Abstract
Purpose:
To evaluate the response of aging rats with sepsis to two different antibiotic regimens.
Methods:
The study was conducted with 30 aging rats (18 month-old) with autologous feces peritonitis. The animals were divided into three groups: Group 0 received no therapeutic intervention (control), while Group 1 received a single dose of 40 mg/kg meropenem and Group 2 received a single dose of 20 mg/kg moxifloxacin. The intervention in both Groups was made 6 hours after induction of peritonitis. The animals were followed up to 15 days for evaluating morbidity and mortality. The weights at baseline were similar in all groups.
Results:
At the end of follow-up, weight loss was significantly greater (p=0.0045) in Group 0 (non-intervention controls). Culture from a blood sample at the end of follow-up was positive in all the animals in Group 0, in two animals in Group 1 and in four animals in Group 2. Morbidity/mortality was significantly higher in Group 0 compared to both Groups 1 and 2 (p=0.003) but the scores were not significantly different between Groups 1 and 2 (p=0.6967).
Conclusion:
Both antibiotic regimens rendered promising results for the treatment of fecal peritonitis.
Key words:
Peritonitis; Carbapenems; Quinolones; Aging; Rats.
Introduction
Sepsis is a severe clinical condition and a common consequence of several infectious diseases. Clinical progression is generally extremely rapid due to an underlying uncontrolled immune response that leads to multiple organ failure with high associated morbidity and mortality rates11 Ludy MJ, Moore GE, Mattes RD. The effects of capsaicin and capsiate on energy balance: critical review and meta-analyses of studies in humans. Chem Senses. 2012;37:103-21. doi: 10.1093/chemse/bjr100.
https://doi.org/10.1093/chemse/bjr100...
2 Wai K, Yazawa A, Watanabe T. Roles as metabolic regulators of the non-nutrients, capsaicin and capsiate, supplemented to diets. Proc Jpn Acad. 2003;79:207-12. doi: 10.2183/pjab.79B.207.
https://doi.org/10.2183/pjab.79B.207...
3 Kobata K, Sutoh K, Todo T, Yazawa S, Iwai K, Watanabe T. Nordihydrocapsiate, a new capsinoid from the fruits of a nonpungent pepper, Capsicum annuum. J Nat Prod. 1999;62(2):335-6. doi: 10.1021/np9803373.
https://doi.org/10.1021/np9803373...
-44 Luo XJ, Peng J, Li YJ. Recent advances in the study on capsaicinoids and capsinoids. Eur J Pharmacol. 2011;650(1):1-7. doi: 10.1016/j.ejphar.2010.09.074.
https://doi.org/10.1016/j.ejphar.2010.09...
.
Populations are aging worldwide, with estimates suggesting that by 2050 more than 20% of the world’s population will be at least 60 years of age55 Kobata K, Toda T, Yazawa S, Iwai K, Watanabe T. Novel capsaicinoid like substances, capsiate and dihydrocapsiate, from the fruits of a nonpungent cultivar, CH-19 Sweet, of pepper (Capsicum annuum L.). J Agric Food Chem. 1998;46:1695-7. doi: 10.1021/jf980135c.
https://doi.org/10.1021/jf980135c...
. This increase in life expectancy heralds a predictable increase in the incidence and severity of many diseases. To a considerable extent, this scenario is the result of the comorbidities typically found in this age group, as well as of age-related immunosenescence11 Ludy MJ, Moore GE, Mattes RD. The effects of capsaicin and capsiate on energy balance: critical review and meta-analyses of studies in humans. Chem Senses. 2012;37:103-21. doi: 10.1093/chemse/bjr100.
https://doi.org/10.1093/chemse/bjr100...
,66 Ohnuki K, Niwa S, Maeda S, Inoue N, Yazawa S, Fushiki T. CH-19 sweet, a non-pungent cultivar of red pepper, increased body temperature and oxygen consumption in humans. Biosci Biotechnol Biochem. 2001;65(9):2033-6.,77 Macho A, Lucena C, Sancho R, Daddario N, Minassi A, Muñoz E, Appendino G. Non-pungent capsaicinoids from sweet pepper synthesis and evaluation of the chemopreventive and anticancer potential. Eur J Nutr. 2003;42(1):2-9. doi: 10.1007/s00394-003-0394-6.
https://doi.org/10.1007/s00394-003-0394-...
.
The incidence of sepsis has increased in the population in general and particularly in individuals who underwent surgery. This is especially evident in the elderly population when mortality rates are higher88 Lee EJ, Jeon MS, Kim BD, Kim JH, Kwon YG, Lee H, Lee YS, Yang JH, Kim TY. Capsiate inhibits ultraviolet B-induced skin inflammation by inhibiting Src family kinases and epidermal growth factor receptor signaling. Free Radic Biol Med. 2010;48(9):1133-43. doi: 10.1016/j.freeradbiomed.2010.01.034.
https://doi.org/10.1016/j.freeradbiomed....
9 Pyun BJ, Choi S, Lee Y, Kim TW, Min JK, Kim Y, Kim BD, Kim JH, Kim TY, Kim YM, Kwon YG. Capsiate, a nonpungent capsaicin-like compound, inhibits angiogenesis and vascular permeability via a direct inhibition of Src kinase activity. Cancer Res. 2008;68(1):227-35. doi: 10.1158/0008-5472.CAN-07-2799.
https://doi.org/10.1158/0008-5472.CAN-07...
10 Haramizu S, Kawabata F, Ohnuki K, Inoue N, Watanabe T, Yazawa S, Fushiki T. Capsiate, a non-pungent capsaicin analog, reduces body fat without weight rebound like swimming exercise in mice. Biomed Res. 2011;32(4):279-84. doi: 10.2220/biomedres.32.279.
https://doi.org/10.2220/biomedres.32.279...
11 Kwon DY, Kim YS, Ryu SY, Cha MR, Yon GH, Yang HJ, Kim MJ, Kang S, Park S. Capsiate improves glucose metabolism by improving insulin sensitivity better than capsaicin in diabetic rats. J Nutr Biochem. 2013;24(6):1078-85. doi: 10.1016/j.jnutbio.2012.08.006.
https://doi.org/10.1016/j.jnutbio.2012.0...
-1212 Li NS, Luo XJ, Dai Z, Liu B, Zhang YS, Yang ZC, Peng J. Beneficial effects of capsiate on ethanol-induced mucosal injury in rats are related to stimulation of calcitonin gene-related peptide release. Planta Med. 2012;78(1):24-30. doi: 10.1055/s-0031-1280217.
https://doi.org/10.1055/s-0031-1280217...
. Patients over 65 years of age already account for more than half of all admissions to intensive care units in the United States, with mortality rate that exceeds 30%1313 Forte GC, Schneider AP. Modulação do gasto energético pela ingestão de capsaicina, cafeína e catequinas: uma revisão sistemática. RBONE. 2012;6(35):207-15.. Explanations include the increase number of invasive procedures performed, and the use of immunosuppressants and aggressive surgeries in this population88 Lee EJ, Jeon MS, Kim BD, Kim JH, Kwon YG, Lee H, Lee YS, Yang JH, Kim TY. Capsiate inhibits ultraviolet B-induced skin inflammation by inhibiting Src family kinases and epidermal growth factor receptor signaling. Free Radic Biol Med. 2010;48(9):1133-43. doi: 10.1016/j.freeradbiomed.2010.01.034.
https://doi.org/10.1016/j.freeradbiomed....
.
Although the focus of much research, little has changed in the management of patients with sepsis over recent decades, the information acquired from basic research has resulted in interventions that are of little or no effect at all in humans, and this may be a consequence of dissociation between the real world, in which more than 60% of the cases of sepsis occur in individuals over 60 years of age, and experimental research, where the majority of the animals studied are young77 Macho A, Lucena C, Sancho R, Daddario N, Minassi A, Muñoz E, Appendino G. Non-pungent capsaicinoids from sweet pepper synthesis and evaluation of the chemopreventive and anticancer potential. Eur J Nutr. 2003;42(1):2-9. doi: 10.1007/s00394-003-0394-6.
https://doi.org/10.1007/s00394-003-0394-...
,1414 Barros PP, Silva GH, Gonçalves GMS, Oliveira JC, Pagnan LG, Arco-e-Flexa L. Hepatoprotective effect of quercetin pretreatment against paracetamol-induced liver damage and partial hepatectomy in rats. Braz Arch Biol Technol. 2017;60(e16160138): 1-10. doi: 10.1590/1678-4324-2016160138.
https://doi.org/10.1590/1678-4324-201616...
15 Higgins GM, Anderson RM. Experimental pathology of the liver. I. Restoration of the liver of the white rat following partial surgical removal. Arch Pathol. 1931;12:186-202. doi: 10.2353/ajpath.2010.090675.
https://doi.org/10.2353/ajpath.2010.0906...
16 Fiszer-Szafarz B, Nadal C. Lysosomal enzyme activities in the regenerating rat liver. Cancer Res. 1977;37(2):354-7. PMID: 832261.
17 Bitencourt S, Basso B, Mesquita FC, Oliveira JR. Capsaicin modulates proliferation, migration, and activation of hepatic stellate cells. Cell Biochem Biophys. 2013;1:1-6. doi: 10.1007/s12013-013-9719-0.
https://doi.org/10.1007/s12013-013-9719-...
18 Macho A, Sancho R, Minassi A, Appendino G, Lawen A, Munoz E. Involvement of reactive oxygen species in capsaicinoid-induced apoptosis in transformed cells. Free Radic Res. 2003;37:611-9. doi: 10.1080/1071576031000083215.
https://doi.org/10.1080/1071576031000083...
-1919 Pierce AA, Duwaerts CC, Siao K, Mattis AN, Goodsell A, Baron JL, Maher JJ. CD18 deficiency improves liver injury in the MCD model of steatohepatitis. Plos One. 2017;12(9):1-16. doi: 10.1371/journal.pone.0183912.
https://doi.org/10.1371/journal.pone.018...
.
Carbapenems and quinolones, among others, have been used to treat severe, intra-abdominal sepsis, since these are effective antibiotics against the principal etiologic agents; however, there is no clear evidence of the superiority of one regimen over the other2020 Takanohashi T, Isaka M, Ubukata K, Mihara R, Bernard BK. Studies of the toxicological potential of capsinoids, XIII: inhibitory effects of capsaicin and capsinoids on cytochrome P450 3A4 in human liver microsomes. Int J Toxicol. 2008;27(3):119-36. doi: 10.1177/1091581809360282.
https://doi.org/10.1177/1091581809360282...
-23.
The objective of the present study was to evaluate the therapeutic response to two different antibiotic regimens in aging rats in which peritonitis was induced using autologous feces.
Methods
The rats were cared for in accordance with the “Guide for the Care and Use of Laboratory Animals” and the study was conducted respecting the ethical principles in animal experimentation. The animal ethics committee (CEUA/CESED) approved the study protocol under number 0022/03092012-1.
This was a prospective, analytical, experimental study with 30 male Wistar rats (Rattus norvegicus). All the animals were adult rats of 18 months of age with no illness or disease. The animals were kept in polypropylene cages measuring 43 x 43 x 20 cm at a controlled temperature of 23 ± 1oC and 12-hour light/dark cycles. Access to food and drink was ad libitum, with food consisting of a nutritionally balanced rodent diet.
The animals were divided into three groups: the non-intervention control group (Group 0), the meropenem group (Group 1) and the moxifloxacin group (Group 2). On day 1 of the experiment, peritonitis was induced in all the animals using a 10% solution prepared with autogenous feces, i.e. 2 grams of feces collected from each rat were diluted and homogenized in 20 ml of 0.9% saline. All the animals in the three groups were inoculated with their respective solution at a dose of 4 ml/kg of weight, a dose that had been confirmed as sub-lethal for that age in a previous study24. In Groups 1 and 2, a therapeutic intervention was performed six hours after peritonitis was induced, with treatment consisting of a single 40-mg/kg dose of meropenem for the animals in Group 1 and a single 20-mg/kg dose of moxifloxacin for those in Group 2.
The animals’ activity, weight, body temperature and respiratory rate with the aim of detecting severe infection were monitored. All the animals that died during follow-up underwent inspection of the abdominal cavity through a midline incision from the xiphoid process to the pubic symphysis. The incision was made using surgical scissors. The inspection aimed to identify abscesses, adherences and macroscopic signs of infection such as pus in the abdominal cavity or in solid organs. At the evaluation moment, using a 30 x 1.5 mm needle, 2 ml of blood were collected from the abdominal aorta and stored into blood culture bottles. After incubation at 35 ± 2oC for 24 hours, blood agar plates were inoculated.
At day 15, the animals that had survived the entire follow-up period were euthanized by intravenous administration of 50 mg/kg ketamine hydrochloride and 10 mg/kg xylazine hydrochloride. They were then submitted to the same protocol of incision, inspection and blood culture described above.
Morbidity and mortality in the animals were stratified by applying a validated score24,25 based on the findings detected after the induction of fecal peritonitis:
Scores 0-3: death before day 15
-
0: death from septic shock in the first 24 hours;
-
1: death between 24 and 48 hours;
-
2: death between 48 hours and 8 days, with obvious clinical signs of severe infection;
-
3: death between 8 and 15 days, with obvious clinical signs of severe infection.
Scores 4-10: survival until day 15, followed by euthanasia
-
4: positive blood culture, moderate clinical signs of infection; abscesses found in the thoracic and abdominal cavities;
-
5: positive blood culture, no clinical signs of infection, abscesses found in the thoracic and abdominal cavities;
-
6: positive blood culture, no clinical signs of infection, abscesses found in the abdominal cavity alone;
-
7: negative blood culture, no clinical signs of infection, abscesses found in the abdominal and thoracic cavities;
-
8: negative blood culture, abscesses found in the abdominal cavity alone;
-
9: negative blood culture, only one small abscess found in the abdominal cavity;
-
10: negative blood culture, no abscess found in the cavities.
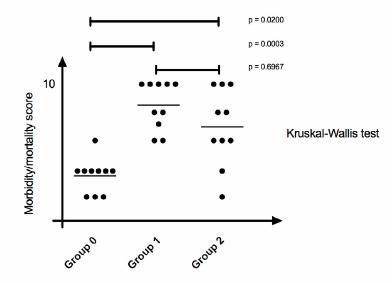
The quantitative variables were described as means and standard deviations. The qualitative variables were expressed as absolute and relative frequencies. The Kruskal-Wallis test was used to evaluate possible differences between the morbidity and mortality scores in the three groups. Dunn’s post-hoc test was then used to evaluate possible group-to-group differences. Analysis of variance (ANOVA) was used to compare the weights of the animals in the three groups. The entire statistical analysis was performed using the Graphpad Prism program, version 7. P-values <0.05 were used to reject the null hypothesis.
Results
Prior to the induction of peritonitis, the mean weight of the animals in Groups 0, 1 and 2 was 402.5 ± 24.2 grams, 416.2 ± 37.4 grams and 380.8 ± 48.5 grams, respectively, highlighting the similarity of the groups (Figure 1). The difference between the initial weight and the final weight of the animals in the three groups is shown in Table 1. Weight loss was significantly greater in the non-intervention control group compared to the two intervention groups; however, Groups 1 and 2 did not differ from each other (Figure 2).
Before the 15-day follow-up was complete, 3 deaths occurred in the control group (Group 0), none in the meropenem group (Group 1) and 1 in the moxifloxacin group (Group 2).
The findings in the cavities varied considerably, with results showing diffuse peritonitis, or single and multiple, intact or ruptured internal abscesses located both in the abdomen and in other organs such as the liver, kidneys and lungs (Figure 3).
Diffuse peritonitis and abscesses located at different sites. A. Diffuse peritonitis; B. Multiple abscesses; C. Internal abscesses; D. Liver abscesses; E. Kidney abscesses; F. Lung abscesses.
Blood culture was positive for all the animals in the control group. Of those submitted to meropenem treatment (Group 1), blood culture was positive in only two, while in Group 2 blood culture was positive in four animals (Table 2).
In Table 3 one can observe the morbidity and mortality scores for each group at the end of follow-up. Analysis of the morbidity and mortality scores, performed using the Kruskal-Wallis test, showed differences between the groups (p=0.003). Following application of Dunn’s multiple comparison test, the difference between the non-intervention control group and the intervention groups was found to be significant. There was no difference between the scores obtained for Group 1 (meropenem) and Group 2 (moxifloxacin) (p=0.6967) (Figure 4).
Discussion
This study provides a pioneering comparative analysis of two treatment strategies for severe sepsis in a population of aging rats. Sepsis was confirmed by positive blood culture in all the animals that were not submitted to any antibiotic intervention, with mortality rate as high as 30% in that group. Both interventions proved superior to the non-intervention control group, with no difference between the two treatment regimens according to a scoring system previously used in other studies24,25. The antibacterial effectiveness of both meropenem and moxifloxacin was confirmed, and there was a reduction in the extent and severity of the infection with both drugs.
There are some limitations associated with this study that need to be mentioned. Although the weight of the animals in the different groups was similar at baseline, their allocation to the groups was not randomized. Additionally, the clinical signs of sepsis could have been better monitored if heart rate, respiratory rate and blood pressure had been measured, indicating a failure to adequately evaluate the severity of sepsis. New monitoring devices such as those used in intensive care could have been useful for monitoring the animals26. The fact that all the animals were of the same sex also merits reflection, since men and women respond differently to infection27. Finally, neglecting to administer resuscitation fluids, which is routine conduct in clinical practice, distances this experiment from the usual management of patients with sepsis.
Despite the fact that the majority of cases of sepsis in humans occur in the elderly, reports on experimental models have frequently omitted the animals age or the models used have involved young animals with no comorbidities, rendering it inappropriate to extrapolate the results found in those studies to the real world.
Although the use of experimental sepsis models plays an important role in understanding the condition, dozens of therapeutic interventions such as corticoids, anti-cytokine antibodies and antithrombin III that proved successful in experimental research failed in clinical trials1616 Fiszer-Szafarz B, Nadal C. Lysosomal enzyme activities in the regenerating rat liver. Cancer Res. 1977;37(2):354-7. PMID: 832261.. Therefore, there appears to be clear dissociation between basic and clinical research. Nevertheless, the inability to translate knowledge acquired in experimental research to clinical trials should not preclude basic research. On the contrary, this should serve as a challenge to research groups to create models that more closely mimic human responses to infectious conditions. In this respect, the development of the so-called “humanized rodents,” in which hematopoietic stem cells are transplanted to the rodents allowing them to acquire a functional immune system similar to that of humans, appears to represent a promising model28. Up to the present time, however, the data obtained remain limited.
Conclusions
Sepsis remains an extremely serious condition, particularly in the elderly. Meropenem and moxifloxacin proved to be effective strategies for the treatment of abdominal sepsis in aging rats.
References
-
1Ludy MJ, Moore GE, Mattes RD. The effects of capsaicin and capsiate on energy balance: critical review and meta-analyses of studies in humans. Chem Senses. 2012;37:103-21. doi: 10.1093/chemse/bjr100.
» https://doi.org/10.1093/chemse/bjr100 -
2Wai K, Yazawa A, Watanabe T. Roles as metabolic regulators of the non-nutrients, capsaicin and capsiate, supplemented to diets. Proc Jpn Acad. 2003;79:207-12. doi: 10.2183/pjab.79B.207.
» https://doi.org/10.2183/pjab.79B.207 -
3Kobata K, Sutoh K, Todo T, Yazawa S, Iwai K, Watanabe T. Nordihydrocapsiate, a new capsinoid from the fruits of a nonpungent pepper, Capsicum annuum. J Nat Prod. 1999;62(2):335-6. doi: 10.1021/np9803373.
» https://doi.org/10.1021/np9803373 -
4Luo XJ, Peng J, Li YJ. Recent advances in the study on capsaicinoids and capsinoids. Eur J Pharmacol. 2011;650(1):1-7. doi: 10.1016/j.ejphar.2010.09.074.
» https://doi.org/10.1016/j.ejphar.2010.09.074 -
5Kobata K, Toda T, Yazawa S, Iwai K, Watanabe T. Novel capsaicinoid like substances, capsiate and dihydrocapsiate, from the fruits of a nonpungent cultivar, CH-19 Sweet, of pepper (Capsicum annuum L.). J Agric Food Chem. 1998;46:1695-7. doi: 10.1021/jf980135c.
» https://doi.org/10.1021/jf980135c -
6Ohnuki K, Niwa S, Maeda S, Inoue N, Yazawa S, Fushiki T. CH-19 sweet, a non-pungent cultivar of red pepper, increased body temperature and oxygen consumption in humans. Biosci Biotechnol Biochem. 2001;65(9):2033-6.
-
7Macho A, Lucena C, Sancho R, Daddario N, Minassi A, Muñoz E, Appendino G. Non-pungent capsaicinoids from sweet pepper synthesis and evaluation of the chemopreventive and anticancer potential. Eur J Nutr. 2003;42(1):2-9. doi: 10.1007/s00394-003-0394-6.
» https://doi.org/10.1007/s00394-003-0394-6 -
8Lee EJ, Jeon MS, Kim BD, Kim JH, Kwon YG, Lee H, Lee YS, Yang JH, Kim TY. Capsiate inhibits ultraviolet B-induced skin inflammation by inhibiting Src family kinases and epidermal growth factor receptor signaling. Free Radic Biol Med. 2010;48(9):1133-43. doi: 10.1016/j.freeradbiomed.2010.01.034.
» https://doi.org/10.1016/j.freeradbiomed.2010.01.034 -
9Pyun BJ, Choi S, Lee Y, Kim TW, Min JK, Kim Y, Kim BD, Kim JH, Kim TY, Kim YM, Kwon YG. Capsiate, a nonpungent capsaicin-like compound, inhibits angiogenesis and vascular permeability via a direct inhibition of Src kinase activity. Cancer Res. 2008;68(1):227-35. doi: 10.1158/0008-5472.CAN-07-2799.
» https://doi.org/10.1158/0008-5472.CAN-07-2799 -
10Haramizu S, Kawabata F, Ohnuki K, Inoue N, Watanabe T, Yazawa S, Fushiki T. Capsiate, a non-pungent capsaicin analog, reduces body fat without weight rebound like swimming exercise in mice. Biomed Res. 2011;32(4):279-84. doi: 10.2220/biomedres.32.279.
» https://doi.org/10.2220/biomedres.32.279 -
11Kwon DY, Kim YS, Ryu SY, Cha MR, Yon GH, Yang HJ, Kim MJ, Kang S, Park S. Capsiate improves glucose metabolism by improving insulin sensitivity better than capsaicin in diabetic rats. J Nutr Biochem. 2013;24(6):1078-85. doi: 10.1016/j.jnutbio.2012.08.006.
» https://doi.org/10.1016/j.jnutbio.2012.08.006 -
12Li NS, Luo XJ, Dai Z, Liu B, Zhang YS, Yang ZC, Peng J. Beneficial effects of capsiate on ethanol-induced mucosal injury in rats are related to stimulation of calcitonin gene-related peptide release. Planta Med. 2012;78(1):24-30. doi: 10.1055/s-0031-1280217.
» https://doi.org/10.1055/s-0031-1280217 -
13Forte GC, Schneider AP. Modulação do gasto energético pela ingestão de capsaicina, cafeína e catequinas: uma revisão sistemática. RBONE. 2012;6(35):207-15.
-
14Barros PP, Silva GH, Gonçalves GMS, Oliveira JC, Pagnan LG, Arco-e-Flexa L. Hepatoprotective effect of quercetin pretreatment against paracetamol-induced liver damage and partial hepatectomy in rats. Braz Arch Biol Technol. 2017;60(e16160138): 1-10. doi: 10.1590/1678-4324-2016160138.
» https://doi.org/10.1590/1678-4324-2016160138 -
15Higgins GM, Anderson RM. Experimental pathology of the liver. I. Restoration of the liver of the white rat following partial surgical removal. Arch Pathol. 1931;12:186-202. doi: 10.2353/ajpath.2010.090675.
» https://doi.org/10.2353/ajpath.2010.090675 -
16Fiszer-Szafarz B, Nadal C. Lysosomal enzyme activities in the regenerating rat liver. Cancer Res. 1977;37(2):354-7. PMID: 832261.
-
17Bitencourt S, Basso B, Mesquita FC, Oliveira JR. Capsaicin modulates proliferation, migration, and activation of hepatic stellate cells. Cell Biochem Biophys. 2013;1:1-6. doi: 10.1007/s12013-013-9719-0.
» https://doi.org/10.1007/s12013-013-9719-0 -
18Macho A, Sancho R, Minassi A, Appendino G, Lawen A, Munoz E. Involvement of reactive oxygen species in capsaicinoid-induced apoptosis in transformed cells. Free Radic Res. 2003;37:611-9. doi: 10.1080/1071576031000083215.
» https://doi.org/10.1080/1071576031000083215 -
19Pierce AA, Duwaerts CC, Siao K, Mattis AN, Goodsell A, Baron JL, Maher JJ. CD18 deficiency improves liver injury in the MCD model of steatohepatitis. Plos One. 2017;12(9):1-16. doi: 10.1371/journal.pone.0183912.
» https://doi.org/10.1371/journal.pone.0183912 -
20Takanohashi T, Isaka M, Ubukata K, Mihara R, Bernard BK. Studies of the toxicological potential of capsinoids, XIII: inhibitory effects of capsaicin and capsinoids on cytochrome P450 3A4 in human liver microsomes. Int J Toxicol. 2008;27(3):119-36. doi: 10.1177/1091581809360282.
» https://doi.org/10.1177/1091581809360282 -
21Kodama T, Watanabe E, Masuyama T, Tsubuku S, Otabe A, Mochizuki M, Bernard BK. Studies of the toxicological potential of capsinoids: II. A 26-week daily gavage dosing toxicity study of CH-19 Sweet extract in rats. Int J Toxicol. 2008;27(Suppl 3):11-27. doi: 10.1080/10915810802513379.
» https://doi.org/10.1080/10915810802513379
-
Financial source:
none
-
1
Research performed at Experimental Research Unit, UNIFACISA, Medical Sciences, Faculty of Campina Grande (FCM), Brazil. Part of PhD degree thesis, Postgraduate Program in Surgery, Universidade Federal de Pernambuco (UFPE). Tutor: Prof. Carlos Teixeira Brandt.
Publication Dates
-
Publication in this collection
May 2018
History
-
Received
18 Jan 2018 -
Reviewed
20 Mar 2018 -
Accepted
23 Apr 2018