Abstract
PURPOSE:
To measure the change in the minimum alveolar concentration of isoflurane (EtISO) associated with epidural nalbuphine and the postoperative analgesic requirements in dogs after ovariohysterectomy.
METHODS:
Twenty four healthy female dogs were randomly assigned to receive saline or nalbuphine at 0.3 or 0.6 mg/kg (n=8 for each group) administered via lumbosacral epidural catheter introduced cranially into the epidural canal. Changes in heart and respiratory rates and arterial blood pressure during surgery were recorded along with the corresponding EtISO. Immediately after tracheal extubation, analgesia, sedation, heart rate, respiratory rate, and arterial blood pressure were measured at predetermined intervals and every 60 min thereafter until the first rescue analgesic.
RESULTS:
A significant decrease in EtISO was associated with epidural nalbuphine at 0.3 mg/kg (26.3%) and 0.6 mg/kg (38.4%) but not with saline in ovariohysterectomized dogs. In the postoperative period, VAS and Colorado analgesic scores were lower for the dogs that received the higher nalbuphine dose, which only required supplemental analgesia 10 h following its administration, compared with dogs that received the lower dose.
CONCLUSION:
Epidural nalbuphine significantly reduces the intra-operative isoflurane requirement and provides prolonged postoperative analgesia after ovariohysterectomy in dogs.
Anesthesia; Epidural; Nalbuphine; Isoflurane; Dogs
Introduction
Epidural analgesia combined with inhalatory anesthesia may provide advantages over the conventional routes of analgesic administration (intravenous or intramuscular), including reduction of the doses of the inhalant agents required to produce anaesthesia and thus the side effects derived from higher doses11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32.. Epidural methadone in dogs undergoing pelvic limb surgical procedures resulted in greater decreases in the EtISO required to maintain anesthesia compared with the same doses administered intravenously22. Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36.. Other opioids are also used with the same goal, such as fentanyl33. Palmer CM, Cork RC, Hays R, Van Maren G, Alves D. The dose-response relation of intrathecal fentanyl for labor analgesia. Anesthesiology. 1998;88(2):355-61.
,
44. Almeida TF, Fantoni DT, Mastrocinque S, Tatarunas AC, Imagawa VH. Epidural anesthesia with bupivacaine, bupivacaine and fentanyl, or bupivacaine and sufentanil during intravenous administration of propofol for ovariohysterectomy in dogs. J Am Vet Med Assoc. 2007;230(1):45-51., sufentanil55. Cohen SE, Tan S, White PF. Sufentanil analgesia following cesarean section: epidural versus intravenous administration. Anesthesiology. 1988;68(1):129-34.
,
66. Herman NL, Sheu KL, Van Decar TK, Rubin JD, Gadalla F, Koff HD, Reynolds JE. Determination of the analgesic dose-response relationship for epidural fentanyl and sufentanil with bupivacaine 0.125% in laboring patients. J Clin Anesth. 1998;10(8):670-7., oxymorphone77. Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9., and especially morphine11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32.
,
88. Pascoe PJ, Dyson DH. Analgesia after lateral thoracotomy in dogs. Epidural morphine vs. intercostal bupivacaine. Vet Surg. 1993;22(2):141-7.
9. Marucio RL, Luna SP, Neto FJ, Minto BW, Hatschbach E. Postoperative analgesic effects of epidural administration of neostigmine alone or in combination with morphine in ovariohysterectomized dogs. Am J Vet Res. 2008;69(7):854-60.
10. Abelson AL, Armitage-Chan E, Lindsey JC, Wetmore LA. A comparison of epidural morphine with low dose bupivacaine versus epidural morphine alone on motor and respiratory function in dogs following splenectomy. Vet Anaesth Analg. 2011;38(3):213-23.
-
1111. Campoy L, Martin-Flores M, Ludders JW, Erb HN, Gleed RD. Comparison of bupivacaine femoral and sciatic nerve block versus bupivacaine and morphine epidural for stifle surgery in dogs. Vet Anaesth Analg. 2012;39(1):91-8..
Epidural use of morphine has been limited though because of the dose-dependent risk of delayed respiratory depression and/or potential urinary retention requires close monitoring of respiratory patterns, which is not always possible in dogs1111. Campoy L, Martin-Flores M, Ludders JW, Erb HN, Gleed RD. Comparison of bupivacaine femoral and sciatic nerve block versus bupivacaine and morphine epidural for stifle surgery in dogs. Vet Anaesth Analg. 2012;39(1):91-8. , 1212. Herperger LJ. Postoperative urinary retention in a dog following morphine with bupivacaine epidural analgesia. Can J Anaesth. 1998;39(10):650-2. and humans1313. Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5..
Nalbuphine is a low lipophilic (octanol-buffer partition coefficient - 9.75) semisynthetic opioid related to both oxymorphone and naloxone; it has relatively potent μ-antagonist and κ-agonist activity. The respiratory depression induced by opioids is primarily mediated by the μ-receptor agonist activity. The μ-antagonist properties of the nalbuphine should produce fewer μ-mediated side effects such as respiratory depression, pruritus, nausea and vomiting1313. Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5. , 1414. Arnould JF, Pinaud M. Pharmacology of nalbuphine. Ann Fr Anesth Reanim. 1992;11(2):221-8..
The epidural administration of nalbuphine combined with an inhalant anesthetic agent to produce the inhalant-sparing effect has not been investigated in dogs, nor has the onset and duration of action of postoperative pain relief been assessed. Therefore, we designed this study to determine if epidurally-administered nalbuphine may reduce isoflurane and postoperative analgesic requirements in dogs undergoing ovariohysterectomy that had received epidural nalbuphine.
Methods
This study was approved by the Animal Care Committee of the Federal University of Mato Grosso do Sul (UFMS) and was conducted under Good Clinical Practice guidelines. Twenty-four female dogs (ASA status 1) from the Zoonosis Control Centre of the municipality of Campo Grande to be spayed were used in this clinical trial. These animals were recruited over one year (2011-2012) and randomly assigned to one of three treatment groups. A variety of breeds were represented, with mixed-breed dogs predominating. Exclusion criteria included a body weight <15 kg or >30 kg; presence of uterine diseases, such as pyometra, dead foetuses, or canine transmissible venereal tumour (CTVT), or evidence of pregnancy; a contraindication to epidural administration (previous pelvic fractures, obesity, dermatitis at the insertion of the epidural needle or coagulopathies); and the presence of pulmonary disease as shown on thoracic radiographs. Additionally, any dog having cardiac arrhythmias, clinical signs of systemic disease, or abnormal laboratory data was excluded from the experiment.
Prior to surgery, the dogs were fasted for 12 h, and water was withheld for 3 h before the surgery. All dogs received a standardized anesthetic protocol consisting of intravenous (cephalic or saphenous vein) pre-anesthesia with acepromazine (Acepran 0.2%; Univet SA, SP, Brazil) 0.05 mg/kg administered via an over the needle catheter (BD Insyte, Becton Dickinson, Cirúrgicas Ltda, Brazil) that was placed prior to the start of the study. Anesthesia was induced with intravenous propofol (Fresofol 1%; Fresenius Kabi AB, Uppsala, Sweden), based on an expected dose of 4-6 mg/kg and given to allow endotracheal intubation. Anesthesia was maintained with isoflurane (Isoforine; Cristália Chemical and Pharmacological Products, Itapira, Brazil) delivered in 100% oxygen to a rebreathing system with a precision vaporizer out-of-the-circuit.
Mechanical ventilation was volume-controlled, with a tidal volume of 8 mL/kg and a respiratory rate set to maintain end-tidal CO2 (EtCO2) between 35 and 45 mm Hg. To maintain normocarbia, pancuronium (Pancuron, Cristália Chemicals and Pharmaceuticals, Itapira, Brazil) (0.06 mg/kg) was intravenously administered in all animals after induction of anesthesia. After completion of the surgical procedure, residual neuromuscular block was reversed using neostigmine (0.04 mg/kg) and atropine (0.02 mg/kg), intravenously. End-tidal gas was sampled from the trachea by inserting a flexible polyvinyl feeding tube through a port in the Y piece of the breathing circuit into the lumen of the endotracheal tube (Dixtal; DX 2021, Dixtal Biomédica Ind e Com, Ltda, Manaus, Brazil). The other end of the feeding tube was connected to the monitor to obtain samples that were reflective of alveolar gas concentration. The animals ' temperatures were maintained at approximately 37°C-38°C with the use of warming blankets (Ortovet; SP, Brazil). All animals received Ringer 's lactated solution (5 mL kg /hour) IV as a maintenance fluid. During the anesthetic procedure, oxygen saturation (pulseoximetry), ECG, blood pressure (oscillometry), body temperature, inspired and end-tidal carbon dioxide and isoflurane were monitored.
Once the animals were induced to anaesthesia and monitored, the surgical site clipped, and baseline measurements taken, a 20- or 18-gauge epidural needle (Perican; B Braun, São Gonçalo, Brazil) was inserted in the lumbosacral space. Correct needle placement was confirmed by the hanging-drop method and by noting no resistance during insertion of a 20- or 18-gauge epidural catheter (Portex epidural catheter, Smiths Medical ASD, Inc., Keene, NH, USA). At L4-L5 (midlumbar level), the epidural catheter was threaded about 8 to 10 cm into the epidural canal, based on the marks of the catheter and the length of the Tuohy needle inserted to reach the epidural space, with negligible resistance through the same needle site. All epidural catheter placements and injections were performed by the same blinded investigator. At the end of each epidural injection, the epidural catheter was flushed with 1 mL of saline and then removed. At the end of the instrumentation period, EtISO was maintained at 1.8%-1.9% for at least 15 min.
All injected epidural volumes were calculated based on the sum of an equivalent volume of saline plus nalbuphine or saline alone, giving a total of 0.36 mL/kg44. Almeida TF, Fantoni DT, Mastrocinque S, Tatarunas AC, Imagawa VH. Epidural anesthesia with bupivacaine, bupivacaine and fentanyl, or bupivacaine and sufentanil during intravenous administration of propofol for ovariohysterectomy in dogs. J Am Vet Med Assoc. 2007;230(1):45-51.. Twenty-four dogs were randomly assigned to one of the following treatments groups: (1) isoflurane ISO/SS, 0.36 mL/kg of epidural saline 0.9%; (2) ISO/NB3, 0.3 mg/kg of nalbuphine chloridrate (Nubain; Cristália Chemical and Pharmacological Products, Itapira, Brazil); or (3) ISO/NB6, 0.6 mg/kg of nalbuphine chloridrate. In a pilot study, a dose of 0.1 mg/kg of epidural nalbuphine was tested in two animals, but without alteration in the MAC or postoperative analgesia. All epidural injections were given 15 min after anesthetic induction, and all surgeries began within 30 min from anaesthetic induction. To improve drug diffusion, the dogs were positioned in dorsal recumbency for at least 5 min following epidural administration of the drug until the start of surgery.
In this study, the time points used to measure the EtISO that involved noxious stimulus were baseline (T0; time 0) before the administration of the drugs; (T15) after pre-anesthetic and anesthetic induction, and the EtISO was held constant for at least 15 min (stabilization period); (T30) 15 min after epidural injections; (T45; 43 ± 6 min) skin incision and subcutaneous tissue dissection; (T60; 54 ± 8 min) midline skin incision; (T75; 65 ± 10 min) left and right ovarian pedicles clamping; and (T90; 82 ± 14 min) end of the surgery.
Thirty min after saline (control) or nalbuphine epidural injections and the start of skin incision, the EtISO concentration was increased or decreased by 0.3% until the next stimulus. Approximately 10 to 15 min were allowed between stimuli for anesthetic equilibration, without positive response. An increase in heart rate ("e15%) or mean blood pressure (>100 mm Hg) within 15 min of skin incision indicated the positive response. If a negative response was detected in the first noxious stimuli step (T45, skin incision and subcutaneous tissue dissection), the EtISO concentration was reduced by 0.3% and the surgical procedure was continued until the next step. This procedure was repeated until the end of surgery. In dogs that had an initial positive response, the EtISO was increased in a reverse order to provide the necessary depth of anesthesia. The dog was required to remain stable at the lowest possible isoflurane concentration between two noxious stimulus periods. The end-tidal concentration at this time was then recorded as the final percentage of isoflurane required. All ovariohysterectomies were performed by the same surgeon, by a routine method by use of the 3-hemostats technique, and the degree of abdominal muscle relaxation (mild, moderate or intense) was evaluated during surgery by the surgeon.
After surgery, inhalant anesthetic was discontinued, with oxygen continued until spontaneous breathing resumed. Tracheal extubation was done when animals no longer tolerated the tracheal tube. All dogs were monitored for clinical signs of postoperative pain. In the control treatment and in both nalbuphine treatments, postoperative monitoring was done closely in the 90 and 120 min and every hour afterwards until 10 h from the epidural injections by the same investigator. Evaluations of analgesia and sedation were made according to the use of a visual analog scale (VAS), on which 0 represents no pain or no sedation and 10 represents to dogs with worst pain possible, and the scale proposed by the Colorado State University Veterinary Teaching Hospital1515. Hellyer PW, Gaynor JS. Acute postsurgical pain in dogs and cats. Comp Cont Edu Pract. Vet. 1998;20(2):140-53., on which 0 represents no pain and 25 the worst pain possible. The additional need for analgesic therapy in all cases in the postoperative period was determined by pain scores of 4 or higher for VAS or 10 or higher for the Colorado scale. In this case, first rescue analgesia was administered with morphine (Dimorf, 10 mg, Cristália Chemical and Pharmacological Products, Itapira, Brazil) (0.5 mg/kg intramuscularly) by the blinded observer. Additionally, patients received tramadol (Tramadon, 10 mg, Cristália Chemical and Pharmacological Products, Itapira, Brazil) (2 mg/kg orally) every 8 h for three days. Analgesia, sedation, heart rate, respiratory rate, and arterial blood pressure were measured at 90 and 120 min after the epidural injections and every 60 min thereafter until the first rescue analgesic.
Motor function was observed for the first 10 h after surgery and the disconnection of inhalant agent until the end of observation period. The dogs were encouraged to stand up and walk around by their owners and anaesthesiologists participating in the experiment. If this was not possible, the dogs were helped to a standing position. If motor function continued to be abnormal after 6 h, motor function was assessed every 2 h until normal motor function was returned as evidenced by no motor weakness, normal gait and the ability to walk unsupported. The range for return of appetite was also assessed by offering food that dogs were accustomed to eating at home. Other side effects such as vomiting, nausea, pruritus, and urinary retention were recorded during the first 12 h following the end of the surgeries in all animals.
Statistical analysis
The quantitative variables were analyzed within groups and among groups by using analysis of variance (ANOVA) for repeated measures, and the post hoc Tukey method was applied. VAS and Colorado score dependent variables were analyzed within and among groups with the nonparametric Friedman 's test (Sigma Stat II, Systat Software Inc., San Jose, USA). For all measurements, mean ± S.D. values or median ± confidence interval were determined. For all comparisons,p<0.05 was considered statistically significant.
Results
Twenty-four female dogs were randomized to three treatments as follows: eight to ISO/SS, eight to ISO/NB3, and eight to ISO/NB6. Mean duration of surgery was 45 ± 8 min (mean ± S.D.) and did not differ significantly among treatments (Table 1). A high degree of abdominal relaxation was reported in all treatments by the surgeon.
Mean ± SD values for demographic data and variables recorded during anesthesia and recovery from anesthesia in 24 dogs premedicated with acepromazine, induced with propofol and anesthetized with isoflurane that underwent ovariohysterectomy after epidural administration of one of three treatments (n=8).
The mean final EtISO requirements for the ISO/SS, ISO/NB3, and ISO/NB6 treatments, respectively, were 1.98 ± 0.10%, 1.46 ± 0.10%, and 1.22 ± 0.10% after the first noxious stimulus (T45; Table 2). EtISO was monitored throughout the anesthetic period until the end of surgery (30-90 min). These values differed significantly among treatments (p<0.05). Compared with the control treatment, EtISO decreased significantly at the time of ovarian clamp (T90) with the ISO/NB3 treatment (26.3% reduction) and with the ISO/NB6 treatment (38.4% reduction). There was a significant reduction (16.4%) between the treatments ISO/NB3 and ISO/NB6.
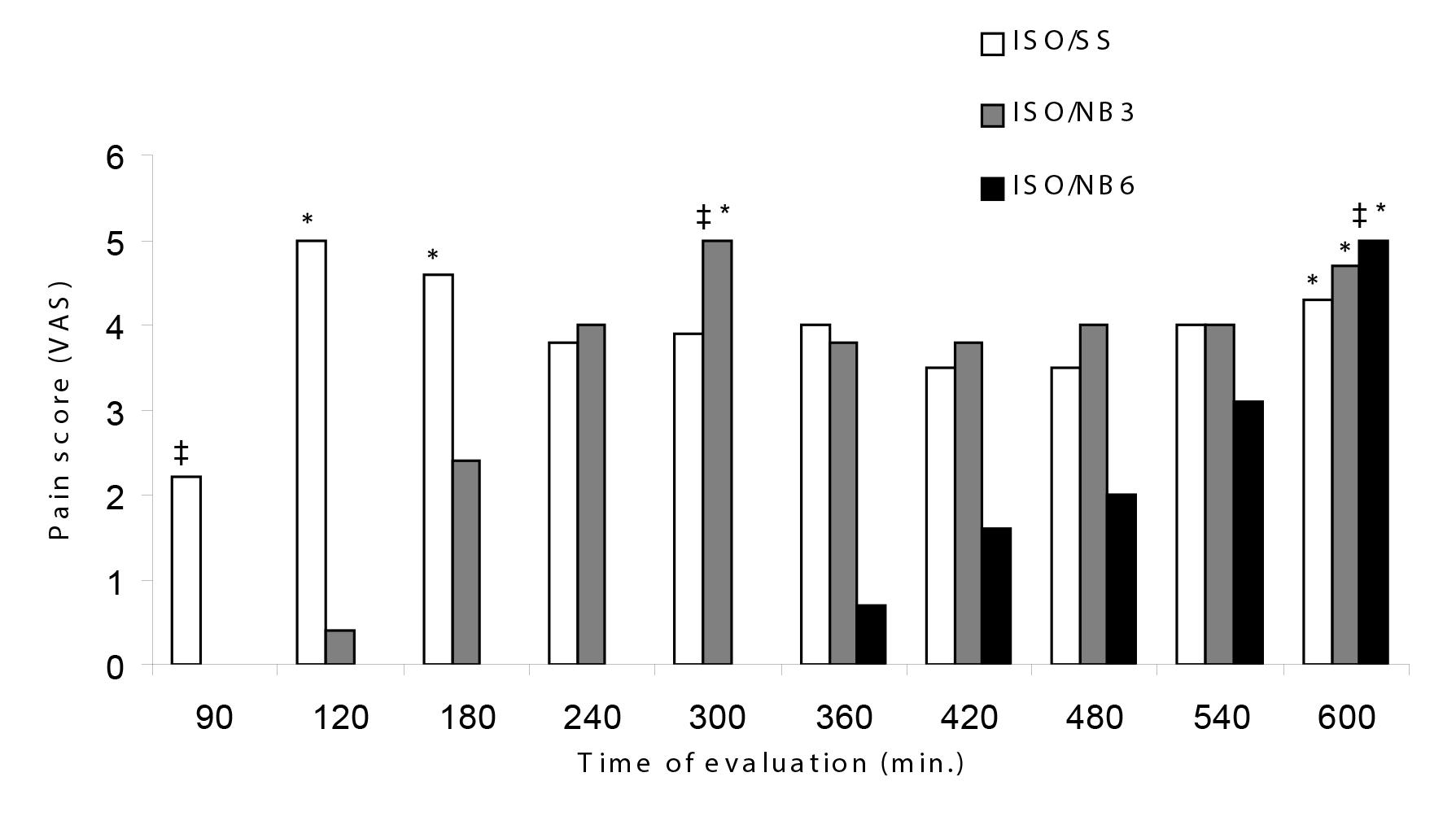
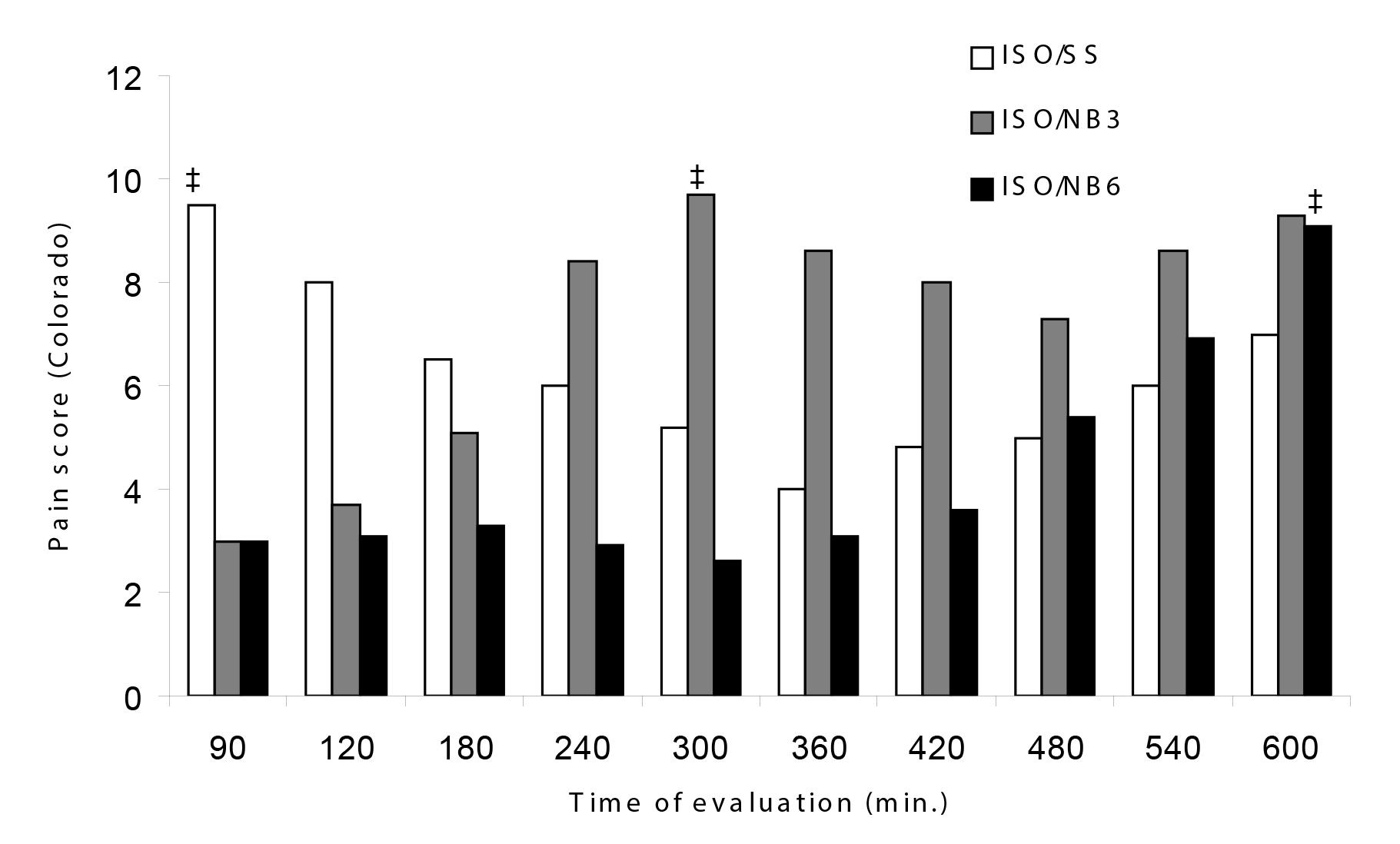
All dogs required the rescue analgesia (VAS score ≥ e 4 or Colorado score ≥ e 10) at any time point of the postoperative period. The VAS score determined when dogs meet the criteria for rescue analgesia between the two nalbuphine treatments, and it was higher compared to the control treatment. The highest VAS scores in the control treatment were recorded 90 min after surgery (median, 2; range, 0 to 4.0). The time to first rescue analgesic was also significantly different (p<0.05) between the nalbuphine treatments when compared to the control treatment and between the ISO/NB3 treatment (240-300 min) versus ISO/NB6 (540-600 min) (Figure 1; p<0.05). For sedation values, according to the same criteria (VAS scores), a decrease in both treatments with nalbuphine was observed with time (Figure 2). For analgesia and sedation, the Colorado score had the highest median value 90 min after surgery in the control treatment (median, 8.4; range 7-10) and was significantly lower for dogs receiving the ISO/NB3 or ISO/NB6 treatment. The Colorado scores were significantly lower in the ISO/NB6 treatment, compared with values for the ISO/NB3 treatment, at 240, 480, and 600 min (Figure 3).
Median pain scores from dogs administered epidurally saline (ISO/SS; 0.36 mL/kg), nalbuphine 0.3 mg/kg (ISO/NB3) or nalbuphine 0.6 mg/kg (ISO/NB6) determined between 90 and 600 min following ovariohysterectomy. Pain was scored using visual analogue system (VAS) on a scale of 0-10; increased scores were indicative of greater pain. ‡Time of the first analgesic rescue. *Significantly (p<0.05) different from value at 90 min.
Median sedation score in epidural saline (ISO/SS; 0.36 mL kg−1), nalbuphine 0.3 mg/kg (ISO/NB3) or nalbuphine 0.6 mg/kg (ISO/NB6) in dogs 90-600 min following ovariohysterectomy. Sedation was scored using visual analogue system (VAS, 0-10), where 10 is deep sedation and 0 represents agitation.
FIGURE 3- Median pain and sedation assessment (Colorado State University Veterinary Teaching Hospital scale) in the same dogs as in Figures 1 and 2. In this proposed score on a scale of 0-25; increased scores were indicative of greater pain and deep sedation. ‡Time of the first analgesic rescue. *Significantly (p<0.05) different from value at 90 min.
The heart rate, EtCO2, arterial oxygen saturation (SpO2), and arterial pressure (systolic arterial pressure, diastolic arterial pressure, and mean arterial pressure) did not change significantly among treatments or when compared with the basal values following epidural administration of ISO/SS, ISO/NB3 or ISO/NB6 treatments until the end of anaesthesia. (Tables 1 and 2). Body temperature was kept stable throughout anesthesia and surgery. There were no differences regarding the incidence of postoperative adverse effects. During the first 12 h following surgery none of the dogs had nausea or vomiting. Return to appetite or drinking water was delayed in control dogs (mean ± S.D., 13 ± 4 h), compared with dogs receiving ISO/NB3 (5 ± 2 h) or ISO/NB6 (3 ± 1 h).
Discussion
This study showed a sparing effect when the inhalant anesthetic agent isoflurane was combined with nalbuphine administered by the epidural route to dogs that underwent ovariohysterectomy. The MAC of isoflurane in our dogs receiving saline solution was 1.98% at approximately 2 h, which was higher than that measured by others for this species1616. Steffey EP, Howland D, Jr. Isoflurane potency in the dog and cat. Am J Vet Res. 1977;38(11):1833-6. , 1717. Pascoe PJ, Raekallio M, Kuusela E, McKusick B, Granholm M. Changes in the minimum alveolar concentration of isoflurane and some cardiopulmonary measurements during three continuous infusion rates of dexmedetomidine in dogs. Vet Anaesth Analg. 2006;33(2):97-103.. The ovarian stimulation model is an adequate and repeatable means of producing visceral stimulation to determine MAC in dogs1818. Boscan P, Monnet E, Mama K, Twedt DC, Congdon J, Eickhoff JC, Steffey EP. A dog model to study ovary, ovarian ligament and visceral pain. Vet Anaesth Analg. 2011;38(3):260-6.. Previous studies used electrical stimulation or mechanical stimuli (tail clamp) based on clinical signs such as palpebral response, jaw tone, and vigour of spontaneous movement in response to noxious stimulation, indicating that these dogs were not deeply anesthetized at the measured concentrations1616. Steffey EP, Howland D, Jr. Isoflurane potency in the dog and cat. Am J Vet Res. 1977;38(11):1833-6. , 1717. Pascoe PJ, Raekallio M, Kuusela E, McKusick B, Granholm M. Changes in the minimum alveolar concentration of isoflurane and some cardiopulmonary measurements during three continuous infusion rates of dexmedetomidine in dogs. Vet Anaesth Analg. 2006;33(2):97-103. , 1919. Grimm KA, Tranquilli WJ, Thurmon JC, Benson GJ. Duration of nonresponse to noxious stimulation after intramuscular administration of butorphanol, medetomidine, or a butorphanol-medetomidine combination during isoflurane administration in dogs. Am J Vet Res. 2000;61(1):42-7. , 2020. Machado CE, Dyson DH, Grant Maxie M. Effects of oxymorphone and hydromorphone on the minimum alveolar concentration of isoflurane in dogs. Vet Anaesth Analg. 2006;33(1):70-7.. Movement at skin incision has been proposed for determining the potency of intravenous anaesthetics2121. Ausems ME, Hug CC, Jr., Stanski DR, Burm AG. Plasma concentrations of alfentanil required to supplement nitrous oxide anesthesia for general surgery. Anesthesiology. 1986;65(4):362-73.; however, it is also used as a standard measure for assessment of inhalant anesthetic agents2222. Quasha AL, Eger EI, 2nd, Tinker JH. Determination and applications of MAC. Anesthesiology. 1980;53(4):315-34..
Currently, clinical and laboratory studies demonstrate the need to treat pain according to individual needs, pain source, pain mechanisms and drug properties2323. Cohen SP, Christo PJ, Moroz L. Pain management in trauma patients. Am J Phys Med Rehabil. 2004;83(2):142-61.. Epidural opioids have been shown to decrease the MAC of inhalant anaesthetics in dogs in a number of studies11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32. , 22. Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36. , 77. Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9. , 2424. Campagnol D, Teixeira-Neto FJ, Peccinini RG, Oliveira FA, Alvaides RK, Medeiros LQ. Comparison of the effects of epidural or intravenous methadone on the minimum alveolar concentration of isoflurane in dogs. Vet J. 2012;192(3):311-5.. Epidural methadone significantly reduces the isoflurane requirement compared with intravenous methadone during femoro-tibial joint surgery22. Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36.. In experimental studies using electrical stimulus, morphine and methadone administered epidurally in dogs reduced the anaesthetic requirement for halothane and isoflurane, respectively11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32. , 2424. Campagnol D, Teixeira-Neto FJ, Peccinini RG, Oliveira FA, Alvaides RK, Medeiros LQ. Comparison of the effects of epidural or intravenous methadone on the minimum alveolar concentration of isoflurane in dogs. Vet J. 2012;192(3):311-5.. In our study, the MAC of isoflurane in dogs was reduced by 26.3% and 38.4% by epidural nalbuphine at 0.3 and 0.6 mg/kg, respectively, when compared with the saline treatment. When compared between nalbuphine treatments, the reduction was 16.4%. The nalbuphine administered intravenously in dogs with a wide dose range (0.5, 1.5, 5.0, and 20.0 mg/kg) produced significant reduction of enflurane MAC (8%) with the lowest dose, with no additional reduction at higher doses2525. Murphy MR, Hug CC, Jr. The enflurane sparing effect of morphine, butorphanol, and nalbuphine. Anesthesiology. 1982;57(6):489-92.. To our knowledge, this is the first clinical study to verify that nalbuphine epidural administration reduces isoflurane requirements in surgical procedures in dogs. Previous studies with epidural nalbuphine in humans were only related to the control of postoperative pain1313. Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5. , 2626. Schmauss C, Doherty C, Yaksh TL. The analgesic effects of an intrathecally administered partial opiate agonist, nalbuphine hydrochloride. Eur J Pharmacol. 1982;86(1):1-7. and the avoidance of side effects induced by other epidural opioids2727. Pongraweewan O, Santawata U, Weerasarn L, Manuwong S, Swasti-xuto O. Epidural nalbuphine for post cesarean epidural morphine induced pruritus. J Med Assoc Thai. 2009;92(6):782-6..
Our study showed a dose-dependent analgesic effect of 0.3 and 0.6 mg/kg epidural nalbuphine compared with saline control in dogs undergoing ovariohysterectomy. This was reflected by the time required to first rescue analgesia (4.5 h compared with 9.5 h following nalbuphine 0.3 mg/kg or 0.6 mg/kg, respectively). Both nalbuphine treatments were associated with significantly lower pain scores on the VAS and Colorado pain scales compared with the control treatment in the first 10 h after epidural injections. The analgesia mediated by epidural nalbuphine is probably caused by potent μ-antagonist and κ-agonist opioid activity. Methadone administered by the epidural route to dogs that underwent femoro-tibial joint surgery had analgesia duration of approximately 7.5 h based on a numerical pain scoring system22. Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36.. These differences in the duration of analgesia may be related to the different drugs, and different subjective pain scales used in our study and those of others22. Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36. , 2424. Campagnol D, Teixeira-Neto FJ, Peccinini RG, Oliveira FA, Alvaides RK, Medeiros LQ. Comparison of the effects of epidural or intravenous methadone on the minimum alveolar concentration of isoflurane in dogs. Vet J. 2012;192(3):311-5.. The cortisol concentration is objective for determining physiologic or neurohumoral stress response in dogs; however, routine measurement of cortisol is clinically impractical2828. Grisneuax E, Pibarot P, Dupuis J, Blais D. Comparison of ketoprofen and carprofen administered prior to orthopedic surgery for control of post-operative pain in dogs. J Am Vet Med Assoc. 1999;215(8):1105-10..
One of the main advantages of epidural administration of opioids is that a small dose of the drugs provides pain relief in the postoperative period. However, there may be side effects. Side effects that occur more frequently after administration of epidural opioids are respiratory depression, pruritus, nausea, vomiting and urinary retention11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32. , 77. Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9. , 1212. Herperger LJ. Postoperative urinary retention in a dog following morphine with bupivacaine epidural analgesia. Can J Anaesth. 1998;39(10):650-2. , 1313. Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5.. Studies on opioids alone or in combination with local anaesthetics report conflicting results on respiratory depression. For instance, one study showed that epidural administration of morphine in dogs anesthetized with halothane was not associated with respiratory depression or other side effects11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32.. However, in another study respiratory depression was found to occur after epidural oxymorphone in dogs anesthetized with halothane77. Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9.. Nalbuphine 's μ-antagonism should produce fewer μ-mediated side effects such as respiratory depression1313. Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5.. In our study with nalbuphine epidural, although respiratory function was not thoroughly investigated, respiratory rate, SpO2, and EtCO2 remained within the physiological range. Mechanical ventilation used during general anesthesia, contributed to the respiratory parameters remained within the physiological parameters.
Despite systemic absorption and supraspinal effects, epidural administration of opioids is not expected to have a significant cardiovascular effect in healthy patients. Epidural administration of morphine in halothane- or isoflurane-anaesthetized dogs did not induce significant cardiovascular alterations11. Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32. , 2929. Pekcan Z, Koc B. The post-operative analgesic effects of epidurally administered morphine and transdermal fentanyl patch after ovariohysterectomy in dogs. Vet Anaesth Analg. 2010;37(6):557-65.. But other studies with other opioids have reported conflicting results for cardiovascular parameters. Epidural administration of oxymorphone in combination with bupivacaine in halothane-anesthetized dogs showed decreased heart rate and blood pressure77. Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9.. Another study showed a decrease in heart rate after epidural methadone in isoflurane-anesthetized dogs, but an increase in blood pressure (systolic arterial pressure)2424. Campagnol D, Teixeira-Neto FJ, Peccinini RG, Oliveira FA, Alvaides RK, Medeiros LQ. Comparison of the effects of epidural or intravenous methadone on the minimum alveolar concentration of isoflurane in dogs. Vet J. 2012;192(3):311-5.. We did not observe any alteration in the cardiovascular system with either dose of nalbuphine epidural in the present study during the anaesthetic period.
Conclusions
The nalbuphine administered epidurally at 0.3 and 0.6 mg/kg diluted in saline reduced the anesthetic requirement for isoflurane in ovariohysterectomized dogs in a dose-dependent manner. Similarly, nalbuphine epidural provided improved postoperative analgesia by increasing the time until the first rescue analgesia was needed. There were no side effects observed in this study.
References
-
1Valverde A, Dyson DH, McDonell WN. Epidural morphine reduces halothane MAC in the dog. Can J Anaesth. 1989;36(6):629-32.
-
2Leibetseder EN, Mosing M, Jones RS. A comparison of extradural and intravenous methadone on intraoperative isoflurane and postoperative analgesia requirements in dogs. Vet Anaesth Analg. 2006;33(2):128-36.
-
3Palmer CM, Cork RC, Hays R, Van Maren G, Alves D. The dose-response relation of intrathecal fentanyl for labor analgesia. Anesthesiology. 1998;88(2):355-61.
-
4Almeida TF, Fantoni DT, Mastrocinque S, Tatarunas AC, Imagawa VH. Epidural anesthesia with bupivacaine, bupivacaine and fentanyl, or bupivacaine and sufentanil during intravenous administration of propofol for ovariohysterectomy in dogs. J Am Vet Med Assoc. 2007;230(1):45-51.
-
5Cohen SE, Tan S, White PF. Sufentanil analgesia following cesarean section: epidural versus intravenous administration. Anesthesiology. 1988;68(1):129-34.
-
6Herman NL, Sheu KL, Van Decar TK, Rubin JD, Gadalla F, Koff HD, Reynolds JE. Determination of the analgesic dose-response relationship for epidural fentanyl and sufentanil with bupivacaine 0.125% in laboring patients. J Clin Anesth. 1998;10(8):670-7.
-
7Torske KE, Dyson DH, Pettifer G. End tidal halothane concentration and postoperative analgesia requirements in dogs: a comparison between intravenous oxymorphone and epidural bupivacaine alone and in combination with oxymorphone. Can J Anaesth. 1998;39(6):361-9.
-
8Pascoe PJ, Dyson DH. Analgesia after lateral thoracotomy in dogs. Epidural morphine vs. intercostal bupivacaine. Vet Surg. 1993;22(2):141-7.
-
9Marucio RL, Luna SP, Neto FJ, Minto BW, Hatschbach E. Postoperative analgesic effects of epidural administration of neostigmine alone or in combination with morphine in ovariohysterectomized dogs. Am J Vet Res. 2008;69(7):854-60.
-
10Abelson AL, Armitage-Chan E, Lindsey JC, Wetmore LA. A comparison of epidural morphine with low dose bupivacaine versus epidural morphine alone on motor and respiratory function in dogs following splenectomy. Vet Anaesth Analg. 2011;38(3):213-23.
-
11Campoy L, Martin-Flores M, Ludders JW, Erb HN, Gleed RD. Comparison of bupivacaine femoral and sciatic nerve block versus bupivacaine and morphine epidural for stifle surgery in dogs. Vet Anaesth Analg. 2012;39(1):91-8.
-
12Herperger LJ. Postoperative urinary retention in a dog following morphine with bupivacaine epidural analgesia. Can J Anaesth. 1998;39(10):650-2.
-
13Fournier R, Van Gessel E, Macksay M, Gamulin Z. Onset and offset of intrathecal morphine versus nalbuphine for postoperative pain relief after total hip replacement. Acta Anaesthesiol Scand. 2000;44(8):940-5.
-
14Arnould JF, Pinaud M. Pharmacology of nalbuphine. Ann Fr Anesth Reanim. 1992;11(2):221-8.
-
15Hellyer PW, Gaynor JS. Acute postsurgical pain in dogs and cats. Comp Cont Edu Pract. Vet. 1998;20(2):140-53.
-
16Steffey EP, Howland D, Jr. Isoflurane potency in the dog and cat. Am J Vet Res. 1977;38(11):1833-6.
-
17Pascoe PJ, Raekallio M, Kuusela E, McKusick B, Granholm M. Changes in the minimum alveolar concentration of isoflurane and some cardiopulmonary measurements during three continuous infusion rates of dexmedetomidine in dogs. Vet Anaesth Analg. 2006;33(2):97-103.
-
18Boscan P, Monnet E, Mama K, Twedt DC, Congdon J, Eickhoff JC, Steffey EP. A dog model to study ovary, ovarian ligament and visceral pain. Vet Anaesth Analg. 2011;38(3):260-6.
-
19Grimm KA, Tranquilli WJ, Thurmon JC, Benson GJ. Duration of nonresponse to noxious stimulation after intramuscular administration of butorphanol, medetomidine, or a butorphanol-medetomidine combination during isoflurane administration in dogs. Am J Vet Res. 2000;61(1):42-7.
-
20Machado CE, Dyson DH, Grant Maxie M. Effects of oxymorphone and hydromorphone on the minimum alveolar concentration of isoflurane in dogs. Vet Anaesth Analg. 2006;33(1):70-7.
-
21Ausems ME, Hug CC, Jr., Stanski DR, Burm AG. Plasma concentrations of alfentanil required to supplement nitrous oxide anesthesia for general surgery. Anesthesiology. 1986;65(4):362-73.
-
22Quasha AL, Eger EI, 2nd, Tinker JH. Determination and applications of MAC. Anesthesiology. 1980;53(4):315-34.
-
23Cohen SP, Christo PJ, Moroz L. Pain management in trauma patients. Am J Phys Med Rehabil. 2004;83(2):142-61.
-
24Campagnol D, Teixeira-Neto FJ, Peccinini RG, Oliveira FA, Alvaides RK, Medeiros LQ. Comparison of the effects of epidural or intravenous methadone on the minimum alveolar concentration of isoflurane in dogs. Vet J. 2012;192(3):311-5.
-
25Murphy MR, Hug CC, Jr. The enflurane sparing effect of morphine, butorphanol, and nalbuphine. Anesthesiology. 1982;57(6):489-92.
-
26Schmauss C, Doherty C, Yaksh TL. The analgesic effects of an intrathecally administered partial opiate agonist, nalbuphine hydrochloride. Eur J Pharmacol. 1982;86(1):1-7.
-
27Pongraweewan O, Santawata U, Weerasarn L, Manuwong S, Swasti-xuto O. Epidural nalbuphine for post cesarean epidural morphine induced pruritus. J Med Assoc Thai. 2009;92(6):782-6.
-
28Grisneuax E, Pibarot P, Dupuis J, Blais D. Comparison of ketoprofen and carprofen administered prior to orthopedic surgery for control of post-operative pain in dogs. J Am Vet Med Assoc. 1999;215(8):1105-10.
-
29Pekcan Z, Koc B. The post-operative analgesic effects of epidurally administered morphine and transdermal fentanyl patch after ovariohysterectomy in dogs. Vet Anaesth Analg. 2010;37(6):557-65.
-
1
Research performed at Division of Operative Technique and Experimental Surgery, Department of Surgery, Federal University of Mato Grosso do Sul (UFMS), Campo Grande-MS, Brazil.
-
Financial source: none
Publication Dates
-
Publication in this collection
Jan 2014
History
-
Received
12 Sept 2013 -
Reviewed
14 Nov 2013 -
Accepted
12 Dec 2013