Abstracts
PURPOSE: To analyze the behavior of cardiopulmonary function in postoperative of laparoscopic Nissen fundoplication. METHODS: Thirty-two patients, 13 males (41%) and 19 females (59%), were evaluated. Their age ranged from 25 to 67 years, with a mean of 44.4 ± 10.9. Pulmonary volumes, respiratory pressures and exercise tests were performed in the preoperative period (PRE) and in the first (PO1), second (PO2), fifth (PO5) and thirtieth (PO30) postoperative periods. RESULTS: Thirty-two patients were evaluated, of whom 59% were females. Mean age was 44.4 ± 10.9 years. Lung volumes had significant decrease at PO1 and PO2 and were similar to PRE values at PO5. Respiratory pressures were altered only at PO1. The distance covered in the 6-minute walk test had significant reduction until PO2, and climbing time in the stair-climbing test significantly increased at PO2. CONCLUSION: Patients submitted to LNF surgery have decreased cardiorespiratory function in the early postoperative period; however, they soon return to preoperative conditions.
Gastroesophageal reflux disease; Videolaparoscopy; Pulmonary function; Exercise testing; Cardiopulmonary function
OBJETIVO: Analisar o comportamento da função cardiopulmonar no pós-operatório de fundoplicatura Nissen laparoscópica. MÉTODOS: Trinta e dois pacientes, 13 homens (41%) e 19 mulheres (59%) foram avaliados. A idade variou de 25 to 67 anos, com media de 44.4 ± 10.9. Os volumes pulmonares, as pressões respiratórias e testes de exercício foram realizados no período pré-operatório (PRE) e no primeiro (PO1), segundo (PO2), quinto (PO5) e trigésimo (PO30) períodos pós-operatórios. RESULTADOS: Trinta e dois pacientes foram avaliados, dos quais 59% eram do sexo feminino. A média de idade foi de 44,4 ± 10,9 anos. Os volumes pulmonares apresentaram diminuição significativa no PO1 e PO2 e foram semelhantes aos valores PRE no PO5. As pressões respiratórias estiveram alteradas apenas no PO1. A distância percorrida no teste da caminhada de 6 minutos apresentou redução significativa até o PO2, e o tempo de subida no teste de escada aumentou significativamente no PO2. CONCLUSÃO: Pacientes submetidos à FLN apresentaram diminuição da função cardiorrespiratória no início do período pós-operatório, no entanto, elas rapidamente regressaram às condições pré-operatórias.
Doença do Refluxo Gastroesofágico; Videolaparoscopia; Função Pulmonar; Teste de Exercício; Função Cardiopulmonar
12 - ORIGINAL ARTICLE
CLINICAL INVESTIGATION
Study on functional cardiorespiratory changes after laparoscopic Nissen fundoplication1 Correspondence Daniele Cristina Cataneo Departamento de Cirurgia e Ortopedia Disciplina Cirurgia Torácica Faculdade de Medicina de Botucatu, UNESP 18618-970 - Botucatu - SP - Brazil Tel.: (55-14) 3811-609 Fax: (55-14) 3815-7615 dcataneo@fmb.unesp.br
Estudo das alterações funcionais cardiorrespiratórias após a fundoplicatura laparoscópica à Nissen
Thaianne Cavalcante SérvioI; Rodrigo Severo de Camargo PereiraII; Daniele Cristina CataneoIII
IFellow Master Degree. Postgraduate Program in General Basis of Surgery. Botucatu School of Medicine, São Paulo State University - UNESP. Brazil. Responsible for acquisition and interpretation of data and manuscript preparation
IIPh.D. Surgeon Assistant, Division of Gastroenterological Surgery. Botucatu School of Medicine, São Paulo State University - UNESP. Brazil. Acquisition and interpretation of data
IIIPh.D. Associate Professor from Division of Thoracic Surgery. Botucatu School of Medicine, São Paulo State University - UNESP. Brazil. Conception, design, intellectual and scientific content of the study
Correspondence Correspondence Daniele Cristina Cataneo Departamento de Cirurgia e Ortopedia Disciplina Cirurgia Torácica Faculdade de Medicina de Botucatu, UNESP 18618-970 - Botucatu - SP - Brazil Tel.: (55-14) 3811-609 Fax: (55-14) 3815-7615 dcataneo@fmb.unesp.br
ABSTRACT
PURPOSE: To analyze the behavior of cardiopulmonary function in postoperative of laparoscopic Nissen fundoplication.
METHODS: Thirty-two patients, 13 males (41%) and 19 females (59%), were evaluated. Their age ranged from 25 to 67 years, with a mean of 44.4 ± 10.9. Pulmonary volumes, respiratory pressures and exercise tests were performed in the preoperative period (PRE) and in the first (PO1), second (PO2), fifth (PO5) and thirtieth (PO30) postoperative periods.
RESULTS: Thirty-two patients were evaluated, of whom 59% were females. Mean age was 44.4 ± 10.9 years. Lung volumes had significant decrease at PO1 and PO2 and were similar to PRE values at PO5. Respiratory pressures were altered only at PO1. The distance covered in the 6-minute walk test had significant reduction until PO2, and climbing time in the stair-climbing test significantly increased at PO2.
CONCLUSION: Patients submitted to LNF surgery have decreased cardiorespiratory function in the early postoperative period; however, they soon return to preoperative conditions.
Key words: Gastroesophageal reflux disease. Videolaparoscopy. Pulmonary function. Exercise testing. Cardiopulmonary function.
RESUMO
OBJETIVO: Analisar o comportamento da função cardiopulmonar no pós-operatório de fundoplicatura Nissen laparoscópica.
MÉTODOS: Trinta e dois pacientes, 13 homens (41%) e 19 mulheres (59%) foram avaliados. A idade variou de 25 to 67 anos, com media de 44.4 ± 10.9. Os volumes pulmonares, as pressões respiratórias e testes de exercício foram realizados no período pré-operatório (PRE) e no primeiro (PO1), segundo (PO2), quinto (PO5) e trigésimo (PO30) períodos pós-operatórios.
RESULTADOS: Trinta e dois pacientes foram avaliados, dos quais 59% eram do sexo feminino. A média de idade foi de 44,4 ± 10,9 anos. Os volumes pulmonares apresentaram diminuição significativa no PO1 e PO2 e foram semelhantes aos valores PRE no PO5. As pressões respiratórias estiveram alteradas apenas no PO1. A distância percorrida no teste da caminhada de 6 minutos apresentou redução significativa até o PO2, e o tempo de subida no teste de escada aumentou significativamente no PO2.
CONCLUSÃO: Pacientes submetidos à FLN apresentaram diminuição da função cardiorrespiratória no início do período pós-operatório, no entanto, elas rapidamente regressaram às condições pré-operatórias.
Descritores: Doença do Refluxo Gastroesofágico. Videolaparoscopia. Função Pulmonar. Teste de Exercício. Função Cardiopulmonar.
Introduction
The gastroesophageal reflux disease (GERD) has been defined as a chronic disorder that results from the backward flow of gastroduodenal content into the esophagus and/or adjacent organs, thus causing a variable spectrum of esophageal and/or extraesophageal symptoms and signs that are followed or not by tissue damage1.
Clinical treatment, in addition to medication, involves lifestyle change, such as those in dietary habits, stress reduction and physical activity practice. In patients with recurrence, who are intolerant to clinical treatment, and complicated GERD, surgical correction of the lower esophageal sphincter (LES) is recommended.
Several studies have shown that videolaparoscopy (VLP) has a number of advantages in relation to laparotomy, such as: pain reduction and lower consumption of analgesics in the postoperative period, smaller skin incision, reduced bleeding, smaller need for hospitalization at Intensive Care Units, fewer infectious complications, lower pulmonary dysfunction, shorter hospitalization periods and, from the viewpoint of surgical stress, it shows less trauma, as measured by stress hormones (ACTH and cortisol)2.
The pneumoperitoneum is usually performed with carbon dioxide, and it is an essential resource for VLP surgery as it enables the visualization and handling of viscera during surgical procedures3. The installation of the pneumoperitoneum must be slow, since it causes increased intra-abdominal pressure (IAP), thus leading to deleterious effects to the cardiovascular, respiratory, renal and metabolic systems4. IAP increase causes the cephalic dislocation of the diaphragm, which results in the reduction of pulmonary volumes and may lead to serious cardiorespiratory complications volumes. As IAP increases, thus allowing for an adequate surgical field, trans- and postoperative complications increase proportionally5.
Additionally, during the surgical procedure, the abdominal viscera are manipulated and, in laparoscopic Nissen fundoplication (LNF) surgery specifically, direct diaphragmatic manipulation occurs. These factors lead to the reflective inhibition of the phrenic nerve, whose afferent route originates from the sympathetic celiac plexus or another upper abdominal sympathetic ganglion, thus promoting diaphragmatic paresis6.
In the postoperative period, the most frequently expected pulmonary complication is atelectasis, which occurs in 10 to 35% of patients7 as an outcome of the abovementioned ventilation alterations. Some authors report that postoperative pain may be related to reduced vital capacity, tachypnea and superficial breathing, leading to the formation of atelectasis, although it is reduced in VLPs8.
Over the years, VLP has been increasingly used for performing most abdominal surgeries, which were previously performed by laparotomy. Hence, the need to evaluate ventilation alterations resulting from the pneumoperitoneum arose by means of a large number of studies found in the medical literature. Various tests and parameters have been evaluated in different surgery types; however, no references have been found in LNF in contrast to the large number of studies related to cholecystectomy. More specifically, no studies using strength tests, such as the 6-minute walk test (6MWT) and the stair-climbing test (SCT), or addressing the outcomes of each of the performed tests in the postoperative convalescence period were found. For this reason, through these tests, conducted at various moments (pre, first, second, fifth and thirtieth postoperative periods), we proposed to evaluate the cardiopulmonary behavior of patients submitted to LNF, since it is a more invasive surgery than cholecystectomy because it directly manipulates the diaphragm.
Methods
This study was conducted at Bauru State Hospital from April 2008 to May 2010, after approval by the Research Ethics Committee of São Paulo State University - UNESP.
All the patients with recommendation for LNF and older than 18 years were included. Thirty-two patients, 13 males (41%) and 19 females (59%), were evaluated. Their age ranged from 25 to 67 years, with a mean of 44.4 ± 10.9.
Those with previous pulmonary disease, history of unstable angina or myocardial infarction less than three months ago, decompensated heart failure, musculoskeletal, neurological or vascular alterations that could prevent deambulation, and resting heart rate higher than 120 bpm were excluded. In anamnesis, the patients were asked about their smoking habits, and a scale for measurement of usual physical activity was applied9. Weight was measured in kilograms (kg), and height in meters (m) in order to calculate the body mass index (BMI). Then, pulmonary function tests were performed (spirometry, ventilometry), respiratory muscle strength (manovacuometry) and cardiopulmonary exercise (6MWT, SCT).
Spirometry was performed by a portable Pony FX® spirometer that had been previously calibrated. The patients remained in the sitting position, using a nasal obturator according to ATS standards10 and South American guidelines11, in order to obtain their forced vital capacity (FVC), forced expiratory volume in first second (FEV1) and maximal voluntary ventilation (MVV). Ventilation was measured by a portable Wright® ventilometer that had been previously calibrated. The patients also remained in the sitting position, using a nasal obturator and breathed calmly for one minute in order to obtain minute volume (MV) and the later estimation of tidal volume (TV) through the quotient by the respiratory rate (RR). The test was repeated 3 times, and the best result was adopted as long as a variation greater than 10% did not occur. Manovacuometry was performed by an analog Salcas® manometer that had been previously calibrated, with a variation capacity of -200 to +200 cm of water. The patient again remained in the sitting position, using a nasal obturator9, in order to obtain maximal inspiratory (MIP) and expiratory (MEP) pressures. The test was repeated 3 times, and the best value was chosen as long as divergence did not exceed 5%. The predicted values were calculated by using the equations proposed for the Brazilian population12.
6MWT was performed on a flat 30-meter corridor in the facilities of Bauru State Hospital, according to ATS standards13. SCT was performed on shadowed stairs in the facilities of Bauru State Hospital, according to standardization by Cataneo and Cataneo14. The patients were encouraged to climb all the cases of stairs with 12.24 meters in height as fast as possible. The test was interrupted by fatigue, intense dyspnea, thoracic pain or exhaustion. The climbing time in the stair climbing test (SCTt) was measured in seconds (s) and the patients' weight was used for estimating power (SCTP) in watts (w) by using the classic formula14.
The intra-operative period was followed by evaluating anesthetic records and surgery descriptions in order to observe surgery time and possible intra-operative complications.
The patients were followed by the same examiner, and all the previously proposed tests were repeated in the first (PO1), second (PO2), fifth (PO5) and thirtieth (PO30) postoperative periods. Only SCT was not repeated at PO1. On each postoperative day, the patients were asked about their pain level through the analog pain scale, which ranges from 0 to 10, where 0 indicates no pain, and 10 indicates unbearable pain15.
The sample's general characteristics were presented by means of descriptive statistics. In all variables, except for pain, analysis of variance for repeated measures was used, followed by the Tukey method for comparison of the means at the moments. Student's t test for dependent populations was used for the variables comparing two moments. The Friedman test was utilized for the pain scale, since the variable did not show normal distribution16. A p value >0.05 was considered statistically significant. The software used to perform all the analyses was SAS (Statistical Analysis System), version 9.2.
Results
BMI ranged from 17.4 to 40.6 with a mean of 28.4 ± 4.8 kg/m2. The sample consisted of non-smokers (75%), smokers (6%) and former smokers (19%). Twelve patients were obese (BMI > 30 Kg/m2). Mean usual physical activity was of 9.2 ± 4.7, and the patients were considered to be moderately active.
All the individuals were submitted to general anesthesia, with mean surgery duration of 152.8 ± 41.07 minutes. No postoperative complications were observed.
Spirometric variables were reduced at PO1 and PO2, and they were similar to PRE values at PO5 (Table 1). The tidal volume did not show statistical differences at any of the studied moments, and minute ventilation showed to be increased at all postoperative moments, but such increase was only significant at one of the moments (Table 1). Maximal respiratory pressures were significantly altered at PO1, and remained, but without significant difference at PO2 and, at PO5, they were already the same as PRE values (Table 1).
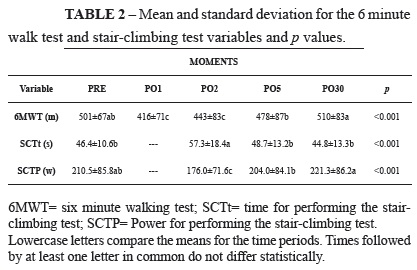
In the strength tests, it was observed that the distance covered in 6MWT showed to be significantly reduced at PO1 and PO2, but normal at PO5. The attributes of SCT (SCTt and SCTP) were altered at PO2, but showed similar values to those found in PRE at PO5 (Table 2).
Although pain at PO1 and PO2 was statistically significant in relation to PRE (p<0.001), it was mild to moderate pain, which was virtually absent at PO5.
Discussion
In our sample, there was a predominance of females, which was in agreement with others studies, where 69.5% and 64%, respectively, were females17,18.
The mean age was 44.4 years, and this was also in agreement with the literature, as it shows increased GERD prevalence associated with age over 40 years, which primarily includes the economically active population, comprising individuals that are more subject to stress and normally related to bad dietary habits17; in addition to the older population, since the ageing process promotes structural and functional modifications in the digestive system, leading to reduction in the intrinsic esophageal innervation and muscle paresis in the lower sphincter, thus increasing GERD incidence. In our sample, age variation was from 25 to 67 years; therefore, most of the individuals were within the age ranges that are more prone to GERD.
Mean preoperative BMI showed that the patients were overweight. A study observed proportionality between BMI increase and reduced functional residual capacity, decreased pulmonary complacency and increased total resistance, affecting hematosis and leading to a decreased oxygenation index19. Our study did not evaluate the same data as that author's, but a linear relation between overweight and the presence of more accentuated postoperative functional pulmonary loss could be observed.
Some authors found a direct association between mean surgery duration over 210 minutes and a higher incidence of pulmonary complication in the postoperative period following abdominal surgery20. Hence, the short surgery duration in our study may not have been sufficient to lead to important pulmonary alterations.
Postoperative pain is cited as a significant cause of ventilatory deficiency, since it limits good pulmonary expansibility, resulting in superficial breathing and tachypnea, which, in turn, contributes to atelectasis formation. Additionally, pain hinders early mobility and deambulation in the immediate postoperative period. These activities help alveolar clearance and prevent pulmonary complications8. In our patients, pain was significant until PO2, which showed the importance of maintaining analgesia and respiratory physiotherapy during this period so as to prevent pulmonary complications. Thus, pulmonary expansibility was not reduced, as observed by the maintenance of PRE TV at all postoperative moments.
FVC and FEV1 were reduced at PO1 and PO2 and returned to PRE values at PO5. Such values were similar to those found in the literature in VLP-similar surgeries21,22, thus pointing out the restrictive characteristic of postoperative ventilatory disorders. MVV showed relevant reduction at PO1 and PO2, which was greater than that found in the literature23. There was a tendency to MV increase in the early postoperative period, and it was significant only at PO2. That occurred due to both TV increase and f increase at these moments because, although these differences were not isolatedly important in relation to PRE values, they resulted in a significantly higher value when multiplied. A greater demand from the organism seems to have occurred, which was probably in order to supply a greater metabolic demand in PO, contrarily to what was observed in the literature21,22, where mean reductions of 20% and 18% were found for MV, and of 26% and 28% were observed for TV at PO1, thus suggesting that these variables showed reduction in PO that resulted from pulmonary complacency reduction and microatelectasis formation. Such disagreement in relation to our study may have occurred due to the fact that surgery duration was not very long or due to the intensive care provided to our patients with the purpose to prevent microatelectasis.
Several studies have evaluated MIP and MEP in the postoperative period of VLP and showed important reductions in these variables ranging from 26% to 47%, respectively in the immediate postoperative period21,22. In our study, smaller alteration was observed for both MIP and MEP, but it was not less relevant as regards the compromising of inspiratory or expiratory respiratory muscle strength. Respiratory muscle dysfunction is related to general anesthesia, tracheal intubation, postoperative pain and supine position in convalescence; however, the best explanation for such alteration is related to diaphragmatic paresis resulting from the reflective inhibition of the phrenic nerve6. There was also a concern about evaluating inspiratory and expiratory muscle strength in relation to the values predicted for the patients, and it was observed that, in PRE, MIP in percentage of the predicted value was already slightly reduced if values above 80% of the prediction were considered to be normal.
At the first two postoperative moments analyzed, reduction in 6MWT was evident, but these values tended to normalize at PO5. As observed in our sample, the 6MWT mean in the postoperative period was of approximately 500m, and this value was higher than 80% of the predicted figure24, which shows these patients' small probability to present postoperative complications according to this parameter. Even at the postoperative moment when 6MWT was smaller, that mean surpassed 400m, and at PO5, it already showed values that were not significantly different from those found in PRE. This fact may be closely related to the absence of postoperative cardiopulmonary complications in our sample.
Similarly, the medical literature relates SCT to cardiorespiratory performance, and there is a linear relation between SCT and oxygen consumption (VO2), which, in turn, proportionally characterizes an individual with higher or lower risk for postoperative complications. Retrospective studies have concluded that patients who were incapable of climbing more than 2 stair cases in the preoperative period showed 82% of risk for postoperative pulmonary complications25. Cataneo et al26 reported that patients who took up to 40 seconds to climb 12.16 meters were very likely to show VO2 above 25 mL/kg/min, which is a value that corresponds to low surgical risk. Power, which also considers patient weight to measure exercise performance, shows lower accuracy than the time variable in SCT14. In our results, power in the preoperative period was slightly higher than 200 w, and according to previous studies14, it would be reasonable to admit the probability that VO2 was approximately 25 ml/kg/min, whereas for SCTt, such value was a little lower. Such difference can be explained by the patients' overweight, since power is directly proportional to an individual's body mass. Therefore, by considering the two variables, SCTt and SCTP, the PRE VO2 mean for these patients would be approximately 25 ml/kg/min, with very low cardiopulmonary risk even for laparotomy, and even at PO2, where SCT was mostly affected; the mean VO2 calculated by the 2 variables was not below 20 ml/kg/min, a value that still keeps surgical risk low in case reoperation is performed at these moments.
These strength tests could be used as indicators for more intense preoperative physical preparation27 in patients showing low exercise capacity. In the group of patients in this study, there was a performance reduction of approximately 20% on the first postoperative days; therefore, in borderline patients, with high cardiorespiratory risk, contribution from physiotherapy would be important until PO5, from which these patients would already be more able to perform their routine activities.
Conclusion
Both respiratory function static tests and cardiopulmonary strength tests show significant reduction in the early postoperative period following LNF surgery, but these values are already normal on the fifth postoperative day.
Conflict of interest: none
Financial source: none
Received: February 10, 2012
Review: April 11, 2012
Accepted: May 14, 2012
1 Research performed at Bauru State Hospital, Part of Fellow Master degree thesis, Postgraduate Program in General Basis of Surgery, Botucatu School of Medicine, São Paulo State University - UNESP, Bauru-SP,Brazil.Tutor: Daniele Cristina Cataneo
- 1. Moraes Filho J, Cecconello I, Gama-Rodrigues J, Castro L, Henry MA, Meneghelli UG. Brazilian consensus on gastroesophageal reflux disease: proposals for assessment, classification and management. Am J Gastroenterol. 2002;97:241-8.
- 2. Crema E, Silva PL, Silva GM, Rodrigues Junior V, Gomes RAS. Operação do refluxo gastro-esofágico isolada ou associada à colecistectomia: avaliação do estresse cirúrgico pela dosagem hormonal e de citocinas. Rev Col Bras Cir. 2006;33(3):151-5.
- 3. Bongart FS, Pranin N, Liu Y, Lippmam M, Davis I, Klein S. Using helium for insufflation during laparoscopy. JAMA. 1991;266:3131-4.
- 4. Richardson J, Trinkle J. Hemodynamic and respiratory alterations with increased intra-abdominal pressure. J Surg Res. 1976;20:410-4.
- 5. Mergh ACM, Oliveira CHS. Alterações pulmonares na cirurgia videolaparoscópica. Rev Bras Anestesiol. 1996;46(4):289-94.
- 6. Dureuil B, Contineau JP, Desmonts JM. Effects off upper or lower abdominal surgery on diaphragmatic function. Br J Anaesth. 1987;59:1230-5.
- 7. Schauer PR, Luna J, Ghiatas AA, Glen ME, Warren JM, Sirunek K. Pulmonary function after laparoscopic cholecystectomy. Surg. 1993;114:389-99.
- 8. Cohen RV, Filho JCP, Schiavon CA, Correa JLL. Alterações sistêmicas e metabólicas da cirurgia laparoscópica. Rev Bras Videocir. 2003;1(2):77-81.
- 9. Pate RR, Pratt M, Blair SN, Haskell WL, Macera CA, Bouchard C et al. Physical activity and public health: A recommendation from the Centers for Disease Control and Prevention and the American College of Sports Medicine. JAMA. 1995;273:402-7.
- 10. American Thoracic Society. Standardization of spirometry. Am J Respir Crit Care Med. 1995;152:2185-98.
- 11. Sociedade Brasileira de Pneumologia e Tisiologia. Diretrizes para testes de função pulmonar. J Pneumol. 2002; 28(Suppl 3):2-237.
- 12. Neder JA, Andreoni S, Lerário MC, Nery LE. Reference values for lung function tests. II. Maximal respiratory pressures and voluntary ventilation. Braz J Med Biol Res. 1999;32:719-27.
- 13. American Thoracic Society. Guidelines for the six minute walk test. Am J Respir Care Med. 2002;166:111-7.
- 14. Cataneo DC, Cataneo AJM. Accuracy of the stair-climbing test using maximal oxygen uptake as the gold standard. J Bras Pneumol. 2007;33:128-33.
- 15. Ferraz MB, Quaresma MR, Aquino LR, Atra E, Tugwell P, Goldsmith CH. Reliability of pain scales in the assessment of literature patients with rheumatoid arthritis. J Rheumatol. 1990;17(8):1022-4.
- 16. Fisher LD. Biostatistics - A Methodology for the Health Sciences. Wiley-interscience, New York, 1993, 991p.
- 17. Pastore R, Crema E, Silveira MDC, Presoto AF, Herbella FAM, Del Grande JC. Eletromanometria esofágica e pHmetria de 24 horas na avaliação pós-operatória da hiatoplastia e válvula anti-refluxo total laparoscópica. Arq Gastroenterol. 2006;43(2):112-6.
- 18. Corrêa MCCSF, Lerco MM, Henry MACA. Estudo de alterações na cavidade oral em pacientes com doença do refluxo gastroesofágico. Arq Gastroenterol. 2008;45(2):132-6.
- 19. Pelosi P, Croci M, Ravagnan I et al. The effects of body mass on lung volumes, respiratory mechanics, and gas exchange during general anesthesia. Anesth Analg. 1998;87:654-60
- 20. Pereira EDB, Faresin SM, Juliano Y, Fernandes ALG. Fatores de risco para complicações pulmonares no pós-operatório de cirurgia abdominal alta. J Pneumol. 1996;22:19-26.
- Chiavegato, L.D., Jardim.J.R., Faresim S.M., Juliano. Y. Functional respiratory changes in laparoscopic cholecystectomy J Bras Pneumol. 2000;26(2):69-73.
- 21. Paisani DM, Chiavegato LD, Faresin SM. Lung volumes, lung capacities and respiratory muscle strength following gastroplasty. J Bras Pneumol. 2005;31(2):125-32.
- 22. Moulim MCB; Miguel GPS; Forti EMP; Costa D. Comparação entre inspirometria de incentivo e pressão positiva expiratória na função pulmonar após cirurgia bariátrica. Fisioter Pesq. 2009;16( 2):166-72.
- 23. Enright PL, Sherrill DL. Reference equations for the six-minute walk in healthy adults. Am J Respir Crit Care Med. 1998;158:1384-7.
- 24. Girish M, Trayner E, Dammann O, Pinto-Plata V, Celli B. Symptom-limited stair climbing as a predictor of postoperative pulmonary complications. Chest. 2001;1147-51.
- 25. Cataneo DC, Kobayasi S, Carvalho LR, Paccanaro RC, Cataneo AJM. Accuracy of six minute walk test, stair test and spirometry using maximal oxygen uptake as gold standard. Acta Cir Bras. 2010;25(2): 194-200.
- 26. Galvan CCR, Cataneo AJM. Effect of respiratory muscle training on pulmonary function in preoperative preparation of tobacco smokers. Acta Cir Bras. 2007;22(2):98-104.
Publication Dates
-
Publication in this collection
27 June 2012 -
Date of issue
July 2012
History
-
Received
10 Feb 2012 -
Accepted
14 May 2012 -
Reviewed
11 Apr 2012