanasia on day 90 after surgery.
The animals underwent anesthesia with the use of hydrochloride of ketamine (50 mg/kg) and xylazine (10 mg/kg) intraperitoneally11..
One median incision of about 3 cm was done with dissection of cellular subcutaneous tissue lateral to right of incision about 2 cm. In this topography was produced a total defect of the wall abdominal as a rectangle of 1.5 x 2 cm in order to create a muscular defect and not only on the line alba.
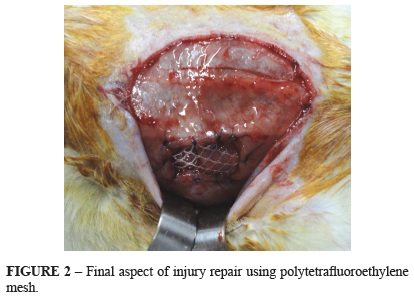
In 16 rats the polyester with collagen was fixed intraperitoneally, with the face coated of collagen glycol-glycerol in contact with the peritoneal cavity. On the other 16 animals was used the polytetrafluoroethylene mesh. They were fixed with simple suture using polypropylene 4.0 (Figures 1 and 2). For the synthesis of skin was used nylon 4.0 in continuous suture.
The analgesia was done with morphine in dose of 2.5 mg/kg subcutaneously. The animals were observed clinically dayly until euthanasia.
The euthanasia was held in gas chamber with the use of dioxide of carbon. After, was observed the aspect of wound, the presence of infection and erosions of mesh to the skin. In peritoneal cavity was evaluated the formation of adhesions between the organs and the wall, classified by Nair et al.12.
The resected specimen was divided into two parts. The right one was introduced in 30 ml of 0.9% saline solution and transferred to the tensiometry; and the left was fixed in cardboard dipped in 10% formalin and sent to microscopic analysis.
The tensiometry evaluated of measure of maximum deformity of tissue and the break tension in Newton per square centimeter (N/cm2) (EMIC, DL30000N model). The surgical specimen was fixed by its ends (cranial and caudal) and submitted to tensile force with speed of 3 mm/minute, till material break. All the procedure was registered on microcomputer in graphic by software Tesc version 1:10 with the value in N/cm 2 of force achieved on time of deformation and rupture.
Histology was realized by coloring the material with hematoxylin-eosin and Masson. Were evaluated the inflammatory process, presence of granulomatous reaction and foreign body reaction, classified as absent, mild, moderate and severe.
The results were compared in each time of evaluation by t-Student´s test to independent samples or by non parametric Mann-Whitney test. In relationship to nominal dichotomous qualitative variables was considered the Fisher´s test for the comparison mesh types in each moment of evaluation.
Results
Operative procedures adequately passed, with adequate anesthesia and surgical time in averaged 30 minutes for each animal. All animals showed good post-operative evolution. From the 32 operated animals, one died on first day post-operatively (Group A). One of Group B30 had abscess of wound and another of Group B30 had skin erosion at mesh site.
All the animals showed intra-abdominal adhesions, predominantly grades II and III (Figure 3).
Table 1 shows intraperitoneal adhesions that occurred in varying degrees. There was no statistic significant difference between groups (p=1).
Comparing the groups A30 and B30, no difference in the tensile strength of tissue (p=0.263) (Figure 4) and maximum deformity (p=0.132) (Figure 4B) was found.
Comparing the groups A90 and B90, no difference in the tensile strength of tissue (p=0.127) or the maximum tissue deformity (p=0529) (Figure 5) was found.
In assessing the inflammatory reaction after 30 days of operation, four animals in Group A30 were absent or slight inflammatory reaction, and three moderate or severe. In the B30 group all animals had moderate or severe reaction, which was statistically significant in the comparison between groups (p=0.026) (Figure 6).
In assessing the inflammatory reaction after 90 days of operation two animals in group A90 had absent or mild inflammatory reaction, and six moderate or severe reaction. One B90 animal had absent or mild a reaction and seven had moderate or severe reaction, with no statistic significant difference in the comparison between groups (p=1) (Figure 7).
In assessing the formation of granulomas and foreign body reaction after 30 days, six animals in Group A30 were classified as absent or mild, and one with moderate or severe reaction. In Group B30 one animal had absent or mild reaction and seven moderate or severe reaction, which was statistically significant in comparison between groups (p=0.010).
In 90 days groups, six animals of Group A90 had granuloma formation and foreign body reaction absent or mild and two moderate or severe. In the Group B90, three animals showed absent or mild reaction and five moderate or severe reaction. In the comparison between Groups A90 and B90 no difference in the formation of granulomas and foreign body reaction of tissues were found (p=0.315).
Discussion
Incisional hernia is a frequent complication in abdominal surgery. In US three to four million laparotomies are performed by year with 200,000 incisional hernias appearing among them13.
There are several techniques to repair hernias of wall abdominal14, but not all are applicable to big hernias. Generally at the end of the operation there is great tension in the suture line and the suture is done in tissues of poor quality. The edge-to-edge repair of the defect of wall abdominal it is many times impossible or maintains inadequate tension, favoring recurrences2.
The intraperitoneal prostheses offer more advantages including the limited need in dissecting the intermediaries plans with less bleeding (only 5% of hematoma or seroma2), and reduction of operative time especially when they are placed by laparotomy15.
An experimental study in pigs using three different meshes (Bard Mesh®, UltraPro® and Gore Infinit®) fixed pre-peritoneally in abdominal wall defects observed no differences between the meshes of polypropylene and of PTFE, suggesting that this latter can be appropriate alternative to replace the polypropylene16.
Studies already demonstrated good results with the polyester mesh with collagen, with lower inflammatory reaction and higher collagen formation7-9. The tension test comparing the polypropylene/polypropylene and polyglecrapone/polydioxanone/oxidized regenerated cellulose, found no difference between the meshes10.
The structure of the prostheses and the design of polytetrafluoroethylene monofilament fiber mesh is the goal to reduce the potential of bacterial colonization16. In this study, was observed only one wound abscess.
Nether was found cases of relapse or fistula formation or intestinal obstructions in both groups, and despite the adhesions, no fibrosis or obstructive bowel erosion.
The adhesions are the result of exudate of fibrin and happen in any type of trauma. These exudates form temporary adhesions and can delay the healing process. Almost all meshes produce adhesions when in touch to intestine surface and it is determined by the size of pores, by structure and surface area of the mesh. The microporous mesh induces intense fibrotic reaction. Mesh of PTFE microporous has lower risk of adhesions, but it is unable of adhere tightly to abdominal wall. These facts illustrate the difficulty in producing a mesh that will adhere well to wall abdominal but not to the 17 intestine. The respect of adhesions formation this work showed no differences between the meshes compared in different moments.
It is recommended to use the polyester and polypropylene with collagen coated sodium hyaluronate/carboxymethylcellulose in hernia repair in which direct contact with the abdominal viscera can not be avoided. Study with 200 experimental rats using eight different mesh types intraperitoneally, concluded that there were no significant differences in the presence of adhesions, tissue incorporation, maximum tensile force and infection among them6.
The analysis of specimens in this study in different time of observation, showed no statistically significant differences in relation to the breakdown point and maximum deformity.
The inflammatory reaction comparing A30 and B30 groups was significantly higher on Group B30 (p=0.026), and not occurred between A90 and B90. That reflects progressive neoformation of tissues and fall of levels inflammatory and of fibrosis, in three months. As more the response inflammatory less it is the fibrinolysis, resulting in more fibroblastic activity and more adhesions formation18.
For some authors19, it is not known the time to form interface between mesh and wall abdominal with force enough to prevent the recurrence. In seven days there is significant inflammatory reaction with neoformation of tissues and it is speculated that after 12 weeks the mesh is fully incorporated in the wallIt was shown that neoformation of tissue happens quickly on the first two weeks19. This can have clinical implications in ventral hernia correction in humans, considering that 74% of the resistance was be reached after two weeks.
These results also corroborates with the recent findings in pigs with defects corrected pre-peritoneally with three different meshes (Bard Mesh®, Ultrapro® and Gore Infinit®). Histologically, the inflammation decreased with time and the incorporation to tissues increased in all the meshes. The authors suggest that the PTFE monofilament mesh can become alternative to polypropylene.
In a comparative study between Parietex® and Surgisis®, the first presented less amount of acute (eosinophils) and chronicle (macrophages) inflammatory reaction than the Surgisis®7.
The porosity is the main determinant of tissue reaction. Poros must be higher than 75 µm to allow the infiltration of macrophages, fibroblasts, vessels and collagen. Meshes with larger pores permit the growth of soft tissues and are more flexible. Granulomatous reaction normally is formed inter fibers as part of reaction of foreign body17..
Comparing the meshes, Group B30 showed presence of granulomas and foreign body reaction significantly higher than group A30 (p=0.010), which was not observed when comparing groups A90 and B90.
In conclusion, the comparative evaluation between the polyester with collagen and polytetrafluoroethylene meshes on the repair of defects of ventral wall of rats showed: 1) no significant difference in relation to the formation of intraperitoneal adhesions after 30 and 90 days of the surgery; 2) the breakdown point and the maximum deformation of the whole mesh/tissue material showed no significant difference in the groups; 3) the group B30 presented inflammatory reaction in suture line and in the wall significantly higher than Group A30; and 4) the Group B30 presented more intense granulomas and reaction type foreign body at the site of the suture than the Group A30.
Conflict of interest: none
Financial source: none
Received: February 21, 2012
Review: April 18, 2012
Accepted: May 14, 2012
1 Research performed at Postgraduate Program, Department of Surgery, Evangelic Faculty of Parana (FEPAR), Curitiba-PR, Brazil.
- 1. Luijendijk RW, Hop WC, van den Tol MP, de Lange DC, Braaksma MM, Ijzermans JN, Boelhouwer RU, De Vries BC, Salu MK, Wereldsma JC, Bruijninckx CM, Jeekel J. A comparison of suture repair with mesh repair for incisional hernia. N Engl J Med. 2000;343(6):392-8.
- 2. Briennon X, Lermite E, Meunier K, Desbois E, Hamy A, Arnaud JP. Surgical treatment of large incisional hernias by intraperitoneal insertion of Parietex(R) composite mesh with an associated aponeurotic graft (280 cases). J Visc Surg. 2011;148(1):54-8.
- 3. Goldenberg A, Matone J, Marcondes W, Herbella FA, Farah JF. Comparative study of inflammatory response and adhesions formation after fixation of different meshes for inguinal hernia repair in rabbits. Acta Cir Bras. 2005;20(5):347-52.
- 4. Salameh JR, Talbott LM, May W, Gosheh B, Vig PJ, McDaniel DO. Role of biomarkers in incisional hernias. Am Surg. 2007;73(6):561-7; discussion 7-8.
- 5. Greenawalt KE, Butler TJ, Rowe EA, Finneral AC, Garlick DS, Burns JW. Evaluation of sepramesh biosurgical composite in a rabbit hernia repair model. J Surg Res. 2000;94(2):92-8.
- 6. Burger JW, Halm JA, Wijsmuller AR, ten Raa S, Jeekel J. Evaluation of new prosthetic meshes for ventral hernia repair. Surg Endosc. 2006;20(8):1320-5.
- 7. Baroncello JB, Czeczko NG, Malafaia O, Ribas-Filho JM, Nassif PA, Dietz AU. The repair of abdominal defects in rabbits with Parietex and Surgisis meshes abdominal wall. Arq Gastroenterol. 2008;45(4):323-9.
- 8. Schulz DD, Czeczko NG, Malafaia O, Schulz GJ, Czeczko LE, Garcia LS, Dietz UA. Evaluation of healing prosthetic materials polyester mesh resorbable film and collagen elastin matrix /polypropylene used in rabbits abdominal wall defects. Acta Cir Bras. 2009;24(6):476-83.
- 9. Araújo UR, Czeczko NG, Ribas-Filho JM, Malafaia O, Budel VM, Balderrama CM, Zimmermann E, Dietz UA. Intraperitoneal meshes in the repair of abdominal wall defects: comparison of polyester with collagen versus polypropylene with polyglycolic acid. Rev Col Bras Cir. 2009;36(3):241-9.
- 10. Pundek M, Czeczko N, Yamamoto C, Pizzatto R, Czeczko L, Dietz U, Malafaia O. Estudo das telas cirúrgicas de polipropileno/poliglecaprone e de polipropileno/polidioxanona/celulose oxidada regenerada na cicatrização de defeito produzido na parede abdominal de ratos. ABCD Arq Bras Cir Dig. 2010;23(2):94-9.
- 11. Damy SB, Camargo RS, Chammas R, Figueredo LFP. Aspectos fundamentais da experimentação animal - aplicações em cirurgia experimental. Rev Assoc Med Bras. 2010;56(1):103-11.
- 12. Nair SK, Bhat IK, Aurora AL. Role of proteolytic enzyme in the prevention of postoperative intraperitoneal adhesions. Arch Surg. 1974;108(6):849-53.
- 13. Bellón JM, Durán HJ. Biological factors involved in the genesis of incisional hernia. Cir Esp. 2008;83(1):3-7.
- 14. Dietz UA, Hamelmann W, Winkler MS, Debus ES, Malafaia O, Czeczko NG, Thiede A, Kuhfuss I. An alternative classification of incisional hernias enlisting morphology, body type and risk factors in the assessment of prognosis and tailoring of surgical technique. J Plast Reconstr Aesthet Surg. 2007;60(4):383-8.
- 15. Benchetrit S, Debaert M, Detruit B, Dufilho A, Gaujoux D, Lagoutter J, Lepere M, Martin Saint Leon L, Pavis d'Escurac X, Rico E. Laparoscopic and open abdominal wall reconstruction using Parietex meshes: clinical results on 2700 hernias. Hernia. 1998;2:57-62.
- 16. Melman L, Jenkins ED, Hamilton NA, Bender LC, Brodt MD, Deeken CR, Greco SC, Frisella MM, Matthews BD. Histologic and biomechanical evaluation of a novel macroporous polytetrafluoroethylene knit mesh compared to lightweight and heavyweight polypropylene mesh in a porcine model of ventral incisional hernia repair. Hernia. 2011;15(4):423-31.
- 17. Brown CN, Finch JG. Which mesh for hernia repair? Ann R Coll Surg Engl. 2010;92(4):272-8.
- 18. Gonzalez R, Rodeheaver GT, Moody DL, Foresman PA, Ramshaw BJ. Resistance to adhesion formation: a comparative study of treated and untreated mesh products placed in the abdominal cavity. Hernia. 2004;8(3):213-9.
- 19. Majercik S, Tsikitis V, Iannitti DA. Strength of tissue attachment to mesh after ventral hernia repair with synthetic composite mesh in a porcine model. Surg Endosc. 2006;20(11):1671-4.
Publication Dates
-
Publication in this collection
27 June 2012 -
Date of issue
July 2012
History
-
Received
21 Feb 2012 -
Accepted
14 May 2012 -
Reviewed
18 Apr 2012